Abstract
Given the scarcity of resources across child-serving systems, cost analyses can provide a framework for comparing evidence-based interventions, informing resource allocation, and guiding stakeholders to invest resources. The economic impact of autism is significant. One intervention found to be efficacious is social skills training (SST); however, there are few economic studies of SSTs. This study addresses the dearth of cost analyses of SSTs in the literature. An ingredients method was used, with cost data collected through informant interviews, program budgets, and the E$timator Tool Kit. Results revealed the SST implementation cost was lower than other autism-focused Early Intensive Behavioral Interventions; families bear the largest proportion of costs; and optimizing personnel-heavy interventions like SST may be possible through high-quality, intensive training of lower wage personnel by experienced trainers who also provide ongoing support and supervision.
Autism is a neurodevelopmental condition characterized by challenges in social interaction and communication, and restricted, repetitive behaviors (Diagnostic and Statistical Manual of Mental Disorders [5th ed., text rev.; DSM-5-TR]; American Psychiatric Association [APA], 2022). Social skill challenges can have significant negative impact on long-term outcomes of autistic individuals, including their mental well-being, academic achievement, and ability to secure employment and live independently in adulthood (Howlin et al., 2013). Since social impairment can impact quality of life (QoL), social skills training (SST) programs for autistic youth have proliferated (Wolstencroft et al., 2018). Studies indicate SSTs contribute to improved QoL; however, it is unclear what costs are associated with their implementation and delivery. Resource scarcity often requires choices regarding which to use and how (Barrett et al., 2020). Understanding the cost of implementation can provide a data-based framework for comparing evidence-based interventions (EBIs), inform resource allocation, and illustrate cost–benefit considerations (Cakir et al., 2020). The purpose of this study was to contribute to the scarce literature by conducting a U.S.-based cost analysis of an autism-focused SST program.
Autism and Quality of Life
There is a rise in autism rates, with recent estimates at 1 in 36 U.S. children (Maenner et al., 2023). Autistic individuals experience diminished quality of life (QoL), compared with neurotypical individuals and those with other neurodevelopmental differences (van Heijst & Geurts, 2015), making QoL improvement for autistic individuals a priority for research and practice. Social-communication difficulties may have a profound effect on children’s social development, as autistic children are more likely to face social rejection, bullying, and feelings of loneliness and isolation (Kerns et al., 2015). In adulthood, social challenges may reduce independence and impact employment, relationships, and mental and physical health (Rai et al., 2018).
Economic Costs of Autism
The documented increase in autism rates, combined with the extended support autistic individuals often require, creates an economic concern. Compared with non-autistic individuals, autism is associated with higher economic costs for individuals, families, health insurance systems, and state financial aid programs, along with productivity loss for adults and caregivers (Rogge & Janssen, 2019). For example, autistic children aged 3–17 years have US$3,020 higher annual healthcare costs and US$14,061 higher nonhealthcare costs, compared with non-autistic children (Lavelle et al., 2014). Costs in adulthood are incurred from care and lost productivity for autistic individuals and their parents, with lifetime per capita incremental societal cost of autism estimated at US$3.2 million (2003 prices; Ganz, 2007). Recently, Cakir et al. (2020) assessed the average per capita lifetime cost of autism in the United States in 2019 to be US$3,566,881, with costs in the United States reaching nearly US$15 trillion by 2029. Identifying interventions that improve outcomes of autistic individuals is critical, as well as studies that illustrate cost benefits associated with expenses avoided due to improved functional outcomes from interventions (Cakir et al., 2020).
Common Types of Economic Evaluations
Economic evaluation is an umbrella term for a family of methodologies, including cost analysis, cost feasibility analysis (CFA), and cost-effectiveness analysis (CEA), which examine allocation of resources to an intervention with some approaches examining cost against outcomes (Levin et al., 2018). Due to limited resources in public and private agencies, difficult choices must be made about distribution (Barrett et al., 2020). Understanding costs informs resource allocation, increasing the likelihood of implementation integrity and encouraging investment of resources (Barrett et al., 2020). For example, cost-effectiveness analyses are designed to compare interventions or innovations based on how much they cost relative to the outcomes that are yielded, while cost feasibility is focused on the sufficiency of resources to implement a program.
Cost analysis identifies the total cost for implementation and may inform resource allocation, independent of effectiveness data (Levin et al., 2018). While a societal perspective in public health and education fields is preferred, more targeted perspectives (e.g., school perspective) are still useful for understanding ingredients and associated intervention costs (Barrett et al., 2020). Cost analysis is by itself useful to describe resources required to ensure program implementation fidelity, predict expected cost of different versions, and understand resource distribution and financing across stakeholder groups (Levin et al., 2018).
