Abstract
This study aims to determine the prevalence and risk factors of violent events leading to Acquired brain injury (ABI). Research was conducted through the SPAVO helpline which provides anonymous and immediate support and connect individuals with necessary resources and guidance. Data were collected using four specific questions from the BR.A.I.N. Screening Questionnaire and questions were asked regarding violence characteristics. Out of 729 females, 61% encountered physical violence, with 32% facing a heightened risk of ABI. These findings highlight the significant risk of ABI among female survivors of intimate partner violence and assist policymakers, frontline professionals regarding the needs of this population.
Introduction
Acquired brain injury (ABI) is often called the silent epidemic for survivors of intimate partner violence (IPV) (Haag et al., 2022a). ABI results from injury to the brain, which may occur due to direct trauma to the head (resulting in traumatic brain injury [TBI]) or from nonimpact mechanisms such as lack of oxygen (hypoxia or anoxia) due to strangulation attempts. TBI and hypoxic/anoxic injuries are mechanisms of ABI that are most commonly sustained from physical violence in IPV. In this project, we adopt the term ABI to encompass both the direct trauma to the brain due to the biomechanics of the violent event and the lack of oxygen resulting from strangulation attempts against the victim. IPV-related ABI has been significantly overlooked. IPV incidents that cause ABI may result in more severe long-term difficulties, such as physical, social, neuropsychological, and mental health issues (Karakurt et al., 2021; Valera et al., 2019). Traditionally, studies investigated the nature of IPV and brain injury (BI) separately; only recently, studies have started to examine these issues together (Murray et al., 2016; St Ivany & Schminkey, 2016). It is important to mention that, in the context of IPV, repeated episodes of head injuries can occur (St Ivany & Schminkey, 2019). While there is limited research, it remains plausible that women subjected to recurrent head trauma within the context of IPV could face heightened susceptibility to develop long-term neurological consequences, for example, dementia, chronic cognitive difficulties (St Ivany & Schminkey, 2019). Given these concerns, early-stage screening becomes crucial in identifying individuals who may be at increased risk for such consequences and who may require additional evaluation (Campbell et al., 2018).
Reviews (Haag et al., 2022b) and empirical studies report original prevalence data of IPV-related TBI ranging from 19% (Iverson et al., 2019) to 75% (Valera et al., 2019; Valera & Kucyi, 2017) and as high as 100% (St Ivany et al., 2018). A history of physical abuse to the head, face, or neck that put women at risk for ABI was reported by anywhere between 35% and 100% of respondents in a few studies (Haag et al., 2022; Monahan & O'Leary, 1999). In the study of Monahan and O'Leary (1999) participated 26 women from a shelter and the 35% reported a history of head trauma and the 44% reported loss of consciousness at the time of the injury.
A study by Valera et al. (2022) included 52 women with a history of IPV, of whom 29% reported incidents of strangulation. The study included both women residing in shelters and those not residing in shelters (Valera et al., 2022; Valera & Berenbaum, 2003). The frequency of strangulation incidents and/or severe BIs was higher among women residing in shelters. However, the rates of at least one and multiple mild head injuries were almost identical in the two groups, showing that that BIs are not restricted to shelter populations (Valera & Berenbaum, 2003). The study suggests that although severe BIs and choking episodes are more common among women in women's shelters, milder head injuries may occur both among women in women's shelters and among women who do not live in women's shelters. These findings underscore the importance of recognizing the potential for head injury in both contexts and addressing the broader problem of violence and its associated health risks. Corrigan et al. (2003) support the fact that women who have experienced IPV are at risk for mild traumatic brain injury. From this study 30% of women reported a period of loss consciousness after the head injury and 67% of women reported residual problems that were potentially head-injury related (Corrigan et al., 2003).
Similarly, Zieman et al. (2017) included 115 individuals with a history of head trauma because of domestic violence. From those individuals, 88% reported more than one injury and 81% reported a history of loss of consciousness related to their injuries (Zieman et al., 2017). Previous studies highlight a notable disparity between reported prevalence and the actual incidents, revealing a significant gap between reported incidents and their factual occurrences (St Ivany et al., 2018). First, individuals with IPV commonly do not seek immediate medical care for their injuries for a number of reasons, including control by their abuser, social and financial dependence, lack of insight into the severity of their injuries, and poor decision-making abilities as a result of their multiple BIs (Monahan & O'Leary, 1999). For example, Zieman et al. (2017) demonstrated that only 21% of individuals with head trauma as a result of domestic violence sought medical attention at the time of injury (Zieman et al., 2017). Ideally, IPV survivors should receive medical attention immediately after the events leading to BI and their medical records would reflect the incident. Also, in many cases, even when women seek medical help may leave the emergency department without being screened for BI and be informed about the risks of further neurologic symptoms that may arise the hours and days post injury (Haag et al., 2022b). The vast majority of these BIs are mild and often do not receive appropriate medical attention. Additionally, emergency departments may not be fully aware of the intersection between IPV and BI, further limiting timely identification and care (Valera & Berenbaum, 2003). Specifically, emergency department professionals primarily encounter BIs in young men, often resulting from motor vehicle accidents or high-risk behaviors. Additionally, women with IPV-related BI may present with addiction and/or mental health issues which may mask the effects of BI (WHO, 2014). Lastly, COVID-19 has exacerbated IPV and IPV-related TBI, posing further difficulties for women to seek medical attention and identification (Haag et al., 2022b).
