Abstract
Objective:
We evaluated the modified diagnostic criteria for disseminated intravascular coagulation (DIC), which was published by the Japanese Society of Thrombosis and Hemostasis (JSTH) in 108 patients with suspected infectious DIC.
Material and methods:
The diagnoses of the patients were as follows: DIC (n = 63), pre-DIC (n = 22), and non-DIC (n = 45). The efficacy of the diagnostic criteria for DIC was evaluated using a receiver–operating characteristic analysis.
Results:
Although the area under the curve for global coagulation test (GCT) scores in the diagnosis of “DIC” was high that for the diagnosis of “DIC and pre-DIC” was low, suggesting that the addition of antithrombin (AT), soluble fibrin (SF)/thrombin–AT complex (TAT), and reduced platelet count (PLT) values was required to diagnose “DIC and pre-DIC.” Using GCT score with the AT, SF/TAT, and reduced PLT values, the cutoff value of the DIC score for the diagnosis of “DIC and pre-DIC” was 5 points.
Discussion and conclusion:
The modified JSTH’s diagnostic criteria for DIC, which used the GCT score and the reduced PLT, AT, and TAT/SF values, were useful for diagnosing “DIC and pre-DIC.”
Introduction
Disseminated intravascular coagulation (DIC) is often associated with severe organ failure and a bleeding tendency in various underlying diseases
1
–4
and is reported to be associated with a high rate of mortality.
5
–7
Several diagnostic criteria for DIC have been proposed, including the Japanese Ministry Health, Labor and Welfare (JMHLW) DIC diagnostic criteria,
8
the International Society of Thrombosis and Haemostasis (ISTH) overt-DIC diagnostic criteria,
9
and the Japanese Association for Acute Medicine (JAA) DIC diagnostic criteria.
10
In these 3 diagnostic criteria, global coagulation tests (GCTs), such as the prothrombin time (PT), platelet count (PLT), fibrinogen and fibrin and fibrinogen degradation products (FDP), or
