Abstract
Background:
The complexity of health concerns associated with unregulated substance use has led to increased hospital utilization by people who use unregulated substances. Health care providers have described inadequate knowledge to adequately support this patient population during hospitalization.
Aims:
The aim of this research was to explore health care providers’ perspectives on harm reduction and substance use education in hospital settings.
Methods:
A qualitative secondary analysis was conducted using an interpretive lens. The research was conducted across three hospitals in one city in Southwestern Ontario. To guide the research, 31 health care providers, the majority being nurses, participated in either focus groups or individual interviews based on preference. All focus group or interview data were analyzed using an ethnographic method of analysis focusing on the hospital environment and education.
Results:
Health care providers described two interconnected states regarding harm reduction and substance use education: the current state and the desired state. Key themes which emerged in the current state and desired state include: (a) insufficient education, (b) lack of resources, (c) inconsistent policy, (d) culture of stigma and suboptimal care, (e) enhanced education, (f) resources, (g) policy change, and (h) culture shift and optimal care.
Conclusion:
Findings of this study demonstrate the need for supportive policies, adequate resources, and enhanced harm reduction and substance use in hospital settings. Addressing these gaps is essential to transforming hospital culture and improving care for people who use unregulated substances. These insights can inform future policy, practice, education, and guide new research initiatives.
Background
The United Nations Office on Drugs and Crime (2021) reports a rising frequency of substance use and attributable mortality. Cellulitis, deep vein thrombosis, abscesses (Wright et al., 2020), and endocarditis (Bearnot & Mitton, 2020; Gray et al., 2018) are common complications associated with injection substance use. Due to the complexity of health concerns, people using unregulated substances increasingly require hospital services (Kim et al., 2018), contributing to significant financial strain on the health care system (Tsybina et al., 2021).
Despite the frequency of hospital encounters, people who use unregulated substances often report delaying medical care due to stigmatization in hospital settings (Chan Carusone et al., 2019; Summers et al., 2018). Unregulated substance use refers to the consumption of psychoactive substances that are not produced or distributed through controlled channels. They often vary in potency, composition, and may be contaminated, increasing the risk of overdose and other health harms (WorkSafeBC, n.d.).
People who use unregulated substances often describe pain and withdrawal mismanagement in the hospital, which represents a barrier to accessing care (Bearnot & Mitton, 2020; Chan Carusone et al., 2019; Summers et al., 2018). When hospital care is accessed, leaving against medical advice (Chan Carusone et al., 2019; Strike et al., 2020; Summers et al., 2018; Tan et al., 2020) or being discharged from hospital for substance use (Kosteniuk et al., 2022) have been commonly described. These disruptions in care are associated with worsening infections or health conditions, leading to greater long-term costs to the health care system (Summers et al., 2018; Wright et al., 2020).
It has been demonstrated that people who use unregulated substances often continue use while in hospital (Strike et al., 2020; Tan et al., 2020). Despite this, Canadian health care providers frequently report inadequate knowledge and preparation to care for this population (Gagnon et al., 2020; Kestler et al., 2021; Lacroix et al., 2018; Pauly et al., 2015; Watts et al., 2023; Wiercigroch et al., 2021). Several Canadian studies have elaborated on misunderstandings of unregulated substance use, concluding that additional education could potentially reduce stigmatization and enhance knowledge of health care providers (Gagnon et al., 2020; Jenkins et al., 2022; Pauly et al., 2015). Education is consistently described as a critical component of effective care for people who use unregulated substances (Dogherty et al., 2022; Gagnon et al., 2020; Lacroix et al., 2018; Pauly et al., 2015).
Several Canadian studies have described the importance of policy change to support people who use unregulated substances in hospital (Hyshka et al., 2019; McNeil et al., 2016; Pauly et al., 2015). Typically, a zero-tolerance policy has been described in relation to substance use in Canadian hospitals (Hyshka et al., 2019; McNeil et al., 2016; Pauly et al., 2015). People who use unregulated substances recognize potential risks associated with substance use in hospital, such as injecting in public spaces or syringe sharing, compounded with abstinence policies, which may lead to leaving the hospital prematurely (McNeil et al., 2016). In contrast, community-based harm reduction services are viewed as nonjudgmental and supportive (McNeil et al., 2016). This contrast highlights the need for hospital policies, protocols and guidelines that are aligned with harm reduction principles and support safe and equitable care for people who use unregulated substances.