Economic Evaluations of Autism Interventions
While interventions for autistic individuals have proliferated, few accompanying economic evaluations exist. The available few focus on cost-effectiveness of Early Intensive Behavioral Intervention (EIBI), such as applied behavior analysis (ABA; Sallows & Graupner, 2005); discrete trial training (DTT; Chasson et al., 2007); and the Early Start Denver Model (ESDM; Cidav et al., 2017). Costs of EIBI programs for autism are substantial, with annual costs for individual recipients to be between US$40,000 and US$60,000, although reported cost estimates for EIBI programs in other countries like the United Kingdom and Sweden may be lower depending on whether costs were categorized as education versus therapeutic (Rogge & Janssen, 2019). Despite high costs of EIBI implementation, cost-effectiveness studies report significant savings (Cidav et al., 2017). For example, Cidav et al. (2017) used data from a randomized efficacy trial of the ESDM compared with children receiving treatment as usual. Although children receiving ESDM had on average US$14,000 higher annualized health-related costs, they used therapeutic services less frequently, resulting in savings of US$19,000 annually per child.
There is a shift in type of autism-related services utilized and related costs as autistic children grow (Cidav et al., 2017). From ages 3 to 6, costs and utilization of EIBIs, occupational, physical, and speech therapy are large for families of autistic children (Ganz, 2007). However, as autistic children enter upper elementary years and beyond, there is greater demand for mental health and social skills interventions (Cidav et al., 2017). Despite the need, cost analyses are scarce, with a literature review identifying one economic evaluation of an SST from the United Kingdom and none in the United States. Wang et al. (2022) examined cost-effectiveness of a LEGO-based therapy in U.K. schools, where 126 autistic students learned social skills through building LEGO models in small groups. Total average cost was £14,272.80 per year (US$17,233.69) or £113.28 (US$136.78) per child. Compared with usual support, LEGO-based therapy produced marginal cost reduction and marginal improvement in quality-adjusted life years (Wang et al., 2022). In the United States, Smolkowski et al. (2022) conducted an economic analysis of We Have Skills (WHS), a nonautism-specific eight-session social skills intervention implemented in general education. We Have Skills cost US$69 per student first year with an effect size of 0.25; authors estimated cost-effectiveness ratio of US$276 per student, which was more cost-effective than similar programs.
Social Skills Training
As autistic children move to adolescence, social skills interventions are critical, resulting in an increase in SST programs (Wolstencroft et al., 2018). Studies substantiate SST as an evidence-based practice by the National Professional Development Center on autism (NPDC; Steinbrenner et al., 2020), improving social skills (Soares et al., 2021), social anxiety (Schohl et al., 2014), quality of play (Yoo et al., 2014), problem behaviors (Solomon et al., 2004), and loneliness (Mandelberg et al., 2014). SSTs are among the most widely received therapies for autistic children because cost, time, and location are often barriers to accessing clinical interventions (MacCormack et al., 2015). Pickard et al. (2018) surveyed autism service providers and families, finding SSTs received high ratings for perceived value from families and service providers. Community-based SST programs also occur in naturalistic settings, which can increase skill generalizability (MacCormack et al., 2015).
Common features of SST programs include having several autistic individuals in sessions led by one to three interventionists. Common topics include emotional recognition and regulation, social competence, social problem solving, and social communication (Rao et al., 2008). Groups meet in community settings once per week for 12 weeks or more, with sessions lasting 60 to 90 min. Evidence-based SSTs draw from principles of cognitive behavioral therapy (CBT), ABA, and behavioral skills training (BST; Moody & Laugeson, 2020). For example, psychoeducation, role-playing, behavioral rehearsal, and homework assignments are common in CBT, and in vivo coaching, performance feedback, and generalization opportunities are consistent with ABA and BST (Hassan et al., 2018; Moody & Laugeson, 2020). Successful SSTs include generalization supports (Hassan et al., 2018), train in natural settings (Kasari et al., 2016), use peer-mediated models (Koenig et al., 2010), require homework assignments for home and community practice (Laugeson et al., 2014), and include parent training (Cappadocia & Weiss, 2011). Despite effectiveness and popularity, however, few studies examine implementation cost. This is a gap in the literature, as translation of evidence-based practices (EBPs) into authentic community-based settings has continued to challenge researchers and practitioners (Barrett et al., 2020).
The community-based SST implemented in this study is a novel program designed to teach key social skills necessary targeting specific developmental periods, with a focus on learning and applying components of social skills in a group setting. Participants were enrolled in the program by their parents, following a detailed intake interview where the education director asked questions about the child’s academic and cognitive levels as well as their behavioral functioning. The education director determined whether the child had the verbal skills required to participate in the SST. Once enrolled, groups meet weekly, and skills are taught through explicit direct instruction, modeling, and rehearsal with feedback. Each 1 hr and 15 min session has a lead and assistant interventionist. Topics covered during the program include conversational skills (e.g., turn-taking, initiating conversation, and staying on topic); perspective-taking; self-confidence and assertiveness; and emotional regulation and self-awareness, with the goal of increasing impulse control (e.g., inhibition of inappropriate responses) and flexibility of thought and action.
