Abstract
Objective
This study evaluates the impact of travel distance and surgical timing on outcomes in patients undergoing palate surgery.
Design
A retrospective cohort study analyzing patient data from electronic medical records. Univariate and Kruskal-Wallis analyses assessed associations between distance, timing, and outcomes.
Setting
A single academic, American Cleft Palate Craniofacial Association -approved tertiary craniofacial center in North Carolina.
Patients, Participants
One hundred and ninety-eight patients who underwent palate surgery from 2016 to 2023. Exclusion criteria included age >12 years, submucosal clefts, out-of-state residence, and lack of follow up.
Interventions
Palate surgery categorized as early (<11 months), standard (11-13 months), or late (>13 months).
Main Outcome Measure(s)
Age at first craniofacial visit, age at surgery, time between visit and surgery, emergency department (ED) visits within 30 days of surgery, and incidence of velopharyngeal insufficiency (VPI) or speech therapy referral by age 3.
Results
Median age at palate surgery was 10.1 months. Increased distance was significantly associated with increased age at clinic presentation (P = .042) and surgery (P = .041), but not increased time between first visit and surgery (P = .811). Earlier surgery was associated with reduced ED visits (P = .0159) and speech therapy referrals (P = .0255). VPI incidence was 11.4%, with no significant correlation to timing or distance.
Conclusions
Increased travel distance is associated with later primary palate surgery. Addressing geographic disparities is crucial to improving patient outcomes.
Introduction
Cleft palate is among the most common birth defects in the United States, with an estimated 1 in 1687 children affected at birth. 1 The gold standard for treatment of pediatric patients born with cleft palate is surgery to repair the cleft palate before the age of 2 and longitudinal care, with care from an American Cleft Palate Craniofacial Association (ACPA) approved multidisciplinary team. 2 Previous studies results have demonstrated that care at an ACPA-approved craniofacial clinic results in higher adherence to care guidelines. 3 However, ACPA clinics are not uniformly distributed across the United States. As a result, many patients seek community-based care or travel great distances for care at an ACPA-approved craniofacial clinic.3,4
Palatoplasty has been widely accepted as the standard of care for patients with cleft palate since the eighteenth century and is a cornerstone of craniofacial care. 5 Despite widespread adoption of the procedure, the proper timing of surgery and its potential impact on both speech and midface growth is the subject of much debate.6,7 The ACPA currently recommends patients undergo palate surgery at 9 to 14 months, with a large body of research supporting this recommendation.2,8,9 Within these relatively broad surgical timing recommendations, literature examples of what constitutes “early,” “standard,” or “late” palate repair surgery are limited. Shaffer et al classified “early” palatoplasty as occurring before 11 months of age, “standard” palatoplasty as between 11 and 13 months, and “late” palatoplasty as being at age greater than 13 months. 10 However, other literature examples of such classification recommendations are limited, and the question of proper palate repair surgery timing is rapidly evolving. Recently, a large-scale randomized control trial of 558 patients concluded that palatoplasty at age 6 months resulted in better outcomes for patients, adding further confusion to the discussion of ideal timing for primary palate surgery. 11
According to the National Academies of Sciences, Engineering and Medicine, access to care is defined as “timely use of personal health services to achieve the best possible health outcomes.” 12 Studies have concluded that greater distance from health care services is associated with worse clinical outcomes. 13 The impact of distance traveled for care is particularly relevant for patients born with cleft palate, as up to 48% of patients drive >1 h for craniofacial care. 4 These trends are theorized to be a result of unequal distribution of ACPA clinics across the United States, with the Southeast being the most poorly served of all geographic regions. 14
The importance of timely surgery for patients born with cleft palate, coupled with the existing evidence that access to craniofacial care in the Southeastern United States is limited, were the primary drivers for the development of this study. We aimed to determine the association between distance traveled for care at our ACPA-approved craniofacial clinic, the age at which patients with cleft palate present for care and undergo palate repair surgery, and various clinical measures of patient outcomes. In addition, we sought to develop a robust geographic model to elucidate the state level distribution of patients seeking care at ACPA-approved craniofacial clinics in North Carolina to better understand state level trends in craniofacial care.
Methods
Patient Selection and Data Extraction
This study was an IRB-approved (IRB Number: 24-1831) retrospective cohort analysis conducted at a single academic research center. Patients who received repair surgery for cleft of the hard or soft palate from January 1, 2016 to December 31, 2023, and follow-up care from the study-craniofacial clinic were included. Palate surgeries were performed by 4 surgeons (2 otolaryngologists, 1 plastic surgeon, and 1 oral-maxillofacial surgeon) with surgical practices typical for the institution. Patient data were extracted from the electronic medical record (EMR) by searching the EMR for individuals who underwent palate repair surgery (CPT: 42200). Demographic data, zip codes, surgery details, no-show rates, and follow-up information were extracted for those who met inclusion criteria.
Inclusion and Exclusion Criteria
Patients included in the study were 0 to 12 years old at the time of data extraction and received palate repair surgery and follow-up care during the aforementioned time at the study-craniofacial clinic. Criteria for exclusion included the following: age >12 years old at time of data extraction, cleft of the submucosa only, zip code location outside of the state of North Carolina, and absence of follow up with the study-craniofacial clinic.
Demographic Analysis and Surgical Timing Categorization
Basic demographic data (age, sex, race, and language) were analyzed using Microsoft Excel. Distance data was also preliminarily analyzed in Microsoft Excel to determine general distance trends (median distance traveled, minimum, and maximum distance) ahead of more thorough analysis via Stata and Geographic Information Systems (GIS) mapping software.
Age at first study-craniofacial clinic visit, age at palate repair surgery, and time elapsed between first clinic visit and surgery were determined by comparing study-craniofacial clinic and surgery notes with each patient's date of birth (DOB) according to the EMR.
