Abstract
Purpose:
To summarize COVID-19 research endeavors by ophthalmologists/researchers in terms of publication numbers, journals and author countries, and to detail key findings.
Methods:
The LitCovid database was systematically reviewed for ophthalmology-focused COVID-19 articles. The quality of the evidence was assessed for articles investigating conjunctivitis in COVID-19 patients.
Results:
There were 21,364 articles in LitCovid on June 12, 2020, of which 215 (1%) were ophthalmology-focused. Of articles on COVID-19 transmission, 3.3% were ophthalmology-focused. Ophthalmology-focused articles were published in 68 journals and originated from 25 countries. The top five countries publishing ophthalmology-focused articles (China, India, United States of America, Italy, and United Kingdom) produced 145/215 (67%) articles. A total of 16 case reports/series from eight countries reported that conjunctivitis can be the initial or the only symptom of COVID-19 infection. Conjunctivitis may occur in the middle phase of COVID-19 illness. A total of 10 hospital-based cross-sectional studies reported that between 0% and 31.6% of COVID-19 patients have conjunctivitis or other ocular conditions, with a pooled prevalence of 5.5% reported in a meta-analysis. Viral RNA was detected in conjunctival swabs of patients with and without ocular manifestations, after resolution of conjunctivitis, after nasopharyngeal swabs turned negative and in retina of deceased COVID-19 patients.
Conclusion:
Within 3 months of declaring the COVID-19 pandemic, 215 ophthalmology-focused articles were published in PubMed, concentrating on disease manifestations and transmission. The reported presence of conjunctivitis or other ocular conditions in COVID-19 patients is varied. Clinicians should be alert for ocular involvement in COVID-19 infections and possible ocular transmission even in patients without ocular symptoms.
Introduction
In December 2019, a series of pneumonia cases of unknown cause emerged in Wuhan, China.
1
Facilitated by an integrated global economy and modern air travel, the virus quickly spread. On March 11, 2020, COVID-19 (
International awareness of COVID-19 has been attributed to Dr. Wenliang Li, an ophthalmologist in Wuhan, China. 4 Ophthalmologists are at high risk of acquiring COVID-19 likely due to a combination of examination proximity and contact with mucous membranes. Ophthalmologists, including the original whistleblower Dr. Wenliang Li, were among the first physicians to die from the virus. 5 Ophthalmologists were among the initial investigators to study the virus and to advise on both treatment and protective measures for physicians, patients, and populations.
This paper summarizes research endeavors by ophthalmologists into COVID-19 and the relevant findings through a systematic review on ophthalmology-focused COVID-19 publications. To place these research endeavors into a larger context, we compared ophthalmology-focused publications to all publications on COVID-19.
Methods
Eligibility criteria, search, data source, and study selection
All ophthalmology articles on COVID-19 in PubMed were considered eligible and were included in the analyses. This is because our study aims included all ophthalmology research and clinical endeavors against COVID-19. Among identified ophthalmology-focused COVID-19 articles we further manually classified them into eight categories: original data, sharing experience, meta-analysis, review (without meta-analysis), recommendation, guideline, discussion/comment, and editorials. Articles containing original data were further examined in details.
The database LitCovid was searched. LitCovid is a curated literature hub for tracking up-to-date scientific information about the 2019 novel coronavirus, SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2), commonly referred to as COVID-19. It is the most comprehensive resource on this subject, providing a central access to COVID-19 relevant articles in PubMed and updating articles daily. 6 LitCovid has a more sophisticated search function than existing resources. It identifies roughly 35% more relevant articles than do conventional keyword-based searches for entries such as “COVID-19” or “nCOV.” 7
LitCovid uses a two-step search approach. First, a set of articles are retrieved from PubMed with the query “coronavirus”[All Fields] OR “ncov”[All Fields] OR “cov”[All Fields] OR “2019-nCoV”[All Fields] OR “COVID-19”[All Fields] OR “SARS-CoV-2”[All Fields]. Next, search results are human reviewed and relevant articles identified and curated with assistance from an automated machine-learning and text-classification algorithm. 6 Irrelevant articles are then discarded. Articles are manually assigned by LitCovid group to eight broad categories when applicable: general information, disease mechanism, transmission dynamics, diagnosis, treatment, prevention, case report, and epidemic forecasting. 6 LitCovid supports OR, AND, NOT, and phrase searches. 6 However, the specification “[All fields]” does not work in the LitCovid search. Pre-prints are not included in LitCovid.
We performed a search for ophthalmology-focused articles in LitCovid on June 12, 2020 using the query “eye OR ophthalmology OR ophthalmologist OR ophthalmic OR ocular OR conjunctivitis OR conjunctiva OR slit-lamp OR ‘Slit lamp’.” No language or date restrictions were applied. The journal of the publication was extracted with Python 3.8.3 using Integrated Development and Learning Environment (IDLE). 8 The country of origin of the publication was assigned based on country of the first author as in prior publications.9–12 Information on the country of the first author was extracted with Python 3.8.3 using IDLE first. 8 The extracted country information was then manually confirmed or corrected. Articles with no author affiliation/country listed (1789 out of 21,364 (8%) for all articles and 0% for ophthalmology-focused articles) were excluded from the statistics by country but were included in the analyses by journal.
