Abstract
Clinical and economic outcomes associated with venous thromboembolism (VTE) patient adherence to the American College of Chest Physicians (ACCP) anticoagulant (AC) treatment guidelines are incompletely understood. Patients with ≥1 inpatient or ≥2 separate outpatient claims for deep vein thrombosis and/or pulmonary embolism, based on International Classification of Diseases, Ninth Revision, Clinical Modification codes, were identified from the IMS PharMetrics Plus database. Patients had continuous insurance coverage for 12 months before (baseline) and after (follow-up) the index event (first VTE claim) but no baseline VTE claims. The ACCP recommends minimum AC treatment durations (3 or ≥6 months) dependent upon patient risk profiles. Patients were grouped into study cohorts based on their adherence status (adherent vs nonadherent) to the recommended minimum treatment durations. Patient baseline characteristics, health-care resource utilization, and associated costs were evaluated. The VTE recurrence and bleed-related hospitalization were measured during follow-up. Multivariate regression analysis was utilized to compare clinical and economic outcomes of cohorts. Of the 81 827 study patients, 74% (n = 60 550) were AC adherent. After controlling for key patient characteristics, risks for all-cause hospitalization (adjusted odds ratio [AOR]: 0.85, P < .0001), VTE recurrence (AOR = 0.92, P = .0014), and bleeding-related hospitalization (AOR = 0.74, P < .0001) were lower among adherent patients, as were all-cause health-care cost (−US$2121, P = .0003) and VTE-related (−US$2294, P < .0001) and bleed-related (−US$248, P < .0001) medical costs during the follow-up period. Approximately one-quarter of the study population was AC nonadherent; these nonadherent patients had more VTE recurrences, utilized more inpatient services, and had higher health-care costs.
Keywords
Introduction
Venous thromboembolism (VTE), encompassing deep vein thrombosis (DVT) and pulmonary embolism (PE), is a major health concern associated with significant mortality and morbidity. 1 –3 It is the third most common cause of vascular disease–related death 4 and poses a substantial economic burden on the health-care system. In the United States, approximately 1 million people develop symptomatic VTE annually. 1 The economic burden of VTE is not restricted to the index event but is amplified by the costs and utilization of medical resources for managing recurrent VTE events. 5,6 The average total annual VTE-related health-care payment per patient is estimated to be over US$30 000, and the annual total health-care cost associated with VTE ranges from US$7.5 to US$39.5 billion. 7 –9
The length of oral anticoagulant (OAC) therapy to prevent thrombosis recurrence is based on recommendations from the American College of Chest Physicians (ACCP) clinical practice guidelines. 10 –12 The minimum duration of anticoagulant (AC) therapy recommended by the ACCP guidelines is dependent upon patient risk profiles. 10 –12 The ACCP recommends that patients with provoked VTE or unprovoked VTE but with a high risk of bleeding receive at least 3 months of AC therapy. For patients with unprovoked VTE and a low or moderate risk of bleeding, or patients with cancer, the ACCP recommends extended AC therapy. 10 –12 Patient adherence to the guideline-recommended treatment durations for VTE has not been well studied, especially in terms of health-care costs as a measure of potentially reducing the clinical and economic burden of VTE.
The present study assessed the real-world adherence to the ACCP guidelines for OAC treatment duration for an index VTE event. This study further evaluated the clinical and economic outcomes associated with patient adherence or nonadherence to OAC treatment durations.
Materials and Methods
Data Source
Data were extracted from the IMS PharMetrics Plus database. The database encompasses over 150 million unique patients and consists of health-care claims data from various commercial health and managed care plans in the United States since 2006. Information on patient demographics, patient insurance type and enrollment information, medical diagnoses and procedures for inpatient and outpatient care, prescription medication fills, and medical and pharmacy payments was available. The IMS PharMetrics Plus database also contains data from Medicare supplemental plans covering patients above the age of 65, an important segment of the study population as advanced age is a risk factor for the development of VTE.
Study Population
Claims data from January 1, 2008, to March 31, 2014, were used to enroll eligible patients with at least 1 inpatient claim or 2 separate outpatient claims, at least 30 days apart, for DVT and/or PE based on the International Classification of Diseases, Ninth Revision (ICD-9) diagnostic codes. The period from January 1, 2009, to March 31, 2013, was defined as the index identification period. A diagnosis of DVT was identified by ICD-9 codes of 451.11, 451.19, 451.2, 451.81, 451.83, 451.84, 451.89, 451.9, 453.2, 453.40, 453.41, 453.42, 453.8, 453.82, 453.83, 453.84, 453.85, 453.86, 453.87, 453.88, 453.89, and 453.9, and a diagnosis of PE was identified by ICD-9 codes of 415.11, 415.12, and 415.19. The first VTE claim during the index identification period was defined as the index VTE event (ie, DVT, PE, or DVT/PE). In addition, patients in the study were required to be 18 years of age or older on the date of the index VTE event and had evidence of use of anticoagulation therapy within 30 days following the date of the index VTE event. Patients were required to have continuous medical and prescription coverage during the 12 months before (baseline period) and 12 months after (follow-up period) the index VTE event date and had no VTE claims during the baseline period. Patients were required to receive warfarin, unfractionated heparin, low-molecular-weight heparin, fondaparinux, or non-vitamin K oral anticoagulants (NOACs) for a total duration of ≥30 days or had at least 2 OAC prescription (Rx) fills (AC use) during the study follow-up. The Computerized Registry of Patients with Venous Thromboembolism (RIETE) bleeding risk score was used to categorize patients into high (score >4), intermediate (score 1-4), and low (score <1) bleed risk categories. 13
During the follow-up period, patient adherence to the ACCP ninth edition guidelines for AC treatment duration was evaluated as follows: (1) for patients with provoked VTE or unprovoked VTE but with high risk of bleeding as per the RIETE bleed score, at least 3 months of AC therapy duration was considered adherent based on the ACCP guidelines and (2) for patients with unprovoked VTE and a low or moderate risk of bleeding as per the RIETE bleed score, or patients with active cancer, 6 months of AC therapy was used as the minimum duration in order to be considered adherent, as the ACCP recommends extended AC therapy in these groups. 10 –12 Patients with the following baseline characteristics were defined as having provoked VTE: pregnancy, oral contraceptive use, trauma, recent hospitalizations, or recent surgeries occurring during the last 30 days prior to the index event; patients without those baseline characteristics and those with cancer were identified as having nonprovoked VTE. 10 –12 Patients were grouped into 2 study cohorts based on their adherence status to the ACCP-recommended AC minimum treatment duration (adherent vs nonadherent). The AC treatment duration was defined as the time from the index event date to the first date of anticoagulation discontinuation. Patients are considered to have discontinued their anticoagulation therapy if there is a gap of greater than 30 days between the end date of previous AC prescription (prescription claim date plus the days of supplies) and the health insurance claim date of the next AC prescription. The date of anticoagulation discontinuation was defined as the end date of the last AC prescription before AC discontinuation plus 30 days or the patient disenrollment rate or the end of study period, whichever is the earliest. This grace period of 30 days at the end of each anticoagulation period was given since changes in AC dosages are common.
