Abstract
Objectives
The aims of this pilot study were (1) to develop a cancer prevention module consisting of an animated video and a short questionnaire, (2) to assess new knowledge gained by the participants, and (3) to solicit feedback for improving the cancer prevention module.
Methods
Volunteers who previously agreed to be contacted regarding research studies were approached via email. After completing the cancer prevention module, a list of cancer prevention recommendations was provided. Newly gained knowledge was assessed, and feedback was solicited.
Results
Overall, 290 of 3165 individuals contacted completed the online module (9.2%), and 38.6% of the participants indicated that they learned something new about cancer prevention measures. A similar proportion, 41.4%, mentioned that they learned about measures that were recommended and due. Paradoxically, response rate was the lowest in the ≥50 year old age group although this group reported the highest rate of learning about new cancer prevention measures. Feedback was favorable in that 70.7% mentioned that the recommendations were helpful to them personally, 69.3% felt motivated to take action to reduce their risk of cancers, and 67% would recommend the online module to their friends and family.
Conclusion
We developed an online cancer prevention module which seems to be suitable for promoting cancer prevention measures as feedback was favorable, and new knowledge was gained. Future efforts will focus on using the module to promote cancer prevention measures to the general public particularly for the ≥50 year age group.
Introduction
Cancer is the second leading cause of death in the United States (US) and imposes a significant burden on our health care system. 1 Approximately 1.8 million new cancer cases are expected to be diagnosed in 2020 in the US, and at least 42% of those cases could be prevented. 2 Breast, cervical, colorectal, and lung cancer screening measures are tools for early detection and for reducing mortality. 2 However, these tools are often underutilized for various reasons. Low socioeconomic status, lack of health insurance, and limited health literacy are known factors preventing people from obtaining cancer prevention measures.3-5 However, increasing awareness through education about the importance of cancer screening can improve adherence.6-9 Cancer screening can be cost-effective in comparison to cancer treatment, and full implementation of screening programs throughout the entire population remains an important goal for the health care system. 10
Cancer incidence and mortality are higher in Arkansas than the national averages for cancer of the cervix (9.8 vs 7.6 per 100,000 for incidence and 3.4 per 100,000 vs 2.3 for mortality), colorectum (43.8 vs 38.7 for incidence and 16.8 vs 14.2 for mortality), and lung (78.1 vs 59.2 for incidence and 57.5 vs 41.9 for mortality). 11 For female breast cancer, the incidence rate in Arkansas, 117.5, is lower than that of the US, 125.2 per 100,000 per population. However, the mortality rate is higher in Arkansas (21.6 vs 20.6 per 100,000 per year). Lower rates of cancer screening (72.9% vs 80% for Pap smear in the past 3 years, 73% vs 77.6% for mammogram in the past 2 years, and 65.4% vs 67.7% for colorectal cancer [CRC] screening) and human papillomavirus (HPV) vaccination (38.3% vs 53.2% for 2+ doses in ages 13–17), and higher rates of current adult smoking (22.3% vs 17.1%) are at least partially responsible for these disparities. 11 Therefore, our long-term goal is to increase cancer screening and HPV vaccination and to decrease smoking among people in our state in order to decrease cancer incidence and mortality.
Technology has the potential of revolutionizing health care delivery. Some successes have been reported with use of internet interventions for promoting health-related education12,13 and treatment. 14 For example, Miller et al. 13 demonstrated increase in CRC screening using an iPad app which allowed patients to order their own screening tests, and to forward automated electronic messages for follow-up reminders and support. In the current study, we developed an online module for promoting cancer prevention measures including cancer screening, HPV vaccination, smoking cessation, and weight loss. This module consisted of one-minute animated video, and a brief questionnaire written at a 5th to 8th grade reading level. The video was designed to demystify cancer and to reduce its stigma by describing its etiologies and what steps can be taken to prevent it. This module was tested in volunteers who were mostly Arkansans and who had previously agreed to be contacted for research studies. The suitability of this module for promoting cancer prevention measures was assessed; feedback was solicited to improve the module, and whether the module was successful in increasing knowledge that was assessed.
