Abstract
Objectives
This study aims to evaluate the perceived impact of extreme weather events from 2017 - 2024 on delivery of radiotherapy in Puerto Rico (PR), including effects on radiation oncologists, medical physicists, clinical staff, and patients. A secondary objective is to identify resources and strategies that may strengthen resiliency and support continuity of care in radiation oncology clinics located in weather-vulnerable regions.
Methods
We developed a comprehensive online cross-sectional survey to evaluate clinic emergency preparedness and the impact of extreme weather events on radiation oncology clinic stakeholders in PR. Potential participants were identified through the American Society for Radiation Oncology (ASTRO) membership directory and were invited to participate via email and direct outreach.
Results
Fourteen radiation oncologists and four medical physicists were invited to participate, with a response rate of 56% (n = 10), representing 71.4% of radiation oncology clinics in PR. Among respondents, 90% reported clinical disruptions due to extreme weather events from 2017 to 2024. The most commonly reported impacts were property damage (90%), communication failures between providers, patients and staff (90%), power outages (80%), and school and/or childcare closures (80%). A majority (90%) supported developing comprehensive supportive resources, including professional society resources, to enhance disaster preparedness and operational resiliency.
Conclusion
Radiation oncology providers in PR reported significant disruptions in care delivery from extreme weather events and identified a need for strong resiliency measures. Institutional policy, coupled with targeted support from professional societies, may reduce lapses in treatment, safeguard vulnerable patients – particularly those with complex treatment plans – and improve continuity of care and outcomes in weather-prone regions.
Plain Language Summary
Extreme weather events such as powerful hurricanes are becoming more common, especially in vulnerable places such as Puerto Rico. When Hurricane Maria struck in 2017, it exposed how fragile health systems can be during these crises. Cancer care is especially at risk because patients often depend on strict treatment schedules. Most past research has focused on the experiences of cancer patients, with limited attention given to the oncology providers that care for them. These providers have valuable insights on how to better prepare clinics and care for patients after extreme weather events. In our study, we surveyed oncology providers in Puerto Rico to understand how extreme weather events affect providers, patients, and staff, as well as how health systems prepare for and respond to these events. We found that nearly all providers were negatively impacted by extreme weather events. Providers, patients, and staff frequently experienced shortages in food, clean water, transportation, electricity, and healthcare access. Providers reported that strong community partnerships and institutional emergency plans were the most effective tools for getting cancer care quickly back on track. They also recommended and requested that professional medical societies create official platforms to share patient education, resources, and even financial support during such emergencies. By learning from the resilience of oncology providers in Puerto Rico, health systems everywhere can strengthen disaster preparedness, reduce harm to patients, staff, and providers, and improve the continuity of life-saving cancer care when extreme weather events occur.
Keywords
Introduction
Climate change is an increasingly pressing public health issue, driving an estimated six-fold increase in extreme weather events since 1980. 1 Even short disruptions of just 2 days, caused by power outages or interruptions to food and fuel supply chains, can negatively impact oncology patient outcomes and survival.2-7 High-intensity, climate-fueled hurricanes pose particular threats to healthcare delivery. Hurricane Maria, which struck Puerto Rico (PR) in 2017, exemplified these vulnerabilities, devastating infrastructure and contributing to nearly 3,000 excess deaths.2-5,7,8
Most research on this topic has focused almost exclusively on oncology patients, overlooking oncology providers.5-7 Providers bring critical insights into operational challenges, preparedness gaps, and opportunities to strengthen resiliency in cancer care systems following extreme weather events.5,6 Our study addresses this gap by examining radiotherapy delivery in PR, a setting characterized by the time-sensitive nature of cancer treatment and heightened regional vulnerability to extreme weather events.4,5 By assessing providers’ perceptions across multiple dimensions – including impacts on physicians, medical physicists, clinical staff, and patients, clinic operations and preparedness planning – we aim to capture a more comprehensive view of the health system-wide effects of extreme weather events. In addition, we seek to identify existing and desired resources that could enhance disaster preparedness, recovery, and long-term resiliency in oncology care delivery.
Methods
Survey Design
A comprehensive cross-sectional online survey was designed using Qualtrics Survey Software to assess providers’ perceptions regarding extreme weather events’ impact on radiation oncology care. The survey included multiple-choice and open-ended questions in English regarding respondent demographics, impact on providers (physicians and medical physicists), perceived impact on clinic staff and patients, clinic infrastructure, emergency preparedness, and suggested improvements. Responses were analyzed to assess variation of clinic locations and geographic distribution. The survey was modeled after a prior survey investigating California wildfires’ impact on oncology care and tailored to address extreme weather events in PR. 6 The survey was validated using semi-structured interviews and pilot testing to ensure clarity and alignment with the aim of our study. Pilot testing was performed from August-September 2023, with a small sample of independent US-based providers (n = 10) providing feedback on the survey’s format and content. This research was determined to be IRB exempt and conforms to STROBE guidelines. 8
Survey Distribution
The American Society for Radiation Oncology (ASTRO) membership directory, one of the largest professional oncology societies, was utilized to identify radiation oncologists and medical physicists practicing in PR. Through collaboration with a local physician in PR, two additional oncologists were identified and included in the survey. In total, 14 radiation oncologists and four medical physicists were invited via email to participate in the survey. Responses were collected using Qualtrics during a 12-week period from October 17th, 2023, to January 9th, 2024, with monthly automated email reminders. To enhance the response rate, a team member personally contacted the office staff of non-responding providers through personalized emails and phone calls in Spanish.