Assessment of the quality of the evidence
The quality of the evidence was assessed for articles investigating ocular involvement in COVID-19 patients, a major concern of this review. Three types of original studies included: case-reports/case series, cross-sectional studies/surveys, and meta-analyses. For case reports and case series, the tool used to evaluate the methodological quality of case reports and case series published by Murad et al. 13 was used. For cross-sectional studies, the checklist recommended by the Agency for Healthcare Research and Quality was applied. 14 For meta-analyses, the measurement tool published by Shea et al was used. 15
Data analyses
This review involved categorical data only. Frequencies and percentages were used in the analyses. Percentages were calculated as the number of occurrences in a subcategory among the sum of all subcategories. The number of publications by country may be influenced by population size and COVID-19 infection rate in a country. We thus calculated the country-specific publication productivity adjusted for population size and COVID-19 infection rates. Data on country population were obtained from the Worldometer. 16 Data on the total number of confirmed COVID-19 cases by country on June 12, 2020 were obtained from Our World in Data. 3 Publication productivity adjusted for population size was calculated as the number of publications in a country divided by the corresponding country population. Productivity adjusted for infection rate was computed as the number of publications from a country divided by the country’s COVID-19 infection rate, which is the number of confirmed COVID-19 cases on June 12, 2020 divided by the country’s population.3,16
All data used in this study were publicly available thus Institutional Review Board (IRB)/Ethics Committee approval was not required. The study adhered to the tenets of the Declaration of Helsinki.
Results
Total number of publications and by journal and country
A total of 21,364 articles were registered in LitCovid on June 12, 2020. Of these, 308 were found in the initial search for ophthalmology-focused publications. The abstracts of these 308 articles were reviewed and 93 articles were excluded. Detailed reasons of the exclusion are shown in Figure 1. In all 215 ophthalmology-focused articles were included accounting for 1.01% of all COVID-19 related publications in LitCovid.
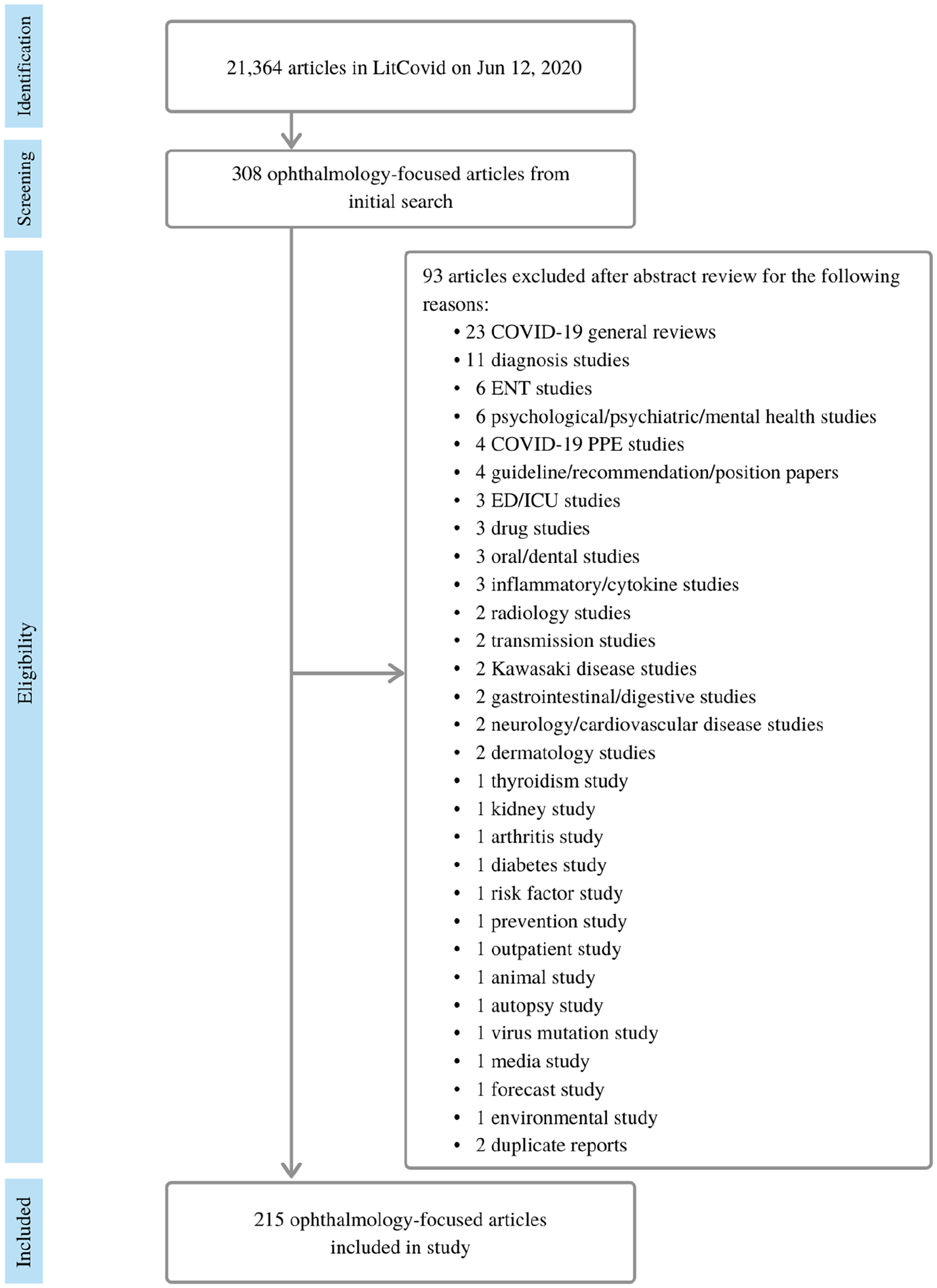
Diagram showing article selection process.
