Abstract
This article reviews the importance of a team approach in feline chronic pain management for optimal outcomes. It discusses the role of different stakeholders and the importance of collaboration, communication and strategies for improved experiences for cats and caregivers on their journey. Chronic pain is maladaptive and negatively impacts on all domains of animal welfare. It can occur by itself, but most commonly is secondary to other chronic conditions. Ensuring that cats suffering from chronic pain are managed effectively requires a collaborative approach between all stakeholders, including client care staff, veterinarians, veterinary nurses or technicians, veterinary support staff and clinic management, as well as the cat and the caregiver. The journey starts with clinical signs displayed by the cat and perceived by the caregiver, and ends, for most cases, with end-of-life considerations. Diagnosis of chronic pain and design of a treatment plan result from a partnership between the caregiver and veterinary team. Management of chronic pain is focused on maintaining quality of life while empowering caregivers to be part of the healthcare team, avoiding adverse effects from medication and balancing comorbidities. The journey for cats and their caregivers is influenced by numerous factors, including the clinical condition of the cat and the caregiver’s response to different burdens, but mostly by the care they receive from the clinic and veterinary teams involved in the process. Empathetic communication is paramount and helps to optimise the cat’s care while supporting caregivers.
Plain language summary
This article reviews the importance of a team approach in feline chronic pain management for optimal outcomes. It discusses the role of different stakeholders and the importance of collaboration, communication and strategies for improved experiences for cats and caregivers on their journey. Chronic pain is maladaptive and negatively impacts on all domains of animal welfare. It can occur by itself, but most commonly is secondary to other chronic conditions. Ensuring that cats suffering from chronic pain are managed effectively requires a collaborative approach between all stakeholders, including client care staff, veterinarians, veterinary nurses or technicians, veterinary support staff and clinic management, as well as the cat and the caregiver. The journey starts with clinical signs displayed by the cat that are observed by the caregivers. The diagnosis of chronic pain and the design of a treatment plan result from a partnership between the caregiver and the veterinary team. Management of chronic pain is focused on maintaining quality of life while empowering caregivers to be part of the healthcare team, avoiding adverse effects from medication and balancing comorbidities. The journey for cats and their caregivers is influenced by numerous factors, including the clinical condition of the cat and the caregiver’s response to different burdens, but mostly by the care they receive from the clinic and veterinary teams involved in the process. Empathetic communication is paramount and helps to optimise the cat’s care while supporting caregivers from the initial assessment until, for most cases, end-of-life decisions.
Keywords
Introduction
Veterinary medicine has evolved substantially in recent decades. Patients are living longer, and a large portion of clinical practice today involves the management of chronic conditions, including chronic pain.1 –5 Chronic pain in cats is likely to be underdiagnosed yet negatively affects quality of life. Identification and management of chronic pain require the participation of specific stakeholders, with the cat being the primary focus and each stakeholder having a different role to play (Figure 1, Table 1).
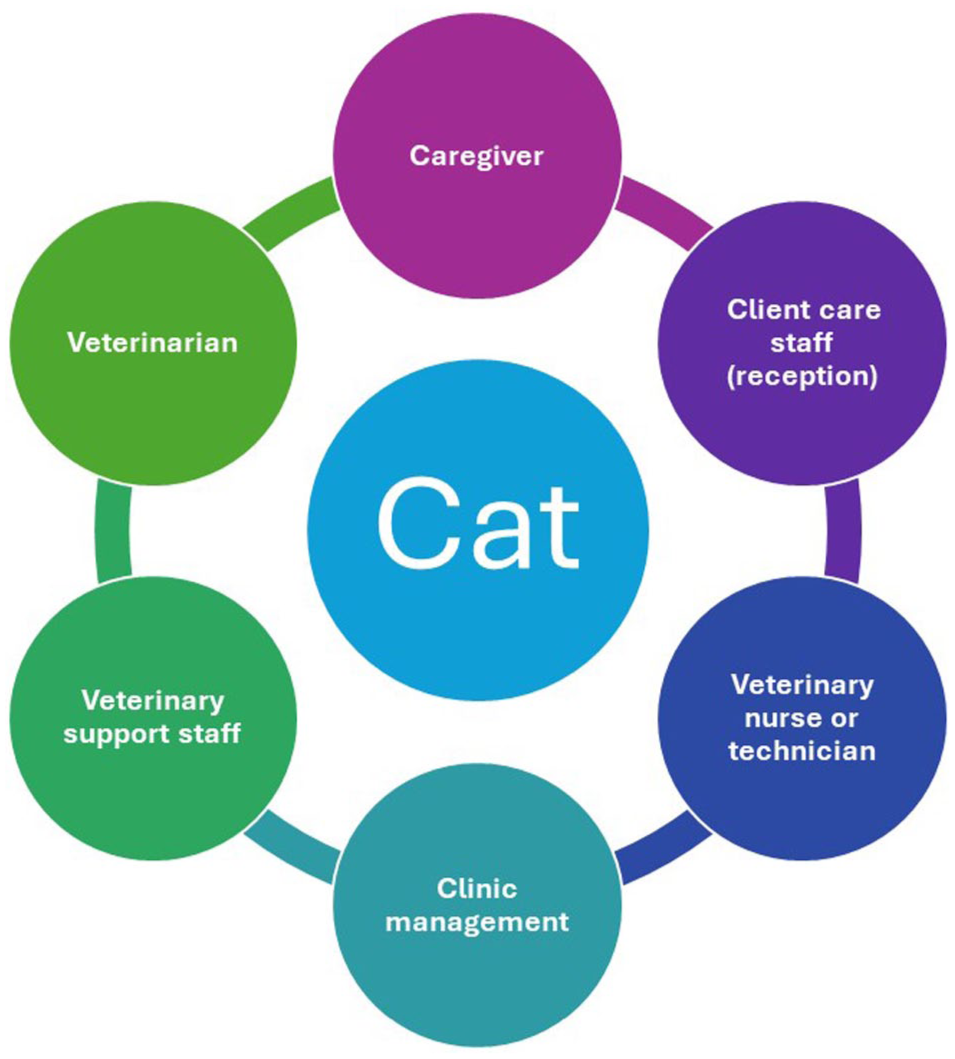
Stakeholders involved in the care of the cat with chronic pain. The primary focus is the patient, with a team approach being the most effective way to achieve the best outcome
Stakeholders in feline chronic pain management