Patients were categorized as receiving “early,” “standard,” or “late” palate repair surgery, through utilization of timing categories previously outlined by Shaffer et al. 10
Distance Traveled for Care and Timing of Care
Univariate analysis was conducted via Stata to determine the relationship between distance traveled for care at the study-craniofacial clinic, age at palate repair surgery and the following variables: (1) age at first visit to the study-craniofacial clinic, (2) age at palate repair surgery, and (3) time between first craniofacial clinic visit and palate surgery.
Coefficient estimates, P-values, and confidence intervals were calculated to evaluate associations between variables, while R² values quantified the proportion of variance explained by the relationship. Statistical significance was defined as P < .05. Following preliminary analysis which showed a wide distribution of timing data, histograms were created via Stata and edited with the help of ChatGPT to improve appearance.
The Kruskal-Wallis equality-of-populations rank test, a nonparametric method to determine whether a statistically significant difference exists between the medians of 2 or more independent groups, was performed to determine the relationship between (1) distance and (2) timing of palate repair surgery with several clinical measures of interest. This test was selected following preliminary analysis which demonstrated that values for both distance and timing of palate repair surgery were not normally distributed.
Investigation of the Relationship Between Distance, Surgical Timing and Clinical Measures
For patients aged 3 or older at the time of data collection, study-craniofacial notes were reviewed to determine presence or absence of velopharyngeal insufficiency (VPI). Patient referral to speech therapy (ST) was determined through review of study-craniofacial clinic notes at or around 2 years of age, as speech evaluation at age 2 was standard practice for the study-craniofacial center. The presence or absence of an emergency department (ED) visit for a reason related to surgery, including bleeding, infection, pain control, or wound dehiscence, in the 30 days postsurgery was also recorded.
The following categorical variables were included in analysis:
ED visit (ED): whether a patient visited the emergency department within 30 days of surgery with complaints related to surgery. Of note, patients with ED visits unrelated to surgery were coded as 0 (categorical: 0 = no, 1 = yes). FU (follow up): whether a patient had a follow-up visit within 30-days of surgery (categorical: 0 = no, 1 = yes). PND (prenatal diagnosis of cleft palate): whether the patient received a diagnosis of cleft palate prenatally (categorical: 0 = no, 1 = yes). ST (speech therapy): whether the patient received a referral to ST at 2-year clinic visit (categorical: 0 = no referral, 1 = referral). VPI: whether a patient received a diagnosis of VPI by 3 years of age (categorical: 0 = no, 1 = yes).
The test statistic and P-values were computed for each comparison. A P-value < .05 was considered statistically significant. The results of the Kruskal-Wallis test were visualized using bar plots of the P-values for clarity and to highlight significant findings. Results were input into ChatGPT to generate a visual representation of the data.
Geographic Information System Map Generation
All mapping and analysis were performed in ArcGIS 3.0 desktop GIS software. Geocoding, or the process of using precise address information, such a street addresses or zip code, was used to create point features that were mapped and analyzed within the system. First, patient zip codes and the zip code of the study-craniofacial were geocoded using the Esri World Geocoding Service. Following initial analysis which revealed unexpected state-level distribution trends, the location of the 3 other in-state craniofacial centers were added to subsequent analysis.
After geocoding, Network Analyst Toolset was used to create service areas around both the study-craniofacial clinic and the 3 other craniofacial clinics. Service areas, or geographic spaces able to be accessed by driving a specified time or distance, were mapped for both the study-craniofacial clinic and the other in-state clinics. For the data set, 20, 40, 60, and 120 min. service areas were created. The 20, 40, 60, and 120 min. intervals were chosen specifically, as these time intervals reflect meaningful thresholds of increasing travel burden commonly used in geographic access literature, and because the time intervals aligned with natural break points in the dataset. For reference, the greatest possible distance a patient could travel from the study-craniofacial clinic while maintaining in-state residence was ∼350 miles.
The Origin-Distance Cost Matrix tool within the Network Analysis Toolset was used to determine the driving time and driving distance between each study participant, the study-craniofacial clinic, and each other craniofacial clinic within North Carolina. For our solution, the algorithm was set to optimize by travel time. For example, for participant A to get to medical facility 1, it might take 30 min, and require driving 24 miles. For each participant, each in-state craniofacial clinic was ranked 1 through 4 based on whether it was the first, second, third, or fourth closest facility to their residence.
Patient density was displayed using the Heat Map symbology style, which draws point features that depict the density of features dynamically. The Heat Map symbology style was chosen secondary to its ability to effectively display densely concentrated data points located in close geographic proximity. Areas with high patient density are indicated by lighter colors, while areas with fewer features are represented with darker colors.