Purpose of the Study
Social challenges in autistic individuals contribute to poorer QoL, and the growing population of autistic individuals makes it costly for various stakeholders (Rogge & Janssen, 2019). Research on autism-focused social skills interventions largely focuses on efficacy, not economic evaluations. Yet, economic evaluations are critical for identifying which services are a good investment of resources and contribute to positive outcomes (Barrett et al., 2020). This study details a cost analysis of a novel community-based SST, which will contribute to understanding resources required, predicting program costs, understanding distribution of costs across stakeholders, and will serve as a foundation for future economic evaluations (Levin et al., 2018). The study was guided by the following questions: (a) What are the total costs and ingredients associated with implementing one run of a community-based SST? and (b) How does the total cost of one round of the SST change with different values for prices or quantities of key ingredients (i.e., a sensitivity analysis)?
Method
Community Involvement
This study used cost data from community-based implementation of a 40-week SST during September 2018 to June 2019 and was developed through community-academic partnership where the university engaged in an agreement with the community agency to provide program evaluation services. Cost analysis questions and data were developed with the agency leadership. Results of the cost analysis and recommendations were shared with the community partner.
Community-Based SST
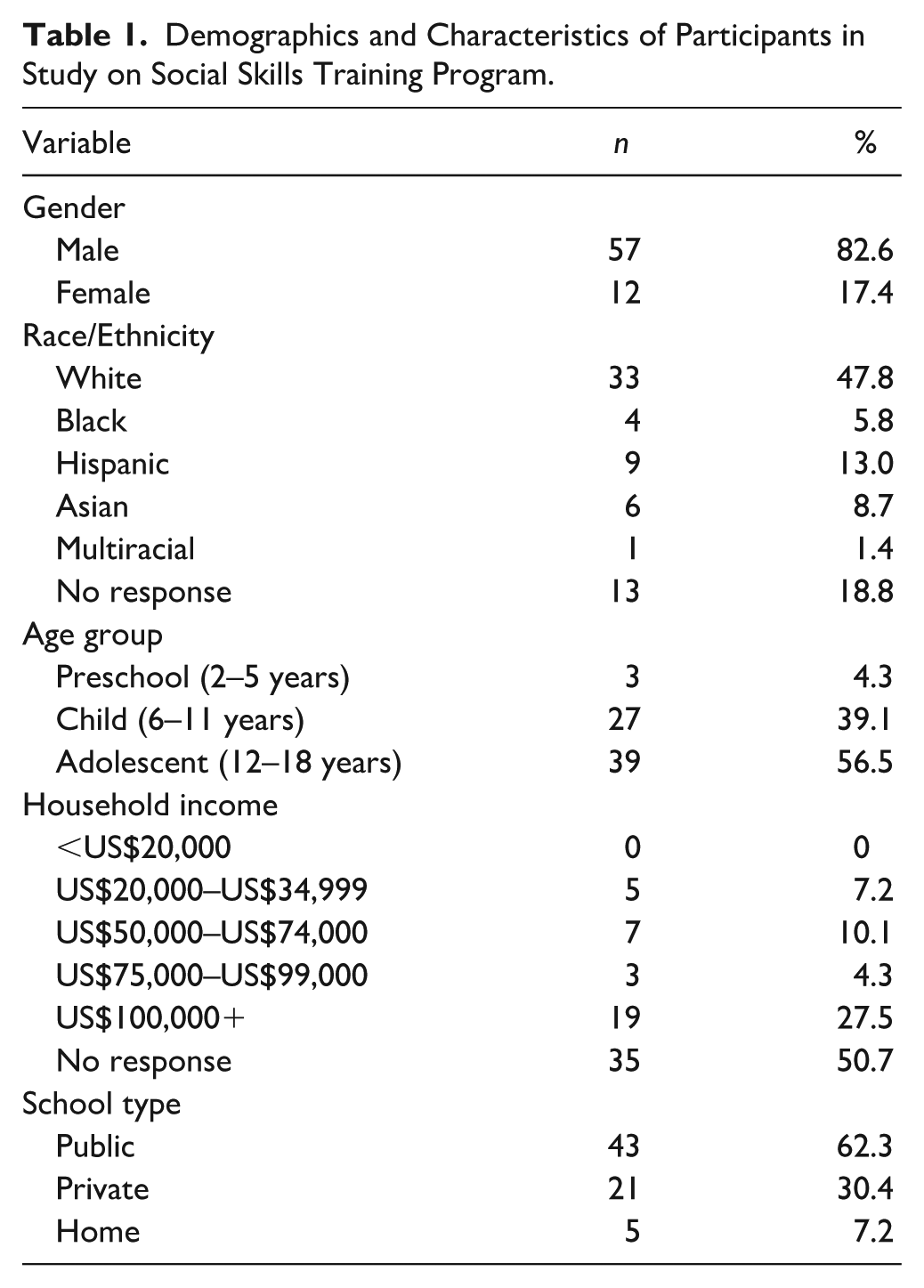
This study focused on costs of the program for 67 autistic children in the 2018 to 2019 school year (see Table 1 for demographics). Clients were enrolled in one of five levels: primary (PreK/K), lower elementary (first/second), upper elementary (third to fifth), Tweens (sixth to eighth), and Teens (9th–12th). Clients received developmentally appropriate, differentiated training in social competence, social problem solving, social communication, and emotional recognition and regulation. This program included 30 lessons and 10 community outings with clients attending sessions once a week (average: 60 min/week) and conducted by a lead interventionist and interventionist assistant (ratio of two professionals to eight students). Lead interventionists were certified special education teachers with a master’s degree. Intervention assistants were school-based paraprofessionals, advanced undergraduate, or graduate students in psychology or education; they were required to have at least 2 years of experience working with autistic individuals or similar disabilities. All interventionists completed training with the education director.
