Abstract
Objectives
The aim of this study was to investigate the antiemetic, behavioural and physiological effects of oral maropitant treatment before the administration of brimonidine ophthalmic solution in healthy cats.
Methods
Five cats received oral maropitant 8 mg or no treatment (control) 18 h before the administration of one drop of brimonidine solution in both eyes. Each cat was administered each of the two treatments, with a washout period of 1 week. The incidence of emesis, retching, sialorrhoea and lip-licking after brimonidine administration was recorded, while behavioural and physiological parameters, including heart rate, mean blood pressure, respiratory frequency and rectal temperature, were recorded before and 0, 30, 60, 90, 120, 180 and 240 mins after brimonidine administration.
Results
Emesis and retching were not observed when maropitant was administered. However, 4/5 cats exhibited vomiting and retching in the absence of maropitant pretreatment. The incidence of emesis and retching after brimonidine administration was significantly lower in the treatment group than in the control group. Sialorrhoea occurred in one cat in the control group, while all cats showed lip-licking after brimonidine administration. There were no significant differences in the incidence of sialorrhoea and lip-licking between the two groups. Although behaviour scores were comparable between the two groups, those obtained during heart rate, mean blood pressure and respiratory frequency measurements were significantly lower than the baseline scores; this indicated a sedative effect after brimonidine administration. The heart rate and mean blood pressure significantly decreased after brimonidine administration in both groups, while there were no intergroup differences in the heart rate, mean blood pressure, respiratory frequency and rectal temperature.
Conclusions and relevance
Oral maropitant treatment before the administration of brimonidine ophthalmic solution in cats can alleviate emesis and retching without affecting the sedative effects of brimonidine and important physiological parameters.
Introduction
Brimonidine, an alpha (α)2-adrenoceptor agonist available as an ophthalmic solution, has been reported to have sedative effects in healthy cats. 1 To date, there has only been one study investigating the sedative and physiological effects of brimonidine in cats. Because brimonidine ophthalmic solution offers the advantages of non-invasive administration and minimal effects on cardiopulmonary function in cats, it is considered useful for clinical application. However, emesis, which is a well-known complication of other α2-adrenoceptor agonists such as medetomidine, dexmedetomidine and xylazine in veterinary medicine,2–6 has also been reported as an unpleasant clinical complication of brimonidine. 1
Previous studies in cats reported that oral maropitant, a neurokinin 1 (NK1) receptor antagonist, prevented or lowered the incidence of emesis induced by α2-adrenoceptor agonists, including xylazine and dexmedetomidine combined with morphine, although maropitant is not approved for oral administration in cats.7–9 We hypothesised that oral maropitant can prevent or lower the incidence of emesis induced by brimonidine ophthalmic solution without affecting the sedative and physiological effects of brimonidine in healthy cats. Accordingly, the aim of the present study was to evaluate the antiemetic, behavioural and physiological effects of oral maropitant treatment before the administration of brimonidine ophthalmic solution in healthy cats.
Materials and methods
Animals
This study, designed as a prospective, randomised, crossover experimental trial, included five experimental normal cats (three spayed and two intact) with a mean ± SD age of 5.7 ± 2.3 years, a mean weight of 4.3 ± 0.5 kg and no clinical signs. No abnormalities were detected during routine physical examinations, including measurements of heart rate (HR), respiratory frequency (fR), rectal temperature (RT) and mean arterial blood pressure (MAP). All cats were judged to have an American Society of Anesthesiologists’ physical status of 1. 10 The animals were maintained under uniform conditions in an institutional animal laboratory. All cats were fasted and served water, for 16 h before brimonidine administration. All experimental procedures were approved by the Animal Care and Use Committee of Kurashiki University of Science and the Arts (approval number 29-03).
Treatments
Each cat was administered each of the two treatments, with a washout period of 1 week between treatments. In the treatment group, the animals received 8 mg of oral maropitant (Cerenia; Zoetis), 18 h before the instillation of one drop of brimonidine ophthalmic solution (Aiphagan ophthalmic solution 0.1%; Senju Pharmaceutical) in the left and right eyes. In the control group, the animals received no treatment before brimonidine administration. Cases 1 and 2 received the control treatment first, while cases 3–5 received the experimental treatment first. The brimonidine solution was delivered via an eye dropper (Novel No 3; MI CHEMICAL) similar to that used in a previous study, 1 wherein approximately 58.6 ± 3.3 µl was delivered via one drop. In the present study, the left and right eyes received one drop each in immediate succession. After each administration, the nasolacrimal duct was occluded by a finger placed across the medial canthus for 10 s.