Research has consistently demonstrated the link between IPV-related head trauma and postconcussive symptoms (PCSs). In a study by Jackson et al. (2004), 53 women who had experienced IPV participated, with 77% reporting PCSs, including headaches, dizziness, cognitive difficulties, and emotional challenges. Moreover, a significant correlation was found between the frequency of head injuries and the severity of cognitive symptoms, suggesting that routine screening for BI and PCSs in IPV survivors is crucial (Jackson et al., 2004). Similarly, Campbell et al. (2018) examined central nervous system (CNS) symptoms in women with IPV-related head injuries, women with IPV but no head injuries, and women with no IPV history. CNS symptoms were significantly more prevalent among IPV survivors, particularly in those with probable BI, even after controlling for depression and posttraumatic stress disorder (PTSD) symptoms. However, this study relied solely on self-reports without additional neurological testing, a limitation acknowledged by the authors (Campbell et al., 2018). Recent research further supports these findings, emphasizing that IPV-related BI presents with distinct and persistent PCSs compared to psychological trauma alone. Chiou et al. (2023) found that women with probable IPV-related BI reported more severe cognitive and sensory impairments than those without BI, reinforcing the need for targeted clinical assessments. Additionally, Smirl et al. (2019) highlighted the cumulative effects of repeated IPV-related BI, noting that chronic head trauma can exacerbate PCS and lead to long-term neuropsychological consequences. These findings emphasize the necessity of early detection and specialized interventions for IPV survivors at risk of BI.
Research indicates that the chronicity, frequency, and intensity of IPV significantly impact the risk of ABI among survivors. IPV-related violence often escalates over time, leading to repeated head trauma and increased exposure to mechanisms such as strangulation and severe shaking (Haag et al., 2022; Thompson et al., 2006). Studies suggest that prolonged exposure to IPV is associated with a higher likelihood of repeated traumatic events, further compounding the risk for both immediate and long-term neuropsychological consequences (Thompson et al., 2006). Chronic IPV exposure has been linked to a range of physical and mental health consequences, including cardiovascular disease, PTSD, and cognitive deficits, underscoring the urgent need for early identification and intervention (Haag et al., 2022b; WHO, 2021).
This study aims to determine the prevalence of ABI risk among females who called SPAVO (Association for the Prevention and Handling of Violence in the Family). Specifically, we assess whether female participants reported incidents that placed them at risk for ABI based on mechanisms of injury (e.g., head trauma, strangulation) and whether they self-reported symptoms consistent with ABI. We also aim to examine the characteristics of violence (intensity, frequency, chronicity) associated with incidents that put females at risk for ABI. To our knowledge, this is among the few European studies addressing these questions and capturing IPV-related ABI prevalence in females. We hypothesize that a high percentage of females who called SPAVO and reported physical IPV were at risk for ABI based on violent mechanisms of injury. Additionally, we hypothesize that characteristics of violence (e.g., intensity, frequency, chronicity) are associated with ABI risk. Lastly, we hypothesize that females classified as at high risk for ABI will self-report a greater number of PCSs than females who reported only psychological violence or females who experienced physical violence but were not classified as at risk for ABI. From a practical perspective, classifying the prevalence of traumatic BI associated with IPV will provide important data for policymakers to address the needs of this population and provide guidance for health professionals working with females with IPV.
Materials and Methods
Sample and Procedures
This study employs a cross-sectional observational design, conducted as part of the larger BR.A.I.N. Project (Bridging the Gap between IPV and Head Injury: Assessment, Prevalence, and Neuropsychological Insights, project website: https://brainprojectcyprus.org). The BR.A.I.N. Project is a European initiative aimed at addressing the critical gap in research and screening regarding the intersection of IPV and BI. While IPV-related BIs are increasingly recognized, many survivors go undiagnosed due to a lack of standardized screening tools. This project among others seeks to bridge this gap by developing and validating a screening tool specifically designed to assess IPV survivors’ risk for ABI. This study, as part of the BR.A.I.N. Project, enables a comprehensive examination of the incidence of violent events and associated factors contributing to the risk of ABI among females who sought assistance through the SPAVO helpline from November 2021 to December 2022. Ethical approval for the project was granted by the Cyprus Bioethics Committee (EEBK/ΕΠ/2021/11).