Demographics and Characteristics of Participants in Study on Social Skills Training Program.
Cost Data
The study used program implementation costs from September 2018 to June 2019 including costs paid by the community-based agency, external nonprofit organization, and each family/student, making findings generalizable to various stakeholders. Cost data should be interpreted within the economic context of the time period when data were collected. The following methods were used to capture implementation costs.
Key Informant Interviews and Questionnaire
The agency’s education director and executive director provided information about the program and resources through three interviews and a questionnaire adapted from the Center for Benefit-Cost Studies of Education (CBCSE) E$timator Interview Protocol (Hollands et al., 2015). Interviewees provided detailed accounts of activities and resources needed to run the community-based SST, including units of labor, training, equipment, supplies, and overhead. Records of expenditures for specific inputs were also collected from interviewees.
Program Budget and Other Costs
The community agency’s expenditures across 2018 to 2019 were used to capture costs and triangulate information from interviews, leading to a list of ingredients and their value.
Some lower-valued materials or costs were not directly accounted for (e.g., low-cost office supplies) and instead were estimated (E$timator Tool Kit; Hollands et al., 2015).
Description of Ingredients and Costs
Personnel Costs for Program Coordination, Administration, and Planning
Administrative staff included the education director, executive director, operations manager, and program coordinator. The Executive Director’s role was company oversight and governance. The education director planned, developed, and implemented the SST program; trained interventionists; conducted intakes; and communicated with parents. The operation manager managed payroll and facilities, while the program coordinator managed registration of clients, applied for grants, and handled program inquiries. All administrative staff were full-time (40 hr/week) and paid an annual salary for the SST program and two other concurrent programs. The education director dedicated 30 hr/week, while other staff spent approximately 15 hr a week specifically on the SST program. Hourly wage for administrative staff was determined by annual salary divided by 2,080 hr, the number of hours in a work year (on average, 40 hr/week, 52 weeks/year; National Center for Education Statistics, 2020).
Personnel Costs for Interventionists and Assistants
Eight interventionists who were certified special education teachers with a relevant master’s degree and 5 to 10 years teaching experience and eight assistants who held bachelor’s degrees and experience working with children with disabilities delivered the intervention. Program delivery occurred in classroom settings at the community-based agency. Interventionists and assistants spent 5 hr/week (40 weeks/year) delivering the program and 2 hr annually in training with the education director. Interventionist and assistant time were priced hourly with US$40/hr for interventionists US$20/hr for assistants.
Curriculum, Other Materials, and Training
Interventionists and assistants accessed free lesson plans and materials in print and electronically. Print materials provided to them during training and implementation represented printing costs that were calculated through E$timator.
Facilities and Annual Utilities
The SST was provided in a residential suburban area of a large metropolitan city in the southeast of the United States. The space was chosen due to its proximity to schools that collaborated with the nonprofit, as well as its convenience to major roadways. Three conference rooms (two were 200 sq. ft and one was 500 sq. ft.) and an office space (900 sq. ft.) in a leased commercial, single-story building were dedicated to planning and delivering the SST program. It was estimated that the rooms were used for the SST 25% of the time. Therefore, facility cost was calculated by multiplying the annual rental cost by 25%.
Equipment
Necessary equipment included desks and conference tables, student chairs, whiteboards, supplies, IT and website expenses, and fees and subscriptions for client registration and management. The lifetime of furniture was estimated through Internal Revenue Manual, Property and Equipment Accounting section (Internal Revenue Service [IRS], 2021). Cost of equipment was based on percentage use for the intervention. About 25% of conference room furniture was estimated for implementation, and 75% of office furniture was estimated toward planning, assuming 30 of 40 hr/week were spent running the SST program.
Description of Tuition Fees and Scholarships
While not an implementation cost, there were stakeholder-specific payments/monetary contributions that subsidized the cost of ingredients. Fifty-five families each paid US$2,400 for one program cycle, and 12 families paid subsidized fees as some of their fees were covered by scholarships. The community-based agency provided four full (worth US$2,400 each) and partial scholarships (US$1,400 each) to families requiring financial assistance. Four partial scholarships (worth US$1,000 each) were funded by a separate autism-focused nonprofit organization.
