Abstract
Background:
Flecainide is a useful antiarrhythmic for atrial fibrillation (AF). However, because of ventricular proarrhythmia risk, a history of myocardial infarction (MI) or coronary artery disease (CAD) is a flecainide exclusion, and stress testing is used to exclude ischemia. We assessed whether absent/mild coronary artery calcium (CAC) can supplement or avoid the need for stress testing.
Methods:
We assessed ischemic burden using regadenoson Rb-82 PET/CT in 1372 AF patients ≥50 years old without symptoms or signs of clinical CAD. CAC was determined qualitatively by low dose attenuation computed tomography (CT) (n = 816) or by quantitative CT (n = 556). Ischemic burden and clinical outcomes were compared by CAC burden.
Results:
Patients with CAC absent or mild (n = 766, 57.2%) were younger, more frequently female, and had higher BMI but lower rates of diabetes, hypertension, and dyslipidemia. Average ischemic burden was lower in CAC-absent/mild patients, and CAC-absent/mild patients showed greater coronary flow reserve, had fewer referrals for coronary angiography, and less often had obstructive CAD. Revascularization at 90 days was lower, and the rate of longer-term major adverse cardiovascular events was favorable.
Conclusions:
An easily administered, inexpensive, low radiation CAC scan can identify a subset of flecainide candidates with a low ischemic burden on PET stress testing that rarely needs coronary angiography/intervention and has favorable outcomes. Absent or mild CAC-burden combined with other clinical information may avoid or complement routine stress testing. However, additional, ideally randomized and multicenter trials are indicated to confirm these findings before replacing stress testing with CAC screening in selecting patients for flecainide therapy in clinical practice.
Introduction
Atrial fibrillation (AF) is highly prevalent and associated with substantial morbidity and mortality. 1 Achieving and maintaining normal sinus rhythm is a worthy goal in many AF patients for relieving symptoms and improving quality of life and functional capacity. 2 -4 Flecainide is a Vaughn-Williams class IC drug initially developed for the treatment of ventricular arrhythmias 5 and subsequently shown to be effective for supraventricular arrhythmias including AF. 6 -8 However, the Cardiac Arrhythmia Suppression Trial (CAST), which tested whether flecainide could reduce sudden death in patients with depressed ventricular function and ventricular ectopy after myocardial infarction (MI), showed increased mortality. 9,10
Analysis of CAST patients identified non-Q-wave MI, a substrate for subsequent ischemic events, as a particular risk factor for the flecainide-related ischemic/arrhythmic death. 11,12 Flecainide’s ischemia-related arrhythmic risk was confirmed in animal and additional clinical studies. 13 -15 Subsequently, FDA and professional societies have restricted flecainide to supraventricular arrhythmias in the absence of myocardial infarction/ischemia or dysfunction. 16 -18
With these restrictions, a vast amount of observational and randomized clinical trials data over the past 3 decades have shown flecainide to be a safe and effective AAD for acute and maintenance therapy of AF, 18 -29 and current guidelines give flecainide a IA (strong) indication for treatment of AF in patients without structural heart disease. 16 -18 However, those being considered for flecainide initiation are recommended to undergo cardiac stress testing to rule out the presence of inducible myocardial ischemia. 18
Myocardial ischemia generally occurs in the presence of underlying atherosclerotic CAD, and the presence of coronary artery calcium (CAC) on computed tomography (CT) is a sensitive marker of anatomic CAD and a potent prognostic indicator of subsequent MI risk. 30 Conversely, the absence of CAC is associated with a very low risk for future cardiovascular ischemic events, including in elderly patients at risk of AF. 31 -34 We tested whether the absence or a mild burden of CAC predicts a very low risk of a positive stress test and of cardiovascular events in patients being considered for flecainide therapy, possibly eliminating the need for stress testing.