Table 1 details the publications breakdown by category. The largest number of all LitCovid publications was in the “Prevention” category, which represents prevention, control, response, and management strategies as defined by LitCovid group. 6 This was also the largest category for those articles with an ophthalmology-focus. In the category of “Transmission,” 3.3% were from ophthalmology-focused publications. Ophthalmology-focused publications were also found in the categories of disease mechanism, diagnosis, and treatment. There were no ophthalmology-focused publications in the category of “Epidemic Forecasting,” that is, modeling and estimations of COVID-19 spread.
Number of publications by article categories as assigned by LitCovid.
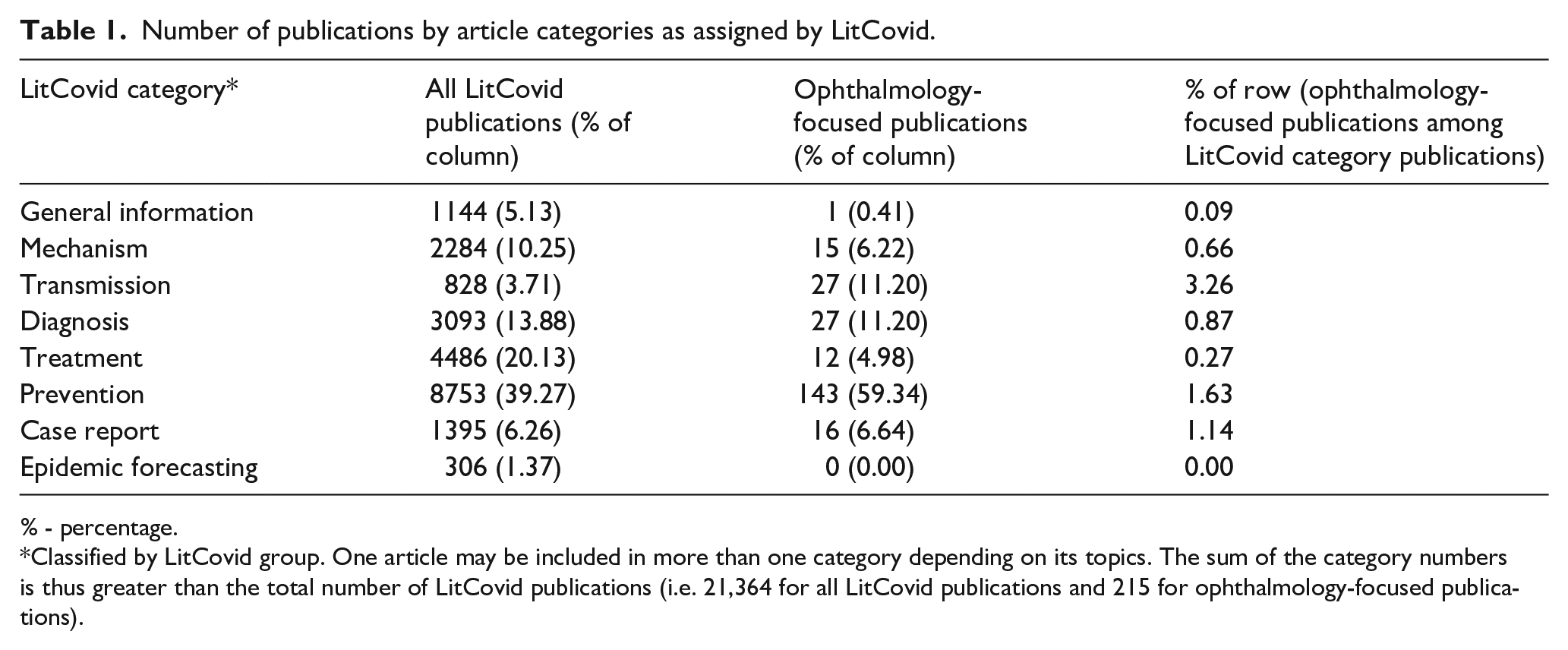
% - percentage.
