Abstract
In low-resource settings, adults with unrepaired cleft palate often have limited access to surgery. Palatal obturators have been proposed as an alternative to surgery in older patients. This study explored the experiences of 5 adults fitted with obturators while awaiting primary palatoplasty in Paraguay. Despite initial discomfort, patients reported improved eating, speech, and self-esteem. Ultimately, however, all chose surgery, viewing it as a more permanent solution for speech issues. These findings highlight that while obturators offer benefits, patients prioritize surgery for long-term outcomes. This study points to the need for further research to identify strategies to optimize patient acceptance and outcomes of obturator use before they can be considered a feasible alternative to surgery for adults in low-resource settings.
Background
The global burden of orofacial clefting is estimated at 529,759 disability-adjusted life years with an estimated global prevalence of 4.6 million. 1 Most of these patients reside in low- and middle-income countries (LMICs) where access to cleft care is limited. To this end, many patients around the world do not receive primary surgical treatment in the first years of life when it is most likely to be of benefit in terms of speech development. 2 In many LMICs, adults with an unrepaired cleft palate represent between 13% and 32% of all patients.3,4 In centers with limited resources, younger children are invariably prioritized for surgery, as primary palatoplasty in older patients carries greater morbidity with less consistent outcomes. To this end, adults with unrepaired cleft palates, if they are offered a palatoplasty at all, face lengthy waits for surgery. While wait times for adults with unrepaired cleft palate have not been reported in the literature, given that children may wait as much as 9 months for primary palatoplasty in many LMICs, it is anticipated that adults can face waits of several years. 5
In light of this burden of disease, cleft care teams in low-resource areas have considered the use of palatal appliances either as a direct treatment or to serve as a temporizing therapy until surgery in adult patients with unrepaired cleft palate. 6 While obturators and other appliances are described as an alternative to surgical correction, little has been published on their use in patients with unrepaired cleft palate and it is unclear what patients’ perceptions of them are. Understanding patients’ attitudes to palatal appliances could help to identify barriers to their wider application. To explore this topic on which little is known, we undertook a qualitative study of adult patients with unrepaired cleft palate who used a palatal appliance while awaiting primary palatoplasty at a cleft center in Asuncion, Paraguay.
Methods
Design
This exploratory qualitative study aimed to understand the experiences of adult patients with an unrepaired cleft palate who trialed a palatal appliance prior to primary palatoplasty. Qualitative research allows a deeper exploration of how individuals process their experiences across social domains. 7
Participants
Participants were recruited through Operation Smile Paraguay between March 2021 and September 2024. Operation Smile Paraguay is a non-governmental organization that has operated a comprehensive cleft care center in Asuncion since 2005. The center offers surgery, nutrition and psychosocial support, speech language therapy, and dental and orthodontic care to patients from across the country.
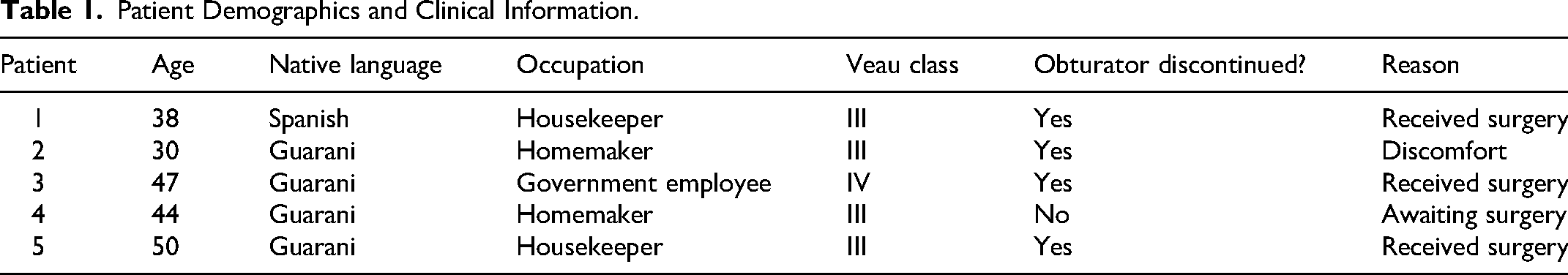
Patients were eligible to participate if they were over the age of 18 and had an unrepaired Veau II-IV cleft palate. Patients with a syndromic diagnosis or condition that could compromise speech beyond the presence of a cleft palate (severe cognitive impairment, mutism, deafness), who were edentulous, or had another major health condition were excluded. As qualitative research does not a priori aim for epidemiological representativeness and given the relatively low incidence of adult unrepaired cleft palate patients at the center, a pragmatic recruitment strategy was adopted. 8 Based on a grounded theory approach, if thematic saturation had not been achieved, additional patients would be recruited. Table 1 summarizes some socio-demographic features, ages and types of cleft of participants.
Patient Demographics and Clinical Information.