Methods
Study Design, Objectives, and Primary Hypothesis
The Objective of this report was to compare results of CAC score with ischemic burden, assessed by regadenoson Rb-82 PET/CT, in AF patients ≥50 years old without pre-scan clinical signs or symptoms of CAD. We hypothesized that absence or low burden (<100 Agatston Units [AU]) of CAC could complement or eliminate the need for cardiac stress testing by predicting a very low risk of a positive stress test and of subsequent major adverse coronary events (MACE) in candidates for flecainide therapy. 35 The primary comparisons of interest in absent/mild versus moderate/severe CAC (≥100 AU) cohorts were: 1) average ischemic burden, 2) percentage of patients with ischemic burden ≥5% (threshold for clinical concern), and 3) percentage of patients with ischemic burden ≥10% (threshold for referral to angiography). Additional comparisons of interest were coronary flow reserve, referral for angiography, the finding of obstructive CAD (≥70% stenosis), and 90 day and long-term MACE. Comparisons also were made for CAC = 0 versus >0 CAC score.
Data Source, Study Population, and Institutional Review Board Approval
Intermountain Healthcare is a large, self-insured, 24 hospital, 215 clinic medical system that services over one-half of the population of Utah and also portions of Idaho and Nevada. To identify the study subject cohort, the Intermountain Healthcare nuclear medicine medical records, contained within the Intermountain’s electronic medical records Enterprise Data Warehouse (EDW), were searched from March 2014 to March 2020 for patients ≥50 years of age who had a diagnosis of AF but were without a prior history of CAD or MI and without prior exposure to flecainide and who underwent regadenoson stress Rb-82 PET/CT testing to evaluate coronary ischemia in relation to their AF therapy and not for angina. A study flow diagram is shown in Figure 1. The study was approved by the Intermountain Healthcare Institutional Review Board with a waiver of consent.

Study flow diagram.
Radionuclide Perfusion Stress Testing and Coronary Calcium Scanning
Cardiac positron emission tomography (PET) stress testing was performed on a Siemens Biograph (LSO crystal, 3-dimensional–list mode, 16-slice CT) camera using rubidium-82 chloride (Rb-82) as the perfusion marker. Weight-based Rb-82 dosage ranged between 30 and 40 mCi for both rest and stress images. CT images, obtained at the beginning of the imaging protocol, were reviewed for the presence or absence of coronary calcium. Early in the study, low attenuation CT scans were obtained and interpreted qualitatively (n = 816); subsequently, quantitative coronary calcium scoring was performed and analyzed using the Agatston method (n = 556). 36
After CAC determination, patients were injected with Rb-82 under the PET camera for immediate myocardial blood flow imaging with list mode acquisition for 7 minutes. Pharmacologic stress was achieved with regadenoson 0.4mg/5 ml IV over ten seconds. Both gated rest and stress images were acquired and iteratively reconstructed using the manufacturer’s recommended protocol.
The reading and interpretation of PET/CT studies were performed by one of an experienced group of cardiologists who were board-certified in nuclear cardiology. The PET MPI images were analyzed using commercially available software packages (QPS/ QGS; Cedars-Sinai Medical Center and Corridor4DM, Invia Medical Imaging Solutions). Whether then to proceed to coronary angiography after PET was left to each patient’s cardiologist, but in general an ischemic burden of ≥10% is regarded in Intermountain as an indication for coronary angiography.
Study Variable Analysis and Endpoints
Patient demographics, results of PET/CT and CAC testing, coronary angiography and coronary interventions, and clinical outcomes at 90-days and longer-term were extracted from the EDW database. MACE was defined as all-cause mortality, myocardial infarction, coronary intervention (coronary angioplasty/stenting; coronary bypass surgery), ventricular fibrillation, and cardiac arrest. Deaths outside of the system were identified by accessing the State of Utah Death Certificate Registry and the National Death Index.
