Abstract
Objective
Identify predictors of overall survival (OS) after hypopharyngeal/laryngeal cancer in Florida.
Material and Methods
We conducted a retrospective cohort study using data from the Florida Cancer Data System (FCDS) on patients diagnosed with hypopharyngeal or laryngeal cancer from 2010-2017. Primary outcome was OS. Hazard ratios (HRs) were estimated from univariable and multivariable Cox regression models for OS. Data was analyzed from November 1, 2022, to June 30, 2023.
Results
We analyzed 6771 patients, who were primarily male (81.2%), White non-Hispanic (WNH) (78.2%), publicly insured (70.1%), married (51.8%), and residents of urban counties (73.6%). Black patients were more likely to be younger at diagnosis (38.9%), single (43.4%), to have distant SEER stage disease (25.6%). Median OS were lowest among patients who were uninsured (34 months), with hypopharyngeal site disease (18 months), and a smoking history (current: 34 months, former: 46 months, no smoking: 63 months). Multivariable Cox regression analysis showed worse OS for single/unmarried vs married (HR 1.47 [95%CI: 1.36-1.59], P < .001), history of tobacco use (current: HR 1.62 [95%CI: 1.440-1.817], P < .001; former smokers: (HR 1.28 [95%CI: 1.139-1.437], P < .001) vs no history). Improved OS was observed among White Hispanics (WH) vs WNH (HR .73 [95%CI: .655-.817], P < .001) and women vs men (HR .88 [95%CI: .807-.954], P = .002). Geographical mapping showed that mortality rates were highest in census tracts with low income and education.
Conclusion
Our findings suggest that sociodemographic and clinical factors impact OS from hypopharyngeal/laryngeal cancer in Florida and vary geographically within the state. These results will help guide future public health interventions.
Introduction
Laryngeal carcinoma accounted for approximately 12 380 new cases and 3820 deaths in the United States in 2023. 1 Hypopharyngeal malignancies are less common, with approximately 2500 new cases annually. 2
Although laryngeal and hypopharyngeal cancer are distinct diseases, they are often grouped together in medical literature due to close proximity, shared risk factors, and similar treatment approaches. 3 Squamous cell carcinomas (SCC) account for about 95% of laryngeal and hypopharyngeal malignancies. 2 These cancers are most common in men between the fifth or sixth decades of life. 4 Currently, these malignancies are primarily managed with a combination of surgery, radiation, and chemotherapy. Hypopharyngeal malignancies are associated with higher morbidity and mortality due to a lack of early specific symptoms. 5
Disparities in survival rates based on race/ethnicity and sociodemographic factors are well-documented in literature for patients with laryngeal cancer. 6 Disparities among patients with hypopharyngeal SCC is less well documented. A Surveillance, Epidemiology, and End Results (SEER) database study by Divakar et al 7 noted that laryngeal cancer mortality rate did not improve in a similar manner to the incidence rate, citing potential factors such as advanced disease at presentation, differences in health care access, treatment delays, and changes in referral patterns.
Patterns of mortality from cancer are geographically diverse. Mokdad et al 8 found that the age−standardized county-level head and neck cancer (HNC) mortality rates in the southern United States (US) were higher than other regions in the US from 1980 to 2014. Another study highlighted divergent trends within the southern US, showing that from 1990-2017, laryngeal cancer mortality in Florida declined by 9.5%, whereas in Mississippi, it increased by 12.8%. 9
To reduce deaths related to laryngeal and hypopharyngeal cancer, we must examine disparities in the distribution of risk factors at a more localized level, such as the state level. The present study utilized the Florida Cancer Data System (FCDS) to investigate sociodemographic and geographical characteristics, as well as overall survival (OS), among patients diagnosed with laryngeal or hypopharyngeal SCC in Florida. This study enables the identification of specific areas where targeted public health initiatives can be established or strengthened.
Patient & Methods
This project was conducted in compliance with ethical principles, and was exempt from review, approval, or oversight by the University of Miami Miller School of Medicine Institutional Review Board (IRB). This retrospective cohort study followed the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) reporting guideline. 10
Patient Selection
We established specific criteria for the selection of cases in our study based on data obtained from the FCDS, a de-identified comprehensive cancer registry encompassing all cancer diagnoses in Florida dating back to 1981.
