Abstract
A 19-year-old male presented with facial frostbite and severe oropharyngeal edema after prolonged riding of a snowmobile without any facial covering. The diffuse swelling eventually progressed to airway obstruction, requiring a surgical airway. No alternative explanation was found for his presentation, making this the first case found in the literature of airway obstruction secondary to environmental cold exposure.
Introduction
We present a case of severe oropharyngeal edema leading to airway obstruction secondary to environmental cold exposure. While the pathophysiologic effects of cold exposure on the lower airways have been previously described, we believe this is the first case report of environmental cold exposure leading to complete upper airway obstruction. 1–3 Although treatment options for airway edema are similar regardless of the cause of the injury, we hope to increase awareness of this rapidly life-threatening outcome of environmental cold exposure.
Case Report
In April 2022, a previously healthy 19-year-old male presented to a nursing station in Nunavut, Canada, with significant facial swelling. The day prior, he had been riding his snowmobile for approximately 8 h without any face covering, with an ambient temperature of −21 °C. Although his speed was unknown, at this temperature, snowmobile speeds of 40 km/h and 80 km/h would produce a windchill equivalent of approximately −34 °C and −38 °C, respectively. 4 He noticed worsening facial swelling and pain overnight, prompting him to seek medical attention. Initially, he was transported to a local health center due to concerns about facial frostbite. There was increasing concern for airway compromise as he was having difficulty managing his secretions. An episode of mild hypoxia with oxygen saturations in the low 90's was noted, and this improved with supplemental oxygen. Prior to transport to tertiary care, the patient was given ceftriaxone and metronidazole, dexamethasone, and a tetanus booster.
He arrived at the tertiary care referral center in Manitoba just over 24 h from his initial health care contact. He displayed evidence of facial tissue damage consistent with frostbite, including fluid-filled bullae to the lips and chin and erythema of the cheeks, and was noted to have profound edema to his face, lips, and oral mucosa (Figure 1). He was unable to open his eyes. The oropharyngeal swelling was so severe that he was unable to swallow or manage his secretions. He could not form words and was noted to have positional stridor. Given the concern for airway compromise, anesthesia, otolaryngology, and plastic surgery were urgently consulted. An awake fiberoptic scope was performed in the ED that showed significant upper airway and epiglottic swelling (Figure 2), and the decision was made to proceed with an awake intubation in the operating room.
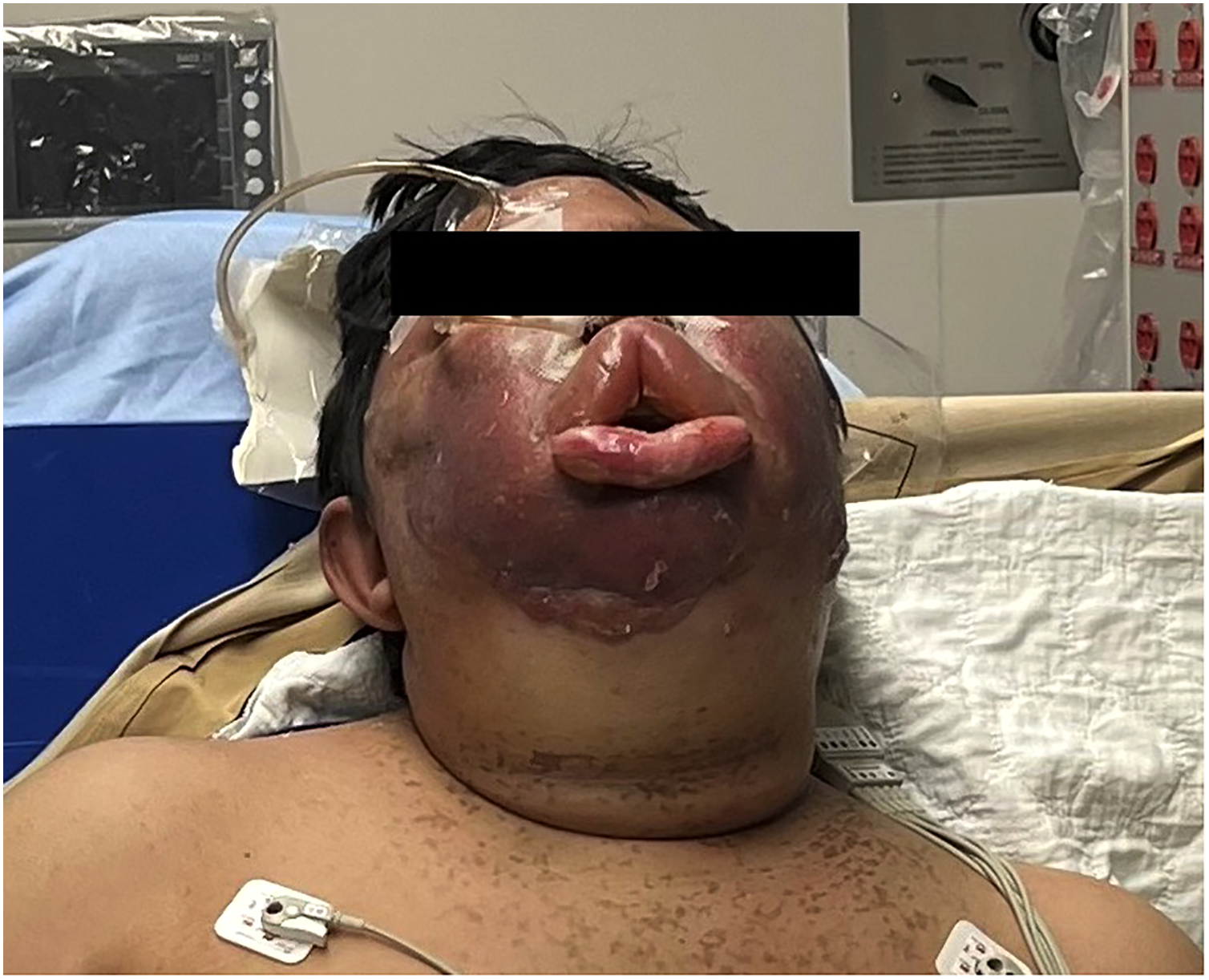
Facial swelling upon arrival to the tertiary care hospital.
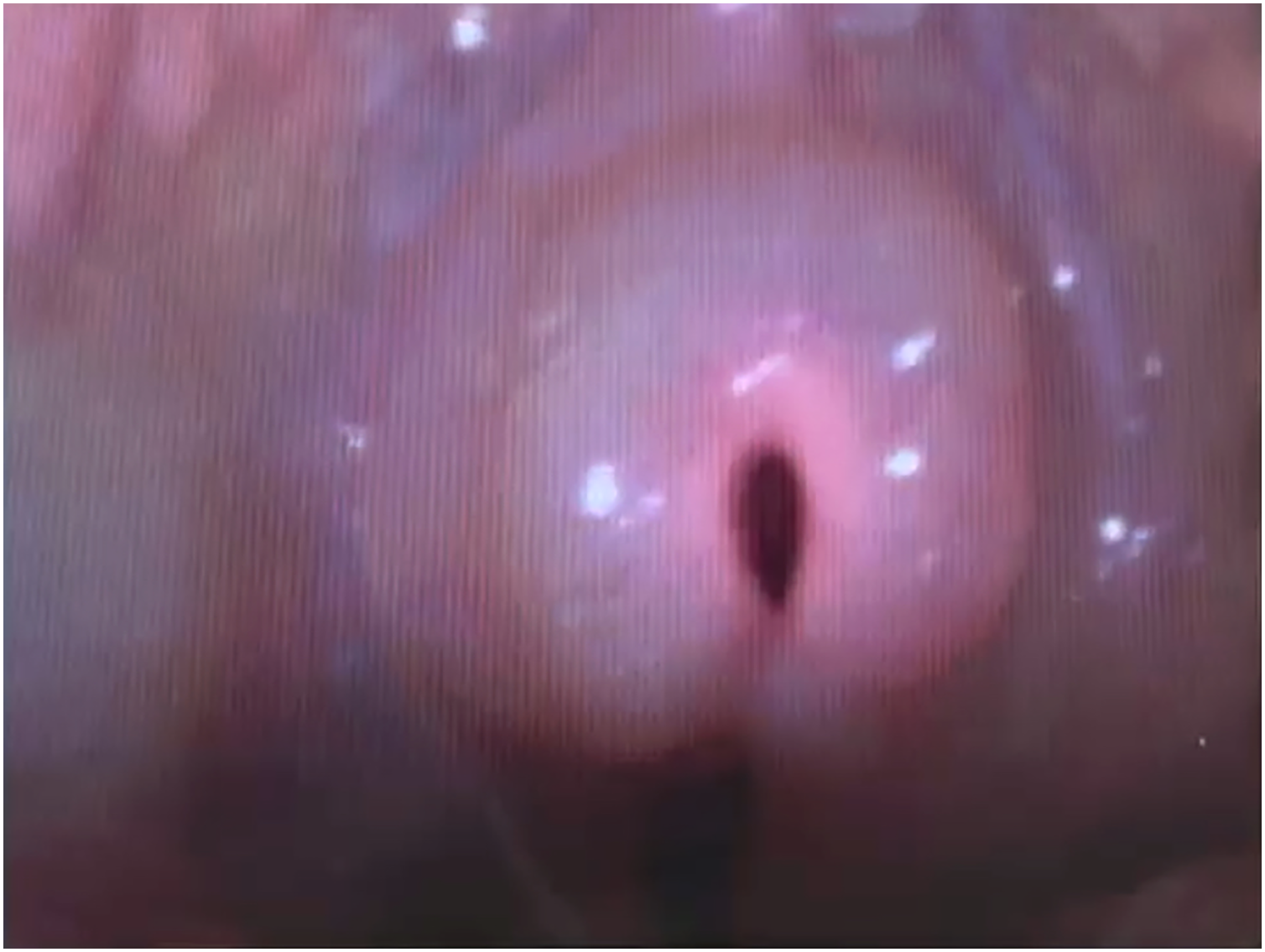
Upper airway swelling seen on flexible fibreoptic scope.