Variable summary statistics are presented as frequencies for discrete variables or as means with standard deviations (std) or medians with interquartile ranges (IQR) for continuous variables. Analysis of variance and Fisher’s exact tests were utilized to examine baseline and clinical characteristic differences for continuous and discrete variables, respectively. The PET and 90-day outcomes were examined using multivariable logistic regression unadjusted and adjusted for baseline and clinical characteristics that significantly differed in the univariate analyses. Long-term MACE at a median of 575 days (IQR: 210,1064) was examined using Cox proportional hazards regression analysis adjusted for the same factors as the 90-day MACE. A P-value of ≤0.05 was considered significant for the primary comparisons.
Results
Characteristics of Study Patient Population
A total of 1372 patients met entry criteria, of which CAC could be quantified as mild, moderate, or severe. CAC was absent (n = 433) or mild (n = 333) in 766 (57.2%) and moderate /severe in 573 (42.8%). Demographics of this study population are summarized in Table 1. Patients with CAC absent/mild were younger, more frequently female, and had higher BMI but lower rates of diabetes, hypertension, hyperlipidemia, and smoking. CAC burden was determined qualitatively by low dose attenuation CT in 816 and by quantitative CT in 556 subjects. Baseline characteristics of these subsets were generally similar, except that qualitatively assessed subjects had more prior heart failure (Supplementary Table 1).
Demographics of the Overall Study Population and CAC Absent/Mild Versus CAC Moderate/Severe Subjects.

Abbreviations: CAC, coronary artery calcium; BMI, body mass index; HF, heart failure; CAC absent/mild, CAC <100 or qualitative absent or mild CAC; CAC moderate/severe, CAC ≥100 or qualitative moderate/severe CAC.
a Unadjusted P-values from Fisher’s exact tests for categorical variables and ANOVA for continuous variables.
Results of CAC and Stress PET Comparisons
Of those with CAC present, coronary calcium burden was mild (visually mild or <100 AU) in 40.8%, moderate (visually moderate or 100-299 AU) in 26.4%, and severe (visually severe or ≥ 300 AU) in 32.7%. Stress PET-tests were interpreted as showing no ischemia in 82.6%, mild ischemia (1%-4% ischemic burden) in 8.5%, moderate ischemia (5%-9% ischemic burden) in 5.1%, and severe ischemia (≥10% ischemic burden) in 3.8%.
Primary and Secondary Comparisons and Outcomes
Patients with absent/mild CAC showed substantially improved outcome measures compared to moderate/high CAC. Average ischemic burden was lower (0.8% ± 3.0% vs 1.5% ± 4.0%) as were frequencies of ischemic burden ≥5% and ≥10% (Table 2). Significant advantages also were noted in coronary flow reserve, referrals for coronary angiography, presence of obstructive CAD, and 90-day total MACE (Table 2). Longer term outcomes during a median follow-up time of 575 days (IQR: 210, 1064) also favored CAC absent/mild subjects (Table 2).
