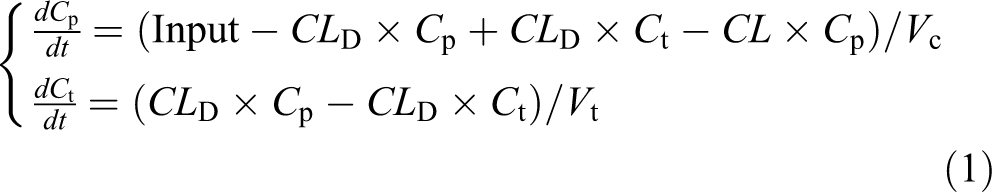Abstract
Objective:
To examine the electrophysiological, hemodynamic, and antiarrhythmic effects of the novel antiarrhythmic agent AZ13395438.
Methods:
The ion channel-blocking potency of AZ13395438 was assessed in Chinese hamster ovary cells stably expressing various human cardiac ion channels and in human atrial myocytes. The in vivo electrophysiological, hemodynamic, and antiarrhythmic effects of intravenously administered AZ13395438 were examined in anesthetized rabbits, in anesthetized naive dogs, and in dogs subjected to rapid atrial pacing (RAP) for 8 weeks. Pharmacokinetic/pharmacodynamic (PKPD) modeling was applied to predict the potency of AZ13395438 in increasing atrial and ventricular refractoriness.
Results:
AZ13395438 potently and predominantly blocked the atrial repolarizing potassium currents IKur, IAch, and Ito in vitro. In vivo, AZ13395438 caused a concentration-dependent and selective increase in atrial refractoriness with no or small effects on ventricular refractoriness and repolarization and on hemodynamics in both rabbits and dogs. The PKPD modeling predicted unbound plasma concentrations of AZ13395438 of 0.20 ± 0.039, 0.38 ± 0.084, and 0.34 ± 0.057 µmol/L to increase the right atrial effective refractory period by 20 milliseconds in the rabbit and in the naive and the RAP dogs, respectively. In the RAP dog with atrial fibrillation (AF), AZ13395438 significantly increased AF cycle length and successfully converted AF to sinus rhythm in 12 of the 12 occasions at an unbound plasma concentration of 0.48 ± 0.076 µmol/L. During saline infusion, conversion was seen only in 4 of the 10 occasions (P = .003 vs AZ13395438). Furthermore, AZ13395438 reduced AF inducibility by burst pacing from 100% to 25% (P < .001).
Conclusion:
AZ13395438 can be characterized as a mixed potassium ion channel-blocking agent that selectively prolongs atrial versus ventricular refractoriness and shows promising antiarrhythmic efficacy in a clinically relevant animal model of AF.
Keywords
Introduction
Atrial fibrillation (AF) is the most common sustained arrhythmia encountered in clinical practice, occurring in approximately 1% to 2% of the general population. 1 In the Caucasian population, the prevalence increases with age from <0.5% at 40 to 50 years of age to 5% to 15% at 80 years of age and the lifetime risk of developing AF is 25% in those who have reached the age of 40. Previous estimates suggest that 6 to 7 million people in Europe and the United States have AF. 1 The AF is a progressive disease and several projections indicate that the prevalence will at least double during the next 50 years as the population ages. The disease is associated with substantially increased morbidity and mortality conferring to a 5-fold increased risk of stroke and a doubled mortality rate independent of other known predictors of death. Furthermore, AF is associated with heart failure, frequent hospitalizations, a poor quality of life, and a significant socioeconomic burden. 1
Management of patients with AF aims at reducing symptoms and preventing severe complications, therapeutic goals that need to be pursued in parallel. Depending on the severity of the AF-related symptoms, the acute clinical management of AF should strive toward acutely restoring sinus rhythm (conversion of AF) or acute management of heart rate. No matter if a rate control or rhythm control strategy is chosen for long-term management of AF, the initial therapy should always include adequate antithrombotic treatment. Current treatment guidelines recommend initiation of therapy with safer, although eventually less efficacious, antiarrhythmic agents with attention paid to the underlying structural heart disease. 1 The presently available pharmacological options for AF management have limited efficacy and comes with considerable risks, particularly proarrhythmia. 2 –4 An attractive prospect for improved AF management is the search and introduction of drugs that selectively target ion channels engaged in atrial repolarization. Such atrial repolarization-delaying agents would at least theoretically increase atrial refractoriness, restore, and maintain sinus rhythm without undesired effects of impulse propagation and cardiac contractility and circumvent ventricular proarrhythmia liability. 5 –7 Presently, there are few such agents in clinical use or under clinical investigation. Vernakalant is approved in Europe for conversion of recent onset AF. It blocks atrial early repolarizing currents including the atrial ultra-rapid delayed rectifier current (IKur) but also shows high affinity to the fast sodium channel. XEN-D0103 is an investigational and selective IKur blocker in early clinical testing which is the case also for NTC-801, an agent that selectively blocks the acetylcholine-activated inwardly rectifying potassium (K+) current (IKACh). 4,8
AZ13395438 ((2S)-3-{[(1R,2R)-2-(dipropylamino)-1,2-dipyridin-2-ylethyl](propyl)amino}propane-1,2-diol) is a novel investigational antiarrhythmic agent. The objective of the present study was to characterize its ion channel-blocking potency in vitro and electrophysiological and hemodynamic effects in anesthetized rabbits and dogs in vivo. Furthermore, the antiarrhythmic efficacy was assessed in dogs subjected to 8 weeks of rapid atrial pacing (RAP) to induce atrial remodeling and fibrillation.