This article reviews the importance of a team approach in feline chronic pain management for improved experiences and optimal outcomes during the journey that cats and their caregivers go through, from the development of the first clinical signs to diagnosis, treatment and monitoring, until end-of-life considerations. It includes a brief overview of the current literature related to the management of chronic pain in cats, how it impacts on a cat’s behaviour and welfare, and strategies for improved experiences for cats and their caregivers on their journey. It also discusses the role of the different stakeholders and the importance of collaboration and effective communication among them, with the primary goals of maintaining quality of life for the cat and reducing caregiver burden.
Chronic pain in cats: where are we today?
Chronic pain is maladaptive. It persists beyond the duration of an acute disease and may be amplified by alterations in pain signals, perception and emotional response.14–16 There are many causes of chronic pain in cats (Table 2) and, although degenerative joint disease (DJD) is the most studied,22–24 analgesia should be included in the management of any chronic condition that causes pain. For example, dental disease is common in cats of all ages (Figure 2) and is a cause of significant pain.25–29 Along with management such as extractions, analgesia should be prescribed. Cancer is commonly diagnosed in older feline patients and is likely to be associated with pain, for example, from tissue damage (compression, invasion, capsule distension) (Figure 3) 30 or via paraneoplastic inflammatory mediators. 31 Affected patients often have comorbidities that may contribute to discomfort (eg, DJD). The cornea and other ocular structures are well innervated, 32 hence corneal ulceration, sequestra, uveitis, glaucoma and other eye conditions should be considered painful (Figure 4). Dermatological disease such as otitis or pruritic conditions may be a cause of chronic pain (Figure 5). 33 Neuropathic pain, and postoperative (Figure 6) or post-traumatic pain, are characterised by a heightened response to sensory stimulation and central sensitisation.16,17,34
Examples of conditions causing chronic pain in cats


Dental disease is prevalent in cats and a cause of chronic pain. Courtesy of Samantha Taylor

Oral squamous cell carcinoma in a 12-year-old cat. This type of cancer is painful and has a cyclooxygenase (COX) overexpression pattern. Affected cats should be provided with analgesia including COX inhibitors. Courtesy of Samantha Taylor