An evaluation of the efficacy of DIC treatment in relation to the JMHLW DIC score at the beginning of treatment showed that it was more effective in pre-DIC patients than in overt-DIC patients and that the prognosis grew progressively worse as the DIC score increased. 13 These findings suggest that an early diagnosis and treatment are essential for improving the outcomes of patients with DIC. It is therefore necessary to change the GCTs and hemostatic molecular markers (such as soluble fibrin [SF], plasmin–plasmin inhibitor [PI] complex [PPIC], and thrombin–antithrombin [AT] complex [TAT]) that are used in order to diagnose DIC at an early stage. 14 Although nonovert DIC was proposed by the ISTH/SSC subcommittee, the criteria for diagnosing early-phase DIC have not been well established. 15 –18
Recently, the Japanese Society of Thrombosis and Hemostasis (JSTH) proposed a modified version of the JMHLW DIC criteria. 19 In the present study, this scoring system was evaluated for diagnosing DIC in infectious patients with and without DIC. Table 1 shows the modified JSTH DIC criteria for patients with infectious diseases.
The Modified Diagnostic Criteria for DIC Established by Japanese Society of Thrombosis and Hemostasis.
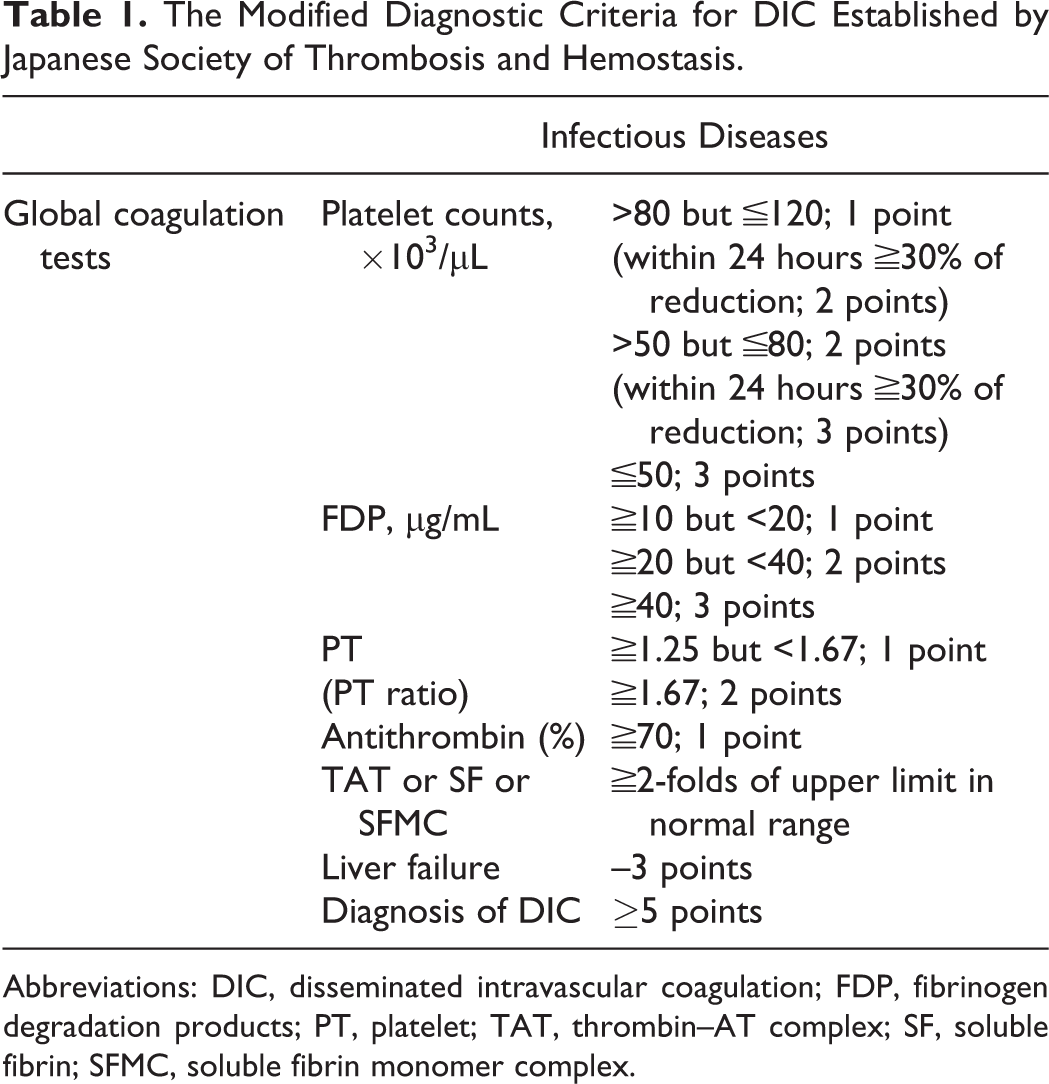

Abbreviations: DIC, disseminated intravascular coagulation; FDP, fibrinogen degradation products; PT, platelet; TAT, thrombin–AT complex; SF, soluble fibrin; SFMC, soluble fibrin monomer complex.
Materials and Methods
The present study included a total of 108 patients having infectious diseases with suspected DIC who were treated from January 1, 1989, to December 31, 2014. Sixty-three patients were diagnosed according to the JMHLW diagnostic criteria, 8 and it was possible to determine the presence of hemostatic abnormalities within 7 days before the onset of DIC in 22 patients; these were considered to be pre-DIC cases. 20 Forty-five patients did not develop DIC during their clinical course (non-DIC; Table 2). The study protocol was approved by the Human Ethics Review Committee of the Mie University School of Medicine. This was carried out in accordance with the principle of the Declaration of Helsinki. The cases in which one or more of the following laboratory findings were present were included in the following study: a PLT of ≦ 120 × 103 per/μL; an FDP value of ≧ 10 μg/mL; a fibrinogen level of ≦ 1 g/L; and a PT ratio of ≧ 1.25.
