Abstract
Deep learning (DL) application has demonstrated its enormous potential in accomplishing biomedical tasks, such as vessel segmentation, brain visualization, and speech recognition. This review article has mainly covered recent advances in the principles of DL algorithms, existing DL software, and designing strategies of DL models. Latest progresses in cardiovascular devices, especially DL-based cardiovascular stent used for angioplasty, differential and advanced diagnostic means, and the treatment outcomes involved with coronary artery disease (CAD), are discussed. Also presented is DL-based discovery of new materials and future medical technologies that will facilitate the development of tailored and personalized treatment strategies by identifying and forecasting individual impending risks of cardiovascular diseases.
Introduction of Deep Learning
In recent years, deep learning (DL) application has accomplished numerous biomedical tasks, such as vessel segmentation, brain visualization, and speech recognition. The primary purpose of DL is to find the methods that can cognitively identify patterns in a big size of data, predicting foreseen outcomes of interest based on confirmed patterns. 1
Deep learning is referred to an artificial intelligence (AI) function, whereas deep reinforcement learning is a subfield AI that uses DL models. 2 Artificial intelligence, a broad control of creating intelligent machines, thus far has focused on data collection for billing, electronic medical records, and the development of high-tech procedures including robotic surgery and access to health care. Machine learning (ML), in turn, is a subset of AI wherein machines autonomously acquire information by extracting patterns from large databases. 3 Machine learning is closely related to the fields of statistics and data mining and thus usually relies on model-based approaches in which a variety of algorithms can be programmed and reciprocally applied to each other. 4 The utility of a DL or ML-based algorithms and models will depend on factors such as data obtained from image analysis, selection of algorithms, and nature of modeling task. 5
An example of DL-based approaches applied to cardiovascular diseases is provided by a computerized model of the blood vessel that has demonstrated its immense usefulness in segmentation and analysis of the clinical data involved with coronary heart diseases. 6 As the complexity of the vascular artery depicted in the 3-dimensional (3-D) representation greatly hinders the timely detection of pathologic status, such as blocked regions and leaky vessels, AI approaches on a set of available images for the regions of interest (ROIs), such as anterior/posterior, dorsal/ventral, and medial/lateral borders and neighboring landmark structures in the blood vessel, have offered enormous clinical benefits. 7 Subsequently, software and model-based algorithms on cardiovascular devices are rapidly growing and evolved with DL.
Deep learning approach also has distinctive drawbacks, such as the necessity of extensive adjudicated data in training, lack of standardization in design, and lack of data efficiency in training. 8 Once an AI system gets deployed after initial training with historical data, AI systems need to be trained continuously by data from clinical studies for further improvement, but current health-care environment is not yet ready for sharing data on the system and thus shows restricted applicability to clinical trials. Therefore, a thorough understanding of the strength and drawback of currently reported DL approaches is crucial for its application to cardiovascular diseases.
This review mainly covers the need for DL, the basics of DL algorithms and existing data sources of pathological images, and the development strategy of DL models involved with cardiovascular devices. Recent progress in tailored and personalized cardiovascular devices, especially cardiovascular stent for angioplasty, for improving diagnoses, intervention, and outcomes in CAD treatment is also discussed.
Algorithms and Software for DL
Algorithms for DL Application
The predictive modeling process in ML is about the task of learning a mapping function from inputs to outputs known as function approximation. 9 It was defined that ML algorithms work to assess the mapping function (f) of output variables (Y) given input variables (X), expressed in Y = f(X). It was also reported that each ML algorithm requires various assumptions on the underlying functions whose best formula can be obtained by repeated practice of those algorithms. Modern DL has focused on training the back-propagation algorithms that can lead to its own decision-making by updating its weights, such as multilayer perceptron networks, convolutional neural networks (CNNs), and long- and short-term memory recurrent neural networks. 10,11
As described in Table 1, ML algorithms frequently employed in practice include artificial neural networks (ANNs), support vector machines (SVMs) classifier, linear and logistic regression, and tree-based methods (decision trees and regression trees). 2 Additionally, modified algorithms, such as CNN and k-nearest neighbors (KNNs; each classified object is compared with its k nearest training examples through a distance function), are also utilized for the classification process.