Uveitis in a cat diagnosed with feline infectious peritonitis. As well as managing the disease process, analgesia should be provided. Courtesy of Lumbry Park Veterinary Specialists
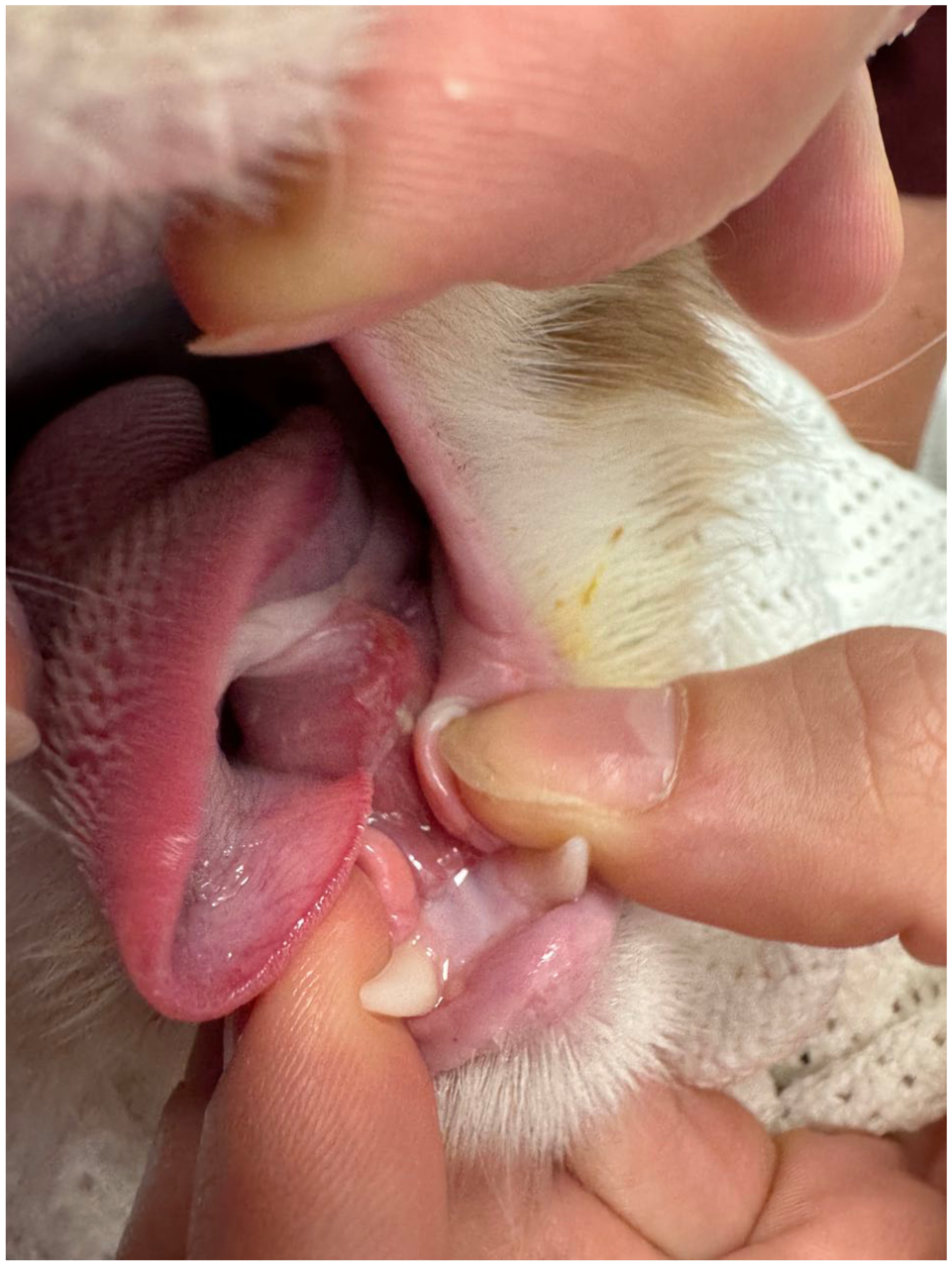
Eosinophilic granuloma under the tongue of a 2-year-old cat, resulting in complete anorexia. Courtesy of Samantha Taylor
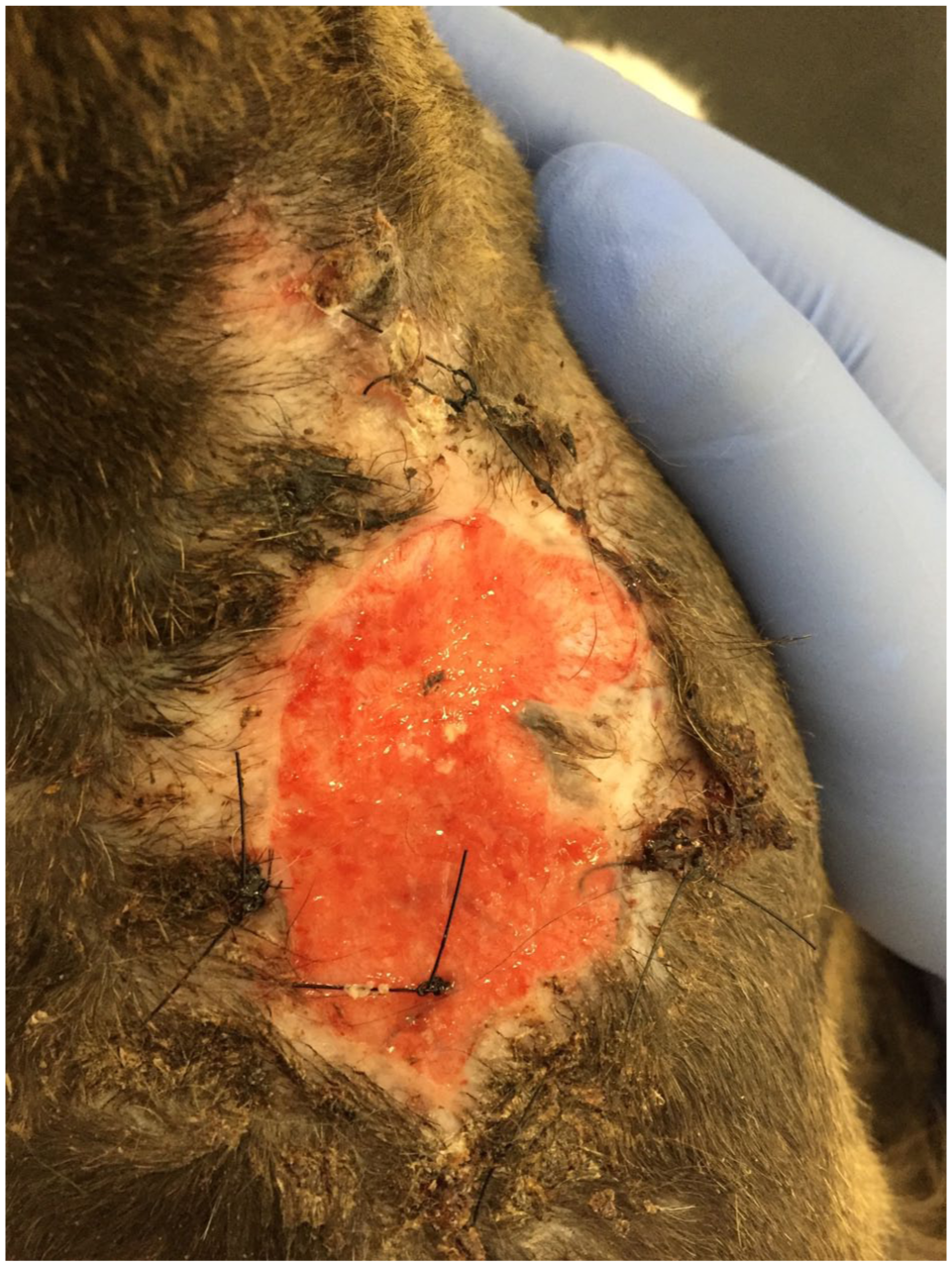
Persistent self-trauma of a surgical wound after removal of a soft tissue sarcoma in an older cat. Courtesy of Samantha Taylor
Medical pain is an underrecognised, and hence undertreated, cause of chronic pain. 14 Medical pain refers to non-surgical or traumatic pain, encompassing pain associated with distension, inflammation or ischaemia of the thoracic or abdominal visceral organs or cavities. 1 It may be hard to localise, change with time or in relation to feeding, and be accompanied by nausea, inappetence and gastrointestinal dysmotility (eg, constipation, ileus). Management of medical pain may be complicated by contraindications to some analgesics, lack of definitive diagnosis, and interactions between medications used to treat the underlying disease and analgesics (eg, corticosteroids and non-steroidal anti-inflammatory drugs [NSAIDs]), as well as difficulty monitoring the efficacy of analgesics. The caregiver burden of administering multiple medications to, and care of, a sick cat should also be considered (see later). Examples of medical pain include prevalent conditions, such as pancreatic and hepatobiliary disease, gastrointestinal diseases, upper and lower urinary tract diseases, and peritonitis/pleuritis.
Although the prevalence of chronic pain in cats is unknown, we can infer prevalence from these associated conditions. Radiographic changes consistent with DJD/osteoarthritis (OA) are common in cats, especially as they age,35–39 with up to 92% of cats having degenerative changes detected on radiographs. In the UK, periodontal disease and tooth structure disorders have a prevalence of 13.9% and 1.7%, respectively. 2 Neoplasia (12.3%) and mass-lesion disorders (11.6%) are commonly attributed causes of mortality in cats aged over 5 years. 3 Behavioural disorders were the attributed cause of mortality in 1.5% of cats aged over 5 years, 3 and there is a growing awareness of the association between chronic pain and problem behaviour. 40 It is a valid assumption that a significant proportion of cats with the aforementioned conditions suffer from chronic pain.
Stakeholders in feline chronic pain management
Ensuring that cats suffering from chronic pain are managed effectively requires a collaborative approach between all stakeholders (Figure 1, Table 1).
The cat
The journey of the cat with chronic pain starts with the disease process leading to behavioural changes that are detected by the caregiver and diagnosed by the veterinary team. It is followed by the initial treatment plan and continued monitoring (Figure 7).