Methods and Materials
These experiments were approved by the local ethics committee on animal experiments in Gothenburg, Sweden (applications 6-2008, 129-2010, and 281-2009).
Ion Channel-Blocking Effects In Vitro
The ion channel-blocking potency of AZ13395438 was assessed in Chinese hamster ovary (CHO) cells stably expressing the human cardiac ion channels hKir3.1/hKir3.4, hERG, hKvLQT1/hminK, hKv1.5, hKv4.3/hKChIP2.2, hCav1.2, or hNav1.5 and in freshly isolated human atrial myocytes (IKur and Ito only). Electrophysiological studies on recombinant ion channels were performed using a high-throughput planar patch clamp assay (IonWorks HT, Molecular Devices, LLC, Sunnyvale, California, or, for IKACh, QPatch, Sophion Bioscience A/S, Ballerup, Denmark) and standard extracellular and intracellular solutions. 9,10
The hKir3.1/hKir3.4 current, corresponding to IKACh, was activated by 10 μmol/L carbachol and an increase in the extracellular K+ concentration from 4 to 50 mmol/L. The cells were clamped at −90 mV, corresponding to baseline, incubated with the compound for 90 to 120 seconds and then stimulated by carbachol/high K+. The current metric was the current amplitude at the end of the sweep.
The hERG current, corresponding to IKr, was evoked by a 1 second step to +40 mV from a holding potential of −70 mV, a 2 second step to −30 mV, and finally a 500 millisecond step to −70 mV. The current metric was the peak current amplitude at −30 mV.
The slow outward hKvLQT/hminK current, corresponding to the IKs current, was evoked by a voltage step from a holding potential of −80 to +40 mV for 4 seconds. The current amplitude was calculated by measuring the mean current toward the end of the pulse (3.8-3.9 seconds) and subtracting the mean current at the beginning of the pulse (110-150 milliseconds).
The hKv1.5 current, corresponding to IKur, was evoked using a voltage protocol consisting of ten 200 millisecond pulses from −70 to 20 mV, delivered at a rate of 1 Hz. The current metric was the amplitude at the end of the last activation pulse.
The outward hKv4.3/hKChIP2.2 current, corresponding to Ito, was evoked by 3 voltage steps to +20 mV from a holding potential of −90 mV. The pulses were given at a rate of 3 Hz, the duration of the first 2 pulses was 50 milliseconds and the last pulse was 1 second. The current metric was the peak current amplitude of activation pulse 3.
The hCav1.2 current, corresponding to the ICa ,L current, was activated by a voltage step to −10 mV from a holding potential of −60 mV. The current metric was the peak amplitude at 10 −mV.
The hNav1.5 current, corresponding to the fast inward sodium current, was evoked by a train of 50 millisecond voltage steps to 0 mV from a holding potential of −90 mV; 8 voltage pulses of this type were delivered at 3 Hz. The current metric was the peak amplitude at 0 mV of the last pulse.
All recordings were carried out at room temperature (22°C). Voltage protocols were elicited before and after the addition of AZ13395438 and effects of the compound on the current metrics were studied at concentrations ranging from 0.03 to 33 μmol/L.
Isolation and recording of currents from freshly prepared human atrial cardiomyocytes were performed using conventional patch clamp technique as previously described in detail. 11 In brief, the currents were measured using the whole-cell variant of the patch clamp method. Current amplitude and kinetics were allowed to stabilize (>5 minutes) before experiments were begun and were elicited by a series of voltage pulses given at 1 Hz using a 1 second voltage pulse to +60 mV from a holding potential of −75 mV. Ito was measured as the peak current amplitude at the beginning of the 1 second voltage pulse. IKur was defined as the current measured at the end of the 1 second voltage pulse minus the current remaining after 1 mmol/L 4-aminopyridine was added to the cell bath. This concentration of 4-aminopyridine completely abolishes IKur and allows determination of the amount of IKur present in the current recorded at the end of the voltage pulse. Voltage protocols were elicited before and after the addition of AZ13395438 at concentrations ranging from 0.03 to 10 μmol/L.
