Abstract
Background: Levosimendan (CAS: 141505-33-1) is a myocardial calcium sensitizer that improves myocardial contractility in various forms of heart failure. It produces a moderate improvement in cardiac output (CO) without an improvement in blood pressure (BP) in verapamil and metoprolol poisoned rodents. Aim: To assess the effect of various levosimendan dosing regimens on hemodynamics in a rodent model of propranolol poisoning. Method: Male Wistar rats (350-450 g) were anesthetized, ventilated, and instrumented to record BP, heart rate (HR), and CO. Propranolol was infused continually. When BP dropped to 50% of baseline rats received 1 of 7 treatments: (1) 0.9% saline (control), (2) levosimendan 36 μg/kg loading dose then 0.6 μg/kg per min, (3) levosimendan 0.6 μg/kg per min, (4) epinephrine 0.5 μg/kg per min, (5) levosimendan 70 μg/kg loading dose then 1.2 μg/kg per min, (6) levosimendan 1.2 μg/kg per min, and (7) levosimendan 70 μg/kg loading dose alone. Hemodynamics were recorded every 10 minutes for 70 minutes. Cardiac output, mean arterial pressure, and HR for each group were compared with control. Results: All groups had comparable baseline and maximal toxicity hemodynamics prior to initiation of treatment. Levosimendan did not improve CO or BP with any dosing regimen. Blood pressure tended to be lower than control for all doses of levosimendan. Epinephrine significantly improved BP but not CO compared to all other treatment groups. Survival did not differ between groups. Conclusions: Unlike in verapamil and metoprolol poisoning models, levosimendan did not improve CO or survival in propranolol poisoning. Epinephrine improved BP, but not CO, suggesting that its actions were due to peripheral vasoconstriction.
Introduction
Beta-adrenergic receptor antagonists (BBs) and calcium channel blocking agents are 2 of the most common classes of drug involved in severe cases of deliberate self-poisoning, leading to significant myocardial depression, hemodynamic compromise, and shock. Treatment of shock may be problematic and often requires treatment with multiple inotropic and pressor drugs to support the hypotensive patient. 1 –5
Levosimendan is an inotropic agent that improves myocardial contractility by increasing the sensitivity of troponin-C to calcium. However, it does not increase intracellular calcium, adenosine triphosphate concentrations, or myocardial oxygen demand. 6 ,7 It is also a mild inhibitor of phosphodiesterase-III and causes relaxation of peripheral vascular smooth muscle by an agonist action on vascular smooth muscle voltage-gated potassium channels. 8 As a result, levosimendan produces an increase in cardiac output (CO) and a reduction in afterload. Previously, we have reported that levosimendan infusion resulted in a moderate, but significant, improvement in CO in both verapamil and metoprolol poisoned rats. However, it did not result in an associated increase in systemic blood pressure (BP). 9 This suggests that the vasodilatory effects of levosimendan may antagonize the benefits resulting from an improvement in CO in cardiovascular drug poisoning. 9 –11
In a swine model of verapamil poisoning, Kurola et al reported similar results to those observed in our previous work. They observed that a single bolus dose of levosimendan caused improvement in survival and CO but not BP. 12 To date, there are a limited number of studies reporting the effects of levosimendan in experimental BB poisoning. Leppikangas et al reported that a single bolus injection of levosimendan at a dose of 1.2 mg, approximately 50 μg/kg, improved cardiac function and BP in a swine model of propranolol toxicity. 13 The degree of propranolol poisoning in this study was described as “moderate” and there may have been some mismatch in the severity of poisoning between the control group and the levosimendan group prior to the initiation of treatment. 14 Additionally, levosimendan was only administered as a single dose rather than as an infusion as is usually the case in the clinical setting. Finally, the positive control treatment arm used dobutamine, a relatively weak indirectly acting catecholaminergic inotrope that also produces vasodilation.
In our previous study of metoprolol poisoned rodents, levosimendan produced a moderate improvement in CO and survival but not BP. 15 In this study, we examined the effects of levosimendan in propranolol poisoning, utilizing our previously described rodent model of cardiovascular drug toxicity. 9 ,10 ,15 We aimed to assess whether our previously utilized dosing regimen or higher doses of levosimendan would have an effect on hemodynamic compromise in propranolol poisoning. Levosimendan was administered as a loading dose only (as reported by Leppikangas et al), and as an infusion with and without a loading dose, at 2 doses. Propranolol was chosen as the toxicant in this study as this is one of the most toxic BB agents in overdose with both beta-adrenergic receptor antagonism effects and sodium channel blocking effects that result in cardiac conduction disturbances that become apparent in supratherapeutic doses.
Method
Male adult albino Wistar rats were utilized in this randomized open-label study. A single investigator performed the experiments once the surgery was completed, thus blinding was not involved. The method was similar to that described previously. 9
Animals
Consent was obtained from the Monash University Animal Ethics Committee. Only male adult albino inbred Wistar rats (11-14 weeks old) were used to avoid potential hormonal complications associated with the estrus cycle of the female rat.
