Abstract
The US military has reported that embedding physical therapists (PTs) with forward-deployed personnel reduces the impact of nonsevere musculoskeletal (MSK) injuries. This paper describes a pilot program that embedded a PT with outdoor professionals working in Grand Teton National Park (GTNP). The PT spent 3 summer seasons providing onsite care in multiple locations within GTNP. Individuals who received care included search and rescue personnel, trail crew, wildlife biologists, wildland firefighters, and law enforcement officers. The PT performed 111 consultations for a wide range of MSK disorders. The lower extremity was the most frequently treated region (38.7%; n=43). Sixty-seven percent of consultations (n=74) were for symptoms that had a gradual onset with no specific injury. Fifty-six percent of consultations (n=62) were for symptoms of 3 months or more duration. Physical therapy treatments emphasized self-management and included exercise prescriptions, manual therapy, taping, and pain control using transcutaneous electrical nerve stimulation. Based on the preliminary findings from this pilot program, embedding PTs has the potential to increase access to care for nonsevere MSK injuries that occur in outdoor professionals employed in US National Parks. Further study is needed to assess the cost/benefit as well as the short- and long-term impacts of embedding PTs.
Keywords
Introduction
Outdoor professionals in the US National Park Service (NPS) perform many duties, including search and rescue (SAR), emergency medical care, law enforcement, trail maintenance, firefighting, and protection of wildlife.1,2 The ongoing performance of these duties often results in exposure to repetitive and potentially injurious musculoskeletal (MSK) loading associated with long-distance hiking/running while carrying heavy loads, as well as climbing, helicopter activities, and tasks such as frequent bending, lifting, and carrying. 3 The likelihood for MSK injury is potentiated by environmental conditions that may lead to slips or falls in dangerous terrain as well as the adverse physiologic effects of dehydration, fatigue, and reduced motor control associated with exposure to heat, cold, and/or hypoxic conditions at high altitudes.4–11 Considering these factors, it is likely that NPS personnel who work in the backcountry (i.e., wilderness or remote environments) are at risk of sustaining MSK injuries following an isolated injury or overuse. However, there is a paucity of literature that describes the mechanisms and prevalences of these conditions.
One reason for this limited research is that the evaluation and treatment of MSK injuries for backcountry NPS personnel may be complicated by the backcountry locations where many of the injuries occur. These locations potentially can make it difficult and time consuming to seek front-country medical care, especially for nonemergent problems.3,9 Additionally, as with other high-performance teams such as military special operations 12 who work in close knit groups, NPS personnel may tend to underreport injuries when the loss of a team member can affect team readiness. This practice can lead to small injuries worsening and becoming more severe.
A potential way to mitigate the impact of nonserious MSK problems is to provide onsite physical therapy consultation and treatment by embedding specially trained physical therapists (PTs) within backcountry environments.13–16 The value of embedding PTs has been demonstrated by the US military, where specialty-trained US Army and Navy PTs act as onsite point-of-contact care providers for MSK injuries that occur in forward-deployed special operations personnel such as US Army Special Forces, Navy SEALs, and US Army Rangers.17–22 There is evidence that these embedded military PTs provide rapid, mobile onsite evaluation and field management of nonserious MSK injuries, resulting in fewer evacuations, reduced use of advanced medical care, and improved mission efficiency.18,20,22 It is unknown, however, whether these findings also would occur if PTs were embedded with NPS personnel.
This concept report describes a pilot program in which a PT was embedded in a variety of locations in Grand Teton National Park (GTNP) to provide onsite care for NPS personnel and provides information regarding the anatomic locations, symptom duration, and mechanisms of onset of clinical conditions for which backcountry personnel sought physical therapy care.