Patients underwent an initial assessment by all members of the team, including a plastic surgeon, speech language therapist, audiologist, orthodontist, dentist, and nutritionist. Eligible patients that agreed to participate in the study were fitted with an acrylic palatal appliance which included a short palatal lift extension to elevate and partially obturate the soft palate by the team orthodontist. No speech bulb extension was used. Patients were subsequently followed weekly for the first month post-appliance fitting by the team orthodontist to assess for any points of wear that needed to be relieved or any other adjustments. During visits, patients were also seen by the speech language therapist to discuss strategies to reduce gag reflex and improve adherence to the appliance.
Interviews and Analysis
While the authors’ a priori aim was to conduct a reflexive thematic analysis to explore patients’ experience with obturators, 9 this was not feasible as participants were unable to commit to the lengthy interview times required. Instead, semi-structured interviews regarding the patients’ experience with the obturator were completed by one of the authors over the telephone using an interview guide (Supplemental Data File) developed by the senior authors. Subsequent data collection, analysis and reporting were informed by conventional content analysis. 10 Participants were offered a telephone interview after each clinical assessment, and all participated in a final interview at the end of the study period. To this end, participants had the opportunity to meet with the interviewer on multiple brief occasions, picking up on discussions from earlier visits. The mean individual interview time was 5 min. Each interview ended when the participant had no further comments to make. Visits were continued up to 6 months or until the patient underwent primary palatoplasty. All patients were offered the opportunity to continue with the obturator in lieu of surgical correction.
The interviews were immediately transcribed from Spanish or translated from Guarani (a national language of Paraguay) into Spanish. Each interview was coded to maintain anonymity and confidentiality. After transcription, themes and sub-themes were identified by 2 authors fluent in Spanish and English. Each interview transcript was read several times by these authors to ensure their familiarity with the raw data. Relevant quotes were then translated into English.
Ethics
The study was approved by the University of Southern California Institutional Review Board in the United States, in conjunction with local research approval (Operation Smile Paraguay). Participants’ confidentiality was protected by providing a unique identifier number, no sharing details of their places of living, and encryption of transcripts.
Results
Two major themes were identified—experience using an obturator, and reasons for discontinuing obturator use. Subthemes under the former theme included comfort, speech and eating, and self-esteem. Subthemes under reasons for discontinuing obturator use included speech concerns, inconvenience, and permanence.
Experience Using Obturators
Comfort. Early on following introduction of the obturator, most patients described discomfort which improved with refinements by the orthodontist and ongoing desensitization.
At first the obturator bothered me; it made me feel bad. But I knew I had to get used to it. The first few days it was very difficult to use—I couldn't eat or drink anything with the obturator. Afterwards I got used to it wonderfully. (P1)
Three participants reported initial discomfort and difficulties using the obturator, and 2 reported minimal discomfort. By 6 months, only 1 participant expressed ongoing discomfort, albeit improved, with the use of the obturator. Self-reported adherence to regular wearing of the obturator improved over the study period.
Speech and eating. Most patients reported early and persistent improvements in eating, which they felt helped their daily quality-of-life as the frequency with which food became lodged in their cleft was greatly reduced.
It was great to use the obturator. I could eat without any problem, could suck, and the food didn't get stuck in the [palate opening]. (P2)
Psychological impact and self-esteem. Participants who described significant improvements in eating and more modest gains in speech reported an improved sense of well-being.
It was easier for people to understand me and it made me feel very good about myself. (P3)
Even patients who had discomfort with the obturator described an improvement in their self-esteem as they viewed the experience as preparation for the next step in their treatment, most notably their palatoplasty.
Reasons for Discontinuing Obturator
Speech concerns. Despite reporting that the obturator improved their speech, all patients opted to discontinue its use and receive surgery instead in the hope that palatoplasty would lead to greater improvements in their intelligibility. All patients stated that while the obturator was effective it didn’t fully solve their communication challenges.
I continue using the obturator - my eating and speech improved a lot. I would still like to have surgery for many reasons, for example to speak better. (P4)
I wanted to have surgery so I could speak well. (P5)
Inconvenience. A sixth patient eligible to participate in the study did not return to the center after the impression was taken for their obturator as they found the need for the frequent adjustments at the center inconvenient. Additionally, even those participants who continued using the obturator frequently missed scheduled appointments, often due to challenges taking time off work.
Permanence and completion of care. While no patients required a replacement obturator owing to loss or damage over the 6 months, this was a concern raised by the participants to members of the team. Surgery was viewed as a necessity rather than a choice, reflecting their desire for a permanent solution to both functional and psychosocial challenges. One patient shared that after all the dental work she had undergone, she was eager to have surgery to “speak better and be understood.” Patients expressed that by pursuing palatoplasty they were completing their cleft care.