The journey of the cat with chronic pain
Pain impacts on a cat’s welfare
Animal welfare can be defined as ‘the physical and psychological, social and environmental well-being of animals’. 41 In simple terms, it might be thought of as the life experience of an animal from his/her own perspective. It is a state that can change over time, influenced by physical and emotional experiences, and which runs on a spectrum from very good to poor. Good animal welfare involves physical health and positive emotions, such as pleasure and contentment. Poor animal welfare comes not only from ill health, injury and disease, but also from negative emotions such as frustration or fear, which we call suffering. 42 Although there is no single widely accepted definition of animal welfare, modern frameworks, such as the Five Domains Model, have helped advance this science. The Five Domains Model is a device for facilitating systematic, structured, thorough and coherent assessments of animal welfare, and for qualitatively grading welfare compromise and enhancement. 43 If we think about it, pain negatively affects all five domains of animal welfare (Figure 8, Table 3). Pain is, by definition, an unpleasant experience and negatively affects nutrition, use of the environment, health and behaviour. Veterinary professionals are expected to understand the multidisciplinary science of animal welfare,44,45 and have an ethical and medical duty to prevent, diagnose and treat pain.46,47

(a) The Five Domains Model and (b) the negative influence of pain in all domains. The first four domains (ie, functional/physical domains) focus on factors that lead to negative or positive subjective experiences. Such experiences result in the fifth domain (ie, the animal’s mental state). Adapted from Mellor et al. 43 Courtesy of Beatriz Monteiro
Considerations for the assessment of animal welfare based on the Five Domains Model, and examples of the consequences of pain for each domain

Pain leads to behaviour changes
Pain affects physical, emotional, social and cognitive domains; 48 the behavioural changes seen in cats with chronic pain reflect these multidimensional impacts. Such behaviour changes might be perceived as a problem by the caregiver. When they do, they are called problem behaviours, with the recognition that these are problems from the caregiver’s perspective. Problem behaviours that can result from pain include decreased social interaction and tolerance of handling, excessive grooming over a painful area on the body, increased hiding, defensively aggressive behaviours, and house soiling when it is difficult to access the litter tray/box or the litter tray/box becomes associated with pain. 40 Many of these changes are driven by fear of pain and its negative emotional impacts. As a feature of their natural history, a healthy environment for cats relies on a sense of safety and the ability to access safe spaces, 49 which includes vertical height. When cats have chronic pain and their ability to access these safe spaces decreases, their sense of safety and emotional wellbeing is negatively affected.
Veterinary visits can cause stress and result in negative experiences
An important hindrance to the diagnosis of chronic pain is the effect of the stress of the veterinary experience, including transport, examination and returning home after the visit. Both pain and fear are strong stimuli that animals will work to avoid. Therefore, when veterinary visits become associated with pain and fear, cats will show increased stress and avoidance behaviours, making it harder for veterinarians to obtain meaningful responses from the cat during physical examination.50 –53 It also makes it more difficult for caregivers to bring their cats to the veterinarian or deters them from attending, creating a vicious cycle. Some stress is inherent for cats when leaving their territory, 54 but veterinary teams can implement feline-friendly procedures and environments to mitigate stress and improve the veterinary experience.49,55 Even small changes can achieve a marked improvement in the cat’s and caregiver’s experience (Figure 9).

Examples of cat-friendly interactions. Cats can be kept in their carriers for (a) physical examination and (b) blood pressure monitoring. (c) If they must be removed from the carrier for blood pressure monitoring, gentle handling and the use of headphones to avoid noise disturbance to the cat can contribute to reducing fear and stress. Courtesy of Samantha Taylor
The caregiver
The journey of the caregiver has many opportunities for connection and engagement with the veterinary team to improve the early detection and management of feline chronic pain (Figure 10). Historically, veterinary medicine has taken a paternalistic approach, which has shifted, in line with human medicine, to a more autonomous approach in which a partnership between patient and clinician is developed. 56 However, unlike human medicine, veterinarians operate in a tripartite system including the caregiver (often the legal owner), the patient and the clinician. There remains discussion on who is being given more autonomy: the caregiver or the patient? 57 Language matters; there is a move to start using terms such as contextualised care,58,59 which considers the individual needs of the caregiver and the cat (Table 4). Interdisciplinary collaboration may be needed to ensure a holistic approach. 60 Caregivers need to be involved in the discussion of how best to manage the chronic pain in their cat; costs, frequency of follow-up appointments, formulation and frequency of medication, adjunctive therapies, modifications to the environment and husbandry, and caregiver and cat factors should be discussed before a final care plan is agreed upon. The caregiver needs to be aware that no care plan is final and if they (or the cat) are not able to meet aspects of it or if the cat is not responding, this is normal and further adjustments will be considered.