Harm reduction is a philosophy of care with the goal of reducing harms associated with unregulated substance use, rooted in principles of human rights and social justice, emphasizing nonjudgmental support, prioritizing individual well-being without a requirement of abstinence (Harm Reduction International, 2025). Canadian literature supports enhancing health care providers’ education on substance use and harm reduction, which requires collaboration with experts in the field (Braithwaite et al., 2021; Hyshka et al., 2019; Kestler et al., 2021), supporting harm reduction policies and protocols (Hyshka et al., 2019; McNeil et al., 2016; Pauly et al., 2015) and enhanced education in health care and educational institutions (Gagnon et al., 2020). No Canadian studies were found, however, that specifically explored substance use and harm reduction education from the perspective of health care providers in hospital settings. This indicates that further research is required to understand this phenomenon from the perspective of health care providers to inform education, practice, and policy (Harm Reduction International, 2025).
This study focused on Canadian perspectives of substance use and harm reduction education, recognizing the distinct nature of Canada’s health care system. Unlike the United States, where 33% of adults and 43% of low-income individuals report financial barriers to care (Osborn et al., 2016), Canada’s publicly funded model presents different challenges and opportunities. Moreover, provider roles and treatment protocols, such as fewer restrictions on prescribing opioid agonist therapies like suboxone (Kestler et al., 2021), further distinguish the Canadian context.
The purpose of this research was to seek an understanding of health care providers’ perspectives on substance use and harm reduction education in hospital settings. By illuminating foundational educational needs, this study aimed to inform health care institutions, educational institutions, educators, policy makers, and government officials in developing strategies and policies that better support the health care of people who use unregulated substances.
The following research questions were used to guide and inform this study:
Method
Design
This secondary analysis was guided by interpretivism, which emphasizes contextual meaning-making and diverse social realities (Creswell, 2009; Curtis & Keeler, 2022; Schwartz-Shea & Yanow, 2012). Data were drawn from the larger mixed-method study Methamphetamine Harm Reduction 2020–2024 (Forchuk, Serrato, & Scott, 2023; Forchuk, Serrato, Scott, et al., 2023; Forchuk, Silverman, et al., 2023), where participants consented to secondary use of their data. The primary study gathered quantitative and qualitative data from people with lived experience of methamphetamine use, and qualitative data from health care providers working in hospital settings with experience with patients who use methamphetamine. The present study exclusively focused on provider focus groups and interviews, emphasizing education (Forchuk, Serrato, & Scott, 2023; Forchuk, Serrato, Scott, et al., 2023; Forchuk, Silverman, et al., 2023).
Setting and Sample
In the primary study, participants were eligible to participate if they were employed in hospitals in Southwestern Ontario where the study was being conducted and had experience with patients who use methamphetamine. Convenience sampling was used with recruitment from participating hospitals via emails, posters, and referrals from the Methamphetamine Harm Reduction Advisory Group, which included frontline health care providers. Ethics approval was obtained from Lawson Health Research Institute and Western University Research Ethics Board for the primary study (REB ID #115779).
Procedures
Health care providers participated in 13 individual interviews and 5 focus groups over the course of 1 year. Individuals who chose to participate in focus groups did so at times coordinated to suit both their availability and that of other group members. Due to COVID-19 restrictions, participants were offered a choice between virtual or in-person sessions. In cases where participants preferred in-person interviews or focus groups, these were conducted in a private location within the hospital, facilitated by a research assistant.