Statistical Analysis
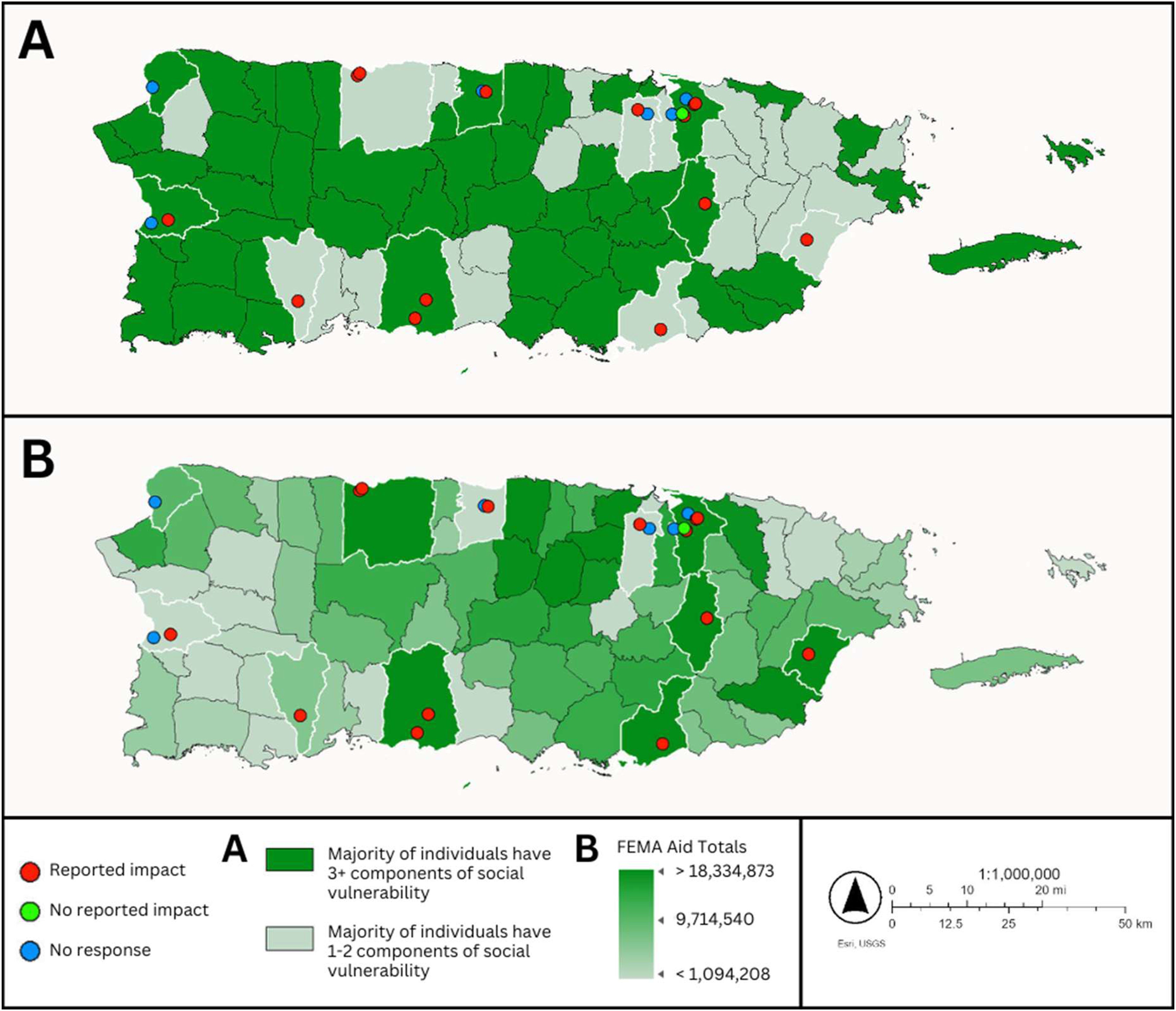
Provider demographics and clinic characteristics were summarized with descriptive statistics, including frequencies and percentages. Pearson’s χ2 tests were performed to investigate the likelihood of observed differences in the impact of extreme weather events on providers, patient and staff groups, (P-value 0.05). RStudio Desktop 2023.12.1-402 was used for all statistical analyses. Surveyed clinic locations were mapped according to US Census data on social vulnerabilities and FEMA aid distribution. 9
Results
Respondent Demographics
Demographic and Clinic Characteristics of Radiation Oncology Providers and Clinics in Puerto Rico (Survey Respondents n = 10)

a“Yes” represents the total number of responses to the question “Has your practice(s) been impacted by any of the following extreme weather events since 2017? This can include any aspect of your practice including, but not limited to, impacts on you, your staff, patients, operations, and/or clinic infrastructure. *Please select all that apply*”

Impacts on Practices & Personnel
Perceived and Self-Reported Impacts of Extreme Weather Events on Radiation Oncology Providers, Staff, and Patients in Puerto Rico (2017 to 2024)

aNine respondents answered these prompts directly. An n of 10 is used to account for the one respondent who indicated being unaffected by climate disasters.
bPearson χ2 values identify the differences in values between perceived impact on patients and physician/physicists.
cStatistical significance cut-off of P = 0.05.