Evaluation of Patient Baseline Demographics and Clinical Characteristics
Patient demographics consisting of age, gender, and geographical region were assessed at the index date. Clinical characteristics assessed included VTE risk-related characteristics, Charlson comorbidity index (CCI) scores, and key comorbid conditions. The proportion of patients in each cohort with each type of VTE risk-related characteristic was assessed during the baseline period. Venous thromboembolism risk–related characteristics included type of index VTE event (DVT, DVT/PE, and PE) and whether the event was a provoked or nonprovoked VTE event, as defined using the criteria described above. The CCI score is used as an estimation of patients’ comorbidity levels. 14 The proportion of study patients with selected key comorbid conditions was also determined and compared between the adherent and nonadherent cohorts; key comorbidity conditions included congestive heart failure (CHF), coronary heart disease (CHD), diabetes, chronic kidney disease, myocardial infarction (MI), stroke/transient ischemic attack (TIA), cancer, and severe infectious diseases.
Bleeding Risk
The RIETE is a data registry of consecutive patients with confirmed VTE that includes each patient’s comorbid conditions, type of treatment, and treatment outcomes such as VTE recurrence, bleeding complications, and death. A bleeding risk score has previously been developed based on the data from the RIETE registry. 13,15 The proportion of patients with the following RIETE bleeding risk score levels was determined and compared between the adherent and nonadherent cohorts: high risk (score >4), intermediate risk (score 1-4), and low risk (score <1).
Venous Thromboembolism Treatment Information
Venous thromboembolism treatment for the index VTE event was assessed for the overall population and each study cohort. The use of the following OACs for treatment was examined: warfarin, rivaroxaban, dabigatran, and apixaban. The proportion of patients receiving OAC therapy only, OAC and injectable AC therapy, or injectable AC therapy alone was also evaluated.
Resource Utilization and Costs
Resource utilization and associated payments incurred for inpatient and outpatient services, including office visits and emergency department (ED) visits, and outpatient prescriptions filled were evaluated. Inpatient resource utilization was stratified by all-cause hospitalization, bleed-related hospitalization, and VTE-related hospitalization, which is defined as hospitalizations associated with a bleed or VTE diagnosis code, respectively, at any position of the hospital discharge diagnoses. The impact of patient adherence status on all-cause hospitalizations, bleed-related hospitalizations, and VTE-recurrence was evaluated by logistic regression. Venous thromboembolism recurrence is defined as either hospitalizations or ED visits associated with VTE diagnosis at any position of the recorded diagnosis codes. Adjusted odds ratios (AORs) describing the likelihood of each resource utilization end point or VTE recurrence by the status of adherence vs non-adherence were reported. An AOR < 1.0 indicated adherence was associated with a lower likelihood of resource use compared to nonadherence. Conversely, an AOR > 1.0 indicated adherence was associated with a higher likelihood of resource utilization than nonadherence.
Total payments for services provided during the baseline and follow-up periods were determined for the following categories: inpatient services, office visits, ED visits, outpatient prescription (Rx) use, medical health care services (inpatient or outpatient health-care services, exclusive of pharmacy services), and total health-care services (inpatient and outpatient services, inclusive of pharmacy services). Differences in health-care payment between baseline and follow-up periods were compared. The impact of adherence to AC treatment duration on total health-care payments and VTE- and bleed-related medical health-care payments was also evaluated.
Statistical Analysis
Descriptive statistics were used to summarize patient demographics, clinical characteristics, health-care payments, and health-care resource utilization. T tests and χ2 tests were used to detect statistically significant differences in continuous and categorical variables, respectively. Multivariable logistic regression model analysis was used to evaluate the impact of adherence status on all-cause hospitalizations, bleed-related hospitalizations, and VTE recurrences during the follow-up period, while controlling for differences in patient characteristics. Generalized linear model regressions with gamma data distribution and log transformation were used to evaluate the impact of AC adherence status on total all-cause health-care payments and both VTE- and bleed-related medical health-care payments. The covariates used in the regression models included AC adherence status, age, gender, US geographical region, health plan type, CCI, index VTE type (PE vs DVT vs both), provoked VTE status, RIETE bleed risk, key comorbid conditions, and the type of ACs used. A critical value of .05 was used to determine statistical significance. All statistical analyses were carried out using SAS 9.3.
Results
Study Population
A total of 81 827 patients with an index VTE event who met the patient selection criteria were identified from the IMS PharMetrics Plus database and included in the analysis. The mean age of the study sample was 55 years, and the median age was 56 years. Patients included in the study were grouped into 2 cohorts based on their adherence to the recommended AC treatment duration: adherent (n = 60 550) and nonadherent (n = 21 277; Figure 1). The determination of patient adherence status is outlined in Figure 1. Of all patients with VTE, 74% were adherent to the ACCP-recommended treatment duration.
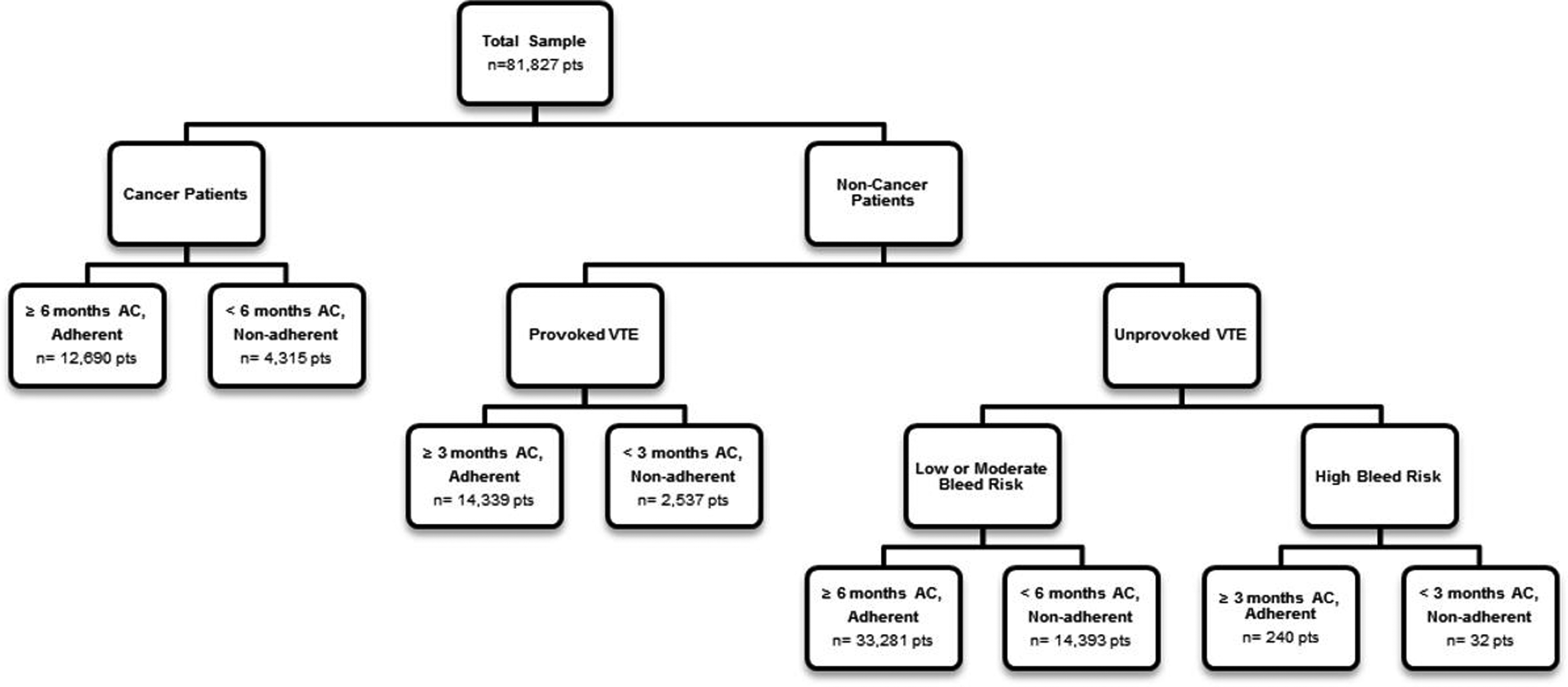
Diagram of patient adherence status determination.
