Abstract
The COVID-19 pandemic has introduced many new stressors for parents worldwide. This study investigated the link between parents’ cumulative stress and psychological distress during the pandemic. Parents’ emotion dysregulation was further examined as a moderator between cumulative stress and psychological distress. A total of 155 parents in the United States participated in the present study. Path analysis was conducted to evaluate the effects of cumulative stress, including COVID-19-related stress, general stress, and parental stress, as well as emotion dysregulation on parents’ psychological distress, including depression and anxiety. The present findings indicated that parents’ general stress, parental stress, and emotion dysregulation predicted symptoms of depression. Emotion dysregulation further exacerbated the effect of parental stress on depression. Parents’ general stress and emotion dysregulation were also predictive of anxiety symptoms. In addition, emotion dysregulation exacerbated the effect of COVID-19-related stress on parental anxiety. This study revealed that parents’ stress and emotion dysregulation were additively and interactively associated with their psychological distress. The findings inform researchers and practitioners that parents’ stressors have cumulative effects on their psychological distress and that emotion dysregulation can worsen the negative effect of stress on mental health in challenging times, such as the pandemic.
Keywords
The coronavirus disease (COVID-19) pandemic posed a major threat worldwide given its health, social, and financial implications (Dawes et al., 2021; Palacios Cruz et al., 2021; Prime et al., 2020), resulting in a host of challenges for families such as financial insecurity, disrupted routines, social isolation, and reduced resources (Adams et al., 2021; Dawes et al., 2021; Fontanesi et al., 2020; Li et al., 2022). Coupled with other preexisting stressors, parents’ multifaceted and heightened levels of stress were concerning, as they were linked to poorer family dynamics and mental health (Adams et al., 2021; Cheng et al., 2021; Cheung et al., 2022; Frankel et al., 2023).
Parents’ Experience of Cumulative Stress and Psychological Distress
In their conceptual model, Prime et al. (2020) postulated that unprecedented COVID-19-related stressors such as job loss, confinement, and social distancing have a significant impact on parental well-being. The cumulative risk model further asserts that parents’ experiences of stressors can “stack up” and result in poorer mental health (e.g., Everhart et al., 2008; Roskam & Mikolajczak, 2022; Shaw et al., 2016). Furthermore, parents with multiple and greater levels of adversities (e.g., divorce, physical victimization, incarceration) have markedly worse mental and physical health than their counterparts (Borja et al., 2019). Likewise, risk factors such as unemployment, single parenthood, and child disability can accumulate to predict parental burnout (Roskam & Mikolajczak, 2022). Indeed, the studies conducted before the pandemic revealed the negative effects of parents’ perceived stress on mental health. For instance, Thomason et al. (2014) found that parenting stress longitudinally predicted symptoms of depression in mothers at postpartum. In addition, mother–child dysfunctional interaction and mothers’ symptoms of depression cyclically predicted one another. Other family members also play a role in mothers’ depression. For example, mothers’ and fathers’ preexisting symptoms of anxiety, parenting stress, and their partners’ depression were related to the persistence of postpartum depression longitudinally (Vismara et al., 2016). As such, multiple parental risk factors can accumulate or interact with each other to worsen parents’ mental health. For example, spousal perceptions of coparenting quality might moderate the association between parenting stress and general distress, such that the association was significant when coparenting quality was perceived to be high (Turgeon et al., 2023).
A pair of studies conducted during the COVID-19 pandemic similarly revealed that parents’ stress was negatively related to their mental health. However, the relation was dependent on third variables including parents’ gender, racial discrimination, and negative emotions during the pandemic (Cheung et al., 2022; Park et al., 2022). Notably, Park et al. (2022) found that Korean American fathers’ parental stress was predictive of their psychological distress. As for Korean American mothers, parental stress interacted with racial discrimination to predict psychological distress. As such, discrimination moderated the stress–distress association. In another study, Cheung et al. (2022) found that fathers’ perceived COVID-19-related stress and negative emotions during the pandemic additively predicted their symptoms of depression. However, for mothers, perceived COVID-19-related stress interacted with negative emotions during the pandemic, such that their stress was linked to symptoms of depression only when their negative emotions were high.
Taken together, the literature reveals a negative relation between parents’ stress and mental health in studies both before and during the COVID-19 pandemic. Consistent with the cumulative stress model, the stressors perceived by parents accumulate to affect their mental health. Moreover, third variables such as discrimination, negative emotions, mindfulness, and coparenting, can further moderate the link between parents’ perceived stress and mental health (Cheung et al., 2022; Park et al., 2022; Turgeon et al., 2023; Wang et al., 2021).
The Role of Parents’ Emotion Regulation in Mental Health
According to Gross (1998), emotion regulation is a process that involves modulating emotions and modifying emotional responses. Gratz and Roemer (2004) further postulated that emotion dysregulation entails difficulties in accessing adaptive emotion regulation strategies, maintaining emotional awareness and clarity, accepting emotional responses, engaging in goal-directed behavior, and exercising impulse control. Recent studies revealed that parents’ ability to regulate emotions is central to their mental health (Coo et al., 2022; Töz et al., 2023). Notably, when parents exhibit emotion regulation difficulties, they also experience psychological distress, such as symptoms of depression and anxiety (Cardoso & Fonseca, 2023). In a study involving new mothers (Haga et al., 2012), those who engaged in maladaptive emotion regulation strategies such as rumination, self-blame, and catastrophizing were more likely to report postpartum depression. In another study (Wolff et al., 2020), parents who had difficulty accessing emotion regulation strategies were more likely to experience symptoms of depression.