Procedures
The cats were moved into the cage in the experimental room for acclimatisation at 16:00 h on the day before brimonidine administration. Maropitant was orally administered to each cat in the treatment group at 17:00 h on the same day, and all cats received brimonidine ophthalmic solution at 11:00 h on the following day, following which they were moved back into their cage. Emesis and associated effects were observed for 60 mins after brimonidine administration. After the first 60 mins, the cats remained in the cage, without human interaction between the subsequent assessments. Behavioural and physiological evaluations were made by placing the cats on the examination table at baseline (30 mins before brimonidine administration) and 0, 30, 60, 90, 120, 180, and 240 mins after brimonidine administration. Behavioural assessments were made by a single observer (CT) blinded to the treatment order.
Evaluation
All cats were observed for emesis, retching, sialorrhoea and lip-licking. Emesis was defined as the forceful expulsion of gastric contents. Episodes of emesis separated by >5 s were considered individual events. Retching was defined as the rhythmic contraction of the diaphragmatic and abdominal muscles without the expulsion of contents. The time of occurrence and the total number of emesis and retching episodes were recorded for each cat. Sialorrhoea was defined as the collection of clear or frothy fluid around the lips, with or without dripping. Lip-licking was defined as licking of the lips.
Physiological parameters were measured in the following order: HR, fR, RT and MAP. HR was measured using a stethoscope, fR was measured from thoracic movements, RT was measured using a digital thermometer and MAP was measured using an electronic oscillometric device (petMap; Ramsey Medical), with the cuff attached to the left forelimb. These measurements were conducted with minimum physical restraint of the animals by a single investigator (HM).
Behavioural evaluation was based on five categories, namely posture, eye appearance, activity, tail position and response to interaction with a single investigator, which were modified from a previous study. 1 All categories were evaluated during measurement of the physiological parameters on the examination table. Table 1 shows the scoring system for all five categories. A higher total score (sum of scores for the five categories) indicated excitation or anxiety, while a lower total score indicated calmness or sedation. For evaluation of the treatment effect, the total score was calculated during the measurement of each physiological parameter (ie, HR, fR, RT and MAP). The scores obtained at baseline served as the reference values.
Description of the scoring system used for behaviour assessments in healthy cats that received oral maropitant before the administration of brimonidine ophthalmic solution

Statistical analysis
The significance of differences in the incidence of emesis, retching, sialorrhoea and lip-licking, which were considered all-or-none events, was examined using Fisher’s exact test. The behavioural assessment data are reported as medians (ranges), while the physiological parameters are reported as means ± SEMs. The physiological parameters and behavioural scores were analysed using Friedman’s test for repeated measures for evaluation of the time effect in each treatment. When a significant difference was found by Friedman’s test, Dunn’s test was used to compare the baseline value with that at the particular time point. Values at each time point were compared between the two groups using the Wilcoxon test. All statistical analyses were performed using GraphPad Prism 8. A P value of <0.05 was considered statistically significant.
Results
Emetic events
Emesis after brimonidine administration was observed in four cats in the control group (case 1, 40 mins; case 2, 19 mins; case 4, twice at 13 mins and once at 44 mins; and case 5, 24 mins) (Table 2) and none of the cats in the treatment group. Thus, the incidence of emesis was significantly lower in the treatment group than in the control group.
Incidence of emesis, retching, sialorrhoea and lip-licking in cats receiving 8 mg of maropitant orally at 18 h prior to brimonidine ophthalmic administration, and in cats receiving no treatment (control)

Retching after brimonidine administration was also observed in four cats in the control group (case 1, 39 mins; case 2, 19 mins; case 4, 13 mins and 43 mins; and case 5, 14 mins) and none of the cats in the treatment group. Thus, the incidence of retching was significantly lower in the treatment group than in the control group.
Sialorrhoea was observed in one cat (case 4) at 50 mins after brimonidine administration in the control group. None of the cats in the treatment group exhibited sialorrhoea. The incidence of sialorrhoea was thus comparable between the two groups. Lip-licking was observed with both control and maropitant treatment in all five cats.
