Abstract
Background
Vaccine hesitancy among young Chinese remains a challenge, contributing to low vaccination rates for the nonavalent Human Papillomavirus (HPV) vaccine. This study evaluated the knowledge and acceptance of this vaccine among students at a southern Chinese university and identified factors influencing these outcomes.
Methods
This cross-sectional, anonymous questionnaire survey was conducted from April to November 2023 at a multi-campus university in southern China. The questionnaire was comprised of three sections: the first collected demographic data; the second evaluated students’ knowledge of the nonavalent HPV vaccine on a scale from 0 to 15, with cut-off points at 5 and 10 delineating low, medium, and high knowledge levels, respectively; the third section assessed vaccine acceptance on a scale from 8 to 40, using scores above the 50th percentile as the benchmark for positive acceptance.
Results
Among the participants, 18% demonstrated low-level, 40.20% medium-level, and 41.70% high-level knowledge of the nonavalent HPV vaccine. Notably, 71.95% of respondents showed positive acceptance, whereas 28.05% expressed negative acceptance. Male students and those with lower economic conditions (monthly living expenses below 1000 RMB, P = 0.004; 1000-1499 RMB, P = 0.012) exhibited lower knowledge levels. As for acceptance, female students and those with higher monthly living expenses (1000-1499 RMB, P = 0.007; 1500-1999 RMB, P = 0.002; over 2000 RMB, P = 0.002) demonstrated greater vaccine acceptance. A positive correlation was noted between the level of knowledge and vaccine acceptance (rs = 0.256, P < 0.001).
Conclusions
Gender and economic status are significantly associated with nonavalent HPV vaccine knowledge and acceptance among university students. These findings highlight the potential impact of targeted educational initiatives, especially for economically disadvantaged male students, in enhancing vaccine uptake rates.
Plain Language Summary
Many young people in China are hesitant to get the nine - valent HPV vaccine, which protects against certain types of viruses that can cause cancer. This study looked at how much students at a university in southern China know about the nine - valent HPV vaccine and whether they are willing to get vaccinated. We asked students to fill out a survey between April and November 2023 to gather this information. The survey showed that knowledge about this vaccine varied: about 18% of the students knew very little, 40% had a moderate understanding, and roughly 42% knew a lot about this vaccine. Interestingly, more than 70% of the students were open to getting the vaccine, but about 28% were not. We found that male students and those with less money generally knew less about the vaccine and were more likely to not accept it. There was also a clear link between how much students knew about the vaccine and their willingness to get vaccinated. This suggests that teaching students more about this vaccine, especially boys and those from poorer backgrounds, could encourage more of them to get vaccinated. This is important because increasing vaccine rates can help prevent diseases spread by the virus.
Introduction
Human papillomavirus (HPV) is a prevalent sexually transmitted pathogen comprising covalently closed double-stranded circular DNA viruses that specifically target human skin and mucosal tissues. Researchers have identified over 100 HPV subtypes, categorized into low-risk (eg, HPV6, 11, 40) and high-risk (eg, HPV16, 18, 31, 33) subtypes. 1 It has been reported that more than 85% of genital wart cases are associated with low-risk subtypes, particularly HPV6 and 11. 2 Additionally, these subtypes are implicated in the development of recurrent respiratory papillomatosis. 3 Infection with high-risk HPV strains can lead to malignant tumors in the reproductive system, including cervical, penile, and anal cancer, with cervical cancer being the most prevalent.4,5 Epidemiological data from 2020 indicate that cervical cancer was one of the top ten high-risk malignancies in China’s cancer incidence spectrum. 6 A modeling study revealed that the lifetime cost of treating various stages of HPV-related cancers in China exceeds USD 17,000. 7 Beyond the economic impact, HPV infection imposes significant physical and psychological burdens on those affected. Given that sexual contact is the primary transmission route for HPV, its societal impact is profound.8,9 Consequently, the prevention of HPV infection is of paramount importance.