Data Collection
During the original study, focus groups or interviews were conducted using video teleconferencing software as well as in person, following strict masking and social distancing protocols. Interviews and focus groups were semi-structured and facilitated by trained qualitative researchers. Questions focused on the current perception of harm reduction strategies in hospital, issues associated with the lack of harm reduction strategies in hospital, barriers, or facilitators to implementation of harm reduction strategies, and future recommendations. Focus groups lasted between 30 and 60 minutes, were audio recorded, and transcribed verbatim. Transcripts were deidentified and validated by members of the research team. Transcriptions were securely stored with Lawson Health Research Institute. Consent forms were stored securely in double-locked cabinets in the Lawson Health Research Institute. Participants received a $5 coffee gift card for their participation in the focus groups or interviews.
For this secondary analysis, two of the authors were involved in the original data collection, transcription, and analysis. The data were accessed through Lawson Research Institute and had previously been de-identified. Data were re-validated by the primary author for this secondary analysis to ensure accuracy of all transcripts prior to analysis.
Data Analysis
Given the complexity of hospital culture and provider perspectives, Leininger’s (2006) thematic ethnographic approach was used for data analysis. The four phases of data analysis described by Leininger (2006) include: (1) data collection and documentation, (2) categorization of emergent themes, (3) examination of patterns within broader social and cultural environments, and finally (4) abstraction and confirmation of major themes (Leininger, 2006). To maintain analytic flexibility, no formal theoretical framework was applied during analysis, though harm reduction was later considered in the discussion (Curtis & Keeler, 2022). The theme of education emerged early in the original study. Early in data collection, three researchers with extensive experience in qualitative analysis began to develop descriptors related to education, paying close attention to the culture of the hospital. The three researchers, as members of the Methamphetamine Harm Reduction Advisory Group, provided emic perspectives that informed and deepened the analysis. Following data collection, all transcripts were reviewed for themes, patterns, and explanations as they related to education in broader social and societal constructs and contexts. Saturation of themes occurred at this stage. Finally, major themes and recommendations were confirmed by all three researchers.
Rigor and Reflexivity
Investigator triangulation, audit trails, and reflexivity were used in this secondary analysis to enhance rigor (Heaton, 2004). Ongoing consultation with the primary investigator ensured validation and accuracy of the findings (Heaton, 2004). An audit trail was used to document data analysis procedures, research activities, and decisions (Lincoln & Guba, 1985). During the write-up of the analysis, assigned participant numbers were originally left in to ensure accuracy of analysis. During the final stage, however, participant numbers were removed to maintain confidentiality due to the sensitive nature of the topic. Reflective journaling was also utilized as a method to enhance rigor (Szabo & Strang, 1997). Reflexive entries were discussed with the primary investigator during all stages of the research.
Results
The study sample included a total of 31 health care providers, working in various roles across 3 hospital settings in 1 city in Southwestern Ontario. There was a total of 26 registered nurses who participated in the study, 3 of whom specialized in public health, 5 of whom specialized in mental health, and the remainder worked in acute care. Sample participants who did not identify as registered nurses included two managers, one nurse practitioner, one epidemiologist, and one social worker.
Multiple themes were identified during this analysis, which can be understood in two distinct categories: the current state and the desired state. In focus groups and interviews, health care providers discussed the desire to move from the current state to the desired state and factors involved in this culture shift as it related to education. Subthemes discussed as they relate to the current state included: (a) insufficient education, (b) lack of resources, (c) inconsistent policy, and (d) culture of stigma and suboptimal care. Subthemes discussed as they relate to the desired state included: (a) enhanced education, (b) resources, (c) policy change, and (d) culture shift and optimal care. Themes represented an interconnection between the current state and desired state described by health care providers, and the influence on culture in the hospital setting is conceptualized in Figure 1.