Program Description
Development
The idea for the pilot program was developed by the authors working in conjunction with key personnel at GTNP. Author DJ had extensive prior experience as a SAR ranger at GTNP and identified a potential need for forward-based physical therapy services. Author DH had substantive experience in forward-based physical therapy services during several combat deployments with US Army Special Forces and proposed adaptation of the military model for personnel at GTNP. All 4 authors developed the fundamental structure of the proposed pilot program and met with GTNP officials and backcountry personnel to assess their specific needs in terms of physical therapy care for nonserious MSK problems. A key issue was that backcountry personnel who sought physical therapy needed to travel from remote areas in the park and then drive 25+ mi in a high-traffic area to the nearest physical therapy clinics in Jackson, WY. Considering the time commitment, a physical therapy visit could take several hours out of workdays. To address this concern, the authors proposed a pilot program based on the military model to embed a mobile PT in GTNP who would be able to evaluate and treat patients in and near their work environment. Officials at GTNP reviewed and supported this program.
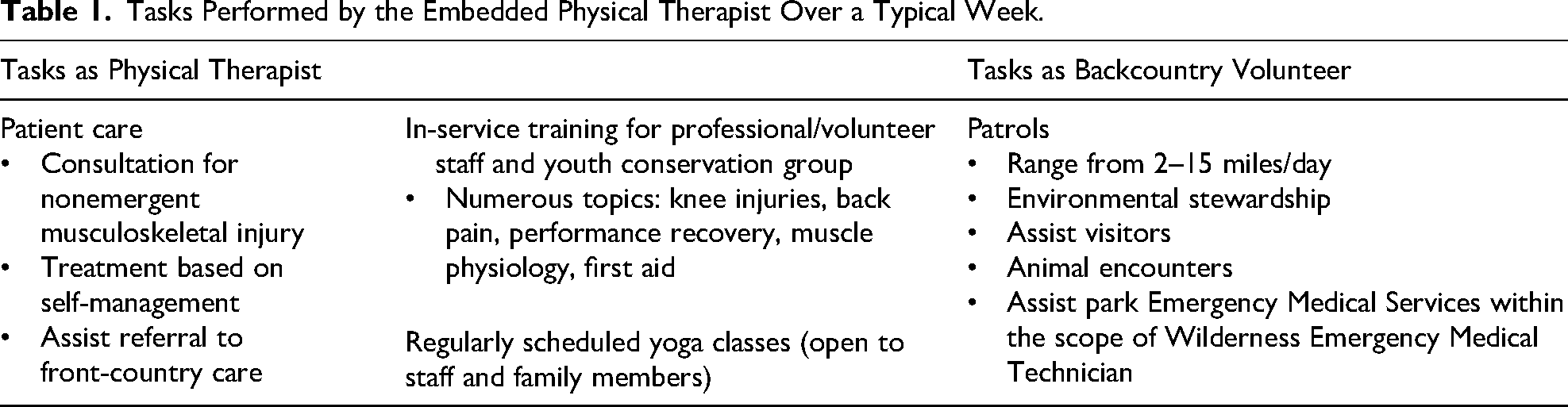
The embedded PT (author PFB) was classified as a volunteer backcountry ranger and provided pro bono direct-access/point-of-care consultation and treatment. The embedded PT had extensive clinical experience, including advanced training and specialty certification in orthopedic PT, and was a nationally registered emergency medical technician with wilderness certification (ie, Wilderness Emergency Medical Technician). He was licensed to practice physical therapy in the state of Wyoming, where GTNP is located. When not providing patient care, the embedded PT performed the duties commensurate with a volunteer backcountry ranger, including patrols, assisting with Emergency Medical Services as a Wilderness Emergency Medical Technician, ensuring backcountry safety, and assisting with environmental stewardship (Table 1).
Tasks Performed by the Embedded Physical Therapist Over a Typical Week.
At the inception of the pilot program, the embedded PT met with and provided in-service training for several departments in GTNP to discuss the purpose and scope of the pilot program. The departments included SAR rangers, trail crew, law enforcement, wildlife biology, wildland fire, backcountry volunteers, and dispatch. Examples of the unique job demands for the different departments are listed in Table 2.
A List of Key Physical Demands for Individuals Who Work in Different Backcountry Departments Within Grand Teton National Park.

PT consultation was offered to individuals who were professional or volunteer NPS personnel who participated in backcountry activities without medical restriction and who did not have a current or previous Workers’ Compensation claim for the conditions for which they were seeking care. Potential participants were informed that de-identified patient data obtained by retrospective chart review would be submitted for publication unless they did not desire this. Individuals who did not wish to have their de-identified information submitted for publication were still eligible to receive PT consultation and care.