Pre-experiment Procedures
Animals were anesthetized initially with isoflurane (Aerrane, Baxter Health Care, Toongabbie, NSW, Australia) in an enclosed Perspex anesthesia box. Once unconscious, 80 mg/kg intraperitoneal pentobarbital, a long-acting barbiturate agent, was administered (Ilium Pentobarbitone, 60 mg/ml, Troy Laboratories, Smithfield, NSW, Australia). Animals were placed on a heating pad and under a heating lamp to maintain body temperature between 36°C and 38°C. A midline skin incision was made in the neck and the trachea was isolated and cannulated and the animals were ventilated (10 mL/kg and 55 breaths/min) using an Ugo Basile model 7025 Ventilator (Comerio, VA, Italy). The left carotid artery was identified, isolated, and cannulated and a MLT1402 T-type Ultra Fast Thermocouple probe (AD Instruments, Castle Hill, Australia) was passed through the canula for aortic blood temperature measurement for CO estimation by the thermodilution technique. The left and right jugular veins were identified, dissected, and isolated from the surrounding subcutaneous tissue and cannulated with double lumen polyethylene catheters (Intramedic, North Rocks, Australia) for infusion of drugs and fluids. Similarly, the left femoral artery was identified and dissected from its fascial sheath, isolated, and cannulated with single lumen polyethylene tubing (BD Diagnostics, Sparks, Maryland) for arterial BP monitoring using an ADInstruments MLT844 physiological pressure transducer and ML110 bridge amp (ADIstrusments, Castle Hill, Australia). A rectal temperature probe was inserted for tissue temperature monitoring. Cutaneous electrocardiogram (ECG) electrodes were placed for single lead recording of heart rate (HR) and rhythm. Continuous data collection for ECG, arterial BP, rectal, and core temperature was performed using a PowerLab 4/30 data acquisition system and Chart Version 5.0 software (ADInstruments, Castle Hill, Australia). Cardiac output was estimated sequentially with the PowerLab cardiac output system and Cardiac Output Module Software (ADInstrument, Castle Hill, Australia). Briefly, 100 μL of cold Hartmanns solution (Baxter Healthcare Pty Ltd, Toongabie, Australia) was injected via the left internal jugular vein and a thermodilution curve was recorded from the carotid thermistor probe on PowerLab Chart Software. Cardiac output was calculated using the area under the curve by Cardiac Output Module found in PowerLab Chart Software. Cardiac output is reported in mL/min per 100 g of animal weight to be able to standardize and compare CO across animals of varying body weights in a similar way to which cardiac index is used to standardize this parameter to body surface area in humans. Average CO for healthy rats is reported as 20 to 25 mL/min per 100 g of animal weight. 16
Once surgery was completed, animals were allowed 30 minutes for equilibration. Prior to commencement of experiment baseline HR, mean arterial pressure (MAP), systolic BP (SBP), QRS duration, and CO were recorded. Hemodynamic parameters were then recorded at peak toxicity (time 0) and every 10 minutes during treatment for 1 hour or until death. Two syringe pumps were used for drug infusion during the experiment (Graseby 3100; Terumo model STO 523). Animals were euthanized at the end of the experiment.
Experimental Protocol
There were 10 animals per study group. Animals were administered propranolol (Sigma Chemicals, Missouri) made up to a concentration of 20 mg/mL in 0.9% saline solution by continuous infusion of 24 mg/kg per h until MAP fell to 50% of baseline (time 0). Propranolol infusion was then reduced to 12 mg/kg per h to maintain toxicity. Once toxicity was established, HR, MAP, SBP, electrocardiographic QRS duration (QRSD), and CO were recorded and animals were randomly assigned to 1 of 4 treatment groups (10 rats in each group).
The treatment groups were:
Control. Rats received 0.9% saline loading dose of 10 mL/kg infused over 10 minutes followed by normal saline infusion of 10 ml/kg per h for 60 minutes.
Levo with loading and infusion (Levo-LI). Rats were administered levosimendan (Simdax®, 2.5 mg/ml, Orion Corporation, Finland) 36 μg/kg in 10 mL/kg of NSaline as loading dose, infused over 10 minutes followed by 0.6 μg/kg per min as an infusion dose in 10 mL/kg per h 0.9% saline for 60 minutes.
Levo infusion only (Levo-I). Rats received levosimendan 0.6 μg/kg per min as an infusion with 10 ml/kg of 0.9% saline as loading dose, infused over 10 minutes, which was then continued at 10 mL/kg per h for 60 minutes.
Epinephrine infusion (Epi). Rats received 0.5 μg/kg per min of epinephrine (1 mg/ml, AstraZeneca Pty Ltd, Australia) as a continuous infusion with 10 mL/kg loading dose of 0.9% saline followed by 10 mL/kg per h over 60 minutes.
High-dose Levo infusion with loading dose (HDLevo-LI). Rats received levosimendan 70 μg/kg in 10 mL/kg of 0.9% saline as loading dose, infused over 10 minutes followed by 1.2 μg/kg per min as an infusion dose in 10 mL/kg per h 0.9% saline for 60 minutes.
High-dose Levo infusion only (HDLevo-I). Rats received levosimendan 1.2 μg/kg per min as an infusion dose with 10 mL/kg of 0.9% saline as loading dose, infused over 10 minutes, which was then continued at 10 mL/kg per h for 60 minutes.
High-dose Levo loading dose alone (HDLevo-B). Rats received levosimendan 70 μg/kg in 10 mL/kg of 0.9% saline as loading dose, infused over 10 minutes followed by 10 mL/kg per h NSaline as an infusion for 60 minutes.
The treatment protocol lasted a total of 70 minutes. Ten minutes for loading-dose infusions or 0.9% saline for those groups not receiving a loading dose, followed by 60 minutes for maintenance infusion. Heart rate, CO, QRS duration, SBP, and MAP were measured every 10 minutes for the duration of treatment. All animals received a 10 mL/kg loading dose of fluid and 10 mL/kg per h as an infusion with their respective treatments.
Data were analyzed and plotted graphically as mean ± standard error of the mean for the variables every 10 minutes until the end of the 70-minute treatment protocol or death using Graph Pad Prism Version 4.03 Software (GraphPad Software, Inc). QRSD was calculated at each time point as a mean of 5 consecutive QRS complexes from the end of the PR-interval to the commencement of the T-wave.
Statistical Method
Continuous hemodynamic measurements were compared using one-way analysis of variance and Dunnet posttest comparing each treatment group to control for normally distributed data or Kruskal-Wallis posttest for nonparametric data. Differences in mortality were assessed by Kaplan-Meier survival curve analysis.