Types of Algorithms Commonly Used in the Machine Learning Process.

The example of new DL algorithms can be found from GraphSAGE, a general inductive framework that leverages node feature information to generate node embedding for previously unseen data. 11 The power of graph neural network applied to the modeling process of the variables between nodes in a given graph greatly improved the efficacy of the graph analysis. 12 Another example can be found from a product produced by a company called RSIP Vision 13 that used an algorithmic image segmentation technique called U-Net to separate the myocardium from the visceral and parietal pericardium layers of the heart within the 3-D computed tomography (CT) images. This cutting-edge DL algorithm based on CNN showed its efficiency in the analysis of 3-D CT images of the functioning heart, reducing the error due to misinterpretation of images.
The core principle that explains the objective of all DL algorithms is highly relevant to the predictive modeling process. Various algorithms, such as DeepSea, 14 Deep Variant, 15 DeepPep, 16 DeeperBind, 17,18 DeepRT, 19 Modelhub, 20 and Deep CNN, 21 have been applied to numerous research projects involved with cardiovascular devices or medicine.
Working Mechanisms of DL Algorithms
As shown in Figure 1, the life cycle of a typical DL application consists of numerous steps whose number is dependent on the nature of the projects, starting from collecting raw data and ending with monitoring predictions. Those steps generally include data sourcing, data labeling and adaptation, create/update model, model training, model evaluation, model versioning, model implement, and validating model and monitoring predicted outcomes. 20,22

Deep learning life cycle management.
Data sets used in DL projects are typically grouped into training, validation, and test subsets. The training set encompasses all available data and is used to design the prototype model. The validation set is used to assess overall model performance before the learning process begins with model hyperparameters that are set by the user (ie, batch size, gradient descent algorithm, learning rate) and influence how the weights are updated via back-propagation. Then, repeated multifold training and cross-validation are executed by running the validation set against a testing set. This validation process verifies whether or not the accuracy of the ML model has reached a sufficient level.
The early approaches of DL dealt with layer-wise training and unsupervised methods including an autoencoder that uses a neural network for dimensionality reduction where the data were condensed into fewer features. Clustering is a typical unsupervised technique in the ML process that uses condensed features rather than labeled data. As obtaining the large amounts of labeled data needed for training is not an easy task, semisupervised learning methods based on deep generative models, such as variational autoencoders and generative adversarial networks that improve the discriminator performance using unlabeled data, are trained end-to-end with high accuracy. 23
Reinforcement learning is an area of ML and compose 3 basic ML paradigms along with supervised and unsupervised learning. Reinforcement learning is dealing with how software agents take actions in an environment to maximize cumulative outcomes. Its application to the cardiovascular diseases has been scarce, but it was envisioned that reinforcement learning models will be popular in clinical practices, such as helping stent placement or remote percutaneous coronary intervention. 24
Once an algorithm and training prototype is defined, the algorithm iteratively performs adapting its internal parameters to fit the training data through optimization of an objective function. Finally, an independent test set can be used to assess its reproducibility after achieving complete optimization. The major challenge of DL approaches comes from the assessment of efficiency of these steps, while avoiding overfitting due to high bias that can be resolved by data augmentation and reducing architecture complexity. 25 Thus, DL algorithms should not be so specific to the bias in the original data on which it was initially trained to perform well on an independent test set.