11
Our inclusion criteria encompassed cases related to hypopharyngeal cancer (ICD codes C13.0–C13.9) and laryngeal cancer (ICD codes C32.0-C32.9). Additionally, we included cases with histological features consistent with squamous cell carcinoma (SCC) (ICD-O-3 codes 8050-8052, 8070-76, 8078, 8082-84) (Figure 1).
12
Flowchart of exclusion and inclusion criteria.
Predictor Variables
Variables collected by FCDS and included in our analysis were the following: age, sex, race, ethnicity, marital status, insurance status, cigarette tobacco smoking status, SEER 2010 stage of disease, zip code, census code, date of diagnosis, date of last contact, and mortality status at date of last contact.
Age at diagnosis was dichotomized into two groups: <60 years and ≥60 years. Self-identified race groups included Whites and Blacks. Other groups, including Native American, Asians and those of other Asian descent were excluded due to their small representation (1%–2%). Other factors included self-identified ethnicity (Hispanic or non-Hispanic), marital status at time of diagnosis (never married (single, unmarried, or domestic partner), previously married (separated, divorced, widowed), married (including common law)), SEER 2010 disease stage (in-situ, local, regional, distant, unstaged). Insurance status (uninsured, private insurance, public insurance (Medicaid, Medicare, TRICARE, Military, Veterans Affair, Indian/Public Health Service)) Tobacco cigarette smoking status was categorized as “never used”, “current user”, “former user”, or “unknown”. Florida counties were considered urban or rural based on the 2010 Census Bureau’s urban-rurality classification.
FCDS does not collect information on education and income, as such, we linked each patient’s census code to the American Community Survey (ACS) census bureau data to infer information about the patient’s education level (% with at least a bachelor’s degree) and income (median income in the last 12 months). For this study, we grouped these variables into quartiles. 13
Additionally, we explored whether the lack of Medicaid expansion in Florida under the Affordable Care Act (ACA) in 2014 impacted OS. Therefore, we categorized patients diagnosed pre- (2010-2013) and post-ACA (2014-2017).14,15
Statistical Analysis
All statistical analyses were performed with IBM SPSS Statistics, Version 28.0 (Armonk, NY). Associations between categorical variables were examined using chi-square tests. The primary outcome was overall survival (OS) defined as the time from date of diagnosis to date of death or last contact date. Survival curves and median survival were estimated by the Kaplan-Meier method. Log-rank test was used to determine if there was a statistically significant difference between OS curves. Univariable and multivariable cox proportional hazards regression models were used to assess predictors of OS, with results reported as unadjusted and adjusted hazard ratios (HRs) with 95% confidence intervals (95% CI). Kaplan-Meier survival plots were customized using the SAS V.9.4 (SAS Institute) NewSurv macro. 16 ArcGIS maps were designed using ArcGIS Pro 3.0 software. A P value of <.05 was considered statistically significant. Data was analyzed from November 1, 2022, to June 30, 2023.
Results
Patient and Clinical Characteristics
Demographics and Other Characteristics of (N = 6771) Hypopharyngeal/Laryngeal Cancer patients Diagnosed From 2010-2017. Tests Were Adjusted for all Pairwise Comparisons Using the Bonferroni Correction.

aTests were adjusted for all pairwise comparisons using the Bonferroni correction.
Demographics and Other Characteristics of (N = 6771) Hypopharyngeal/Laryngeal Cancer patients Based on pre-vs Post-ACA Medicaid Expansion Period. Tests Were Adjusted for all Pairwise Comparisons Using the Bonferroni Correction.

Compared to WNH and White Hispanics (WH), Black patients were more likely to be older, single/unmarried (43.4%) and come from census tracts within Florida with lower median household incomes (50.7%) and education (48.3%) and were more likely to have distant SEER stage disease (25.6%). Black (8.2%) and WH (8.5%) patients were more likely than WNH (5.6%) to be uninsured. Black (16.7%) and WNH patients (13.6%) were more likely than WH (7.4%) to be diagnosed with hypopharyngeal SCC. There was no significant difference in treatment rates based on race/ethnicity (P = .409).