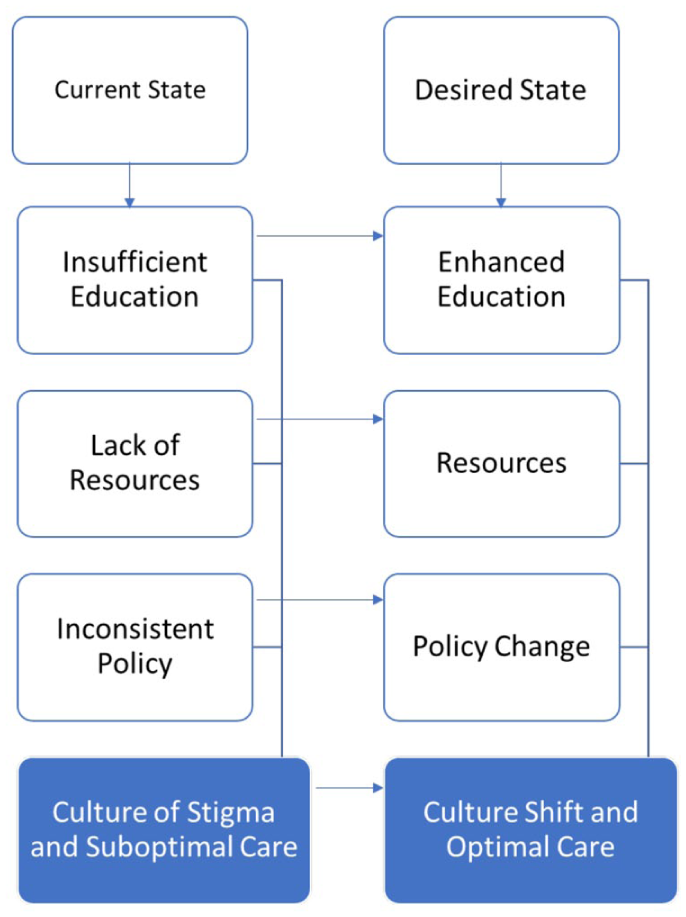
Interconnectivity Between the Current State and Desired State.
Current State
Insufficient Education
Lack of education on substance use and harm reduction was a prominent theme across nearly all focus groups and interviews. Health care providers described a lack of awareness of available education in hospital and general misunderstandings of harm reduction. Health care providers discussed insufficient education prior to entering the workforce, reinforcing higher level education was foundational to navigating complex situations involving people who use unregulated substances. “My university degree. . .only had a handful of lectures on drug use, . . . I guess we really don’t get a huge education on how to handle individuals who do use drugs.”
Health care providers explained they were frequently unable to distinguish intoxication or withdrawal symptoms associated with specific substances, highlighting the importance of knowledge of the specific effects of substances. Health care providers described screening tools that could aid in the evaluation of withdrawal symptoms, such as the Clinical Institute for Alcohol Withdrawal (CIWA; Sullivan et al., 1989) and Clinical Opiate Withdrawal Assessment Scale (COWS; Wesson & Ling, 2003); however, they explained there was little education on how to utilize these tools. “We do have the COWS assessment that helps. . .but I mean, there’s not a lot of education on that. The majority of the nurses here don’t know how to use it.”
Nearly a third of health care workers provided examples of harm reduction that were contradictory to principles of harm reduction. When asked about harm reduction, health care providers often identified that they were unclear on the concept of harm reduction:
We had a lot of theft of. . .needles and syringes. . . I know that our PWID [people who inject drugs] population was part of the issue of why we removed those supplies from the nurses’ servers. . .and made them centralized so they’re less accessible. . .Not sure if that would be a harm reduction strategy in hospital.
Although most health care providers described no education in hospital, a couple of participants did identify that there was a substance use online learning module in their organization. Health care providers identified gaps in this learning module, as there was no mention of harm reduction or stigma. Most importantly, health care providers felt this module was insufficient to guide care.
Widely throughout all focus groups and interviews, health care providers discussed insufficient education to provide care to people who use unregulated substances. Health care providers shared their frustration with insufficient education and frequently described being unable to meet the needs of people who use unregulated substances. Health care providers felt strongly about the lack of education; however, they raised other important points relative to the current state of education, including the lack of resources available in hospital.
Lack of Resources
Focus group and interview discussion revealed there was a perceived lack of available resources to support frontline health care providers caring for people who use unregulated substances. Some health care providers mentioned there were some resources available in hospital, such as addiction consult services; however, most health care providers stated there were no resources at all. “You can’t change what isn’t there. . .I haven’t heard of anything. . .I don’t know of anybody who’s a specialist in addiction, or you know that can help people, right?”