Study Outcomes Overall and in CAC Absent/Mild Versus CAC Moderate/Severe Subjects.a
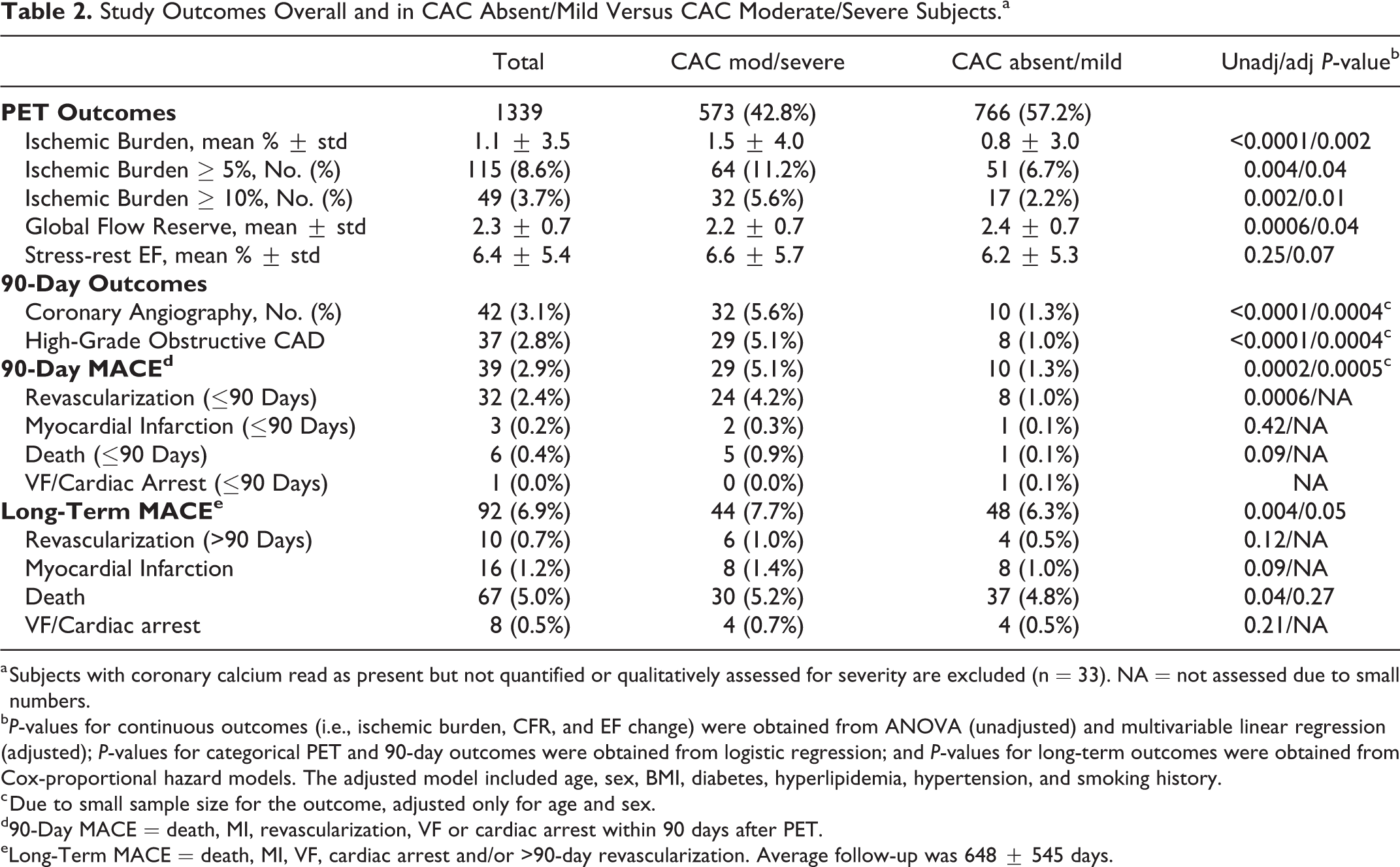
a Subjects with coronary calcium read as present but not quantified or qualitatively assessed for severity are excluded (n = 33). NA = not assessed due to small numbers.
b P-values for continuous outcomes (i.e., ischemic burden, CFR, and EF change) were obtained from ANOVA (unadjusted) and multivariable linear regression (adjusted); P-values for categorical PET and 90-day outcomes were obtained from logistic regression; and P-values for long-term outcomes were obtained from Cox-proportional hazard models. The adjusted model included age, sex, BMI, diabetes, hyperlipidemia, hypertension, and smoking history.
c Due to small sample size for the outcome, adjusted only for age and sex.
d90-Day MACE = death, MI, revascularization, VF or cardiac arrest within 90 days after PET.
eLong-Term MACE = death, MI, VF, cardiac arrest and/or >90-day revascularization. Average follow-up was 648 ± 545 days.