Behaviour assessments
In the control group, the behaviour scores during HR measurement (BhvHR) at 90, 120 and 180 mins after brimonidine administration were significantly lower than the baseline value; this result was seen at 60 and 180 mins in the treatment group (Figure 1a). The behaviour scores during MAP measurement (BhvBP) at 60, 90 and 120 mins after brimonidine administration were significantly lower than the baseline value in the control group. In the treatment group, BhvBP exhibited a significant decrease at 90 and 120 mins after brimonidine administration (Figure 1b). The behaviour score during fR measurement (BhvfR) exhibited a significant decrease at 60, 90 and 120 mins after brimonidine administration in the control group and at 120 mins after brimonidine administration in the treatment group (Figure 1c). Finally, the behaviour score during RT measurement (BhvRT) at 60 mins after brimonidine administration was significantly lower than the baseline score in the control group. In the treatment group, a decreasing tendency was observed, although the differences from baseline were not significant (Figure 1d).

Behaviour scores (Bhv) during physiological measurements of the (a) heart rate (HR), (b) mean arterial blood pressure (MAP), (c) respiratory frequency (fR) and (d) rectal temperature (RT) in five cats before (baseline; BL) and after administration of brimonidine ophthalmic solution into the left and right eyes. The cats in the control group (C; white circles) received no treatment before brimonidine administration, while those in the treatment group (M; black circles) received oral maropitant 18 h before brimonidine administration. Each cat was administered each of the two treatments, with a washout period of 1 week between treatments. Data are expressed as medians (ranges). *Significantly different from baseline (P <0.05)
There were no significant intergroup differences in BhvHR, BhvBP, BhvfR and BhvRT at any time point.
Physiological measurements
There were no significant intergroup differences in HR, MAP, fR and RT at any time point. HR after brimonidine administration was significantly lower than the baseline value at 60 and 120 mins in the control group and 60, 90, 120 and 180 mins in the treatment group (Figure 2a), while MAP exhibited a significant decrease at 60 and 90 mins in the control group and 60 mins in the treatment group (Figure 2b). There was no significant change in fR after brimonidine administration in either group (Figure 2c). While RT remained unchanged after brimonidine administration in the control group, it exhibited a significant decrease at 240 mins after brimonidine administration in the treatment group (Figure 2d).
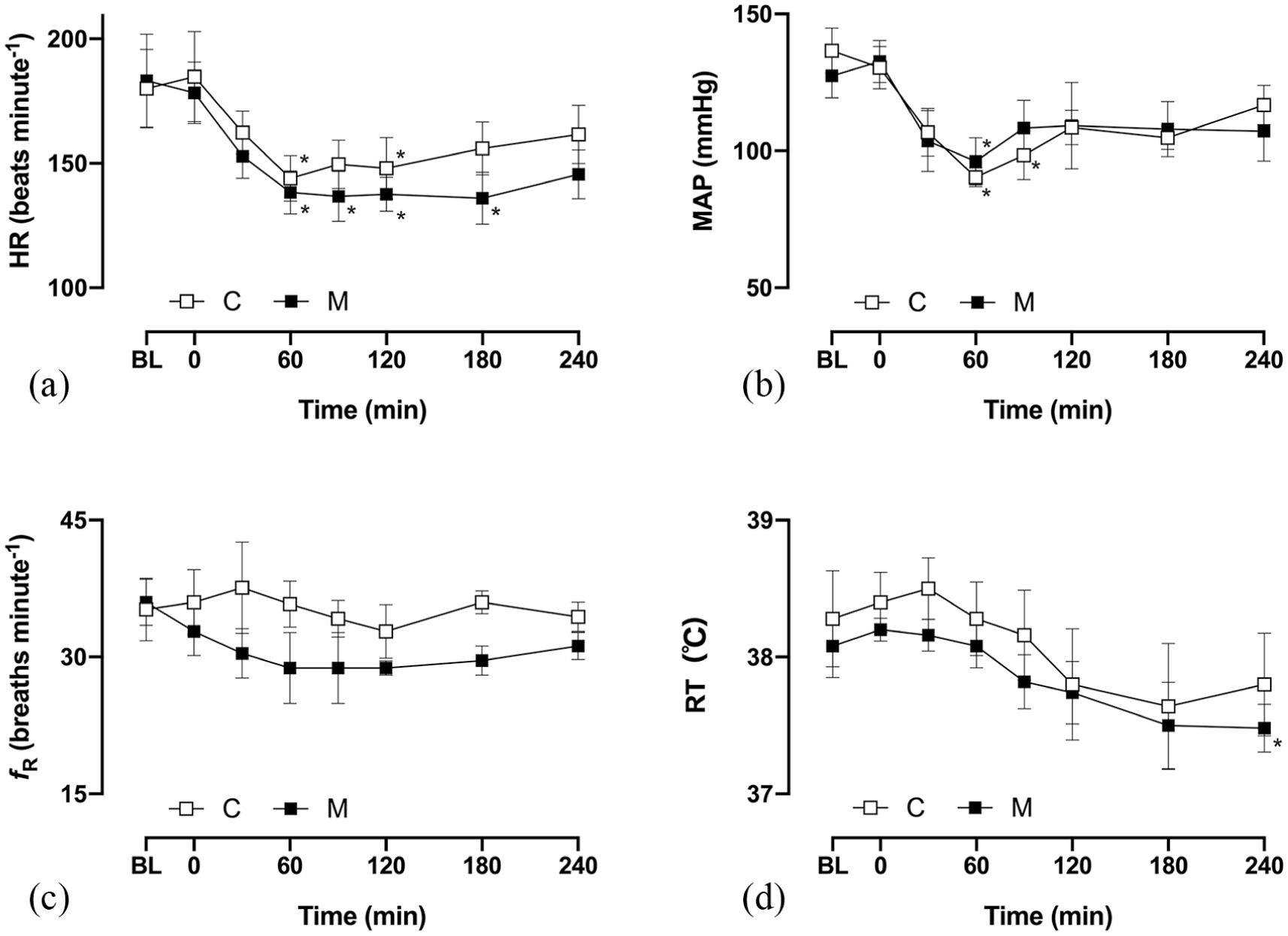
Measurements (mean ± SD) of the (a) heart rate (HR), (b) mean arterial blood pressure (MAP), (c) respiratory frequency (fR) and (d) rectal temperature (RT) in five cats before (baseline; BL) and after administration of brimonidine ophthalmic solution into the left and right eyes. The cats in the control group (C; white squares) received no treatment before brimonidine administration, while those in the treatment group (M; black squares) received oral maropitant 18 h before brimonidine administration. Each cat was administered each of the two treatments, with a washout period of 1 week between treatments. *Significantly different from baseline (P <0.05)
