Abstract
Innovations are critical for improving clinical practice and nursing education, and for enhancing learning and practice change for frontline nurses and nursing students. Continuous innovation for delivering safe care and improving patient outcomes is needed. Merely demonstrating the effectiveness of research innovations is not enough to promote their uptake and use in practice. A 2021 study in cancer research reported that moving research into practice takes about 15 years. Implementation science, a systemic process of identifying the most relevant approaches to move research into practice, has emerged as an effective way to bridge the research-practice gap. The purpose of this article is to discuss why and how Implementation Science is necessary to promote the uptake of innovations in clinical and educational practice.
Keywords
Implications for Knowledge Translation
Bridging the knowledge-to-practice gap is critical in nursing practice. Traditional methods to effect the uptake of innovations and bring change are not effective. Use Implementation Science methods to develop strategies for increasing and hastening the update of innovations.
In health care, innovation can be conceptualized as “invention + adoption + diffusion. It may be a novel idea, product, service, or care pathway that has clear benefits when compared to what is currently done” (Kelly & Young, 2017, p. 121). In this article, innovation is defined more specifically as “programs, practices, principles, procedures, products, pills, and policies” (the 7Ps) (Brown et al., 2017, p. 3) which could improve health care and patient outcomes. Nurses regularly generate innovations to address existing and emerging clinical problems in order to deliver safe care, improve patient outcomes, and enhance the quality of care (Asurakkody & Shin, 2018; Salmond & Echevarria, 2017). In an educational context, educators use innovations to optimize educational curricula and content to enhance student and nurse learning in clinical and classroom settings (Halstead, 2020). The nature of innovations in education is different from innovations in clinical settings because it entails new teaching and learning approaches and methods to enhance learning and build competencies. In either setting, the uptake of innovations is critical in improving nursing practice and advancing nursing education (Kaya et al., 2015).
Innovations are generally tested for their effectiveness and evaluated for bringing change and optimizing outcomes through interventional research. However, merely demonstrating the effectiveness of innovations is not enough to promote their adoption and use for practice change (Bauer & Kirchner, 2020). Morris et al. (2011) reported that it takes about 17 years to move research innovations into practice. Khan et al. (2021) estimated a gap of 15 years for the translation of evidence-based practice in cancer control. It is a commonly held assumption that if an innovation or intervention is deemed effective in interventional research and its findings are published in peer-reviewed journals, the relevant target audience and stakeholders will incorporate the innovation into their practice (Bauer & Kirchner, 2020). However, research has demonstrated that this passive process of uptake of innovations is ineffective and may only work under certain conditions (i.e., settings with sufficient resources, moderate or high level of expertise and motivation of stakeholders, and presence of self-identified champions) (Vedel et al., 2018). Therefore, active approaches and methods are needed to enhance the uptake of innovations and evidence-based interventions in practice (Bauer & Kirchner, 2020; Curtis et al., 2017).
In nursing, a large amount of evidence-based knowledge is generated, but only a small percentage of this knowledge is translated into practice (Zullig et al., 2020). Implementation science (IS), a systemic process of identifying the most relevant approaches to move research into practice, has emerged as an effective way to reduce this research-practice gap (Nilsen & Birken, 2020). Implementation practice is the use of strategies to facilitate clinician and stakeholder uptake and utilization of innovation in routine practice (Metz, 2019). This article discusses why and how IS is necessary to promote the uptake of innovation in clinical and educational practice.
Why Implementation Science?
IS offers a range of theoretical and methodological approaches and tools to expedite the uptake of research innovations in practice (Bauer & Kirchner, 2020; Rapport et al., 2018). Research conducted through the effective use of implementation tools, theories, methods, and approaches enables researchers and practitioners to actively engage with the context within which innovations are introduced (Bauer & Kirchner, 2020), and to involve multiple stakeholders who may benefit from the uptake of innovations (Straus & Tetroe, 2013). Utilizing IS allows for understanding contextual factors, barriers, and facilitators at multiple levels (i.e., individual, organizational, and system) which may impede or facilitate the uptake of innovations in practice. IS methodologies enable the mitigation of challenges to the use and uptake of innovations (Nilsen, 2015). When barriers and facilitators to the introduction and uptake of innovations are known, the impact of innovative, evidence-based interventions can be optimized (Brown et al., 2021) to change clinical and educational practices.
