Abstract
The aim of this study is to evaluate the effect of these new generation hemostatic agents on early-stage soft tissue healing of warfarin-treated rats by measuring the tissue factor (TF) activities. Rats in the warfarin group were treated intraperitonally with 0.1 mg/kg warfarin, and rats in the control group were treated with 1 mL/kg saline. All rats had 3 incisions on dorsal dermal tissue applied Celox, Ankaferd Blood Stopper (ABS), or no hemostatic agent. Six rats from each group were killed on day 4, and the other 6 were killed on day 8. Prothrombin time (PT) and TF activities were evaluated, respectively. Both the hemostatic agents positively affected the hemostasis. Warfarin treatment increased the PT levels as expected. Celox-treated dermal tissues had higher TF activity when compared to ABS-treated ones. The ABS affected the early-stage healing positively in clinical aspect, whereas Celox was more effective on hemostasis by means of increasing TF activities.
Introduction
The aim of oral anticoagulant therapy is to reduce blood coagulability to an optimal therapeutic range within which the patient is provided protection from thromboembolic events. This is achieved at the cost of a minor risk of spontaneous bleeding. 1 Dental extractions are performed frequently on patients who receive treatment with an oral anticoagulant. In the past, the anticoagulant treatment has been suggested to be stopped or reduced for several days before a dental extraction. Today, thanks to local hemostasis achieved with gelatin sponge and sutures, dental extractions can be performed in patients treated with oral anticoagulants without interruption or diminution of the medication. 2
Warfarin is one of the coumarin group of drugs and is prescribed for various conditions. It blocks the formation of prothrombin and factors II, VII, IX, and X, which are involved in both the extrinsic and the common coagulation pathways and prevents the metabolism of vitamin K to its active form that is needed for the synthesis of these factors. Other vitamin K-dependent proteins inhibited by warfarin include proteins C and S that are involved in the fibrinolytic system. Because coumarins bind strongly to plasma proteins, warfarin has a half-life of 36 hours and acts slowly. The activity of warfarin is expressed as the international normalized ratio, which is the standard introduced by the World Health Organization 20 years ago. It is a prothrombin ratio obtained by dividing the prothrombin time (PT) by the laboratory control PT. The risk of operative or postoperative bleeding must be balanced against the risk of thromboembolism in patients in whom warfarin is interrupted. 3,4
Ankaferd Blood Stopper (ABS; Ankaferd Health Products Ltd, Istanbul, Turkey) is a standardized unique combined medicinal plant extract, which has been approved in the management of postsurgery dental bleeding and external hemorrhage in Turkey. 5 The ABS is a standardized extract from the following plants: Thymus vulgaris, Glycyrrhiza glabra, Vitis vinifera, Alpinia officinarum, and Urtica dioica. The basic mechanism of action of ABS is through the formation of encapsulated protein network providing focal points for vital erythrocytes to aggregate on. The ABS-induced protein network formation involves blood cells, particularly erythrocytes, without affecting the physiological individual coagulation systems. 6,7
Celox (Medtrade Products Ltd, Crewe, United Kingdom) is made of chitosan (poly-N-acetyl glucosamine) that is a biodegradable, nontoxic, and complex carbohydrate derivative of chitin. Specifically, chitosan appears to function independent of platelets and normal clotting mechanisms as currently understood. 8 Chitosan’s putative capacity to induce clot formation in the absence of coagulation factors or platelets in heparinized rats could prove to be useful in patients with coagulopathies or those who are therapeutically anticoagulated. 9
Tissue factor (TF, thromboplastin factor III) is a low-molecular-weight glycoprotein responsible for the initiation of the coagulation cascade. The TF forms, with factor VII/VIIa, a complex that directly converts factor X and also factor IX to their active form. The TF is considered to be the major regulator of normal hemostasis and thrombosis and plays a critical role in hemostasis of all the tissues. Moreover, various tissues and body fluids have been known to have TF activity. 10–12
To our knowledge, there is no study in the literature that evaluates and compares the TF activities of the skins of ABS- or Celox-treated rats in early-stage soft tissue healing. Therefore, the aim of this study is the evaluation and comparison of the effects of 2 brand new local hemostatic agents on the TF activities of dorsal skin tissues in warfarin-treated rats, in early-stage soft tissue healing.