Participants.a
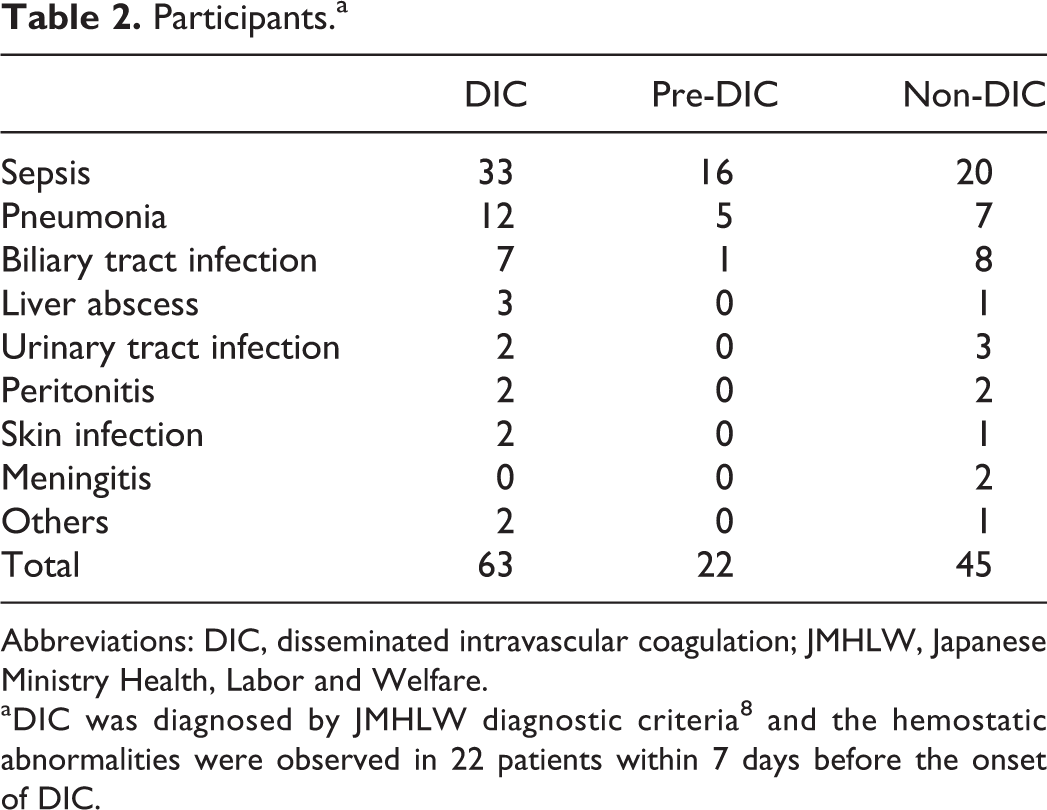
Abbreviations: DIC, disseminated intravascular coagulation; JMHLW, Japanese Ministry Health, Labor and Welfare.
aDIC was diagnosed by JMHLW diagnostic criteria 8 and the hemostatic abnormalities were observed in 22 patients within 7 days before the onset of DIC.
The PT, fibrinogen, PLT,
Statistical Analysis
The data are expressed as the median (25th to 75th percentile). The differences between the groups were examined for statistical significance using the Mann-Whitney U test. The efficacy of the DIC diagnostic criteria was evaluated by a receiver–operating characteristic (ROC) analysis. P values of ≦.05 were considered to indicate statistical significance. All of the statistical analyses were performed using the Stat Flex, software program (version 6; Artec Co Ltd, Osaka, Japan).
Results
There were no significant differences in the age or sex of the patients with DIC, pre-DIC, and non-DIC as diagnosed by the JMHLW DIC diagnostic criteria (Table 3). The JMHLW DIC, ISTH overt DIC, and JAA DIC scores were 7.0; 7.0 to 8.0, 5.0; 4.0 to 5.0, and 5.0; 4.3 to 7.0, respectively, in the DIC group as diagnosed by the JMHLW DIC diagnostic criteria; 5.0; 4.0 to 6.0, 3.0; 2.0 to 4.0, and 4.0; 3.0 to 4.0, in the pre-DIC group as diagnosed by the JMHLW DIC diagnostic criteria; and 4.0; 3.0 to 5.0, 2.0; 2.0 to 3.0, and 3.0; 2.0 to 4.0, respectively, in the non-DIC group (Table 3). The levels of hemostatic markers are shown in Table 4. Although the values of PT ratio, PLT, FDP, AT, TAT, and SF/SFMC in the patients with DIC differed significantly from those in the non-DIC patients, there were no significant differences between the pre-DIC and the non-DIC patients. The mortality rate was higher in the patients with DIC and pre-DIC patients than in the non-DIC patients. The rate of resolution from DIC was similar in both the DIC and the pre-DIC groups. In the diagnosis of DIC in patients without pre-DIC (Table 5), the cutoff value of the DIC score was decided according to the cross point between the sensitivity curve and the 1-specificity curve (Figure 1). The cutoff value of the DIC score was 4 in “GCT,” “GCT + reduced PLT,” “GCT + SF/TAT,” and “GCT + reduced PLT + SF/TAT,” and was 5 in “GCT + AT,” “GCT + reduced PLT + AT,” “GCT + AT + SF/TAT,” and “GCT + reduced PLT + AT + SF/TAT.” The lowest area under the curve (AUC) value was 0.956 in “GCT and reduced PLT” and the highest AUC value was 0.984 in “GCT + reduced PLT + AT + SF/TAT” (Figure 2A). The highest sensitivity was 98.4 in “GCT + SF/TAT” and the highest specificity was 98.0 in “GCT + AT.” The lowest odd’s ratio was 55.0 in “GCT” and the highest odd’s ratio was 649 in “GCT + reduced PLT + AT + SF/TAT.”