How Does Implementation Science Enhance the Uptake of Innovations?
The IS process entails several key aspects that are often illustrated in various models—for example, the Knowledge-to-Action Cycle (Graham et al., 2006) and the Quality Improvement Framework (Meyers et al., 2012), which describe and inform the process of translating evidence and research into practice (Nilsen, 2015). To conduct research guided by implementation theories, frameworks, and models for optimizing the uptake of innovations, researchers, practitioners, and other stakeholders should consider the steps illustrated in Figure 1. These steps are a basic outline and do not offer a one-size-fits-all approach; researchers can tailor the steps as needed.
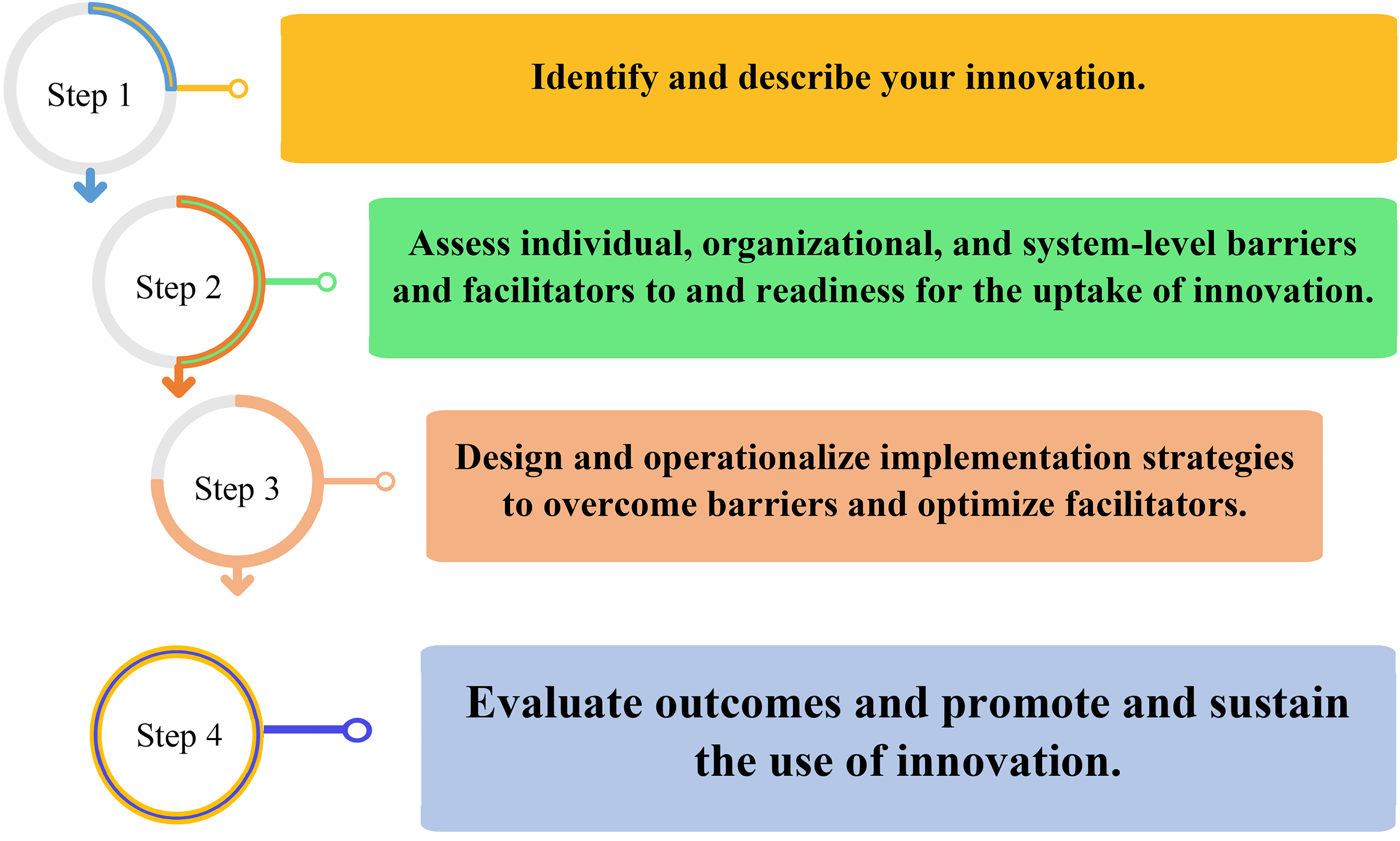
Steps in the Use of Implementation Science for Uptake of Innovations
At each of these steps, various theories, frameworks, models, and methods can inform the effective execution of the step to optimize the intended purpose. For example, the Theoretical Domains Framework (Cane et al., 2012) and the Consolidated Framework for Implementation Research (Damschroder et al., 2009) can be used for the assessment of barriers and facilitators. The Expert Recommendations for Implementing Change (ERIC) strategies (Powell et al., 2015) can be used to design relevant implementation strategies to address barriers. The action, actor, context, target, time (AACTT) framework (Presseau et al., 2019) can be used to operationalize implementation strategies. The Reach, Effectiveness, Adoption, Implementation, and Maintenance (RE-AIM) framework (Glasgow et al., 2019) can be used for assessing relevant outcomes to determine the effectiveness of implementation. Individuals’ and organizations’ readiness can be assessed using theories of readiness such as organizational readiness for change (Weiner, 2009), using surveys (Alsadi et al., 2022).