Classified by LitCovid group. One article may be included in more than one category depending on its topics. The sum of the category numbers is thus greater than the total number of LitCovid publications (i.e. 21,364 for all LitCovid publications and 215 for ophthalmology-focused publications).
COVID-19 articles were published in 2794 journals. The top five journals by number of publications were “British Medical Journal,” “Journal of Medical Virology,” “Nature,” “Lancet,” and “New England Journal of Medicine” (Table 2). For those with an ophthalmology-focus, 68 journals published COVID-19 articles. The top five journals by number of ophthalmology-focused COVID-19 publications were “Eye (Lond),” “Indian Journal of Ophthalmology,” “Ophthalmology,” “Graefe’s Archive for Clinical and Experimental Ophthalmology,” and “Acta Ophthalmologica” (Table 2).
Top five by number of COVID-19 publications for journal and country of first author.
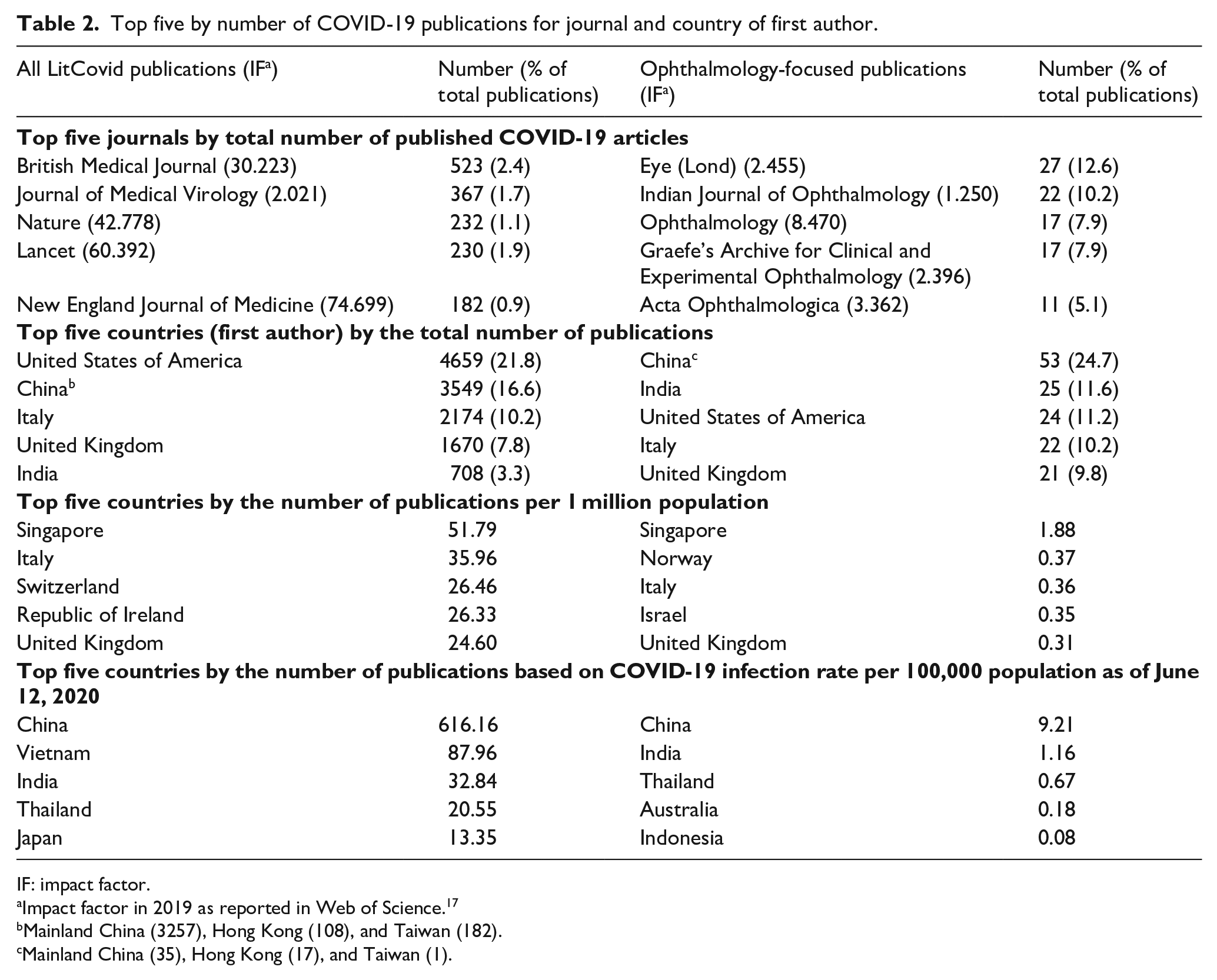
IF: impact factor.
Impact factor in 2019 as reported in Web of Science. 17
Mainland China (3257), Hong Kong (108), and Taiwan (182).