DIC, pre-DIC, and non-DIC Diagnosed by Japanese Ministry of Health, Labor and Welfare Diagnostic Criteria.
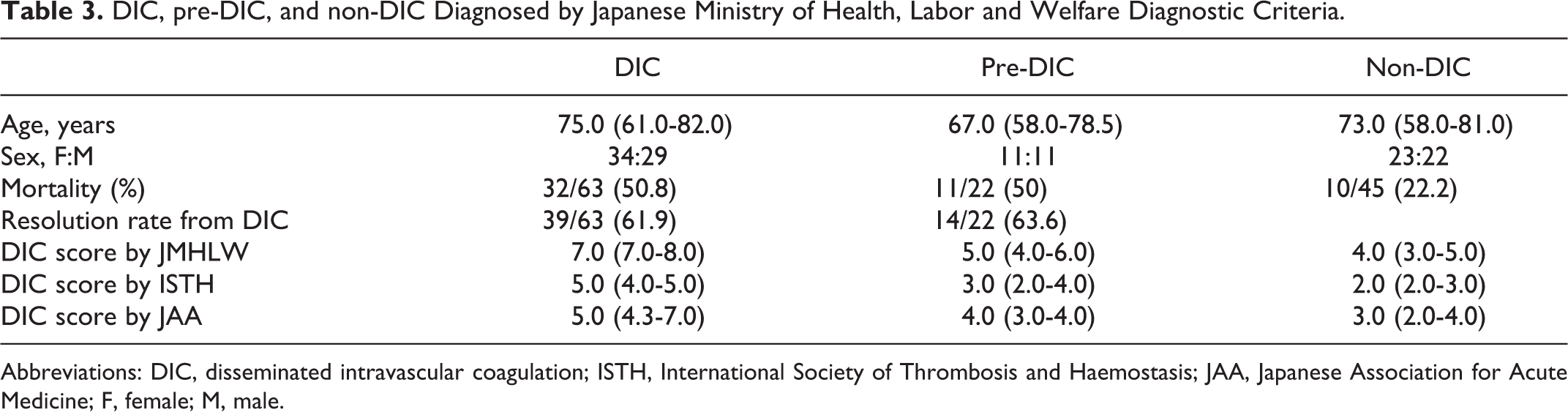
Abbreviations: DIC, disseminated intravascular coagulation; ISTH, International Society of Thrombosis and Haemostasis; JAA, Japanese Association for Acute Medicine; F, female; M, male.
Hemostatic Markers in DIC, Pre-DIC, and Non-DIC.
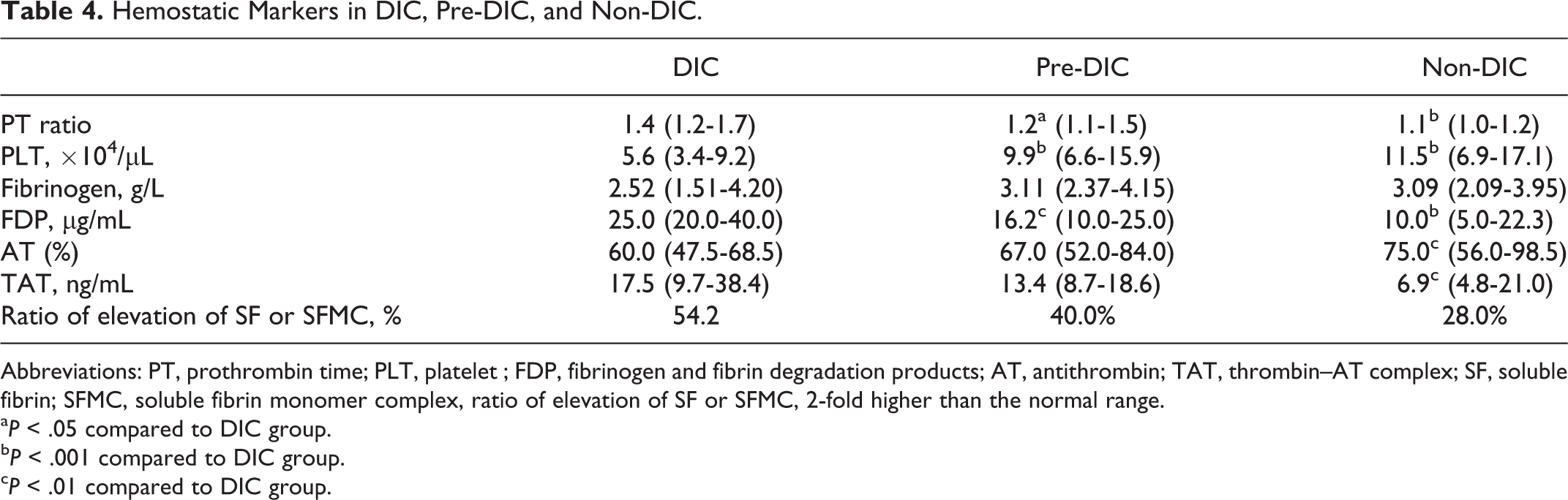
Abbreviations: PT, prothrombin time; PLT, platelet ; FDP, fibrinogen and fibrin degradation products; AT, antithrombin; TAT, thrombin–AT complex; SF, soluble fibrin; SFMC, soluble fibrin monomer complex, ratio of elevation of SF or SFMC, 2-fold higher than the normal range.