Methods
Participants and Recruitment
Eligible participants were volunteers aged 18 years or older who had registered for ARResearch, a registry developed by the UAMS Translational Research Institute which consists of community members mainly from Arkansas willing to participate in research studies of their interest. 15 Participation in this Institutional Review Board (IRB) approved study was solicited via an email written at the 5th to 8th grade reading level (plainpages.org, UAMS, Little Rock, AR, USA). It included the purpose of the research study, eligibility criteria, contact information of the investigators, and a link to the one-minute animation video (Explainify, Fayetteville, AR, USA) and questionnaires. Clicking on the link served as an informed consent process and confirmation of eligibility criteria. This study was registered at clinicaltrials.gov (NCT03810053). Solicitation emails were sent between March 1, 2019 and July 24, 2019 to an equal number of volunteers based on age (18–29, 30–39, 50–49, and ≥50 years) and sex until we ran out of male volunteers in the age 18–29 group. Then, repeat solicitations were sent to this subgroup. Participants completing the online module and feedback questions were compensated with $40 in the form of gift cards.
Online Module
The online module consisted of a one-minute animated video (Supplement 1) followed by a brief questionnaire (Supplement 2A). The video explained common causes, consequences, and the availability of various prevention and early detection methods. The questionnaire solicited age, sex, race, ethnicity, and basic medical history needed to provide appropriate recommendations for mammography, Pap smear, CRC screening, lung cancer screening, HPV vaccination, smoking cessation, and weight loss (see Supplement 3A for a hypothetical example). A list of recommendations was provided based on guidelines (Supplement 2B) from the US Preventive Services Task Force (USPSTF),16-19 American Cancer Society (ACS), 20 American College of Radiology, 21 American College of Obstetricians and Gynecologists, 22 and Advisory Committee on Immunization Practices. 23
After completing the questions in the cancer prevention module and receiving a list of personalized recommendations, the participants were assessed for newly gained knowledge. Whether one had acquired knowledge about cancer prevention measure(s) one did not know about was asked using the question “Did this list help you learn about any actions you did not know about?” If the answer was yes, they were asked which measure(s). They were also asked whether they learned about measure(s) which were due using the question “Did this list help you learn about any actions you have not taken yet?” Participants who were due for breast cancer screening, cervical cancer screening, CRC screening, LDCT lung cancer screening, and/or HPV vaccination were asked whether they were willing to be contacted in 6 months for follow-up. Race and ethnicity were captured, and participant health literacy level was assessed with a single screening question which asked “How confident are you filling out medical forms by yourself?” 24
Feedback Questions
The feedback questionnaire for the online module (Supplement 2C) used a 5-point Likert scale. 25 Input regarding the most desired compensation, social media platforms most commonly used, education level, and whether they were affiliated with the health care field was also solicited. The directed content analysis method 26 was utilized to summarize additional free text suggestions.
6-Month Follow-Up
Participants who identified at least one of five cancer prevention measures (breast cancer screening, cervical cancer screening, CRC screening, LDCT lung cancer screening, and HPV vaccination) which was recommended to them based on their sex, age, and family history but had not been fulfilled at the time of participation in the online module and who agreed to the follow-up (Supplement 2D) were re-contacted by email after 6 months. The uptake of the particular cancer prevention measure(s) was assessed. Participants received an additional $40 in the form of gift cards.
Statistical Analyses
Percent responses among different age groups for all, men, and women were compiled (Figure 1A), and bivariate associations were tested for statistical significance using either chi-square test or Fisher’s exact test. Furthermore, percentages of participants gaining knowledge about cancer prevention measures (Figures 1B and 1D, and Supplement 4) and percentages of participants learning about any of them being due were analyzed in the same manner (Figures 1C and 1E, Supplement 4). Then, associations between health literacy level and gaining new knowledge about each cancer prevention measure were determined using Fisher’s exact test of independence (Supplement 5). Analogous associations were assessed between health literacy level and learning that certain recommended measures are due. Similarly, associations for being affiliated with the health care field and for level of education were assessed using chi-square or Fisher’s exact test (Supplement 5). A two-sided P-value of <0.05 was considered to be statistically significant. Percent response, percent gained knowledge, and percent learned of due measures among different age groups and sex or by cancer prevention measures. (A) Response rates were significantly different among different age groups in all invited (P=0.003) and in men (P<0.001) but not in women (P=0.244). (B) Increasing age correlated significantly with more gained knowledge about cancer prevention measures in all sexes (P<0.001), men (P=0.045), and women (P=0.020). Overall learning rate was 38.6% (112 of 290). (C) Learning about due cancer prevention measures also significantly correlated by age groups for all (P=0.001) and women(P=0.005) but not for men (P=0.248). The overall rate was 41.4% (120 of 290). (D) Percent gained knowledge of specific cancer prevention measures. (E) Percent learned of specific cancer prevention measures due.