Backcountry NPS personnel who sought consultation communicated with the PT by phone, email, or text message, and a time and location were agreed upon. PT consultation was provided in several environments. These environments included a cargo bay with vehicle access near headquarters that also functioned as a winter rescue operations center and provided a sheltered area to see patients. Other consultations occurred at hike-in or boat-in work sites in the backcountry or in a forward rescue area.
Patient Evaluation
A standardized intake form was used to obtain demographic information as well as to document the chief complaint, mechanism of onset, chronicity, and spatial distribution of symptoms. The PT obtained a detailed history and performed a physical examination, including observation, motion assessment, neurologic testing, the administration of special tests, and palpation. Participants who had signs or symptoms that were outside the scope of practice for PT treatment were not treated and were encouraged to contact their primary care provider for further evaluation as indicated.
Physical Therapy Treatment Approaches
Physical therapy treatment was structured around instructing participants in self-management through exercise and ergonomic advice. Following consultation, patient education was provided to assist the patient's understanding of the mechanical basis for their MSK problem and its likely severity. When possible, online sites were accessed to provide visual learning opportunities and references for further patient education. This information was used to develop ergonomic strategies for symptom reduction and prevention that targeted the participant's unique job demands. Patient education also included the potential for emergence of “red flag” signs or symptoms that may occur in the future that could indicate a more serious problem.
Participants were instructed in a variety of self-administered tissue-specific treatments as indicated. These treatments included stretching, strengthening, joint mobilization, and the use of taping. Individuals with high pain intensity levels were issued a transcutaneous electrical nerve stimulator unit and instructed in its use. Participant follow-up was done by phone, text message, or with an in-person visit.
Categorization of Patient Consultations
All data were obtained from a retrospective chart review and were de-identified prior to analysis. Frequency counts were obtained for the number of consultations and for individual patient variables, including department, age, sex, region of symptoms (eg, neck/thoracic spine, low back/posterior buttock, upper extremity, and lower extremity), symptom acuity (eg, acute, 0 to <6 wk; subacute, 6 wk to <3 mo; and chronic, ≥3 mo), and mechanism of onset (eg, gradual with no specific injury or sudden onset of symptoms following a specific injury).
An independent t test was used to determine the differences in participant age by sex, and a one-way analysis of variance with a Scheffe post hoc analysis was used to determine differences in participant age by each of the categorical variables with 3 or more levels. Alpha was set at P<0.01. Cross-tabulation was used to create contingency tables to visually compare the frequencies of different categorical variables. Pearson χ2 analysis was calculated, and cells in which the observed value exceeded the expected value were identified for those comparisons with P<0.05. All analyses were performed using IBM SPSS, version 29 (IBM Corp, Armonk, NY).
Results
Participants
Over parts of 3 summers (2022–24), 70 different NPS personnel sought consultation from the embedded PT. Twenty-seven of these individuals had 1 or more additional consultations for other problems for a total of 111 consultations. Two participants reported previously diagnosed comorbidities (ie, inflammatory spondylopathy and Raynaud's syndrome). Sixteen participants had a history of 1 or more surgeries for orthopedic conditions including total knee or hip replacement, glenoid labral repair, anterior cruciate ligament reconstruction, knee meniscal excision, open reduction and internal fixation for fractures, lumbar microdiscectomy, thoracolumbar fusion, and Achilles tendon repair. No one presented with signs or symptoms that suggested serious conditions such as radiculopathy, bone stress injuries, recurrent compartment syndrome, or rhabdomyolysis. Two participants were encouraged to seek front-country care (1 for acute shoulder and chest wall pain following a fall and 1 for signs and symptoms suggestive of thrombophlebitis). No adverse events related to any PT treatment were reported, and no participants required evacuation.
