Abstract
With a median caseload of 750–1,000 clients, school nurses face setting-specific challenges involving multiple, competing demands. This necessitates effective prioritization to prevent missed opportunities to provide appropriate care. This integrative review synthesizes the current state of the literature related to prioritization among school nurses in the United States. Three themes were identified relating to prioritization among school nursing: knowledge, attitudes and values; self-efficacy and intention to act; and the nursing process. The prioritization behavior of school nurses can be facilitated by organizational and community collaboration and strong evidence-based practice recommendations. High workloads and inadequate resources among school nurses are the most consistently cited barriers to effective prioritization. Additional research on how to improve effective prioritization among school nurses for the improvement of population health outcomes is needed.
School nurses are critical leaders in improving health and quality of life for Americans throughout the lifespan (Bergren, 2017b). School nurses must balance many priorities including acute care needs and preventive and public health tasks (Best et al., 2018; Maughan et al., 2016). While trends within school nursing practice increasingly emphasize leadership and population health management (Bergren, 2017a; Buduhan & Woodgate, 2021; Davis et al., 2021; Hunt et al., 2015), school nurses typically do not spend the majority of their time on these tasks (Davis et al., 2021). School nurses must prioritize their actions to effectively balance these competing demands and maximize their impact, however, little research has been conducted on the phenomenon of nursing prioritization in the school setting. The aim of this integrative review is to synthesize evidence related to prioritization among school nurses in the United States (U.S.).
Background
School nurses face setting-specific challenges involving multiple, competing demands. Ethical responsibilities of nurses in all settings include determining which role demands are of the highest priority in accordance with their professional standards of practice (American Nurses Association, 2015). The role of the school nurse is articulated in the School Nursing Practice Framework™ (formerly the Framework for twenty-first Century School Nursing Practice™; National Association of School Nurses [NASN], 2024). The role includes care coordination (including direct care), community/public health, leadership, and quality improvement, all encompassed within the school nurse standards of practice. School nurses are often the only formally trained health professionals on site in schools and they work with a high degree of independence (Jameson et al., 2022). Trends within school nursing practice increasingly emphasize leadership and population health management as important roles (Bergren, 2017a; Buduhan & Woodgate, 2021; Davis et al., 2021; Hunt et al., 2015). However, responding to acute conditions and acute exacerbations of chronic conditions may take priority over primary prevention and health maintenance activities. Nurses must effectively prioritize their actions to balance competing demands and maximize desirable outcomes (Cho et al., 2020).
Prioritization entails classification of tasks into categories such as those that must be done immediately, those that can wait, and those that will remain undone (Hendry & Walker, 2004). Prioritization includes estimating and ranking risks to the client and potential interventions to avoid poor client outcomes (Jessee, 2019) and clinical decision-making that may result in rationing care due to competing demands (Jones et al., 2015). In acute care settings, the prioritization process is typically focused on individual clients, while the school nurse is responsible for both individual-level and acute care needs and for population-level nursing care (Buduhan & Woodgate, 2021). Furthermore, school nurses must engage in large-scale planning over the course of months or years and because of limited access to high-quality, population-level assessment data, they may struggle to evaluate population outcomes (Daughtry & Engelke, 2018).
Novice nurses often struggle with exercising clinical judgment in prioritizing urgent actions (Goode et al., 2009; Kavanagh & Szweda, 2017). Benner's (1982) foundational work describes how novice nurses progress to expert nurses with an implicit emphasis on the concept of prioritization. Benner discusses the ways in which nurses learn to distinguish the relative importance of factors that will determine care. The novice to expert theory does not explicitly identify prioritization, however, it does describe that nurses distinguish the relative importance of factors that will determine what care they give. Benner's (1982) model is, therefore, consistent with the definitions of prioritization as conceptualized by Hendry and Walker (2004), Jones et al. (2015), and Jessee (2019).
Purpose
While some research on prioritization among school nurses has been published, there is a lack of synthesis and comprehensive analysis of prioritization in this population. This integrative review (Whittemore & Knafl, 2005) includes a synthesis of evidence related to prioritization among school nurses in the U.S. The practice of school nursing varies significantly by country due to varied educational and healthcare infrastructure and regulations, therefore the scope of this review is limited to the U.S. This synthesis can shape future research and enhance school nurse practice models.
Methods
Search Strategy
EBSCO Host was used to search multiple databases simultaneously, which were selected due to their relevancy to nursing or education: Academic Search Complete, APA PsycInfo, CINAHL Complete, Consumer Health Complete, Education Full Text, Education Resources Information Center (ERIC), Health Source: Nursing/Academic Edition, and Professional Development Collection. An initial search was conducted in October 2022 using the search terms “school nursing” or “school nurses” and “prioritization” or “decision-making” to query databases. We consulted with the university research librarian subject specialist to increase the rigor and effectiveness of database search strategies. Consequently, a second query was conducted in November 2022 using the modified search terms of “priorit*” AND “school nurs*.” Final searches were conducted in June and December 2024 of these databases using “priorit*” AND “school nurs*” to identify new work published since the previous search. Additional sources were accessed and considered for inclusion when an included source referenced a primary work that was relevant and uniquely informative.