Returning to Prime et al.'s conceptual model of family well-being during the pandemic (2020), parents with preexisting vulnerabilities, such as poor emotion regulation and mental health concerns, are at a heightened risk for poor outcomes. Supporting this framework, a recent study found an interaction effect between parental emotion regulation and distress on parenting during the national lockdown in Israel (Cohen et al., 2022). Specifically, when parents were emotionally dysregulated, parental distress was negatively related to positive parenting and positively related to negative parenting. Taken together, emotion regulation may be key to parental functioning and mental health.
The Present Study
The present study investigated the extent to which parental stressors, including COVID-19-related stress, general stress, and parental stress, were linked to parents’ psychological distress during the COVID-19 pandemic. These types of stressors were included in this study, as they were commonly reported by parents during the pandemic (e.g., Calvano et al., 2022; Kishida et al., 2021; Wade et al., 2021). Grounded in Prime et al.'s conceptual framework of family well-being (2020) and the cumulative risk model (Everhart et al., 2008; Roskam & Mikolajczak, 2022; Shaw et al., 2016), the present study further evaluated the moderating role of emotion dysregulation between parents’ experiences of stress and psychological distress. Specifically, we hypothesized that parents’ perceived COVID-19-related stress, general stress, parental stress, and emotion dysregulation would additively predict psychological distress, including symptoms of depression and anxiety (Hypothesis 1). In addition, emotion dysregulation would moderate the association between parents’ stress and psychological distress, such that the association would be stronger when emotion dysregulation was high (Hypothesis 2). In this study, parents’ age, gender, income, and living with someone diagnosed with COVID-19 were included as covariates, as previous studies indicated that they were associated with psychological distress (e.g., Gray et al., 2020; Hao et al., 2022; Kim & Kim, 2021).
Method
Participants
The present data were drawn from a larger study conducted between January and June 2021 to examine the effect of the COVID-19 pandemic on families (Vaydich & Cheung, 2023). A total of 155 parents at 18 to 69 years of age (M = 39.66, SD = 7.17; 94.84% female) residing in the United States were recruited through social media platforms and organizations serving families and parents. Of the participants, 80.52% were self-identified as White or European, followed by biracial or multiracial (11.04%), Asian or Asian American (5.19%), Latina/o/x (1.30%), African American or Black (0.65%), American Indian or Alaska Native (0.65%), and other (0.65%). In addition, 86.45% of the parents were married, with a range of one to five children (Mage = 7.83, SD = 5.19). A majority of the parents (80.65%) reported having a university degree or above. The median annual household income before and during the COVID-19 pandemic was US$101,000–US$125,000. A total of 11.61% (n = 18) of the parents reported that someone in their household received a COVID-19 diagnosis at the time of data collection.
Measures
COVID-19-Related Stress
The 36-item COVID Stress Scale (Taylor et al., 2020) was used to assess COVID-19-related stress over the past seven days on a 5-point scale ranging from 1 (not at all) to 5 (extremely). Based on a review of the literature (e.g., Taylor, 2019) and consultation with experts, 58 items were developed (Taylor et al., 2020). The 58-item measure was subsequently shortened to 36 items and demonstrated adequate psychometric properties. Notably, upon exploratory and confirmatory factor analysis (Taylor et al., 2020), the measure resulted in a five-factor model, with subscales including COVID danger and contamination, COVID socioeconomic consequences, COVID xenophobia, COVID compulsive checking, and COVID traumatic stress symptoms. According to Taylor et al. (2020), the COVID Stress Scale demonstrated convergent validity, with significant correlations with pre-COVID trait measures of health anxiety as well as symptoms of obsessive-compulsive checking and contamination. It also demonstrated discriminant validity, with stronger correlations with current anxiety than with current depression (Taylor et al., 2020). The sample items included, “disturbing mental images about the virus popped into my mind against my will” and “reminders of the virus caused me to have physical reactions, such as sweating or a pounding heart.” In this study, the item scores were averaged to create a mean score, with higher scores reflecting greater COVID-19-related stress. The measure demonstrated good internal consistency, with Cronbach's α = .93.
General Stress
The seven-item stress subscale of the Depression Anxiety Stress Scale-21 (DASS-21; Lovibond & Lovibond, 1995) was used to measure parents’ general stress over the past week on a five-point scale ranging from 1 (did not apply to me at all) to 4 (applied to me very much/most of the time). The sample items included, “I found myself getting agitated” and “I found it difficult to relax.” In this study, the item scores were summed, with higher scores indicating greater general stress. The measure demonstrated adequate internal consistency, with Cronbach's alpha = .86.
Parental Stress
The 18-item Parental Stress Scale (Berry & Jones, 1995) was used to assess parental stress on a 5-point scale from 1 (strongly disagree) to 5 (strongly agree). The sample items included, “It is difficult to balance different responsibilities because of my child(ren)” and “The major source of stress in my life is my child(ren).” The raw scores of the negatively worded items were reversed. The final item scores were summed, with higher scores indicating greater parental stress. The measure demonstrated adequate internal consistency, with Cronbach's α = .88.