Sample size was based upon the results seen in our previous studies with verapamil poisoning and levosimendan, where 10 animals per groups were sufficient to detect a 25% increase in CO between control and treatment groups. 9 ,11 All statistical analyses were carried out using GraphPad Prism 4.0 and InStat 3.01 statistical software (GraphPad Software, Inc).
Results
There was no significant difference in baseline MAP, CO, HR, and QRS duration in any groups, prior to the administration of propranolol (Table 1). Also at time 0 (peak toxicity), the hemodynamic parameters were comparable between all groups (Table 2). Animal weights were also similar between groups.
Summary of Baseline Hemodynamic Parameters
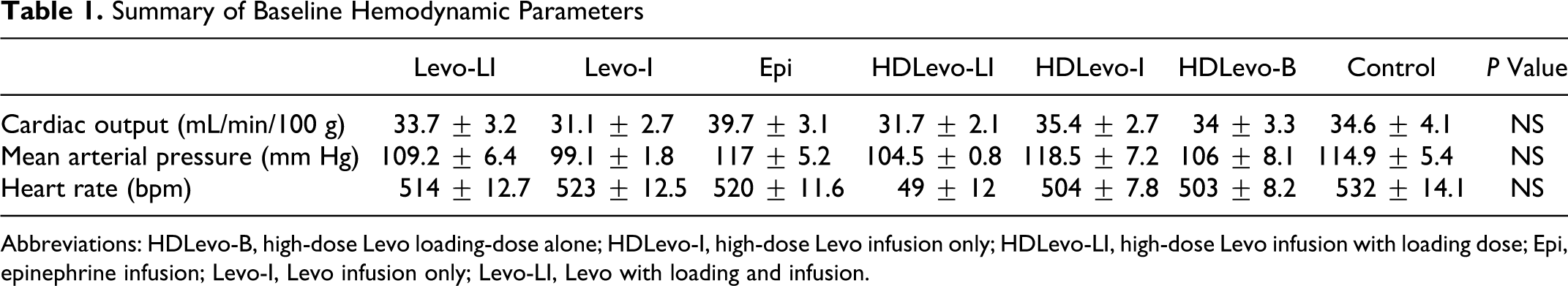
Abbreviations: HDLevo-B, high-dose Levo loading-dose alone; HDLevo-I, high-dose Levo infusion only; HDLevo-LI, high-dose Levo infusion with loading dose; Epi, epinephrine infusion; Levo-I, Levo infusion only; Levo-LI, Levo with loading and infusion.
Summary of Peak Toxicity (t = 0) Hemodynamic Parameters
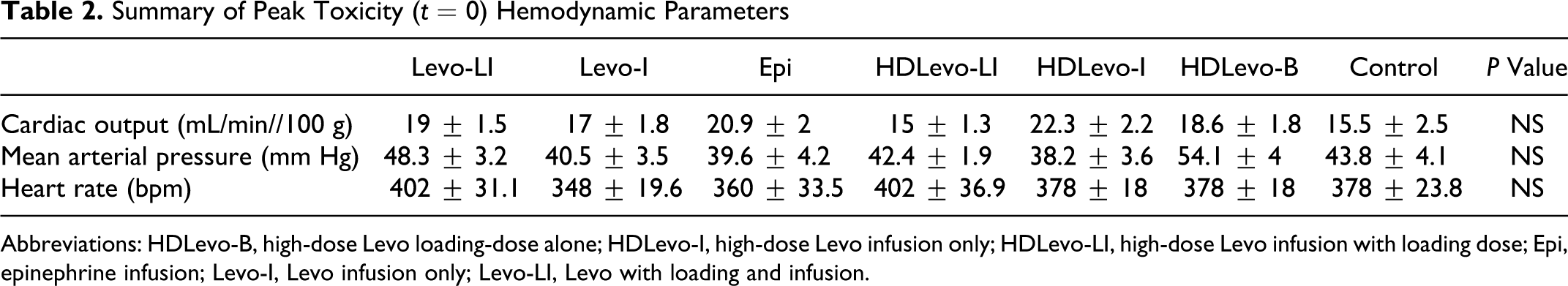
Abbreviations: HDLevo-B, high-dose Levo loading-dose alone; HDLevo-I, high-dose Levo infusion only; HDLevo-LI, high-dose Levo infusion with loading dose; Epi, epinephrine infusion; Levo-I, Levo infusion only; Levo-LI, Levo with loading and infusion.
Survival
There were no differences in survival at any individual time point for any of the 6 treatment groups, when compared to control (Figure 1).
