Abstract
Purpose:
The purpose of this study is to investigate the hispathological, biochemical, and clinical efficiency of Ankaferd Blood Stopper (ABS) in preventing postoperative intraabdominal adhesions.
Method:
A total of 40 Wistar albino species female rats were randomly separated into 4 groups. For the control group, 1 mL normal saline was administered; and for the second, third, and fourth groups 0.5, 1, and 2 mL, respectively, ABS was administered. Statistical analyses were evaluated with Tukey and analysis of variance test.
Findings:
Significant increase was observed in fibroblast and vascularization microscopically with increasing amount of ABS used. Degree of adhesion in the group administered with normal saline was lower compared to the other groups. Adhesion thickness and prevalence macroscopically increased with the increasing amount of ABS used in groups.
Conclusion:
It was determined in our study that ABS is not efficient in preventing intraabdominal adhesions; on the contrary, adhesions were increased with the increased amount of ABS used.
Introduction
The most common causes of intraabdominal adhesions are surgical operations performed in this area. 1 Adhesions lead to workforce, time, and economic losses for patients, operating room resource waste, and longer anesthesia durations. 2,3
In order to prevent the development of postoperative intraperitoneal adhesions or reduce their undesired effects, emphasizing prophylaxis is suggested. To this end, steroid and nonsteroid anti-inflammatories, antihistaminics, anticoagulants, antioxidants, proteolytic enzymes, and plasminogen activators were utilized. 4 Again, to this end, substances such as liquid paraffin or olive oil, 5 high-molecular weight dextran, 6 carboxymethyl cellulose, 7 and hyaluronic acid 8 were used to prevent contact of intestinal peristaltism by remaining in the abdomen for long durations. In other studies, methods such as covering peritoneal surfaces with peritoneal or omental grafts and reducing this contact by increasing intestinal peristaltism with enema or prostigmin were also used. 9 The fact that some of these approaches are expensive, some of them are difficult to implement, their success is limited, and performed studies are not able to deliver significant superiority to each other is the cause of continued research in this area. 10 Today, an ideal method to prevent postoperative intraabdominal adhesions is yet to be discovered.
Ankaferd Blood Stopper (ABS) is an herbal extract that has been folklorically used in traditional Turkish medicinal practice. The ABS consists of a standardized mixture of Thymus vulgaris (thyme), Glycyrrhiza glabra (licorice), Vitis vinifera (unriped grape), Alpinia officinarum (galangal), and Urtica dioica (stinging nettle) plants. 11 In experimental studies conducted with ABS, irritation, sensitivity, and cytotoxicity were not encountered. In other experimental studies, apart from antifungal, antiviral, anti-inflammatory, antithrombin, antiplatelet, antioxidant, antiatherosclerotic, antitumor, cytoprotective, cytotoxic, and hepatroprotective effects, it was also shown that it inhibits nitric oxide production. 12 –14 Today, Ankaferd has been used and has provided positive results in bleeding diatheses, 15 gastrointestinal bleeding, 16 orthopedic bleeding, 17 dental surgeries, 18 nasal bleeding, 19 bleeding occurring in oncological patients, renal artery embolization, 20 topical biological response modifier by acting on protease-activated receptor 1, 21 dermal bleeding, and healing. 15,22,23 Toxicity was determined in systemic administration of ABS. 24
In this study, we would like to research and investigate the hispathological, biochemical, and clinical efficiency of ABS in preventing postoperative intraabdominal adhesions that may occur in rats treated with abdominal operations by administering 3 different doses of ankaferd and normal saline.
Materials and Methods
To investigate the efficiency of ABS in preventing intraabdominal adhesions that may postoperatively occur in rats that underwent abdominal operation, consent was obtained from the Gaziantep University Faculty of Medicine Experimental Animal Production and Research Laboratory ethics committee (dated June 15, 2009 and decree no 06.2009-6). The study was performed by the emergency medicine, general surgery, biochemistry, physiology, and pathology departments.