We established a cooperation with SPAVO, the leading nongovernmental organization handling intimate partner/domestic violence in Cyprus. Participants were recruited directly from the SPAVO helpline (#1440). This helpline, hosted by SPAVO, accepts calls related to domestic violence, including incidents of IPV. The only inclusion criterion was that the participant had to be 18 years of age or older. When individuals called the SPAVO direct helpline, frontline professionals anonymously asked questions regarding (1) attempted strangulation, (2) head and/or neck injuries and/or severe shaking, (3) loss of consciousness, dizziness, loss of memory, and (4) alterations in everyday life due to these incidents. These questions were extracted from the BR.A.I.N. Screening Questionnaire (BSQ), a 14-item screening tool developed as part of the BR.A.I.N. Project to screen for ABI in the context of domestic/IPV. The four items were selected based on their direct relevance to IPV-related ABI, ensuring brevity and feasibility within the crisis helpline setting while maintaining validity in identifying individuals at risk. Risk of ABI was determined using responses to the BSQ, which assessed reported mechanisms of injury, including head trauma, severe shaking, and strangulation. Female participants were classified as “at risk for ABI” if they endorsed experiences that involved a mechanism known to cause ABI. The screening tool was administered in a pilot study with 20 individuals to assess its initial reliability and determine key statistical properties. Specifically, we calculated Cronbach's alpha (α = .9) to evaluate internal consistency, indicating strong reliability. Additionally, we examined item response patterns to ensure the questions effectively captured experiences related to IPV and ABI risk. The findings from the pilot study informed minor refinements to question wording and response options, improving clarity and applicability before full-scale data collection. Questions from the screening tool were asked among other questions regarding the date of the call, type of violence, if they visit the hospital after an incident of physical violence, the characteristics of violence such as chronicity (experiencing violence consistently over an extended period), frequency, and intensity (escalation of violence during the past 3 months from the call). Questions assessing the characteristics of violence were developed by SPAVO professionals and included predefined response categories for participants to select from. The full set of response categories is presented in Table 2. PCSs were assessed using a combination of direct symptom-specific questions regarding loss of consciousness, dizziness, and memory loss following an event. The BSQ was selected because it was specifically developed within the BR.A.I.N. Project to assess IPV-related ABI risk. Unlike structured clinical interviews, such as the Ohio State University TBI Interview or the Direct Method of Screening, the BSQ was designed to be brief, accessible, and feasible for administration in contexts where detailed medical histories cannot always be collected.
A total of 794 individuals called the SPAVO helpline from November 2021 until December 2022; two participants were excluded due to missing demographic variables (e.g., sex). From the 792 individuals, 729 (92%) were females and 63 (8%) were males. Hence, our study now focuses on females who survived IPV and excludes males. Figure 1 shows the strobe diagram of the sample.
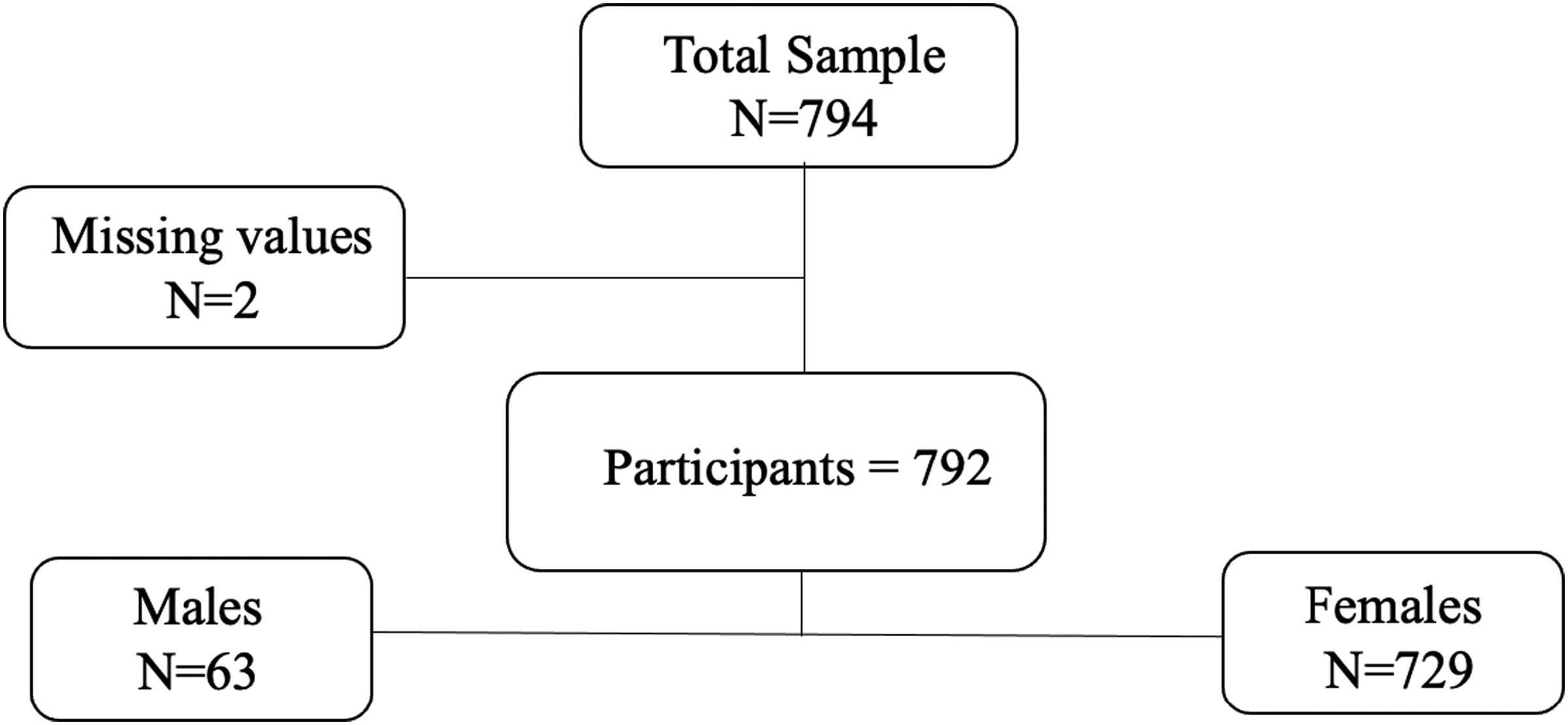
Strobe Flow Diagram.