Fewer patients were uninsured (5.4% vs 7%, P = .006) and diagnosed with distant SEER stage disease post-vs pre-ACA Medicaid expansion (19.8% vs 16.9%, P < .001). Additionally, patients were more likely to have received treatment post-vs pre-expansion (89.5% vs 87.4, P = .008) (Table 2).
Median Survival Times
There were 3787 (55.9%) deaths at last contact. Overall median survival time (MST) was 42 months. Figure 2 displays the Kaplan Meier survival curves and MST for each factor. Black patients had the lowest MST, followed by WNH and WH (33 vs 41 vs 66 months, P < .001). Married patients had a higher MST than single/unmarried and previously married patients (55 vs 31 vs 33 months, P < .001). Privately insured patients had a higher MST than publicly insured and uninsured patients (65 vs 37 vs 34 months, P < .001). Patients with no tobacco smoking history had a significantly longer MST than current smokers and former smokers (63 vs 34 vs 46 months, P < .001). Patients from census tracts with the highest income (>$56,957) (54 months) and highest education (>32.6% with at least a bachelor’s degree) (57 months) had the longest MST (P < .001). Kaplan Meier curves of overall survival (OS) by A) age B) race/ethnicity C) sex D) marital status E) insurance status F) smoking status G) median income H) education I) geographical location J) pre-vs. post ACA Medicaid period K) cancer site L) SEER disease stage, and N) treatment status.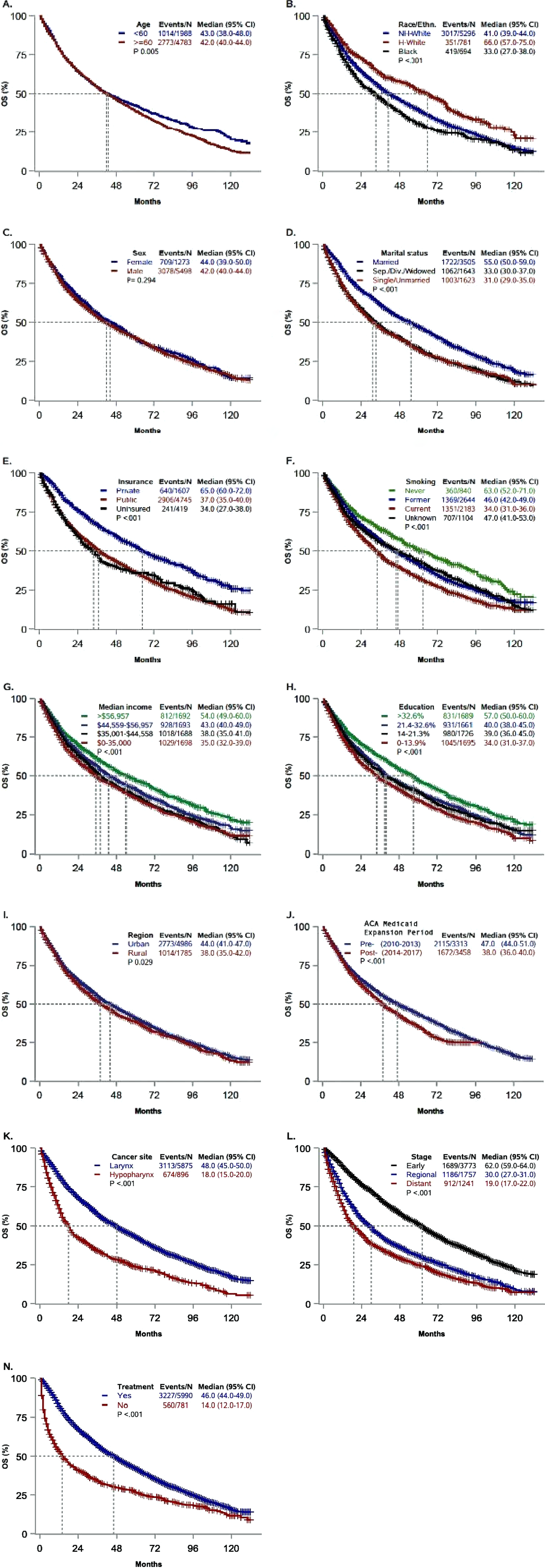
Cox Regression Analysis
Univariable and multivariable Cox Regression Models Assessing Predictors of overall survival (OS) (N = 6771: 3787 died, 2984 Alive).