Mainland China (35), Hong Kong (17), and Taiwan (1).
Authors from 128 countries contributed to all COVID-19 publications and from 25 countries to ophthalmology-focused articles. The top five countries with the most COVID-19 publications by first author were United States of America (USA), China, Italy, United Kingdom (UK), and India for all articles (Table 2). For ophthalmology-focused publications, China was the most prolific, publishing twice as many than the second highest producing country by first author, India. This was followed closely by USA, Italy, and UK (Table 2). Together these five countries produced 145/215 (67%) of the ophthalmology-focused articles.
Adjusting for population size, Singapore had the greatest number of publications by first author for both COVID-19 publications and ophthalmology-focused publications (Table 2). Adjusting for COVID-19 infection rate per 100,000 population, China, India, and Thailand were among the top five prolific countries by first author (Table 2).
Overview of ophthalmology-focused publications
Table 3 shows that the largest type of ophthalmology-focused publications contained original data (27.9%), including case-reports/series, cross-sectional studies/surveys, cell/gene studies, post-mortem exams, and new methods of eye protection. The next most frequent type of publications included information on providing in-person care (urgent eye care, emergency surgery, oculoplastic, orbital, and lacrimal care),18–23 tele-ophthalmology,24,25 resident teaching,26,27 and basic science research in ophthalmology 28 during the COVID-19 pandemic. There were 25 editorials published in 15 journals, with 7 (28%) from the journal “Ophthalmology.”
Publication types of ophthalmology-focused publications.
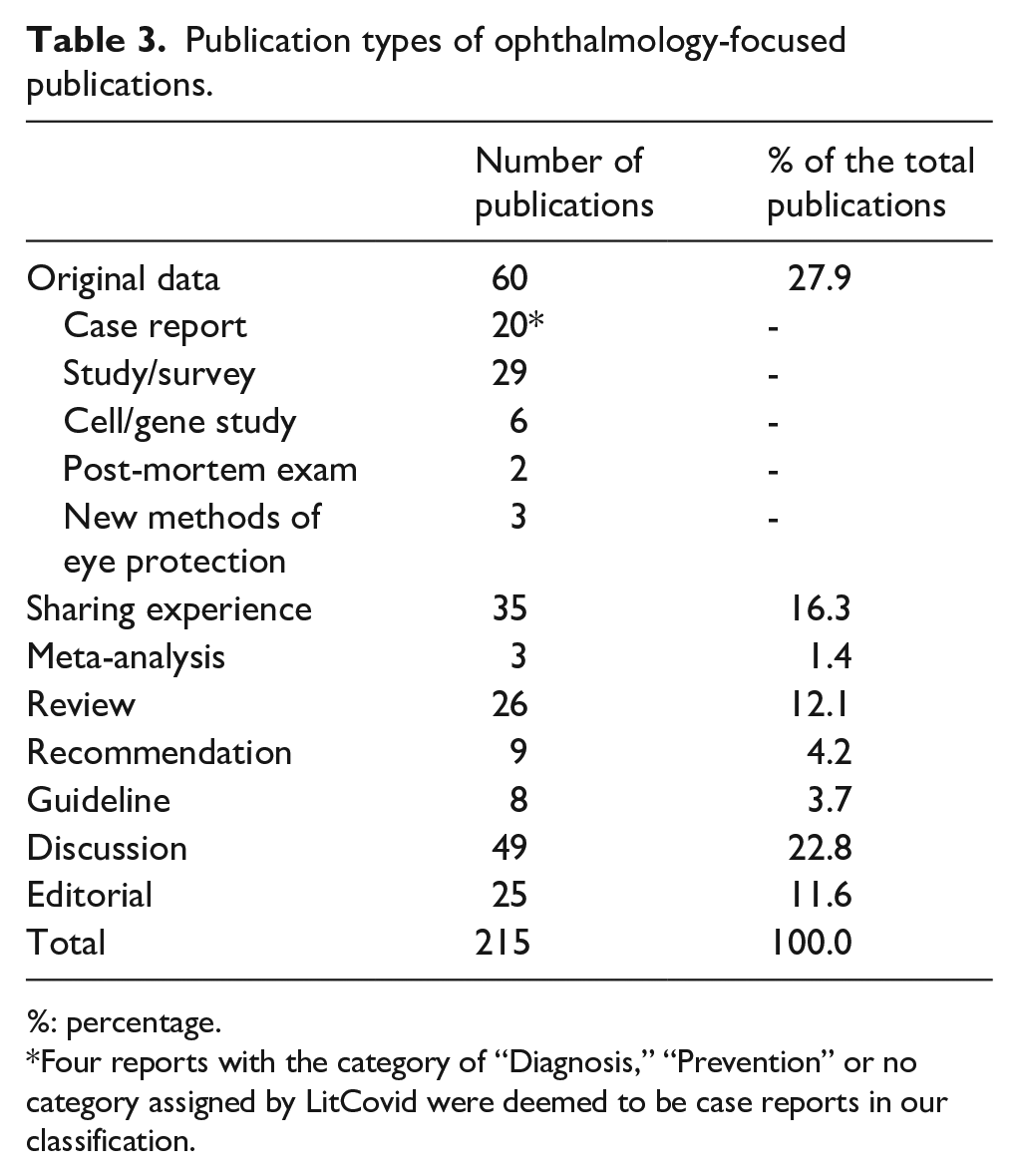
%: percentage.