Although health care providers described a current lack of resources, prior to COVID-19, resources were discussed as being available in hospital to support people who use unregulated substances and staff, such as peer support or patient navigators. Unfortunately, health care providers explained that these resources were no longer available in hospital. “We used to have like a PWID navigator at one point. . .we would have referrals to her and, and she would be the social worker. . .That would help them. . .navigate and look at resources for discharge and work on discharge planning.”
Lack of resources was identified by nearly a third of staff throughout focus groups or interviews, and there was a strong indication that supportive resources would be greatly beneficial moving forward to care for people who use unregulated substances. In the current state, although some resources were available, such as an addiction consult service, health care providers were unaware of this service. Previous resources, such as people with lived experience or patient navigators, were no longer available in hospital, which left health care providers feeling unsupported, unprepared, and even unsafe at times.
Inconsistent Policy
Focus group and interview discussion revealed the importance of supportive policy for harm reduction to be implemented in hospital. Over a quarter of staff mentioned zero-tolerance policies or guidelines in hospital. As health care providers discussed hospital policy, some described feeling conflicted about the current policy, acknowledging potential risks to frontline staff and patients. “The hospital policy would have to change because if they have those substances on them, that’s confiscated by security. It goes to pharmacy to be disposed of.”
A few health care providers discussed a guideline that instructed them to remove sharps containers from people suspected of unregulated substance use. While a couple of health care providers described this action to minimize the harm of accessing syringes in sharps boxes, other health care providers recognized this protocol meant unequal treatment of people who use unregulated substances. Health care providers also recognized that syringe disposal would need to occur outside of the room, which poses an even more significant risk for staff and patients:
We remove sharps containers from within the room. . .when we have patients who inject drugs, which I think actually leads to an increased likelihood of. . .needle incidents, . . .sharp incidents for staff, and obviously they can’t dispose of their sharps as well. . .I think that—that’s a little counterproductive.
Health care providers recognized that policies and protocols may contribute to the marginalization of people who use unregulated substances in hospitals. In addition, policies at times left frontline health care providers feeling conflicted about care provided to people who use unregulated substances. Health care providers felt strongly that insufficient education, inconsistent policies, and limited resources contributed to the current state, which was perceived as a culture of stigma and suboptimal care for people who use unregulated substances in hospital.
Culture of Stigma and Suboptimal Care
Health care providers discussed a culture of stigma in hospital settings toward people who use unregulated substances. Health care providers explained that their challenges of caring for this population were related to a lack of knowledge, leading to suboptimal care. Although some health care providers mentioned personal bias, nearly half of the participants associated the culture of stigma with policies that marginalized people who use unregulated substances and a general lack of understanding of substance use:
I just feel like that type of policy marginalizes them. . .I can understand from a safety perspective, but at the same time. . .it creates a situation where they’re on the fringes of the healthcare system simply because they have to choose between their addiction or their care.
When reflecting further on the current culture of stigma and suboptimal care, health care providers were able to describe the effect limited knowledge has on staff providing care to people who use unregulated substances. “If the hospital doesn’t. . .do a good job of adequately training us on what these harm reduction strategies are, then I think we’re kind of putting ourselves in a position where we risk providing sub-optimal care.”
Health care providers discussed the perpetuation of stigma in hospitals from colleagues passing on personal experiences with people who use unregulated substances, which influenced perceptions. Health care providers also began to unpack what is needed to change the culture of stigma. Resources such as experts in the field working in hospitals to facilitate open communication where concerns could be shared and knowledge could be generated were perceived as important.
Unfortunately, providers frequently described feeling inadequately prepared to provide this type of care, which indicates that more resources and education are needed in the current state. Supportive policies would also be required to foster a supportive environment for health care providers and build confidence. Overwhelmingly, health care providers did not describe substance use or harm reduction education as something that was not wanted or needed in hospital, which highlights movement to the desired state and shift of culture.