Materials and Methods
Animals and Treatment
We operated a total of 24 male Wistar-albino rats weighing 280 to 560 g. The study group included 12 warfarin-treated rats and 12 control group rats. Animals were obtained from Experimental Animals Research Center, Kocaeli University, (Kocaeli, Turkey) surgeries, and after care have also been performed in this unit. The study was approved by Kocaeli University Animal Experiments Local Ethics Committee.
Rats in the control and study groups were injected 1 mL/kg intraperitonal (ip) saline and 0.1 mg/kg ip warfarin (Coumadin Tablet 5 mg; Zentiva Eczacıbaşı İlaç Sanayi ve Ticaret A.Ş., Istanbul), respectively, for 3 days before surgery, stopped on the day of surgery, and continued postoperatively from first day until the day of killing. Six rats in the control and study groups have been killed 4 days after the surgery, and the remaining 6 were killed 8 days after surgery. The rats were killed by high-dose anesthetics.
After the achievement of aseptic and antiseptic conditions, the rats were anesthetized with 90 mg/kg ketamin (Ketalar; Pfizer, Istanbul, Turkey) and 10 mg/kg xylazine (Rompun Bayer HealthCare, Leverkusen, Germany). One rat in the control group died due to a complication of anesthesia; therefore, the study was completed with 23 rats.
As soon as shaving the dorsal skins, 3 incisions were made on all the 23 rats. Incisions were 2 cm long and 2 cm far from each other, perpendicular to the head–tail direction. On the day of surgery, 2 × 20 mm2-sized tissue samples were taken from the margin of the wound for the determination of TF activity. Before suturing, 0.04 g of chitosan granules have been applied to the first wound, and 0.25 mL of ABS has been applied to the last wound. The wound in the middle has been sutured without any hemostatic agent (no hemostatic agent administered [NHAA]) and left to heal naturally. This protocol has been followed in both the control and the study groups.
On the day of killing, the whole dorsal skin including the healing wound area has been totally excised. Three different wound healing areas (chitosan-NHAA-ABS) have been separated from each other and prepared for the determination of TF activity. The TF activity was performed at Department of Basic Medical Sciences, Faculty of Dentistry, Marmara University (Istanbul, Turkey).
Immediately after killing, 2 mL of intracardiac blood sample was taken from all the experimental animals and centrifuged to gain plasma for PT tests. The PT tests were performed in Düzen Norwest Veterinary Laboratories (Ankara, Turkey).
Tissue Sampling
All the skin samples were excised and splitted into 3 pieces so that each wound area had ABS-, Celox-, or nonhemostatic agent-treated regions. All pieces were stored at −94°C and transferred to −24°C 2 days before performing tests. On the day of TF activity determination, the thawed samples were washed with saline, cleaned from blood and veins carefully, dried with filter paper, and wet weights were recorded.
Determination of TF Activity
The skin samples were homogenized in 0.9% NaCl to obtain 10% tissue homogenates. The TF activities of tissue homogenates were evaluated according to Quick 1-stage method using pooled plasma collected from healthy participants. The TF activity was performed by mixing 0.1 mL of tissue homogenate with 0.1 mL of 0.02 mol/L CaCl2, with the clotting reaction being started on addition of 0.1 mL of plasma. All reagents were brought to the reaction temperature (37°C) before admixture. Since the clotting time is inversely proportional to the TF activity, the lengthening of the clotting time is a manifestation of decreased TF activity. 13
Statistical Analysis
All statistical analysis was performed using Statistical Package for the Social Sciences16.0 (SPSS ) software program. The results were expressed as ±standard deviation. Differences between the groups were evaluated using Kruskal-Wallis test. Student t test was used for the comparison of the quantitative data that doachieve 2 independent group’s parametric test possibilities. Mann-Whitney U test was used for the comparison of the quantitative data that does not achieve 2 independent group’s parametric test possibilities. P values less than .05 were considered statistically significant.
Results
Comparison of the TF Activities of Tissue Samples Taken During Surgical Procedure Before any Hemostatic Agent Administration in the Control and the Warfarin Groups
The TF activity between the 2 groups did not differ significantly (P > .05; Table 1).