Discussion
In the present study, we found that pretreatment with oral maropitant significantly decreased the incidence of emesis induced by brimonidine ophthalmic solution in cats. Brimonidine is an α2-adrenoceptor agonist.11–13 In cats, α2-adrenoreceptor agonists stimulate the chemoreceptor trigger zone (CTZ) through the α2-adrenoceptors in the area postrema in the medulla.2,11 In the stimulated CTZ, binding of substance P with NK1 receptors activates the final common emetic pathway, resulting in the induction of emesis. 14 Brimonidine-induced vomiting has been reported in cats and dogs.1,15 Maropitant, an NK1 receptor antagonist, has been reported to inhibit vomiting by blocking the binding of substance P with NK1 receptors in cats.7–9,16 Accordingly, our findings suggest that emesis induced by brimonidine ophthalmic solution in healthy cats in the present study was inhibited by the antagonising effect of oral maropitant on NK1 receptors.
In the present study, maropitant was orally administered 18 h before the administration of brimonidine ophthalmic solution. In previous studies, the incidence of emesis and retching exhibited a significant decrease in cats that received oral maropitant 8 mg at not only 18 h, but also 2–2.5 h before intramuscular administration of a combination of morphine (0.1 mg/kg) and dexmedetomidine (20 µg/kg). However, the authors concluded that a longer interval between maropitant and dexmedetomidine administration resulted in greater antiemetic effects.8,9 Another study showed that the rate of decrease in emesis induced by xylazine was 90% in cats receiving oral maropitant 1.0 mg/kg 2 h before xylazine administration. 7 Accordingly, we believe that oral maropitant administered <18 h (eg, 2 h) before brimonidine administration may also produce sufficient antiemetic effects in cats.
In the present study, oral maropitant pretreatment did not influence sialorrhoea or lip-licking after brimonidine administration. In contrast, a previous study involving oral maropitant treatment 18 h before the administration of morphine and dexmedetomidine found a decrease in the incidence of lip-licking, 8 whereas a result similar to ours was obtained in the study where oral maropitant was administered 2–2.5 h before the same combination treatment. 9 Similar to the previous studies,7–9 the present study evaluated lip-licking as a sign associated with nausea. Unlike emesis, nausea is a multidimensional sensation induced by not only a physiological response, but also emotional and affective components, 17 and it is reportedly induced by the activation of cortical structures involved in conscious perception.18–20 As opposed to emesis or retching, nausea cannot be solely attributed to the effects mediated by NK1 receptors. Therefore, we believe that maropitant may play a role in the suppression of nausea, although it does not have a dominant or direct effect on the occurrence of nausea.