The successful development and marketing of the HPV vaccine have introduced effective measures for the prevention of HPV infections, positioning cervical cancer as the only malignant tumor predominantly preventable through vaccination. 10 Globally, six types of HPV vaccines are available, comprising three bivalent, two quadrivalent, and one nonavalent vaccine.2,11 The World Health Organization deems vaccination of girls aged 9-14 as the most cost-effective public health strategy for the prevention of cervical cancer. 12 Moreover, substantial evidence supports the protective benefits of vaccinating adolescent girls and young women between 15 and 26 years against precancerous cervical lesions. 13 In 2014, the U.S. Food and Drug Administration approved the nonavalent HPV vaccine, targeting not only young women but also young men to prevent genital cancers, precancerous lesions, developmental abnormalities, and genital warts.14,15 Subsequently, on April 28, 2018, this vaccine received approval from the China Food and Drug Administration and was introduced to the market in mainland China, with a recommendation for its use in women aged 16-26.16,17
Research demonstrates that 5-8 years post-vaccination, infection rates for HPV types 16 and 18 have decreased significantly—by 83% among females aged 13-19 and by 66% among those aged 20-24. 18 The HPV vaccine effectively prevents infections of HPV-6, 11, 16, and 18 and associated external genital lesions in males aged 16 to 26. 19 Prompt vaccination within these age groups can facilitate the early eradication of reproductive cancers and precancerous lesions. Despite regional variations, vaccination rates among young men and women in China are predominantly low. 20 Studies reveal a hesitancy rate of 37.57% towards HPV vaccination among female university students, 21 with even more pronounced reluctance observed among males.20,22 Vaccine adoption is influenced by a multitude of factors including vaccine knowledge, acceptance, availability, and cost.20,23 Increasing awareness of HPV and its vaccine has been shown to significantly reduce vaccination hesitancy and enhance its widespread acceptance.24,25 In this context, we conducted a cross-sectional study at a comprehensive university in southern China, spanning three campuses, to explore the knowledge and acceptance of the nonavalent HPV vaccine among university students and to analyze influencing factors. Our findings may offer practical intervention strategies to improve vaccination rates among targeted age groups.
Methods
Study Design
This study rigorously adheres to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. 26 Between April and November 2023, a cross-sectional survey was conducted at a comprehensive university in southern China comprising three campuses: Xianxi, Jiangwan, and Hebin. The Xianxi campus offers engineering, science, agriculture, medicine, literature, and education, while the Jiangwan campus includes science, engineering, arts, management, economics, and law, both sharing similar student demographics. In contrast, Hebin primarily focuses on medical disciplines with a smaller student body.
Recruitment utilized convenience and snowball sampling methods across campuses, with the distribution of emails, links, and QR codes via educational and social media platforms including email, WeChat, QQ, and Xuexitong. This strategy facilitated the dissemination of the informed consent and questionnaire. Participation was contingent upon agreement to the informed consent; those who did not agree were excluded, thus affirming the voluntary nature of the study. The survey was conducted anonymously, ensuring all participant details were de-identified to maintain confidentiality. The online questionnaire mandated responses to all questions, eliminating incomplete submissions and limiting entries to one per device or IP address to prevent duplicate responses. It explicitly stated that there were no right or wrong answers, encouraging participants to answer truthfully.
Inclusion and Exclusion Criteria
The study’s inclusion criteria were: (1) undergraduate status at one of the campuses, (2) awareness of personal health, (3) voluntary participation with informed consent, and (4) capability to understand and accurately complete the questionnaire. Exclusion criteria were: (1) participation under two minutes, (2) uniform responses across all questions, and (3) birthdates outside the typical college age range, such as being identical to the questionnaire completion date. Based on these criteria, 410 participants were ultimately included in the study, which received approval from the Medical Ethics Committee of Foshan University (approval number FUME2023017).
Sample Size
We utilized Power Analysis and Sample Size software, version 15.0, to estimate the necessary sample size. Literature review and pilot study findings indicated that awareness of the nonavalent HPV vaccine among university students was 60%, with an acceptance rate of approximately 70%.27,28 For precise analysis of the factors affecting vaccine awareness and acceptance, and with a tolerance of δ = 0.05 and a confidence level of 95% (1 – α), the estimated required sample sizes were 363 and 318 participants, respectively. Opting for the larger estimate and accounting for a 10% dropout rate, we set the required sample size at 400.
Data Collection
Informed by previous studies’ questionnaires and expert advice,29-31 we developed and validated a questionnaire, achieving a Cronbach’s Alpha of 0.897 to collect data. The questionnaire comprises three sections: the first gathers demographic data, including gender, age, major, ethnicity, academic level, monthly living expenses, and family location. The second section, consisting of 15 questions, evaluates students’ knowledge about the nonavalent HPV vaccine, with scoring options of correct (1 point), uncertain (0 points), and incorrect (0 points); scores range from 0-5 for low knowledge, 6-10 for moderate, and 11-15 for high knowledge. The third section, with eight questions, measures acceptance of the vaccine, using a 5-point Likert scale (1 for strongly disagree to 5 for strongly agree) to assess attitudes toward HPV prevention, control, vaccine promotion, and vaccination itself. Scores range from 8 to 40, with higher scores denoting greater acceptance. Scores above the 50th percentile (P50) indicate positive acceptance, while those below signify negative acceptance.