Conditional formatting was applied to highlight significant impacts. The darker the shade of red, the more highly endorsed that experience was by respondents.
Operational and Infrastructure Impacts on Radiation Oncology Clinics in Puerto Rico due to Extreme Weather Events (2017-2024)

aNine respondents answered these prompts directly, n = 10 is used to account for the one respondent who indicated they were unaffected by extreme weather events.
Conditional formatting was applied to highlight significant impacts.
Health System Preparedness
Nine respondents reported implementing a workplace emergency preparedness plan, with seven including patient transfers, and six offering emergency preparedness counseling to patients. Most respondents felt their workplace was somewhat or very well prepared for an extreme weather event. Institutional preparedness plans were the most helpful resource, followed by local/state health department partnerships and community-based organizations. 80% of respondents agreed their professional society has a responsibility to prepare clinicians for climate-related care disruptions through an official platform offering patient education materials, online resources and financial assistance/grants.
Discussion
This study provides important insights into the impact of extreme weather events on delivery of radiotherapy in PR, building upon existing literature while introducing novel evidence of provider perspectives.2-7 PR municipalities serving more socially vulnerable patients often receive less disaster relief funding and experience higher rates of disrupted care.5,6 This disparity underscores the importance of developing both community-based and institutional preparedness strategies that intentionally address the needs of vulnerable patient populations and their specific treatment needs.2-7,9,10
One-third of respondents reported inadequate workplace preparedness, highlighting opportunities for professional societies to advance cost-effective resiliency strategies and support their implementation through a variety of channels including grants. For example, sample ‘catch-up’ radiation schedules are an evidence-based tool to mitigate the harms associated with treatment interruptions. 4 Comprehensive cancer control plans offer additional frameworks for disruption.5,9 Coordinated efforts among institutions, policymakers, and supply chain stakeholders are critical for ensuring treatment continuity and reducing care gaps.3,7 Emerging technologies such as ReadyMapper – which tracks real-time migration during extreme weather events – may further enhance preparedness, though their utility may be constrained by cost, licensing requirements, and patient consent.2,11
Our study has limitations. Providers reported patient and staff experiences indirectly rather than these groups being directly surveyed, which may introduce reporting bias. Recall bias is also possible given the extended timeframe (2017-2024). The sample size was inherently limited by focusing on a small island and a specific medical specialty. Additionally, the total number of oncology providers in PR is unknown as no centralized registry exists. To mitigate this limitation, we identified participants through the ASTRO membership directory, one of the largest professional oncology databases. While non-ASTRO providers in PR may have been excluded, ASTRO members likely represent the broader provider population given their wide geographic distribution. 5 Although English proficiency requirements for PR medical schools reduce the likelihood of language barriers, some providers with limited proficiency may have abstained from participation. 12
Despite these limitations, the study has several notable strengths. Focusing on PR, a region highly vulnerable to extreme weather events, provides crucial insights into challenges of cancer care delivery in disaster-prone contexts. The culturally sensitive survey design and direct outreach facilitated a representative sample that included medical physicists, whose perspectives have been largely absent from prior research, thereby broadening understanding of the full oncology care team’s experiences.5,10 Additionally, our use of validated survey methods, including pilot testing, strengthens the reliability and credibility of our findings. Together, these contributions enhance the evidence base for advancing disaster preparedness, recovery, and resiliency in radiation oncology.
Conclusion
While the unique challenges of PR may limit the generalizability of our findings, many are relevant across diverse practice settings and can be expanded upon through future research that characterizes the most effective interventions and catch-up schedules for disruptions in care. A bilingual longitudinal survey that integrates broader support staff perspectives (radiation therapists, administrative assistants, etc.), direct patient-reported outcomes and assesses clinical site demographics and their experiences individually would strengthen our findings and reduce recall bias.
Our findings underscore the devastating impacts of extreme weather events on both providers and patients, while highlighting opportunities for policy interventions in radiation oncology. This study reinforces the need for robust, equitable disaster preparedness strategies that safeguard vulnerable patients and ensure continuity of complex cancer treatments.2,3,5,7 Professional societies could play a critical role in supporting these efforts by developing adaptable guidelines, resource mobilization, and advocacy.2,3,5,7 By systematically reassessing after extreme weather events and addressing resource and preparedness deficits, healthcare systems may strengthen resiliency, reduce treatment disruptions, and ultimately improve oncology patient outcomes and survival.
Footnotes
Ethical Approval
This research study was found to be IRB exempt.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