Results
Email solicitations were sent to 3165 individual ARResearch volunteers, and 290 (9.2%) responded. The respondents were comprised of 87 men (30%), 200 women (69%), and 3 responding “neither” (1%). The response rate was higher for men (10.4%) than women (8.6%) but not significantly. The response rates were significantly different among different age groups for all participants (P=0.003) and for men (P<0.001) (Figure 1A). The response rates were the lowest in the ≥50 years group for all (6.5%), men (5.0%), and women (7.4%). The most common race among our respondents was Caucasian (82.4%), and Hispanics comprised 4.8% of all participants.
An example of responses from a hypothetical participant (Supplement 3A) and the summary of actual responses (Supplement 3B) are shown. A majority (66.9%) had never smoked tobacco and most were overweight or obese (67.9%). A large proportion of our participants had no history of breast cancer (86.5% of female participants) or CRC in their immediate family (82.1% of all). HPV vaccination was recommended for 13.2% of participants, mammography for 45.5%, Pap smear for 92.5%, CRC screening for 22.7%, and LDCT screening for 1.7%.
While 38.6% (112 of 290) participants gained knowledge about new cancer prevention measures, 41.4% (120 of 290) indicated that they found out about recommended cancer prevention measures that were due. The percentages of respondents who gained knowledge about cancer prevention measures was significantly different across age groups (P<0.001) with 33.3% in the 18–29 year old group, 28.6% in the 30–39 year old group, 35.5% in the 40–49 year old group, and 59.7% in the ≥50 years group (Figure 1B). Therefore, while survey response rate was the lowest in the ≥50 years group (6.5%, Figure 1A), the proportion gaining knowledge about cancer prevention measures was the highest in this age group (59.7%, Figure 1B).
The proportion of respondents who learned about recommended cancer prevention measures that were due differed significantly (P=0.001) among age groups as well (Figure 1C). The highest proportion was in ≥50 years of age (55.2%), followed by 50% in the 40–49 year old group, 36.5% in the 18–29 year old group, and 26.2% in the 30–39 year old group.
Percentages of respondents who gained knowledge about new cancer prevention measures are shown by each measure in Figure 1D. The three most frequently learned cancer prevention measures were LDCT (27%), HPV vaccination (23%), and weight loss (19.7%). Furthermore, there was a significant difference among the different age groups who gained knowledge about LDCT (Supplement 4A, P<0.001).
The proportions of respondents that learned about recommended measures that are due are grouped by each measure in Figure 1E. LDCT (23.8%) was the measure with the highest percentage among all age groups. Significant difference among the different age groups was also found for learning being due for LDCT (Supplement 4B, P<0.001) and mammography (Supplement 4C, P=0.006).
A majority of the participants answered either extremely confident (72.1%) or fairly confident (23.1%) to a question “How confident are you filling out the medical forms by yourself?” to assess health literacy (Figure 2A). The feedback to the online module (Figure 3) was very favorable. A majority stated that they liked the animated video (90.1%) and found the video entertaining (83.5%). About 50% responded that they learned something new from the video, 69.3% felt motivated to take action to reduce their risk of cancer, and 61.7% felt encouraged to disseminate information about cancer screening measures. Furthermore, 94.5% responded that the questions were easy to answer, 70.7% responded that the recommendations were helpful to them personally, and 67% responded that they would recommend promoting the online module through social media. Summary of responses assessing healthy literacy, social media use, affiliation with health care field, and education level (n=290). (A) Health literacy was assessed by asking “How confident are you in filling out medical forms by yourself?” and the majority (72.1%) responded extremely. (B) Social media platforms one used included Facebook (85.2%), Instagram (30.3%), Twitter (15.9%), and Snapchat (8.6%). (C) When asked whether one was working and/or studying in the health care field, approximately half (48.3%) responded “yes.” (D) The most commonly attained highest level of education was “more than college (37.9%)” followed by “finished college (34.8%).” Summary of feedback responses which were favorable overall (n=290). (A) Liked the animation video. (B) Found the video entertaining. (C) Learned something new from the video. (D) Felt encouraged to take actions toward reducing their changes of cancer after watching the video. (E) Felt encouraged to tell others about cancer prevention and early detection after watching the video. (F) Questions were easy to answer. (G) Found the list of recommendations to prevent cancer helpful for then personally. (H) Would recommend the cancer prevention module to their friends and family through social media.