Data Analysis
Data were analyzed using International Business Machines Corporation Statistical Package for the Social Sciences (IBM SPSS) version 23.0. Descriptive statistics such as frequencies and percentages were used to summarize participants’ demographics, academic level, and levels of knowledge and acceptance. Symmetrically distributed data were described using means and standard deviations (M ± SD), while skewed data were described using medians and interquartile ranges [M (P25, P75)]. The Wald chi-square test was employed to explore differences in knowledge and acceptance levels across various participant characteristics.
To control for confounding factors, multifactorial regression analysis was employed to separately investigate the influencing factors of knowledge and acceptance. Multivariate analysis involved ordered logistic regression for knowledge levels (low, medium, high), validated using a test for parallel lines, and binary logistic regression for acceptance levels (positive, negative), adjusted by stepwise regression and assessed for fit with the Hosmer-Lemeshow test. Spearman’s correlation was utilized to examine the relationship between knowledge and acceptance. All statistical tests were two-sided, with a significance threshold set at P < 0.05.
Ethical Statement
This study received approval from the Medical Ethics Committee of Foshan University on January 6, 2023 (approval number: FUME2023017), situated at 33 Guangyun Road, Shishan Town, Nanhai District, Foshan City, Guangdong Province, China. It adhered to principles of informed consent, anonymity, and confidentiality. Participants reviewed the informed consent document detailing the study’s nature, potential risks, benefits, and the rights to refuse or withdraw at any time during survey participation. Survey participation commenced only after obtaining consent; otherwise, participation was terminated.
Results
Demographic Characteristics
Of the 523 university students who consented to participate in the survey, 410 provided valid questionnaires after excluding 93 for completing the survey in under two minutes and 20 for submitting evidently incorrect birthdates, achieving a validity rate of 78.40%. The average age of these university students are 20.68 ± 1.56 years. Furthermore, 96.10% of the participants were aware of the nonavalent HPV vaccine.
Knowledge of the Nonavalent HPV Vaccine and Influencing Factors
The knowledge scores regarding the nonavalent HPV vaccine were 10.0 (7.0, 12.0). Specifically, 74 participants (18.0%) exhibited low knowledge levels, 165 (40.2%) demonstrated medium levels, and 171 (41.7%) showed high knowledge levels (refer to Table 1). Concerning specific questions, 23.73% of college students did not believe that “both men and women can be vaccinated with the nonavalent HPV vaccine,” 25.42% thought that “the nonavalent HPV vaccine should be administered before the first sexual encounter,” and 40.92% were unsure whether “the nonavalent HPV vaccine can prevent colorectal cancer.”
Differences in Knowledge and Acceptance According to Demographic Characteristics (N = 410).

Note. 1 renminbi (RMB) = 0.138 United States dollar (USD).
*P < 0.05.
Ordered Logistic Regression Analysis of Knowledge About Nonavalent HPV Vaccine.

Abbreviations: SE: standard error; OR: odds ratio; CI: confidence interval.
*P < 0.05.
aReference group.
Acceptance of the Nonavalent HPV Vaccine and Influencing Factors
The acceptance score for the nonavalent HPV vaccine among university students was 32.0 (31.0, 38.0). Median scores for attitudes towards prevention and control were 16, for vaccine promotion were 12, and for vaccination were 4. Scores below the median of 32.0 indicated negative attitudes, whereas scores above indicated positive attitudes. Accordingly, 295 participants (71.95%) displayed positive attitudes, and 115 participants (28.05%) had negative attitudes.
Significant statistical differences in vaccine acceptance were found based on gender (χ2 = 40.799, P < 0.001) and monthly living expenses (χ2 = 10.969, P = 0.012), with no significant differences for other characteristics (see Table 1).
Binary Logistic Regression Analysis of Participants’ Acceptance of Nonavalent HPV Vaccine.