Inclusion and Exclusion Criteria
The inclusion criteria for this review included literature reviews with directly relevant findings, intervention studies, and observational studies published in English between 2007 and 2024 with a focus on prioritization processes of U.S. school nurses. Exclusion criteria were studies focused on prioritization of non-school nurses, editorials, book reviews, commentaries, letters to the editor, expert opinion, and practice guidelines. Screening for inclusion and exclusion criteria was completed based on the title and abstract of each record. If the source appeared to meet inclusion criteria or it was unclear whether it should be excluded based on the initial screen, the full text was obtained and reviewed by the primary author to ensure no evidence was prematurely excluded. Inclusion and exclusion criteria were then applied to a full text review of remaining records.
Literature Synthesis Method
During the data analysis stage (Whittemore & Knafl, 2005), two researchers completed multiple readings and comparisons of the sources of evidence were conducted using an iterative approach. An inductive approach without preconceived codes or categories was used. First, a matrix table was created as a data reduction tool to assist in synthesis. Common themes and patterns were identified through repeated readings and comparisons (Whittemore & Knafl, 2005). Remaining authors contributed to the analysis to produce the final matrix and write-up. Additional details on data analysis iterations are provided in Figure 1.
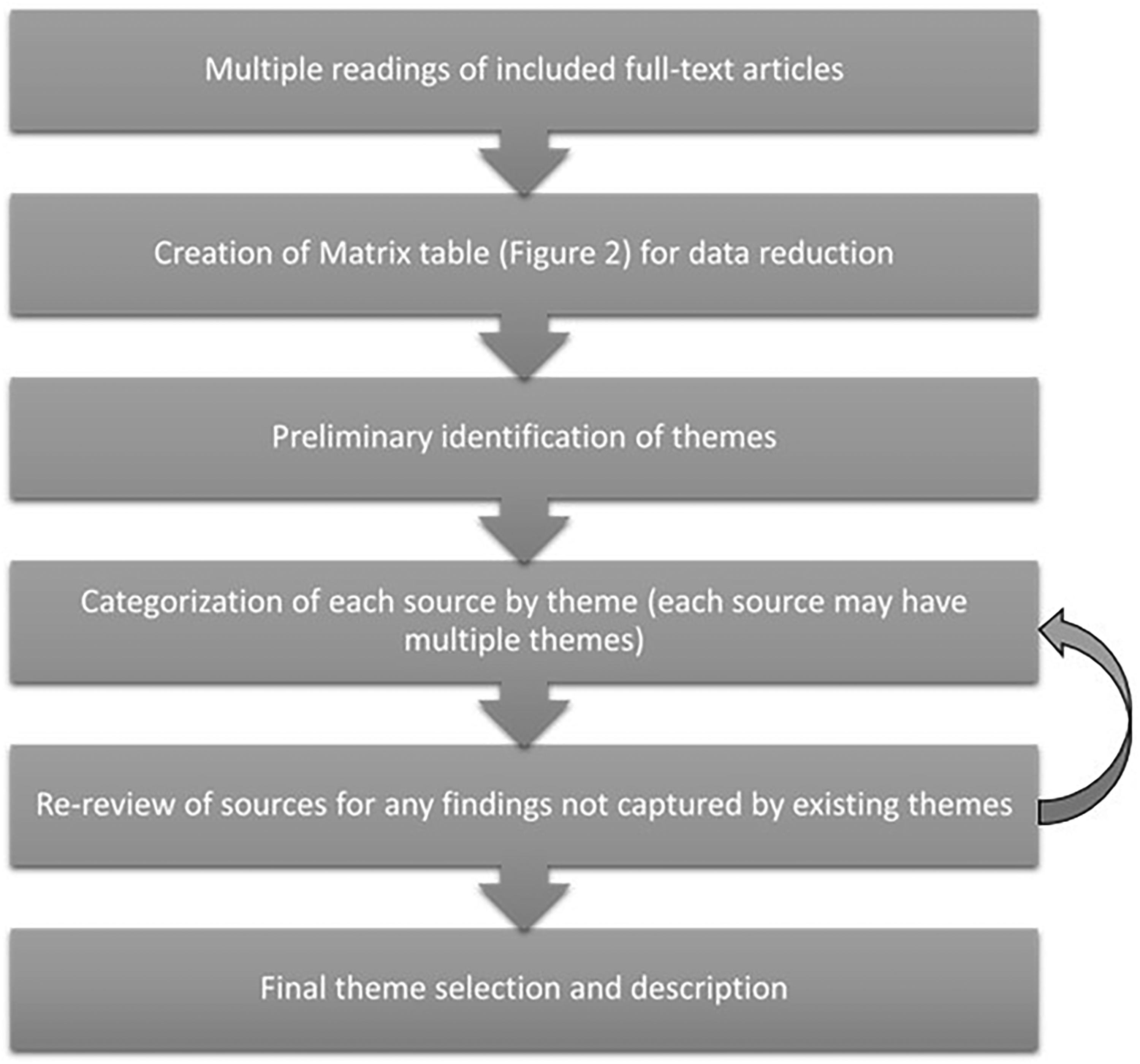
Data Analysis Flowchart.