Desired State
Enhanced Education
Enhancing education was a prominent theme mentioned in nearly every focus group or interview. A few health care providers discussed the importance of understanding the physiology of substance use. Approximately half of health care providers felt that understanding the motivations behind substance use was more important and foundational to understanding the complexity of addiction and caring for people who use unregulated substances:
But there are so many different reasons why people use meth, and what drives them. So in my opinion, I feel like we need to understand what those are before we can properly help people. . .and provide them with appropriate harm reduction strategies.
There was also a recognition among health care providers that trauma, abuse, and mental health conditions were often concurrently occurring for people who use unregulated substances, and understanding this link was fundamentally important. This recognition extended to understanding the behaviors of people who use unregulated substances, which were at times related to concurrent conditions and substance use disorder:
Understanding their behaviors because. . .that. . .is a huge component for how people have difficulty dealing with it, and they’d rather let them sign out AMA [against medical advice] or just go on their merry way. . .If we had strategies in place for them—how to handle this behavior, because in. . .this general hospital setting, we do not do very well with that at all.
Health care providers felt that more education regarding harm reduction strategies was important to caring for people who use unregulated substances. Health care providers described wanting to provide the same resources that were available in the community, such as sterile needles and safe injection techniques. It was recognized; however, health care providers would require additional education on community resources, which was thought to ultimately improve patient care. Health care providers did elaborate on current challenges to education, including staffing shortages, increased workload, and stress associated with the COVID-19 pandemic. Due to these challenges and lack of education, health care providers highlighted the need for supportive resources for staff as an integral part of the movement toward the desired state.
Resources
Health care providers shared several ideas regarding the value of adding resources in hospitals for the support of staff and people who use unregulated substances. A wide range of resources were discussed; however, nearly half of the participants discussed specialized expert teams as imperative to supporting frontline health care providers and people who use unregulated substances:
I would say for the vast majority of nurses, I think we would be happy to have a team able to support us in caring for these patients who had that specialized training, who we knew that we could call on if we had any questions, if we needed them to come assess the patient.
Over a quarter of health care providers further thought it would be beneficial to have people with lived experience in hospital to support people who use unregulated substances and educate frontline staff on substance use and harm reduction. “Peer support, I think, would be huge. . .You hear that so many times, and the evidence is overwhelming that supports. . .peer support.”
Resources discussed by health care providers ranged from having addiction experts in hospital, specialized addiction teams, people with lived experience, counseling services, or screening tools. Several health care providers interviewed mentioned there was a substance use expert in hospital who was available to consult patients; however, health care providers still felt this was insufficient to provide support for this growing population and that to facilitate movement into the desired state, concrete resources would be required.
Policy Change
Policy change was discussed as an important element to supporting harm reduction and substance use education in hospital. A few health care providers suggested policy should be reviewed initially to better understand the context of the hospital environment and how current policy is supporting or negating the needs of frontline staff and people who use unregulated substances. “So that’s where you look at the policies of the hospital. . .I would look at that, and then I would look at how is the hospital addressing these needs and what policies need to be put in place?”
Health care providers described the zero-tolerance policy at the hospital, and when reflecting, they acknowledged this may not be an evidence-based approach to care. Health care providers frequently reflected on safe injection sites during interviews and often agreed that a major challenge to the implementation of harm reduction in hospital was the current zero-tolerance policies. When health care providers further explored policy, they explained that this would be imperative to moving toward a harm reduction organization. Health care providers described policy as providing safety and protection from potential perceived legal ramifications of safe consumption in hospital. In addition, health care providers recommended looking to other institutions or standards of care to fully understand the level of care that should be provided in hospital to people who use unregulated substances. “It would be nice to know what the standard of care is, . . .if there is a standard of care, it would be really nice from a nursing lens to know. . .how do other places support harm reduction in patients?”
Overall, the policy was perceived to offer safety to health care providers caring for people who use unregulated substances and could provide suggestions for specific care of this population based on evidence-based practice and guidelines. It was suggested that policy, along with education and resources, created the potential for cultural change in the hospital, moving toward the desired state.
Culture Shift and Optimal Care
Health care providers acknowledged the current state in hospital and reflected on opportunities to change the culture. During discussions, nearly all health care providers perceived enhanced education to be a large component of changing the culture of stigma. “I think education is probably quite key. . .It’s not even just the nurses, it’s all staff. . .I would feel like that would probably be really key to changing the culture regarding stigma.”