What is the Evidence for the Effectiveness of Implementation Science?
Several systematic and narrative reviews (e.g., Cassidy et al., 2021; Goorts et al., 2021; Kilbourne et al., 2020) demonstrated the usefulness of IS for the uptake of evidence-based interventions in bringing about change in clinical practice. Kilbourne and colleagues illustrated how using IS led to enhancing chronic disease management, improving the delivery of primary care mental health services for depression, HIV prevention, patient safety initiatives, and diabetes prevention programs. They noted that five shared elements in these successful programs were (a) development and use of a shared agenda among researchers and multiple stakeholders; (b) utilization of IS theories, frameworks, and models; (c) evaluation of implementation efforts, programs, and initiatives; (d) empowerment of implementers to increase the sustainability of implementation; and (e) guided adaptations of interventions to increase uptake from the evidence and knowledge users (Kilbourne et al., 2020). Cassidy et al. (2021) reviewed 41 studies about clinical practice guidelines in nursing to ascertain the use and impact of implementation strategies (e.g., audit and feedback, educational meetings, facilitation, and local opinion leaders) for the uptake of guidelines. They reported that multicomponent implementation strategies had a positive impact on nursing practice outcomes (e.g., professional knowledge, skills, and practice), knowledge outcomes, patient health outcomes (e.g., patient health status and satisfaction), and resource use. These examples demonstrate the effectiveness of IS in enhancing the uptake of innovations in practice; there are numerous other discipline-specific examples published in the literature.
Implications for Nursing
Nurse researchers and clinicians must take an active role in integrating IS into the design, implementation, and uptake of nursing-specific innovations (e.g., clinical practices and patient-centered interventions). Merely designing, delivering, and evaluating innovative nursing interventions in clinical practice, without incorporating the principles and methodologies of IS, may not result in sustainable disruptive changes in practice. Nurse researchers and clinicians must work together with relevant stakeholders to design, implement, and evaluate innovations to bring meaningful change. Nurses in clinical settings should learn about and apply IS tools and methods to actively participate in implementation and help optimize the uptake of the innovations resulting from researchers’ efforts (Reynolds & Granger, 2023). The large amount of published nursing research can take years to be translated into practice. Therefore, IS-trained nurses can be instrumental in bringing significant practice changes through proactive and systematic uptake of innovations (Boehm et al., 2020).
Conclusion
The increasing complexity of health-care systems and practices requires rapid uptake and implementation of innovations in nursing education and practice. However, effective uptake of innovations is not possible without a structured, systematic process of innovation uptake readiness assessment, exploration of multilevel barriers, and use of tailored implementation strategies. IS offers the tools, methods, and approaches to ensure effective and efficient uptake of innovations with the involvement of multiple stakeholders including patients, administrators, managers, health-care professionals, and policymakers. To effect disruptive change, nurses need to move beyond traditional methods of changing practices, to more active methods of optimizing the uptake of innovations in practice.
Cite this article: Younas, A. (2023). Uptake of innovations in nursing: The necessity for implementation science. Creative Nursing 29(2).
Footnotes
Declaration of Conflicting Interests
The author is Editor-in-Chief of Creative Nursing.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biography