Statistical Analyses
Statistical analyses were performed using IBM SPSS Statistics 29.0 (IBM, 2023). Descriptive statistics were used to describe the frequency of violence each month, the types of violence, and characteristics such as chronicity, intensity, and frequency. We also examined the prevalence of IPV incidents that put females at risk for ABI, the prevalence of, and the prevalence of incidents that reached healthcare services after incidents of physical violence. Data were categorical, and each variable was reported as a frequency count and percentage of the total sample. Chi-square analyses were used to identify whether incidents that put females at risk for ABI are independent from characteristics of violence, such as chronicity, intensity, and frequency of violence, and between incidents that put females at risk for ABI and incidents that reached healthcare services after incidents of physical violence. A two-tailed P < .05 was considered statistically significant unless otherwise indicated.
Results
Figure 2 illustrates the number of calls received each month from November 2021 to December 2022. As shown in Figure 2, February 2022 saw the highest number of calls, followed by June and July of 2022, then December 2021 and January 2022.
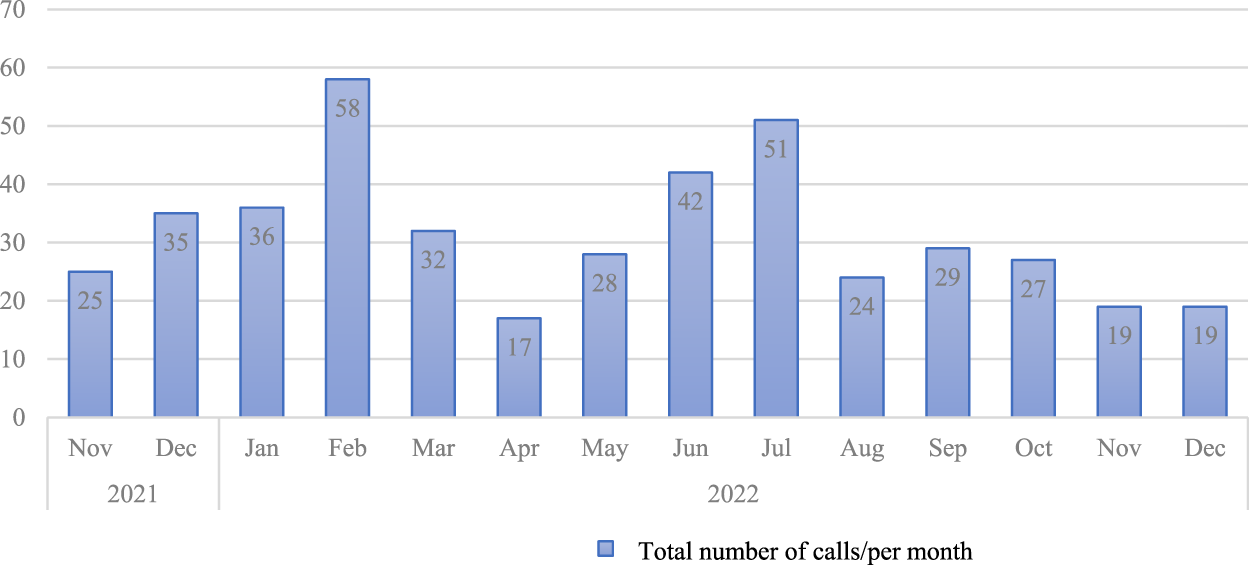
Number of Calls per Month During the Data Collection Period.
Females reported experiencing more than one type of violent act. Specifically, 706 female participants (97.8%) reported psychological violence, 442 (61.2%) physical violence, 60 (8.4%) sexual violence, 183 (25.5%) economic violence, 110 (15.3%) harassing surveillance, and 63 (8.8%) electronic violence. Additionally, 188 females (26.2%) reported receiving death threats from the perpetrator, and 76 (10.6%) reported that the perpetrator used an object or a gun during the violence incident. Out of 729 females, 473 (66.2%) reported experiencing violence for more than 7 months. Specifically, 90 (12.6%) reported violence lasting 7–12 months, 156 (21.8%) for 2–3 years, and 106 (14.5%) for more than 10 years. Concerning the intensity and frequency of violence, 384 (53.9%) reported an increase in both over the past 3 months. Table 1 provides more details on the types and characteristics of violence.
Frequency of Types and Characteristics of Violence Within the Sample.

It was not possible to get an answer because either the call was ended, either the individual did not want to answer the question.
