Abstract
Objective
Evaluate the use of cortical bone grafts (CBGs) for nasal floor reconstruction on alveolar bone graft (ABG) outcomes in unilateral cleft lip and palate (UCLP).
Design
Retrospective cohort study.
Setting
North-American cleft centers.
Subjects
Fifty-three children with nonsyndromic UCLP treated with secondary ABG.
Methods
Center 1 (n = 23) utilized CBG for nasal floor reconstruction, while Centers 2 (n = 10), 3 (n = 10), and 4 (n = 10) did not. Occlusal radiographs, taken 6 to 18 months after ABG, were assessed by 6 calibrated raters using the Standardized Way to Assess Grafts (SWAG) Scale. Weighted kappa statistics measured intra and interrater reliabilities. SWAG scores comparisons in the apical, middle, and coronal thirds of the alveolar cleft were conducted between the centers. The Kruskal–Wallis test was used to determine significant differences, with a P-value of <.05 considered statistically significant.
Results
Intrarater reliability was very good (κ = 0.858), and interrater reliabilities were good (κ = 0.717). Significant differences were initially found in overall SWAG scores across centers (P = .003), with Center 1 achieving the highest mean overall SWAG score (5.16 ± 0.99) compared to Centers 2, 3, and 4 (4.48 ± 1.37, 4.58 ± 1.44, and 3.72 ± 0.65, respectively). Center 4 exhibited statistically significant lower scores compared to Centers1, 2, and 3, and was excluded from secondary analyses. After exclusion, no significant differences remained among Centers1, 2, and 3 (P = .135) for overall SWAG scores or apical third SWAG scores (where CBG is inserted). No significant differences were observed in the middle (P = .055) or coronal (P = .131) thirds across centers.
Conclusions
CBG in secondary ABG procedures for CUCLP patients showed outcomes comparable to cancellous-only grafts, with a trend toward improved apical scores in CBG-treated patients.
Introduction
Secondary alveolar bone grafting (ABG) is a key procedure in the management of complete unilateral cleft lip and palate (CUCLP), aiming to close the cleft and restore bone continuity for dental and orthodontic rehabilitation.1–6 ABGs also help reconstruct the nasal floor and nasolabial soft tissue framework, contributing to improved function and esthetics. 5
While secondary ABG techniques have evolved significantly over time, challenges persist, particularly in achieving consistent bone fill in the apical region of the cleft.4,7,8 Cortical bone grafts (CBGs) have emerged as a technique for nasal floor reconstruction, where a thin cortical bone sheet from the iliac crest is placed to seal the nasal mucosa and improve graft stability.5,9–11 Compared to cancellous-only grafts, CBGs are proposed to enhance bony bridge formation, improve alveolar height, and create symmetry in the piriform apertures.5,12–16 However, direct comparisons between these techniques remain limited.
This study aims to assess the impact of employing a CBG for nasal floor reconstruction on the outcomes of secondary ABGs in patients with nonsyndromic CUCLP. The specific aims of the study were to compare the bony bridge formation, as quantified by the Standardized Way to Assess Grafts (SWAG) score, across the coronal, middle, and apical thirds of the alveolar cleft to determine if CBG offers superior bony bridge formation, particularly in the apical region, which is known to present grafting challenges. 17 The hypothesis posits that the reconstruction of the nasal floor with a CBG will lead to improved bony bridge formation when compared to cancellous bone grafts only.
Methods
Patients and Surgical Method
This multicenter retrospective cohort study reviewed clinical records of patients with CUCLP who were consecutively treated at their respective surgical centers between January 2000 and January 2008. This study was approved by the IWK Health Center Research Ethics Board.
The inclusion criteria for patients included:
Nonsyndromic CUCLP Consecutively treated patients with ABGs at their respective centers Postsurgical maxillary occlusal radiographs 6 to 18 months following secondary ABG. All surgeries, including primary repairs and secondary ABG, were performed at the respective centers. syndromic clefts incomplete clefts, bilateral cleft lip and palate primary ABG incomplete records patients lost to follow-up.
The exclusion criteria included:
Surgical Technique
At Center 1, patients underwent a CBG to reconstruct the nasal floor followed by packing of cancellous bone prior to the eruption of the cleft-side permanent central incisor, following the protocol outlined by Precious. 5 A sheet of cortical bone was harvested from the ipsilateral iliac crest, shaped to fit the nasal floor, and inserted into the alveolar cleft defect with the cortical side adjacent to the nasal mucosa (Figure 1).