A total of 40 Wistar albino species female rats between 8 and 10 months of age and weighing 300 ± 30 g were used in this study. The rats were randomly divided into 4 separate groups, and were not given any food a day prior. Hairs in the abdominal area were sheared. After the skin was sterilized with betadine solution, 70 mg/kg ketamine hydrochloride (HCl; Ketalar, Eczacıbaşı, Istanbul, Turkey), was administered intramuscularly. The abdomen was penetrated by making an approximately 4-cm laceration in the abdominal midline. After that, the antimesenteric front area of cecum was traumatized with a sterile sponge until serosal hemorrhagic petechiae formed. The control group was administered 1 mL normal saline; the second, third, and fourth groups were administered 0.5, 1, and 2 mL ABS, respectively, on the traumatized area by spraying with a syringe postmortem. Following these administrations, the peritoneum was sealed with 3/0 vicryl and the abdominal wall was sealed with continuous 3/0 prolene.
The rats were taken into their cages after the study. They were kept under surveillance in ventilation-controlled rooms at 22°C to 24°C temperature. Oral feeding started on the first day following the operation. Standard rat diet was given for 10 days. The rats were narcotized by intramuscular administration of 70 mg/kg ketamine HCl upon sterile conditions on the 11th day, with no food given a day prior. The abdomen was penetrated by making an approximate 4-cm laceration on the abdominal midline. Adhesion degree was macroscopically observed using Blaur macroscopic scale (Table 1). Three cubic centimeter of blood was drawn and placed in the biochemistry tubes for performing biochemical tests. They were stored at 2°C to 8°C after being centrifuged in the laboratory.
Blauer Macroscopic Scale.

Individual incisions were cut from the adhesion area, liver, spleen, kidney, and cecum for histopathological examination and sent to the pathology laboratory in 10% formalin solution. The preparates were histopathologically stained with hematoxylin-eosin and masson trichrome and then evaluated in terms of fibrosis and granulation tissue. Zühlke Microscopic adhesion classification was used for the microscopic evaluation (Table 2). A histopathological examination was performed by a single pathologist under light microscope sightlessly.
Zühlke Microscopic Adhesion Classification.

Disqualification Criteria From Research
Rats that died during the experiment were not included in the research.
Statistical Analysis
Statistical analyses were performed according to Turkey and analysis of variance tests. Correlation between the variables was evaluated with a Pearson correlation test. Results were evaluated under a 95% confidence interval, and a “P” value lesser than .005 was considered “significant,” and lesser than .001 was considered as highly significant.
Findings
Adhesions that occurred in our study were generally between damage-inflicted cecum serosa and omentum or small intestines.
Although no wound site infection was observed, in groups 1 and 2, 3 rats in group 3, and 6 rats in group 4 were diagnosed with abdominal area wound site infection (on incision area). Intraabdominal infection was not observed in rats that developed wound site infection. One rat each from groups1 and 2 and 2 rats each from groups 2 and 3 died and were not included in the study. In penetrated abdomens of the dead rats, widespread necrosis and tissue destruction was observed (Figure 1).