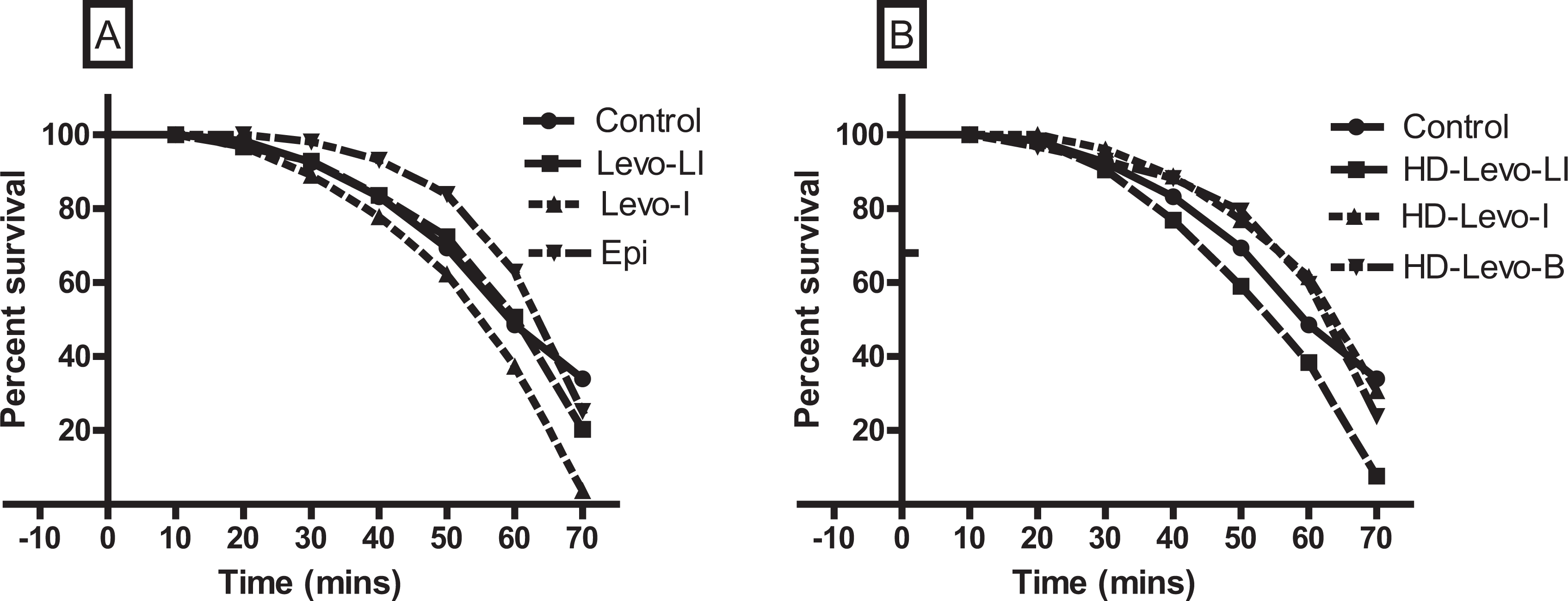
Kaplan-Meier survival curves of animals poisoned with propranolol treated with various levosimendan regimens. Panel A shows levosimendan infusion with loading dose (Levo-LI) and without loading dose (Levo-I) and epinephrine (Epi) versus control. Panel B shows high-dose levosimendan infusion with loading dose (HDLevo-LI), high-dose infusion alone (HDLevo-I), and loading dose alone (HDLevo-B) versus control. There were no significant differences in survival at any time point for the different treatment groups (n = 10 per group).
Cardiac Output
Levosimendan failed to produce a statistically significant increase in CO for both the loading dose with infusion (Levo-LI) and infusion alone (Levo-I) arms of the study. High-dose levosimendan produced a moderate but a nonsignificant increase in CO, at the t = 10 time point only. Epinephrine did not increase CO at any time point during the study (Figure 2).
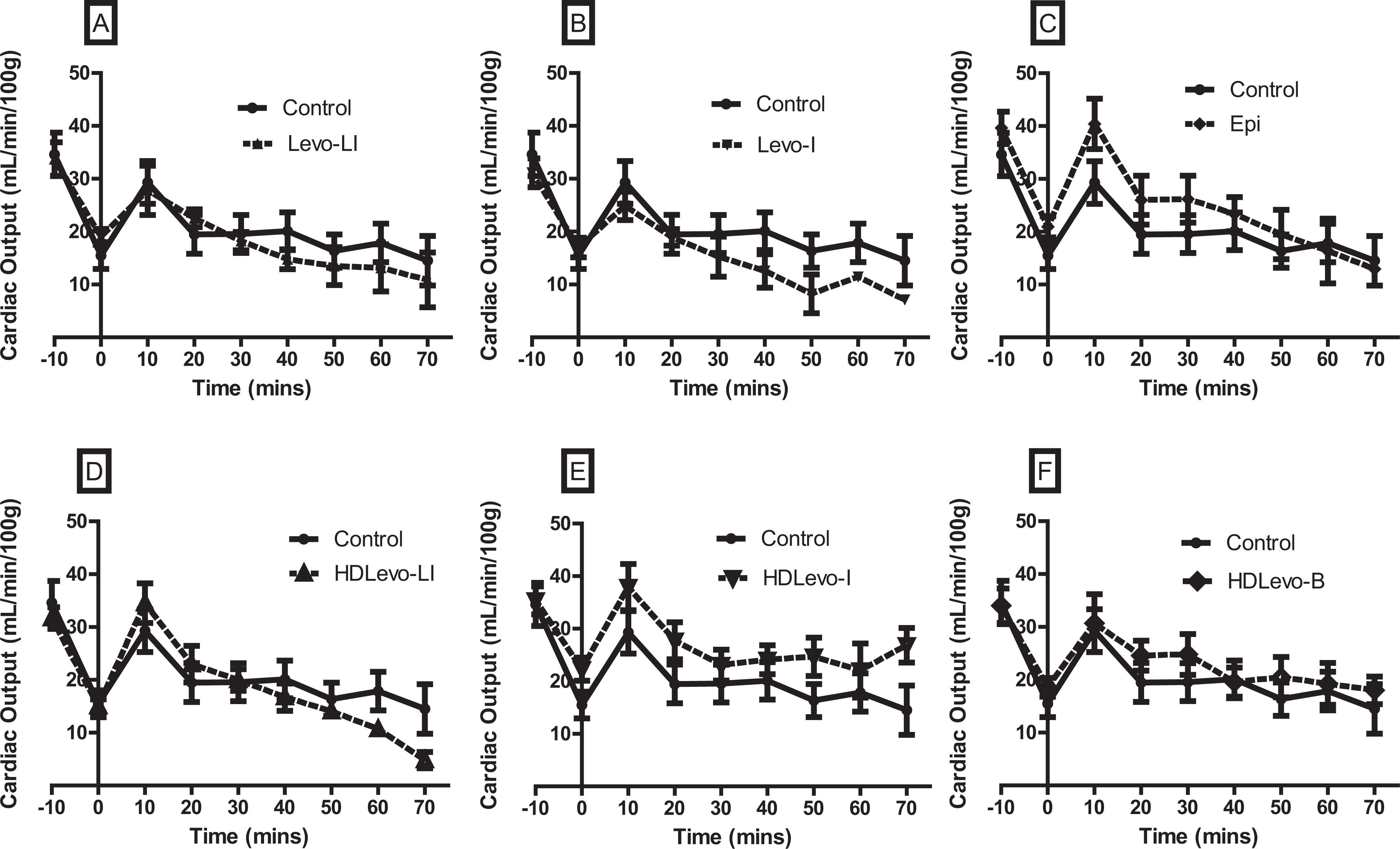
Cardiac output (CO) versus time for animals poisoned with propranolol and treated with various levosimendan dosing regimens (n = 10 animals per group). Panel A shows levosimendan infusion with a loading dose (Levo-LI), panel B shows levosimendan infusion without a loading dose (Levo-I), and panel C shows epinephrine (Epi) infusion versus control. Panel D shows high-dose levosimendan infusion with a loading dose (HDLevo-LI), panel E shows high-dose levosimendan infusion without a loading dose (HDLevo-I), and panel F shows high-dose levosimendan with a loading dose only (HDLevo-B). There were no significant differences in CO at any time point for any of the treatment groups. Data are expressed as mean ± standard error of the mean (SEM). Cardiac output is expressed in mL/min per 100 g of body weight of rat.