The journey of the caregiver of cats with chronic pain
Contrasting scenarios of two cats of the same sex, age and body weight, and with similar degrees of degenerative joint disease in similar joints
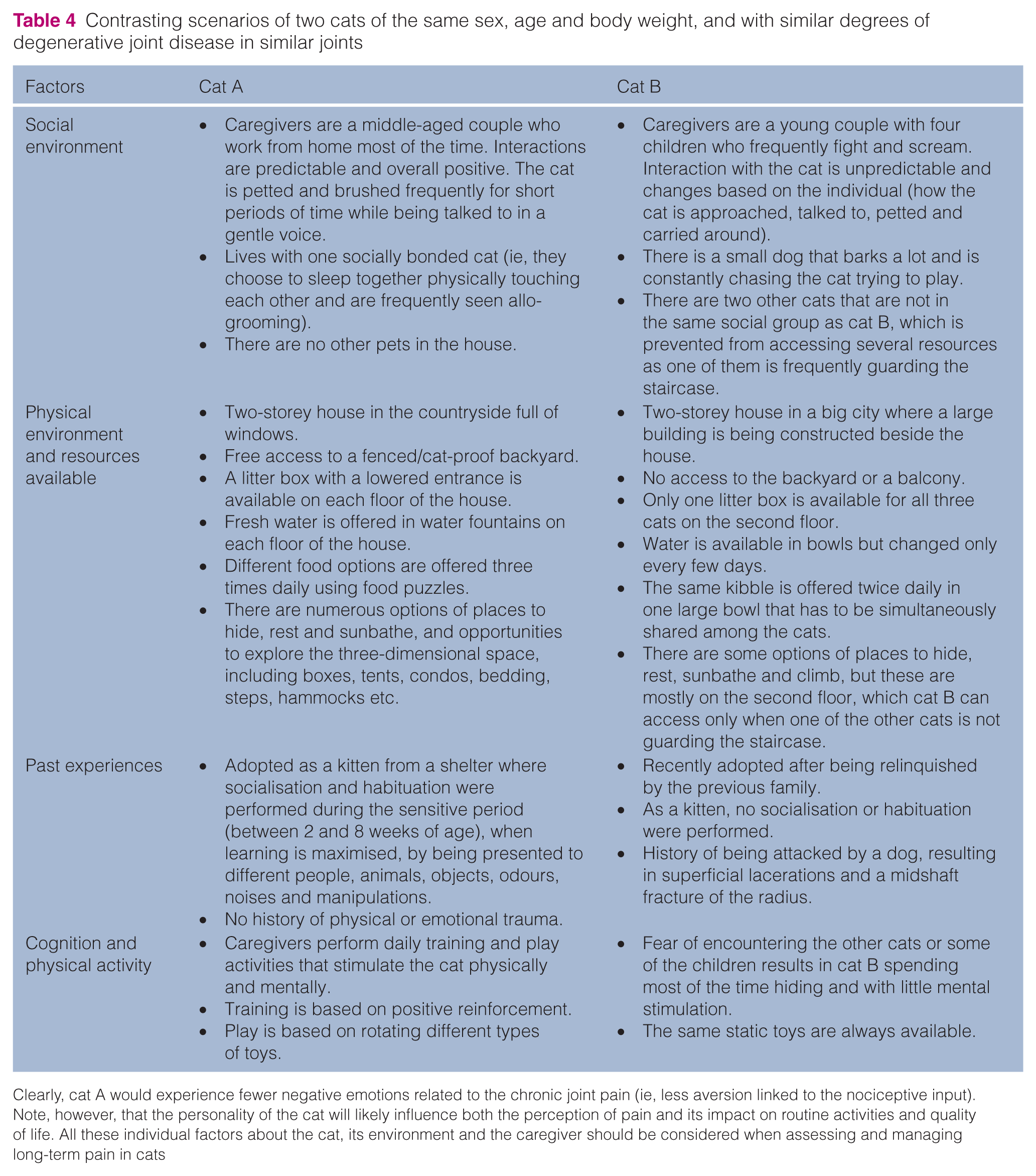
Clearly, cat A would experience fewer negative emotions related to the chronic joint pain (ie, less aversion linked to the nociceptive input). Note, however, that the personality of the cat will likely influence both the perception of pain and its impact on routine activities and quality of life. All these individual factors about the cat, its environment and the caregiver should be considered when assessing and managing long-term pain in cats
One of the main challenges in identifying chronic pain in cats is the low rate of medicalisation in cats, as a significant proportion of cats are not seen by veterinary professionals for routine appointments and preventive healthcare. A study from 2012 showed that 52% of US caregivers had not taken their cat to their veterinarian in the previous 12 months and only 37% said they had attended a routine appointment in the same period. 61 Without cats and their caregivers regularly attending the clinic, the opportunity to diagnose conditions and raise awareness about the behavioural changes associated with common causes of chronic pain, specifically DJD/OA and dental disease, is lost.
Research has shown that focusing on the caregiver’s relationship with their pet, tying preventive care into the cat’s overall health and happiness, and emphasis on the personal experience with the veterinarian helps caregivers to appreciate the value of preventive health care. 62 We can extrapolate that similar strategies are likely true when discussing the holistic requirements of managing chronic pain in cats. Pain management in cats is most likely to be successful if their caregivers are both willing and able to administer the medication, make the required environmental modifications and return for regular follow-up appointments.
As a feature of their natural behaviour, husbandry and slow disease progression, chronically painful conditions present differently in cats compared with dogs.14,18,23,48 Recognition and diagnosis of chronic pain in cats lies in part with the need for their caregivers to observe and report changes in their cat’s behaviour 63 and to detect changes in those same behaviours when cats are treated with analgesia.63,64 Experience also demonstrates that when caregivers are aware their cats are in pain, they are motivated to treat them. What commonly occurs, in the view of the authors, is that the gradual decline that is characteristic of many chronic pain conditions takes time to be recognised and, if treatment lapses, the caregiver’s attitude can revert to an acceptance of a cat’s behaviour as ‘normal ageing’ even as the cat’s pain worsens. Short video clips of cats in their homes taken by caregivers can be instrumental in reflecting on behavioural change and communicating with veterinarians (Figure 11). Behaviours that should be captured will change for the different pain conditions but represent an important tool clinicians can use for engagement, education and monitoring.
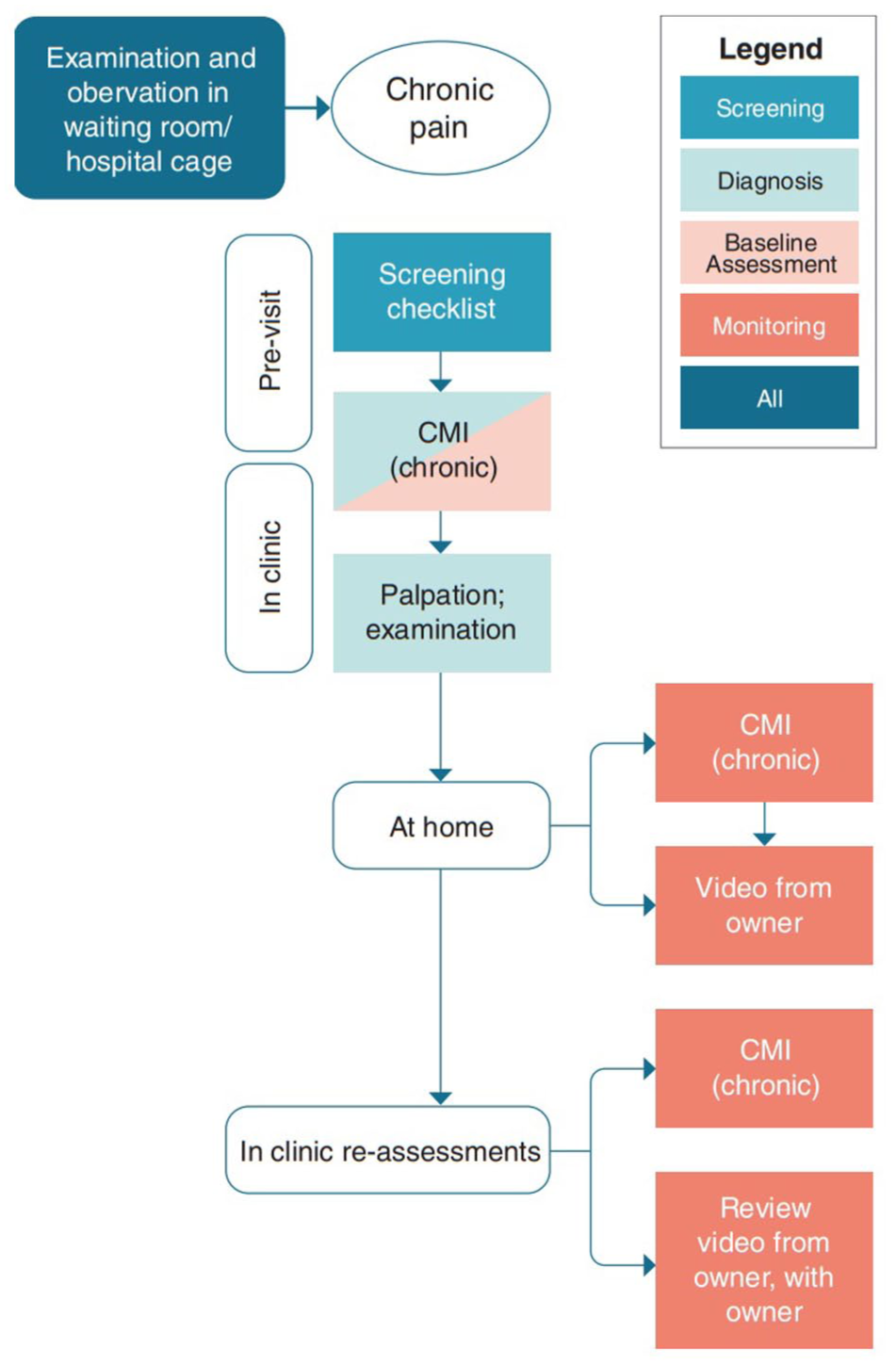