Emotion Dysregulation
The 36-item Difficulties in Emotion Regulation Scale (DERS; Gratz & Roemer, 2004) was used to measure parents’ dysregulation of emotions on a 5-point scale ranging from 1 (almost never) to 5 (almost always). The DERS has six subscales including lack of emotional awareness, nonacceptance of emotional responses, limited access to emotion regulation strategies, difficulties engaged in goal-directed activities, lack of emotional clarity, and impulse control difficulties. The sample items included, “When I’m upset, I believe that there is nothing I can do to make myself feel better” and “When I’m upset, I become angry with myself for feeling that way.” In this study, the item scores were summed, with higher scores indicating greater emotion dysregulation. The measure demonstrated good internal consistency, with Cronbach's alpha = .93.
Symptoms of Depression
The seven-item depression subscale of the DASS-21 (Lovibond & Lovibond, 1995) was used to measure parents’ symptoms of depression over the past week on a 5-point scale ranging from 1 (did not apply to me at all) to 4 (applied to me very much/most of the time). The sample items included, “I felt that I had nothing to look forward to” and “I was unable to become enthusiastic about anything.” In this study, the item scores were summed, with higher scores indicating greater symptoms of depression. The measure demonstrated adequate internal consistency, with Cronbach's alpha = .89.
Symptoms of Anxiety
The seven-item anxiety subscale of the DASS-21 (Lovibond & Lovibond, 1995) was used to measure parents’ anxiety symptoms over the past week on a 5-point scale ranging from 1 (did not apply to me at all) to 4 (applied to me very much/most of the time). The sample items included, “I was worried about situations in which I might panic and make a fool of myself” and “I felt scared without any good reason.” In this study, the item scores were summed, with higher scores indicating greater anxiety symptoms. The measure demonstrated acceptable internal consistency, with Cronbach's alpha = .78.
Sociodemographic Data
Participants reported sociodemographic data such as gender, age, race, relationship status, annual household income, level of education, and COVID-19 diagnosis in the household.
Procedures
Prior to participation, participants gave consent and completed the anonymized online survey via Qualtrics from January to June 2021. The present study was conducted in accordance with the APA Code of Ethics. Ethics approval was obtained at the second author's university institutional review board.