Results
Demographic Data
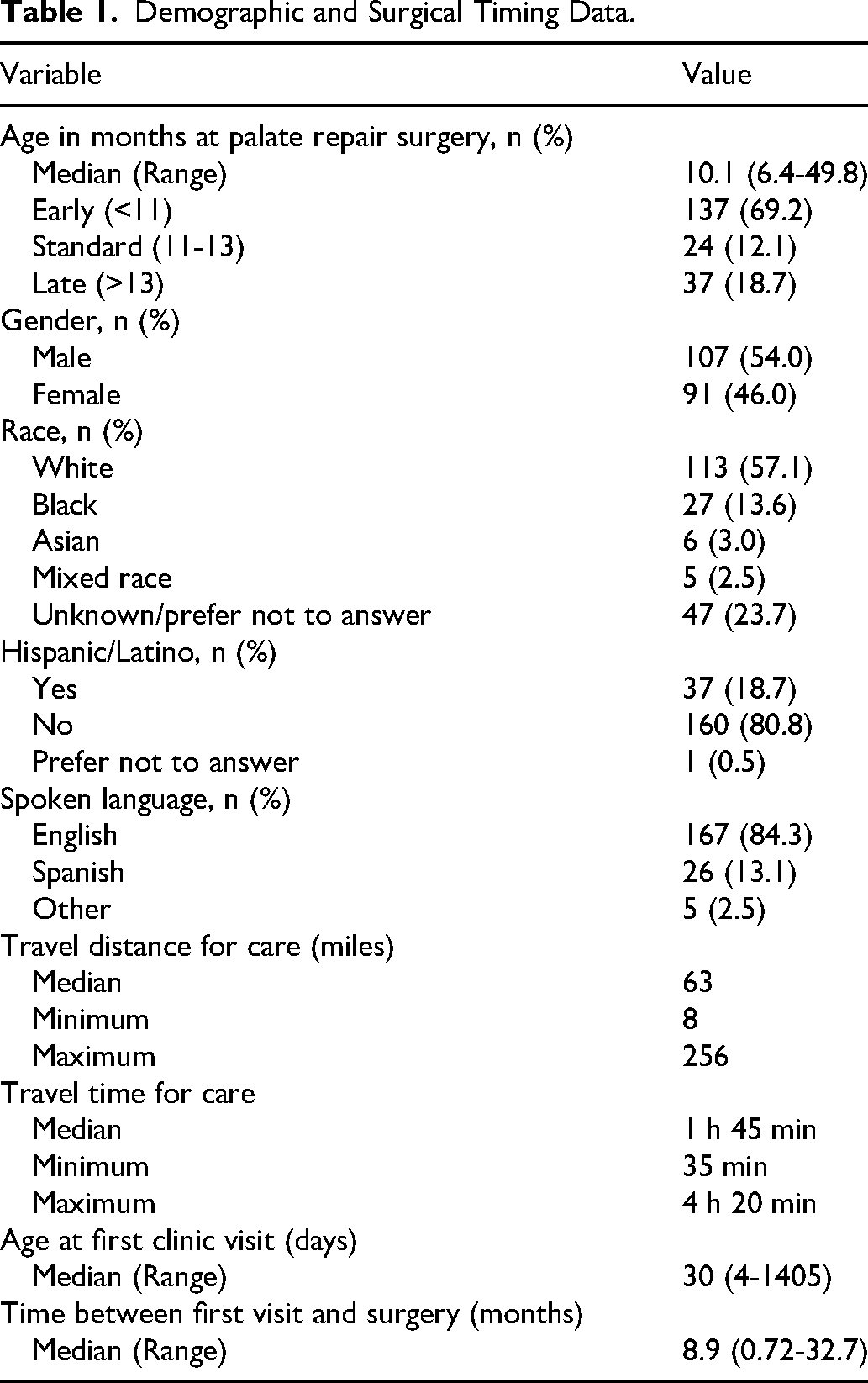
In total, 198 patients who received palate repair surgery by a surgeon at the study-craniofacial clinic between January 1, 2016 and December 31, 2023 met inclusion criteria and were included in the study. The cohort of 198 patients showed a slight male predominance with 107 male patients (54%), and 91 (46%) female patients. Most patients were white (57.1%) and did not identify as Hispanic or Latino (80.8%). Most patients spoke English as their primary language (84.3%), though a notable 13.1% of patients spoke Spanish as their primary language. Full demographic data is displayed in Table 1.
Demographic and Surgical Timing Data.
Institutional Trends for Timing of Repair Surgery for Cleft Palate
The median age of patients at the time of first visit to the study-craniofacial clinic was 30 days (range: 4-1405) (Table 1). The median duration of time between first visit to the craniofacial clinic and palate repair surgery was 8.9 months (range: 0.72-32.7). The median age at time of palate repair surgery was 10.1 months (range: 6.4-49.8). In total, 137 patients (69.2%) underwent “early” (<11 months) palate surgery, 24 underwent “standard” (11-13 months) palate surgery, and 37 (18.7%) underwent “late” (>13 months) palate surgery.