Flow diagram to guide the assessment of chronic pain in cats. The core elements are physical examination/palpation and the use of pain scoring tools (Table 6). Note how the caregivers and the veterinary team have important roles to play in the initial assessment and reassessments for monitoring response to treatment. CMI = clinical metrology instrument. Adapted with permission from Gruen et al. 18 This figure has been modified from the original and the recommendations for assessment of acute pain have been removed
Several tools have been developed to assist with caregiver engagement and education, although little research has been performed on their impact. There is evidence, however, that the way in which caregivers obtain healthcare information has changed,65,66 and that engagement using animations, social media clips and AI-driven motion analysis apps may increase awareness of painful conditions in cats. Tools such as the Musculoskeletal Pain Screening Checklist (MiPSC), 7 Montreal Instrument for Cat Arthritis Testing (MI-CAT) 67 or a custom message from the clinic can be sent to caregivers before their visits or timed to coincide with dates such as International Cat Day (8 August) or Chronic Pain Awareness Month (September). Instructions and examples of how to capture short videos of their cat’s behaviour in the home may be especially helpful for both caregiver and veterinarian.
Caregiver burden
As part of the caregiver journey, it is also important to acknowledge the effects on the human–animal bond and caregiver burden that accompany chronic pain conditions. Often, the changes in a cat’s behaviour (and ‘problem behaviours’ as described above) affect the bond between cats and their caregivers, and can affect the entire household. For example, when a cat with chronic pain no longer tolerates play initiation by a younger cat (or a toddler), he or she may display defensively aggressive behaviour to increase distance, especially when the cat’s ability to escape by running or jumping is impaired. This can have a lasting impact on the social dynamics in the home. 68 There is also an emotional burden that comes with worry about the pain their cat is suffering, their cat’s quality of life and the potential for nearing end-of-life decisions. 66 Administration of medications adds to the care burden (see later). Finally, it is impossible to ignore the financial burden that comes with the diagnosis, treatment and follow-up of chronically painful conditions.69,70 Taking these factors together, it is critical that the veterinary team recognises and supports cat caregivers throughout this journey.
Challenges with medicating cats
It is well known that administering medications to cats, particularly orally, is challenging, and can result in non-compliance, inadequate treatment of illness or management of pain, and human injury.70,71 In a situation of chronic illness and pain, there may be additional challenges; for example, poor appetite precluding the addition of medications to treats, or pain increasing a cat’s resistance to handling or restraint for medicating. For this vulnerable group of patients, the experience of forced medicating may result in pain, stress, protective emotions and avoidance of interactions with caregivers,70,72 damaging the caregiver–cat bond and even intensifying the experience of pain. 73
Open dialogue with caregivers, acknowledgement of the difficulties and adapting the pain-management plan to suit the individual cat and caregiver can optimise compliance. Table 5 provides tips for increasing medication compliance in cats with chronic pain.
Tips for increasing medication compliance in cats with chronic pain