The highest number of consultations was performed for members of the SAR rangers (n=35), followed by the trail crew (n=28) and law enforcement (n=20). Sixty-three (56.7%) of the consultations were for males. The mean age of males was 42.2 (14.9) y and was greater than the mean age of females (33.2 [10.9] y; P<0.01). The mean age for those with acute symptoms was 45.5 (15.7) y) and was greater than that of those with subacute symptoms (33.9 [12.3] y) or chronic symptoms (36.0 [12.4] y; p<0.01). The mean age of backcountry volunteers was 69.5 (5.7) y and was greater than that for all other departments (P<0.01). The mean age of SAR rangers was 40.7 (9.1) y and was greater than that for the trail crew (26.7 [5.7] y; P<0.01). There were no other age-related differences.
Region of Chief Complaint Symptoms
The lower extremity was the most frequent region for which individuals requested consultation (n=43), followed by upper extremity (n=31), low back/posterior buttock (n=25), and neck/thoracic spine (n=12). When assessing the frequency of chief complaint symptoms by department, 46% of the consultations (n=16) for SAR rangers were for lower extremity problems, 40% of law enforcement consultations (n=8) were for low back/posterior buttock pain, and 39% of trail crew consultations (n=11) were for upper extremity problems (Table 3). There was no significant difference in the frequency counts of location of chief complaints by departments.
Incidence of Region of Chief Complaint Symptoms for Participants From Different Departments Within Grand Teton National Park.

Symptom Acuity
A total of 55.9% of consultations (n=62) were for conditions that were described as chronic (≥3 mo), 27.9% (n=31) were for conditions described as acute, and the remaining 16.2% (n=18) were for conditions described as subacute
Mechanism of Onset of Chief Complaint Symptoms
The mechanism of onset of 67% of symptoms for consultation (n=74) was reported to be gradual with no specific injury, whereas the remaining 33% of symptoms (n=37) were reported as of sudden onset following a specific injury. Neck/thoracic spine problems were more likely to be associated with gradual onset with no specific injury, whereas lower extremity problems were more likely to be reported as of acute onset following injury (P=0.04; Table 4). There were no associations between the mechanism of onset and symptom acuity or department.
Comparison of the Incidence of Regions of Chief Complaint Symptoms by the Mechanisms of Onset of Symptoms.
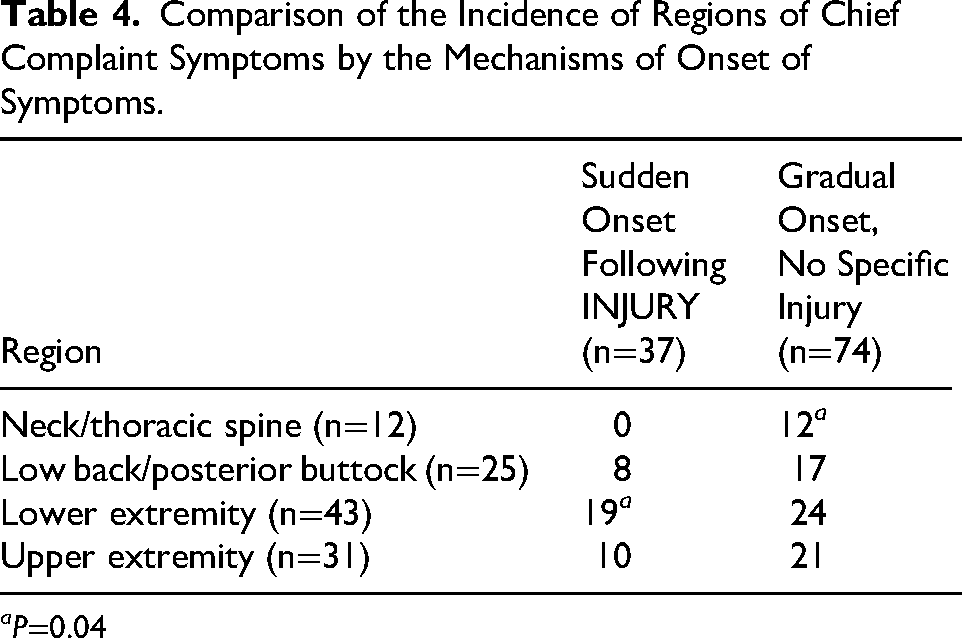
aP=0.04
Discussion
The intent of this pilot program was to investigate whether the military model of embedding PTs would have potential for increasing access to care for NPS personnel who often work in remote areas. Over 3 consecutive summer seasons, the embedded PT was able to travel by vehicle, hiking trail, and/or boat to numerous locations within the park to provide care while “working out of a rucksack” (Figure 1).