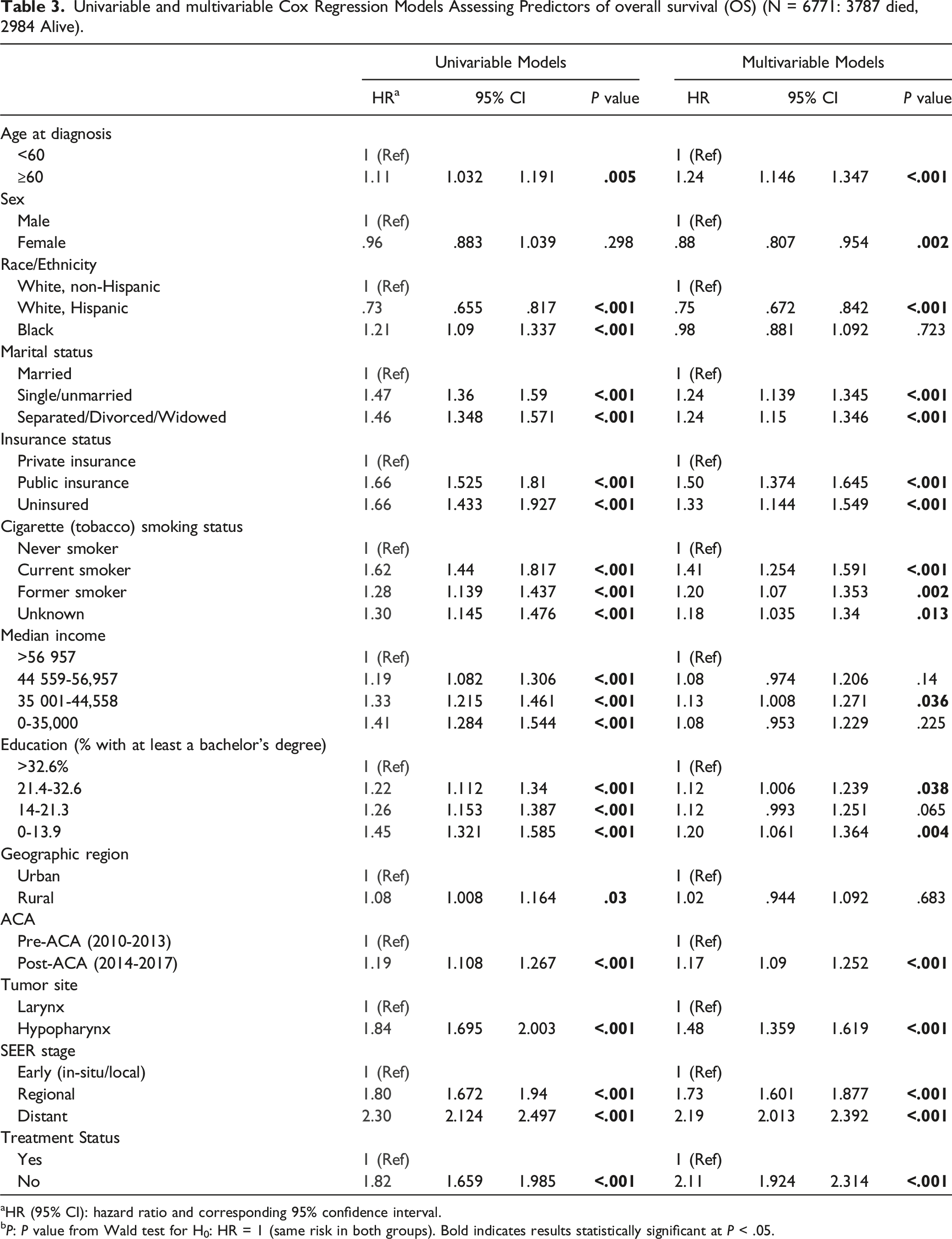
HR (95% CI): hazard ratio and corresponding 95% confidence interval.
bP: P value from Wald test for H0: HR = 1 (same risk in both groups). Bold indicates results statistically significant at P < .05.