Cost Analysis Strategy
The ingredient method (Levin et al., 2018) was used to estimate SST costs from a community-based agency, family, and external nonprofit organization perspective. The following steps were included (a) identify ingredients for implementation (e.g., opportunity costs for personnel time), (b) assign monetary values to units for each ingredient (e.g., hourly wages for interventionists), (c) multiply number of units by values assigned (e.g., number of interventionists by hourly wages), (d) sum costs to determine costs per ingredient and total costs, and (e) apportion costs across systems or activities. Major categories of ingredients included direct costs of personnel, facilities, equipment, and materials. Indirect costs included network infrastructure (Internet connectivity) and administrative costs.
Total Costs by Stakeholders and Sensitivity Analyses
Cost analysis results are presented by cost to each stakeholder to provide a clear picture of who bears a share of the cost of this community-based SST.
Sensitivity analysis considered how main cost drivers affect total costs when varied. First, as staffing is often the most expensive ingredient (Lindstrom Johnson et al., 2020), sensitivity analysis tested different assumptions about salaries and experience for interventionists and assistants. The present interventionists’ pay is commensurate with national rates for special education teachers with 10 to 14 years of experience, so the sensitivity analysis included special education teachers with less experience (1–5 years), more experience (20+ years), and using teaching assistants as interventionists. Second, intervention- and autism-specific training, and use of trained professionals, are critical elements for successful SST program implementation (Dixon et al., 2016) so training and personnel support were included in the sensitivity analysis. To increase generalizability, the sensitivity analysis was costed with U.S. national average prices obtained from E$timator. The following scenarios were considered:
Interventionists: The first scenario varied personnel credentials.
Special education teachers with 1 to 5 years of experience (US$26.29/hr) or 20+ years of experience (US$63.13/hr); teaching assistant (US$18.53/hr).
Personnel support: The second scenario varied credentials of the education director.
Lower cost option being school counselors (US$31.23/hr); moderate cost option being school psychologists (US$38.37/hr); most expensive cost option being special education teachers with 20+ years of experience (US$63.13/hr).
Amount of training: The third scenario varied the number of training hours provided to support the SST implementation.
2 hr per 6 months (4 hr a year); 4 hr per 6 months (8 hr a year); 6 hr per 6 months (12 hr a year)
Results
Ingredients and Costs per Stakeholder