Baseline Demographics and Clinical Characteristics
Baseline demographics are presented in Table 1. For the study population, patients who were adherent to the recommended duration of AC treatment were older than nonadherent patients (mean age = 55.39 vs 55.11 years, P = .0104). Compared to nonadherent patients, a higher proportion of adherent patients were ≥75 years old (10.3% vs 9.4%, P < .0001) and female (48.5% vs 46.7%, P < .0001).
Baseline Demographics of Study Cohorts.
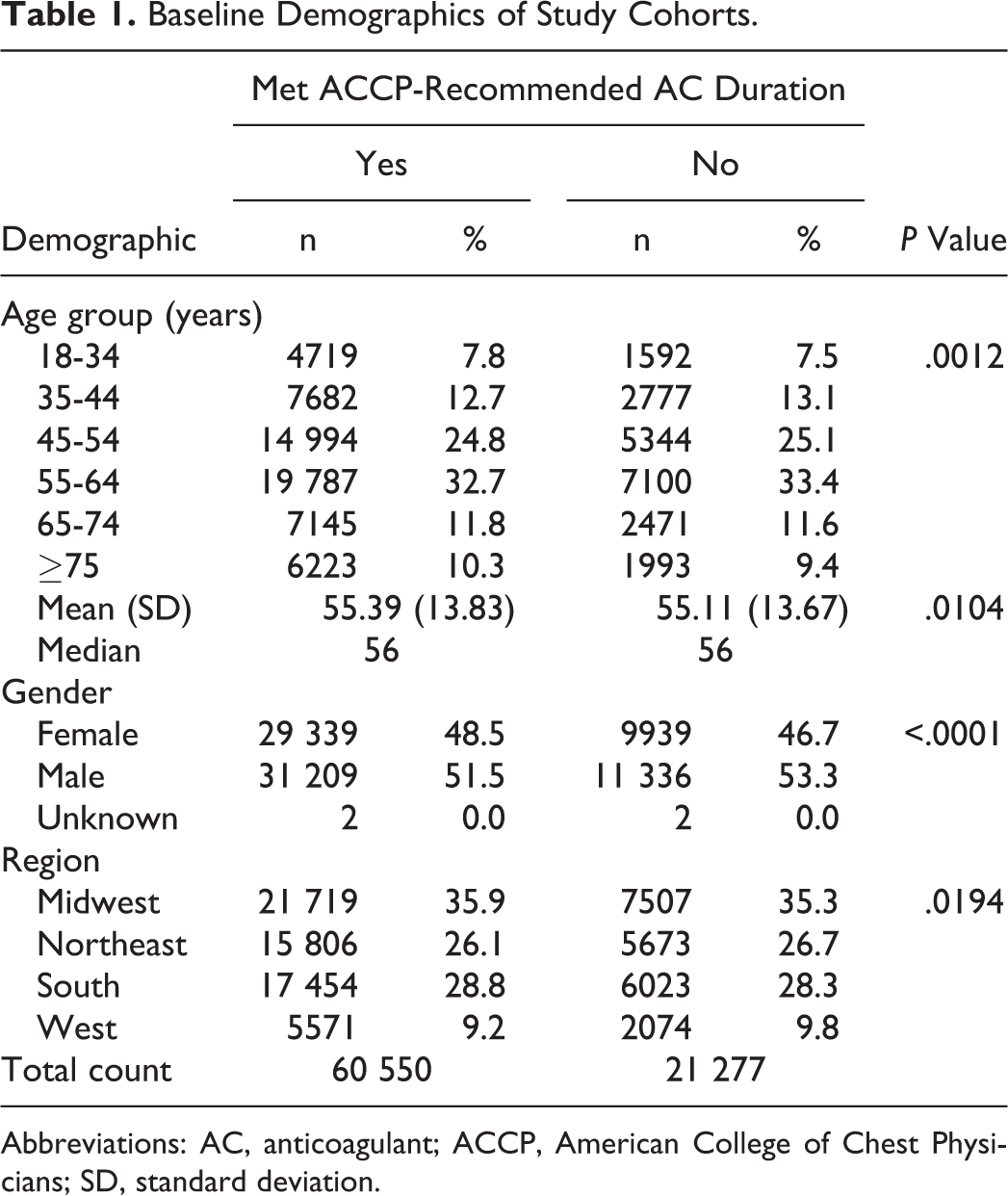
Abbreviations: AC, anticoagulant; ACCP, American College of Chest Physicians; SD, standard deviation.
Clinical characteristics of the study sample are presented in Table 2. Nearly two-thirds (61%) of patients had an index event associated with DVT only (n = 50 140). There were 21 150 (26%) patients with an index event associated with PE only, and 10 537 (13%) patients had an index event associated with both DVT and PE diagnoses. Mean CCI score (1.67 vs 1.59, P < .0001) was higher for patients who were adherent versus nonadherent. More adherent patients had comorbidities of CHF (7.3% vs 6.3%, P < .0001), CHD (15.1% vs 14.5%, P = .0272), diabetes (18.7% vs 18%, P = .0252), MI (4.1% vs 3.5%, P = .0002), and stroke/TIA (4.7% vs 3.8%, P < .0001). More adherent patients had high RIETE bleed risk levels (1.9% vs 1.0%, P < .0001) than nonadherent patients (Table 2).
Clinical Characteristics of Study Cohorts.