Mean Arterial Pressure
Blood pressure worsened with time in all levosimendan treatment groups in comparison to control group animals. However, epinephrine infusion was associated with a statistically significant increase in MAP at t = 10, t = 20, and t = 30 time points compared to control (Figure 3).
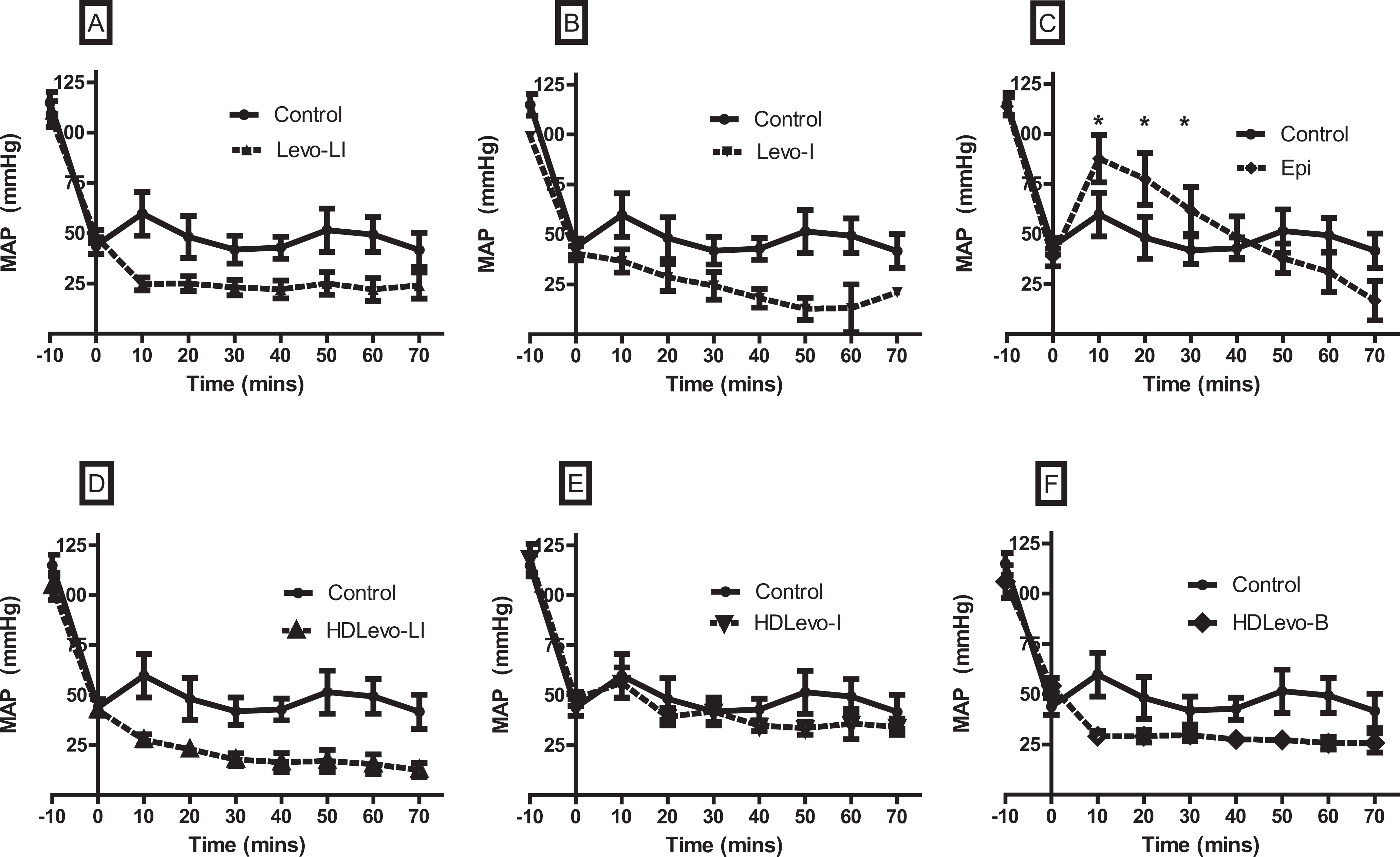
Mean arterial pressure (MAP) versus time for animals poisoned with propranolol and treated with various levosimendan-dosing regimens (n = 10 animals per group). Panel A shows levosimendan infusion with a loading dose (Levo-LI), panel B shows levosimendan infusion without a loading dose (Levo-I), and panel C shows epinephrine (Epi) infusion versus control. Panel D shows high-dose levosimendan infusion with a loading dose (HDLevo-LI), panel E shows high-dose levosimendan infusion without a loading dose (HDLevo-I), and panel F shows high-dose levosimendan with a loading dose only (HDLevo-B). Epinephrine produced a significant increase in MAP compared to control at t = 10, 20, and 30 time points (*P < .05). Epinephrine also produced a significant increase in MAP compared to all levosimendan groups at t = 10, t = 20, and t = 30 minutes (except HDLevo-I). In all levosimendan treatment groups there was no difference in blood pressure compared to the control at any individual time points. Data are expressed in mm Hg as mean ± standard error of the mean (SEM).