Machine Learning Models and Software for DL Application
There is an increased number of DL software and models built for biomedical applications. Most DL software engineers utilize one of the popular technologies, such as Tensorflow, Keras, PyTorch, and MXNet, which enable them to build and train their algorithms and create the brains inside AI. 26 Deep learning generally requires researchers to use supercomputers or high-end workstations with multicore processors, but graphics processing units mostly designed for gaming programs have enabled DL to perform on desktop machines with the help from cloud services, such as Amazon AWS and Google Cloud, or special-purpose DL hardware, such as Google’s tensor processing units. 27
Numerous DL software and pretrained models, such as AlexNet, 28 VGG Network, 29 InceptionNet, 30 and ResNet, 31 are freely available for new projects, which significantly saved the time and computationally costly steps of DL. However, it is still challenging to efficiently share and reuse established software and trained models. In applying pretrained models to new DL tasks, the issues involved with limited interpretability and generalizability of the existing models due to missing source code or data sets should be resolved. 10
Recently, enormous efforts have been spent to address the problems of the existing models using a centralized web repository. 20 Researchers explore centralized web repository like OpenML that is an online platform built to share and organize tasks such as building ML models, collecting data sets, and conducting medical projects. 32 Model Zoo is an open, collaborative centralized repository for ML models, in which researchers combine several models stored via traditional file repositories. 33 Kipoi is another community-based platform to share and reuse DL models for genomics, which currently includes more than 2000 models applied to 21 different genomic projects. 34 ModelHub was also developed to explore, reuse, and test the ML models on vascular injury. 20
There should be an advanced cloud-based platform equipped with properties such as advanced data-driven search, on-the-fly predictions, and organized discussion boards, yet to be developed for software engineers to quickly explore, reuse, and share DL models for biomedical applications. 35
Deep Learning Application to Cardiovascular Devices
Cardiovascular Stent
Coronary artery disease (CAD) is a leading cause of heart failure and death in the world. A significant source of atherosclerosis, a major cardiovascular disease, is due to narrowing and hardening of the vessels carrying oxygen-rich blood to the heart. 36 The accumulation of plaque on the capillary and artery walls disrupts the heart functions to pump blood to distal body parts. Angioplasty, known as balloon angioplasty, is a minimally invasive, endovascular procedure to widen narrowed or obstructed arteries or veins, typically to treat atherosclerosis. 37
A coronary artery stent is a mesh tube deployed in the lumen of the coronary artery during angioplasty to prevent vessel reocclusion. The cardiovascular stent consists of a sequential-ring construction of a series of struts and connecting elements known as a bridge. An open-cell configuration allows for greater flexibility and adaptability. It can access to side branches and shows enhanced resistance to fracture. 38 The strut thickness of stents was identified as an independent predictor of in-stent restenosis (ISR). 39 As the strut thickness increases, the risk of subacute thrombosis and the chance of endothelialization increase, mainly due to delay in full neointimal coverage. 40 Most of currently available stents are made of metal, titanium, or metal composite and produced by laser-cutting metallic tubes. A single strand of cobalt alloy wire was folded into a sinusoidal wave by continuous sinusoid technology that enables the final product equipped with higher deliverability and conformability to the vessel wall. 41,42
There are bare metal stent and drug-eluting stent (DES), which releases drug loaded in the coated layers or systems on the stent surface. Drug-eluting stent has been effective in reducing the risk of late restenosis, even though they still cause late-stage thrombosis. 43 A variety of new stent designs, coatings, and resources have emerged in the biomedical society following the first generation of DES-containing sirolimus. To achieve a controlled and sustained release of antiproliferative agents, current DES utilizes various polymeric blends with biodegradable or nonerodible properties in stent surface coating that can also serve as the carriers of drug or stem cells. 44,45
Bioresorbable vascular scaffolds (BVSs) are fabricated to offer mechanical support and delivery of drug like DES, followed by complete resorption over 4 to 5 years. Bioresorbable vascular scaffold based on biodegradable polymeric blends have additional benefit of complete resorption and signify the integral step in future stent development. Clinical trials and registries confirm the efficacy and safety of up-to-date stents, but a more significant number of trials and a more extended period of follow-up are necessary to assess the effectiveness of recently developed novel stents. 46
New Platforms for Cardiovascular Stents
One of the most troublesome issues involved with coronary stent implantation is ISR, that is, the narrowing of coronary artery lumen at the stent-placed sites. 47 In-stent restenosis caused by balloon angioplasty is attributed to 3 factors: The elastic response that occurs after the overstretching of the vessel, neointimal hyperplasia, and adverse remodeling. 48,49 As compared to ISR after balloon angioplasty, the pathophysiology of ISR displayed a more profound cellular and proliferative response and less thrombogenic potential.