In multivariable analysis, while controlling for all the covariates in Tables 1 and 2, worse OS was maintained among older patients (≥60 y), single/married or previously married, publicly insured, uninsured, history of tobacco smoking, diagnosis post-Medicaid expansion, hypopharyngeal SCC, regional or distant disease, and untreated; improved OS was maintained for WH vs WNH. Female patients (aHR .88 [95%CI: .807-.954], P = .002) had higher OS than males. Statistically significant results for Black race/ethnicity (P = .723) and rural county location (P = .683) were not upheld in the multivariable model.
Geospatial Mapping Analysis
At the census tract level, we observed mortality rates for hypopharyngeal and laryngeal SCC were highest in Northern Florida. Additionally, we observed the highest mortality rates in areas of Florida characterized by lower income and education levels (Figure 3). Median household income and education by census tract in the state of Florida, 2010-2017. The state is colored by median income and education, respectively. Circle size is proportional to the amount of mortality for each census tract.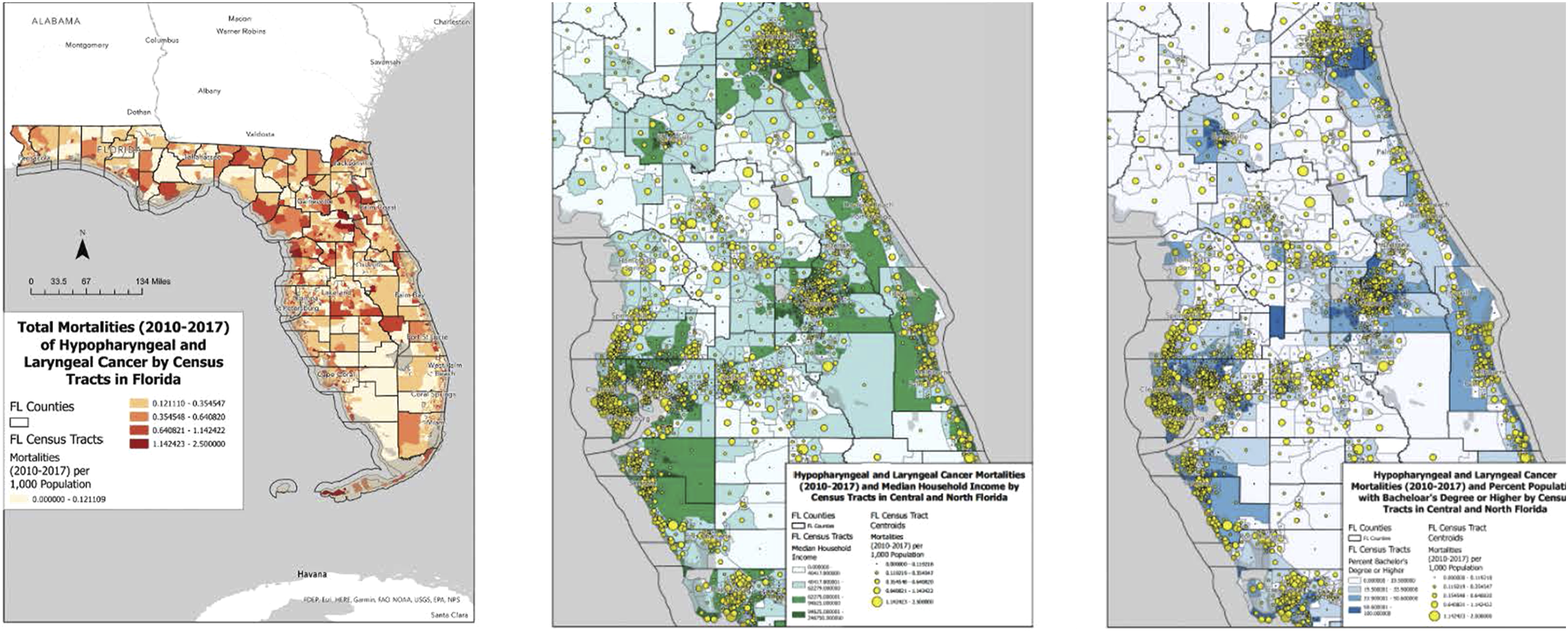
Discussion
Our analysis revealed that age, sex, race/ethnicity, marital status, tobacco smoking status, insurance type, education, income, geographical location, stage of disease, and treatment status were associated with OS from hypopharyngeal/laryngeal SCC in Florida. While previous studies explored the impact of these factors related to laryngeal cancer outcomes such as treatment approaches, disease stage at presentation, and survival status, 6 there is limited literature discussing such disparities at a more localized level.17–19
Blacks had lower MST and OS than WH and WNH in univariable analysis. However, multivariate analysis showed similar OS rates for Black and WNH patients, contradicting many studies showing racial disparities in laryngeal cancer OS,13,20–25 and aligning with few that have found no significant difference.26,27 There are several reasons to have suspected that Blacks would have had lower OS than Whites. Black patients often have larger tumors, more advanced disease at presentation, and differences in treatment rates.13,20,28,29 Additionally, non-white patients are more likely to experience treatment delays.30,31 In our study, Black and WNH patients had similar treatment rates. However, Black patients were more likely to be single, younger, less educated, poorer, and be uninsured at presentation. These factors likely worsened OS; however, it is unknown whether other unstudied factors might explain the lack of racial disparities in OS between Blacks and WNH.