Analytic Strategy
Path analysis was conducted to examine the fit of the hypothesized model to the data. The data were missing completely at random (MCAR) according to Little's MCAR test, χ2(121) = 127.06, p = .34. Full information maximum likelihood estimation was used to treat the missing data at the item level. To facilitate the interpretability of the moderation effects, COVID-19-related stress, general stress, parental stress, and emotion dysregulation were centered on the mean. To examine the moderation effect of emotion dysregulation between stress and symptoms of depression and anxiety, the three types of stress, emotion dysregulation, and the three interaction terms between stress and emotion dysregulation, respectively, were entered into the path model. When the moderation effects were significant, post hoc simple slope tests (Aiken et al., 1991) were conducted to evaluate the differences between the slope coefficients when emotion dysregulation was low (i.e., 1 SD below the mean) versus high (i.e., 1 SD above the mean).
Results
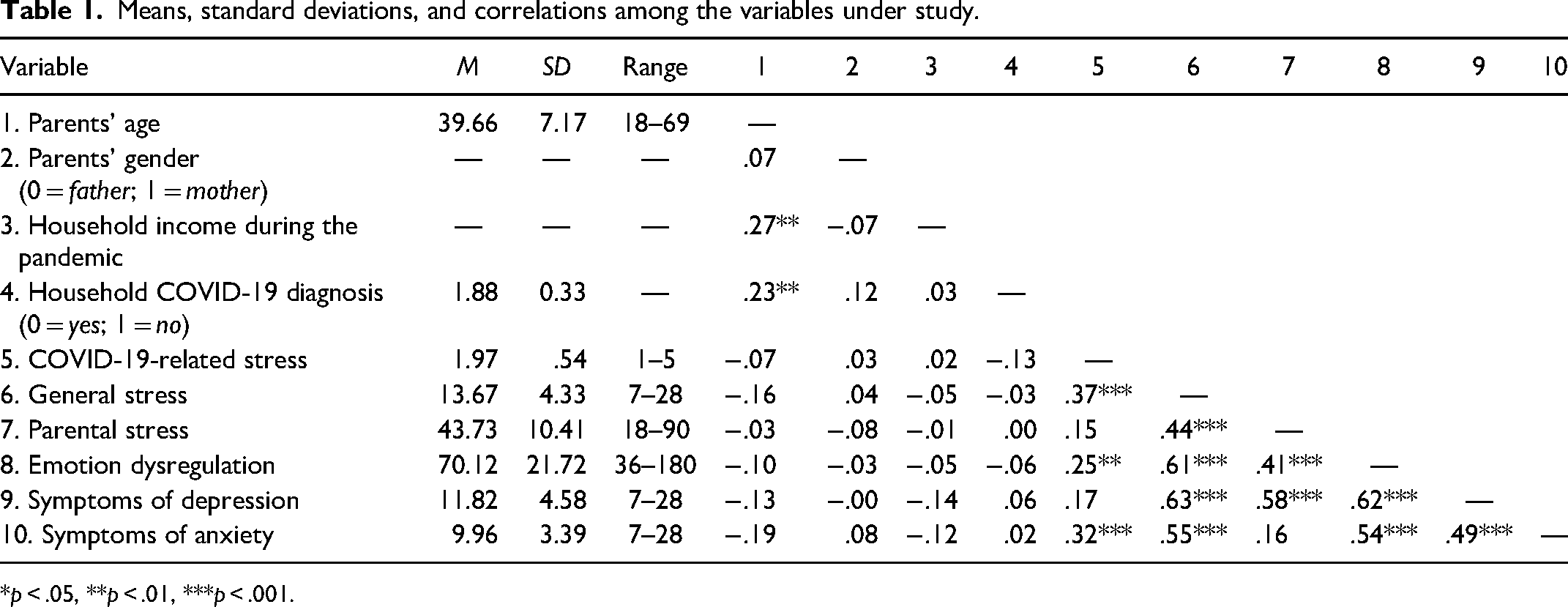
Table 1 shows the means, SDs, and zero-order correlations of the study variables. COVID-19-related stress was related to general stress (r = .37, p < .001), emotion dysregulation (r = .25, p = .001), and symptoms of anxiety (r = .32, p < .001). General stress was related to parental stress (r = .44, p < .001), emotion dysregulation (r = .61, p < .001), and symptoms of depression (r = .63, p < .001), and anxiety (r = .55, p < .001). Parental stress was related to emotion dysregulation (r = .41, p < .001) and symptoms of depression (r = .58, p < .001). Emotion dysregulation was related to symptoms of depression (r = .62, p < .001). Symptoms of depression and anxiety were related (r = .49, p < .001). Based on the established severity ratings of DASS-21 (Lovibond & Lovibond, 1995), participants of this study experienced severe levels of general stress, symptoms of depression, and symptoms of anxiety. Path analysis indicated that the moderation model fit the data well, χ2(34) = 33.75, p = 0.48, CFI = 1.00, TLI = 1.00, RMSEA = 0.00, SRMR = 0.07 (see Figure 1 and Table 2).
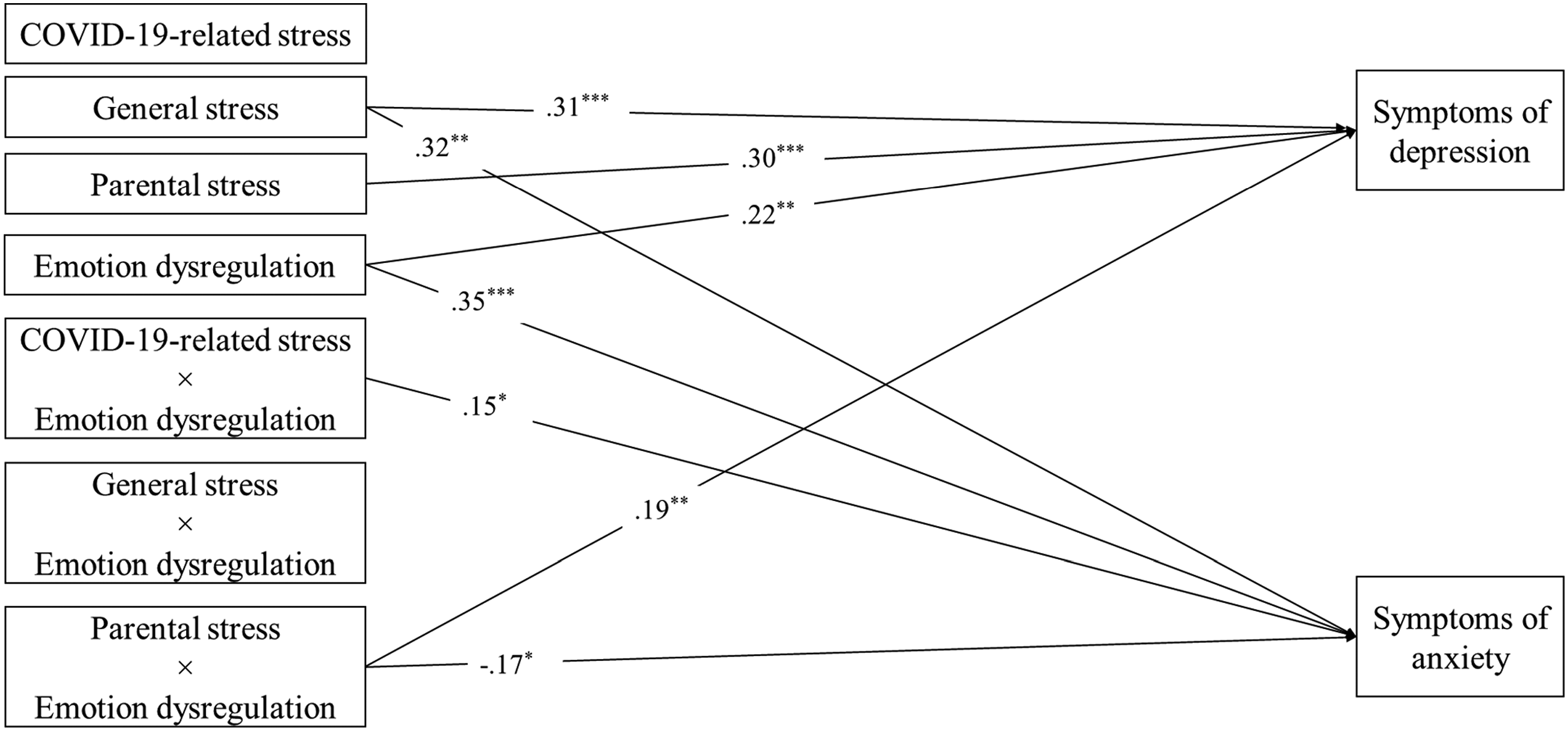
Final model of emotion dysregulation as a moderator between parents’ stress and symptoms of depression and anxiety, with age, gender, income, and living with someone diagnosed with COVID-19 as covariates. Nonsignificant paths are not depicted for clarity. χ2(34) = 33.75, p = .48, CFI = 1.00, TLI = 1.00, RMSEA = 0.00; SRMR = 0.07. *p < .05; **p < .01; ***p < .001.