The TF activities of the Control and the Warfarin Groups’ Tissue Samples Taken During Surgical Procedure Before Hemostatic Agent Administration (Day 0).a
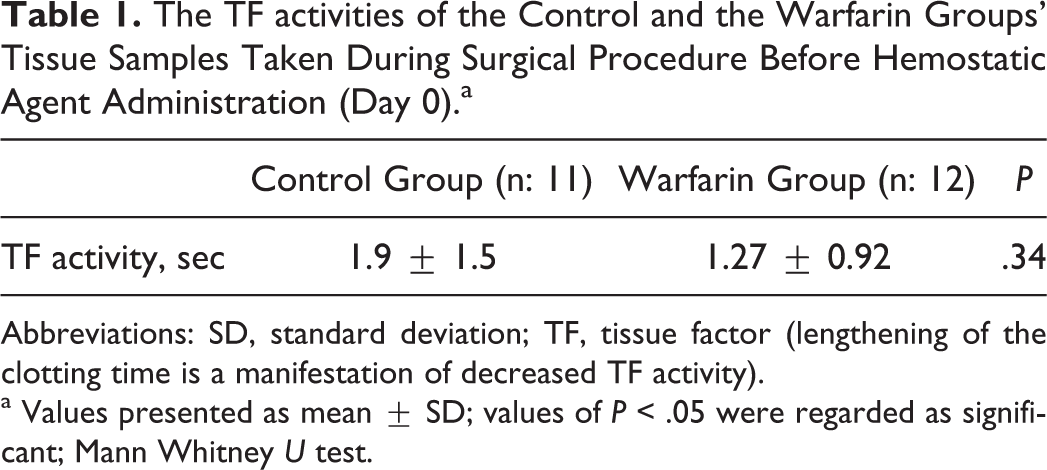

Abbreviations: SD, standard deviation; TF, tissue factor (lengthening of the clotting time is a manifestation of decreased TF activity).
a Values presented as mean ± SD; values of P < .05 were regarded as significant; Mann Whitney U test.
Prothrombin Time Comparison
The PT values were analyzed on the fourth and eighth days. In the control group, no change was observed in PT values on days 4 and 8; however, in the warfarin group, the PT values significantly increased on day 8 when compared to day 4 (P = .005). The PT values of the warfarin group were significantly longer than the control group both on the fourth and on the eighth days (P = .014, P = .0001; Table 2).
The PT Comparison on the 4th and 8th Days.a
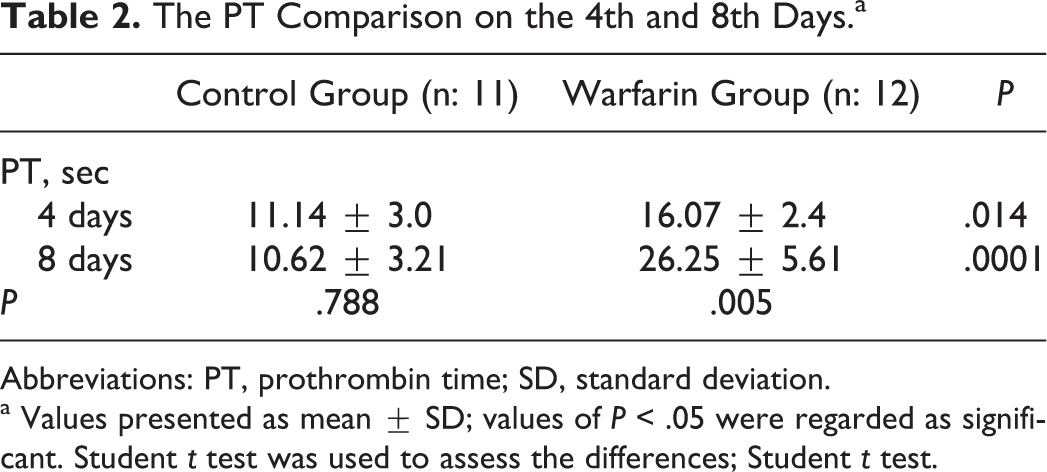
Abbreviations: PT, prothrombin time; SD, standard deviation.
a Values presented as mean ± SD; values of P < .05 were regarded as significant. Student t test was used to assess the differences; Student t test.