Electrophysiological and Hemodynamic Effects in the Anesthetized Rabbit
Male New Zealand White rabbits (n = 5) were anesthetized with ketamine and medetomidine, intubated, and artificially ventilated. Catheters for drug infusions, arterial blood pressure recording, and blood sampling were inserted into marginal ear veins and the left carotid artery, respectively. A 4F quadripolar electrophysiological recording catheter was advanced into the right jugular vein and positioned high up in the right atrium for recording of an electrogram and for pacing. The effective refractory period in the right atrium (RAERP) was determined at a current strength approximately 20% above the threshold for capture. A custom-made personal computer-based programmable stimulator and a constant current pulse generator were used for stimulation at a cycle length of 250 milliseconds. A premature extra stimulus was introduced after every 10th paced basic beat with increments of 2 milliseconds until capture. The needle electrodes were placed subcutaneously for recording of a surface electrocardiogram (ECG). The signals were amplified by custom-made amplifiers and recorded at a frequency of 200 to 1000 Hz. Data were processed with PharmLab v.6.0 (AstraZeneca R&D, Mölndal, Sweden), a custom-made software developed for acquisition and analysis of physiological signals measured in experimental animals.
Approximately 20 minutes after the completion of the preparation when the rabbit was hemodynamically and electrophysiologically stable, control measurements were undertaken. Subsequently, 3 increasing doses of AZ13395438 were administered as 15-minute consecutive intravenous infusions followed by washout for 60 minutes. The electrophysiological measurements and recordings were carried out according to a predefined protocol and arterial blood for subsequent analysis of AZ13395438 concentrations and ex vivo protein binding were drawn at predefined time points. The primary variable of interest was the predicted (see methods for pharmacokinetic/pharmacodynamic [PKPD] modeling below) unbound plasma concentration increasing RAERP by 20 milliseconds (C eu20). If possible, the unbound plasma concentration increasing the QT interval by 10 milliseconds (C eu10) was also predicted.
Antiarrhythmic Efficacy Assessment of AZ13395438 During 8 Weeks of RAP in Dogs
Five female Beagle dogs (13.5-14.9 kg body weight) were implanted with a neurostimulator (Itrel 3, Medtronic Inc, Minneapolis, Minnesota) in a subcutaneous pocket and connected to a pacing electrode inserted via the right jugular vein and positioned endocardially in the right atrium by means of fluoroscopic guidance. Once every week during an 8-week RAP period the pacemaker was temporarily switched off. If the conscious dog was in AF and the episode lasted longer than 5 minutes, either saline or AZ13395438 (1:1 randomization, Figure 1) was intravenously administered for 30 minutes maximum. At occasions when the pacemaker was switched off and AF was not observed, burst pacing (50 Hz for 5 seconds) was applied in an attempt to induce AF. If AF lasting >5 minutes could be induced, AZ13395438 or saline was infused as described above. If sinus rhythm was restored by any of the interventions, the infusion was stopped and an attempt to reinduce AF by burst pacing was immediately undertaken. Arterial blood was sampled after a successful conversion and after any reinducibility attempt. Subsequently, the pacemaker was turned on and the dog was brought from the laboratory to its normal pen housing. Hence, except for the weekly interventions (lasting for 45 minutes maximum) during which the pacemaker was turned off, the dogs were subjected to continuous RAP.

Randomization to AZ13395438 (AZ) or saline (Ve) treatment (30 minutes infusion maximally) aiming at restoring sinus rhythm in 5 dogs subjected to rapid atrial pacing (RAP) for 8 weeks. Antiarrhythmic efficacy was assessed once every week when RAP was discontinued and treatment was given only if an AF episode lasting more than 5 minutes was observed; otherwise the pacemaker was turned on again. Before commencement of RAP the dogs were randomized to the specific treatment to be administered at week 1. If no treatment was given at week 1 (as AF was seen or the episode was shorter than 5 minutes), the dog remained on the same randomized treatment at the next efficacy assessment (in this case week 2). The figure illustrates at what occasions during the pacing period the dogs were randomized to either AZ13395438 (open cells) or saline (filled cells). Empty cells indicate that no treatment was given and AZ or Ve within the cells indicate that AZ13395438 or saline, respectively, was infused. In total, AZ13395438 and saline was administered at 12 and 10 occasions, respectively. For further details see Methods section. AF indicates atrial fibrillation.
During the antiarrhythmic efficacy assessments, the target unbound plasma concentration of AZ13395438 at the end of the 30 minutes infusion was 0.6 µmol/L. Dosing regimens in each individual dog were defined through pharmacokinetic simulation taking into account ex vivo plasma protein binding and pharmacokinetic characteristics of AZ13395438 generated in separate experiments before the RAP was initiated. Hence, each dog was individually dosed at infusion rates ranging from 0.11 to 0.19 µmol/kg per min.
For estimation of the dominating AF frequency and cycle length, digitized (1 kHz) ECG signals from lead II were detrended and denoised using Coiflet Wavelet algorithms. 12 QRST complexes were then canceled using an average beat subtraction algorithm based on QRST complex detection by template matching. The derived signal was subjected to a discrete Fourier transformation (30 seconds intervals), displayed as a power spectrum, and the dominating frequency was subsequently estimated.