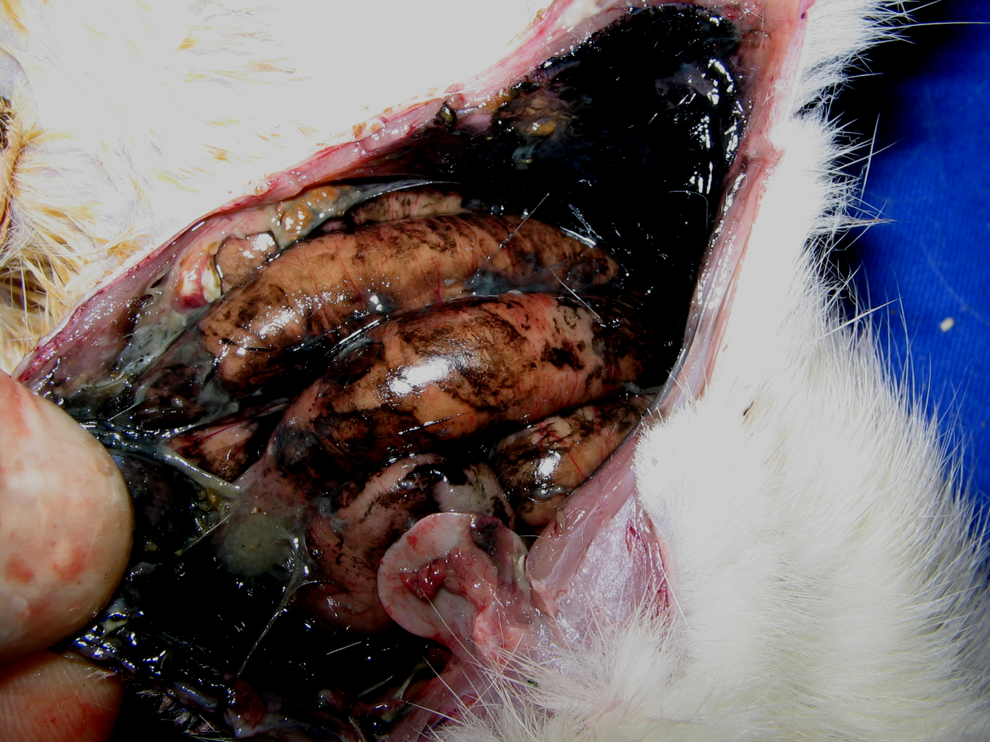
Common necrosis and tissue damage in intraabdominal region of rats that died.
In the microscopic examination, 88.9% of the rats in group 1 were analyzed as grade 1, while 75% of the rats in group 4 were determined as grade 3 and 4 (Table 3). During microscopic examination, in groups 2, 3, and 4, with the increasing ABS amount used, the grade degree and average grade values (Table 4) were significantly increased compared to the control group (fibroblast and vascularization increase was observed; P > .05). Taking mean ± error values into consideration, this difference was also graphically significant (Figure 2).
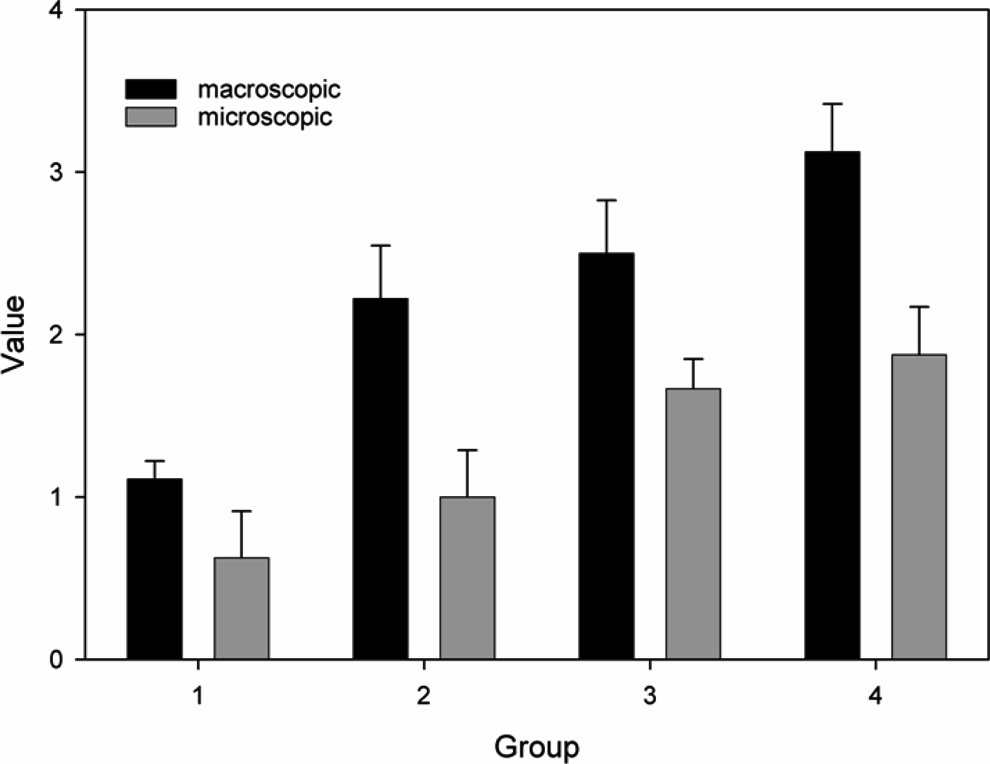
Graphical outcome of mean ± error values for macroscopic and microscopic evaluation.