I am already grown up and that's all [surgery] I need to finish my treatment. After all I’ve done in dentistry and others, I only need my surgery. I want to be able to speak better and be understood. (P2)
Discussion
Despite being described as an option for non-operative management of cleft palate, particularly secondary deformities such as large fistulas, the published literature on the use of obturators and palatal appliances in patients with an unrepaired cleft palate is limited. A few case reports have been described for adult patients with cleft in LMICs, reporting positive results in speech, feeding, and aesthetics.11–13 In a case report from India, a 25-year-old man reported improved aesthetics, swallowing, and speech intelligibility using a cast partial hollow-bulb obturator. 11 Two additional reports from Brazil reported similar benefits of a palatal appliance.12,13 A 48-year-old woman reported satisfaction due to improved masticatory efficiency, phonetics, social activity, and quality of life using an obturator and mandibular prosthesis. 12 In another report, a 41-year-old man described improved comfort, speech, mastication, esthetics, and quality of life using an implant-supported fixed denture and obturator. 13
Although all patients in the current study noted improvements in speech and eating during their experience with obturators, they ultimately chose to undergo surgery to further enhance their speech. The desire for improved speech as a primary reason for pursuing surgery highlights the importance of speech in both psychosocial well-being and societal integration. This was clearly reflected in one patient who, while using the obturator, expressed that it bothered her but recognized it was beneficial, as her speech had been difficult to understand. Her self-esteem was closely linked to whether others could understand her speech. The current study shed light on patient misconceptions regarding the relative contributions of speech therapy, obturator use, and surgery to improving longstanding speech dysfunction. Several participants thought the palatoplasty would provide an immediate correction of their speech; additional counselling was required to explain that intensive speech therapy would be required to correct active speech errors not only with the obturator, but after surgery as well. Others have demonstrated that speech language therapy should be undertaken while using an obturator to improve speech, rather than utilizing an obturator alone or implementing speech therapy after obturator use. 14 In the current study, surgery was viewed as more likely to definitively address speech difficulties. While surgery can provide a permanent solution, it alone does not address longstanding compensatory misarticulations. Additionally, if complications arise, surgery may even further compromise speech.15–17 Limited ability to access speech therapy due to a lack of trained speech language pathologists or other socioeconomic factors (cost, time from work), further compound the ability of patients in LMICs to achieve optimal speech outcomes. Even if improvements are made with therapy, speech impairments are more difficult to correct completely for adult patients with cleft.15,18
This study is not without its limitations. Firstly, the sample size for this study was small and the experiences of patients in the current report may not be generalizable to other patients at the same center or other LMICs and should be interpreted within the specific context of its setting in Paraguay. Specifically, it is unclear how patients who self-selected to try the obturator differed from those who opted not to participate in the study and therefore were not offered an obturator. Secondly, patient numbers were limited and included only women, most of whom worked within the home. Thirdly, the appliance used for all patients did not use a speech bulb or extended palatal lift; while we speculate that this might have improved patients’ tolerance of the device, it is also possible that it led to less improvement in speech outcomes as reported by patients and hence greater interest in pursuing surgery. It is unclear whether the use of a speech bulb would have resulted in greater speech improvements and made patients more receptive to continuing with the palatal appliance. Additionally, we were unable to corroborate patients’ subjective reports of improved speech with objective pre- and post-intervention measures as nasometry was not consistently performed. Finally, all participants in the study were candidates for and interested in undergoing palatoplasty, and it is unclear whether patients with significant comorbidities for whom surgery was contraindicated would have been more willing to continue with the obturator.
The current study has paved the way for several new areas of investigation within our group, namely the application of technology used to fabricate dental aligners to rapidly produce 3-dimensionally printed obturators which can be incrementally adjusted without the need for regular patient visits. Such designs could allow for the inclusion of speech bulbs and lead to improved speech outcomes and long-term use by select patients.
Conclusions
While uncommonly seen in high-income countries and underrepresented in the literature, speaking or adult patients with unrepaired cleft palate represent a significant population presenting to LMIC cleft centers. In settings where access to surgery is constrained, obturators have been suggested as one modality to address the unmet needs of adults with cleft conditions globally. The study explored the experiences of adults with unrepaired cleft palate with obturators in their own words. Based on this exploratory study, patients’ perception that surgery would be more effective than an obturator in improving their speech was a major barrier to adherence, and points to a need to focus on appliances that optimize speech outcomes while minimizing patient discomfort.
Supplemental Material
sj-docx-1-cpc-10.1177_10556656251390716 - Supplemental material for Experiences of Obturator Use in Adults With Unrepaired Cleft Palate: A Qualitative Study
Supplemental material, sj-docx-1-cpc-10.1177_10556656251390716 for Experiences of Obturator Use in Adults With Unrepaired Cleft Palate: A Qualitative Study by Barbara Salazar, Jonathan Diaz, Magaly Benitez, Paulina Ocampo, Julio Recalde, Miguel Fariña, Belen Aguilar, Silvia Velasquez, Allyn Auslander and Michael Bezuhly in The Cleft Palate Craniofacial Journal
Footnotes
Ethical Considerations
This study was approved by the University of Southern California Institutional Review Board, in conjunction with local research approval (Operation Smile Paraguay). Participants’ confidentiality was protected by providing a unique identifier number, no sharing details of their places of living, and encryption of transcripts.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Operation Smile Canada.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