Means, standard deviations, and correlations among the variables under study.
*p < .05, **p < .01, ***p < .001.
Parameter estimates of the mediation model.
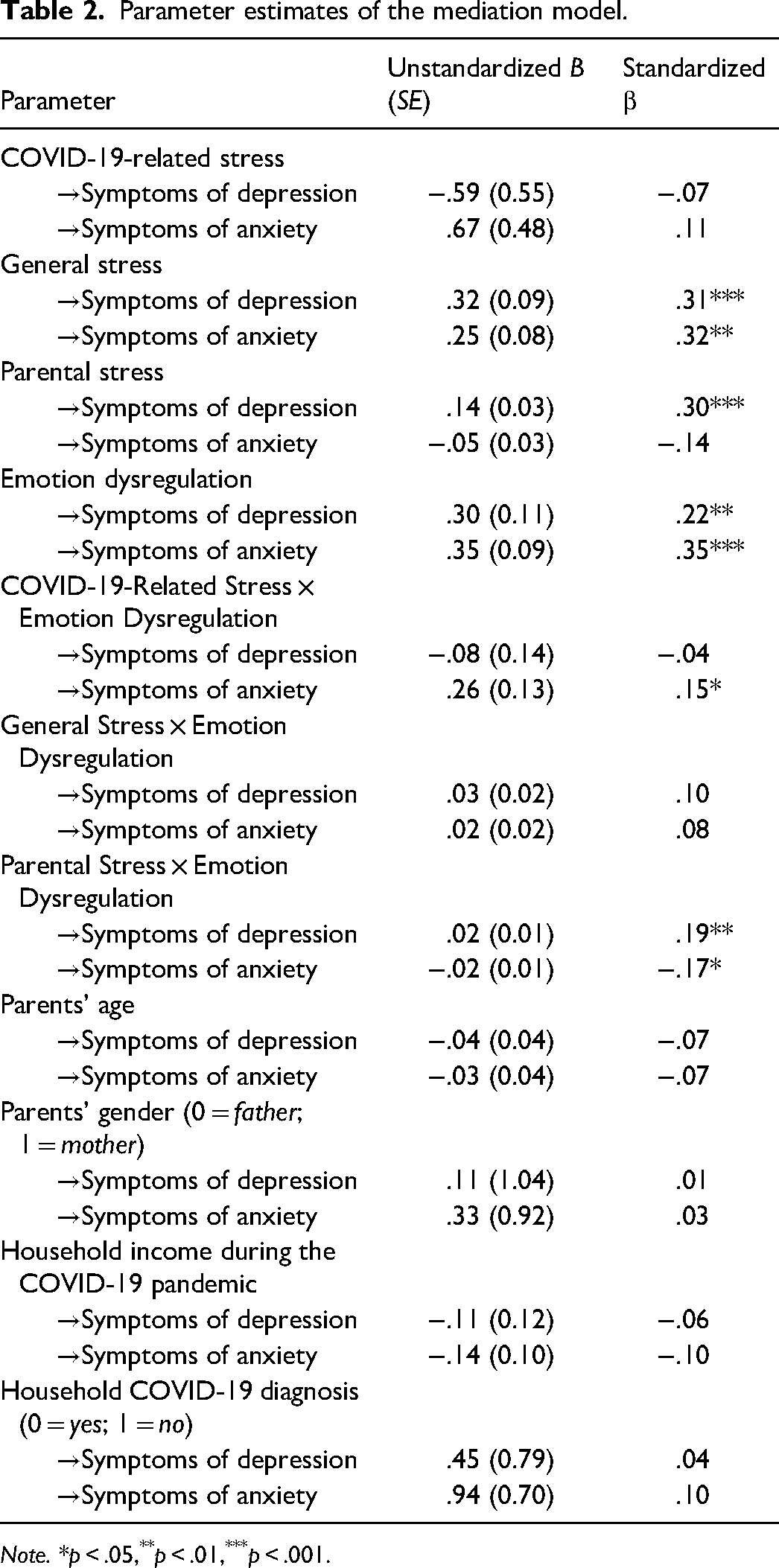
Note. *p < .05,**p < .01,***p < .001.
Hypothesis 1: Parents’ cumulative stress and emotion dysregulation would additively predict psychological distress, including symptoms of depression and anxiety.
In the path model, general stress (β = .31, p < .001), parental stress (β = .30, p < .001), and emotion dysregulation (β = .22, p = .005) additively predicted symptoms of parental depression. However, COVID-19-related stress (β = −.07, p = .283) was unrelated to symptoms of parental depression.