Numerical Adhesions Outcomes of Patients According to Zulke Microscopic (Grade) and Blauer Macroscopic (Phase) Classification.
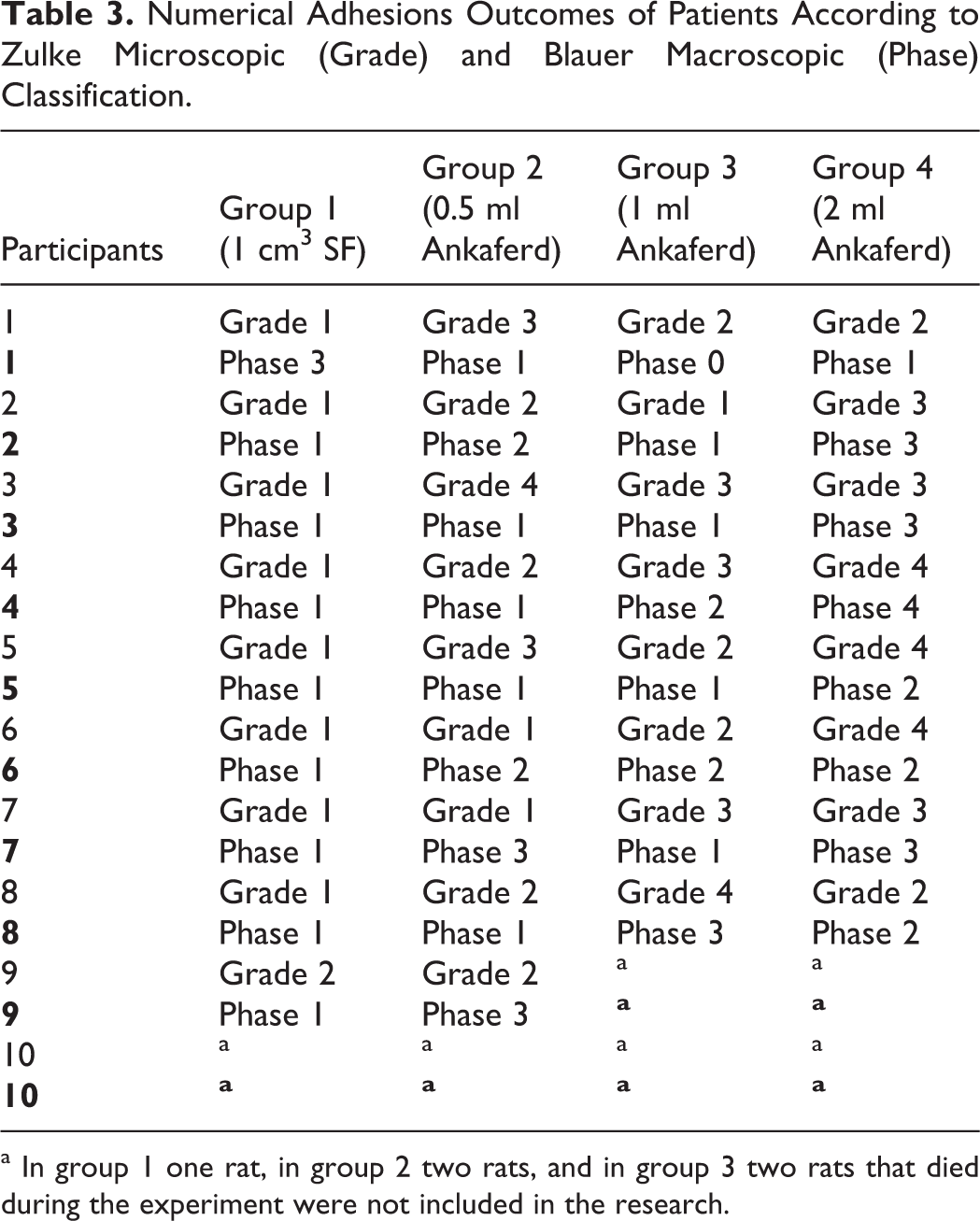
a In group 1 one rat, in group 2 two rats, and in group 3 two rats that died during the experiment were not included in the research.