Comparison of the TF Activities of Tissue Samples Taken on the Fourth Day After Hemostatic Agent Administration in the Control and the Warfarin Groups
No significant difference has been noted between the groups on the fourth day (P > .05; Table 3).
The TF Activity Comparison of Tissue Samples After Heamostatic Agent Administration on the 4th Day.a
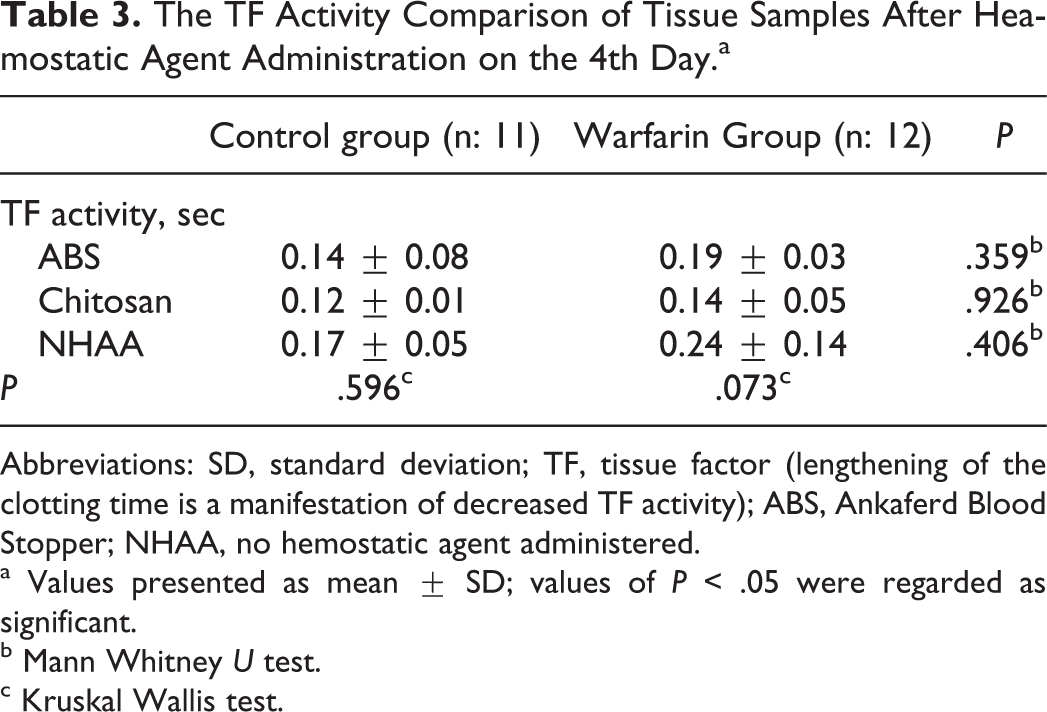
Abbreviations: SD, standard deviation; TF, tissue factor (lengthening of the clotting time is a manifestation of decreased TF activity); ABS, Ankaferd Blood Stopper; NHAA, no hemostatic agent administered.
a Values presented as mean ± SD; values of P < .05 were regarded as significant.
b Mann Whitney U test.
c Kruskal Wallis test.
Comparison of the TF Activities of Tissue Samples Taken on the Eighth Day After Hemostatic Agent Administration in the Control and the Warfarin Groups
No significant difference has been noted between the control and the warfarin groups on the eighth day for ABS, chitosan, or NHAA tissue samples (Table 4).