Four reports with the category of “Diagnosis,” “Prevention” or no category assigned by LitCovid were deemed to be case reports in our classification.
Quality of evidence for studies on ocular manifestations and transmissions in patients with COVID-19
Of the 16 case reports/series assessed, 13 (81.3%) met all reporting requirements (Supplemental Material) and 3 received “unsure” in 1–2 questions from 8 questions assessed. Results of all 16 case reports/series were included in this review. For all cross-sectional studies, the assessment for evaluators being masked to the status of COVID-19 patients was either “No” or “Unclear.” At least 4/11 reporting requirements were met in 10/14 (71.4%) articles on ocular manifestation and transmission (Supplemental Material). Results from these 10 studies were analyzed. The cut-off 4/11 was chosen because the answer “Not applicable” was found in 1–3 items assessed, which mostly related to missing data handling and report. For meta-analyses, 2 studies fulfilled 6 and 7 reporting requirements each from a total 11 questions assessed (Supplemental Material). The third meta-analysis received a “Yes” in 3/11 questions. This study was not included in our detailed analysis.
Ocular manifestations in patients with COVID-19
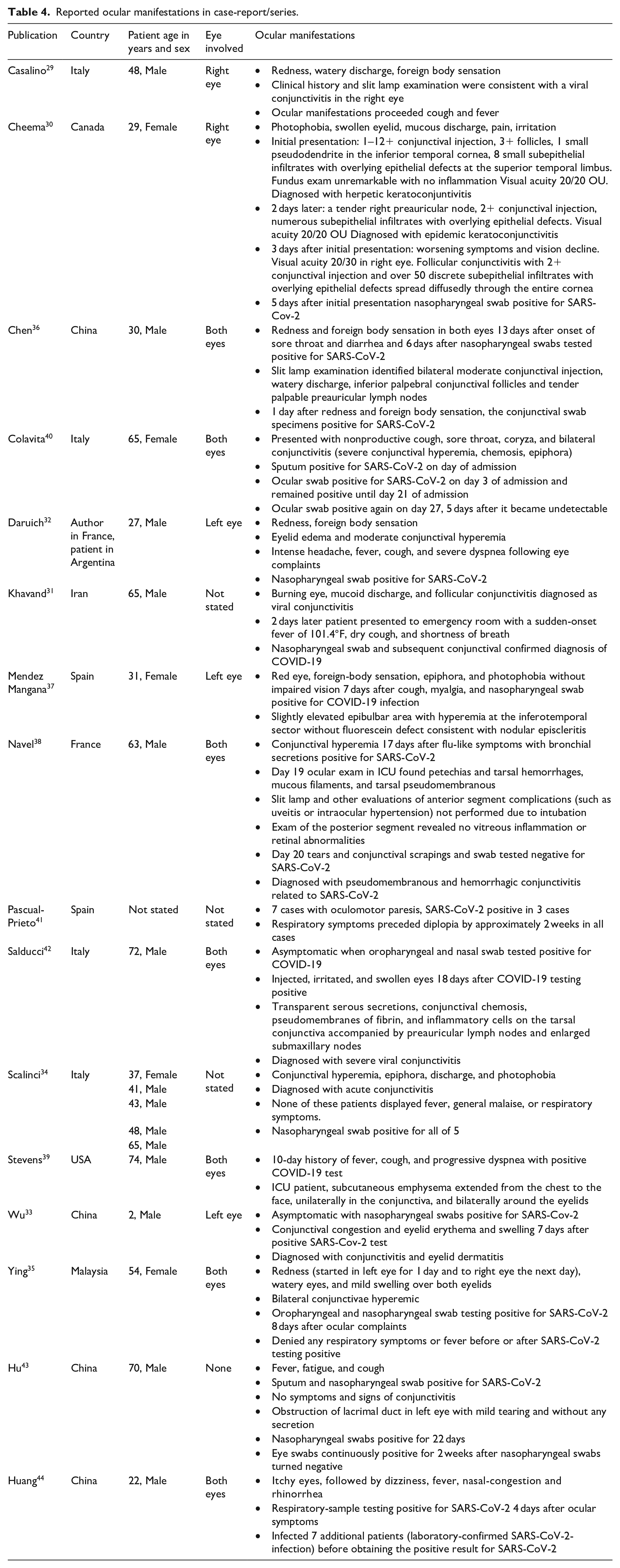
A total of 14 case reports and 2 case series (consisting of 5 and 7 patients) from China, Italy, France, Canada, USA, Spain, Iran, and Malaysia indicated that conjunctivitis or keratoconjunctivitis as evaluated by ophthalmologists can be the initial symptom of COVID-19 infection,29–32 and may be the only presenting feature of COVID-19.33–35 Conjunctivitis, episcleritis or orbital emphysema have also been reported to occur during the middle phase of COVID-19 illness, starting on day 7–19 after the onset of COVID-19.36–39 Detailed ocular manifestations are shown in Table 4.