When health care providers further explored cultural change in hospital, they identified the requirement of a specialized team with expertise in substance use disorders. Frontline staff described a specialized team as being able to support people who use unregulated substances and health care providers. Over time, this would increase health care providers’ capacity to provide care to people using unregulated substances. More importantly, health care providers identified that change needed to come from the top of the organization to gain support, which in turn could help facilitate educational opportunities for frontline health care providers and, in turn, change culture:
I think that needs to be a cultural change, and to be a cultural change, I think it needs to come from the top. But on top of that, I think it can’t just be one education day and one education session. Maybe it needs to be something yearly or every two years.
Health care providers went on to describe the need for a process to hold people accountable for the stigmatization of people who use unregulated substances. In addition, health care providers would need to be able to recognize their personal bias to improve relationships with people who use unregulated substances. This solidifies the need for both policy and education to drive cultural change and optimal care of people who use unregulated substances.
Health care providers recognized there would be some barriers to changing the culture of stigma in hospital. Overwhelmingly, health care providers explained that if frontline staff felt supported and were educated, barriers could be broken down. Health care providers again reiterated the inability to drive change in hospital when supportive policy, education, and resources are not currently in place.
Discussion
Consistent with existing literature, health care providers reported limited knowledge of substance use disorders and harm reduction (Gagnon et al., 2020; Kestler et al., 2021; Lacroix et al., 2018; Pauly et al., 2015; Watts et al., 2023; Wiercigroch et al., 2021). Participants described educational gaps both prior to entering the workforce and upon entry to hospital practice, reinforcing the need for more robust substance use and harm reduction education. This study builds on prior research by examining provider perspectives on hospital-based harm reduction and substance use education and factors shaping their understanding.
While participants acknowledged the importance of understanding the physiology of substance use disorders, they emphasized the need to recognize psychosocial drivers, including mental health conditions and behavioral patterns, as essential for providing adequate care. Many described a lack of awareness, which may have perpetuated stigma and reinforced person bias. Health care providers advocated for trauma-informed approaches and a deeper understanding of co-occurring conditions to improve communication and care.
Participants identified a broad range of educational priorities, including: screening and diagnosis, withdrawal management, specific substance use disorders, harm reduction principles, co-occurring conditions, medical complications, safe prescribing practices, recovery-oriented systems of care (Gorfinkel et al., 2019), motivational interviewing, brief interventions (Gorfinkel et al., 2019; Registered Nurses Association of Ontario [RNAO], 2015), social determinants of health, population health promotion models, the transtheoretical model of change, trauma-informed care, and cultural safety (RNAO, 2015). Despite the availability of the COWS, participants reported inadequate training in their use, which is consistent with other research findings (Wiercigroch et al., 2021).
A key finding was the widespread misunderstanding of harm reduction. While Canadian literature often links harm reduction in relation to opioid agonist therapy or naloxone (Kestler et al., 2021; Lacroix et al., 2018; Wiercigroch et al., 2021), this specific study revealed misconceptions such as removing sharps containers or relocating syringe supplies to deter the use of substances. These actions contradict harm reduction philosophy and increase risk. These misunderstandings may stem from institutional policies, such as zero-tolerance approaches and removal of sharps containers from rooms of patients suspected of substance use. Although zero-tolerance policies are documented (Hyshka et al., 2019; McNeil et al., 2016; Pauly et al., 2015), their impact on harm reduction implementation remains underexplored. Despite this, health care providers generally recognized existing policies contributed to the marginalization of people who use unregulated substances and expressed a desire to improve hospital environments through policy reform. Participants also identified resource gaps, particularly the absence of addiction consult services, peer support, and patient navigators as barriers to equitable care (Braithwaite et al., 2021; Hyshka et al., 2019; Kestler et al., 2021). These gaps reflect broader systemic inequities in access to educational resources and institutional support, which disproportionally affect marginalized populations. These resources were viewed as essential to shifting hospital culture and improving outcomes, with funding and institutional support.