Total ingredients, descriptions, and attendant costs are detailed in Table 2. Program inputs included both variable and fixed costs. Variable costs were administrative and intervention personnel, training materials and hours, and session materials (printing of materials, classroom supplies). Since the community-based agency ran two other programs, a proportion of the week was estimated to be spent on the SST. Fixed costs included annual rental, furniture, and IT/website subscriptions. Fixed costs (US$6,996.99) comprised 1.96% of the total program cost. Most costs (98.04%) were variable, with personnel taking up the largest percentage of costs.
Ingredients and Costs for Implementing 40-Week Social Skills Training (SST) Program in the 2018 to 2019 School Year.
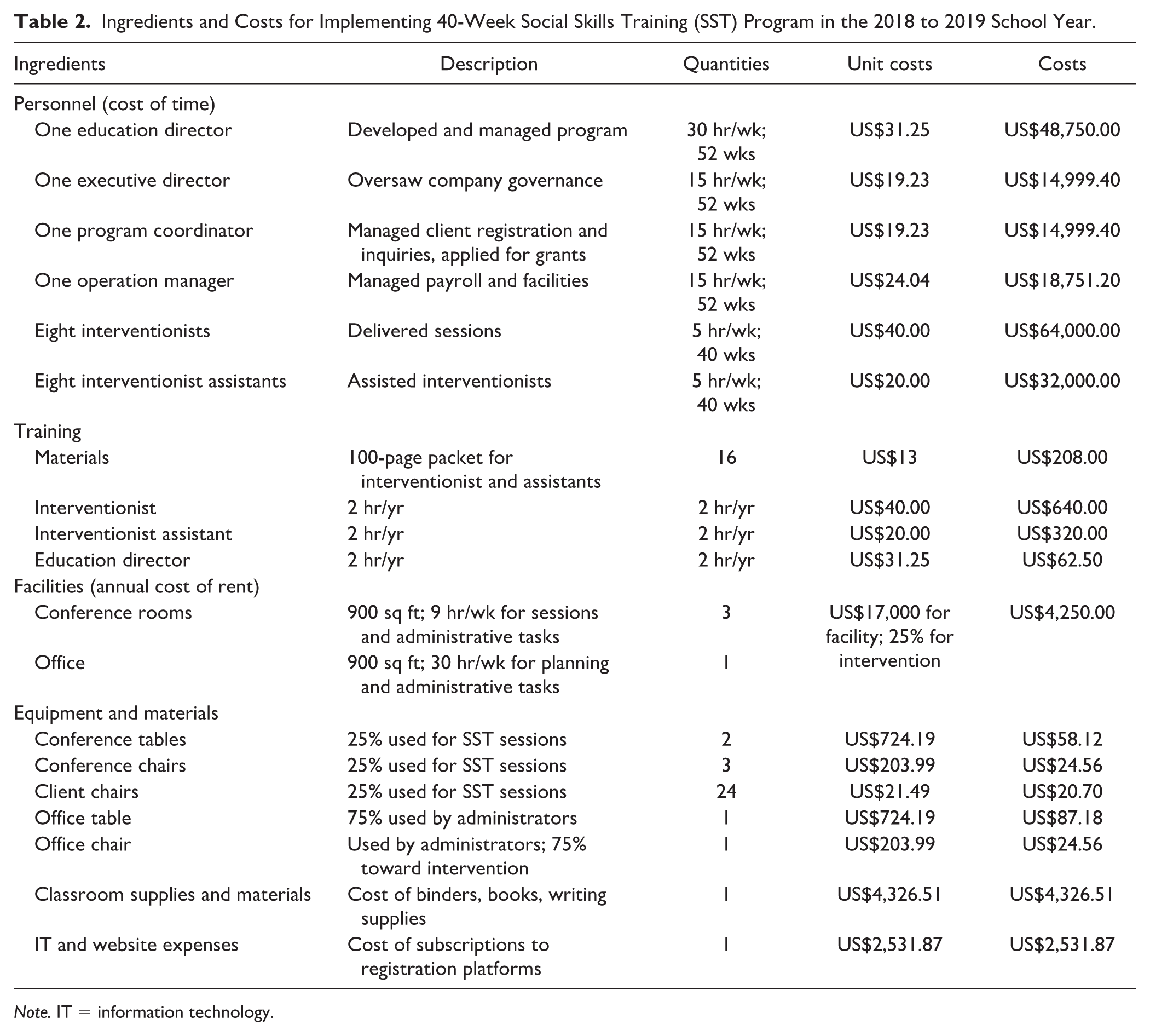
Note. IT = information technology.
Total cost of running the SST for one cohort was US$206,054.00 (average cost per participant = US$3,075.43), delivered to 67 students by eight interventionists and eight assistants. The greatest proportion of program cost was spent on personnel (US$193,500; 93.91%), followed by equipment and teaching materials (US$7,519,13; 3.56%); facilities (US$4,250; 2.06%); and training materials (US$1,230.50; 0.60%). The total average cost per student was US$3,075.43. Costs were paid by several stakeholders: families, community-based agency, and a nonprofit organization. Program costs were distributed across stakeholders after considering tuition fees and scholarships. The cost of running the SST program was largely covered by families (US$141,600; 64% of costs), followed by the community-based agency (US$75,654; 34.19% of costs), and, finally, the nonprofit organization (US$4,000; 1.80%).
Sensitivity Analysis
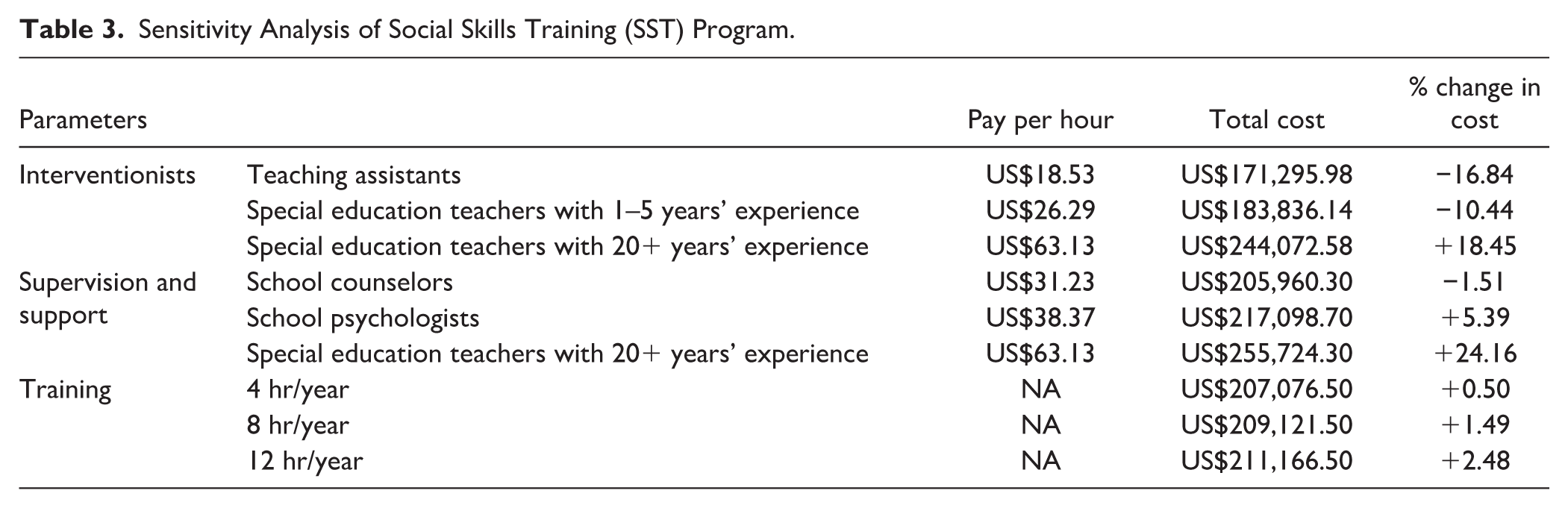
Sensitivity analyses varied three cost drivers and assessed implications for total implementation costs, including interventionist and supervisor credentials, and training hours with all estimates including overhead (see Table 3). SST program cost estimates were sensitive to these cost drivers. First, costs were sensitive to staff credentials and wages, reflecting that personnel costs are the largest share of SST program costs. For interventionists, using teaching assistants represents the greatest decrease in program cost (16.84% decrease), followed by special education teachers with less than 6 years of experience (10.44% decrease), while having special education teachers with more than 20 years of experience was the most expensive (18.45% increase in program costs). For supervision and support staff, utilizing school counselors resulted in negligible program cost savings, while having school psychologists as interventionists increased program costs by 5.39% and having special education teachers with extensive experience (20+ years) represented the greatest increase (24.16%). Finally, increasing training hours only resulted in an increase in program costs between 0.50% (double the training currently provided) and 2.48% (to increase the amount of training by six times).