Data Evaluation and Quality Appraisal Method
The level of evidence and quality analysis for each source of evidence is recorded in Table 1. The full text of each included article was reviewed using the Johns Hopkins Nursing Evidence-Based Practice Quality Guide (Dang et al., 2022). The sources were determined to be high quality (Category A) if they were recent (within the last 5 years based on the first literature search in 2022), described clear and consistent generalizable results and conclusions, applied trustworthy scientific evidence, and/or was systematic and comprehensive in approach. The sources that were a mixture of low- and high-quality elements were categorized as good quality (Category B). Sources were determined to be lower quality (Category C) if they were over 5 years old from the time of the first literature search in 2022, did not describe a clear method, had inconsistent or unclear results or conclusions, and/or had a small sample size. Due to limited evidence on the topic of prioritization in the specific population of school nurses, no sources were excluded based on quality appraisal alone.
Integrative Literature Review Matrix: Prioritization in School Nursing.
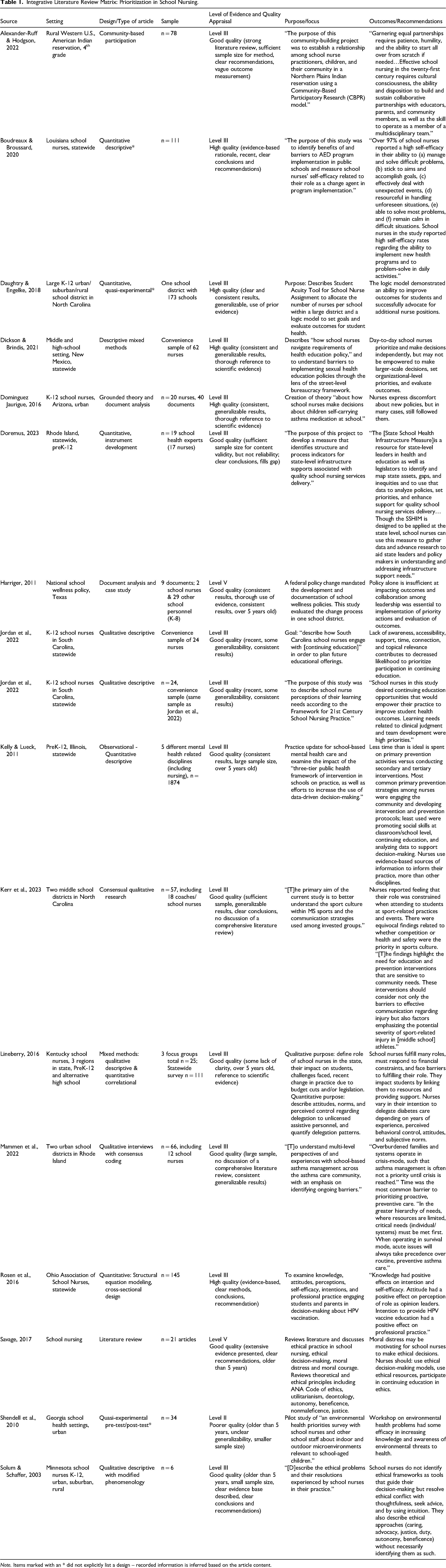
Note. Items marked with an * did not explicitly list a design – recorded information is inferred based on the article content.
Results
Database searches resulted in 321 sources of evidence for potential inclusion in this review. After initial title and abstract screening, 249 records were excluded, and the remaining 72 articles were sought for full text. All 72 articles were reviewed for inclusion and exclusion criteria resulting in 56 sources being excluded and 16 included. One relevant primary source was obtained because it was cited by an included article and met all inclusion criteria except for the date range of 2007–2024. This source is included in the final analysis despite its age because of its quality and unique contribution to the understanding of moral distress and ethical decision-making by school nurses (Solum & Schaffer, 2003). A total of 17 sources were included in the data analysis. A PRISMA-style diagram was used to visually represent the searching process and results, found in Figure 2 (Page et al., 2021).