The TF Activities Comparison of Tissue Samples After Hemostatic Agent Administration on the 8th Day.a
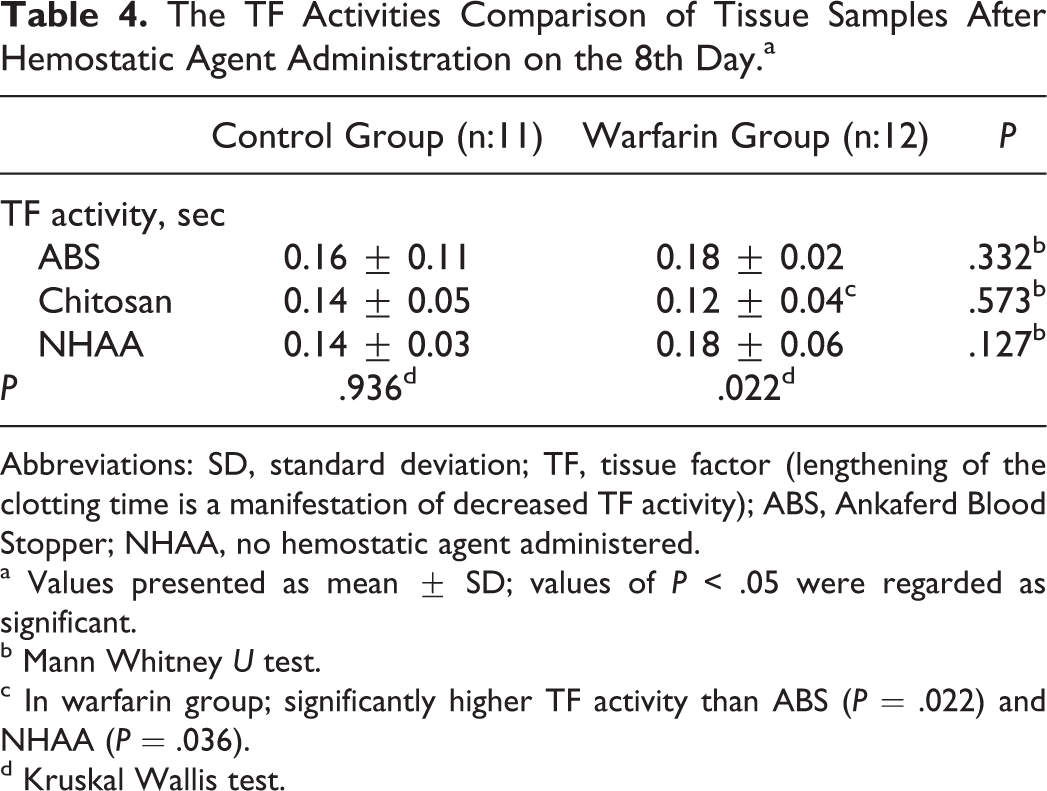
Abbreviations: SD, standard deviation; TF, tissue factor (lengthening of the clotting time is a manifestation of decreased TF activity); ABS, Ankaferd Blood Stopper; NHAA, no hemostatic agent administered.
a Values presented as mean ± SD; values of P < .05 were regarded as significant.
b Mann Whitney U test.
c In warfarin group; significantly higher TF activity than ABS (P = .022) and NHAA (P = .036).
d Kruskal Wallis test.
In the control group, no significant difference was detected in the TF activities of the tissue samples taken on the eighth day. On the other hand, TF activities of the tissues were significantly different in the warfarin group (P = .022). Chitosan-administered tissue samples had higher TF activity than ABS-administered or NHAA tissue samples (P = .022 and P = .036, respectively; Table 4).
Comparison of TF Activities of Tissue Samples Taken on Days 0, 4, and 8
All tissue samples’ TF activities increased from days 0 to 4,and this increased value remained until day 8 in both the control and the warfarin groups (Table 5).