a P < .05 compared to DIC group.
b P < .001 compared to DIC group.
c P < .01 compared to DIC group.
Relationship Between Diagnostic Criteria and Diagnostic Ability for DIC versus non-DIC.
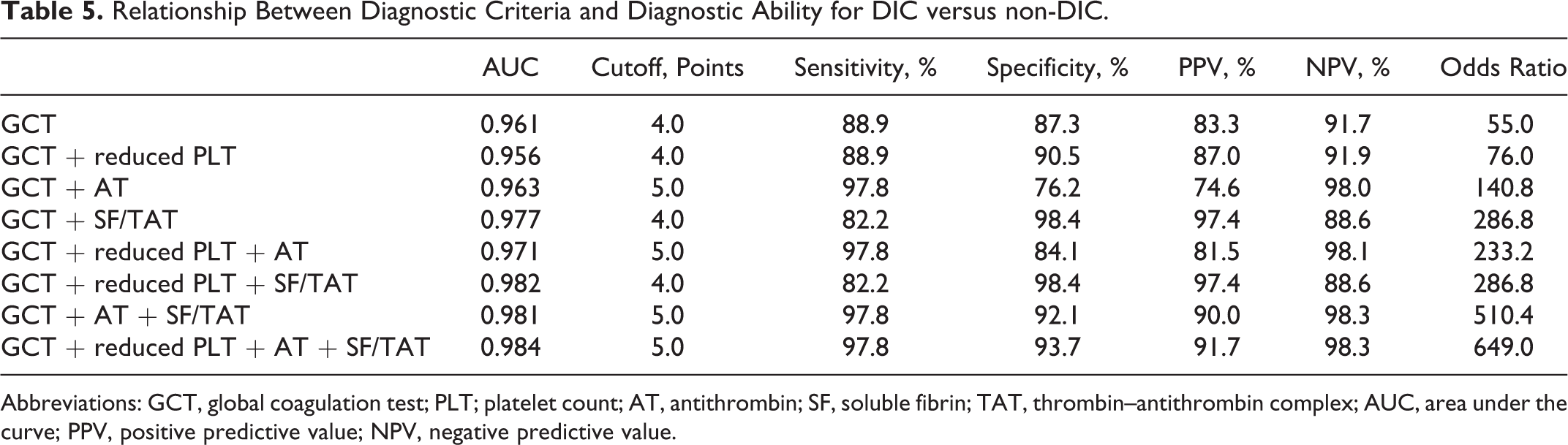
Abbreviations: GCT, global coagulation test; PLT; platelet count; AT, antithrombin; SF, soluble fibrin; TAT, thrombin–antithrombin complex; AUC, area under the curve; PPV, positive predictive value; NPV, negative predictive value.