Sixty-four respondents provided free text suggestions for improving the cancer prevention module. These responses were grouped in 4 broad categories: (1) providing more details about cancers and prevention measures (29.1%), (2) questions for assessing the risk of cancers to be more detailed (17.7%), (3) resolve technical difficulties (11.3%), and (4) others (41.9%). Comments displaying appreciation for the conciseness of the video and questionnaire and the efficiency of the short questionnaire to assess cancer risk were grouped in the “Other” category (data not shown).
Responses to questions regarding social media platforms used, educational attainment, and affiliation with the health care field are shown in Figures 2B–2D. Facebook was the most commonly used platform among our participants (85.2%) followed by Instagram (30.3%) and Twitter (15.9%). About 72.8% respondents had a college degree or higher and 48.3% were affiliated with the health care field. Our participants indicated that the most desired compensation for participating in the online module for the future intervention was “a chance to win a $500 gift card” (78.6%), and that the most desired compensation for participating in the 6-month follow-up survey was “$10 gift cards for each participant” (46.5%) (data not shown).
No significant associations between health literacy level and gaining knowledge about new cancer prevention measures were found except for HPV vaccination (Supplement 5A). Those with lower health literacy (35.7%) were more likely to gain knowledge about HPV vaccination compared to those with higher health literacy (13%, P=0.034). Those not affiliated with the health care field were more likely to learn about the benefit of weight loss with respect to cancer risk (17.3% vs 6.4%, P<0.01), and more likely to be due for HPV vaccination (18.7% vs 9.3%, P=0.02) (Supplement 5B and 5C, respectively). The high level of education was inversely associated with learning about the positive role of smoking cessation in cancer prevention (Supplement 5D, P=0.04).
Summary of due cancer prevention measures fulfilled at 6-month follow-up.
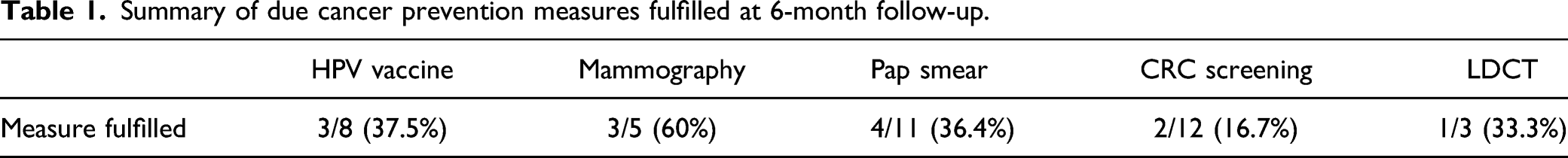
Summary of barriers to fulfilling due cancer prevention measures.

Discussion
The feasibility of using an online module for increasing compliance with cancer prevention measures was examined in this pilot study. An online module consisting of a one-minute animated video and a short questionnaire was developed and administered among volunteers who had previously agreed to participate in research studies. The online module was well received and those who participated demonstrated increased knowledge about cancer prevention measures. In addition, about a third of recommended measures due were fulfilled at 6-month follow-up.
Despite the fact that these volunteers had previously agreed to be contacted about research studies, the participation rate, through email solicitations, was low. However, the recruitment rate was similar to another study which used advertising banners on Facebook to enroll in a survey study about HPV and cervical cancer. Among the 3312 people who visited their research study online homepage, 394 (11.9%) expressed interest in participating in their study, and only 243 (7.3%) completed their online survey. 27 It may be that a more personalized approach is needed. Indeed, a meta-analysis reported that personalized telephone calls increased the uptake of CRC screening with the effect size ranging from unadjusted risk ratio (RR)=1.29 [95% confidence interval (CI) = 1.12–1.49] to RR=1.34 (CI = 1.13–1.60). On the other hand, automated telephone call reminders playing a recorded message had no effect on screening uptake. Other forms of automated reminders like emails and text messages also did not show any effect in screening uptake. 28
In the current study, the lowest response rate to the email solicitations was recorded for the age group of 50 years and older (Figure 1A), yet this age group was the highest in gaining knowledge about cancer prevention measures (Figure 1B). The risk of cancer increases with age. 29 As per a report from 2017 on cancers worldwide, approximately 70% of all cancer incidences and 87% of all cancer-associated mortalities occur in people over 50 years of age. 30 Therefore, a future focus will be to effectively target this age group for recruitment.