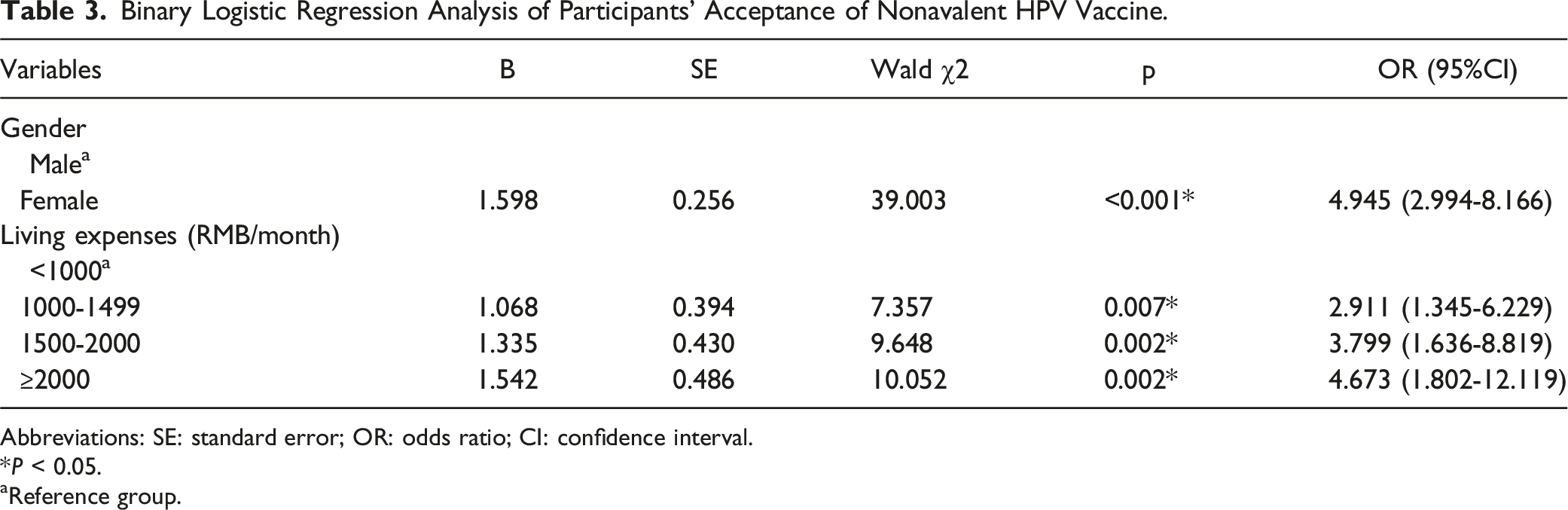
Abbreviations: SE: standard error; OR: odds ratio; CI: confidence interval.
*P < 0.05.
aReference group.
Correlation Between Participants’ Knowledge Level of the Nonavalent HPV Vaccine and Their Acceptance
Correlation Between Knowledge and Acceptance.

Discussion
In response to vaccine hesitancy among young adults in China and generally low vaccination rates, we conducted a cross-sectional study on three campuses of a southern Chinese university. This study assessed university students’ knowledge and acceptance of the nonavalent HPV vaccine and explored influential factors. Our findings offer actionable insights to enhance vaccination efforts within targeted age groups.
The study revealed that while 96.10% of participants were aware of the 9-valent HPV vaccine, and more than half held a positive attitude towards it, their overall knowledge remained limited, mirroring findings from previous research. 32 There were prevalent misconceptions among the participants about the vaccine, especially regarding the target groups for vaccination, appropriate conditions for receiving the vaccine (eg, whether one has engaged in sexual activity or has children), and the vaccine’s impact on HPV infection rates. Specifically, 23.73% of the participants incorrectly believed that not all men and women are eligible for the 9-valent HPV vaccine, 25.42% erroneously thought it should be administered before one’s first sexual encounter, and 40.92% were uncertain about the vaccine’s efficacy in preventing other types of cancer, such as colorectal cancer. These findings underscore the urgent need to enhance health education among college students to correct these misconceptions.
The study highlighted gender as a significant predictor of knowledge and acceptance of the nonavalent HPV vaccine. Male students demonstrated lower awareness compared to females, consistent with findings from previous research.33-35 This gender disparity may be attributed to perceived risk differences; diseases caused by HPV are often perceived as more prevalent among women, thus generating higher demand for vaccination among females. However, HPV does not exhibit gender-specific susceptibility but does show site-specific susceptibility.36,37 A Brazilian meta-analysis showed the highest HPV incidence rates at anatomic sites such as the penis, cervix, and anus, followed by the oral cavity. 37 Frequent gynecological exams in women, combined with heightened sensitivity to changes in reproductive organs, likely contribute to higher detection rates of HPV in women. This has fostered a misconception that women are more vulnerable to HPV, thereby marginalizing the relevance of vaccination for men. 34 Our findings also indicate that gender not only affects knowledge but also acceptance of the vaccine. Logistic regression showed that female students had a more favorable attitude towards the vaccine, mirroring a report from Italy. 38 These attitudes likely reflect the higher perceived threat of HPV among women, fostering greater trust in the vaccine’s benefits, particularly concerning its safety and effectiveness, and potentially strengthening their health beliefs and reducing hesitancy to vaccinate. 39 Future efforts to promote vaccination behavior in the target age group should focus on male students.