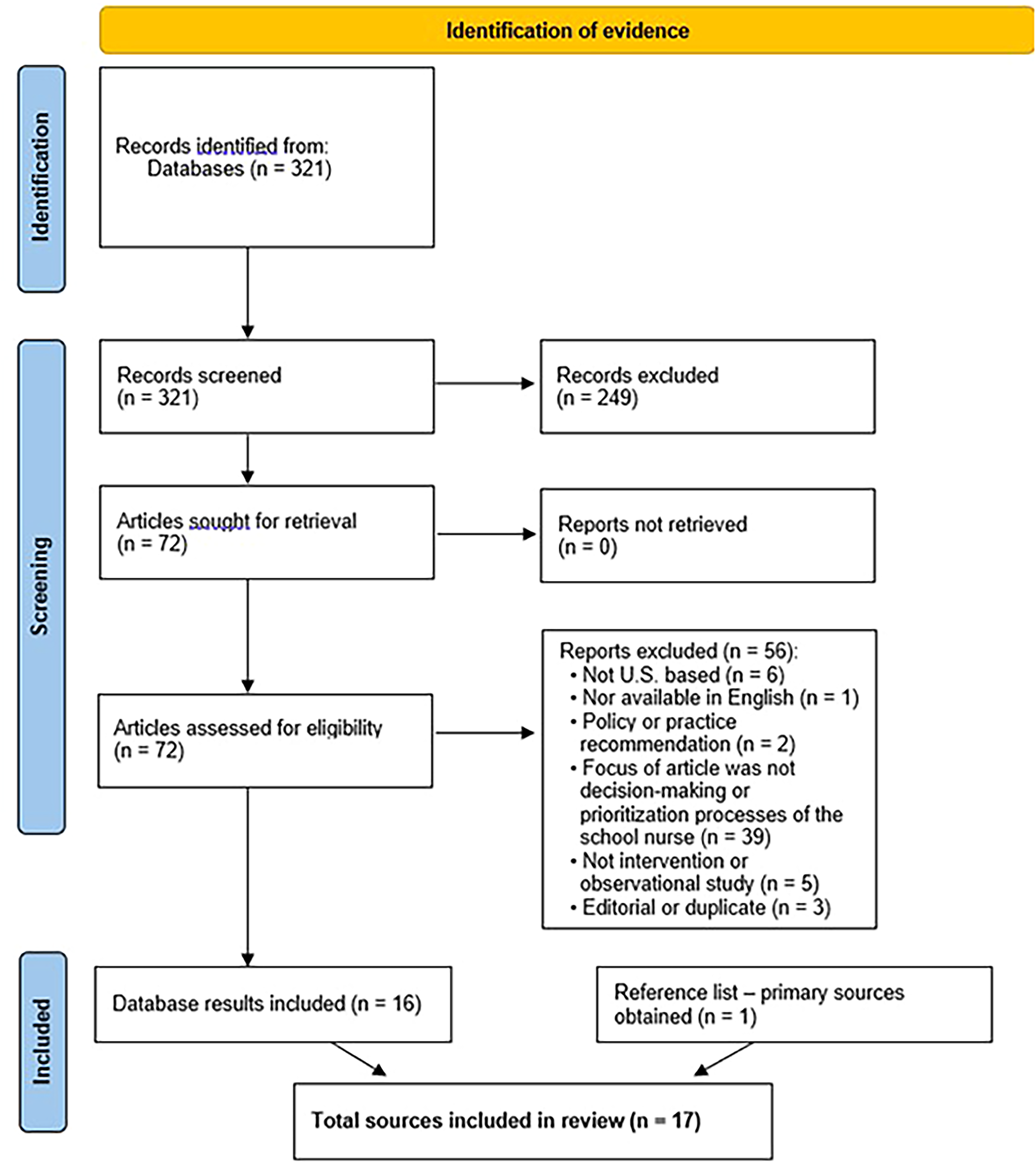
PRIMSA Diagram.
One literature review with directly relevant findings and one case study with document analysis are included in the results. Six studies were quantitative, eight studies were qualitative, two were mixed methods, and one was community-based participatory research. Among the included studies, most had a statewide sample (n = 8). Two studies included urban, suburban, and rural school nurses, one was rural only, three were urban only, and three did not specify a population density. Geographical distribution comprised studies from the Northeast (n = 2), Southeast (n = 7), Southcentral (n = 1), Midwest (n = 3), and Western region (n = 3) of the U.S. One study included only middle- and high-school settings, one included only middle school, three included pre-Kindergarten through high-school, five were K-12, one was only fourth grade, and the remaining five studies did not specify any grade setting.
The highest level of evidence was found to be Level II (n = 1) and the lowest was Level V (n = 2); the remaining sources (n = 14) are Level III on the Johns Hopkins Nursing Evidenced-Based Practice guidelines. Five studies were appraised as high quality, eleven as good quality, and one was poorer quality. Quality appraisal for each article is included in Table 1.
Integrative Synthesis
School nurses navigate and integrate both the academic and health practice domains giving them a unique vantage point. Three themes were identified in reviewing the literature as factors that impact prioritization among school nurses: knowledge, attitudes, and values; self-efficacy and intention to act; and the nursing process. Additionally, these themes each encompass facilitators and barriers to effective prioritization and decision-making for school nurses, which are discussed separately.