There are new stent platforms on new material and strut designs after multifacet and long-term therapeutic applications and DL-based analysis from clinical studies to avoid ISR and lessen thrombogenic potential. For instance, the “Element Stent Platform” (Boston Scientific, Marlborough, MA) is made of a platinum–chromium alloy that is denser than stainless steel or cobalt–chromium. 50 The strut thickness of “Element Stent Platform” is about 81 µm and exhibits high radial durability and radiopacity. Another example is provided by designing bifurcation stents that have been designed to overcome the difficulties encountered during bifurcation procedures. 51 The range of the restenosis rate is between 28% and 54%, even though the first-generation bifurcation stents including Nile Croco, Tryton, Multi-Link Frontier, and Sidekick were not DES.
Bioresorbable stent (BRS) technology has triggered complete resorption of the scaffold that liberates the vessel from its long-term contact with foreign material and potentially restores vessel anatomy and physiological shear.
52
The risk of late-stage thrombosis is eliminated, as the foreign substance is replaced with connective tissue or the scaffold segment healed with matured endothelium. The BVS system made of polylactic polymers became the first to be commercially available and was followed by those made of other BRS material, such as magnesium alloys, poly-
There are reported side effects from BVS, such as poor healing and late adverse reactions, that may result in vessel injury, platelet deposition, poor deliverability, and rheological disturbances. 54 Other drawbacks to BRS include an increased scaffold fracture risk with overdilatation of BRS; thus, distinctive size modification is not feasible. 45 The front runner, everolimus-eluting Absorb BVS (Abbott Vascular, Santa Clara, California), failed to demonstrate its promise. 55 As Absorb BVS resorbs, the resorption time appears to be slower than initially thought and its strut thickness has created a potential late-stage thrombosis, necessitating extended dual-antiplatelet therapy.
A DL-based method is proposed for automatic detection and segmentation of struts malapposition of BVS 56 that may cause typical restenosis and late-stage thrombosis. A ROIis spontaneously assigned for each strut based on its size and location. Subsequently, dynamic programing is used to analyze the boundary of each strut within the ROI that leads to the interpretation of struts malapposition. A DL-based model will surely lead to new flat form of advanced cardiovascular stents.
The Modeling Process of Coronary Artery Circulation
Numerous approaches have been introduced to design the ML models for the coronary artery circulation that is predictably governed by energy, mass, and momentum conservation. 57 The pathological status of a coronary artery is monitored in clinics using such advanced techniques as 3-D CT angiography, optical coherence tomography (OCT), and ultrasound. The DL algorithms have been developed for the complete integration of the 3-D OCT of the blood vessel that enables simultaneous quantifying of the levels of the pathological segment as well as structural and molecular progress of atherosclerotic plaques. 58 This approach leverage computer vision technology to transform cellular and biological levels of receptor-binding affinity into quantitative molecular values by automatically detecting and tracking pathological segment or frames in the coronary artery.
A fully automated framework was designed for identification of coronary anomalies from 3-D CT image stacks or intravascular ultrasound (IVUS) image sequences. 59 The proposed computer-aided detection uses a DL approach to accurately segment arteries, locate blockages, and precisely place the struts and shape of implantable stents, avoiding injury risks due to improper placement. The DL approach showed an accuracy of an overall F-measure of 77.7% and a mean distance of 0.15 mm from manually annotated struts in metallic stents, and an overall F-measure of 77.4% and a mean distance of 0.09 mm from manually annotated struts in bioabsorbable stents.