ABI and IPV
Among the 729 female participants, 442 (61.2%) reported physical violence. We excluded the rest who reported no physical violence and focused on those at risk of BI. Of the 442, 140 (32%) may be at significant risk of sustaining a BI. Notably, these individuals reported a total of 176 incidents potentially leading to BI, with 67 (15.3%) involving strangulation and 109 (24.7%) involving hits to the head, severe shaking, or both. We categorized the sample into three groups: those experiencing psychological violence, those encountering physical violence at risk for BI, and those experiencing physical violence but they were not at risk for BI (namely individuals who did not endorse incidents involving head trauma, severe shaking, strangulation, were categorized as experiencing physical violence without BI risk in this context), to examine their reports of PCSs. Of the 140 female participants at risk for BI, 37 reported experiencing PCSs, including symptoms such as loss of consciousness, dizziness, confusion, and memory loss. Among these, 21 indicated these incidents led to changes in their daily lives. In contrast, only two out of 269 participants reporting solely psychological violence and two out of 302 who experienced physical violence without risk of BI reported PCSs. Chi-square analysis revealed a statistically significant difference in PCS reports between female participants facing psychological violence and those at risk of BI due to physical violence, χ2(1) = 67.47, P < .001. A similar pattern emerged when comparing those at risk of BI due to physical violence with those not at risk, χ2(1) = 75.77, P < .001. Among the 442 females reporting physical violence, 5.9% sought healthcare services following incidents involving head injuries or strangulation, and 9.2% for other reasons. The remaining 337 (84.9%) did not seek healthcare services. Table 2 provides more details on these variables.
ABI and IPV and the Association of Characteristics of Violence and Risk for ABI.

Note: ABI: acquired brain injury; IPV: intimate partner violence.
It was not possible to get an answer because either the call was ended, either the individual did not want to answer the question.
Characteristics of Violence and ABI
Among female participants who experienced physical violence, 251 (57.3%) reported violence lasting over 2 years, and 256 (58.6%) noted an increase in the frequency and intensity of violence over the past 3 months. Table 2 offers more insights into these characteristics. Chi-square analyses were conducted to examine the relationship between the chronicity of violence and incidents of strangulation or head injuries. The results showed a significant association between chronicity and head injuries, χ2(5, N = 305) = 11.49, P < .05 (see Table 3). Additionally, a chi-square analysis examined the relationship between the intensity and frequency of violence and incidents of strangulation or head injuries, revealing a significant association between intensity of violence and incidents of strangulation, χ2(2, N = 301) = 9.92, P < .05 (see Table 4).
Chi-Square Analysis of Association Between Chronicity of Violence and Trauma to the Head or Strangulation Incidents.
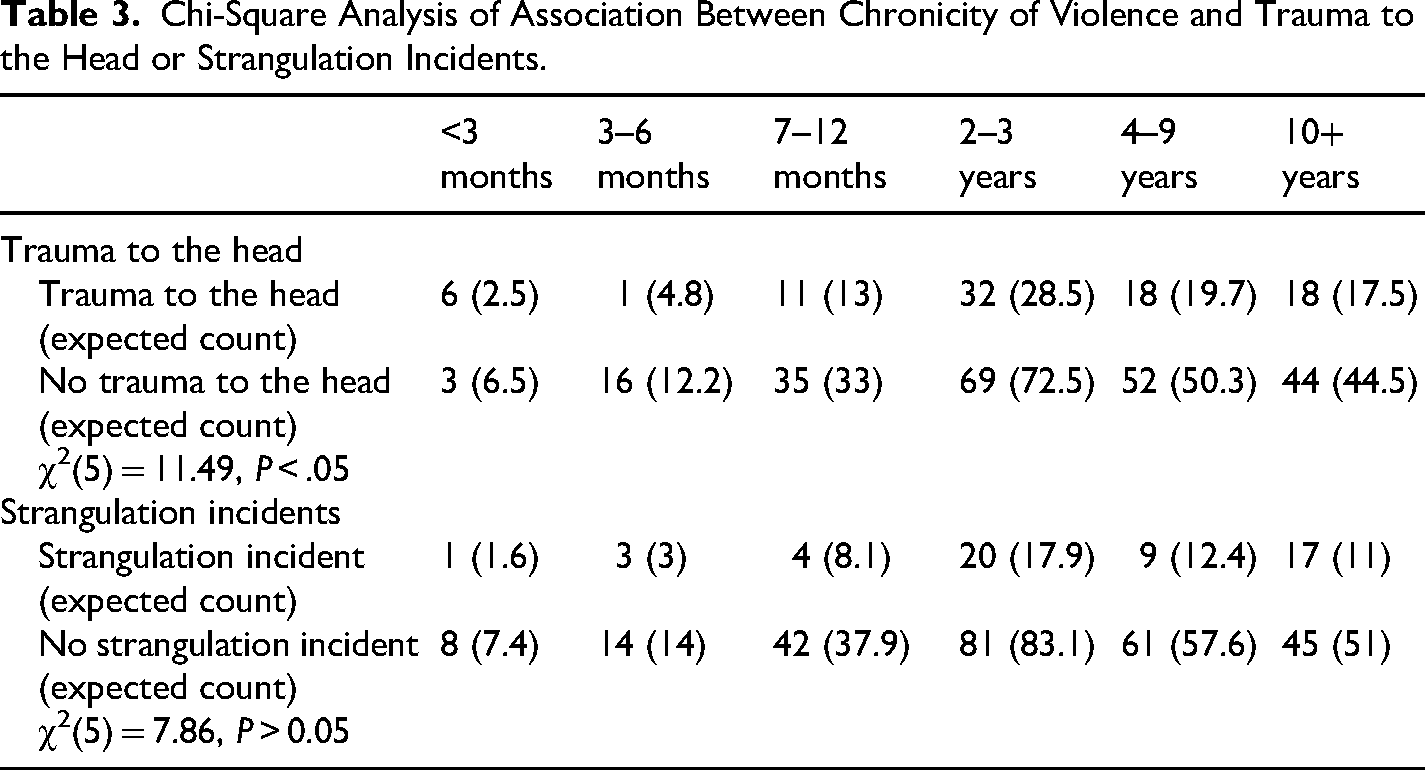
Chi-Square Analysis of Association Between Intensity of Violence and Trauma to the Head or Strangulation Incidents.