In the present study, behaviour scores obtained during measurements of different physiological parameters showed significant decreases or decreasing tendencies at 60–180 mins after brimonidine administration, regardless of the use of maropitant pretreatment. These results were in accordance with those of the previous study on brimonidine application in cats. 1 In addition, we found no significant intergroup differences in any behaviour score at any time point. This finding suggests that oral maropitant administration 18 h before brimonidine administration does not affect the sedative effect of the drug. Brimonidine ophthalmic solution is absorbed through the conjunctiva, cornea and mucous membrane of the nasal cavity before it passes through the blood–brain barrier to affect the central nervous system via α2-adrenoceptors,1,21 resulting in sedation. Meanwhile, maropitant is an NK1 receptor antagonist with low affinity for adrenoceptors, including α2-adrenoceptors. 22 Accordingly, we speculated that maropitant would not alter the sedative effects of brimonidine in healthy cats and confirmed the same in the present study.
In the present study, HR and MAP exhibited significant decreases from baseline at 60–180 mins after brimonidine administration in both the treatment and control groups. These findings are consistent with those in the previous study. 1 Moreover, there were no significant intergroup differences in these parameters at all time points after brimonidine administration. Alterations in cardiovascular parameters after brimonidine administration are considered characteristic of α2-adrenoceptor agonists, similar to other agonists.1,23–26 However, no study has reported alterations in HR or blood pressure after maropitant administration alone in conscious cats. It has been suggested that changes in HR and MAP are induced by α2-adrenoceptors, not NK1 receptors. Therefore, the finding that oral maropitant pretreatment did not affect the cardiovascular changes induced by brimonidine was justified in the present study.
The previous study showed that brimonidine ophthalmic solution did not significantly alter fR in cats. 1 A similar result was observed in the present study, regardless of the use of oral maropitant pretreatment.
In contrast to the finding in the previous study, 1 where RT significantly decreased after brimonidine administration in cats, the present study found no changes in RT in the control group. The reason for this discrepancy remains unclear. In the cats that received maropitant, RT exhibited a significant decrease at 240 mins after brimonidine administration. However, there were no significant intergroup differences in RT at any time point, which suggests that maropitant did not affect RT after brimonidine administration.
Administration of brimonidine ophthalmic solution at home before visiting a veterinary clinic may be useful for sedation and alleviation of psychological stress, fear and anxiety in cats. 1 However, emesis or retching can be an unpleasant complication. Our findings showed that oral maropitant treatment 18 h before brimonidine administration can prevent emesis or retching without altering the sedative effects of brimonidine. For example, if the owner or guardian is instructed to administer brimonidine ophthalmic solution at 9:00 h before taking the cat to the veterinary clinic at 10:00 h, oral maropitant should be given at 15:00 h on the previous day. However, further studies should evaluate the effects of maropitant on nausea, which is represented by signs such as lip-licking, after brimonidine administration in cats.
From a practical aspect, such a two-step treatment is not ideal, even though it could relieve cats from anxiety or stress. Conversely, oral gabapentin treatment was also reported to calm cats without obvious unpleasant effects, such as vomiting.27,28 Although both ophthalmic brimonidine and oral gabapentin treatments have the same goal of calming cats and reducing their stress or anxiety, a pharmacological approach is different for each of these treatments. In veterinary practice, it is very important to have multiple options to achieve one purpose. In the present study, ophthalmic brimonidine treatment combined with pretreatment with maropitant was observed to be another effective treatment for calming cats and reducing their stress or anxiety without causing emesis; however, it was not the simplest procedure.
This study has some limitations. First, potential statistical errors cannot be denied because of the small sample size. Second, the brimonidine and maropitant doses were standardised regardless of the body weight or body surface area of each cat. In other words, the dose per body weight or body surface area varied among cats, which could have influenced the results.
Conclusions
Oral maropitant administered 18 h before the instillation of brimonidine ophthalmic solution can alleviate emesis induced by brimonidine without altering the sedative effects of the drug or physiological parameters such as HR, MAP, fR and RT in healthy cats. Thus, oral maropitant pretreatment could be useful for the prevention of emesis in cats that require brimonidine for sedation or alleviation of fear or anxiety.
Footnotes
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
This study involved the use of experimental animals outside of internationally recognised high standards (‘best practice’) of individual veterinary clinical patient care. The study therefore had ethical approval from an established committee as stated in the manuscript.
Informed consent
Informed consent (either verbal or written) was obtained from the owner or legal custoidan of all animal(s) described in this study for the procedure(s) undertaken.