Most patients with cleft palate attended their first visit to the study-craniofacial clinic within 100 days of birth. (Figure 1A). Most patients received surgery within 10 months of their first clinic visit (Figure 1B). Palate repair surgery most often occurred between 9 and 12 months of age, with the greatest number of patients undergoing surgery at 9 and 10 months of age, respectively (Figure 1C). Each timing histogram displayed a right skew and a long right tail, indicating a sizable number of patients exceeded the cohort median for each time measure.
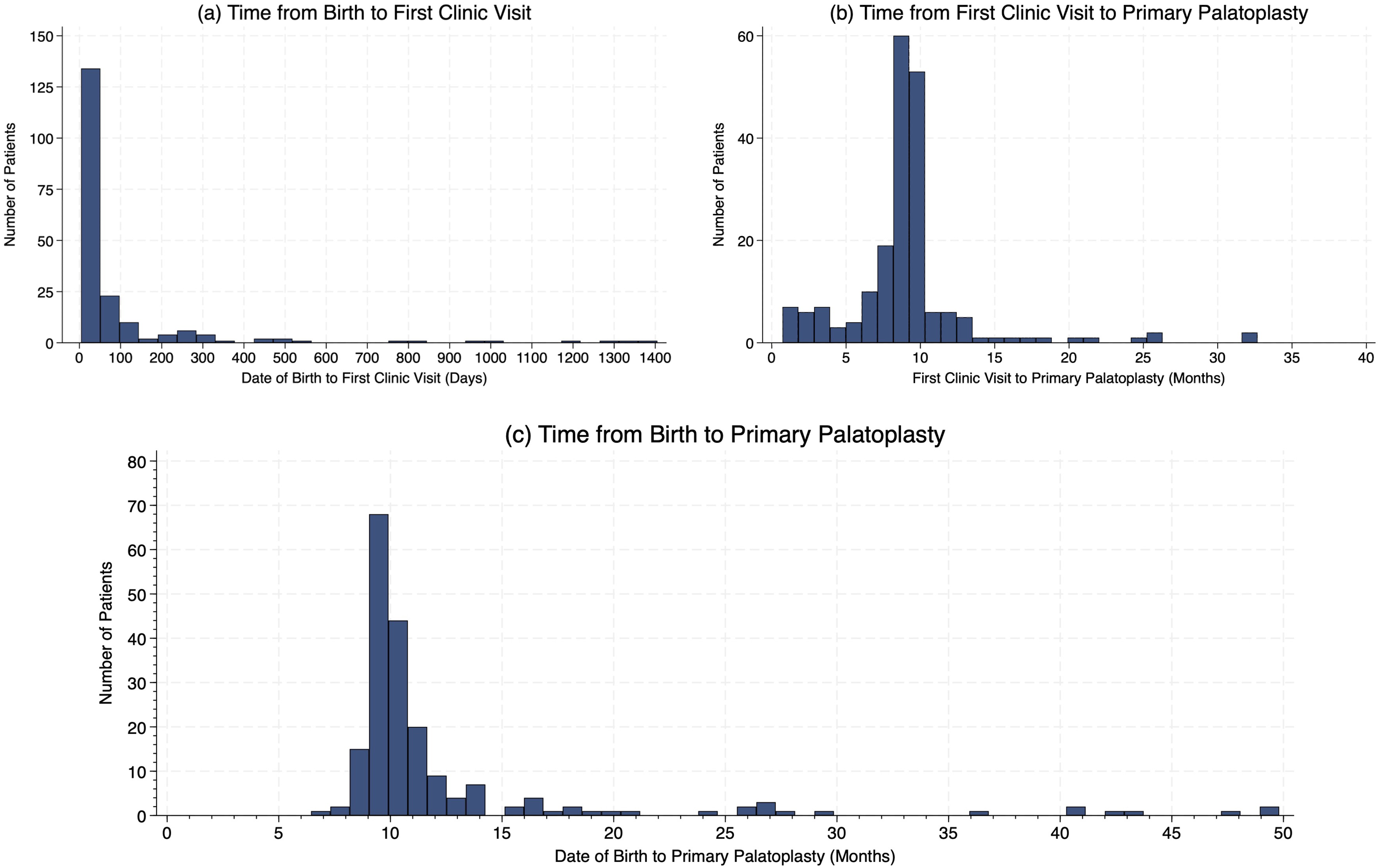
Distribution of time intervals between birth, first clinic visit, and palate surgery in patients with cleft palate.
Geographic Distribution of Patients
Patients seeking care at the study-craniofacial clinic were broadly distributed across the state, with 2 “hot spot” areas of particularly high patient concentration (Figure 2A). The first “hot spot” was centered around the study-craniofacial clinic and extended ∼50 miles into the surrounding area. The second “hot spot” was located ∼75 miles south-east of the study-craniofacial clinic. Of note, for patients in the second “hot spot” area the study-craniofacial clinic represented the closest ACPA-approved clinic, of the 4 total clinics in the state, despite being ∼75 to 100 miles away. The majority of patients traveled <120 min to receive care (Figure 2B). However, our results also show that a sizable proportion of patients who received care at the study-craniofacial clinic were geographically closer to 1 of the 3 other craniofacial clinics located within the state.
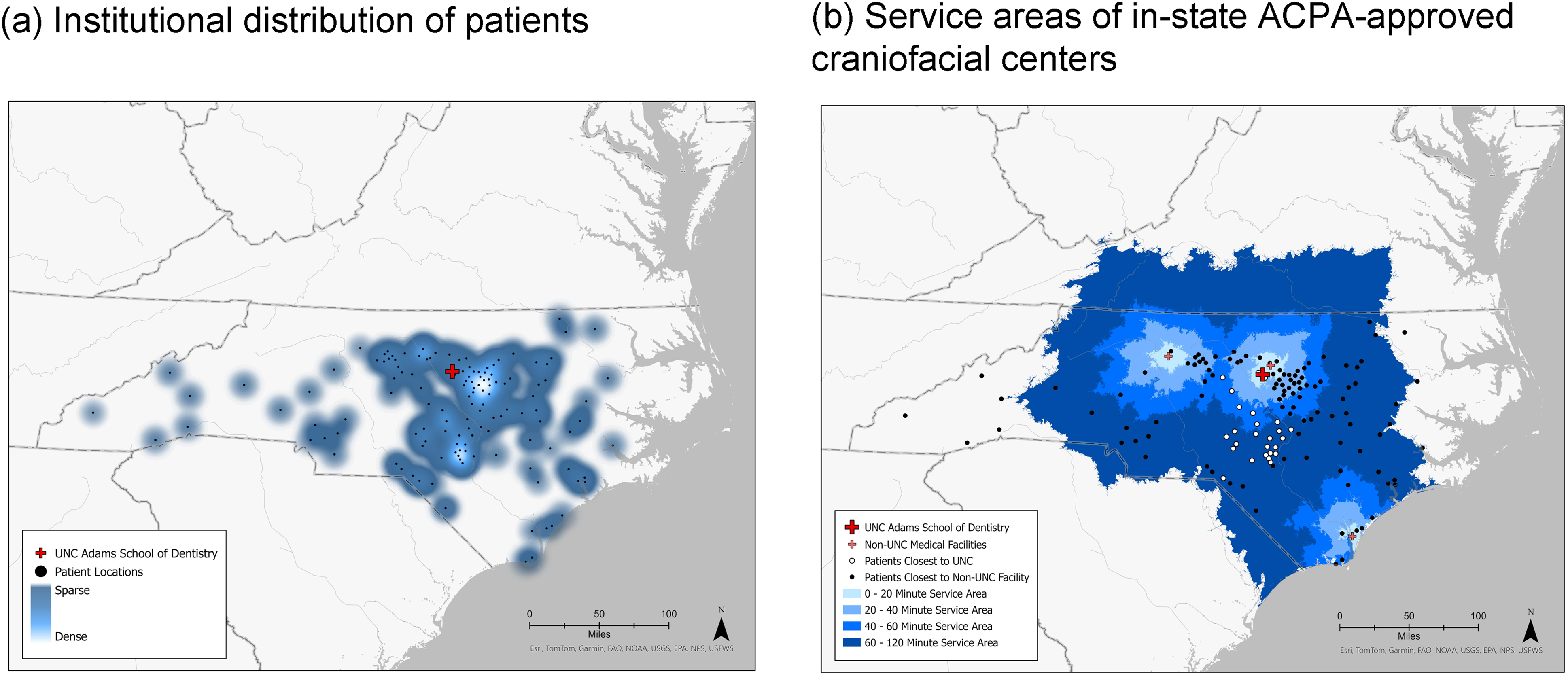
Geographic distribution of patients receiving care for cleft palate from 2016 to 2023.