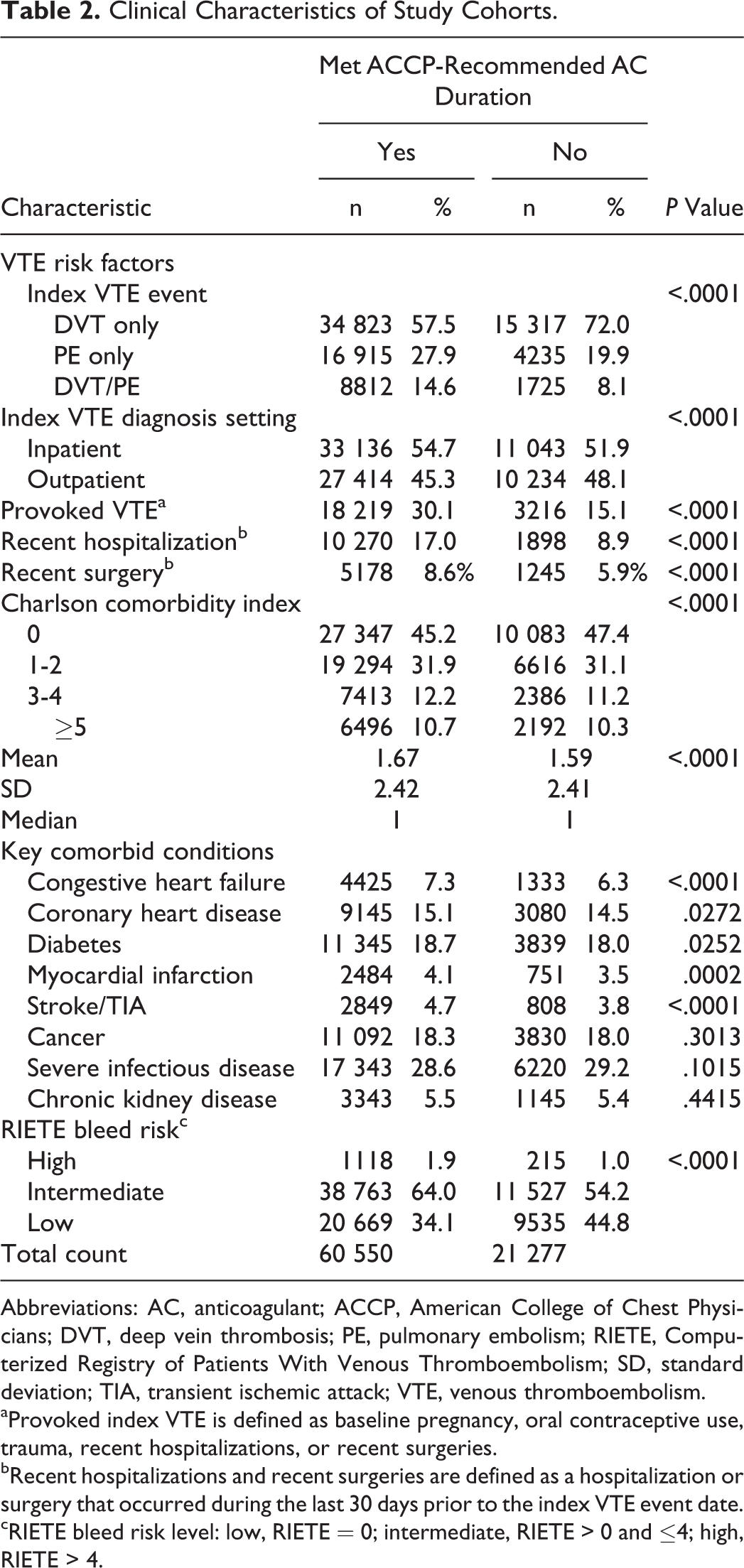
Abbreviations: AC, anticoagulant; ACCP, American College of Chest Physicians; DVT, deep vein thrombosis; PE, pulmonary embolism; RIETE, Computerized Registry of Patients With Venous Thromboembolism; SD, standard deviation; TIA, transient ischemic attack; VTE, venous thromboembolism.
aProvoked index VTE is defined as baseline pregnancy, oral contraceptive use, trauma, recent hospitalizations, or recent surgeries.
bRecent hospitalizations and recent surgeries are defined as a hospitalization or surgery that occurred during the last 30 days prior to the index VTE event date.
cRIETE bleed risk level: low, RIETE = 0; intermediate, RIETE > 0 and ≤4; high, RIETE > 4.
Patient VTE Treatment Characteristics
Patient VTE treatment information is presented in Table 3. Among patients included in this study, 74% (n = 60 550) were adherent to the ACCP-recommended treatment duration. A large percentage of the study population (95.0%, n = 77 698) received at least 1 OAC treatment, with warfarin as the most common OAC.
Venous Thromboembolism Treatment Type.
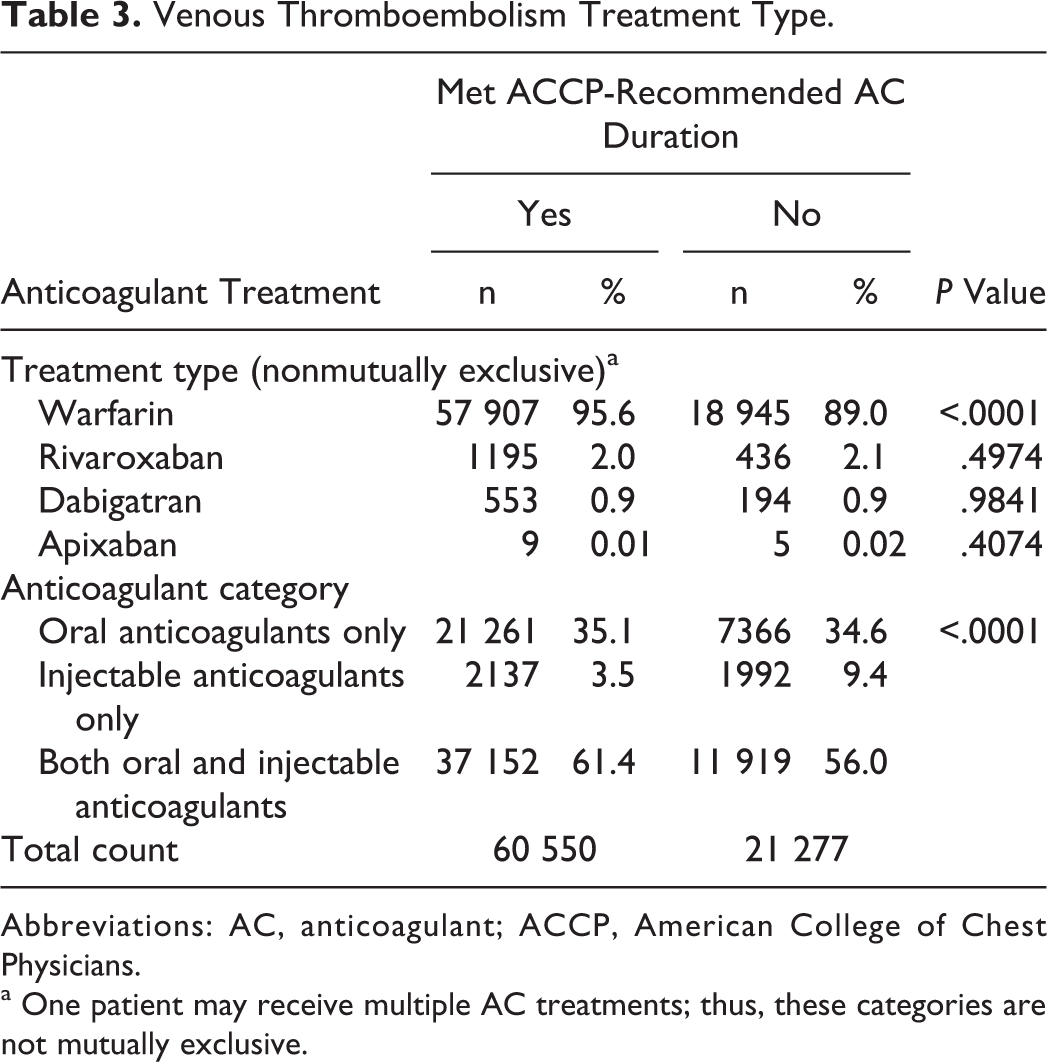
Abbreviations: AC, anticoagulant; ACCP, American College of Chest Physicians.