Heart Rate
There were no differences in HR at any individual time point with any of the 6 treatment groups compared to control. Heart rate decreased gradually with time for all treatment groups (Figure 4).
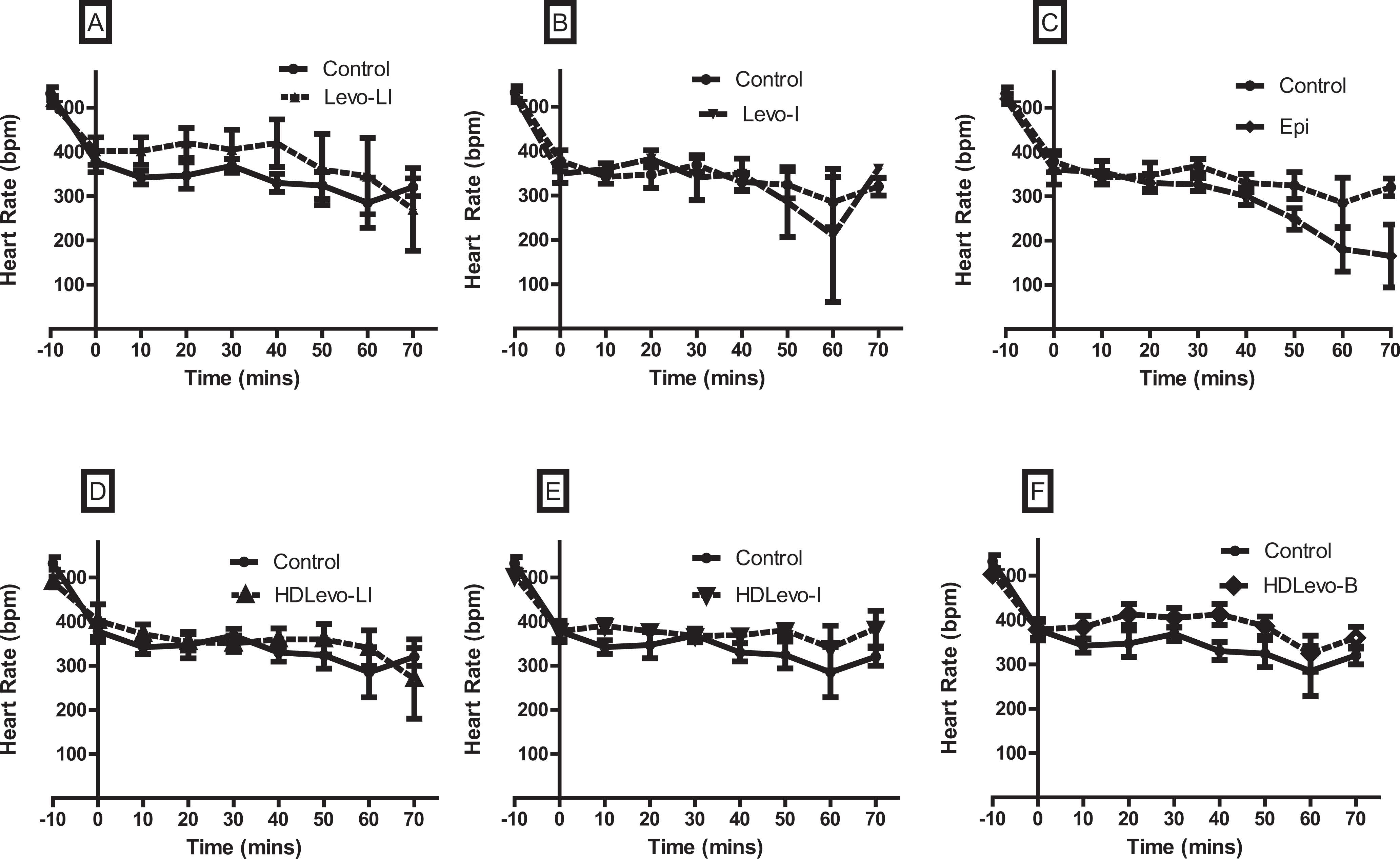
Heart rate versus time for animals poisoned with propranolol and treated with various levosimendan-dosing regimens (n = 10 animals per group). Panel A shows levosimendan infusion with a loading dose (Levo-LI), panel B shows levosimendan infusion without a loading dose (Levo-I), and panel C shows epinephrine (Epi) infusion versus control. Panel D shows high-dose levosimendan infusion with a loading dose (HDLevo-LI), panel E shows high-dose levosimendan infusion without a loading dose (HDLevo-I), and panel F shows high-dose levosimendan with a loading dose only (HDLevo-B). Heart rate was no different from control at any time point for any treatment group. Data are expressed as beats per minute (bpm) as mean ± standard error of the mean (SEM).
QRS Duration
There was a gradual increase in QRS duration in all treatment groups that did not differ over time, at any of the individual time points, when compared to control (Figure 5).