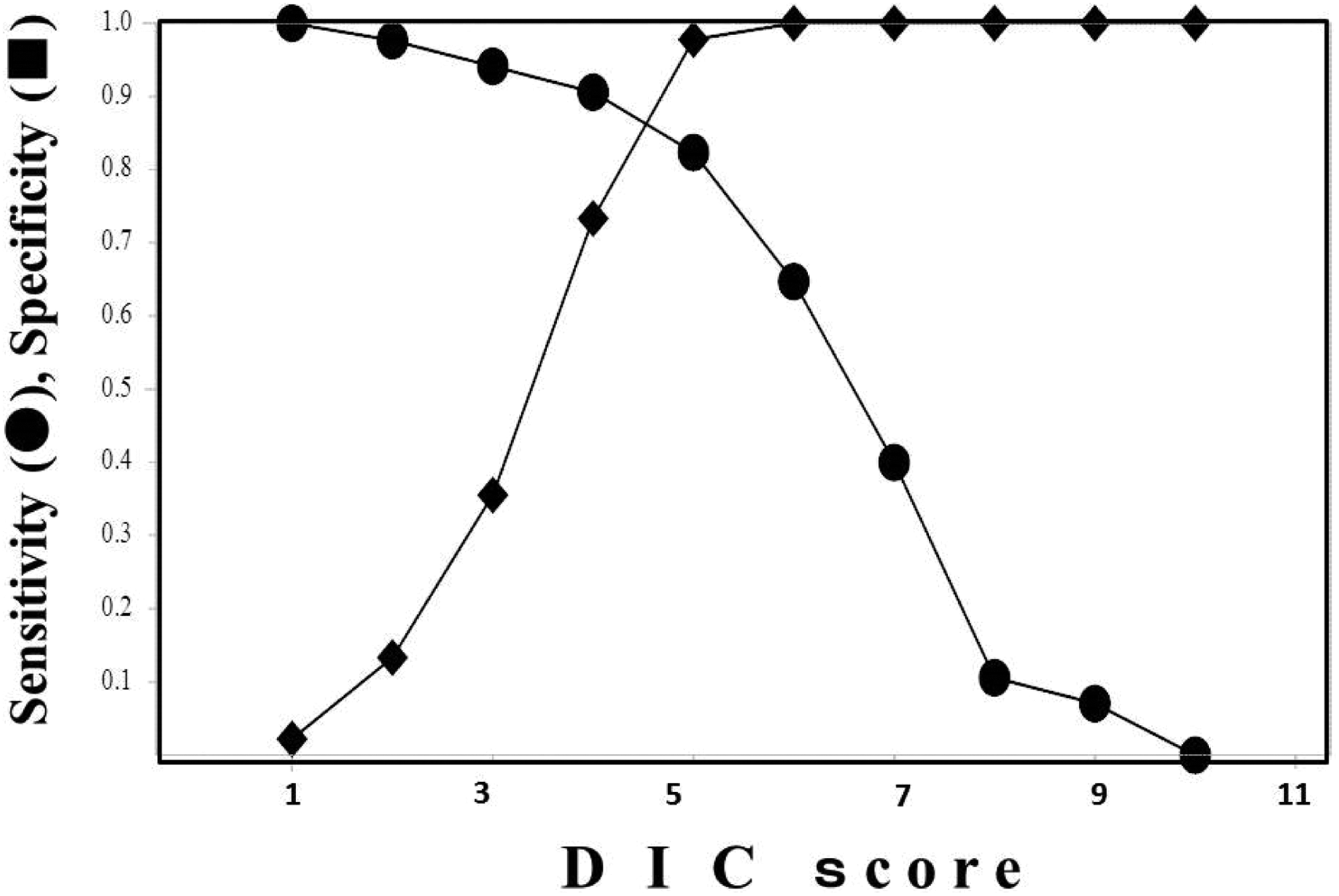
The sensitivity curve and the 1-specificity curve for disseminated intravascular coagulation (DIC). The cutoff value of the DIC score for the diagnosis of DIC was decided according to the cross-point between the sensitivity curve and the 1-specificity curve.