In addition, general stress (β = .32, p = .001) and emotion dysregulation (β = .35, p < .001) additively predicted symptoms of parental anxiety. However, COVID-19-related stress (β = .11, p = .165) and parental stress (β = −.14, p = 0.121) were unrelated to symptoms of parental anxiety. Hence, Hypothesis 1 was partially supported.
Hypothesis 2: Emotion dysregulation would moderate the association between parents’ stress and psychological distress.
In the path model, the interaction between parental stress and emotion dysregulation (β = .19, p = .006) predicted symptoms of parental depression. Post hoc simple slopes test showed that the slope of parental stress was significantly different from zero when emotion dysregulation was high, but not when it was low. That is, the relation between parental stress and symptoms of depression revealed a significantly positive relation when emotion dysregulation was high (i.e., 1 SD above the mean), β = .55, p < .001, but not when it was low (i.e., 1 SD below the mean), β = .11, p = .29 (see Figure 2).
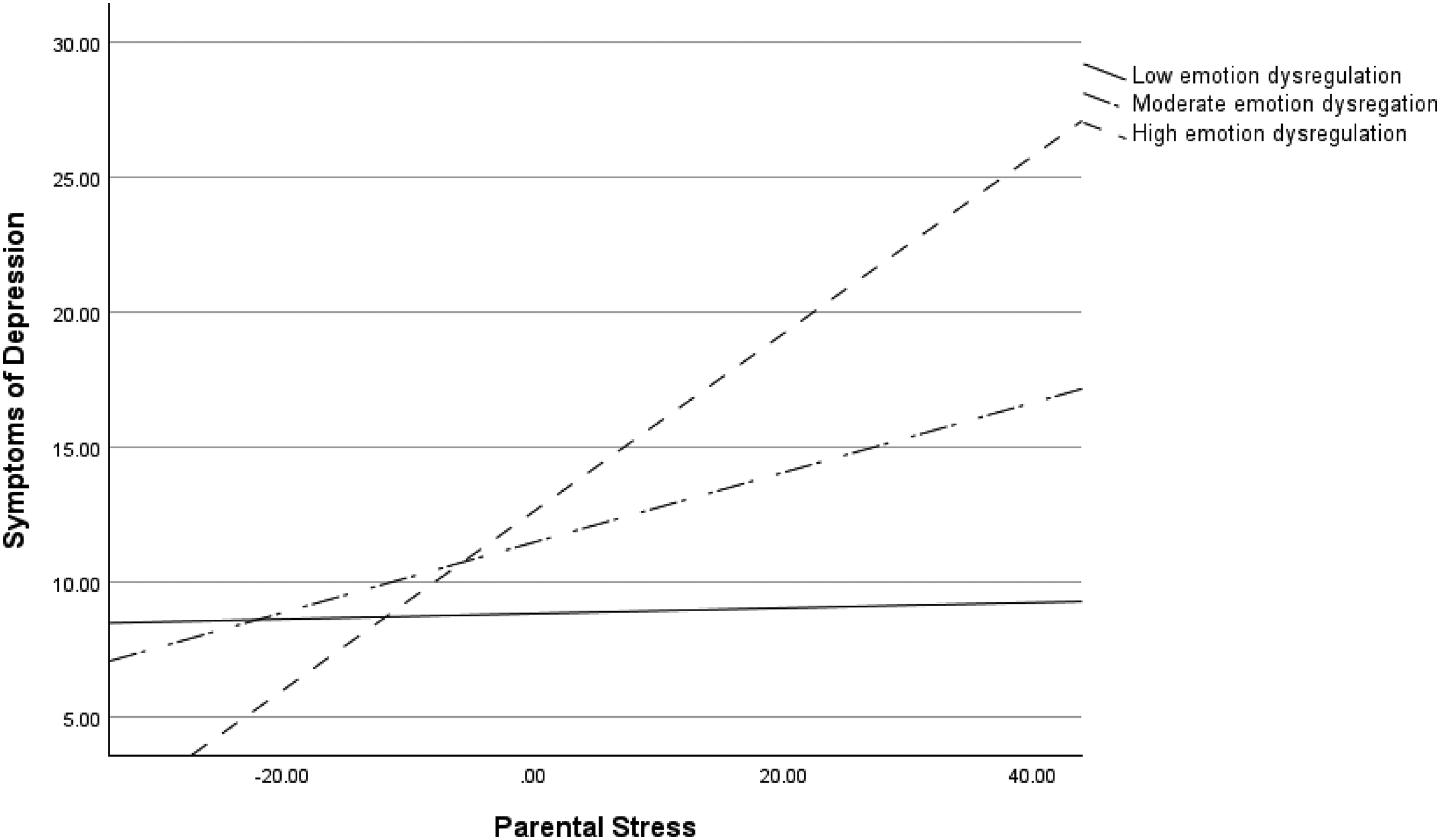
Interaction effect of parental stress and emotion dysregulation on symptoms of depression.