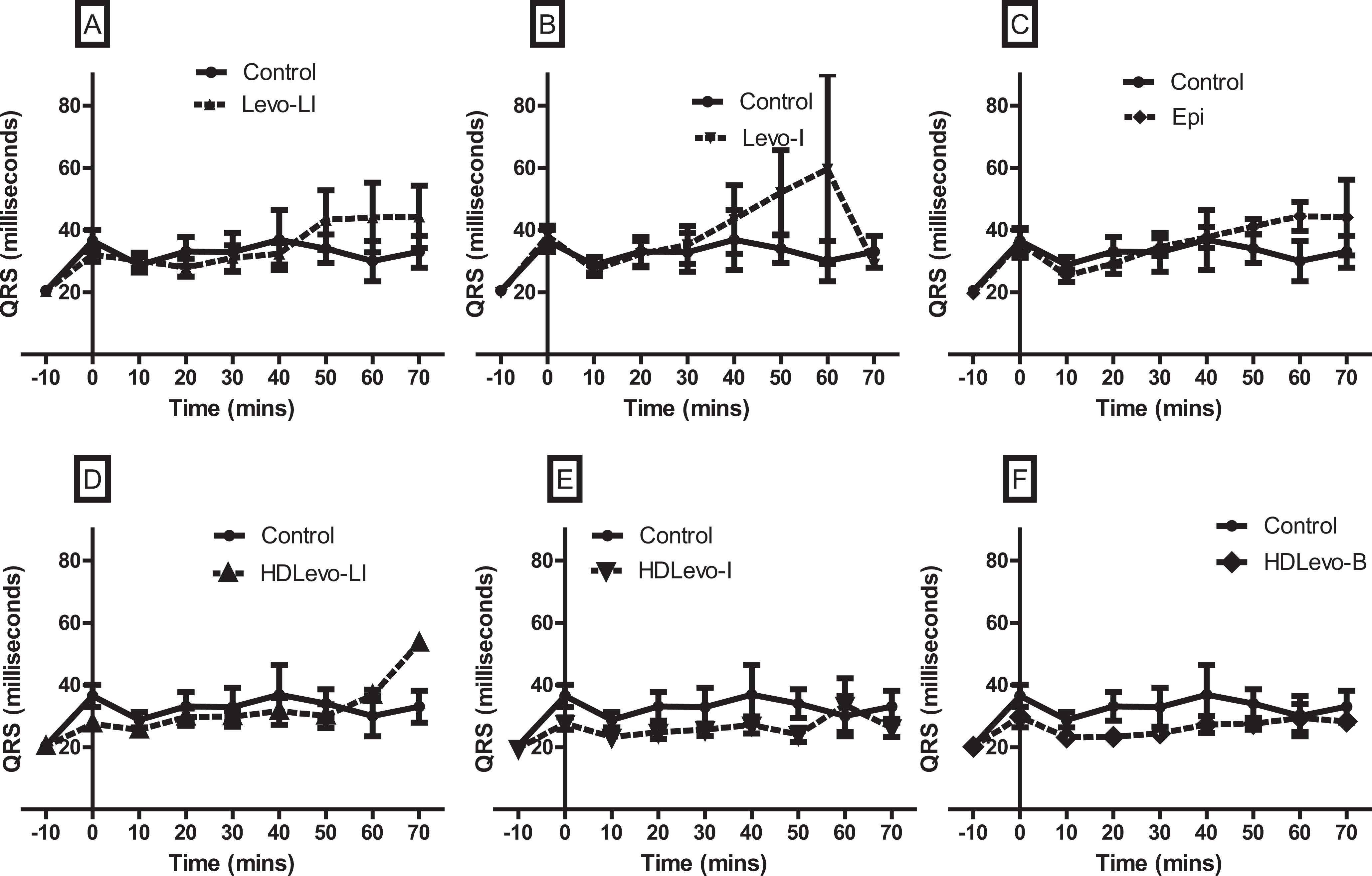
QRS duration versus time for animals poisoned with propranolol and treated with various levosimendan-dosing regimens (n = 10 animals per group). Panel A shows levosimendan infusion with a loading dose (Levo-LI), panel B shows levosimendan infusion without a loading dose (Levo-I), and panel C shows epinephrine (Epi) infusion versus control. Panel D shows high-dose levosimendan infusion with a loading dose (HDLevo-LI), panel E shows high-dose levosimendan infusion without a loading dose (HDLevo-I), and panel F shows high-dose levosimendan with a loading dose only (HDLevo-B). In the various treatment groups there was no difference in the QRS duration at any time point compared to the control. Data expressed in milliseconds ± standard error of the mean (SEM).
Discussion
Poisoning resulting from the overdose of beta-receptor antagonist can lead to bradycardia, hypotension, and shock. In addition, propranolol acts as a voltage-gated sodium channel blocking agent in overdose resulting in significant cardiac conduction delays and ventricular arrhythmias. 17 In severe beta-blocker toxicity, beta-receptor agonists such as epinephrine and isoproterenol may be ineffective in competing with high concentrations of propranolol at beta-adrenergic receptors. High-dose insulin-euglycemia therapy and high-dose glucagon therapy are used to improve myocardial function, without the need to directly stimulate beta-adrenergic receptors. 1 –5,18
Levosimendan increases CO and reduces afterload and is used in the treatment of nontoxicological forms of heart failure. 19 There are very few clinical reports of levosimendan use in cardiovascular drug poisoning. Case reports have described gradual hemodynamic responses to levosimendan, rather than immediate effects. Often, levosimendan was used as a drug of last resort. Thus, any response due to this drug may have been influenced by other coadministered therapies or may have been the result of the natural progression/resolution of the poisoning. 20 ,21
Previously, we have examined the effects of levosimendan on verapamil and metoprolol poisoning. Levosimendan produced a moderate improvement in CO and survival, without a concomitant improvement in BP in verapamil and metoprolol poisoned rodents. 9 ,11,15 Leppikangas et al reported on the effectiveness of levosimendan in experimental beta-blocker poisoning. In their swine model of propranolol toxicity, a single bolus injection of levosimendan at a dose of 50 μg/kg produced an increase in CO, BP, and survival. These improvements were superior to dobutamine. 13 A critique of this study observed that there was a significant difference in peak toxicity BP between the treatment groups. Beta-receptor blockade only appeared to be significant in the control group, as the fall in BP and HR were most evident in this group. 14 Also, the use of dobutamine as the positive control was unusual, given that clinicians are more likely to initially use other direct-acting catecholamine agents, such as epinephrine, to treat severe beta-blocker poisoning. Levosimendan has also been shown to be superior to dobutamine in the clinical setting of chronic low-output heart failure. 22 Finally, Leppikangas et al administered levosimendan as a single bolus dose and did not proceed with an infusion.