a One patient may receive multiple AC treatments; thus, these categories are not mutually exclusive.
Comparison of Unadjusted Health-Care Resource Utilization and Costs Between Study Cohorts
The unadjusted all-cause health-care resource utilization during the baseline and follow-up periods for the adherent and nonadherent cohorts is shown in Table 4. Compared to baseline period, the unadjusted mean number of all-cause hospitalizations and days in hospital were increased during the follow-up period for both adherent and nonadherent patients. The amount of increase in the mean number of hospitalizations (0.67 adherent vs 0.82 nonadherent, P < .0001) and the mean number of days in the hospital (4.28 days for adherent vs 6.46 days for nonadherent, P < .0001) was significantly greater for nonadherent patients than adherent patients.
Unadjusted All-Cause Health-Care Resource Utilization Compared Between Adherent and Nonadherent Cohorts.
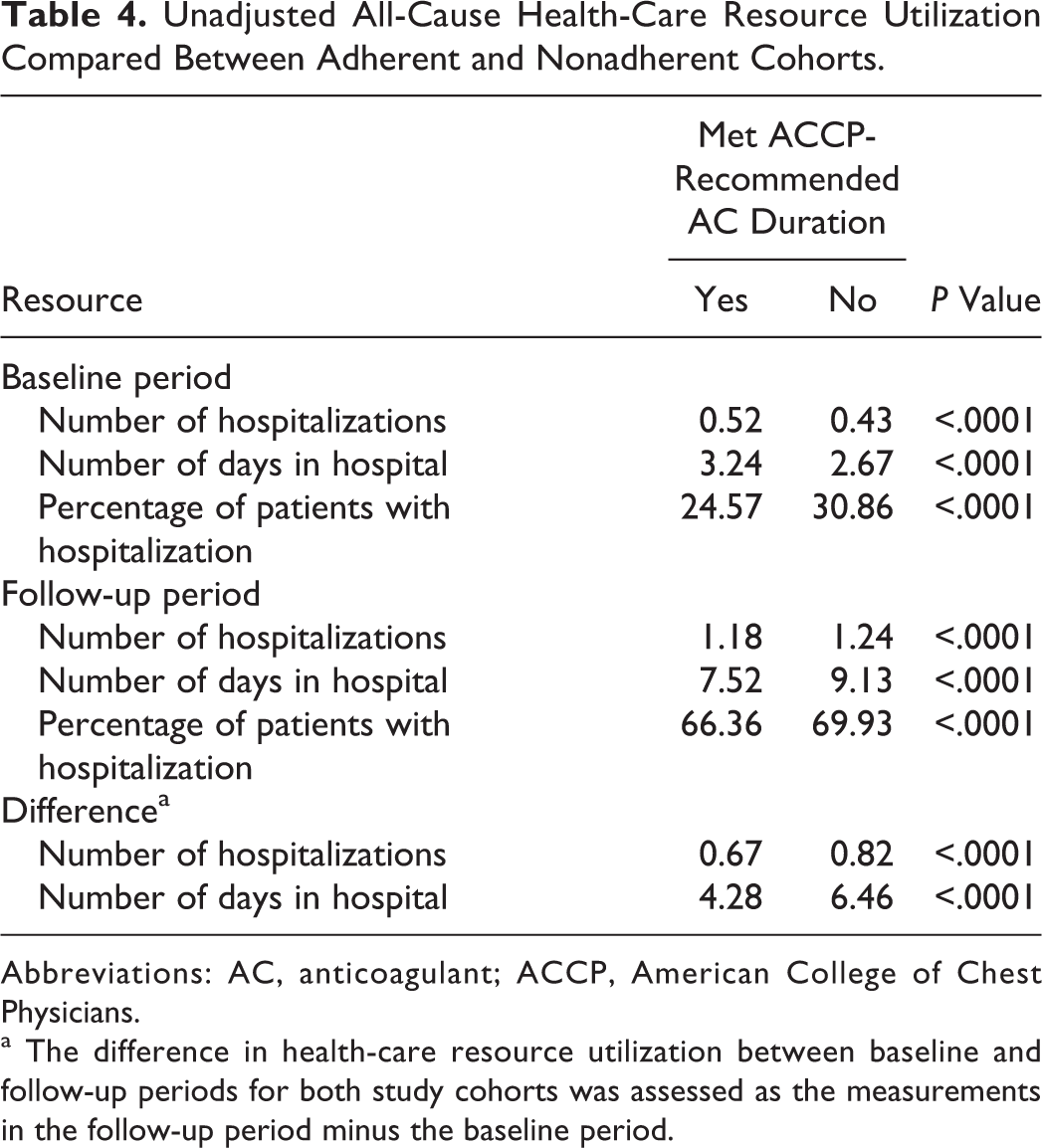
Abbreviations: AC, anticoagulant; ACCP, American College of Chest Physicians.
a The difference in health-care resource utilization between baseline and follow-up periods for both study cohorts was assessed as the measurements in the follow-up period minus the baseline period.
The unadjusted difference in all-cause health-care payments between the follow-up period and baseline period is shown in Figure 2. The unadjusted health-care cost for inpatient, ED visits, outpatient services, and prescription use increased during the follow-up period (Figure 2). The unadjusted mean cost increase for inpatient services was higher for nonadherent patients than adherent patients (mean inpatient US$11 355 adherent vs US$17 217 nonadherent, P < .0001). In contrast, adherent patients had higher increases in the mean cost for outpatient services, office visit, and pharmacy services than nonadherent patients. Overall, the unadjusted mean change from baseline total medical cost, exclusive of pharmacy services, was higher for nonadherent patients than adherent patients (US$20 973 adherent vs US$23 020 nonadherent, P = .0006). Additionally, the unadjusted mean difference in total health-care cost, inclusive of pharmacy services, was numerically lower but not statistically significant in difference between patients who were adherent versus nonadherent (US$23 627 adherent vs US$24 621 nonadherent, P = .1094).