Electrophysiological Characterization in the Anesthetized Dog
The dogs subjected to 8 weeks of RAP and 4 naive dogs were anesthetized with propofol, buprenorphine, and sodium pentobarbital and artificially ventilated. Blood gases and pH in arterial blood were measured and, if necessary, adjusted. The rectal temperature was kept between 37.7°C and 39.2°C by covering the animals and by external heating.
Percutaneous catheters for administration of anesthetics, sodium bicarbonate, Ringer solution, and AZ13395438, respectively, were inserted into the brachial veins. A polyethylene catheter was inserted into the left femoral artery and advanced to the level of the aortic arch for blood pressure recording by means of a pressure transducer and for blood sampling. For recording of right atrial and ventricular electrograms and for atrial and ventricular pacing, two 6F quadripolar electrophysiological recording catheters were advanced into the right femoral vein and positioned high up in the right atrium and in the apex of the right ventricle. To reach the left atrium for recording and pacing, a 7F quadripolar electrophysiological catheter was inserted into the left jugular vein, via the right atrium, and positioned in the coronary sinus. All electrodes were advanced via introducers by means of the Seldinger technique and correctly positioned through fluoroscopic guidance. The RAERP and the left atrial and the right ventricular effective refractory periods (LAERP and RVERP, respectively) were determined at a stimulation current strength approximately 1.2- to 2-fold above the threshold for capture at a basic cycle length of 350 milliseconds. The effective refractory periods were measured as described above. A 7F transducer was positioned in the left ventricle via the right carotid artery for measurement of the maximal rate of left ventricular pressure development (max dP/dt). All signals were amplified, recorded and sampled, and data processed as described above.
Approximately 1 hour after the completion of the animal preparation, predrug (control) measurements were carried out. After 2 control measurements the dogs were administered AZ13395438 as 2 consecutive 45-minute infusions at different rates followed by a washout (drug-free) period for approximately 90 minutes. Hemodynamic and electrophysiological measurements were repeatedly carried out during the infusion and washout and arterial blood samples for determination of plasma levels of AZ13395438 and ex vivo plasma protein binding were drawn at predefined time points.
Determination of AZ13395438 in Plasma and Ex Vivo Protein Binding
Blood samples were centrifuged for 5 minutes (5000 g at 4°C). The plasma was stored at −20°C until analysis. The drug analysis was performed on a short reversed-phase high-performance liquid chromatography (HPLC) column with rapid gradient elution and mass spectrometric (MSMS) detection. Plasma for measurement of ex vivo plasma protein binding was transferred to a dialysis plate with a membrane separating the plasma from a phosphate buffer. After equilibrium dialysis with incubation at 37°C for 18 hours, plasma and buffer samples were precipitated with acetonitrile and centrifuged. The supernatant was diluted with water and 0.2% formic acid (1:1) and then 20 times with acetonitrile (37.5%, 0.2% formic acid) before analysis on a reverse-phase HPLC column with gradient elution and MSMS detection.
Pharmacokinetic/Pharmacodynamic Modeling of Electrophysiological Variables
Pharmacokinetic analysis was performed by fitting a 2-compartmental model to the concentration–time profiles after the constant intravenous infusions, according to the following equations:
where C p and C t represent the concentration of test compound in plasma and peripheral compartment, respectively. The CL denotes clearance and CL D the intercompartmental distribution parameter. The V c and V t are the volumes of the central and peripheral compartment, respectively. The test compound input is defined as several consecutive constant intravenous infusions with variable lengths. All measured plasma concentrations were expressed as unbound plasma concentration, calculated from total plasma concentration and individual ex vivo plasma protein binding. Subsequently, individual parameter estimates were used to calculate individual test compound plasma concentrations at the times when the test compound induced change in the recorded variables using equation (1).
For modeling purposes, the effect variables were expressed as delta milliseconds change compared to an initial reading taken before the start of infusion.
13
The temporal differences between plasma concentration and effect were demonstrated by inspection of the hysteresis which was observed by plotting plasma concentrations versus the change of the effect parameter in time order. A first-order distribution delay of the test compound to and from the biophase was assumed to be the rate-limiting step, and an effect-compartment model was used, where the concentration in the effect compartment (biophase) is linked to the plasma compartment by a first-order rate equilibrium rate constant k
e0. The rate of change of test compound in the effect compartment can then be expressed by
where C p represents the plasma concentration as a table function and C e the concentration in the effect compartment.
The half-life of the equilibrium constant (t
½ke0) was estimated as
The concentration in the biophase was assumed to be directly proportional to an increase in the recorded variable according to the exponential relationship
where a and b define the slope in the exponential equation (4). The primary goal of fitting equation 4 to the response–time data was to calculate the unbound plasma concentration of AZ13395438 (C
eu20) resulting in a 20 millisecond (RAERP and LAERP) or 10 millisecond (RVERP and QT interval) increase in response by rearranging equation 4 and solving for C
eu20:
Individual regression analyses were carried out using WinNonlin (Version 4.1. Pharsight Corporation, St Louis, Missouri, USA) and user-specified models. Model selection was based on goodness-of-fit and precision of parameter estimates.