Lower health literacy level correlated significantly with gaining knowledge about HPV vaccination (Supplement 5A). Likewise, not being affiliated with the health care field was correlated with learning about HPV vaccination being due (Supplement 5C). Interestingly, no significant association was found with educational level and gaining knowledge about HPV vaccination. Gaining knowledge about the benefits of weight loss was associated with not being affiliated with the health care field (Supplement 5B) and associated with levels of education at a marginal statistical significance (Supplement 5F). Likewise, lower levels of education were marginally associated with gaining knowledge about mammography (Supplement 5E). These associations were expected as higher healthy literacy level, higher level of education, and being in the health care field should make one more knowledgeable about cancer prevention methods.4,31-36
The barriers to cancer prevention measures uptake we found in this study were consistent with barriers that have been reported in other studies,3-5 including cost, lack of insurance, and time required. In addition to these previously known barriers, we identified patient confusion about when screening tests are due as a barrier. One provider recommended LDCT every 5 years instead of yearly as recommended by the USPSTF (Supplement 2B). Similarly to discordant recommendations between provider and professional societies, different societies endorse different screening parameters. For example, the ACS recommends colonoscopy to high-risk group aged 40 years and above, while USPSTF does not make such a recommendation. Taken together, screening/prevention measure recommendations vary between providers and societies, which can contribute to patient confusion, and ultimately to loss of follow-up.
The strength of our study was the well-designed module intended to fill a gap in knowledge about the importance of cancer prevention measures for the general public. Its shortcoming was relying on self-reporting for assessing learning. Nevertheless, the online module increased knowledge and demonstrated uptake of overdue cancer prevention measures and could be utilized to promote them among the general population. A better method of soliciting participation would need to be explored. As a number of studies have reported smartphones to be the most widely available high-tech communication device,37-39 texting potential participants a single-click link to the online module could be a solicitation method more easily adapted by the masses, including by those in older age groups. 37
Conclusion
The online module which consisted of one-minute animated video and a short questionnaire was developed and was successful in increasing knowledge about cancer prevention measures. Furthermore, a third of due cancer screening was performed within the 6-month follow-up period. Interestingly, those who were 50 years and older were less likely to participate in the study but more likely to gain knowledge about cancer prevention measures they were not aware of previously. Therefore, our future efforts would expand the use of this online module to the general population of Arkansas in a manner easy enough for the older age group to participate.
Supplemental Material
sj-pdf-1-ccx-10.1177_10732748211037908 – Supplemental Material for Assessing the Feasibility of an Online Module for Promoting Cancer Prevention Measures
Supplemental Material, sj-pdf-1-ccx-10.1177_10732748211037908 for Assessing the Feasibility of an Online Module for Promoting Cancer Prevention Measures by Sumit K. Shah, Brittany E. Demmings, Milan Bimali, Kristie Hadden and Mayumi Nakagawa in Cancer Control
Footnotes
Acknowledgments
The authors would like to thank Benjamin J. Lieblong, PhD for critical review of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article: This work was funded by the Arkansas Biosciences Institute (the major component of the Tobacco Settlement Proceeds Act of 2000), the Drs Mae and Anderson Nettleship Endowed Chair of Oncologic Pathology, the Cancer Prevention and Population Sciences Program Pilot Project Award from the Winthrop P. Rockefeller Cancer Institute at UAMS, and grants from the National Institutes of Health (U54 TR001629, UL1 TR003107, and CA143130).
Ethical approval
This study was approved by the Institutional Review Board (#228815) at UAMS. A solicitation email sent included the purposes of the research study, eligibility criteria, contact information of the investigators, and a link to the one-minute animation video and questionnaires. Clicking on the link served as an informed consent process and confirmation of eligibility criteria. This study was registered at ![]() (NCT03910053).
(NCT03910053).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