A new lumped-parameter model (LPM) for coronary hemodynamics was developed for the whole coronary network that is based on CT scans of a patient-specific geometry, including the right coronary tree, 60 which is absent in most ML models. From a device perspective, as the polymer layer of DES and applied tissue region is considered a coupled system, an integral equation called the Volterra integral equation was derived for assessment of the drug-release amount from DES. 61
The ML model called “CircAdapt” was introduced as an educational tool for medical students. 62 It is an LPM that describes the hemodynamic interaction between the left and right ventricles defined by the pressure gradient and that can be numerically solved and proposed to enhance the therapeutic efficiency against coronary artery disease. This model requires relatively few model parameters, such as heart rate or peripheral resistance, which can simulate various physiological and pathophysiological status, including exercise or hypovolemic shock. The proposed model allowed medical students to understand cardiovascular physiology, map the progression of crucial disease processes, and classify the severity of the disease. An LPM was subsequently incorporated into an e-learning environment, which helps users to find the proper solution to abnormal cardiovascular physiology in a clinical context. 63
The Image Analysis of Cardiovascular Stent
Numerous approaches can be adapted to investigate the optimal feature annotation of the biomedical devices in a data set, as they were inserted or implanted in the vessels. The ROI in a blood vessel were initially estimated through a broad interpretation of the vessel geometry. 64 For this purpose, a semantic classification method with a curve approximation was applied to each image frame to provide an accurate labeling of ROIs in the circulation. 65
For annotation purposes, a manually annotated set of points was introduced with coordinates (xs, ys) upon being derived from a manual tracing protocol designed for a volumetric study of blood circulation. The resolution value for each axis was extracted using a CNN. 6 The pixel values were stored in a 2-D grid as an array of numbers, and a small grid of parameters called kernel and an optimizable feature extractor will be applied to each image position.
The step to visually recognize the structures of interest was followed through recording the number of images with the given structures. 66 This procedure utilized the triplanar view in MiPAV implemented in Java, a freely available medical image processing software package from the National Institutes of Health. 67 MiPAV serves as a user-friendly graphical tool to analyze optimal descriptors of the local appearance of blood vessels in the image frames, such as longitudinal measures for height, width, and length of the ROIs. The medial/lateral borders within vessels were delineated based on both local placement and algorithm models, which allowed for an efficient interpretation of automatic vessel segmentation.
Angiography enables visualization of the blood flow in the blood vessels and its branches. They comprise the full scale covering from feature selection to its extraction, allowing for a more concise depiction of each object with the help from a DL-based approach conducted in a short period. An identification of struts location and shape maintenance is integral for angioplasty surgery and its follow-up in CAD patients. There are 2 cases of incomplete stent deployment: malapposition (not entirely in contact with the luminal wall) or underexpansion (not completely expanded even though correctly positioned to the luminal wall). 59 The incomplete stent deployment generally leads to inefficiency, restenosis, and late-stage thrombosis.
The imaging modality currently used as the reference for verifying the correct apposition of a stent is intravascular OCT. 68 Also used is a catheter-based imaging technique called IVUS that provides a sequence of tomographic images of the internal vessel morphology. 69 Even though the resolution in OCT images is higher than that in IVUS images, the lower penetration depth (1.5 mm in OCT vs 5 mm in IVUS) restrains competence of OCT to assess vessel remodeling and plaque burden. An OCT catheter placement usually requires the intubation of the coronary opening to offer proper administration of contrast agent, which constraints the analytic accuracy of orifice lesions. 70
In authors’ laboratory, echocardiogram image classification and labeling process based on the ROI approach has been performed via combining dynamic learning and domain knowledge, which uniquely identifies and describes the layout of each image for assessment of the disease progress as well as placement of cardiovascular devices in blood vessels. 71 After preprocessing feature extraction, each concept on drug-loading systems applied on biomedical devices were aggregated as a set of local image features using novel aggregation methods, such as content-based image retrieval methods 72,73 and Eigen thumbnail image appearance modeling process. 74
Deep Learning–Based Optimization and Efficacy Assessment
Variables in DL Models for Efficacy Assessment
A DL-based model will be developed to predict the relationship between the stent-preserved blood flow and the factors involved with functions of the cardiovascular stent. The DL model predicts the changes in the blood flow and the release rate of loaded drug (ie, immunosuppressive agents) from the stent as a function of the internal (ie, loading dose and surface thickness, etc) and external (ie, endothelial function, the intima layer diffusivity, etc) variables, as described in Table 2. The adapted approach will lead to the reconstructing the internal model rules that explain the maintenance of the normal blood flow and the effective concentration of immunosuppressive drug at the intima layer against in-stent–induced thrombosis or restenosis.
Input/Output Parameters Used in the Deep Learning Modeling Process.

Abbreviations: BP, blood pressure; NP, nanoparticle.