As for anxiety, the interaction between COVID-19-related stress and emotion dysregulation (β = .15, p = .04) and the interaction between parental stress and emotion dysregulation (β = −.17, p = .04) predicted symptoms of parental anxiety. Follow-up post hoc simple slopes test showed that the slope of COVID-19-related stress was significantly different from zero when emotion dysregulation was high, but not when it was low. That is, the relation between COVID-19-related stress and symptoms of anxiety revealed a significantly positive relation when emotion dysregulation was high (i.e., 1 SD above the mean), β = .29, p = .006, but not when it was low (i.e., 1 SD below the mean), β = .01, p = .95 (see Figure 3). However, post hoc simple slopes test revealed that the slope of parental stress was not significantly different from zero when emotion dysregulation was high (i.e., 1 SD above the mean), β = −.20, p = .08, nor when it was low (i.e., 1 SD below the mean), β = .00, p = 1.00. That is, although the interaction effect on anxiety was significant in the path model (β = −.17, p = .04), a closer examination revealed a zero-slope between parental stress and symptoms of anxiety, regardless of the level of emotion dysregulation. As such, the relation between parental stress and symptoms of anxiety did not differ as a function of emotion dysregulation. Based on these findings, hypothesis 2 was partially supported.
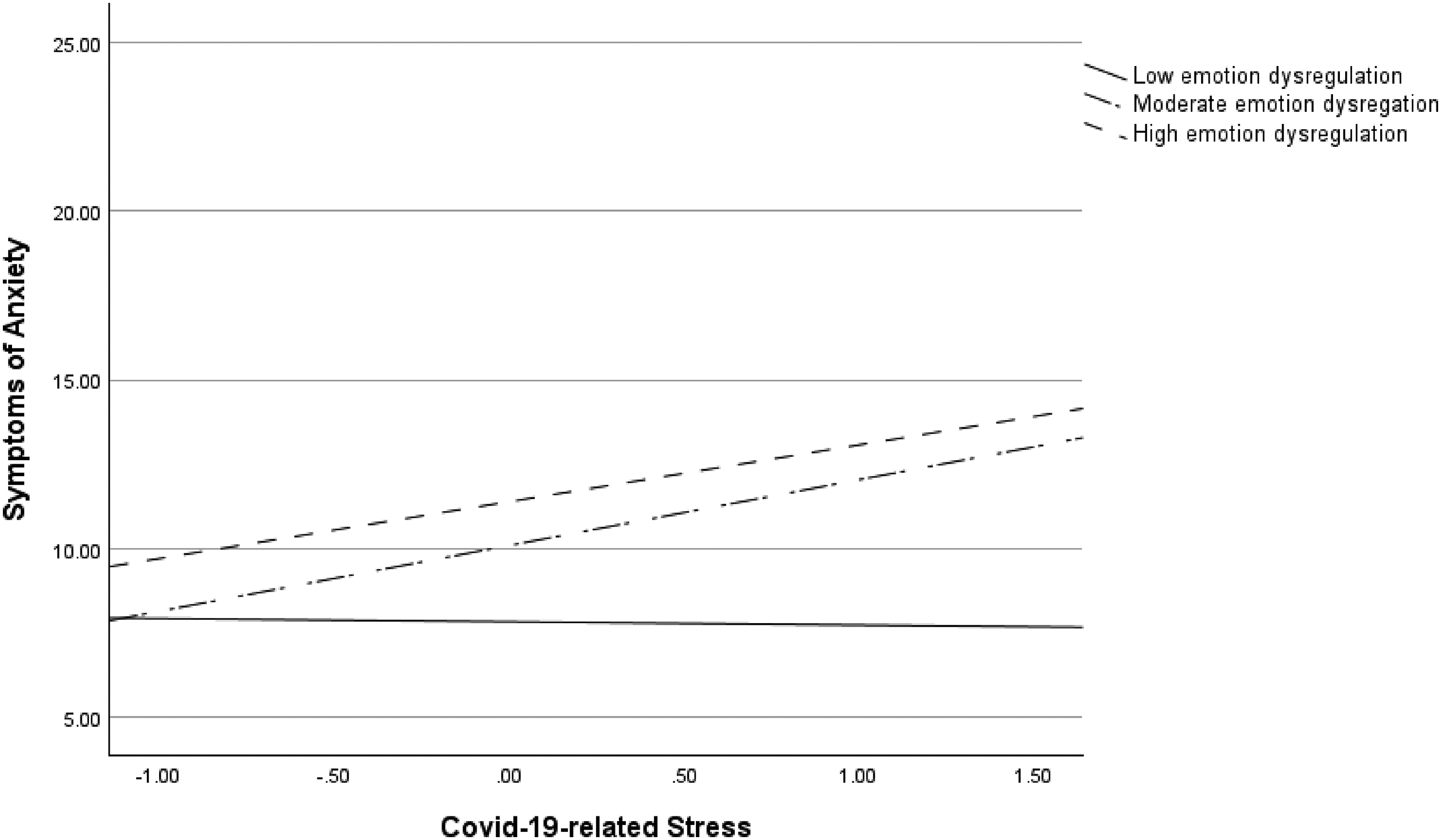
Interaction effect of parents’ COVID-19-related stress and emotion dysregulation on symptoms of anxiety.