The "Hispanic paradox" has been observed in other HNC cancers, where WH have better survival than WNH. 32 In our study, WH made up 11.5% of the cohort and had improved OS compared to WNH in univariable and multivariable Cox regression models. We hypothesize that the survival benefit in our cohort is linked to smoking habits and early-stage diagnosis in WH patients. WH patients in our study were less likely to be current smokers and more likely to be diagnosed with early (in-situ/local) SEER stage disease at presentation. Further research is needed to identify the drivers of this benefit, especially among Hispanic subgroups. It would be worth investigating if this relationship holds in heavily WH areas, like Miami-Dade County, Florida.
Our study also revealed significant differences in OS based on gender. Multivariable cox regression analysis showed that females with hypopharyngeal/laryngeal SCC had higher OS compared to males, similar to previous studies.13,19,21–23,33 However, one study observed lower OS in females with laryngeal cancer, 31 suggesting some slight variation in the gender disparity. Lower OS among males is typically attributed to their higher tobacco and alcohol consumption, both behaviors that confer a higher risk of developing HNC, 34 especially when used together. 35
We found that uninsured or publicly insured patients had worse OS than those with private insurance, which aligns with previous studies.21,29,36 Chen and Halpern et al 21 conducted a retrospective review of 7019 advanced laryngeal SCC patients, and showed that uninsured and Medicaid patients had lower OS compared to privately insured patients. Mehta et al 29 found that at every stage of laryngeal cancer, uninsured patients had lower OS than those privately insured, and Medicare patients had higher OS than those who were uninsured. Insurance status is important to examine in the context of cancer disparities as public insurance/no insurance status may limit patients’ access to adequate medical care and delayed care due to costs. 31 For instance, a previous study found that HNSCC patients with Medicare/Medicaid insurance were less likely to receive adjuvant therapy. 37
Florida is a good example to study cancer disparities considering it is among the few states that declined Medicaid expansion. Several previous studies have analyzed the impact of Medicaid expansion on HNC patients.14,15,38,39 Cannon et al 15 found fewer HNSCC patients were uninsured post-Medicaid expansion than pre-expansion. However, they found this difference to be negligible in Medicaid non-expansion states. Patel et al 14 found that Medicaid expansion states had lower proportions of uninsured HNC patients with advanced stage (T4 and N2c) than non-expansion states, but this difference was insignificant when assessing overall stage (I-IV). We observed a slight decrease in distant SEER stage hypopharyngeal/laryngeal cancer post-expansion. Interestingly, a diagnosis of hypopharyngeal/laryngeal SCC post-Medicaid expansion was linked to poorer OS. The cause of this is unknown and needs further study. Future studies should compare states based on Medicaid expansion to better understand the effect of health care policies on hypopharyngeal/laryngeal SCC survival.