Figure 3 illustrates the spatial distribution and institutional trends in timing of care for patients who received care for cleft palate at the study-craniofacial clinic during the study period. Each panel shows state-level geographic trends in patient access and timing of care, with the red cross denoting the location of the study-craniofacial clinic. Each circle represents a patient, with increased circle size corresponding to increased elapsed time. Panel (a) shows the distribution of patients based on the number of days from date of birth to the first clinic visit, with values ranging from 4 to 1405 days. Panel (b) represents the time from first clinic visit to surgery with a range of 22 to 994 days. Panel (c) demonstrates the interval from date of birth to palate surgery with days grouped into categories spanning from 196 to 1515 days. In each panel, the circles in the immediate area surrounding the study-craniofacial clinic were generally smaller in size indicating smaller time values. The proportion of larger circles increased as distance from the study-craniofacial center increased, particularly in the eastern part of the state, indicating many patients located further had larger time values.
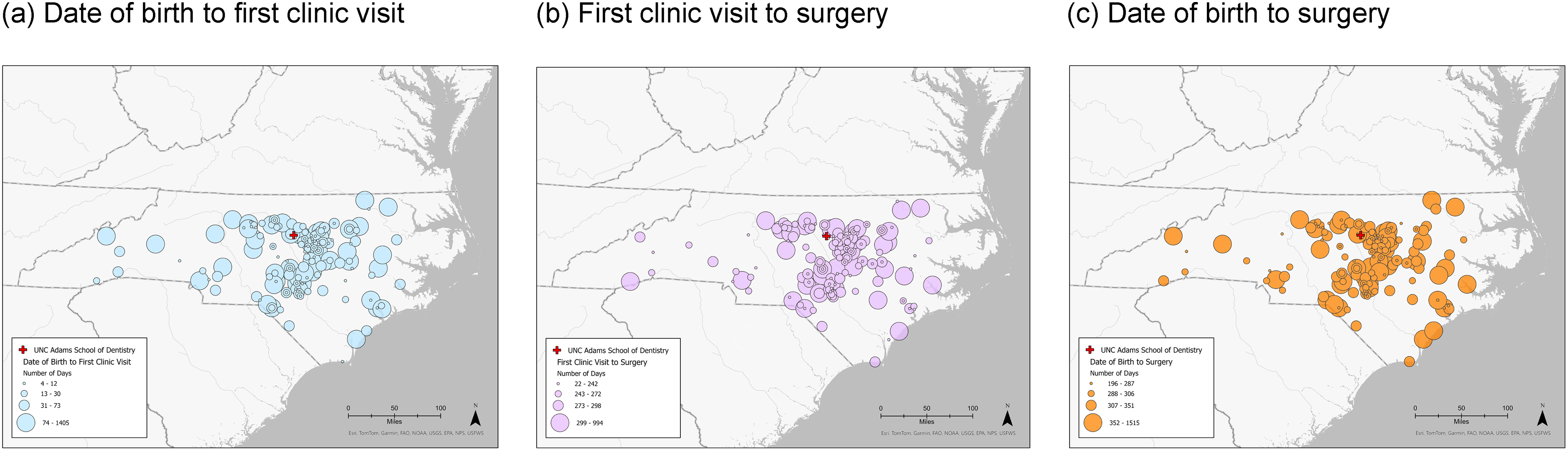
State level trends in timing of care for patients reviewing surgery for cleft palate from 2016 to 2023.
The Role of Distance Traveled on Care for Patients with Cleft Palate
Investigation of the statistical relationship between distance traveled for care and timing of care for patients with cleft palate is shown in Table 2. The coefficient estimates for each measure reflect the relationship between distance and the time intervals, with corresponding standard errors, P-values, confidence intervals, and R² values.
Effect of Distance Traveled on Measures of Care.
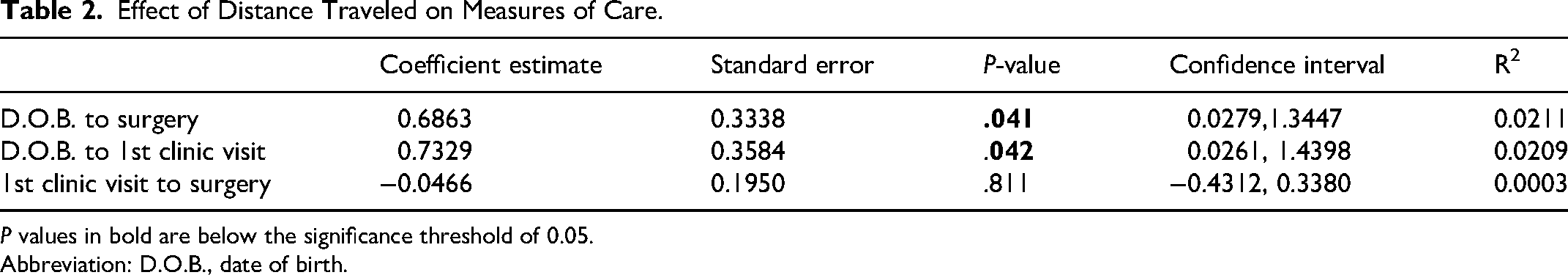

P values in bold are below the significance threshold of 0.05.
Abbreviation: D.O.B., date of birth.