Equipment and Supplies Carried in a Backpack by the Physical Therapist to Provide Consultation and Treatment in the Backcountry Environment.
NPS personnel sought consultation for a wide range of nonemergent MSK conditions. Not surprisingly, considering job-related loading demands, chief complaints in the lower extremity were most prevalent, followed by the upper extremity. Most of the problems had been present for >3 mo. Interestingly, two thirds of the conditions for which people sought consultation were reported to be of gradual onset without specific injury, suggesting that a high number of these conditions resulted from repetitive strain and overuse. This high number becomes important because commonly seen conditions associated with repetitive strain and overuse such as chronic back pain, tendinopathy, and plantar fasciitis can be potentiated by modifiable intrinsic factors, such as isolated muscle shortening and weakness, combined with ergonomic issues. These conditions are often ignored in the early stages until further, more serious injuries occur. One advantage of having an embedded PT is the provision of early onsite consultation, and initiation of intervention and ergonomic advice potentially may manage these conditions by exercise and ergonomic adjustments before more serious injuries occur.
An interesting question relates to the prevalence and mechanism of chief complaint symptoms that may be associated with specific task exposures encountered by people in different departments in the park (Table 2). For example, a nonsignificant trend was observed in which SAR rangers had a high frequency of recurrent lower extremity injuries. This high frequency could be consistent with their demands for running, hiking, technical climbing, and helicopter insertions in dangerous, irregular terrain where slips and falls, as well as lower extremity overuse injuries, are common. Individuals involved in law enforcement had high frequencies of persistent low back/posterior buttock pain that may be associated with prolonged sitting in service vehicles while wearing duty belts and heavy protective gear as well as the demand for episodic lifting and carrying. Members of the trail crew had high frequencies of recurrent arm/forearm soft tissue injury and wrist or hand problems, which are consistent with their repetitive use of hand tools. Understanding the prevalence of these clinical conditions between different departments can be of great value to embedded PTs. This information would be helpful to develop individually tailored off-season conditioning programs that can be monitored in person or remotely. Interestingly, some unique injuries included a strain of the flexor carpi radialis muscle associated with the position of a chainsaw grip forcing the wrist into prolonged flexion with radial deviation and a fractured fifth metacarpal sustained while evading a grizzly bear.
An additional potential, but not yet proven, benefit of embedding PTs is that the therapist works in the same environment as the patient population. This proximity enhances the PT's knowledge regarding the specific complexities of the job and leads to comradery with the shared goal to “keep people on the trail.” By practicing in this environment, the embedded PT can act as a community-based care provider with emphasis on the self-management approach. This emphasis has the potential to empower individuals seeking care through knowledge of the problem, its likely cause, anatomic correlates, likely trajectory of symptoms, and potential for red flags.23,24
It is important to note that, like all backcountry care providers, embedded PTs require many core skills to be safe and contributing members of remote and wilderness teams. These skills include first aid training at the level of Wilderness First Responder or higher, wilderness survival skills, proficiency in land navigation, knowledge of backcountry ethics, and an understanding of animal precautions and radio communication.13,16,25–27
Table 2 describes additional activities that were part of the embedded PT's normal week. In addition to direct patient care, authors PFB and KB participated in wellness programs that included the provision of in-services to a wide array of park personnel, including youth groups and volunteers, as well as conducting yoga classes on a regular basis. When on backcountry patrol as a volunteer backcountry ranger, the embedded PT provided first aid care to visitors within the scope of practice for a Wilderness EMT.
Limitations
The data described in this paper were obtained by retrospective chart review and may be subjected to selection bias and recall bias. It is important to note that some of the reported injuries were not job related and may have occurred during physical conditioning activities or recreational sports. The relatively small sample sizes for many of the frequencies of the categorical variables may result in some of the statistical comparisons being underpowered.