Statistically Macroscopica and Microscopicb Mean Grade Outcomes of Groups.
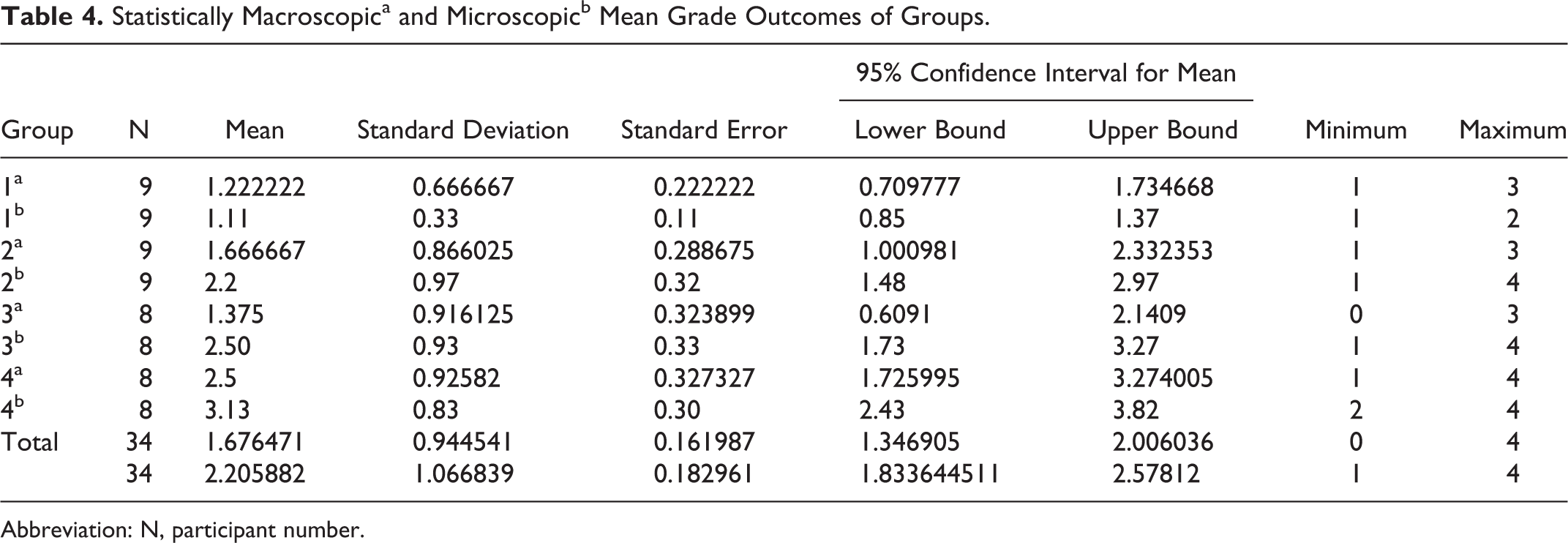
Abbreviation: N, participant number.
When evaluated macroscopically, groups and rats present in phases has been summarized in Table 3. When the control group and groups administered with ABS were individually compared macroscopically, a significant difference was determined statistically and graphically (Figure 1; P <.05). Although the difference between groups 2 and 3 was not statistically significant, the difference between groups 2 and 4 was significant. Staging degree and average grade degree macroscopically increased as the amount of ABS used in the groups increased (Table 4; adhesion thickness and prevalence also increased).
When the total antioxidant status (TAS), total oxidative status (TOS), and oxidative stress index (OSI) values of the groups were compared according to the Pearson correlation test, a statistically significant degree of positive correlation was established between OSI values of groups 1 and 2 (R2 = .998, P < .01), and a significant degree of negative correlation was established between OSI values of groups 2 and 3 (R2 = .894, P < .01; Table 5).