For the “Date of Birth to Surgery” time measure, the coefficient estimate was 0.6863 (P = .041), indicating a statistically significant positive association between distance and time to palate repair surgery. Similarly, the interval from “Date of Birth to First Clinic Visit” had a coefficient estimate of 0.7329 (P = .042), also showing a significant positive relationship. In contrast, the interval from “First Clinic Visit to Surgery” had a coefficient estimate of −0.0466 (P = .811), suggesting no significant association between distance traveled and timing of care. Of note, the R² values for all models were low, indicating the impact of distance traveled for care has a small, but statistically significant, impact on “Date of Birth to Surgery” and “Date of Birth to First Clinic Visit.”
Clinical Factor Results and Associations With Distance Traveled and Surgical Timing
Of the 198 patients included in the study, 36 (18.2%) had evidence of an ED visit within 30 days of surgery and 15 (7.6%) did not have a follow-up visit with craniofacial center staff within 30 days of surgery. Evidence of prenatal cleft palate diagnosis was present for 59 (32.1%) patients and 171 (86.8%) received referral to speech therapy at the study-craniofacial center. VPI was present in 20 (11.4%) of patients between at the age of 3 years.
Results of the Kruskal-Wallis test to assess the relationship between ED visits, FU, PND, ST, and VPI and both distance traveled for care and age at palate repair surgery are shown in Figure 4. The variables assessed were. For each variable, the yellow bars represent P-values for distance, while the orange bars represent P-values for surgical timing. The red dashed line marks the significance threshold (P = .05).
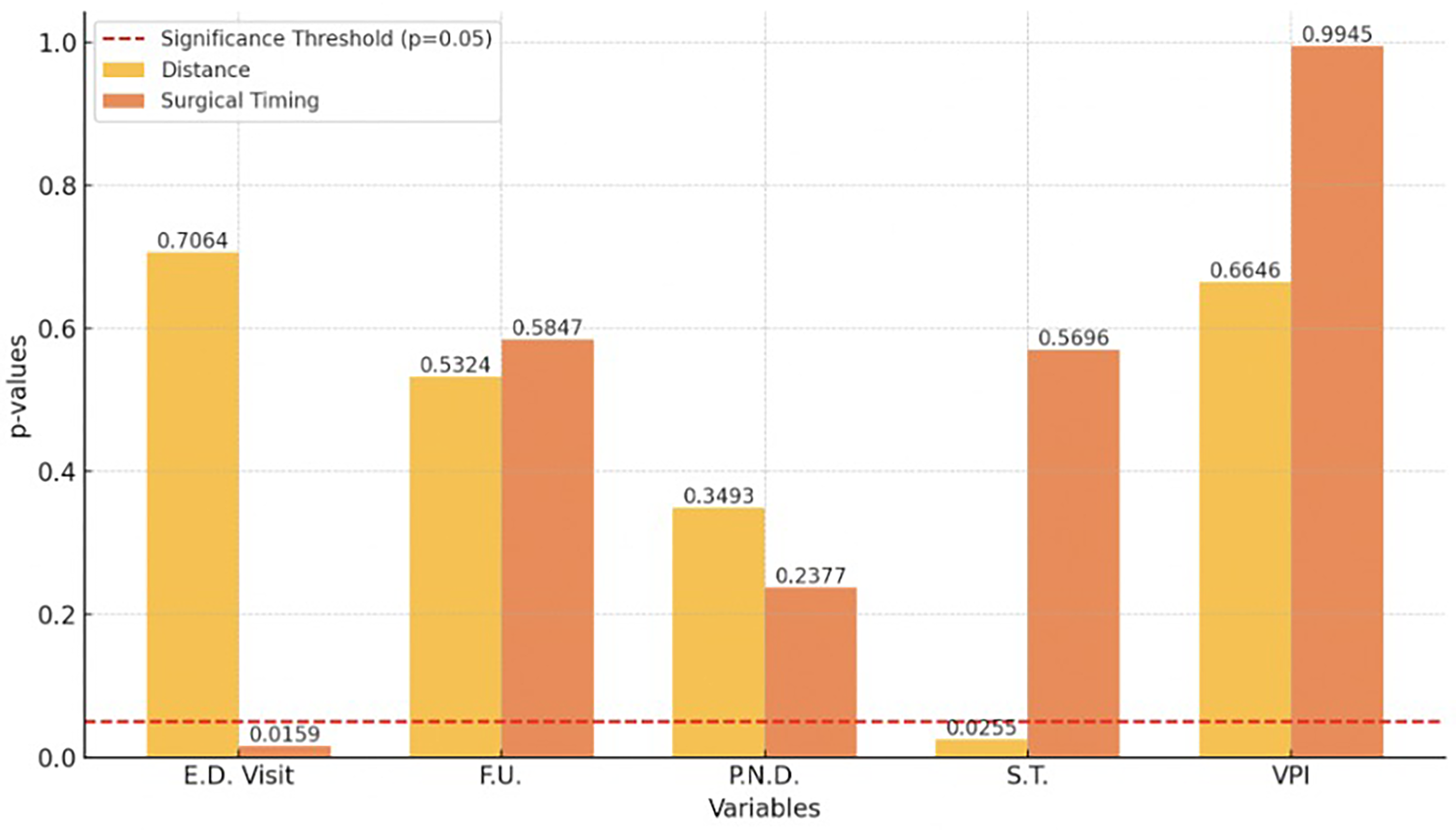
Kruskal-Wallis test results for the association of distance traveled and surgical timing with measures of care.
For “E.D. Visit,” the P-value for distance was .7064, indicating no significant association between the 2 variables, while surgical timing showed a statistically significant relationship (P = .0159). For “FU,” distance (P = .5324) nor surgical timing (P = .5847) had significant associations. For “PND” no significant relationship was found between surgical timing (P = .2377) or distance (P = .3493). For “ST,” surgical timing was found to have a significant association (P = .0255), while distance (P = .5696) was not. Finally, for “VPI,” neither distance (P = .6646) nor surgical timing (P = .9945) were found to have a significant relationship.