Statistics
Results are presented as means ± standard error of the mean and n indicates number of observations. Student t test, repeated measures analysis of variance, Dunnet multiple comparison test, and Fisher exact probability test were used for statistical evaluation. A P value less than .05 was considered as statistically significant.
Results
Ion Channel-Blocking Effects In Vitro
AZ13395438 blocked several cardiac ion channels in a concentration-dependent manner. In CHO cells, the recombinant hKv1.5 and hKir3.1/hKir3.4 channels were most potently blocked by the compound whereas hKv4.3/KChIP2.2 and hNav1.5 were less sensitive to the block (Table 1). The late repolarizing channels hERG and hKvLQT1/hminK as well as hCav1.2 were not markedly affected within the concentration range studied.
Ion Channel-Blocking Profile of AZ13395438 in Human Atrial Myocytes or Chinese Hamster Ovary (CHO) Cells.a

Abbreviation: CHO, Chinese hamster ovary; IC50, half maximal inhibitory concentration; SEM, standard error of the mean.
aData given as best-fit values ± SEM. Curves were fitted to replicate data using nonlinear regression by means of a 4 parameter logistic (curve top, slope and IC50 variable, curve bottom normalized to 0).
In acutely isolated human atrial cells, AZ13395438 blocked IKur and Ito at equal potency. When compared to the effects seen in the CHO cells, the potency was markedly higher (Table 1).
Electrophysiological Action in Anesthetized Rabbits
The infusion of AZ13395438 was associated with a concentration-dependent increase in RAERP (Figure 2), whereas the QT interval was only minimally altered. Hence, at the end of each infusion, the RAERP increased by 9 ± 2, 21 ± 6, and 46 ± 11 milliseconds (all P <.05 vs predrug). The corresponding changes in the QT interval were −1 ± 1, 0 ± 1, and 3 ± 3 milliseconds, respectively. PKPD modeling was applied to predict the unbound plasma concentration of AZ13395438 increasing RAERP by 20 milliseconds (Ceu20) and QT interval by 10 milliseconds (Ceu10). The average protein binding in the rabbits was 44% (range 36%-50%). The modeling showed that C eu20 for RAERP was 0.2 ± 0.039 µmol/L. The C eu10 for the QT interval could not be predicted due to the small effects on QT (Figure 3). Heart rate, mean aortic blood pressure, and atrioventricular conduction time (measured as the interval from the end of the P wave to the start of the Q wave of the surface ECG) were not significantly altered by AZ13395438 (data not shown). When compared to the predrug level, the QRS interval was marginally, but statistically significantly, increased at the end of the third infusion of AZ13395438 (from 36 ± 1 to 41 ± 1 milliseconds, P < .01).

Concentration-dependent changes in the right atrial effective refractory period (RAERP) and the QT interval by AZ13395438 in anesthetized rabbits. AZ13395438 was administered as 3 consecutive 15-minute intravenous infusions and RAERP measurements were carried out at the end of each infusion at the unbound (Cu) plasma concentrations indicated in the figure and at a cycle length of 250 ms. Results shown are means ± standard error of the mean (SEM; n = 5); *P < .05 versus predrug.

Observed change in the right atrial effective refractory period (RAERP) in anesthetized rabbits during 3 consecutive 15-minute intravenous infusions of AZ13395438 followed by washout for 60 minutes, plotted against unbound plasma concentration in time order (left panel). Simulation of the AZ13395438-induced changes in RAERP plotted against effective unbound plasma concentration (C eu, right panel).
Antiarrhythmic Efficacy of AZ13395438 During 8 Weeks of RAP in Dogs
Five dogs were subjected to RAP for 8 weeks. On a weekly basis, the pacemaker was turned off and the presence, inducibility, and reinducibility of AF were examined. In total, 22 episodes of AF lasting more than 5 minutes were observed and at these instances either AZ13395438 (n = 12) or saline was infused for 30 minutes maximum in an attempt to restore sinus rhythm. Following the conversion, the drug or saline infusion was immediately stopped and an arterial blood sample was taken. AZ13395438 successfully restored sinus rhythm at all attempts whereas saline converted 4 of the 10 episodes only (P = .003 vs AZ13395438, Figure 4). The time to conversion was 488 ± 78 seconds during AZ13395438 infusion and 1010 ± 330 seconds during saline infusion. The unbound plasma concentration of AZ13395438 at the time of the conversion was 0.48 ± 0.076 µmol/L. The infusion of AZ13395438 was associated with a progressive increase in AF cycle length. Hence, immediately before the conversion of AF was observed the AF cycle length had increased from 73 ± 1 (predrug) to 89 ± 2 milliseconds (P < .001). Following the successful conversion of AF by AZ13395438, an attempt to reinduce AF was carried out. In only 3 of 12 attempts could AF be reinduced (P < .001 vs the inducibility prior to AZ13395438 infusion, Figure 3). Immediately after the inducibility attempt, the unbound plasma concentration of AZ13395438 had fallen to 0.26 ± 0.04 µmol/L.