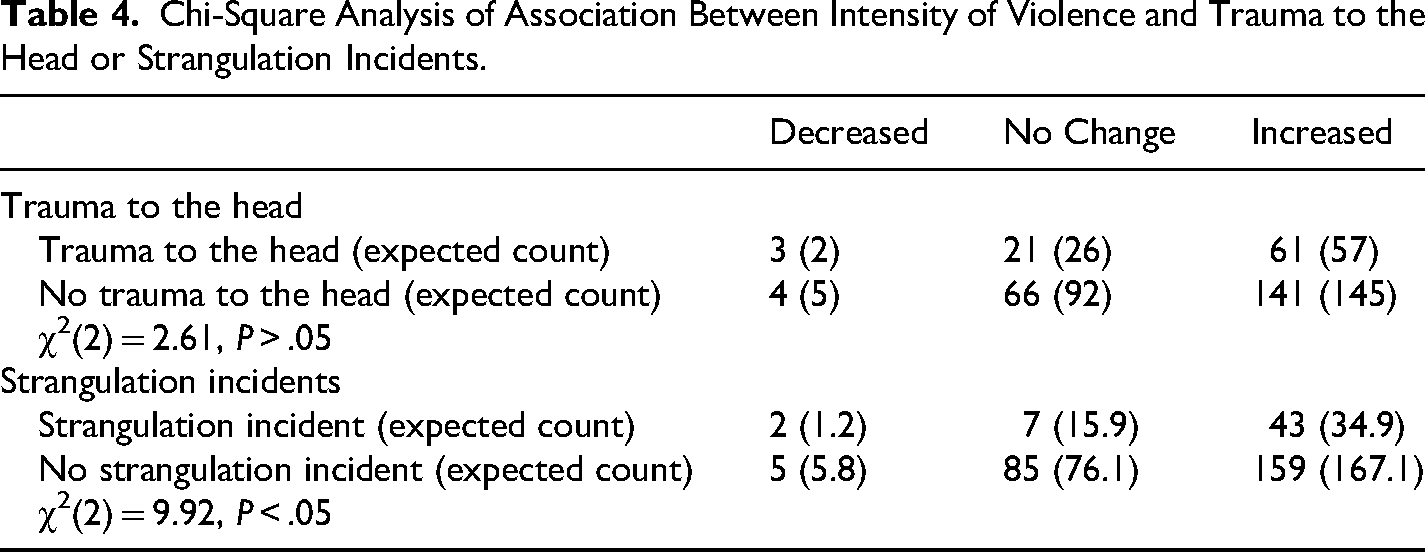
Discussion
This study sheds light on a very important and overlooked issue: the occurrence of physical violence and abuse-related BI against females. To our knowledge, this study is one of the few in Europe, and the outcomes of the present study inform the literature with important evidence on IPV and ABI, and the needs this population may have. This study is also the first one which took place in Cyprus, an Eastern Mediterranean island and European Union (EU) member state with a population of approximately 1.2 million (Statistical Service of Cyprus, 2021). Like other southern Mediterranean nations, Cyprus is characterized by strong family networks, which, while offering support, can also contribute to sociocultural stigma that deters IPV survivors from seeking help (Haag et al., 2022). Despite high literacy rates and EU-aligned legal frameworks, IPV remains a pressing issue, with underreporting influenced by social norms and fear of repercussions. Access to specialized IPV and ABI services is still developing, emphasizing the need for targeted interventions that address both legal and healthcare barriers. Understanding these cultural factors is critical for improving screening, support services, and policymaking tailored to women in Cyprus and similar regions (WHO, 2021). The findings are alarming, with a significant percentage of females experiencing incidents that may result in ABI. Moreover, more than half of female participants who reported physical abuse have suffered it for more than 2 years. Our study indicates that the chronicity of violence is associated with a higher likelihood of experiencing more frequent and intense incidents. This escalation in violence is linked not only to an increased risk of head and/or neck trauma but also to a heightened likelihood of repeated trauma. The data from our study supports a connection between the ongoing nature of violence and its impact on the frequency and intensity of traumatic incidents, emphasizing the need for interventions to address this pattern.