Despite the availability of best practice guidelines (RNAO, 2015), many providers were unaware of the standard of care for this population. As Gagnon et al. (2020) noted, nursing students recognized harm reduction as a philosophy to guide care; however, they were unable to translate this philosophy into practice. In the absence of harm reduction policy in hospitals, health care providers may feel stuck between evidence-based practice and policies that are aligned with criminalization, further increasing the stigmatization of this population. These dynamics are highlighted in the findings of this study and further supported by previous research (Pauly et al., 2015, 2017). These dynamics underscore the need to address structural oppression, including policy, education, and communication practices, to foster equitable care environments. Harm reduction policy development in hospitals may enhance care of people who use unregulated substances, reduce discharge AMA, and respond to health care providers’ requests for guidance and further education on harm reduction (Lennox et al., 2021). Recommendations of harm reduction policy in hospitals occur regularly in the literature (Hyshka et al., 2019; Lennox et al., 2021); however, only a few Canadian hospitals have described them in practice in Canadian literature (Canadian Research Initiative in Substance Misuse, 2020; Dogherty et al., 2022).
Future research should examine hospitals where harm reduction policies have been introduced to explore contextual differences and cultural shifts. Encouragingly, some participating hospitals have begun implementing policy and resource changes reflecting institutional recognition of these needs.
Limitations
This study was also conducted in one city in Southwestern Ontario. As such, findings may not be transferable to alternative settings. Convenience sampling was utilized for this study; therefore, participants may have been motivated or interested in the topic of harm reduction, which may have impacted the findings. The sample was largely composed of Registered Nurses, which represents a limitation as no physicians, psychiatrists, or pharmacists were included in the sample. This study was also conducted during the COVID-19 pandemic, which may have affected recruitment of health care providers, focus group or interview capacities, and the abilities of research staff to recruit participants. This study was also a secondary analysis of qualitative data from a larger study, which focused on methamphetamine harm reduction in hospitals. As such, this study may have been limited by the scope of the original focus group and interview discussion questions, which were designed for the parent study and may not have fully aligned with the research questions guiding this secondary analysis. In addition, participants who opted into the parent study may not fully represent the target population of interest.
Conclusion
This study illuminates care inequities faced by individuals who use unregulated substances in hospital settings as viewed by health care providers. Participants described a disconnect between their desire to provide compassionate care and the constraints imposed by limited education, inadequate resources, and restrictive policies. The findings from this study highlight the need for enhanced training, inclusive policy development, and sustained resources to shift hospital culture, reduce stigma, and promote equity for people who use unregulated substances. These findings further reflect deeper health equity concerns, where institutional power structures, uneven access to educational resources, and barriers to communication contribute to the marginalization of people who use unregulated substances.
Advancing harm reduction and substance use education in hospital requires more than curriculum revision. Addressing educational gaps will require a health equity approach that challenges institutional stigma while promoting inclusive education and policy reform. It demands dynamic and responsive strategies that span the macro, mezzo, and micro levels. These insights offer guidance for hospitals, educators, post-secondary institutions, and policy leaders to redesign care systems that meet the needs of people who use unregulated substances and the providers committed to caring for them.
Footnotes
Acknowledgements
We would like to acknowledge and thank Health Canada who funded the primary study for this research. We would like to thank all our colleagues at the Mental Health Nursing Research Alliance, particularly Jonathan Serrato, Tammy Fisher, and Mathew McGuigan for continuously supporting this work.
Author Roles
All authors contributed to the conception or design of the study or to the acquisition, analysis, or interpretation of the data. All authors drafted the manuscript, or critically revised the manuscript, and gave final approval of the version that was submitted for publication. All authors agree to be accountable for all aspects of the work, ensuring integrity and accuracy.
Data Availability Statement
Currently, the qualitative data used in this research is not accessible due to limitations in our data sharing protocols.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This Study was funded by Health Canada’s Substance Use and Addictions Program. Funding Grant number 2021-HQ-000041.
Ethical Approval
Ethics approval was obtained from Lawson Health Research Institute and Western University Research Ethics Board for the primary study (REB ID #115779).