Sensitivity Analysis of Social Skills Training (SST) Program.
Discussion
Due to the persistent scarcity of resources across child-serving systems, difficult choices must be made about allocation of available resources (Barrett et al., 2020). Cost analyses can provide a data-based framework for comparing multiple EBP options, informing resource allocation, and persuading stakeholders to invest resources in implementation (Barrett et al., 2020). Despite increases in the rate and economic impact of autism and rising demand for EBPs to address autism-related challenges, there are few economic studies of EBPs apart from EIBIs (Cidav et al., 2017). Given social challenges heavily impact autistic individuals’ QoL and future economic prospects, understanding implementation costs of SSTs is crucial to inform adoption, use, and scale-up (Barrett et al., 2020). This study was conducted to address the dearth of cost analyses of SSTs, upon which future economic evaluations, such as CFA and CEA, can be used to further examine feasibility of SST implementation across settings.
To the best of our knowledge, this is the first study of a cost analysis of a community-based, autism-focused SST program in the United States. One school year of the program, delivered to 67 youth, had a total cost of US$206,054.00 with an average cost per child of US$3,075.43. Notably, this amount is substantially lower than other high-intensity autism-focused treatments with low child–staff ratio and more hours-of-service provision per week, such as EIBI programs (e.g., ESDM; US$45,580 per year per child; Cidav et al., 2017). However, program costs of the community-based SST are substantially higher than two other known economic evaluations of SST programs (US$136.78 per child, Wang et al., 2022 and US$69 per child, Smolkowski et al., 2022). Possible reasons for the higher cost include low adult–child ratio, length of intervention (i.e., 40 weeks vs. 12 or 8), more intensive didactic teaching, and the community location (i.e., rental of space and personnel cost).
The major cost driver of the SST program is personnel, with more than 90% of costs driven by personnel hours. The cost of hiring interventionists, interventionist assistants, and the education director contributed to most of the personnel costs, which aligned with other autism-focused EBIs (e.g., PEERS; Laugeson et al., 2014). It is notable that families pay a significant portion of the SST program costs in addition to already grappling with high costs of multiple healthcare, educational, and therapeutic services (Rogge & Janssen, 2019). Although scholarships are available, a large proportion of funds used to run the program are reliant on grant funding. To more systematically and reliably fund/lower costs for SSTs, insurance coverage is needed (Waisman Center, University of Wisconsin-Madison, 2018). Also, while this SST program included 2 hr of training annually, in alignment with other evidence-based SST programs (e.g., PEERS), PEERS does not require specific training because there are detailed instructions in the intervention manual (Wyman & Claro, 2020). In contrast, the community-based SST does not yet have an intervention manual to guide implementation; thus, interventionists may benefit from more intensive training. However, it is notable that the interventionists are masters’ level trained with extensive experience teaching autistic youth.
Sensitivity analysis showed altering interventionist credentials contributed to the greatest variation in costs, followed by supervision and support staff, and amount of training. Using teaching assistants as interventionists provided the greatest decrease in program cost, while special education teachers with 20+ years of experience were most expensive. Similarly, the most experienced special education teachers as managers resulted in the greatest increase in program costs. Finally, increasing the amount of training did not substantially increase program cost. When adjusting program inputs, it is critical to weigh cost considerations and implications of changing ingredients on the quality and fidelity of implementation and subsequent outcomes.
Findings suggest that optimizing personnel-heavy interventions like the SST may be possible through high-quality, intensive training of lower wage personnel by a highly experienced trainer who provides ongoing supervision. When considering the optimal type of interventionist, authors of PEERS suggest extensive experience working with families of autistic children is necessary (e.g., teachers/educators and mental health professionals; Laugeson et al., 2014). Thus, should hiring teaching assistants as interventionists be the lowest cost option, community-based agencies should prioritize applicants with relevant experience. Employing less experienced personnel must be coupled with rigorous staff training, as poor fidelity and inadequate training are crucial factors affecting turnover and quality of intervention delivery (Pellecchia et al., 2015). Sensitivity analysis suggests combining lower wage staff with increased hours of training could reduce program costs while ensuring fidelity. Importantly, the training content must be tailored to teaching assistants’ needs, with emphasis on both the autistic children’s needs, and SST implementation skills.