Because Leppikangas et al used a higher dose of levosimendan in their single bolus-dose experiments, we decided to assess high-dose regimens of levosimendan in our study to determine whether these would result in a greater improvement in CO. The higher dose of levosimendan in our study caused a nonsignificant but moderate increase in initial CO measurement compared to the lower dose regimens that we assessed. This effect disappeared with time. The degree of improvement in CO was still less than observed in our previous studies treating metoprolol and verapamil toxicity. 9 ,11,15 Furthermore, hypotension also persisted at the higher doses of levosimendan both with and without loading dose administration.
The sodium channel blocking effects of propranolol toxicity are manifested by a prolonged electrocardiographic QRS-interval duration and subsequent ventricular arrhythmias. 23 In our study, there was an increase in QRS duration in all groups that was not influenced by the treatment. In the clinical setting, intravenous sodium bicarbonate is often administered to reverse sodium channel blockade caused by propranolol and other Na+-channel blocking drugs. 24 In severe poisoning respiration is often depressed, resulting in the development of respiratory acidemia. This is known to worsen conduction delays. As a result mechanical hyperventilation is used to reduce blood carbon dioxide concentration and increase blood pH. 25 The rats in our study were mechanically ventilated prior to the onset of toxicity. We postulate that this prevented the development of respiratory failure from propranolol poisoning and as a result the lack of respiratory acidemia may attenuate the effect of sodium channel blockade. However, as we did not measure carbon dioxide concentrations or serum pH in our animals, we are unable to confirm this. Both levosimendan and epinephrine did not reduce QRS duration. We expected such results given that neither drug affects myocardial sodium channels.
It was anticipated that we would observe some improvements in CO, when using comparable doses of levosimendan, to those used in our previous models of verapamil and metoprolol toxicity. The lack of improvement in CO in our current model of propranolol toxicity may be the result of various factors. First, propranolol is known to cause more severe toxicity in overdose than many other commonly used BBs (eg, metoprolol and atenolol). This may be due to its greater lipophilicity and distribution to the myocardium. Also, its dual action of toxicity may influence the degree of myocardial depression in overdose. Beta-receptor antagonism in concert with sodium channel blockade in myocardial cells may have a synergistic action resulting in a degree of toxicity that cannot be easily overcome with the use of a single inotropic agent. In the clinical setting, severe propranolol poisoning must often be treated with multiple inotropic therapies to exert a positive physiological response. We did not test the effectiveness of levosimendan in conjunction with other inotropic therapies.
As in our metoprolol study, we chose to use epinephrine as our positive control catecholamine agent, because it is a more potent direct beta-adrenoceptor agonist than dobutamine, which was used in the study by Leppikangas et al. Epinephrine also has significant alpha-adrenergic receptor activity. We observed that epinephrine significantly improved BP, without an associated improvement in CO. This suggests that epinephrine was not directly stimulating the myocardium, but increasing BP via a primary vasopressor response. This may further suggest that the dose of epinephrine used in this study may not have been substantial enough to overcome the propranolol-induced beta-receptor antagonism. Given the failure of epinephrine-treated animals to have any improvement in survival despite higher BP, it suggests that adrenergic agents may not be the best choice of treatment in this poisoning. Increased BP from vasoconstriction may worsen heart failure in an already failing myocardium.
Limitations
In this current study, anesthetized rats were administered propranolol intravenously, which is not reflective of the human clinical overdose setting. As observed in our previous levosimendan studies using metoprolol and verapamil, we did not observe a decline in HR similar to the drop in BP. 9 ,11,15 In human beta-blocker poisoning, bradycardia (lowering of the HR) is a significant early characteristic. This was observed in the rats prior to death. However, the fall in BP and CO from baseline measurement in this study was significant. Nonetheless, levosimendan has been reported to improve CO in both human and animal models of nontoxicological cardiac failure. 26 ,27
The experimental study was nonblinded and the investigator knew the treatments administered in each experiment, thus observer bias may have been introduced in to data collection. However, given that all data collected in this study was objective, there was little opportunity to make subjective interpretations for the various treatments. The current study used a rodent model of propranolol poisoning. The vasodilation caused by levosimendan in the rat may not be as pronounced among other species. Similarly, this response may not necessarily reflect the human response to levosimendan at the doses used. Finally, the long acting barbiturate, sodium pentobarbitone, used in this study may affect BP and cause myocardial depression, if administered at high doses. However, the dose used in this study was similar to those cited in previous animal research studies, examining cardiovascular physiology of rodents, thus the effects on hemodynamic parameters were minimized. 28
Conclusion
In this model of severe propranolol poisoning we observed no improvement in CO, BP, or animal survival with levosimendan infusion with or without a loading dose, at a recommended clinical dose used by us previously in verapamil and metoprolol poisoning. At the higher dose of levosimendan, there was a moderate, nonsignificant improvement in CO initially, which was not sustained over time. Animals were persistently hypotensive with all levosimendan regimens. In this rodent model of propranolol poisoning, levosimendan exhibited no benefit on CO or BP, at the doses administered. Finally, epinephrine appears to exert its effects primarily through peripheral vasoconstriction in beta-blocker-induced heart failure. This has the potential to worsen heart failure by increasing afterload. Levosimendan should be used with caution, if it is to be considered in the treatment of poisoning-related heart failure in the clinical setting due to its potential to exacerbate hypotension, via its peripheral vasodilatory effects.
Footnotes
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