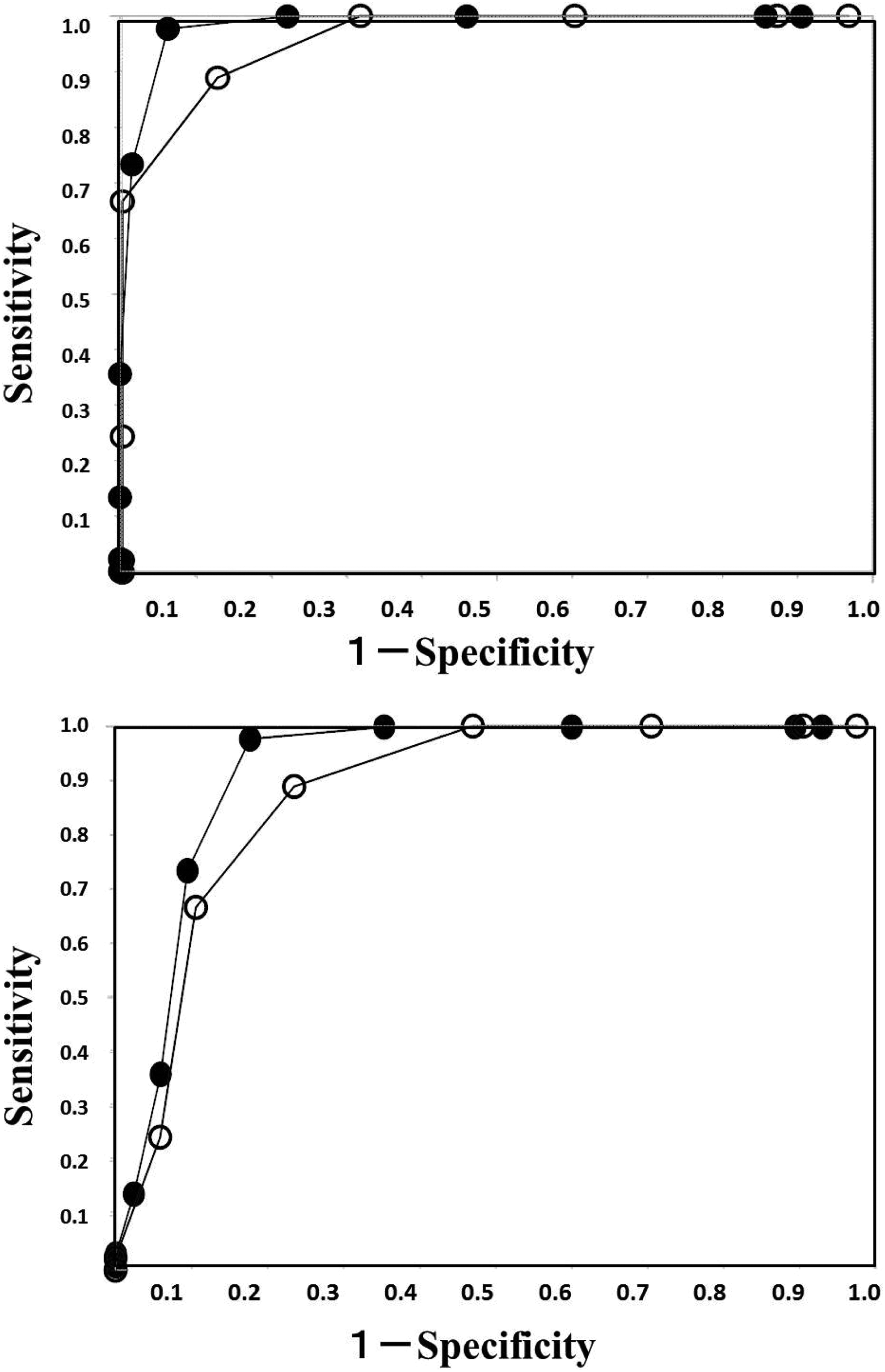
The receiver–operating characteristic (ROC) analysis for disseminated intravascular coagulation (DIC; A) and for “DIC and pre-DIC.” (B) Open circles, global coagulation test (GCT); closed circles, GCT + reduced platelet count + antithrombin (AT) + soluble fibrin/thrombin–AT complex.
In the diagnosis of “DIC and pre-DIC” (Table 6), the cutoff value of the DIC score for “DIC and pre-DIC” was the same as that for “DIC.” The lowest AUC value was 0.882 in “GCT” and the highest AUC value was 0.922 in “GCT + reduced PLT + AT + SF/TAT” (Figure 2A). The highest sensitivity was 97.8 in “GCT + reduced PLT + AT + SF/TAT” and the highest specificity was 98.8 in “GCT + AT + SF/TAT.” The lowest odd’s ratio was 26.0 in “GCT” and the highest odd’s ratio was 205.3 in “GCT + reduced PLT + AT + SF/TAT.” Both the AUC value and the odd’s ratio were higher in the diagnosis of “DIC” than in the diagnosis of “DIC and pre-DIC.”
Relationship Between Diagnostic Criteria and Diagnostic Ability for “DIC and pre-DIC” Versus non-DIC.