A thematic analysis of DL models into translational application against cardiovascular diseases could be followed. The blood flows in the tissues are typically low; thus, all blood flows in the intima layer are considered laminar. As the influence of diffusivity of the polymer film coated on stent surface is minimal, the major contributors should be the loading dose of immunosuppressive agents, thickness, or weigh of polymer film contacted with the intima layer. The differential equations regulating the conservation of mass and species in both tissue and artery domains are counted as a single set in the study. The transport rate of the loaded drug into the intima layer is determined by examining the permeation rate of loaded drug released from polymeric films coated on the stent using the blood fluid dynamics.
A sufficient number of the release profiles of loaded drug obtained under various formulation and physiological conditions make it feasible for the data mining–based numerical modeling process. Therefore, a more accurate measure and new information on the detailed characteristics of such formulation and physiological variables as applied to cardiovascular devices can be obtained by analyzing all or a sufficient number of individual subunits through selected ML-based techniques. After that, the proposed multiple subunits can be optimized in detail to obtain the best product.
The DL model for the relationships between blood flow, the loaded drug-release rate, and onset rate of restenosis was further performed to cover the following procedures: (1) implementation of the DL model, (2) computation of the restenosis index (RX), and (3) validation of the DL model. It was further confirmed that the tracing values of blood pressure and flow based on the model prediction could reflect the onset of stent-induced restenosis.
Classification and Quantitation of Blood Segment for DL Models
After a model is built on the mapping of the global and local features, quantitative information on drug distribution at each segment of the blood vessel can be derived. Overall image architecture was constructed by conversion of analytical data obtained from image analysis tools, such as 3-D CT, OCT, scanning electron microscope/tunneling electron microscope, fluorescence resonance energy transfer, and flow cytometry analysis, to an image format. 75 Recently, DeepVesselNet 76 and EvaluateSegmentation 77 were introduced as tailored architectures to be addressed, when segmenting vessel networks and similar features in 3-D angiographic volume were examined. These approaches have achieved a significant improvement in lowering of memory footprint or network complexity as well as the processing speed, which prevents optimal fitting and a higher degree of accuracy. 78