Finally, ongoing support and supervision is critical for successful implementation of autism-focused EBPs (Dixon et al., 2016). Inadequate support and supervision to lower wage, less experienced staff may result in turnover, an existing challenge in child mental health and community-based disability settings (Sulek et al., 2017). As autistic individuals generally benefit from consistent environments and therapists, high staff turnover would affect continuity and quality of program implementation, potentially jeopardizing client progress (Sulek et al., 2017). Although study of supervision for SSTs is limited, research on ABA program supervision suggests supervisor credentials significantly impact treatment outcomes. Specifically, supervisors with a BCBA had superior outcomes compared with those with bachelor’s or master’s degrees (Dixon et al., 2016). Years of experience a candidate has providing intervention to autistic individuals, as well as their knowledge and skillset in leading SST programs, are critical (Dixon et al., 2016).
Limitations and Future Directions
The results of this study must be interpreted in the context of several limitations. First, this study only examined costs for one unique community-based SST and used local instead of national cost estimates of resources, limiting generalizability to other geographic regions. Replicating costs in subsequent SST implementation studies could enhance generalizability of cost estimates and allow for point and interval estimations. Also, the costs used in this study must be considered in the context in which they were incurred (i.e., 2018–2019). Changes in the broader economic context, such as inflation, will always impact the overall cost of implementation and should be considered when reflecting on generalizability of the current findings. Relatedly, the valuation of indirect costs (i.e., proportion of personnel time spent on SST program vs. other programs; proportion of facility used for SST vs. other programs; administrative costs) was approximated. Adjustments were made for ingredients used for multiple purposes; for example, cost of administrator’s time was estimated by multiplying cost by fraction of time used for the program. It is possible these approximations affected accuracy of the cost analysis. Third, the community-based SST serves a subset of autistic participants without intellectual disability and with limited behavioral problems. Cognitive and behavioral functioning of autistic persons can be variable, however, limiting generalizability to other SST programs serving a wider range of autistic clients. Fourth, this study examined the cost of running one round of the SST for one group of participants. However, some participants re-enroll in the program; thus, ingredient costs may change from year to year depending on number of re-enrolled participants. Finally, use of specific stakeholder perspectives, rather than a social perspective (preferred in public health fields; Barrett et al., 2020), fails to fully consider opportunity cost, and benefits accrued from the intervention, limiting generalizability to other potential stakeholders (e.g., other behavioral health/mental health professionals).
Future directions include conducting further economic evaluations from a societal perspective to understand SST implementation costs in schools through CFA and CEA approaches that consider participant outcomes and fidelity of implementation in the assessment of cost. Social skills training in school settings may be meaningful and generalizable, given the time children spend at school, and that social difficulties can negatively impact peer acceptance, achievement, and mental well-being (Cappadocia & Weiss, 2011). However, autism-related EBPs are rarely successfully implemented in schools, where training, resources, administrative support, and time represent barriers to adoption and fidelity (Locke et al., 2019). Understanding costs to implement an SST program in schools could help districts plan for implementation success.
Given the proliferation of SST programs, this study may encourage economic evaluations of other SST programs, allowing comparison across different SSTs. Furthermore, cost analysis may be extended by conducting fidelity and impact evaluation studies. Regarding program fidelity, an examination of resource use through cost analysis can determine whether an intervention was implemented as designed (Levin et al., 2018). In addition, as researchers, interventionists, and policy makers increasingly seek economic data alongside clinical data to show the value of adopting autism treatments, considerations of potential cost offset into the future should be examined. Future research could explore if participation in SST programs results in significant gains in social and adaptive abilities, and decreased use of other services, leading to cost savings for families. Researchers should also examine economic return on investment over the participants’ lifetime, to see whether SST ameliorates challenges and reduces need for other services.
Implications and Conclusion
This study offers detailed information on the cost of delivering SST that could inform funding, implementation, and scaling-up decisions. Findings can inform future comparative economic evaluations, providing insight into the value of community-based SSTs. Sensitivity analysis also provides valuable information to educators making program adoption decisions and enabling program planning about job descriptions, qualifications, and needed supports for high-quality implementation. Implementation challenges of autism interventions have long been documented (Locke et al., 2019). This study demonstrated a community-based SST can be successfully implemented, where tuition costs were partially subsidized by the agency and an external source. Nevertheless, families bear the biggest cost of intervention. From a public health perspective, further research must determine whether this represents good value through improved functional outcomes over a child’s lifespan. If so, governmental funding and insurance coverage may be considered to ameliorate the high costs of SST for families of children with autism. Finally, EBPs need to be developed and implemented in relation to its acceptance to neurodivergent communities. It is paramount that future development of SSTs is centered around the perspectives and experiences of neurodivergent people.
Footnotes
Author Note
Samantha X. L. Tan completed this research while affiliated with the University of Houston. She is currently an Independent Researcher.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