Conversion of atrial fibrillation (AF) to sinus rhythm and efficacy of AZ13395438 in inhibiting reinduction of AF by burst pacing following successful restoration of sinus rhythm in 5 dogs subjected to rapid atrial pacing for 8 weeks. On a weekly basis, the dogs were checked for presence of AF or, if AF was not seen, subjected to burst pacing to induce AF. For AF episodes lasting longer than 5 minutes, AZ13395438 or saline (1:1 randomization) was infused for 30 minutes maximum in an attempt to restore sinus rhythm.
Electrophysiological and Hemodynamic Effects of AZ13395438 in Naive and Tachypaced Dogs
The electrophysiological and hemodynamic characteristics of AZ13395438 were assessed in anesthetized naive dogs and in the dogs subjected to RAP for 8 weeks. Before administration of AZ13395438, RAERP and LAERP were significantly abbreviated in the dogs subjected to RAP when compared to the naive dogs (Table 2). In contrast, RVERP and the atrioventricular conduction time were significantly longer in the former group whereas ventricular conduction time (QRS interval) and repolarization (QT interval) did not differ between the 2 groups of the dogs. Heart rate, mean aortic blood pressure, and left ventricular max dP/dt were significantly lower in the RAP dogs versus the naive dogs which may indicate a negative impact of the persistent rapid atrial rate on the ventricular function.
Baseline Electrophysiological and Hemodynamic Characteristics in Naive and Dogs Subjected to 8 Weeks of Rapid Atrial Pacing.a

Abbreviations: RAERP, right atrial effective refractory period; LAERP, left atrial effective refractory period; RVERP, right ventricular effective refractory period; AV time, atrioventricular conduction time (measured from the end of the P wave to the start of the Q wave of the surface ECG); HR, heart rate; AOP, aortic blood pressure; max dP/dt; maximal left ventricular pressure development; SEM, standard error of the mean.
aAll variables except HR were recorded or measured at a paced cycle length of 350 milliseconds. Shown are means ± SEM.
b P < .01 versus naive dogs.
c P < .001 versus naive dogs.
d P < .05 versus naive dogs.
The plasma concentration–time profiles of unbound AZ13395438 were similar in the naive and the RAP dogs during the 2 consecutive infusions and the washout period (Figure 5A). The infusion was associated with a concentration-dependent increase in RAERP and LAERP (Figure 5B and C). Quantitatively, the maximal increases were similar in both the right and the left atrium and did not differ between naive and RAP dogs. Likewise, both RVERP and the QT interval increased in a concentration-dependent manner (data for RVERP shown in Figure 5B and C), but the magnitude of the increase was smaller than the increase in atrial refractoriness. The protein binding in the naive and RAP dogs was 85% (range 72%-91%) and 84% (range 68%-95%), respectively. The PKPD modeling of the data predicted a C eu20 for RAERP and LAERP in the naive dogs of 0.38 ± 0.079 and 0.36 ± 0.067 µmol/L and a C eu10 for RVERP of 0.22 ± 0.012 µmol/L, respectively (Figure 6 and Table 3). In the RAP dogs, the corresponding values were 0.34 ± 0.057 (not significant [NS] vs naive dogs), 0.25 ± 0.040 (NS), and 0.35 ± 0.029 (P < .05) µmol/L, respectively (Figure 7 and Table 3). When compared to predrug levels, AZ13395438 did not change the QRS interval, mean aortic blood pressure, left ventricular max dP/dt, or heart rate in the naive dogs (data not shown). Similarly, in the RAP dogs the QRS interval, mean aortic blood pressure, and heart rate were unaltered whereas the ventricular max dP/dt was significantly reduced from 2422 ± 108 to 1977 ± 116 mm Hg/s (P < .001) at the end of the second infusion of AZ13395438. The atrioventricular conduction time and the QT interval were concentration dependently increased in both the groups of dogs (from 45 ± 2 to 62 ± 2 milliseconds [P < .001] and from 159 ± 2 to 170 ± 2 milliseconds [P < .05] in naive dogs and from 93 ± 9 to 119 ± 7 milliseconds [P < .001] and from 165 ± 4 to 186 ± 6 milliseconds [P < .05] in RAP dogs, respectively).

Plasma concentrations (panel A) and effects of an intravenous infusion of AZ13395438 on change in the right atrial (RAERP), left atrial (LAERP), and right ventricular (RVERP) effective refractory periods in anesthetized naive dogs (n = 4, panel B) and anesthetized dogs subjected to 8 weeks of rapid atrial pacing (n = 5, panel C). AZ13395438 was administered as 2 consecutive 45-minute intravenous infusions followed by washout for 90 minutes. Results shown are means ± standard error of the mean (SEM).