Domestic violence is a pervasive issue that affects millions of women globally. Even though, IPV can affect people of any gender, most victims are women (Toccalino et al., 2022). Women are at a higher risk for physical injury than men and at a higher risk for strangulation by an intimate partner than men (Toccalino et al., 2022). During the months of data collection of our study the helpline received 792 calls from which the 63 were about males and 729 were about females. In this study, we use the term sex (female/male) to reflect the biological classification recorded by helpline staff. Participants were not directly asked to self-identify their gender; thus, we avoid using gender-related terminology to maintain clarity and accuracy in reporting. Hence, our study focused on females who have experienced domestic/IPV and found that the highest number of calls for help was made during February of 2022, followed by June and July of 2022. These findings can be explained by the fact that during February Cypriots celebrated Carnival, a period with many parties and increased alcohol consumption, environmental factors which are related to IPV (Devries et al., 2014). Similarly, summer months are associated with many social activities and vacation.
From the findings of our study, 729 females who have experienced domestic/IPV are concerning and highlight the prevalence and severity of this societal problem. Studies have shown that psychological violence, as reported by most participants in our study, can have long-lasting effects on mental health, including depression, anxiety, and PTSD (WHO, 2021). Additionally, a significant percentage of females reported experiencing physical, sexual, economic, and electronic violence, indicating that IPV takes on many different forms and can have serious consequences for survivors. The chronicity of violence reported by individuals in our study is also alarming, with over two-thirds of females experiencing violence for more than 7 months. A large proportion of female participants reported experiencing violence for 2‒3 years, and some reported experiencing violence for 10 or more years. Studies found that chronicity of violence can have serious consequences for survivors (Haag et al., 2022; Thompson et al., 2006). A study conducted in Canada found that women who experienced chronic IPV were at increased risk of developing chronic health conditions, including cardiovascular disease, diabetes, and arthritis (Thompson et al., 2006). This highlights the need for ongoing support and resources for survivors of IPV, as well as prevention and early intervention strategies to prevent further harm. Finally, our findings regarding the increase in intensity and frequency of violence reported by over half of female participants in our study over the past 3 months are consistent with other studies that have found that IPV can escalate quickly. This further emphasizes the need for immediate support and resources for survivors in danger.
The current study's pivotal finding is the substantial risk of ABI in females experiencing domestic/IPV. Out of the 442 female participants who experience physical violence, a substantial 32%—amounting to 140 individuals—were identified as being at a heightened risk for ABI, meaning that there were experienced incidents such as blows to head, severe shaking and strangulation incidents that put them at risk for ABI. Even more important is that the number of total incidents contributing to this risk totaled 176, considering instances where individuals reported more than one traumatic incident. Of notable concern is the alarming prevalence of strangulation incidents reported by these individuals. The high incidence of strangulation incidents reported by participants is particularly concerning, as strangulation is a highly lethal form of violence that often leads to anoxia and ABI (Valera et al., 2022). The fact that such a large proportion of females reported incidents of hits to the head, severe shaking, or both, also underscores the significant risk of ABI in cases of domestic/IPV. Studies conducted in USA and Canada have also explored the link between IPV and TBI, and many have found similarly concerning results. Specifically, physical abuse to the head, face, or neck that put women at risk for ABI was reported by anywhere between 35% and 100% of respondents in a few studies (Haag et al., 2022; Monahan & O'Leary, 1999). It is also worth noting that a significant number of individuals in our study did not seek medical care after experiencing violence, including incidents that may result in ABI. This highlights the need for increased education and awareness around the signs and symptoms of ABI in cases of domestic/IPV, both for healthcare providers and for victims themselves.
Findings relating to self-reports of PCSs are of considerable significance, aligning with prior research (Jackson et al., 2004). Our approach of categorizing the sample into groups based on the nature of violence encountered—psychological or physical—and their associated risk for ABI provided valuable insights into the intricate relationships among these variables. The statistically significant results underline and reinforce the substantial differences in PCS reports between these distinct groups. These outcomes suggest that the observed variations in PCS reports are not random occurrences, but rather indicative of meaningful relationships between the nature of violence and the risk for ABI. Recent studies indicate that IPV-related BI survivors exhibit significantly higher PCSs, including cognitive difficulties, headaches, and sensory impairments, compared to those without probable ABI (Chiou et al., 2023). Additionally, the cumulative effects of IPV-related ABI have been linked to an increased PCS burden, contributing to long-term cognitive and psychological consequences (Smirl et al., 2019). These findings align with our study, which suggests a robust association between the experience of physical violence, particularly when coupled with the risk for ABI, and the occurrence of PCS. In contrast, PCS is not observed or associated with cases of psychological violence and/or physical violence without the risk of ABI. Overall, our results contribute to a deeper understanding of the relationships between the nature of violence, the risk for BI, and the manifestation of PCS, reinforcing the importance of considering these factors in comprehensive assessments of individuals exposed to IPV.