This pilot program provided pro bono care, and therefore, no conclusions may be made regarding cost savings of care associated with embedding PTs. No functional outcome measures were obtained, and the emphasis was on consultation and self-management with follow-up on a patient-requested basis, so no quantitative determination can be made regarding effectiveness of the treatments. These data only reflect findings from summer seasons at GTNP and cannot be generalized to other populations or times of the year.
Future Directions
Future studies using prospective designs to assess cost and benefit would be of great value to determine whether embedding PTs can make meaningful differences in the health and physical performance of backcountry personnel. Given the unique and nontraditional nature of the embedded PT program, this research would be inherently complex but feasible. 28 For example, the analysis needs to compare traditional front-country PT care for nonserious MSK problems with care provided by embedded PTs. This would require sampling from several parks to allow an adequate sample size for meaningful statistical power as well improving the generalizability of the findings. Inherent variations in injury threats between different park environments also would need to be considered. For example, backcountry personnel in GTNP may face different threats than those who work at the Grand Canyon. Personnel in larger, more remote parks with lengthy travel times to a front-country PT clinic would benefit more than those in parks that are closer to populated areas. The data analysis addressing the benefits or effectiveness of care would include a comparison of direct costs for care but also should include other traditional measures such as functional recovery, lost work time, patient satisfaction with care, and recurrence of symptoms. Because the embedded backcountry PTs have an emphasis on primary prevention through instruction in physical conditioning and ergonomics, the impact of embedded PTs on the incidence of new injuries would be of great interest.
Interestingly, it is possible that many intangible effects will be associated with the embedded program. Backcountry personnel would have streamlined access to the embedded PT and early initiation of care or front-country referral. In addition, embedded PTs would benefit the overall mission of the park staff through their participation in backcountry patrols and assistance with emergency medical services.
Moving forward, there are also other promising but uninvestigated potential venues for embedding PTs in the remote and wilderness environments. Conceptually, a major advantage of embedding PTs is to provide onsite care that may reduce or prevent the need for an individual to leave the remote and wilderness area to receive care. This can be important for time-sensitive backcountry tasks such as wildland firefighting, where the loss of individuals on scene can be problematic.29,30 The role of PTs on the wildfire line is being investigated by author DH, who is currently providing PT services in remote areas during wildland firefighting.
Another potential area in which embedded PTs may be of value is during disaster response. In addition to providing care to rescue workers, PTs have core skills in gait training and ambulation that can be of great value in the evacuation of impaired individuals from dangerous areas in disaster locations. PTs in the US Public Health Service are being trained for these activities. 31 PTs are also becoming involved as providers in ultra races, rock climbing, and backcountry expeditions within the community of adaptive athletes.
Another potential area for study includes investigating concepts of performance recovery for outdoor professionals who engage in prolonged physical and psychologically challenging activities32,33 This intervention is currently being used by military special operations personnel and is being piloted in the civilian population.
Conclusions
Based on the preliminary findings from this pilot program, embedding PTs has the potential to be a useful way of expanding access to care for nonsevere MSK injuries that occur in outdoor professionals employed in US national parks. Lower extremity problems were the most common reasons for seeking care. Two thirds of the injuries had a gradual onset, suggesting a high prevalence of repetitive trauma/overuse injuries. Further study is needed to assess the cost benefit as well as the short- and long-term impacts of embedding PTs.
Footnotes
Acknowledgments
The authors are grateful for the invaluable assistance of Scott Guenther, Chris Belino, Nick Armitage, Forrest Young, Jon Politis, and Steven McDavitt on this project.
Author Contribution(s)
Ethical Considerations
This is a retrospective data analysis with all personal patient information de-identified. All interventions were adherent to current evidence-based clinical guidelines.
Consent to Participate and for Publication
This study was reviewed by authorities from the US National Park Service at Grand Teton National Park, Moose, WY 83012, who have granted permission for publication of these data. Individuals did not sign a document of informed consent, but all data from this retrospective chart review have been de-identified.
Data Availability
Deidentified data will be available to those who wish to review the entire dataset.
Financial/Material Support
None. All patient care was provided pro bono by a volunteer physical therapist.