Sensitivity Analyses
Demographics (Supplementary Table 2) and outcome advantages (Supplementary Table 3) were similar in the smaller subset with CAC absent versus CAC >0 except that power was reduced due to smaller numbers with CAC absent. Ischemic burden was lower with CAC = 0 (0.8% ± 3.1% vs 1.3% ± 3.7%), and favorable difference trends were noted in ischemic burden ≥5% and ≥10%. CAC absent patients showed greater coronary flow reserve and had fewer referrals for coronary angiography and fewer findings of obstructive CAD. MACE at 90-day and longer-term MACE rates also were favorable. Adjusted odds or hazard ratios for these comparisons were consistently <1 with significance achieved for longer-term MACE (hazard ratio 0.58 [95% CI 0.35, 0.96]).
The use of quantitatively (vs qualitatively) determined CAC scan increased referrals for coronary angiography and findings of obstructive CAD, but long-term outcomes were similar (Supplementary Table 4).
We also analyzed those prescribed flecainide concomitantly or within 6 months of the stress perfusion test. These numbered 282 subjects, or 21% of the cohort. Their outcomes are compared to those not selected for flecainide in Supplementary Table 5. As expected, flecainide was prescribed for those with generally low ischemic burden. Outcomes in the group selected for flecainide were favorable, with broad overlap with (73%) and relatively similar results to those of the CAC absent/mild group (Table 2).
Discussion
Summary of Study Findings
In this relatively large, single healthcare system experience that enabled simultaneous assessment of CAC and stress-induced coronary ischemia by regadenoson stress PET, we found that ischemic burden was lower in CAC absent/mild patients. Further, CAC absent/mild patients showed greater coronary flow reserve and had fewer referrals for coronary angiography, fewer findings of obstructive CAD, and lower rates for 90-day and long-term MACE. Of further assurance is the lack of a signal for increased MI, VF, or cardiac arrest in these low-calcium score subjects during follow-up, who were in general being considered for antiarrhythmic therapy. These results support the hypothesis that an easily administered, inexpensive, low radiation CAC scan can identify a subset of candidates for flecainide antiarrhythmic therapy that has a low ischemic burden, rarely needs coronary angiography/intervention, and, in selected patient subsets, may be able to avoid or be complemented by stress testing.
Literature Insights
Initial attention to flecainide’s antiarrhythmic properties was directed at its superior efficacy for suppressing ventricular ectopy and excellent general tolerability, although its potential for proarrhythmia was recognized early on. 5,37,38 Subsequently, flecainide was chosen as 1 of the 3 drugs and placebo included in CAST, which tested the “PVC hypothesis” that suppression of ventricular ectopy could reduce sudden arrhythmic death after MI in the setting of reduced ejection fraction. Instead, CAST showed that flecainide and encainide, another potent class IC drug, increased mortality. 9,18 These excess deaths, which included ventricular tachyarrhythmias, asystole, and MI associated with cardiogenic shock, occurred despite suppression of ventricular ectopy. 10,18 Supporting an acute ischemia-triggered proarrhythmic mechanism were observations that although ischemic and arrhythmic events were similar compared to placebo, they were 5 times more lethal, and relative mortality risk was 5 times greater with non-Q wave than Q-wave MI during follow-up. 11,12,15,18
Parallel observations indicated that flecainide was effective and well-tolerated for AF and other supraventricular arrhythmias. 6 -8 After CAST, flecainide’s use became contraindicated in patients with structural heart disease such as those with a history of MI, CAD, myocardial dysfunction/heart failure, or latent myocardial ischemia (assessed by stress testing). 16,17 To address ongoing concerns about residual proarrhythmic potential, flecainide has been the focus of multiple observational and randomized studies and meta-analyses. Fortunately, these generally have shown an excellent safety record for acute IV and oral use and very good and comparable or (versus amiodarone and sotalol) better safety for chronic oral treatment of AF. 18 -29 Flecainide’s efficacy has proven to be superior to other AADs for acute termination of recent-onset AF and at least moderately effective, i.e. equivalent to or superior to other AADs, with the exception of amiodarone, for chronic AF suppression. 18