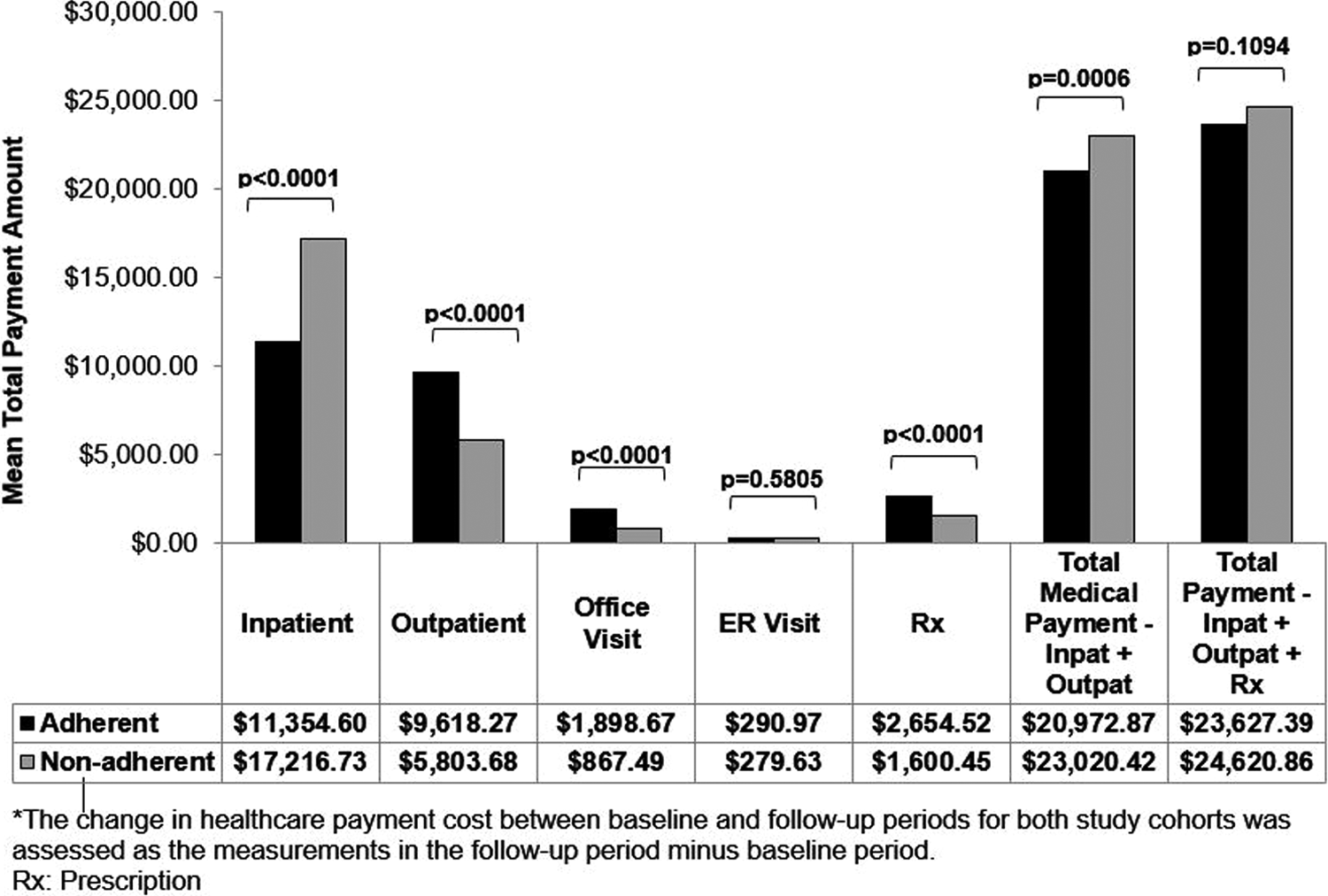
Unadjusted change from baseline health-care payments between adherent and nonadherent patients. Note that the change in health-care payment cost between baseline and follow-up periods for both study cohorts was assessed as the measurements in the follow-up period minus the baseline period.
Unadjusted VTE-related health-care resource utilization and associated costs during the follow-up period for the adherent and non-adherent cohorts are shown in Table 5. Although the mean number of inpatient hospitalizations was higher (0.80 vs 0.76, P < .0001) for adherent patients relative to nonadherent patients, the mean number of days in the hospital (5.06 vs 5.41, P < .0001) was lower, resulting in a significantly lower unadjusted medical payment for VTE-related inpatient services (US$15 047.61 vs US$16 801.28, P < .0001) for adherent patients versus nonadherent patients. However, the number of VTE-related outpatient medical claims during the follow-up period (12.90 vs 9.07, P < .0001) was higher, leading to a higher unadjusted medical payment for outpatient medical services (US$2322.66 vs US$1746.63, P < .0001) for adherent versus nonadherent patients. When inpatient and outpatient services were considered together, adherence to treatment duration was associated with a reduction in unadjusted overall VTE-related medical cost (US$17 370.27 adherent vs US$18 547.91 nonadherent, P < .0001; Table 5).
Follow-Up Period Unadjusted VTE-Related and Bleed-Related Hospital Resource Utilization and Cost: Adherent Versus Nonadherent Patients.