Reported ocular manifestations in case-report/series.
Hospital-based cross-sectional studies reveal that between 0% and 31.6% of COVID-19 patients have conjunctivitis, with 75% reporting rates under 4.0%.45–52 The presence of patient reported ocular symptoms ranges between 5.0% and 26.8%.53,54
Two meta-analyses reported that conjunctivitis presented in 1.1% of COVID-19 patients 55 and that the pooled prevalence of conjunctivitis or conjunctival congestion among COVID-19 patients was 5.5% (95% confidence interval 1.6%-9.4%). 56
Ocular transmissions in patients with COVID-19
Positive conjunctival swabs for COVID-19 were reported in case reports of patients with clinically manifested conjunctivitis,30,31,36,40,43 in patients after the conjunctivitis had resolved for 1 week, 40 or 11 days after nasopharyngeal swabs turned negative. 43 Examining hospital-based patients revealed that positive conjunctival swabs can be found in patients with40,52 and without ocular manifestations.49,57 The reported positive rate ranged from 0% to 16.7% in patients with conjunctivitis or other ocular abnormalities45,51,52 and from 0% to 6.1% in those without conjunctivitis.48–50 A post-mortem study documented that viral RNA was detected in the retina of 3/14 deceased COVID-19 patients. 58
Cell/gene studies reported that the co-expression of the SARS-CoV-2 receptor (i.e. ACE2) was detected in human adult conjunctival, limbal, and corneal epithelium, suggesting the human conjunctival and corneal epithelium may provide an additional entry portal for SARS-CoV-2.59–61 However, no significant expression of the ACE2 in conjunctival samples on the mRNA and protein levels was reported. 62
Discussion
We report that 3 months after the COVID-19 pandemic was declared, ophthalmologists/researchers from 25 countries contributed 215 articles in 68 journals on the subject. These articles centered on understanding the ocular manifestations and transmission of COVID-19 infection and how to manage safe eye care, teaching, and research during the outbreak. Data from 16 case reports/series from eight countries indicate that conjunctivitis can be the initial or only symptom of COVID-19 infection. Conjunctivitis can occur 1–3 weeks after the onset of COVID-19. About 10 studies of hospital-based patients found the presence of conjunctivitis or other ocular abnormalities in patients affected with COVID-19 varied, ranging from 0% to 31.6%. All these 10 studies were derived from single hospital-based clinic records. The possibility of selected samples cannot be ruled out in producing the large variation. A meta-analysis showed a 5.5% (95% confidence interval 1.6%–9.4%) pooled prevalence rate of conjunctivitis or conjunctival congestion among COVID-19 patients. Positive conjunctival swabs have been reported in patients with and without conjunctivitis, including positive swabs 7 days after resolution of the conjunctivitis. Of concern to ophthalmologists is the report that conjunctival swabs can test positive for up to 11 days after nasopharyngeal swabs have turned negative. Viral RNA has been reported in the retina of deceased COVID-19 patients. These results demonstrate that conjunctivitis or other ocular abnormalities may be a presenting symptom of COVID-19 infection and the eye can be a potential source of COVID-19 transmission, even after nasopharyngeal swabs have turned negative. These findings have implications to healthcare providers, policy makers and the public regarding COVID-19 management and prevention.
At the beginning of the COVID-19 outbreak, the disease was thought to be transmitted through respiratory droplets with direct contact. The main impact of this disease was thought to be on the respiratory system. The very first person who alerted that there could be ocular involvement in COVID-19 was a member of the expert task force who visited COVID-19 patients in Wuhan, China. Despite being fully gowned with protective equipment including N95 mask, he was infected by the virus with the first symptom being unilateral conjunctivitis, followed by development of fever.63,64 Since then, “conjunctivitis” has been linked to COVID-19. To date, observations from case reports and cross-sectional studies originating from multiple countries lend support to this suspicion. However, lack of a control group from non COVID-19 individuals makes us difficult to know if conjunctivitis presented more frequently in COVID-19 patients.