Mechanistic Considerations
As a class IC AAD, flecainide has potent use-dependent effects on membrane sodium channel (INa) activity, slowing conduction and suppressing electrical excitability, as recently reviewed by Echt and Ruskin. 18 These effects, which are exaggerated in partially depolarized (ischemic) tissue, appear to explain its proarrhythmic effects seen in CAST. 13,14,39 A recent study has attributed flecainide’s proarrhythmic properties to be a consequence of actions on multiple ion channels, and hence more complex than explained exclusively by its effects on sodium channels, in causing conduction heterogeneity in cardiac myocytes. 40
In recent years, it has been recognized that progressive coronary plaque extent rather than the dichotomous finding of obstructive CAD (e.g., CAD causing ischemia on stress testing) better predicts the risk of a subsequent myocardial infarction. 41 This is because plaque rupture (including of a non-obstructive plaque) rather than occlusive plaque underlies most myocardial infarctions. 41 Most recently, a Western Denmark Heart Registry study in 23,759 symptomatic patients, provided a validation that plaque burden, not stenosis per se, is the main predictor of risk for cardiovascular events and death. 42 In this regard, CAC scan as a marker of coronary plaque extent has a firm pathophysiological basis for complementing or replacing stress testing for ischemia in predicting the risk of a subsequent acute coronary ischemic event during flecainide therapy in asymptomatic subjects. Our findings are consistent with the proposal that a negative stress test plus absent/mild CAC may define the lowest risk population for flecainide therapy.
We recognize that early in disease progression, coronary plaques may be non-calcified. These “soft” plaques are more common in younger patients (i.e., <50 years old). Here, subjects ≤50 were excluded, and the age of AF patients screened for flecainide therapy averaged much older, i.e. 70 years. Also, obstructive soft plaque is largely confined to those patients symptomatic with angina. 43 For this reason, we restricted our population to those being evaluated for AF/antiarrhythmic therapy who were not symptomatic with angina (Consort Diagram, Figure 1). Even in the presence of soft plaque, event rates consistently have been observed to be very low for zero calcium subjects (i.e., <0.1%/year). 44 Thus, Budoff et-al. have argued that the “power of zero [is] stronger than ‘soft’ plaque.” 44 In support, the literature has identified mixed-content plaque, especially those with a spotty calcification pattern, to be a feature of high risk plaques. 44 -46
Clinical Implications
CAC is an inexpensive (generally < $100), low radiation, easily administered and reproducible test that has proven to be a highly sensitive marker of anatomic CAD and a potent prognostic indicator of future MI risk. 30 Conversely, the absence, or mild extent, of CAC has been shown to define a very low risk cohort for a future cardiovascular ischemic event and to be highly prevalent, even in elderly patients. 31 -34 Our observations are consistent with these reports. We found that almost one-third (32%) of candidates for flecainide referred for stress testing had no detectable CAC, and an additional 29% had minimal/mild CAC, and these cohorts were at very low risk of requiring coronary angiography, interventions, or suffering a MACE. Based on this, we believe that absent/mild CAC combined with other clinical information may be used to avoid the need for routine pre-treatment stress testing in selected flecainide candidates or as a complement to stress testing in defining low-risk status for future ischemic events. However, these recommendations should be restricted to subjects asymptomatic for clinical CAD (i.e., primary prevention subjects without angina or anginal equivalents) and to those ≥50 years old (to avoid soft-plaque-only pathophysiology). Ischemia testing should supplement CAC testing in others and in those found to have greater CAC burden.