Pearson Correlation Table for TAS, TOS, and OSI.
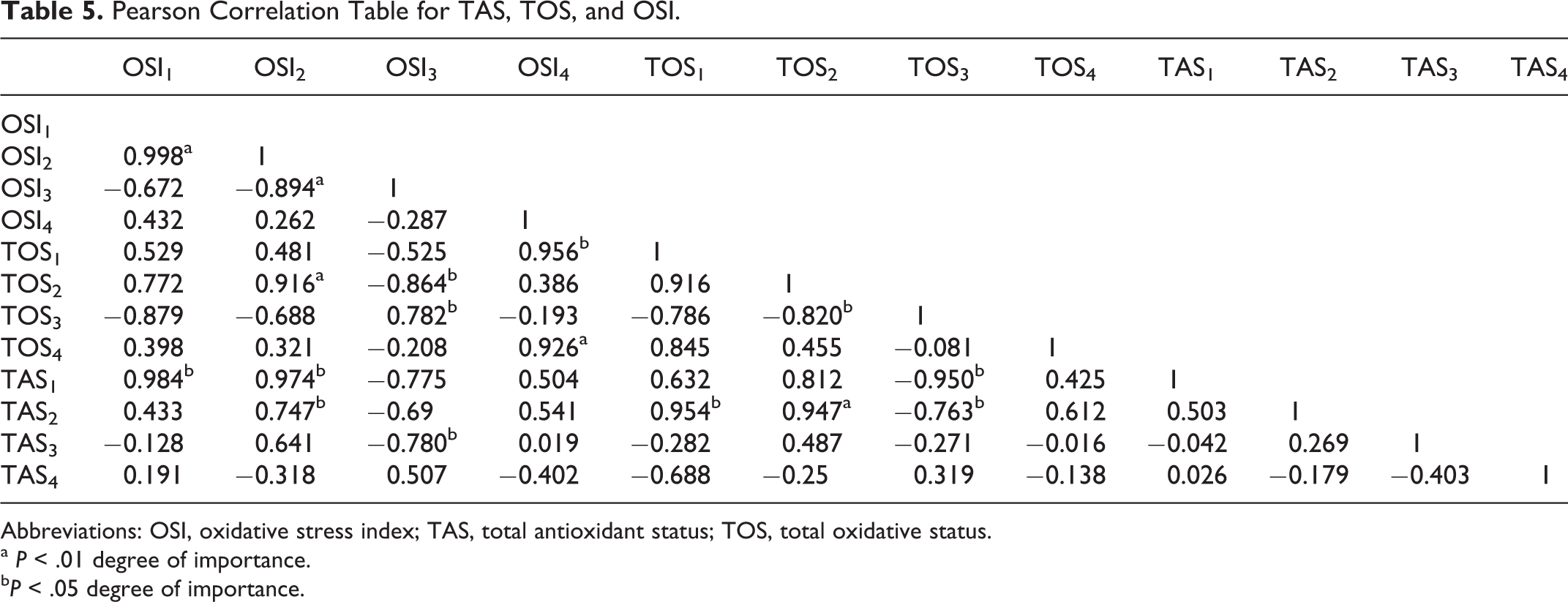
Abbreviations: OSI, oxidative stress index; TAS, total antioxidant status; TOS, total oxidative status.
a P < .01 degree of importance.
b P < .05 degree of importance.
Generally, TAS, TOS, and OSI values were higher in groups in which ABS was used compared to the control group; however, these higher values were not statistically significant (P > .05).