In authors’ laboratory, the scheme presented in Figure 2 was used for the analysis of the amount of loaded drug distributed in the intima layer and further development of the DL model for prediction of changes in blood flow. The ML-based fluid dynamics can be utilized in handling the numerical modeling process. The segmented domain is fixed in a 3-D coordinate system (x-y-z), divided into an artery lumen and its environmental tissues. The segmentation was performed by categorizing the image pixels into systems like drug-loading polymeric support applied to stent surface and surrounding vessel using SVMs 79 that is supervised learning model with associated learning algorithms.
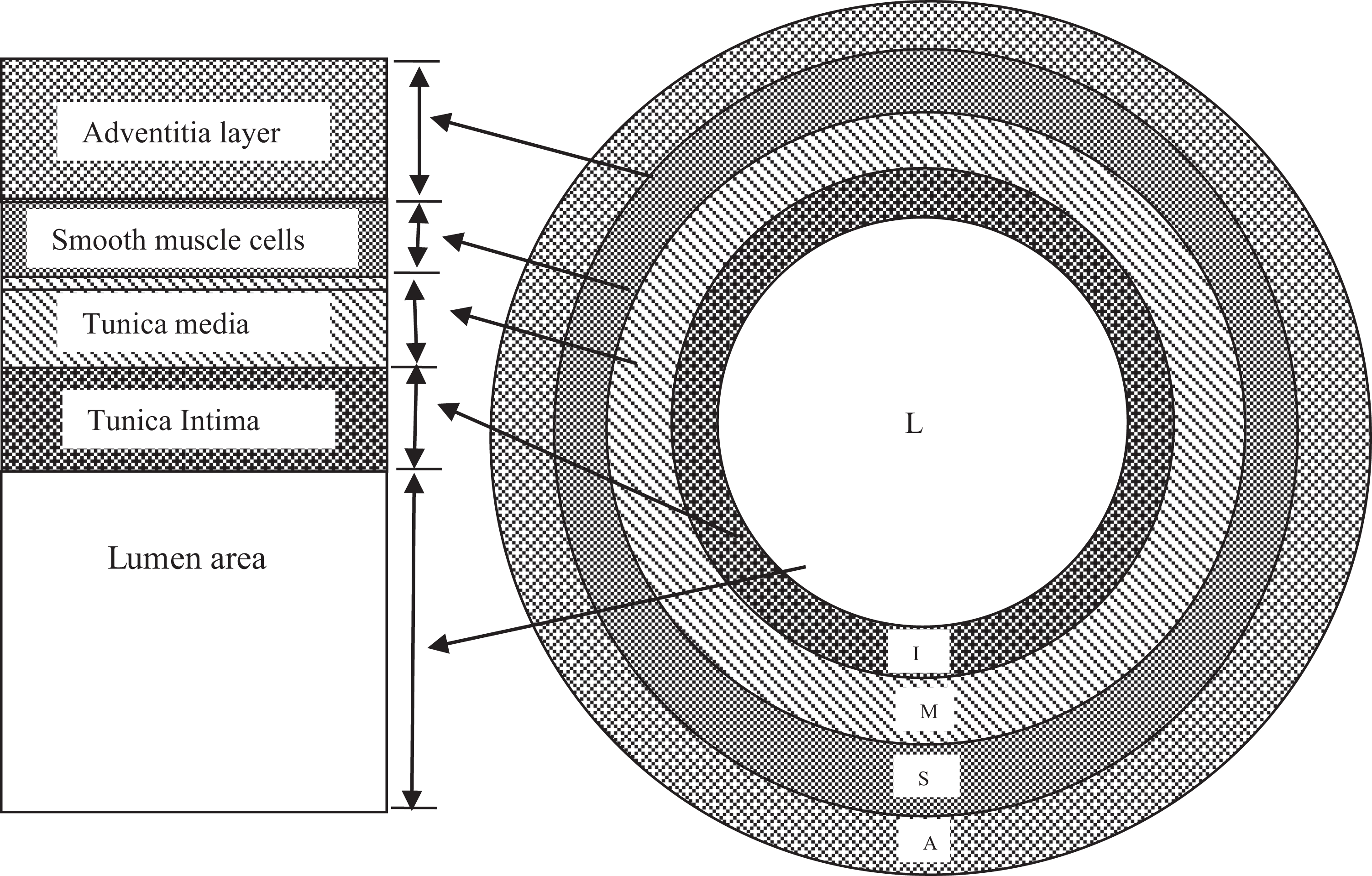
Schematic and relative position in-stent geometry in cross section of the arterial wall consists of the intima and adventitia layers (L: 1.5 mm, E: 0.1 mm, I: 0.05 mm, S: 0.15 mm, A: 0.7 mm, respectively).
The analytical process was subsequently conducted on the quantitative data representing a 3-D feature of drug-loading systems applied to stent surface that was analyzed using automatic data extraction method supplied from Apache Spark MLlib, MathLab, and OpenCV systems. Any relationships among the formulation and physiological variables were established based on input/output parameters described in Table 2.
Cascade ML Model for Cardiovascular Stents
An efficient DL model has been designed for identification of the general relationships between the suppressive efficacy of cardiovascular devices and surrounding physiological conditions in the vessel. The cascade machine learning model (CMLM) is a classifier made of commercially available data mining models and newly designed (in the author’s lab) execution software. 80
As shown in Figure 3, CMLM consists of the 3 component models known as the KNN model, the statistical regression model, and the modified back-propagation neural network. The CMLM works in a series, integrating the estimated value obtained from the base model placed ahead to the base model as an input value placed later in CLML. Moreover, since the models are cascaded in parallel, no resolution of estimations is needed for the subsequent prediction, avoiding the output domain discretion. If the required accuracy reflected with root mean square is not reached, the controller continuously feeds the training data set to the model. It stops when either the maximum epochs allowed is elapsed or the required accuracy is achieved. Thus, accuracy of CLML is greater and training period is shorter as compared to the conventional neural network.

Cascade machine learning model.
For elucidation of the outcome, the RX is calculated based on the variable conditions, the scores in simulation for the formulation variables and the physiological variables, respectively, are subsequently incorporated into simulation 1. The correlation coefficient between each parameter and RX (3, n) is computed using the data mining model built with ANN.