This survey evaluated the influence of economic factors on university students’ knowledge and acceptance of vaccines. Recognizing that students' monthly living expenses more accurately reflect their disposable income—and that such expenses often derive from sources beyond family support, including part-time employment—we used these expenses as an economic indicator. The findings revealed that higher living expenses correlate with increased vaccine knowledge and more favorable attitudes toward the nonavalent HPV vaccine. Despite the benefits, the vaccine’s exclusion from China’s national medical insurance and the high cost of a three-dose regimen—approximately 4000 RMB—render it unaffordable for many. 17 Students with limited financial resources often weigh the costs against the benefits, leading to reduced engagement and overall lower vaccine literacy. Such gaps in understanding can foster vaccine hesitancy. Additionally, economic conditions reflect broader family circumstances, with most students in mainland China not fully financially independent and reliant on parental support. Typically, higher parental education levels correlate with greater family income, 40 which can broaden the array of viable options. Consequently, students from more educated backgrounds are likely to have a heightened health awareness. This finding suggests that interventions addressing vaccine hesitancy should particularly consider students with limited economic resources.
Our study revealed a positive correlation between university students’ knowledge of the nonavalent HPV vaccine and their acceptance of it. Similar findings were reported in studies conducted in the United States, 41 Uganda, 42 and Canada, 43 as well as in a meta-analysis of vaccine acceptance among Ethiopian girls. 44 It is widely accepted that sufficient and clear understanding can enhance behavioral willingness and acceptance. Previous research has indicated that school-based health education generally enhances vaccination confidence and increases vaccination coverage rates.45-48 Consequently, implementing educational and promotional activities in schools is likely to be effective. Universities can enhance students’ understanding of HPV and its vaccines through various methods, such as peer education, health lectures featuring real case studies, distribution of health manuals within student communities, collaboration with campus health services to offer online and offline health consultations, dissemination of information about HPV and the nonavalent HPV vaccine through official university channels, and the introduction of regular HPV screening programs. These knowledge-enhancement strategies could significantly reduce vaccine hesitancy and promote vaccination behaviors among the appropriate age group.
This study has several limitations. Firstly, its cross-sectional design prevents it from establishing causal relationships between knowledge, acceptance, and other variables. Secondly, the use of convenience and snowball sampling methods, and the absence of a sampling framework tailored to the population size of the three campuses, may diminish the sample’s representativeness. Thirdly, external factors such as social media exposure and parental attitudes towards vaccination, which may influence university students’ knowledge and acceptance of the nonavalent HPV vaccine, were not considered in this study. Lastly, it was not possible to control for participants' behavior during the survey, such as online searching for answers, and there may be a bias towards socially desirable responses among medical students, despite instructions to provide honest answers.
Despite its limitations, this study offers valuable insights into college students’ knowledge and acceptance of the nonavalent HPV vaccine, as well as the diverse factors influencing these aspects. The research targeted a varied group of students across different majors, academic years, and family backgrounds, suggesting that the findings may be applicable to comprehensive universities at large. Focusing on pertinent factors through school health interventions, particularly for economically disadvantaged males, is likely to enhance vaccination rates among young people.
Conclusion
In summary, this study examined the knowledge and acceptance of the nonavalent HPV vaccine among university students at a comprehensive university in southern China, focusing on associated factors. Results revealed that while a large percentage of participants were aware of HPV, their comprehensive knowledge about the vaccine was lacking. Both gender and economic status were significantly associated with the students’ knowledge and acceptance of the vaccine, with a positive correlation noted between knowledge and acceptance. These findings underscore the necessity for further research and the development of targeted educational interventions for specific demographics, such as male and economically disadvantaged students, to enhance vaccination rates within these key groups.
Footnotes
Acknowledgments
We extend our sincere gratitude to the participants who consented to partake in this research survey.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors gratefully acknowledge financial support from the Undergraduate Training Program for Innovation and Entrepreneurship at Foshan University (No. 2022-18-133) and the 2023 Teaching Reform Project of Guangdong Provincial “New Medical Science” (No. 2023-0724-204).
Ethical Statement
Data Availability Statement
The original research data can be accessed by contacting the corresponding author.