The TF Activities of Tissue Samples Taken on Days 0, 4, and 8.a,b
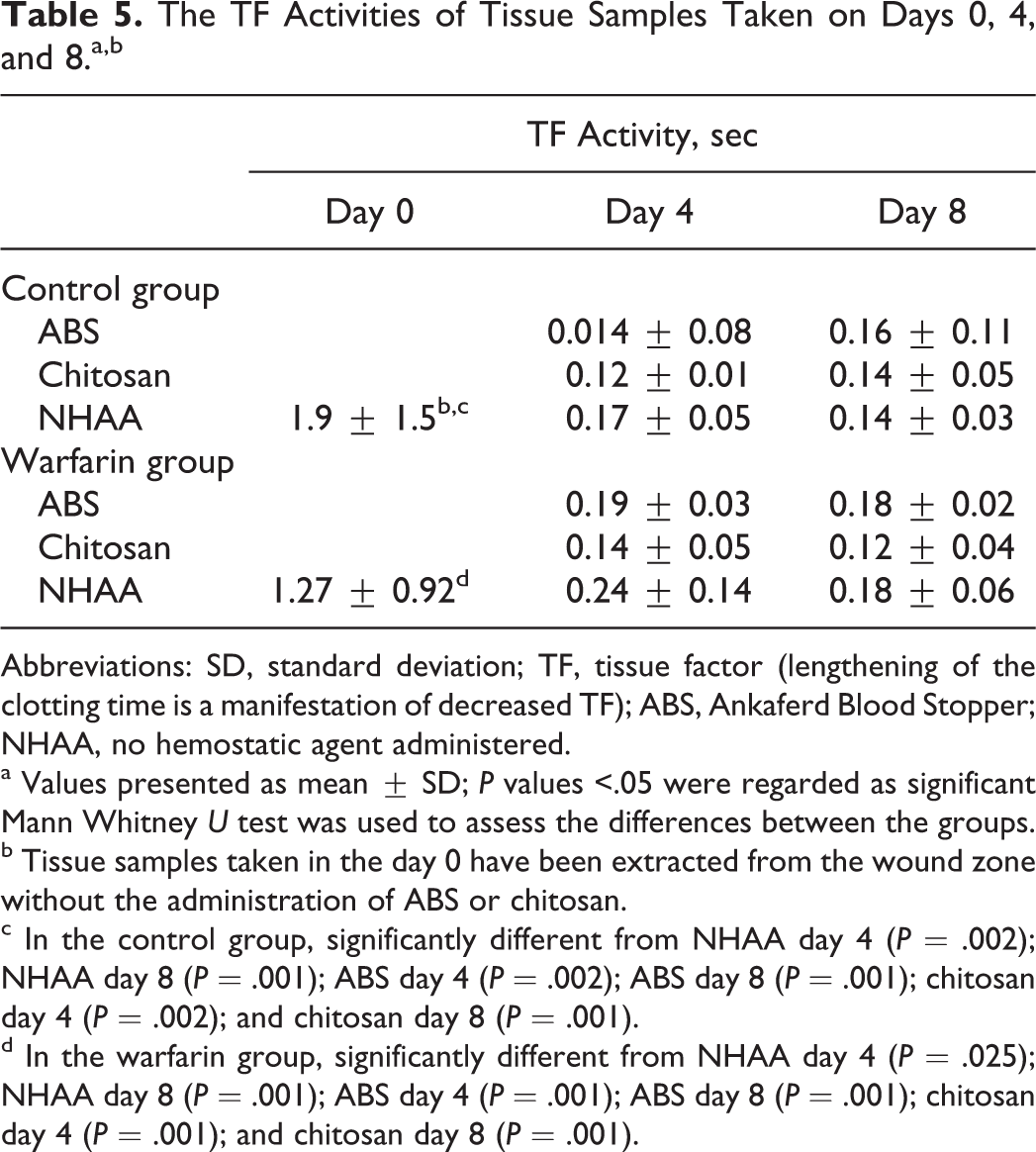
Abbreviations: SD, standard deviation; TF, tissue factor (lengthening of the clotting time is a manifestation of decreased TF); ABS, Ankaferd Blood Stopper; NHAA, no hemostatic agent administered.
a Values presented as mean ± SD; P values <.05 were regarded as significant Mann Whitney U test was used to assess the differences between the groups.
b Tissue samples taken in the day 0 have been extracted from the wound zone without the administration of ABS or chitosan.
c In the control group, significantly different from NHAA day 4 (P = .002); NHAA day 8 (P = .001); ABS day 4 (P = .002); ABS day 8 (P = .001); chitosan day 4 (P = .002); and chitosan day 8 (P = .001).
d In the warfarin group, significantly different from NHAA day 4 (P = .025); NHAA day 8 (P = .001); ABS day 4 (P = .001); ABS day 8 (P = .001); chitosan day 4 (P = .001); and chitosan day 8 (P = .001).
Discussion
The most often and emergency care-needed complication in oral surgery is bleeding. Hemorrhagic diathesis is experienced with some patient groups under anticoagulant therapy. It becomes difficult to achieve the hemostasis without any positive pressure to the area, saturation, or local hemostatic agents. 14–17 Therefore, local hemostatic agents are usually preferred to control bleeding, to act as a matrix to organize the clot by filling bony cavities, and to prevent from secondary bleeding.