Although the viral detection rate in conjunctival and tear samples seems to be low (0% to 16.7% in patients with conjunctivitis or other ocular abnormalities), the risk of ocular transmission remains a possibility, especially when considering the potential that negative conjunctival swab test results may arise from missed window of best sampling time and imperfect test sensitivity. Overall, results of this review offer two implications for clinical management of COVID-19. Firstly, conjunctivitis can be the initial or the only symptom of COVID-19 infection. This suggests that ophthalmologists and other healthcare providers such as emergency room physicians and family physicians should be on alert and practise appropriate self-protection (including eye protection) during the examination and treatment of new patients with ocular complaints. Secondly, when dealing with patients with diagnosed COVID-19 but without ocular complaints or those patients with nasopharyngeal swabs having turned negative, healthcare providers including ophthalmologists should be mindful of the possibility of viral transmission from the eye as positive conjunctival swabs have been reported in COVID-19 patients without conjunctivitis,49,57 and even in patients 11 days after nasopharyngeal swabs turned negative. 43 Recently, a report from Italy identified for the first time that SARS-CoV-2 RNA was identified in a pediatric patient with very mild ocular complaints. 65 This Italian report not only reenforces the findings of this review but emphasizes the above clinical implications offered should be considered when dealing with adult and pediatric patients.
In COVID-19 patients, the conjunctivitis rate and the presence of other ocular abnormalities (0%-31.6%) seems to be greater than the detection rate of SARS-CoV-2 observed from conjunctival samples by means of laboratory analysis (0%-16.7%). One possible explanation is that conjunctivitis and other ocular abnormalities may be caused by SARS-CoV-2 as well as by viruses, bacteria, and factors other than SARS-CoV-2. For example, reports have shown that COVID-19 patients in intensive care units (ICU) treated with continuous positive airway pressure (CPAP) are more likely to have ocular abnormalities than those not treated with CPAP (52.5% versus 30.8%, p<0.01), due to air leaks from the CPAP mask. 66 Such CPAP treatment may result in dry eyes causing ocular discomfort.38,66 Therefore, if conjunctival swabs are SARS-CoV-2 negative, ophthalmologists should look for other potential factors that can cause ocular signs and symptoms in COVID-19 patients, particularly in ICU patients.
Most of the current studies on ocular involvement in COVID-19 are based on case reports/series and hospital-based cross-sectional studies, which are considered level 4 evidence by the Oxford Centre for Evidence-based Medicine. 67 This is not ideal, however, given that we are dealing with a novel disease with many unknown clinical features, these early reports have contributed to advancing our knowledge on COVID-19’s clinical presentation and transmission and have provided important information to clinicians and decision-makers regarding the need for appropriate eye protection. Other examples of level 4 evidence contributing to improved disease understanding are found in the AIDS and sickle cell disease literature.68–70
To date COVID-19 has been reported in over 200 countries. 3 Ophthalmologists from 25 countries have contributed to the global understanding of the pandemic. The collective efforts of ophthalmologists demonstrate that ocular manifestations in COVID-19 patients occur in different ethnic populations, such as China, Italy, France, Canada, USA, Spain, Iran, and Malaysia.
Journal editors may play an important role encouraging and discouraging COVID-19 publications in their journals. 71 We do not know if the top five COVID-19 publication journals mainly reflect the journal editors’ choice. However, 7/25 (28%) editorials in ophthalmology-focused articles were from “Ophthalmology,” which ranks number 3 by journal in ophthalmology-focused publications.
This study has limitations. First, article citations were not evaluated due to the short time period since COVID-19 identification and the lag between publications and citations. Second, the country of origin was assigned based on the first author affiliation only. Although this methodology has been widely used in previous publications,9–12 this may not accurately capture the country of all coauthors. Third, only articles registered in LitCovid were included.
Study strengths include that all peer-reviewed publications in knowledge creation (e.g. case reports, post-mortem exams, and patient surveys) and knowledge dissemination (e.g. reviews and guidelines) were reviewed. The quality of the evidence on ocular issues in COVID-19 was assessed using published evaluation tools before summary.
Conclusion
This systematic review of ophthalmology-focused publications on COVID-19 indicates that ophthalmologists/researchers from 25 countries have published 215 articles in 68 journals within 3 months of the WHO declaration of the pandemic. These publications support the initial suspicion of ocular manifestation and possible transmission in COVID-19 infections and serve to inform best clinical practices. However, it is unknown if the frequency of conjunctivitis in COVID-19 patients differs from that in non COVID-19 individuals. Future population-based studies are needed to overcome the drawback of selected patient samples from case reports and single hospital-based records.
Supplemental Material
sj-pdf-1-ejo-10.1177_1120672121992949 – Supplemental material for Ophthalmology-focused publications and findings on COVID-19: A systematic review
Supplemental material, sj-pdf-1-ejo-10.1177_1120672121992949 for Ophthalmology-focused publications and findings on COVID-19: A systematic review by Ya-Ping Jin, Graham E Trope, Sherif El-Defrawy, Elin Y Liu and Yvonne M Buys in European Journal of Ophthalmology
Supplemental Material
sj-pdf-2-ejo-10.1177_1120672121992949 – Supplemental material for Ophthalmology-focused publications and findings on COVID-19: A systematic review
Supplemental material, sj-pdf-2-ejo-10.1177_1120672121992949 for Ophthalmology-focused publications and findings on COVID-19: A systematic review by Ya-Ping Jin, Graham E Trope, Sherif El-Defrawy, Elin Y Liu and Yvonne M Buys in European Journal of Ophthalmology
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