Knowledge, Attitudes, and Values
Knowledge is a necessary prerequisite for prioritization and decision-making (Boudreaux & Broussard, 2020; Rosen et al., 2016). Strong knowledge among school nurses can facilitate effective advocacy, but when school- or district-level policies are vague, school nurses may rely more on professional standards of school nursing to make decisions (Dickson & Brindis, 2021). However, the surrounding organizational and community environment may be more influential than knowledge in the school setting (Dickson & Brindis, 2021).
Attitudes were described by Rosen et al. (2016) to impact school nurses’ perceptions of their role, which in turn influenced their intention to act. Furthermore, attitudes of other stakeholders, including students, parents, and school administrators may also influence actions that school nurses decide to take (Dickson & Brindis, 2021; Kerr et al., 2023). However, in some contexts, attitudes may not influence school nurse decision-making about prioritization as much as resource constraints. For example, Lineberry (2016) described an inconsistency between school nurse attitudes about delegation and actual decisions to delegate medication administration. The decision to delegate medication administration (when legally permitted) to unlicensed assistive personnel was influenced by high workload and lack of resources, regardless of attitudes (Lineberry, 2016).
Values among school nurses included evidence-based practice (Dickson & Brindis, 2021; Kelly & Lueck, 2011) and practice improvement (Jordan et al., 2022). Also, school nurses prioritize activities they believe are valuable (Boudreaux & Broussard, 2020). While several ethical frameworks are articulated in the literature specific to school nursing practice (Savage, 2017), school nurses do not typically identify ethics as a source of influence for their prioritization and decision-making (Solum & Schaffer, 2003). However, the experience of moral distress when faced with only unpleasant outcomes may be motivating for school nurses to make ethical decisions and to be relieved of the distress (Savage, 2017). Moreover, school nurses engage in thoughtful decision-making informed by their values. They describe the use of ethical principles such as caring, advocacy, justice, autonomy, and beneficence, without necessarily identifying them as such (Solum & Schaffer, 2003). Additionally, the cultural values of the community may influence prioritization, for example, parents may advocate for actions that enhance athletic performance at the expense of health and safety (Kerr et al., 2023).
Self-Efficacy and Intention to Act
Self-efficacy is defined by Bandura (1986) as a belief about one's own capacity to complete a task or goal. Beliefs about one's own future accomplishments influence the level of effort put forward and the likelihood of persisting in the face of difficulty (Bandura, 1986). Boudreaux and Broussard (2020) concluded that school nurses demonstrate high levels of self-efficacy in managing difficult problems, persisting in meeting goals, remaining flexible and responsive, and implementing new programs. In Rosen and colleague's (2016) model, self-efficacy also influences whether a school nurse has an intention to act, for example, whether the nurse intends to provide education about vaccinations for students. In both Boudreaux and Broussard (2020) and Rosen and colleague's (2016) studies, most of the participants had over 10 years of experience as a school nurse. Still, many barriers to action have been documented for school nurses even in the presence of strong beliefs about the importance of an activity, which will be discussed in a separate section.
School health priorities are often determined at a level beyond the individual school nurse and may often shift over time. They may be in direct conflict with one another or compete for attention (Dickson & Brindis, 2021). For example, the nurse may face deadlines for non-urgent assessments, reports, and balance these with more urgent tasks such as medication administration, emergent assessments, and communicating with parents. While nurses may wish to prioritize primary prevention activities, they are constrained by time or prioritization choices of others (Kelly & Lueck, 2011; Kerr et al., 2023; Mammen et al., 2022). This creates a school health environment that is more reactive rather than proactive in preventing illness or injury. Mammen et al. (2022) described a high number of conflicting priorities as being “in crisis mode,” when nurses, school staff, or families have limited resources (p. 2468). In these situations, acute care is typically prioritized over proactive, preventive care (Mammen et al., 2022).
In comparison to other professional disciplines present in the school setting, school nurses are more likely to name evidence-based resources as guiding their decisions to act (Kelly & Lueck, 2011). However, effectiveness in meeting desired health outcomes is not always data-driven (Kelly & Lueck, 2011). School nurses prefer direct observation of students and subjective report over school health data to evaluate mental health interventions (Kelly & Lueck, 2011). Additionally, nurses may sometimes lack the authority to implement evidence-based practices in schools because of the educationally-focused objectives of leadership (Dickson & Brindis, 2021). However, school nurses are perceived by others and identify themselves as important leaders in the school setting (Rosen et al., 2016).