Physiologic wound healing involves a complex interaction between cells, mediators, growth factors, and cytokines. The cascade of events starts with activation of the procoagulant pathway and recruitment of inflammatory cells and is followed by a phase of cellular proliferation and tissue repair/resolution of the injury. Recent studies18–20 indicate that TF, the major initiator of the extrinsic coagulation cascade, is involved in all phases of the host response to wounding, implying a likely central role for TF in wound healing. The TF is found in the adventitia of blood vessels, organ capsules, and the epithelium of skin and internal mucosae. Moreover, various tissues and body fluids have been known to have TF activity. 21–23
In the literature, most of the studies performed in experimental hemorrhagic diathesis model investigated the hemostatic potential and the healing potential of some hemostatic agents clinically or histolocigally. 24,25
The ABS and Celox are the new local hemostatic agents used in dental surgery. To our knowledge, the effects of these local hemostatic agents on TF activity have not been investigated before. Therefore, the aim of this study was the comparison of the effects of ABS and Celox on TF activity in order to evaluate their effects in early stage soft tissue healing. For this purpose, TF activities of hemostatic agents applied on skin samples of warfarin-treated rats were measured.
In our study, we administered warfarin to animals 0.1 mg/kg once daily intraperitonally for 3 days, before the surgery, until the day of killing. Based on our experience, we suggest ip way to be a more effective way of administering warfarin when compared to oral gavage. The PT tests performed on the day of killing confirmed the dose of warfarin used in our study. Different from our study, Elg et al administered 3 mL/kg of warfarin once a day for 4 days with oral gavage before surgery and suggested that antithrombotic effect of warfarin raised from 23% to 81% when the dose was doubled. 26
Similar to our study, Alpaslan et al implanted 3 different hemostatic agents (oxidized regenerated cellulose, gelatin sponge, and collagen sponge) to experimental animals’ subcutaneous tissues and evaluated soft tissue response to them histopathologically 7, 14, 21, 30, and 45 days following their implantation in rats. The results showed that all materials were well tolerated by subcutaneous soft tissues. 27
After the approval of ABS for the management of dental bleeding by Turkish Ministry of Health, ABS has been added to the protocols of prevention and treatment of exaggerated hemorrhage due to dental procedures in Turkey. Accordingly, there are studies in the literature investigating the safety and efficacy of ABS. 28–33 Teker et al made a prospective and controlled study with ABS on children who had tonsillectomy and reported ABS to be safe and effective by reducing the bleeding time and operating time. 28 Göker et al investigated ABS’s in vitro effects on hemostatic parameters. The ABS started a very rapid erythrocyte aggregation when added on plasma or serum. Fibrinogen activity, antigen levels, thrombin time, total protein, albumin, and globulin levels were reduced. 29 According to our results, Celox showed higher TF activity than ABS-applied tissue samples both in the study group and in the control group. In the warfarin group, TF activity of ABS set and nonhemostatic set tissue samples had less TF activity than Celox set tissue samples (8th day). Celox was more effective in increasing TF activity when compared with ABS, but clinic observations have shown no significant difference for hemostasis.
Zacharski and Rosenstein investigated the relation between warfarin therapy and salivary TF. They mentioned that inhibition of TF activity might be involved in the antithrombotic effect of warfarin. 34 Steffel et al stated that long-term treatment with oral anticoagulant warfarin increased soluble TF levels. 35 Different from these studies, in our study, TF activity was not affected by warfarin therapy. The reason for this might be the difference between the methods of the studies, as Zacharski and Steffel investigated TF in saliva and blood.