Observed change in the right and left atrial effective refractory period (RAERP [upper panels] and LAERP [lower panels]) in anesthetized naive dogs during 2 consecutive 45-minute intravenous infusions of AZ13395438 followed by washout for 90 minutes, plotted against unbound plasma concentration in time order (left panels). Simulation of the AZ13395438-induced changes in RAERP (upper) and LAERP (lower) plotted against effective unbound plasma concentration (C eu; right panels).

Observed change in the right and left atrial effective refractory period (RAERP [upper panels] and LAERP [lower panels]) in anesthetized dogs subjected to 8 weeks of rapid atrial pacing, during 2 consecutive 45-minute intravenous infusions of AZ13395438 followed by washout for 90 minutes, plotted against unbound plasma concentration in time order (left panels). Simulation of the AZ13395438-induced changes in RAERP (upper) and LAERP (lower) plotted against effective unbound plasma concentration (C eu; right panels).
Predicted Estimates of Unbound Plasma Concentrations of AZ13395438 Increasing Atrial and Ventricular Effective Refractory Periods in Naive Dogs and in Dogs Subjected to Rapid Atrial Pacing for 8 Weeks.a

Abbreviations: LAERP, left atrial effective refractory period; RAERP, right atrial effective refractory period; RVERP, right ventricular effective refractory period; C eu20, unbound plasma concentration of AZ13395438 increasing LAERP or RAERP by 20 milliseconds; C eu10, unbound plasma concentration of AZ13395438 increasing RVERP by 10 milliseconds; RAP, rapid atrial pacing; SEM, standard error of the mean.
aResults are given as µmol/L and as means ± SEM.
Discussion
The present series of experiments were undertaken to examine the ion channel-blocking potency in vitro and the electrophysiological, hemodynamic, and antiarrhythmic efficacy in vivo of the investigational antiarrhythmic agent AZ13395438. The characterization shows that AZ13395438 may best be described as a mixed K+ ion channel blocker. Consistent with its ion channel-blocking activity, AZ13395438 predominantly increases atrial refractoriness with proportionately smaller effects on ventricular repolarization and refractoriness and possesses promising anti-AF efficacy. Considering these observations, AZ13395438 shares several characteristics in common with the atrial-selective antiarrhythmic agents vernakalant and AVE0118, both of which block early repolarizing currents in the atrium. 14 –17 Vernakalant has demonstrated effectiveness in restoring sinus rhythm in patients with AF and is currently approved for conversion of recent onset AF in Europe. AVE0118, on the other hand, showed very promising antiarrhythmic efficacy in goats with pacing-induced persistent AF and was thus brought into clinical testing for rapid intravenous conversion of AF. However, the outcome of these studies has never been publicly disclosed.
Of the heterologously expressed ion channels studied, Kv1.5 was most potently blocked by AZ13395438. The potent blockade was further verified in the acutely isolated human atrial myocyte. Somewhat surprisingly, the potency was much higher in blocking IKur in the myocyte than Kv1.5 in the CHO cell. A similar difference in blocking potency has previously been described for the IKur-blocking compounds S9947 and AVE0118. 18,19 The reason for the discrepancy is not obvious but may be due to different current recording techniques, that is, automated planar patch clamping versus conventional patch clamping. Differences in α and β subunit interactions may also explain the increased relative potency in blocking Ito versus hKv4.3/hKChIP2.2. 20 An alternative explanation assuming an intracellular blocking site (ie, pore region) may be interference with drug transporters in such a way that the effective concentration at the blocking site differs between the cell types. 21 Kv1.5 is the molecular correlate of IKur in several species including man, dog, and rabbit and plays a crucial role in early atrial repolarization. 5,22,23 As Kv1.5 is selectively expressed in atrial tissue in the human heart, it has been seen as a highly interesting drug target for effective and safe treatment of AF for several years. Very few selective Kv1.5 drug candidates have been forwarded into clinical concept testing, however, and the effectiveness of the approach is still unproven. In a recent study, Pavri and colleagues demonstrated MK 0448 to be a potent blocker of IKur with minimal off target activity in vitro and selective action on atrial versus ventricular electrophysiology and antiarrhythmic efficacy in anesthetized dogs in vivo. 24 Surprisingly, MK 0448 did not increase atrial refractoriness in young healthy participants. The lack of electrophysiological effect was suggested to have been due to attenuated contribution of IKur to atrial repolarization by enhanced vagal tone and the therapeutic value of specific IKur blockade for AF management was questioned. 24 However, considering previous observations of improved efficacy of IKur blockade in remodeled atrial tissue, the clinical value of this strategy still awaits critical assessment in the target AF population. 6,7
AZ13395438 did not only block Kv1.5 but also had affinity toward IKACh. This particular inward rectifier seems selectively expressed in atrial versus ventricular tissue and its blockade has been demonstrated to result in increased atrial refractoriness and antiarrhythmic efficacy while minimally influencing ventricular electrophysiology. 8
In vivo, AZ13395438 was found to selectively increase atrial refractoriness in the rabbit. However, in the dog, AZ13395438 increased the RVERP by approximately 15 milliseconds at the same unbound plasma concentration. The explanation for the ventricular action in dogs may be due to the fact that Kv1.5 messenger RNA (mRNA) and protein have been detected in canine ventricular myocytes. Accordingly, Sridhar and colleagues found that DPO-1, an IKur-selective compound, prolonged action potential duration in canine left ventricular myocytes. 25 Hence, Kv1.5 blockade will inevitably result in increased ventricular refractoriness and QT prolongation in that species. 5,26 On the other hand, one may argue that this is not the primary mechanism underlying the effect seen in the dog ventricle as Kv1.5 mRNA also seems highly expressed in rabbit ventricular tissue and AZ13395438 did not influence ventricular refractoriness in the rabbit in the present study. 22 However, since IKr is critically important for ventricular repolarization in rabbits, the lack of effect on the QT interval may suggest that Kv1.5 is of less relative importance for ventricular repolarization in this species. 27 Moreover, the lack of effect on the QT interval further argues against a blockade of IKr as the underlying cause for the observed increase in the canine ventricular refractoriness. AZ13395438 also showed low potency in vitro in blocking hERG and IKs.