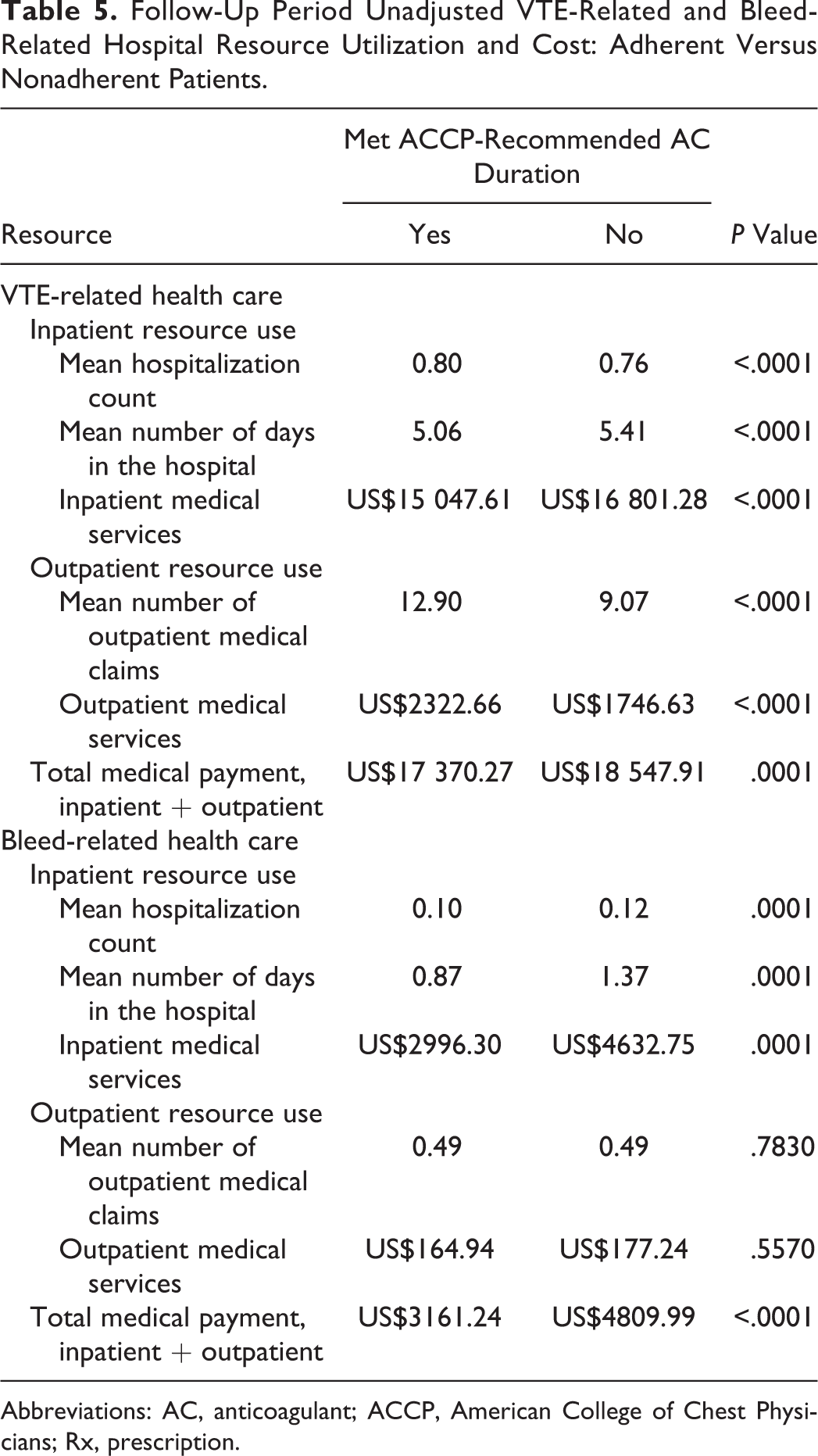
Abbreviations: AC, anticoagulant; ACCP, American College of Chest Physicians; Rx, prescription.
The unadjusted bleed-related health-care resource utilization and associated costs are also shown in Table 5. The mean number of inpatient hospitalizations (0.10 vs 0.12, P < .0001) and the mean number of days in the hospital were lower (0.87 vs 1.37, P < .0001) for adherent patients relative to nonadherent patients, resulting in a significantly lower unadjusted medical payment for bleed-related inpatient services (US$2996.30 vs US$4632.75, P < .0001) for adherent patients versus nonadherent patients. In contrast, the number of bleed-related outpatient medical claims during the follow-up period (0.49 vs 0.49, P = .7830) was similar between the 2 cohorts, which resulted in a numerically lower but not statistically lower unadjusted payment for outpatient medical services (US$164.94 vs US$177.24, P = .5570) for adherent versus nonadherent patients. When inpatient and outpatient services were evaluated together, AC adherence was associated with a reduction in unadjusted overall bleed-related medical cost (US$3161.24 adherent vs US$4809.99 nonadherent, P < .0001).
Comparison of Adjusted Health-Care Resource Use and Costs Between Study Cohorts
After controlling for key patient characteristics, patients in the adherent group had a lower risk of all-cause hospitalizations (AOR: 0.85, confidence interval [95% CI]: 0.82-0.88, P < .0001), bleed-related hospitalizations (AOR: 0.74, 95% CI: 0.69-0.78, P < .0001), and VTE recurrence (AOR: 0.92; 95% CI: 0.88-0.97, P = .0014) in comparison to patients in the nonadherent cohort (Figure 3).
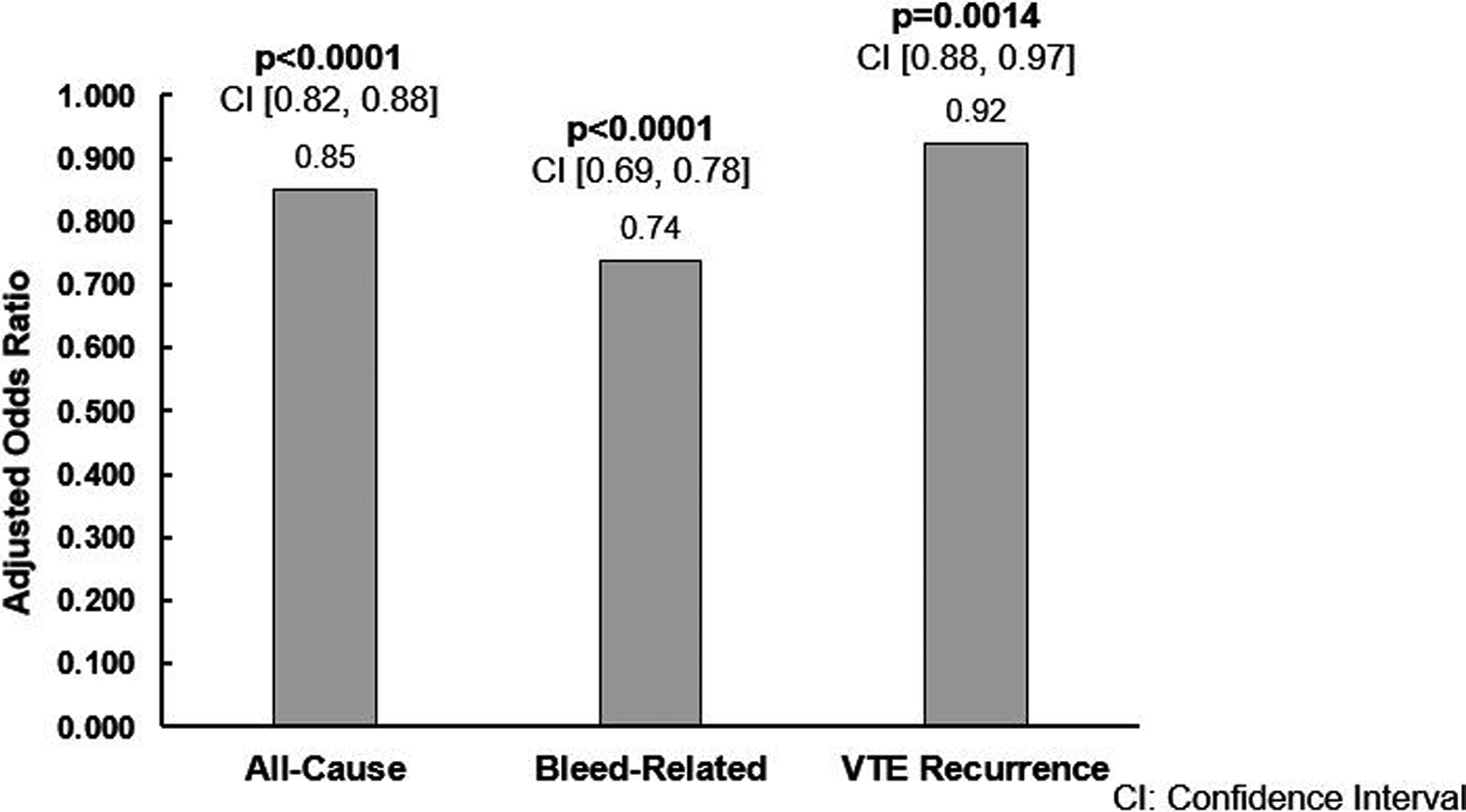
Adjusted odds ratios of all-cause and bleed-related hospitalizations and VTE recurrences of study population, adherent versus nonadherent patients. CI indicates confidence interval.