Kosar et al evaluated the in vivo hemostatic effect of ABS in rats pretreated with acetylsalicylic acid or enoxaparin. The ABS was administered to the cut tail in the studied animals. The duration of bleeding and the amount of bleeding were measured in order to evaluate the hemostatic effect of ABS. In both the groups, topical ABS reduced both the duration and the amount of bleeding volume. 30
Tokgöz et al compared oxidized cellulose and ABS in intravenously heparinized rats and performed partial nephrectomies. Survival times, blood pressures, and total blood loss were noted for 60 minutes, and the ABS was evaluated to be as effective as oxidized cellulose. 31
Cipil et al evaluated in vivo hemostatic effects of ABS on warfarin-treated bilateral hind leg -amputated rats. The duration of bleeding and the amount of bleeding were measured to evaluate the hemostatic effect of ABS. Topical ABS administration to amputated leg shortened the duration of bleeding markedly in both untreated and warfarin-treated rats. 32
Erçetin et al investigated the topical effects and safety of ABS in oral surgery. The ABS was topically applied by homogeneously spraying to the 25 patients during dental interventions. Tissue healing was evaluated at 48th hour by the dentist. They concluded that ABS was useful for the local hemostasis and wound healing in periodontal surgeries. 33
Celox is a new chitosan granular product that works by interacting directly with red blood cells and platelets to form a cross-linked barrier clot, independent of native factors. 36
Similar to the studies with ABS, there are studies in the literature investigating the hemostatic potential and the healing potential of Celox clinically or histolocigally. 9,36–38 Kozen et al compared Celox with 2 other agents, chitosan wafer dressing (HemCon) and zeolite powder dressing (QuikClot) in a lethal hemorrhagic groin injury. They concluded that in the porcine model of uncontrolled hemorrhage, improving hemorrhage control and survival, Celox is a viable alternative for the treatment of severe hemorrhage. 36
Klokkevold et al reported that topical application of chitosan to lingual incisions effectively decreased intraoral bleeding time in a therapeutically anticoagulated (heparinized) rabbit model. 9 Xiaohong et al investigated biocompatibility, adhesion, and hemostatic skills of chitosan sponges and collagen sponges. Performing vein traumas on rabbits, they reported no difference between hemostatic success but very tight adhesion for chitosan sponges to surrounding tissues. The chitosan sponge was degraded much slower than the collagen sponge, but tissue reaction was reported to be better than collagen sponges. 37 In our study, we observed insufficient resorption of chitosan granules. We recommend chitosan granules to be removed carefully and totally from the wound to gain success in early-stage wound healing.
Our study was different from the studies of Cipil et al, 32 since in our experimental model, warfarin-treated rats, was kept alive after surgical procedures. Therefore, adjusting the correct dose of warfarin was indispensable in warfarin-induced hemorrhagic diathesis. In our model, ip dose of warfarin 0.1 mg/kg was useful and effective and can be a good example for further studies, where keeping experimental animals is necessary.
Huri et al applied hemostatic agents to the excision areas and noted no significant difference on the effects of Celox and ABS on hemostasis in 40 Wistar rats with partial nephrectomy. They suggested ABS as an effective agent, as other hemostatics showed no fibrosis, adhesion, or calcification and better histopathological results. 38 Similarly, we noted no significant difference of hemostasis between ABS and Celox clinically.
Based on our observations even though presenting success on hemostasis, the need for the complete removal of chitosan granules from the wound was apparent, because chitosan granules did not have enough tissue biocompatibility and were determent to regular epithelization. However, Celox-applied tissues showed higher TF activity than ABS-applied tissue samples. Although physiologic upregulation of TF in wounds is transient, its effects on the reparative process are reported to be long lasting. Generation of a fibrin-rich matrix supporting the cellular response, at the level of cell migration and sequestration of growth factors, is 1 example of a mechanism through which an early burst of TF following wounding could modulate subsequent events important for healing. 18 In vivo, the multiple contributions of TF to wound healing are difficult to separate. In addition to hemostasis, TF-mediated activation of the procoagulant cascade might also enhance wound healing through paracrine/hormonal effects of factor Xa, 39 thrombin, 40 and other products of coagulation that have been shown to have impact on vascular endothelial growth factor and platelet-derived growth factor generation. 41
Conclusion
As a conclusion, clinical effectiveness and local hemostatic effects of ABS and Celox were satisfactory, as great success was observed for controlling bleeding intraoperatively and postoperatively. Study group’s PT average was significantly higher than control group’s PT average, so dose of 0.1 mg/kg of ip warfarin was satisfactory for this experimental model and can serve as a model for the trials, where keeping the experimental animals rats alive is necessary. Generally, TF activities of ABS-applied tissues were significantly lower than Celox-applied tissues both in the control and in the warfarin group. As a natural cause of healing, TF activities of the control and the warfarin group increased on days 4 and 8 compared to the day of surgery. On the other hand, although providing success in hemostasis, to avoid epithelization troubles granule-formed chitosan should be removed from the wound.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