The electrophysiological effects of AZ13395438 were compared in naive dogs and in dogs subjected to 8 weeks of RAP to induce myocardial remodeling and AF. The RAP was associated with pronounced atrial remodeling shown as significant abbreviations in the right and left atrial refractoriness. These changes are in line with numerous animal studies and clinical observations showing that atrial tachycardia and AF for extended periods result in atrial electrical remodeling. 28 Furthermore, we also found that the atrioventricular node conduction time was significantly longer and ventricular rate was slower in the RAP dogs than in the naive dogs. This observation is in agreement with findings in a recent study by Zhang and Mazgalev who demonstrated pronounced atrioventricular node functional electrophysiological remodeling and slowing of ventricular rate after long-term AF. 29 It was suggested that the increased refractoriness of the atrioventricular node may underlie the spontaneous and progressive slowing of the ventricular rate as the arrhythmia persists. In the present study, we also found the right ventricular effective refractory period to be significantly longer in the tachypaced dogs which indicates that the RAP results not only in atrial, but also in ventricular electrical remodeling. Based on the invasive hemodynamic assessments, it was obvious that the long period of rapid pacing attenuated ventricular function as both arterial blood pressure and left ventricular pressure development were markedly reduced. When establishing our experimental AF model we wanted to avoid chronic atrioventricular blockade and ventricular demand pacing techniques that have been frequently applied in similar AF models. 30 As a means to reduce the impact of the rapid atrial rate on the ventricle, we screened for dogs with long atrioventricular refractory periods. Thus, only dogs with a ventricular response rate below 125 beats per minute (bpm) during atrial pacing at 400 bpm were used in the study. Despite this approach, unpublished results from our laboratory indicate that long periods of atrial tachycardia are associated with attenuated ventricular ejection function. Hence, as several animal and clinical studies have provided evidence that the most consistent ion channel alteration in heart failure is a decrease in Ito, it is likely that such alterations underlie the prolonged ventricular refractory period we observed after 8 weeks of RAP.
In the present study, we applied a PKPD modeling approach to predict the unbound plasma concentration of AZ13395438 increasing the atrial effective refractory period by 20 milliseconds. An increase to such an extent has been suggested to translate into antiarrhythmic efficacy. 31 Based on the PKPD modeling of the exposure data and the efficacy data, the potency of AZ13395438 was found to be similar in naive and tachypaced dogs. Furthermore, the changes in the refractory period were similar in the left and the right atrium. The pronounced effect of AZ13395438 in the electrically remodeled atria is in accordance with findings by others who found that AVE0118 and the selective IKur blocker XEN-D0101, but not the selective IKr blockers dofetilide or ibutilide, significantly increased the effective refractory period in the remodeled atria of the goat and the dog. 5,14
The efficacy of AZ13395438 in converting AF to sinus rhythm and inhibiting reinducibility of AF was assessed weekly in the conscious dog during the 8-week pacing period. When compared to the vehicle, AZ13395438 was significantly more efficacious in rapidly restoring sinus rhythm and effectively inhibited reinduction of AF. The conversion of AF was preceded by a significant increase in AF cycle length which was in line with the previous findings. 14 Considering the fact that the unbound plasma concentration of AZ13395438 at the time of the conversion of AF and the attempt to reinduce AF fell in the ranges of the unbound plasma concentrations where the atrial effective refractory period was increased by 20 milliseconds, one may speculate that in this animal model an increase in atrial refractoriness to such an extent may suffice to result in antiarrhythmic efficacy.
In conclusion, AZ13395438 is a mixed K+ ion channel blocker that selectively prolongs atrial refractoriness and shows promising antiarrhythmic effect in a clinically relevant animal model of AF. Based on these findings, AZ13395438 merits further investigation for antiarrhythmic efficacy in the clinical setting.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The authors are employed by AstraZeneca Plc.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.