The patient was taken to the operating room approximately one hour after his arrival at the tertiary care hospital. Anesthesia made multiple attempts at fiberoptic orotracheal and nasotracheal awake intubation but was unsuccessful due to significant supraglottic edema and anatomical changes. During these attempts, his airway became completely obstructed, and an emergent tracheostomy was performed to provide airway access. He briefly lost a pulse during the procedure, and after a single round of CPR, epinephrine, and successful ventilation via tracheostomy, a return of spontaneous circulation was achieved.
The patient had a fairly unremarkable course in the hospital afterward. Bedside debridement and wound care were performed for his facial wounds. A CT of his head and neck was performed and showed diffuse soft tissue swelling throughout the face and neck without any deep space fluid collection. This was felt to be nonspecific; extensive changes from frostbite could result in this appearance, and the differential would include a diffuse infectious or inflammatory process or anasarca. As such, alternative explanations for his presentation were investigated.
Allergy and immunology specialists were consulted; the patient had normal C1 esterase inhibitor, C4, and serum tryptase levels, and it was felt that his presentation was not related to allergy or sensitivity. Alternative causes of cold-induced airway injury, such as toxicologic inhalations, were not identified once further history was provided. It was hospital policy that he be investigated for COVID-19, given the patient's airway manipulation, and he was found to be COVID-19 positive on rapid PCR (polymerase chain reaction) test, although he had none of the classic signs or symptoms of active COVID-19 infection.