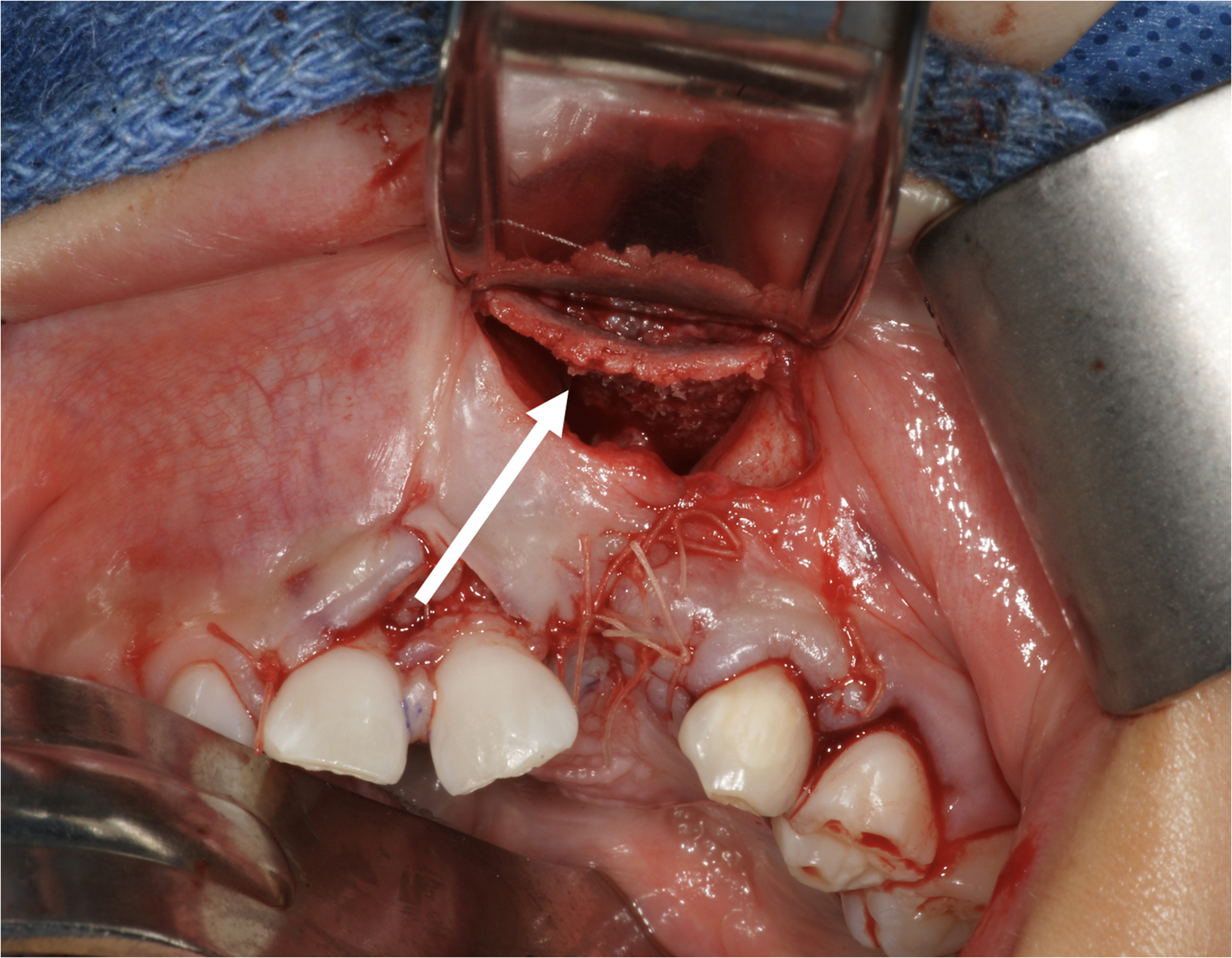
Placement of the cortical bone graft at the level of the nasal floor.
In centers 2, 3, and 4, patients received a similar surgical procedure, with the exception that all surgeons in these centers did not use a cortical sheet to reconstruct the floor of the nasal cavity on the cleft side. Additionally, the surgeons in these centers relied on the cleft side canine development to make the determination for ABGs, rather than utilizing the eruption of the central incisor.
SWAG Analysis
The SWAG Scale, a Standardized Method for Assessing Grafts, has been validated to be a reliable technique to evaluate ABGs.17–19 The SWAG Scale can be used to assess ABGs in mixed and permanent dentitions. This methodology offers a simple scoring system that allows for consistent and reproducible assessments of graft outcomes across different clinicians and research studies.