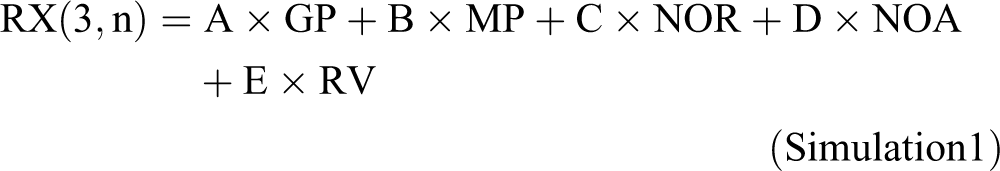
where GP = surface groove pattern conditions, MP = microparticle conditions, MPR = drug-release rate, NOA = drug amount in the intima layer, RV = rest variables (ie, thickness of each region, physicochemical conditions of fluids, cGMP level), and n = expected restenosis rate.
The contribution amount of each variable to the overall RX will be calculated using the following simulation:

where p is the number of variables and aj is the first principle components vector. The formulation and physiological variables are ranked as prognostic factors based on their percentage contribution to the restenosis.
The CMLM can predict the drug-release profiles from polymeric film coated on stent surface and its efficacy as a function of the formulation and physiological variables, leading to the understanding of underlying rules which govern the release profiles and the onset of restenosis. The DL-based framework can provide detailed information on the involved factors, identify the efficient range of variables, and predict the immunosuppressive efficacy of drug from surface-coated carriers. Other ML models based on finite element analysis could be further designed to complement the clinical data and achieve enhanced treatment efficacy of cardiovascular stents.
Future Prospect in DL-Based Personalized Cardiovascular Devices
There seems to be an immense opportunity to utilize a DL approach in the field of cardiovascular devices, medicine, and precision health care. It was envisioned that data analytics along with cognitive computing will eventually govern the field of cardiovascular devices that will be designed and distributed via DL software. The ultimate goal of production of cardiovascular devices based on a DL approach is moving toward the discovery of customized and personalized treatment strategies against various diseases. 81
The personalized cardiovascular device is considered a profound knowledge related to phenotype and ontology that performs pattern recognition of patient profiles. 82 In the DL process, it is ideal to have complete information about existing phenotype categories including various disorders as well as ontology components, and a sufficient and balanced number of patients for each control and participant group. 83,84 The pattern recognition component deals with numerous errors and uncertainties within the data. 85 As it is considered a hard task to achieve an error-free analysis using the conventional statistical methods due to some limitations, 86 an advanced DL method such as a recurrent neural network will retrospectively assess sequential data inputs and determine the contributors linked to acute injury at specific organs, including kidney and heart, ultimately leading to identify and forecast impending risks. 87
From clinical perspective, as the use of biomaterial constructs face several challenges, such as immunogenicity, host inflammatory responses, fibrous tissue formation, biomaterial degradation, and cytotoxicity of degradation products, it is ideal to create the model systems based on patient-specific physiological conditions and pathological status of blood vessels. 88,89 Future medical technologies will directly provide the patient with tailored, personalized devices including stent-mediated angioplasty without any adjustments from the health-care personnel. 7,59,90
Recent advances in augmented reality 91 and 3-D printing technique 88,92 will undoubtedly facilitate the early arrival of personalized cardiovascular devices. Notably, 3-D printing technology will allow better control over the creation of gradients within the device or system, such as mechanical and the growth factors of cells, producing biocompatible, robust, and flexible medical devices with mechanical strength that can withstand the dynamic environment of the blood vessel. 93,94 Based on a DL approach on the patient’s mass and metabolism, a novel 3-D printing technology can produce a customized cardiovascular stent to precisely fit patient vessel’s dimensions and status. 89,95 Also, the amount of drug delivered can be tailored via newly designed DL models, so any potential cytotoxicity of the drug can be alleviated. 96,97
Footnotes
Author Contributions
Y.L. performed the design and classification of MN and DL models and drafted the manuscript. K.V. carried out DL-based formulation optimization and efficacy evaluation process of the cardiovascular devices. M.H.J. participated in DL-based clinical assessment and obtaining therapeutic outcomes of cardiovascular devices. C.H.L. conceived of the study, participated in its coordination, and consolidated to complete the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