Nursing Process
Finally, the nursing process is clear throughout the existing literature related to prioritization in school nursing. The nursing process in all settings includes five sequential steps that nurses apply to their practice in all settings: assessment, diagnosis, planning, intervention, and evaluation (Ackley et al., 2019). This process can be used for critical thinking, prioritization, and decision-making in the school setting. First, the nurse must assess for the presence of a health problem, need, concern, or client preference. In the context of school nursing, the client can be an individual student, a family, or the school community as a whole population (Selekman et al., 2019). Assessment data particularly relevant to school nursing includes social determinants of health affecting their population, which have been associated with poor health outcomes (Daughtry & Engelke, 2018). In the context of limited resources, assessment steps for the school nurse include assessing environmental concerns, cultural traditions, beliefs, and values (Shendell et al., 2010). The State School Health Infrastructure Measure (SSHIM) is an assessment tool that aids in priority setting; it could be used on both a statewide and local level to map assets, health disparities, and overall unmet health needs (Doremus, 2023). Additionally, periodic reassessment over time is necessary as conditions and priorities change within schools and communities.
Next, a diagnosis is made based on a determination of risk, followed by the planning process. Prioritization is described as a process that happens before an action. Here is where the bulk of prioritizing happens as the nurse weighs the possible outcomes of potential actions. For example, in a study of environmental concerns, nurses in one state ranked respiratory infections, mold, and pollen among the top priorities to address in their schools (Shendell et al., 2010). Subsequently, in the planning phase, long and short-term goals are created. Decisions are made about which actions should be taken first, and which can be delayed, or omitted. Actions are chosen based on available time and resources. School nurses may have a high degree of independent prioritization and decision-making power day-to-day, however, they often face unclear performance standards (Dickson & Brindis, 2021).
In the school setting, intervention often requires collaboration with diverse sets of stakeholders, including students and parents, district personnel, and legislators (Harriger, 2011; Savage, 2017). Collaboration was found to be particularly necessary to implement priority actions because policy alone does not always result in action (Dominguez Jaurigue, 2016; Harriger, 2011). For example, merely having a school wellness policy may not improve health outcomes (Harriger, 2011). Effective collaboration in meeting the basic needs of students may increase the availability of the school nurse to prioritize more complex tasks appropriate to a nursing level of care, and delegate other tasks to unlicensed assistive personnel (Lineberry, 2016). Furthermore, nursing intervention in the school setting may require resourcefulness when faced with novel situations (Boudreaux & Broussard, 2020) and creativity, especially in low-resourced environments (Dickson & Brindis, 2021).
The final step of the nursing process is evaluation. The nurse evaluates the process by measuring or observing the outcomes including, ideally, the magnitude of the impact. Evaluation may require a great deal of communication and collaboration with school administration and other stakeholders, and can be challenging (Harriger, 2011). Furthermore, the nurse may evaluate whether they have fulfilled their professional duty with fidelity and whether poor outcomes have been prevented (Savage, 2017). School nurses may lack the authority or resources to sufficiently evaluate outcomes and monitor quality on a large scale (Dickson & Brindis, 2021). Daughtry and Engelke (2018) described a pilot study including a school health evaluation plan, which had limited, but promising success. A logic model was developed in a large school district to prioritize key student outcomes and effectively advocate for more school nurse positions. The evaluation plan included a logic model documenting goals, activities, outputs, outcomes, and impact. Ultimately, evaluation will reveal whether the correct goal and action were chosen and cycle back to the beginning of the nursing process: assessment.
Summary of Facilitators and Barriers to Prioritization
School nurses are impacted by both facilitators of and barriers to effective prioritization. Facilitators related to school nurse knowledge, values and attitudes include strong knowledge of laws, policies, professional and evidence-based standards, and health information (Dickson & Brindis, 2021). Continuing education concerning clinical judgment, team building, and empowerment strategies to improve student health outcomes also served as facilitators (Jordan et al., 2022). Professional identity as a leader in the school setting (Rosen et al., 2016) may also facilitate effective prioritization and decision-making. Additionally, the experience of moral distress can also be a facilitator of ethical decision-making among school nurses (Savage, 2017) who describe ethical principles they use to make decisions (Solum & Schaffer, 2003). However, lack of resources (time, staffing, and financial means) can change prioritization and influence actions more than the nurse's knowledge, values, and attitudes (Boudreaux & Broussard, 2020; Dickson & Brindis, 2021; Jordan et al., 2022; Lineberry, 2016; Mammen et al., 2022).
Self-efficacy and intention to act facilitates prioritization when the school nurse has resources and/or is resourceful (Boudreaux & Broussard, 2020). Further facilitators include creativity, organizational and community support (Dickson & Brindis, 2021), and effective collaboration (Alexander-Ruff & Hodgson, 2022; Harriger, 2011; Lineberry, 2016). High levels of self-efficacy (Boudreaux & Broussard, 2020), support, connection, and awareness of opportunities for improvement were also identified as facilitators (Jordan et al., 2022). Conversely, lack of personal control or perceived lack of control was a barrier to prioritization (Dickson & Brindis, 2021). Further barriers included lack of school nurse authority to implement desired interventions and shifting priorities from other stakeholders (Dickson & Brindis, 2021; Kelly & Lueck, 2011; Kerr et al., 2023; Mammen et al., 2022).