After controlling for differences in patient demographic and clinical characteristics, adherence to the recommended AC treatment duration was associated with a significant reduction in all-cause total health-care cost (inclusive of pharmacy services; adjusted mean difference = −US$2121, P = .0003), bleed-related medical health-care cost (adjusted mean difference = −US$248, P < .0001), and VTE-related medical health-care cost (adjusted mean difference = −US$2294, P < .0001).
Discussion
This study of over 80 000 patients contributed to the literature by providing data on the real-world adherence to OAC treatment duration among patients with VTE and assessed the impact of treatment duration adherence on clinical and economic outcomes. Approximately a quarter (26% [21 277 of the 81 827]) of patients with VTE did not receive the minimum AC treatment duration as recommended by the ACCP guidelines. Our study suggested that patients with more comorbidities and those who had intermediate and high RIETE bleed risk were more likely to be adherent to the recommended AC treatment duration. In addition, a diagnosis of PE, which is perceived to be a higher risk disease in comparison to DVT within VTE, for the index event or provoked VTE occurred more frequently in the adherent group. Our findings corroborate previous research that showed AC treatment duration adherence varied by risks of VTE recurrence and bleeding. 15 Kaatz et al also showed that patients with intermediate to high bleeding risk were more likely to adhere to AC treatment durations. 15
A correlation was observed between AC adherence status and differences in hospitalization, and our results suggested that adherence to guideline-recommended AC treatment duration may potentially reduce the use of inpatient services by reducing the risk of hospital admissions, all-cause and bleed-related hospitalizations, and the number of days spent in the hospital after an index VTE event. These reductions were associated with lower total health-care cost and medical health-care cost in the adherent cohort compared to patients nonadherent to the recommended treatment duration. Previous data have shown that hospitalization costs are the main driver for the economic burden of VTE, contributing about half of the total annualized costs per patient. 16 Therefore, improving treatment duration adherence may be an effective means to reduce the costs of VTE in the health-care system.
There are several hypotheses for the observed potential correlation between AC adherence status and differences in hospitalizations and associated costs. An evaluation of the breakdown of hospitalizations by primary diagnosis during the follow-up period showed that multiple disease conditions may have contributed to the differences observed in hospitalization rates (data not shown) between the adherent and nonadherent cohorts. The impact of adherence on each of such disease-specific hospitalizations may warrant further evaluation in future studies. Furthermore, the cause of AC discontinuation is not recorded in the claims database, and discontinuation due to the presence of certain comorbidities could lead to a classification bias in nonadherent patients. We evaluated key comorbidities among the adherent and nonadherent cohorts in the follow-up period and observed no significant differences in comorbidities between the 2 study cohorts (data not shown). As the cause of AC discontinuation is not recorded in this database, future research using either patient data registry or electronic medical records may help to further illustrate on this topic.
Additionally, bleed-related health-care resource utilization and associated costs were shown to be higher in the nonadherent group, and there may be several potential hypotheses for this finding. One potential reason may be that patients in the nonadherent group have experienced greater variation in the quality of warfarin control, including potentially more international normalized ratio (INR) fluctuations. Such variations in INR may be associated with higher bleeding rates, which then lead to an increase in health-care resource utilization related to bleeding. However, due to the absence of INR laboratory results in the claims database, we were not able to confirm this plausible explanation. It is also possible that patients with a higher innate bleeding risk not captured by current bleed risk scores experienced greater bleeding adverse events from the ACs and required the discontinuation of AC therapy. While we have attempted to control for the patient bleed risk levels using the RIETE bleed risk score, it is possible that the current bleed risk measurement may not have fully represented the bleeding risk of all patients. Future clinical studies related to the further development of bleed risk measurements and the association of warfarin usage variation among patients with VTE may be warranted.
Adherence to warfarin therapy has been challenging due to the drug–food interactions and the requirement of routine laboratory monitoring. Concern over the risk of bleeding associated with warfarin therapy has been noted as a key reason for underprescribing and nonadherence. Better management of and simplified therapy approaches in AC treatment, including the use of NOACs for secondary thromboprophylaxis that do not require routine monitoring compared to warfarin and have fewer drug–drug and drug–food interactions, have the potential to further increase the real-world adherence to the ACCP guideline treatment duration and potentially reduce hospital admissions and health-care costs associated with VTE.
Study Limitations
As with other retrospective analysis, the results may be subject to biases from other confounding variables that were not available in the database. The cause of AC discontinuation is not recorded in the claim database, thus, future clinical research using either patient data registry or electronic medical records may be warranted. This study was unable to assess mortality differences between the adherent and the nonadherent cohorts because death data are not available in the database evaluated. Additionally, claims data are subject to possible missing data as well as billing and coding errors, which may lead to under- or overestimation of differences in health-care resource utilization and payments. In the retrospective claim database, we can only establish a correlation or association relationship between patient AC adherence status and the differences in hospitalization but cannot establish such causal relationship. This study defined VTE recurrence as either hospitalizations or ED visits associated with a VTE diagnosis; however, some VTE recurrences may be managed entirely by outpatient services and thus may not be captured in the current study. The minimum durations of 3 and 6 months of AC treatment was used as the criteria for adherence to treatment guidelines. However, the appropriate AC therapy duration should be based on individual patient’s clinical characteristics and may differ from such criteria used in the study. Additionally, the NOACs usage may not be well represented in this study as NOACs were available in the US market toward the end of the study time period. The most commonly used OAC was warfarin, thus, the study findings apply primarily to warfarin users.
Conclusion
Approximately one-quarter of the study population with VTE did not receive treatment with AC therapy for the minimum duration as recommended by the ACCP guidelines. Patients who did not receive outpatient AC therapy for the recommended duration had more VTE recurrences, utilized more inpatient services, and had higher all-cause total costs, bleed-related medical costs, and VTE-related medical costs than patients in the adherent cohort. Further studies examining the potential impact for simplified therapy approaches such as the use of NOACs over warfarin in potentially improving long-term AC adherence rates in secondary thromboprophylaxis and health outcomes are warranted.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: A. C. Spyropoulos is a consultant for Daiichi Sankyo, Inc. W. J. Kwong is an employee of Daiichi Sankyo, Inc. R. Preblick was an employee of Daiichi Sankyo, Inc at the time of study. J. Lin and M. Lingohr-Smith are employees of Novosys Health, which has received research funds from Daiichi Sankyo Inc in connection with conducting this study and development of this manuscript.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by Daiichi Sankyo, Inc.