Limitations
In common with all non-randomized observational studies, our study is subject to selection bias and unresolved confounding. The absence or presence and extent of CAC were determined by 2 methods and by clinical reading by a single imager. Early on, a qualitative assessment was made, whereas later, a standardized and quantitative method was incorporated into Intermountain’s stress PET protocol. However, only slight differences were observed in characteristics or outcomes of these 2 subsets. Performance of the study in a single system increases its consistency, as Intermountain has a standard protocol for CAC and stress PET imaging, interpretation, and reporting. However, this may limit its applicability to centers with substantially differing referral patterns and testing procedures. Although of moderately large size, our study had relatively few clinical events of interest during follow-up, especially in the CAC = 0 or 0/mild cohorts, limiting power to discern intergroup differences. A small number of non-fatal events may have been treated outside of Intermountain, but the proportions of missed events in the 2 CAC groups is likely similar. Our study population is predominantly of European-American (Caucasian) racial/ethnic ancestry, and results may not apply equally to other racial/ethnic groups. CAC may not be a reliable marker of atherosclerotic plaque burden at younger ages; therefore, patients <50 years of age were excluded. Also, we excluded patients with a history of angina or equivalent; these patients should continue to undergo ischemia testing. Our study was not a formal test of the safety of flecainide treatment selected by ischemia testing versus CACS. Only a subset received flecainide therapy, which was based on stress testing results and other, undocumented clinical criteria. We did not have access to cause of death, so that substituting all-cause for cardiovascular mortality likely weakened our MACE outcome comparison. Also, we did not have access to pharmacy claims data and, therefore, we do not have consistent information on the adherence to flecainide in this referral population or its impact on outcomes. Nevertheless, as reviewed by Echt and Ruskin 18 and summarized and referenced above, flecainide’s use in this setting has accumulated an excellent safety record.
Strengths of the study include its moderately large size, the long-standing and well-documented high-quality of the Intermountain electronic medical record system, the extensive expertise and experience of the Intermountain Heart Institute staff with PET/CT imaging, 35,36,47 as well as a stable patient population within the Intermountain system, minimizing out-of-system information loss.
Future Directions
Future directions should include initiatives to more optimally select a low-ischemic, low-proarrhythmic-risk population for flecainide therapy. In addition to additional clinical trials, applying artificial intelligence (machine learning) to this task represents one promising avenue to pursue for this purpose.
Conclusions
Study results in this real-world experience support the hypothesis that an easily administered, inexpensive, low radiation CAC scan can identify a subset of asymptomatic subjects with a low ischemic burden on PET stress testing that rarely needs coronary angiography/interventions and that has excellent clinical outcomes.
However, these results should be viewed as hypothesis-generating because of the retrospective and single-center nature of the study. Larger studies, ideally including randomized and multicenter trials, are indicated to confirm these findings before replacing stress testing by CAC screening for patient selection for flecainide therapy in clinical practice.
Supplemental Material
Supplemental Material, sj-docx-1-cpt-10.1177_10742484211046671 - Absent or Mild Coronary Calcium Predicts Low-Risk Stress Test Results and Outcomes in Patients Considered for Flecainide Therapy
Supplemental Material, sj-docx-1-cpt-10.1177_10742484211046671 for Absent or Mild Coronary Calcium Predicts Low-Risk Stress Test Results and Outcomes in Patients Considered for Flecainide Therapy by Jeffrey L. Anderson, Stacey Knight, Raymond O. McCubrey, Heidi T. May, Steve Mason, Thomas J. Bunch, David B. Min, Michael J. Cutler, Viet T. Le, Joseph B. Muhlestein and Kirk U. Knowlton in Journal of Cardiovascular Pharmacology and Therapeutics
Footnotes
Authors’ Note
All relevant summary data are within the manuscript. All other data files are in the possession of the authors and Intermountain Healthcare. Requests for additional data from these sources can be made through the corresponding author (JLA).
Author Contributions
Conceptualization: JLA. Investigation: JLA, SM, DBM, MJC, VTL. Formal analysis: JLA, SK, HTM, ROM. Data curation: SK, HTM, ROM. Methodology: JLA, SK, HTM. Writing original draft: JLA. Writing review and editing: All authors. Supervision: JLA, SK. Project administration: JLA. Visualization: SK.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