Finally, the nursing process also encompasses facilitators and barriers to prioritization among school nurses. Autonomy to conduct the full scope of the nursing process (Dickson & Brindis, 2021) and assessment tools such as SSHIM can facilitate prioritization (Doremus, 2023). An additional facilitator of prioritization includes effective interdisciplinary collaboration throughout the nursing process (Lineberry, 2016). However, despite evidence-based practice being highly valued, prioritization as part of the nursing process in schools can be facilitated or hindered by access to assessment and evaluation data for their population (Daughtry & Engelke, 2018; Dickson & Brindis, 2021; Kelly & Lueck, 2011; Shendell et al., 2010).
Discussion
Schools are key settings for improving the health of the U.S. population throughout the lifespan (Bergren, 2017b). This integrative review has synthesized evidence related to prioritization among school nurses in the U.S. The findings can inform and create movement toward practice improvement and supportive public policies for school nurses.
Knowledge, attitudes, and values of school nurses influence school nurse prioritization and can be used to guide practice improvements. Knowledge of school policies, evidence-based practice, and professional standards can facilitate prioritization. Generally, school nurses value evidence-based practice highly. Similarly, they value ethical principles and regularly apply them, but may not explicitly know that their choices are based on formal ethical models. Self-efficacy was particularly relevant to prioritization among school nurses with over 10 years of experience as a school nurse, while resource constraints can exert pressure on school nurses to be more reactive than proactive in health protection and improvement. Inconsistent access to population-level health data for assessment and evaluation hinders school nurses’ ability to implement the full scope of the nursing process with a high level of fidelity.
Knowledge of the “best interest standard” may complement the Code of Ethics for school nurses (NASN, 2024) to enhance school nursing practice (Grunin & Malone, 2022). This model encompasses holistic assessment of student/family needs and incorporation of the ethical principles of autonomy, beneficence, nonmaleficence, and justice. It could be incorporated into school health practice more explicitly, rather than relying on school nurses’ implicit application of ethics.
Despite valuing both ethical and evidence-based practice, major barriers to implementing them may include institutional policies, systems, and culture. This suggests that it is imperative for school nurses to be leaders in their organizations and beyond, such as at the state and national levels. A recent survey found that 36.9% of school nurses were not involved in the planning process for reopening schools following closures during the peak of the COVID-19 pandemic (Gormley et al., 2023). This demonstrates that school nurses may not always be invited to the decision-making table, even in the face of a clear health threat. This further suggests an opportunity for school nurses to step into formal and informal positions of leadership to shape school health policies that can best enable them to carry out ethical and evidence-based decisions. For example, school nurses can lead or be key participants in school health advisory or action councils or committees. These councils may conduct formal needs assessments, prioritize school health needs, plan, implement, and evaluate interventions (Hunt et al., 2015). Future research should explore barriers to school nurse participation in these committees.
The second theme, self-efficacy and intention to act, is consistent with and builds upon earlier findings relating to decision-making and prioritization among school nurses. System-level barriers and poor support for potential health initiatives may contribute to low self-efficacy among school nurses. Consequently, low self-efficacy may lead to poor health outcomes for the school population, as discussed in Wagner and colleagues’ (2019). Both planning and evaluation activities must be developed in a way that is specific to the population and community with which the school nurse is engaging (Wagner et al., 2019). However, large scale planning activities may be difficult for school nurses because of systemic barriers, namely lack of time and resources for such activities. While self-efficacy could be an antecedent to effective prioritization, it is possible that self-efficacy is a consequence of effective prioritization over time, rather than a pre-existing facilitator. More research is recommended to study whether self-efficacy among school nurses can be increased and whether this thereby enhances effective prioritization processes and improves student outcomes.
Additionally, self-efficacy and intention to act relate to Endsley's (2017) scoping review of safety and workload among nurses, which defines “missed nursing care” as care left undone. Missed care is often the result of a high workload paired with scarcity of time (Endsley, 2017). While missed care can lead to moral distress (Jones et al., 2015), moral distress may be a motivator for ethical decision-making (Savage, 2017). School nurses often report a lack of time and resources, which places them at risk for missed care, or ineffective prioritization. In acute care settings, missed care is considered a nursing error and can have dire consequences for both client health and the career trajectory of the nurse (Jones et al., 2015). It remains unknown how school nurses make decisions about what care remains undone, if missed care is typically intentional or accidental, and how missed care in the school setting affects health outcomes for school populations. Actions left undone must be acceptable to all school constituents including the nurse, educators, administrators, students, and parents.
The findings of this literature review are consistent with Breitenstein and colleagues’ (2012) discussion of the challenges faced by school nurses in balancing adaptability with fidelity to evidence-based practice. Due to the competing pressures placed upon school nurses, effective prioritization is essential to protect against loss of quality. An effective prioritization framework would provide guidance in choosing the activities that maximize positive outcomes. Little is known about how systems can be improved to facilitate the use of outcomes data among school nurses to evaluate interventions and effectively prioritize in a low-resource environment.