Environmental modifications at home
The caregiver plays an important role in optimising the cat’s environment at home while providing for its behavioural and emotional needs, including a safe place, multiple and separate resources, opportunities for play and predatory behaviour, positive and predictable social interactions with humans and other animals, and respect for the importance of a cat’s sense of smell.19,55,74 At home, caregivers may need to adapt the environment by offering steps or ramps using non-slip surfaces to ensure cats have access to three-dimensional space and resources such as food and water (using raised bowls), litter boxes (with at least one side lowered to facilitate entry and exit), scratching substrates (including different options such as horizontal or vertical) and preferred resting areas (with comfortable and warm bedding) (Figure 12).

Examples of environmental modifications for cats with chronic pain from osteoarthritis. The cat in the hammock by the window is a 20-year-old male cat that can no longer jump to elevated surfaces. He is able to access this perching area and enjoy the morning sun by using the window frame as a step. The cat in the cat condo is a 15-year-old female cat with minor mobility impairment that can climb to the highest perching areas. These strategies provide cats with opportunities to exercise, access safe places and have rewarding experiences. Courtesy of Beatriz Monteiro
The veterinary team
Identifying and diagnosing chronic pain
The recognition and diagnosis of chronic pain by the veterinary team starts with either the diagnosis of a condition that is known to be painful (Table 2), the identification of persistent postoperative pain or from the presentation of a cat with clinical signs (including changes in behaviour) that raise the suspicion that chronic pain may be an underlying cause (Figure 11). The observed behavioural change associated with chronic pain is dependent on the location and type of chronic pain being experienced (Figures 13 and 14). Decreased activity levels, decreased ability to perform activities, changes in appetite, changes in toileting habits, unkempt coat and nails, alopecia, skin rippling, decreased socialisation, general loss of interest and sudden episodes of vocalisation or agitation are the common changes associated with chronic pain.14,18,20,63,75 Veterinary team members must be aware of these changes to enable further investigation to be performed in a timely manner if a cat presents with them.

A cat exhibiting poor coat and demeanour secondary to dental pain. Courtesy of Feline Healthy Ageing Clinic, University of Liverpool

A cat displaying an awkward position while sitting secondary to hip pain. Courtesy of Feline Healthy Ageing Clinic, University of Liverpool
The veterinarian will assess the sensory and emotional components of chronic pain with clinical examination (manipulation or palpation) and using clinical metrology instruments (scales to measure pain or quality of life). They may additionally observe pathology that is likely to cause pain, such as dental disease or other inflammation. 14 These are essentially subjective measures and will depend on the force used and the veterinarian’s interpretation of the response. Imaging can also be used in some conditions to help support the diagnosis, but findings may not correlate with the level of pain the cat experiences. The veterinary team should be aware that stress-induced analgesia can occur in the clinic environment. The stress associated with being transported to and visiting a veterinary clinic can affect how pain is perceived. Protective emotions such as fear typically amplify the pain experience. 76 However, in cases of extreme stress, pain or fear, stress-induced analgesia can occur, reducing the pain experience. This survival mechanism allows, for example, an animal with a broken bone to escape a life-threatening situation by temporarily reducing the pain. 77 Once the animal reaches safety, the pain returns. In practice, pain might be underestimated in patients experiencing high levels of stress, including stress caused by the visit to a veterinary clinic. 19
The whole veterinary team should be trained on how to use validated pain scoring tools for the assessment of pain and monitoring treatment efficacy. However, there is currently no validated scale for assessing feline chronic pain apart from pain linked to DJD (Table 6). Scales that evaluate quality of life assume it is impacted by chronic pain, but these measures are not synonymous with direct pain assessment. They should also recognise that the adaptive component of the cat’s behaviour as the result of chronic pain may not respond rapidly to analgesia; time may be required for the cat to relearn what behaviours it can perform without pain. Finally, the entire team should be trained in cat-friendly environment and interactions (Box 1, Figures 15–18).
Tools used for screening and assessing chronic pain and quality of life in cats*

Reproduced with permission from Monteiro et al 14
All instruments are meant to be completed by caregivers
Recommended for use in clinic because of a higher degree of scientific evidence
CMI = clinical metrology instrument; DJD = degenerative joint disease; HRQoL = health-related quality of life; OA = osteoarthritis
Cat-friendly environment and interactions


A cat and his caregiver positively interacting during a consultation. The cat is provided with an elevated surface with comfortable bedding to rest while the caregiver discusses with the veterinary team. Courtesy of Samantha Taylor

A cat-only ward provides a calm environment for both cats and staff. Covers are used to provide privacy for fearful cats. Courtesy of Samantha Taylor

(a) Despite a limited space, clinics can offer multiple resources and resting areas within cats’ cages. (b) In this example, a reusable box provides a hiding area for safe space as well the opportunity for perching. Courtesy of Samantha Taylor

Example of gentle positioning and head tilt for blood sampling. Courtesy of Feline Healthy Ageing Clinic, University of Liverpool
Managing chronic pain
Management of chronic pain in cats is understudied except for DJD. Multimodal approaches should be implemented using pharmacological and non-pharmacological therapies (Figures 19–22), and include consideration of other aspects of chronic pain (eg, nausea, stress, gastrointestinal dysmotility and mental wellbeing) in a comprehensive pain management plan that engages the caregiver. 14 Details of dosages and considerations for prescribing various analgesics are available elsewhere.14,18,19

Decision tree for prioritising pain management therapies. This figure outlines a tiered approach to chronic pain management in cats. Tiers are presented from highest recommendation (most evidence for effectiveness) to lowest, although all therapies presented have some evidence to support their use. Physical modalities include laser therapy, pulsed electromagnetic field therapy, acupuncture and transcutaneous electrical nerve stimulation. Surgical procedures for chronic pain include top-tier treatments, such as dental procedures, removal of painful lesions, joint stabilisation and replacement, and amputation, and lower-tier (salvage) procedures, including arthrodesis, denervation and excision arthroplasty. AntiNGF mAb = anti-nerve growth factor monoclonal antibody; NSAID = non-steroidal anti-inflammatory drug; PSGAGs = polysulfated glycosaminoglycans; TCAs = tricyclic antidepressants. Adapted with permission from Gruen et al. 18 This figure has been modified from the original and the recommendations related to acute pain in cats and acute and chronic pain in dogs have been removed