Findings regarding the relationship between chronicity of violence and incidents of strangulation, hits to the head, and/or severe shaking, as well as the relationship between frequency and intensity of violence and these incidents, are also important. These results imply that the risk of head trauma may escalate over time, particularly when a woman is exposed to physical violence persistently across years. Furthermore, our results suggest a notable increase in strangulation incidents in tandem with the rise in both the frequency and intensity of violence.
Limitations and Future Directions
The present study is perhaps the first study on IPV and ABI conducted in Europe taking place in a small eastern Mediterranean island country with its unique geopolitical–cultural characteristics. It provides important data on the prevalence of violent acts that put females at risk for ABI. A limitation of our study is that the data collected were anonymous as victims of IPV called through the crisis line to report an incident or ask for help. Findings indicate that many females who experience IPV and ABI do not seek medical attention. Due to the anonymous data collection strategy, follow-up interviews or assistance was not possible. Future research could examine effective ways to educate frontline professionals and guide victims who call the anonymous hot lines. Moreover, emphasis will be given to improve screening and diagnosis of ABI in this population, including developing tools that are sensitive to the unique challenges faced by victims of IPV (Goldin et al., 2016). As a part of our project, we have created the BSQ specifically for the screening of BI in the context of violence. We are currently in the process to validate this screening tool and, in the future, to be used by frontline professionals and make referrals where is needed. Given the high prevalence of ABI among females who experience IPV, there is a need for interventions that address the physical and mental health consequences of ABI in this population. Future studies could explore the effectiveness of existing interventions, such as cognitive rehabilitation or trauma-focused therapy, in improving outcomes for females with IPV-related BI. Crucially, it is recognized that the self-report nature of data collection introduces the potential for recall bias. Also, it is important to note that the observed increase in intensity of violence among over half of the participants may, in part, reflect a sample bias. Given that recruitment occurred through an IPV helpline, it is likely that many individuals sought assistance precisely due to an escalation in violence, meaning our sample may be skewed toward those in crisis. This should be considered when interpreting the generalizability of our findings regarding IPV intensity and chronicity.
While this study provides valuable insights into the prevalence of violent acts and associated risks for ABI among females who sought assistance through the helpline in Cyprus, the unique geopolitical–cultural characteristics of this small eastern Mediterranean island country should be considered. The findings may not be universally applicable, and caution is advised when generalizing them to different cultural or geographical contexts. Future research in diverse settings is warranted for a more comprehensive understanding of the broader implications of IPV and ABI.
Conclusion
Our findings regarding the prevalence and consequences of IPV are consistent with other studies that have highlighted the serious public health issue that IPV represents. It is crucial to prioritize prevention and early intervention strategies, provide ongoing support and resources for survivors. It is essential to ensure that females have access to safe spaces and resources to seek help when they need it, as well as to continue to educate communities about the warning signs of IPV and how to support survivors (WHO, 2021). In addition, our study highlights the urgent need for increased awareness, education, and screening efforts to prevent and address the significant risk of ABI in cases of IPV. Future research should continue to explore this important topic and identify effective strategies for prevention and intervention.
Footnotes
Acknowledgments
The authors would like to wholeheartedly thank the dedicated staff at SPAVO for their invaluable contribution to this study. Their careful and meticulous work in data entry was essential in providing the necessary information for our study.
Ethical Considerations
This study was conducted in accordance with ethical standards and received approval from the Cyprus National Bioethics Committee. The research protocol was reviewed and approved by the committee under approval number EEBK/ΕΠ/2021/11. The SPAVO-1440 helpline ensured confidentiality and anonymity for all participants, providing immediate support and connecting them with necessary resources.
Consent to Participate
Informed consent to participate in this study was obtained verbally from all participants. The data were anonymized and collected through the helpline of the Association for the Prevention and Handling of Violence in the Family (SPAVO). The Cyprus National Bioethics Committee approved this method of obtaining consent, given the confidential and sensitive nature of the study and the fact that data collection was conducted over the phone.
Consent for Publication
This manuscript does not contain any data from individual persons, including individual details, images, or videos that would require informed consent for publication.
Authors’ Contributions
Conceptualization: Flora Nikolaou.
Methodology: Flora Nikolaou, Michalis Michaelides, Yelena Goldin, and Fofi Constantinidou.
Data collection: Flora Nikolaou.
Data analysis: Flora Nikolaou.
Writing‒original draft preparation: Flora Nikolaou.
Writing‒review and editing: All authors contributed equally.
Funding acquisition: Flora Nikolaou, Fofi Constantinidou, Iro Michael, and Andri Andronikou.
The authors confirm their authorship and contributions to this paper titled “Prevalence and Characteristics of Acquired Brain Injury in Female Victims of Domestic/Intimate Partner Violence: Insights from a Cross-Sectional Study in Cyprus.” All authors have reviewed and approved the final version of the manuscript for submission.
Funding
The authors disclosed receipt of the following financial support for the research: The study was supported by the Ministry of Justice and Public Order of the Republic of Cyprus under the National Mechanism for Women's Rights. The funders were not involved with the decision to publish, and preparation of the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
Certain data can be made available from the corresponding author on reasonable request.