Discussion
The present study found unique associations between parents’ stress, emotion dysregulation, and psychological distress during the COVID-19 pandemic. Supporting the cumulative stress model, parents’ experiences of general stress, parental stress, and emotion dysregulation were related to symptoms of depression. In addition, general stress and emotion dysregulation were related to symptoms of anxiety among parents. Consistent with the model of family well-being during the pandemic (Prime et al., 2020), parents’ preexisting vulnerabilities, as indexed by poor emotion regulation, interacted with COVID-19-related stress to predict anxiety, such that the stress–anxiety link was stronger when parents experienced high emotion dysregulation. Similarly, emotion dysregulation interacted with parental stress to predict symptoms of depression, such that the stress–depression link was only significant when parents were highly dysregulated.
Supporting previous research (Calvano et al., 2022; Kishida et al., 2021), general stress was commonly reported during the pandemic and it was directly related to parents’ psychological distress, including their symptoms of depression and anxiety. In the face of new challenges, parents who were agitated, overreactive, and difficult to relax in general were particularly vulnerable. While there was a direct association between parental stress and symptoms of depression (see also Calvano et al., 2022), a closer examination of the path model revealed that the link was exacerbated by emotion dysregulation, such that the positive parental stress–depression link was significant when parents were highly dysregulated. On the contrary, when parents exhibited adaptive emotion regulation, parental stress was not associated with depression at all. This finding points to the potential significance of emotion regulation in times of stress. Even when parents reported feeling overwhelmed caring for their children and balancing responsibilities, as long as they were equipped with adaptive emotion regulation skills, they experienced fewer symptoms of depression and anxiety during this difficult period.
As a risk factor from the pandemic, COVID-19-related stress was not directly related to parents’ symptoms of depression or anxiety. The null findings were inconsistent with the literature, which had previously found that pandemic-related stress was associated with symptoms of parental depression and anxiety (Calvano et al., 2022; Cheung et al., 2022). Nevertheless, the moderation analysis did reveal that emotion dysregulation worsened the effect of COVID-19-related stress on parental anxiety. Once again, when parents exhibited high emotion dysregulation, COVID-19-related stress was positively associated with anxiety. In contrast, when parents exhibited low emotion dysregulation (i.e., when they were regulated), COVID-19-related stress was not associated with anxiety. During the pandemic, COVID-19-related stress such as worries about the healthcare system, stores running out of groceries and cleaning supplies, and the virus in general could provoke anxiety among people, including parents. However, when parents were less emotionally dysregulated, that is, when they were able to exercise adaptive emotion regulation strategies, maintain emotional clarity and awareness, accept their emotions, and engage in goal-directed behavior and impulse control, then they did not become anxious amid experiences of COVID-19-related stress.
Implications for Family Counselors
In this study, COVID-19-related stress was not directly related to symptoms of parental depression and anxiety. Although parents experienced stress due to the pandemic, general stress and parenting stress were better predictors of mental health concerns they reported. Furthermore, parenting stress was related to symptoms of depression, but only when parents experienced difficulty regulating their emotions. Similarly, COVID-19-related stress was associated with symptoms of anxiety, again, only when parents experienced higher levels of emotion dysregulation. As such, family counselors should prioritize enhancing parents’ emotional regulation to support stress management during challenging times. Improving emotion regulation skills may be an important way counselors can help parents manage immediate stressors as well as parental stress. Mental health interventions for parents should highlight emotion regulation as a major skillset to support mental health and better equip parents to cope with sudden stress more adaptively.
Limitations and Future Directions
The present findings should be interpreted in light of several limitations. First, a self-report survey was used in this study, which could give rise to self-report bias and common method bias (Podsakoff et al., 2012). Hence, future studies should utilize a multimethod and multiinformant approach to assess the variables of interest (Podsakoff et al., 2012). In the study of stress, for instance, researchers may seek partner-report and collect physiological or hormonal data (Totenhagen et al., 2023). Next, the participating mothers were predominantly White, college-educated, and living in the western United States (Totenhagen et al., 2023). The participants also reported similar median annual household income before and during the COVID-19 pandemic (see Participants section). As such, the current sample might not be representative of parents across the United States, or of mothers worldwide, who reported reduced financial security and job loss (Calvano et al., 2022). Future studies should include more ethnically and socioeconomically diverse samples to increase generalizability. Third, the present study was cross-sectional. In addition, participants reportedly experienced severe levels of general stress and symptoms of depression and anxiety at the time of data collection. As parents’ dysfunctions might have been heightened during the pandemic, future studies should collect longitudinal data to capture trajectories of change, directionality of effects, and mediation processes underlying parents’ mental health (Cole & Maxwell, 2003; Maxwell & Cole, 2007). Finally, the present study examined the role of stress and emotion dysregulation on parents’ psychological distress. In light of the current findings, researchers should further examine the role of parental emotion dysregulation in mental health, particularly during challenging times. Given that parents’ stress and mental health are central to children's internalizing and externalizing problems (Cheung & Wang, 2022; Prime et al., 2020; Thompson et al., 2022), future research should also integrate and extend the present findings in relation to child outcomes.
Conclusion
Notwithstanding the limitations, this study lent support to the conceptual model of family well-being during the pandemic and the cumulative stress model (e.g., Prime et al., 2020; Roskam & Mikolajczak, 2022). Specifically, our findings indicated differential effects of multiple stressors on parents’ psychological distress. The findings also revealed moderation effects, such that parents’ emotional dysregulation worsened the effects of COVID-19-related stress and parental stress on mental health. Drawing from these findings, interventions focused on enhancing parents’ emotion regulation merit future investigations.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