The patient made a complete recovery in the hospital. His tracheostomy was decannulated, and he was discharged home in stable condition after making a full recovery.
Discussion
Existing literature on environmental causes of significant upper airway edema approaches nonexistent. The effects of environmental cold exposure on the lower airways have been well described, including cold-induced asthma, bronchoconstriction, and pulmonary edema.1,2 These effects are more pronounced during high-output activities during which airway temperatures are decreased due to increased minute ventilation and incomplete air conditioning by the nasal and oral mucosa.3,5 An explanation for why our patient instead had such a dramatic presentation of upper airway swelling was not readily evident. One possible explanation was his extended use of a snowmobile; the high speed and lack of protective barrier covering his lower face may have increased the penetration of cold air into his oral cavity and upper airway. Theoretically, this may have allowed for prolonged cold air penetration to these typically more protected upper airway tissues, leading to damage and edema.
The most common examples of cold-induced oropharyngeal and upper airway edema are found in toxicologic literature, typically related to recreational or unintentional inhalation of gases at extremely low temperatures. As with our patient, these cases describe significant mucosal and oropharyngeal edema secondary to cold injury, and in severe cases, include tissue necrosis and frostbite.6,7
Consideration was given to the possibility that he had facial frostbite with a concurrent infectious etiology (such as Ludwig's angina) as an explanation for his oropharyngeal and airway swelling. This was felt to be unlikely, as the patient was missing many of the classic history and physical exam findings of a deep neck space infection, and his lack of fever and unremarkable WBC rise did not support this diagnosis. 8 He also had a CT scan that did not show any evidence of deep space abscess.
Although a serum tryptase level was normal, it was drawn more than 24 h from symptom onset and therefore was not definitive for ruling out anaphylaxis. 9 However, the patient was lacking other clinical evidence of an anaphylactic reaction and had no identifiable allergic triggers on history, making anaphylaxis unlikely. The patient had normal C1 esterase inhibitor and C4 complement levels, and after reviewing his medications, it was felt that his presentation was not related to hereditary or drug-induced angioedema. 10
Although the patient was found to be COVID-19 positive on rapid PCR, he did not endorse any symptoms prior to his presentation. It is possible that the pro-inflammatory state of an active COVID-19 infection contributed to his impressive condition. 11 Unfortunately, there was no viral load result available, and given the patient's lack of symptoms, we cannot be sure that his result represented an active COVID-19 infection. 12
Conclusions
We have shown a case of oropharyngeal and upper airway swelling secondary to environmental cold exposure, causing airway obstruction in a young adult. This represents an extreme case of cold-induced upper airway injury, which is more commonly seen in toxicologic literature from inhalational sources. However, the patient's history was consistent with environmental exposure, and no convincing alternative explanation was found on the workup. This would, therefore, represent the first case we are aware of in the literature of an environmental cause of cold-induced airway obstruction. Given the life-threatening nature of his injuries, this is an important case of which clinicians should be aware.
Regardless of the cause of oropharyngeal edema, the primary goals of management remain the same. Frequent airway assessments and early intubation for airway protection are paramount. Concerns over progressive signs of airway obstruction should trigger specialist involvement. As in this case, early treatment for infectious etiology, such as Ludwig’s angina with broad-spectrum antibiotics, is reasonable, as well as systemic steroids to help reduce airway swelling. Consideration should be given to alternative causes of angioedema, such as anaphylaxis and hereditary angioedema.
Footnotes
Author Contribution(s)
Conception of case report (SC, JB, SL). The patient was contacted for consent by SC. Data collection and literature review performed by SC. Draft manuscript preparation (SC). Manuscript editing (JB, SL). Approval of final manuscript (all authors).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Patient Consent Notes
Written consent from the patient was provided before the time of writing. He has consented to the use of photos and videos of his presentation for the purposes of education related to this case report.