Our study showed that married individuals at diagnosis had higher overall survival than single/unmarried or previously married people, which is consistent with other studies.13,40–43 A previous study found that unmarried persons with oral and laryngeal cancer were more likely to have metastatic disease. 43 Unmarried people may have worse outcomes due to lack of emotional and financial support, and the relationship between stress, depression, and tumor growth, response, and regression through inflammatory markers and stress hormones.44,45 Marital status may also affect treatment selection, with one study showing that married patients with laryngeal cancer were more likely to receive definitive treatment. 43
We investigated the impact of rural-urban geography on mortality rates for laryngeal and hypopharyngeal cancer and found OS to be lower among rural county dwellers in the univariable cox regression model, but not maintained after adjusting for co-variables. Zuniga and Lango et al 46 and Kim et al 47 did not observe significant differences in laryngeal cancer 5-year survival rates based on geography. In contrast, Misono et al 24 observed lower OS among patients treated at rural hospitals for incident T1 glottic SCC. Ravikumar et al 17 found lower OS among patients in small rural towns in New York compared to urban areas. The higher mortality rates in rural communities might be attributed to limited financial resources and access to health care facilities. Future studies would benefit from exploring the impact of distance to care on OS.
This retrospective study has certain limitations. As with other database studies, the accuracy and consistency of the collected patient data may be subject to inaccuracies and inconsistencies. Information, such as tobacco behavior, relies on self-reporting and may be susceptible to bias. The FCDS database does not collect data on the quantity of tobacco smoked or alcohol consumed, both are relevant factors considering the dose-response relationship between alcohol/tobacco use and cancer risk. Additionally, median income and education are derived from census data from the U.S Census Bureau, which may not be as accurate as collecting direct data from patients. An additional limitation in our analysis is the choice of staging system. Our study defined early disease (in-situ and local) using the SEER staging system, which is the default system in the FCDS database. With over 50% of patients in our cohort exhibiting "early stage" disease, SEER stage may not offer as much detailed information about the extent of the cancer as offered by the T classification in the TNM system, which may limit the precision of our study. Despite these limitations, we have confidence in the reliability of this study’s findings as it presents a comprehensive representation of the Florida population.
Conclusion
Our study identified sex, race/ethnicity, geographical location, marital status, insurance status, education, income, pre-vs post-ACA Medicaid expansion, disease stage, tobacco smoking status and treatment status as predictors of lower OS from hypopharyngeal/laryngeal SCC. Our geographical mapping analysis emphasized the impact of education and income on OS from this disease in Florida.
In essence, our research offers crucial insights for a range of stakeholders, such as policymakers, community organizations, health care professionals, and researchers, specifically in Florida. Our mapping analysis is instrumental in pinpointing areas within the state where it is crucial to prioritize head and neck screening initiatives and allocate resources for prevention programs. Furthermore, our data supports the initiation of health education campaigns addressing alcohol and tobacco abuse, as well as the prevention and early detection of head and neck cancers in Florida’s hotspots where the morality rates from head and neck cancer are disproportionately high. Additionally, this information may act as a catalyst for the development of new policy initiatives aimed at reducing mortality from hypopharyngeal/laryngeal cancer post-diagnosis. This may include measures such as Medicaid expansion, the provision of psychosocial support services for cancer patients, and increased funding for access to cancer care in underserved regions within Florida.
Our future research will aim to analyze risk factors at the neighborhood level in specific areas of Florida, such as Miami-Dade County, with the goal of providing more targeted guidance for public health interventions.
Footnotes
Author Contributions
UE and EF devised the project, the main conceptual ideas, and research question. UE, IR analyzed the data. UE wrote the paper with input from all authors. AA, IB, ML, GF, SP, AD, LS, DW, EK, IR, EF provided input and edits on the final draft of the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