The NASN (2020) Prioritizing School Nursing Practice Activities tool was developed during the COVID-19 pandemic to assist school nurses in prioritizing their activities during this time of significantly increased workload, and will be maintained for ongoing management of school nurse practice for potential application during times of significant resource strain (K. Stanislo, personal communication, September 22, 2022). In this tool, activities prioritized as urgent result in “serious adverse consequences” or would immediately impact health and well-being if not completed. This relates to the theme of self-efficacy present in the findings of this review and the concept of missed nursing care. The extent to which school nurses can successfully predict interventions that will influence students’ immediate needs of health and well-being, as well as avoid serious adverse events is unknown. Furthermore, it is unknown to what extent these predictions result in an intention to act and/or result in actual intervention.
An additional consideration of the NASN tool (2020) is whether an activity will prevent illness; activities are an urgent priority if they would have a large impact on the population, but high priority (lower than urgent) if they would have a small impact. While this is consistent with the public health nursing principle of seeking to achieve the greatest good for the greatest number of people (American Nurses Association, 2013), the concept of prioritizing activities which produce larger magnitudes of results was not explicitly discussed in other sources included in this literature review. It is unknown how school nurses might determine the magnitude of impact for potential interventions, nor whether the greatest good is a value among school nurses when prioritizing actions.
For activities remaining uncategorized from the first questions in the tool, the nurse should consider whether the activity addresses “students at risk for concerns that will impact their health and academic performance.” These activities are a high priority if no one else in the community is addressing the health need. However, if other community partners are already doing the activity, it would be categorized as a medium priority. The phenomenon of how school nurses assess whether health needs are being met by the community did not emerge in this literature review.
The last inquiry to be made, according to the NASN (2020) tool, is whether interventions are mandated by state law or funding is tied to activity completion. If an activity has not been prioritized by previous assessment questions, the only available actions are to discontinue or delay the activity. If mandated interventions are evidenced-based, the tool's recommendation is that the activity can reasonably be postponed “due to circumstances.” Activities that are mandated, but not evidence-based, may be delayed and advocacy is recommended to change the regulatory policy. These circumstances included the COVID-19 pandemic which has strained school health personnel and finances, although the logic could be extrapolated to include any circumstance in which resources are limited (K. Stanislo, personal communication, September 22, 2022).
Limitations
This integrative review has some limitations. First, the scope was limited to research conducted in the U.S. International studies may inform the understanding of how school nurses can effectively prioritize and make decisions; however, it was important to limit this review to the U.S. because of major differences in educational and health care structures globally. Furthermore, this review was limited to studies published in the 15 years prior to the first literature search in 2022 and may have overlooked older studies. The results allowed for inclusion of relevant, older primary sources, which may have mitigated this limitation. Additionally, while two researchers collaborated to review the full text of selected sources, they were not subject to independent confirmation of the findings. Selection bias was minimized by including edge cases unless clear evidence arose from full-text review that the study did not meet inclusion criteria. Interpretive bias was also addressed by reporting the author’s original words in the literature review matrix when possible, to represent study purposes and findings. Finally, this study was limited by a lack of Level I research on this topic, with only one Level II study available meeting inclusion criteria. This further supports the assertion that additional research is necessary on the topic of prioritization among school nurses.
Conclusion
Unique demands are placed upon school nurses compared to nurses in other settings. Additionally, school nurses in different contexts may face different demands depending on their level of resources and setting characteristics. Understanding prioritization among school nurses is a precursor to enhancing evidence-based practice. Prioritization is a context-specific skill that can be learned and taught and must be applied to maximize benefits to clients and minimize adverse outcomes. Prioritization models or frameworks have been developed for nurses to apply to specific health conditions; however, these frameworks have not been evaluated in terms of usage, acceptability, and efficacy. There may also be low awareness of available frameworks, such as the NASN Prioritizing School Nursing Practice Activities tool (2020) for school nurses practicing in low-resource settings. Greater awareness of these tools can assist nurses in articulating priority activities to school leadership.
Barriers to effective prioritization, such as non-evidence-based regulatory policies and lack of time or resources, may hinder the school nurse's ability to prioritize according to their values or to fulfill their professional responsibility. Future research on the application of innovative prioritization frameworks is necessary to understand and support school nurse praxis and outcomes measurement. School nurses must apply ethical principles, predict which actions are likely to lead to which outcomes, and then weigh the costs and benefits of their practice decisions to effectively prioritize and achieve desired outcomes. It is imperative for future research to deepen our understanding of how school nurses prioritize and identify opportunities to strengthen prioritization in this setting so that school nurses can optimize the use of limited resources.
Footnotes
Author Contribution(s)
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