Discussion
Appropriate timing of surgical repair of cleft palate is widely held to be of great importance for patient outcomes and has been the subject of debate within the field for many decades.8,11 The ACPA currently offers no exact recommendation for timing of primary palate surgery, recommending that the decision be made on an individual patient basis by multidisciplinary care teams. 2 This recommendation likely comes as a result of the large body of conflicting evidence on the topic, as recommendations for surgical timing vary widely from 6 to 36 months.8,10,15 Complicating this issue is the difficulty and heterogeneity in assessment of patient outcomes following palate repair surgery. Assessed outcomes vary throughout the literature, but commonly reported patient outcome measures following palate repair most often include the following: proportion of patients with age appropriate speech development, rate of VIP development, and number of patients that need revision surgery.10,11
A recent large scale, international randomized control trial published by the New England Journal of Medicine concluded that primary palate surgery at 6 months was associated with decreased rates of VPI at age 5 compared to surgery at 12 months. 11 The results of this study clearly illustrate the impact of carefully timed surgical intervention for patients born with cleft palate, and were the motivation for this institutional investigation of current surgical timing practices and the impact of distance traveled on surgical timing.
In this retrospective investigation of 198 patients who underwent surgical repair of cleft palate at our institution, we present several key findings: (1) the median age at which patients at our institution undergo surgical repair of cleft palate is ∼10.1 months, (2) increased time to palate repair surgery is related to increased time to initial clinic visit but not increased duration of time between first clinic visit and surgery, (3) the median distance traveled for care by patients in our state is 63 miles, (4) distance traveled for care results in statistically significant increases in time to surgical repair of cleft palate, (5) surgical timing and distance traveled for care have some effect on postsurgical complication rates, and (6) a sizable proportion of patients seeking care for cleft palate within North Carolina bypass other more geographically proximal ACPA-approved craniofacial clinics to receive care at the study-craniofacial center.
An Institutional Review of Cleft Palate Surgery Timing
Despite the ongoing debate regarding optimal timing for cleft palate surgery, there are few studies that have elucidated institutional practices regarding timing of surgical intervention. One study conducted at a large tertiary cleft craniofacial clinic from 2005 to 2015 reported the median timing of primary surgery to be 12.6 months. 10 The study authors also found that “late” age at the time of palate surgery (>13 months) was associated with increased rates of speech and language delay compared to “early” (<11 months) and “standard” (11-13 months) surgical timing. 10
From 2016 to 2023, the median age of surgical intervention for patients with cleft palate was 10.1 months (range: 6.4-49.8). This data indicates that our institution tends to perform primary surgery for cleft palate patients earlier than previously reported data, which has defined standard age at palate surgery as 11 to 13 months. 10 While the ACPA currently puts forth no exact recommendation for timing of first surgery for patients with cleft palate, investigation of institutional practices of surgical timing are important to provide surgeons with a framework for care of their own patient populations. 2
The Impact of Distance Traveled for Care
Recent census data from 2020 showed that North Carolina had the second largest population of individuals living in rural areas in the United States with 3.5 million individuals, or 33% of the state population, having a rural place of residence. 16 Previous studies have documented significant regional variation in access to ACPA-approved craniofacial clinics, citing the South Eastern portion of the country as the area with most limited access. 17 In this study, we found the median distance traveled for care to be 63 miles (Table 1), with the largest proportion of patients traveling 40 to 120 min for care (Figure 2). These results concur with the results of a previous investigation of craniofacial patient travel trends in North Carolina which found patients travel a mean travel distance of 80.2 miles and have an average travel time of 91.7 min. 4
Increased patient travel time for care has been repeatedly demonstrated to be associated with poorer health outcomes. 13 This relationship has been illustrated for numerous pathologies, including head and neck cancer, diabetes, and mental health disorders.13,18 Though somewhat debated, the primary mechanism underlying this trend is thought to be time-based delays in receiving care. 13 Interestingly, a recent investigation by Asadourian et al into mechanisms underlying access and outcome disparities for patients with cleft palate showed no relationship between distance traveled and delays in clinical or surgical care for cleft palate patients in Rhode Island. 19
The results of this study show that distance has a significant impact on timing of primary cleft palate surgery (Table 2). Further, this relationship appears to be related to the impact of distance on age of first clinic presentation as opposed to “lag time” between first clinic visit and surgery. These results directly conflict with the previous investigations of this effect, likely as a result of the large rural population in the state in which this study was conducted. 19 Though the effect size of distance traveled to care was not observed to be large, these findings are still of great significance, as small differences in timing of primary surgery for patients with cleft palate have been found to results in significant differences in patient outcomes. 10
The Relationship Between Surgical Timing and Distance on Surgical Complications
Measurement of complications following surgery for cleft palate vary across the literature. Most studies include some measure of speech outcomes, most often including the rate of development of VPI, in addition to more generalized measures of speech function such as frequency of speech therapy.10,15,20 However, there are numerous important features that complicate the applicability of speech outcome measurements as a measure of cleft palate repair success, including debate about when to measure speech function and concerns about the confounding effects of surgery type and surgeon experience.20,21 Many studies include measurement of more traditional, short-term surgical outcome measures, including readmission rates, emergency room visits within the first 30 days, and length of hospital stay. 22
For the purposes of this study, we assessed speech therapy referrals, development of VPI, ED visits within 30 days of surgery, and frequency of 30-day follow up. These measures were chosen because they allowed for determination of both short-term and long-term complications and their relationship with both timing of cleft palate surgery as well as distance traveled for care.
Of the complications assessed, only ED visits within 30 days of surgery were found to have a statistically significant relationship with timing of palate repair surgery. Previous assessment of the relationship between ED visits and surgical timing of cleft repair are limited, but one study found that early cleft repair had an association with increased rate of ED visits. 22 However, other studies have shown that timing of surgical repair for patients with cleft palate had no relationship with postsurgical complication rates. 11 In the context of this study, this finding is potentially related to age-related physiological differences, particularly the immune and respiratory system, or variability in nutrition status with patient age.