A cat being given a tablet in a soft tasty treat. Courtesy of Laura Watson, iCatCare

A 16-year-old cat with osteoarthritis after receiving a subcutaneous injection of monoclonal antibody anti-nerve growth factor. The opening on the top of the carrier makes it easy for the veterinarian administering the injection and less stressful for the cat, which is brought to the clinic monthly for the treatment. The carrier is always accessible to the cat at home and is impregnated with the cat’s own pheromones from previous occupancy, helping to reduce stress during transport and veterinary visits. Courtesy of Beatriz Monteiro
A cat undergoing acupuncture treatment for chronic pain. Courtesy of Samantha Taylor
Communication skills
Communicating to caregivers that their cat is in pain, and why, can be challenging and requires time and a sensitive approach. Effective communication can result in a better understanding of the patient’s welfare and improve the relationship between the caregiver and the veterinary clinic.90,91 Approaches such as signposting, ‘chunk and check’ and reflective listening (Table 7) bring emotional preparation, build trust, provide clarity and encourage shared decision-making, which improves the caregiver’s experience. 92 Discussing chronic pain with caregivers can be a challenge, particularly in cats, as changes in behaviour relating to pain can be very subtle. A large part of communicating with caregivers surrounding chronic pain entails education to help them understand their pet’s condition, using non-technical language.
Effective communication requires recognising the emotional challenges that caregivers face while caring for a cat with chronic pain. Caregivers often experience complex emotions such as anger, guilt and despair, which are evident in various forms of grief. 93 Acknowledging and adapting conversations to address these emotions is essential. 94
Telemedicine
Caregivers recognise the benefits of telemedicine,95,96 especially with regard to reducing the stress they and their cat experience in attending the veterinary clinic.95,97 The value of telemedicine to help with behavioural concerns 95 and follow-up appointments 96 has also been recognised. Telemedicine is well placed to assist in the ongoing management of chronic pain cases to ensure that medication is being given appropriately, 70 facilitate adjustments to the cat’s environment and care to ensure their needs are still being met,20,49 and to continue to monitor the response to the management plan via repeat use of validated pain scoring tools. 98 Although telemedicine use increased in 2020 during the early COVID-19 pandemic, 97 its overall uptake remains low95,96 despite willingness on the part of caregivers to pay for this service.95,96,99 Application of telemedicine should become an important part of the management plan of all feline chronic pain cases. 98
Hospice and palliative care
Hospice and palliative care are critical components of end-of-life care. 100 Hospice care is provided when patients are diagnosed with a life-limiting illness, and the plan changes from curing a condition to caring for their comfort and quality of life. Palliative care is provided when patients have incurable or curable diseases, to ensure relief from clinical signs. 74
The strengthening of the human–animal bond has driven the evolution of palliative care in veterinary medicine. As pets are increasingly viewed as family members, there is a heightened demand for veterinary professionals to educate caregivers on areas such as quality of life and comfort. 101 The earlier in the disease process these conversations occur, the better. Not only does this prepare the caregiver for future treatment and management, but it also obtains a baseline of the cat’s current quality of life, enabling more successful treatment monitoring. Using validated health-related quality of life or pain scoring tools, such as the Feline Musculoskeletal Pain Index (FMPI),78,79 the Cat HEalth and Wellbeing (CHEW) questionnaire 84 or the online VetMetrica tool,86,102 not only monitors the patient, but can also help to educate the caregiver. Completing these questionnaires regularly, relying on observations made by the caregiver, allows them to visually understand their cat’s needs emotionally as well as physically.
Caregivers experience an emotional burden during hospice and palliative care for their cat, and the veterinary team’s role in this is to ensure the right resources are provided and reassurance is given to the owner. When the cat’s quality of life begins to deteriorate, caregivers can experience anticipatory grief, which is where the caregiver begins emotionally preparing for the loss of their pet. 93
End-of-life decisions
Although the end of a patient’s life is inevitable, careful planning and thoughtful decision-making can ensure that the process is as peaceful and pain-free as possible for the patient and the caregiver. Assisting the caregiver to reach this decision can be difficult and requires a balance between the cat’s physical comfort and the caregiver’s emotional readiness to let go.
The caregiver’s assessment of their cat’s health often differs in comparison to the veterinary professional’s assessment;86,101 therefore, using quality-of-life scoring tools can support the caregiver when making the end-of-life decision. As discussed above, feelings of anticipatory grief can overwhelm the caregiver’s decision-making ability. This type of grief can bring a high caregiver burden, bringing feelings of anxiety, dread and guilt. Informing caregivers that these feelings are normal, listening to their concerns, and addressing them with empathy and sensitivity can help them feel supported. 93 Ensuring they are well informed and involved in the end-of-life decision-making process can reduce negative emotions associated with grief. 103
The experience of the caregiver during the euthanasia process can also impact on grief, especially in relation to the care and empathy offered at the time and the way the animal is handled. 104 Therefore, the euthanasia process itself should be carefully considered and individual to the patient and the caregiver, whether this occurs at home or in the clinic.
Caregivers can be provided with support by the veterinary team after the euthanasia, whether this is through follow-up communication or providing resources that are freely available. By providing this support, the team can prevent the caregiver from feeling isolated or experiencing disenfranchised grief, where they feel their grief is not acknowledged by society. 105
Conclusions
The journey of cats with chronic pain and their caregivers is influenced by numerous factors, including the clinical condition of the cat and the caregiver’s response to different burdens, but mostly by the care they receive from the clinic and veterinary teams involved in the process, through several opportunities for interactions between all these stakeholders. Chronic pain is likely to affect many cats with increasing incidence as they age. Management of these patients is focused on maintaining their quality of life while empowering caregivers to be part of the healthcare team. Empathetic communication is paramount and helps to optimise the cat’s care while supporting caregivers on the journey from initial assessment until, for most cases, end-of-life decisions.
Footnotes
Conflict of interest
Beatriz Monteiro works as a full-time employee at Zoetis. The remaining authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
This work did not involve the use of animals and therefore ethical approval was not specifically required for publication in JFMS.
Informed consent
This work did not involve the use of animals (including cadavers) and therefore informed consent was not required. No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.