Discussion
Injury of the peritoneal surfaces caused by mechanical, chemical, thermic, infectious, and foreign body factors initiates the events resulting in adhesion development. Damaged mesothelial cells induce fibrin occurrence by causing thromboplastin release. An inflammatory exudative reaction characterized by cellular elements and fibrin exudation from small venules in the traumatized area begins. 25,26 Agents used for prevention of adhesion become effective on these mechanisms. 27 –30 Today, the number of abdominal surgery interventions experienced by individuals is increasing in parallel to the increase in average life expectancy. Therefore, the importance of adhesions developing during the postoperative period has been understood better following the increase in relaparatomies. Adhesions hamper intraabdominal penetration in relaparatomies and lead to the disfigurement of anatomical structures in intraabdominal organ injuries and hard-to-control bleeding, and consequently cause the duration of operation to last longer. 31 Many studies have been performed in order to mitigate all these negativities related to adhesions. The fact that some of these approaches are expensive, some of them are difficult to implement, their success is limited, and performed studies are not able to deliver significant superiority to each other is a cause of continued research in this area. 10
Tekin et al 32 used phospholipid in the experimental study and normal saline in the control group. A specific decrease was observed compared to the control group in adhesion development both macroscopically and microscopically, and this decrease was statistically significant (P < .05). Günay et al, 33 Ezberci et al, 34 and Alataş et al 35 used aprotinin–methylene blue, tenoxicam, and daflon in the experimental studies, respectively, and compared with the control groups administered normal saline. In the groups where active substances were used, adhesion development was determined to be significantly lower statistically compared to the control group (P > .05). Similar other experimental studies have aimed at adhesion with aprotinin, methylene blue, tenoxicam, daflon, phospholipids, and many other similar active substances. 32 –34 In all of these studies, the effect of the active substance in preventing adhesion was determined to be superior to normal saline.
In bleeding control, ABS is a standard herbal ingredient; it is a stable and sterile medicinal product which functions as a hemostasis regulator and is used for controlling external body injuries, traumatic cuts, dental operation, minor and major bleeding occurring spontaneously or after surgical interventions, and creating rapid hemostatic effect. 36
Today, in many centers ABS is being used to control bleeding that occurs during intraabdominal operations. However, there is only one study in the literature conducted on its efficiency in preventing postoperative adhesions. 37 In this experimental study performed by Cömert et al 37 with a single ankaferd dose (3 mL), it was determined that ABS is more efficient in preventing adhesion compared to the control group and the group administered normal saline. Adhesive degree was found to be lower. Although minor inflammatory changes were seen, toxic effects were not observed. In our study, as the amount of ABS used in the groups increased, macroscopically adhesion thickness and prevalence and microscopically fibroblast and vascularization increase were determined to be significantly higher compared to the control group. This increase was also statistically significant (P > .05). Again in the study groups (groups 2, 3, and 4) as the amount of ABS used increased, a statistically significant increase was determined macroscopically in staging degree and microscopically in average grade degree (P > .05).
When TAS, TOS, and OSI values of the groups were compared, specifically positive correlation was determined between the OSI values of groups 1 and 2, and negative correlation was determined between the OSI values of groups 2 and 3. When these mean values were compared, it was also statistically very significant (P < .01). No significant difference was observed when TAS, TOS, and OSI values of the control group and groups administered with Ankaferd were compared. When groups administered with varying doses of Ankaferd (groups 2, 3, and 4) were compared to each other, no statistically significant difference was established between TAS, TOS, and OSI values (P > .05).
Limitations in the Study
In our study, only normal saline was used as a control group. Substances used in previous studies (aprotinin, methylene blue, tenoxicam, daflon, phospholipids, etc) and ABS were not compared. The amount of ABS used was expressed in kilogram, held under different doses, and requires support of similar studies. It was observed that more detailed and important results regarding the efficiency of ABS were obtained when compared with different substances at different doses. These results alone are not sufficient to show that utilization of ABS for controlling bleeding in intraabdominal operations is disadvantageous.
In conclusion, grade degree (fibroblast and vascularization increase) and staging degree (adhesion thickness and prevalence) increased microscopically and macroscopically as the amount of ABS used in the groups increased. In this study, efficiency of ABS in preventing intraabdominal adhesions was not determined. On the contrary, it was observed that it increases adhesions compared to the control group. No significant difference was established when TAS, TOS, and OSI values of the control group and groups administered with ankaferd were compared. The insignificance of this difference shows that the cause of adhesions that occurred in participants who were administered ankaferd is not associated with oxidative stress mechanism means.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support from any company. All the expenditures were paid by the authors.