Frequency of speech therapy referrals was the only complication found to have a statistically significant relationship with distance traveled for care. The relationship between distance traveled for care and need for speech therapy is difficult to explain, as previous research on this subject is limited. No significant relationship between surgical timing and need for speech therapy was found, despite previous literature evidence that increased age at surgery for cleft palate has been demonstrated to result in increased need for speech therapy. 10 Most likely, this finding is related to disparities in access to speech therapy resources for patients in rural areas, as many of the patients traveling far distances for care live in more rural areas of the state. Speech therapy resources in rural areas are limited, and patients living in rural areas may have been more likely to seek speech therapy through the study-craniofacial clinic, as it may have represented their only option for care. 23 Patients living closer to the study-craniofacial clinic, in more urban areas, may have opted for speech therapy outside of the study-craniofacial center, in favor of community-based care that was more convenient. As a result, the observed differences in rates of speech therapy referrals may be unrelated to differences in prevalence of speech dysfunction, and instead a result of underlying geographic variation in community speech therapy resources.
The development of VPI is often discussed as an important outcome for patients undergoing cleft palate surgery. 8 Estimates of the frequency of VPI development in patients born with cleft palate vary widely but generally are approximately 10% to 20%.10,11,20 In this study, 11.4% of patients developed VPI, a finding which is consistent with previous literature. Interestingly, no significant relationship was found between VPI development rate and age at cleft palate surgery or distance traveled for care. While some previous studies have reported the impact of surgical age on VPI development, this finding was unexpected. 10 The results of this study lend credence to the hypothesis that age at primary cleft palate surgery does not significantly impact the rate of VPI development, but the lack of consensus in the literature illustrates the need for more investigation into this topic.
Limitations
There are several limitations of this study. Due to the retrospective nature of this study, the results of this study cannot establish a causative relationship between distance traveled for care at the study-craniofacial center and timing of palate repair surgery. It is possible that other factors, including but not limited to socioeconomic status and spoken language at home, were relevant to the relationship we observed.
Distance traveled for care was estimated using zip codes extracted from patient charts, and thus limited the specificity of the GIS portion of our work. In addition, patients with zip codes located outside of the state were excluded to allow for streamlined mapping analysis using the GIS program. Though the number of patients seeking care from outside the state was small (n = 3), the exclusion of these patients may have impacted our assessment of distance traveled for care on patient outcomes.
Patients with submucous cleft palate were also excluded from this study to limit the potentially confounding effects of variable palatoplasty type. 24 However, the decision to exclude said patients also may limit the generalizability of these results. Finally, rates of VPI were assessed at age 3 for patients included in this study. Though previous studies have shown that VPI can be reliability assessed as young as age 3, a proportion of patients may present as late as 5 years. 20 As a result, it is possible that calculations of VPI rates were skewed.
Implications and Future Directions
In recent years, the concept of patient access to care has become of great interest within the medical field at large. Though difficult to define exactly, Penchansky and Thomas posited that access to care could be defined as the fit between the patient and the healthcare system and was mediated by 4 major components: availability, accessibility, accommodation, and acceptability. 25 Given the large rural population in North Carolina, where this study was conducted, the concept of variable access to care and its impact on patients born with cleft palate is important to consider. 16 Previous investigations into the relationship between distance traveled for care and care outcomes for patients born with cleft palate have primarily been conducted in areas without the large rural population as in the state where this study was conducted. 19 The findings of this study thus represent a valuable contribution to the literature and provide necessary information about care trends for the 66 million individuals in the United States who live in rural areas. 26
Indeed, the findings of this study support the hypothesis that rural residence has measurable, significant impacts on timing of care for patients born with cleft palate. Unexpectedly, we found that many patients who traveled greater distances for care bypassed other ACPA-approved craniofacial clinics located in the state and ultimately sought care at the study-craniofacial clinic. The reasons for this finding are difficult to parse out, given the retrospective nature of this study, but are likely related to one of all of the components of access to care outlined above. 25 It is possible that care at these other institutions is difficult to schedule (availability) or other institutions do not have all the resources needed by patients (acceptability).
Broadly, the most important future direction of this work would be the establishment of a centralized process to encourage patient referrals to craniofacial clinics based on their location. Admittedly, the establishment of such a process would be difficult and time consuming but would be of great benefit to a large proportion of patients. At the level of our institution, further investigation into individual patient rationale for seeking care at craniofacial clinics located further away through qualitative study would be helpful. With this information, measures to compensate for initial care delays, such as advising surgeons to expedite surgical scheduling for patients traveling further distances for care, could be pursued. However, the impact of these actions may be limited given the status of medical care in this state. Therefore, it is paramount that state level measures to increase healthcare accessibility be undertaken for the betterment of patient outcomes at our institution and beyond.
Conclusion
We present an 8-year, single institution review of surgical timing practices for patients with cleft palate and an investigation of the impact of distance traveled for care on timing of palate surgery and complication rates. This study found that the median age at time of palate surgery was 10.1 months, lower than previously reported averages and is closer to the ideal age of palate surgery that was recently proposed by a large-scale randomized control trial. 11 Further, we found that increased distance traveled for care was associated with increased patient age at cleft palate surgery. This study provides the foundational information needed for future efforts to improve timely access to cleft and craniofacial care in states, such as ours, with large rural populations.
Footnotes
Acknowledgments
The authors thank the faculty and residents at The University of North Carolina Adam's School of Dentistry for their support in data collection and analysis. The authors would also like to acknowledge the utility of ChatGPT in helping to produce visual representations of the data.
Ethical Approval
This study was approved by the Institutional Review Board (IRB Number: 24-1831).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data generated and analyzed for the purposes of this study are available from the corresponding author upon request.