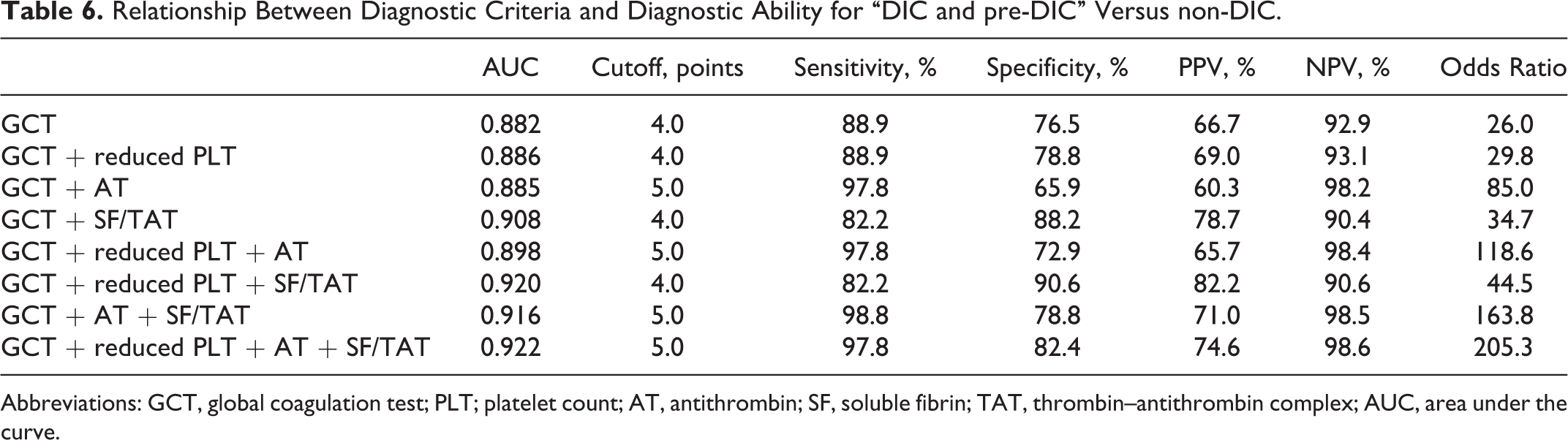
Abbreviations: GCT, global coagulation test; PLT; platelet count; AT, antithrombin; SF, soluble fibrin; TAT, thrombin–antithrombin complex; AUC, area under the curve.
Discussion
Suspected DIC patients were classified into 3 groups: overt-DIC, pre-DIC, and negative DIC (non-DIC). A previous report 13 showed that the outcome of DIC was improved by early treatment. Although the early diagnosis of DIC is considered to be important for improving its prognosis, the diagnostic criteria for pre-DIC have not been established. Previously, several reports 3,13 referred to the state within 1 week before the onset of DIC as pre-DIC. In the present study, there were no significant differences in any markers in the pre-DIC and non-DIC group. The ISTH guidance for the diagnosis and treatment of DIC recommends the diagnosis of DIC by a scoring system rather than by a single marker. 11 The JAA proposed DIC diagnostic criteria that use GCT scores to diagnose the early phase of DIC 10 ; they show high sensitivity but low specificity for DIC. 12 Several modified diagnostic criteria for nonovert-DIC have been proposed that use GCT scores, hemostatic molecular marker levels, and the change in GCT values 15 –18 ; however, these have not been sufficiently evaluated.
In the DIC group, which was diagnosed according to the JMHLW DIC diagnostic criteria, the median ISTH overt DIC score and the JAA DIC score using the GCT score were 5.0 and 5.0, respectively. In addition, GCT score displayed a high AUC value in the ROC analysis, suggesting that GCTs are useful in the diagnosis of overt-DIC. In contrast, in the diagnosis of DIC in patients with pre-DIC, the AUC and odd’s ratio were low in the GCT score. The addition of AT reduced PLT and SF/TAT increased the AUC and odd’s ratio, suggesting that, in combination with hemostatic molecular markers, the change in the PLT and GCT score values could increase both the sensitivity and the specificity in the diagnosis of both DIC and early DIC (DIC + pre-DIC). An ROC analysis also showed that the adequate cutoff value for the diagnosis of DIC was 5 points instead of the 6 points proposed by the JSTH. This is because the JSTH committee for the DIC diagnostic criteria only focused on the suitability of each hemostatic marker for the diagnosis of DIC, and not on the scoring system for the DIC diagnostic criteria, which use a combination of hemostatic markers, the GCT score, and a reduced PLT value.
In conclusion, the modified JMHLW diagnostic criteria for DIC, which use the GCT score, a reduced PLT value, and the hemostatic molecular marker levels, can be used to diagnose both overt-DIC and pre-DIC.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported in part by a Grant-in-Aid from the Ministry of Health, Labour and Welfare of Japan for Blood Coagulation Abnormalities and from the Ministry of Education, Culture, Sports, Science and Technology of Japan.