The scoring process (Table 1) involves dividing the cleft site into three sections: apical, middle, and coronal thirds (Figure 2). Each third is assigned a score of 0, 1, or 2 based on the presence or absence of bone bridging. A score of 2 indicates the unequivocal presence of a bony bridge within that third, while a score of 0 or 1 indicates the absence of bone bridging. If roots are exposed a score of 0 is given while if no roots are exposed then a score of 1 is given. It is important to note that for a bony bridge to be considered present, it must be clear and unambiguous, although complete filling of the entire third with bone is not necessary (Figure 2).
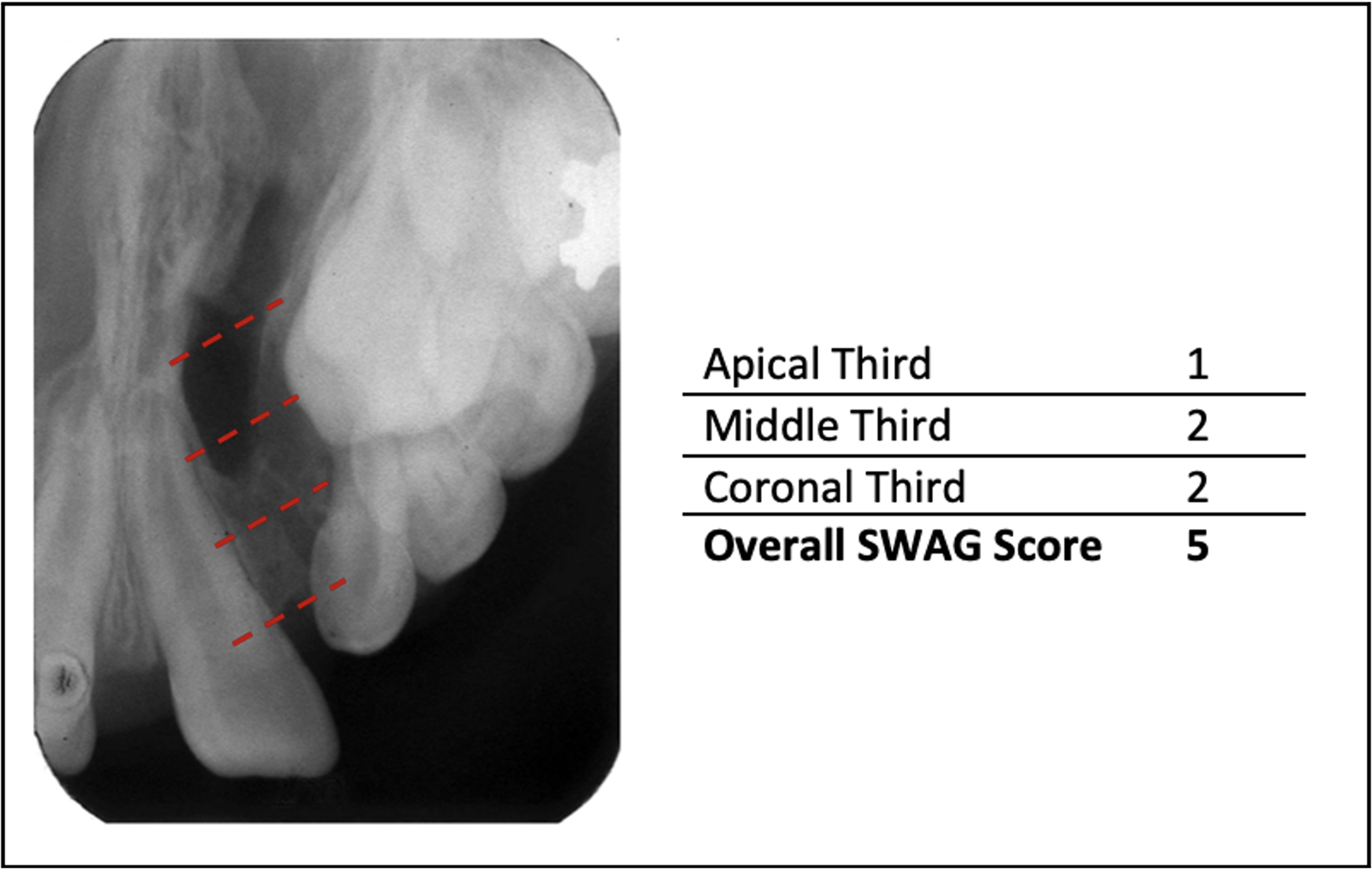
Example of graft rating using the SWAG Scale.
SWAG Scale Scores.a
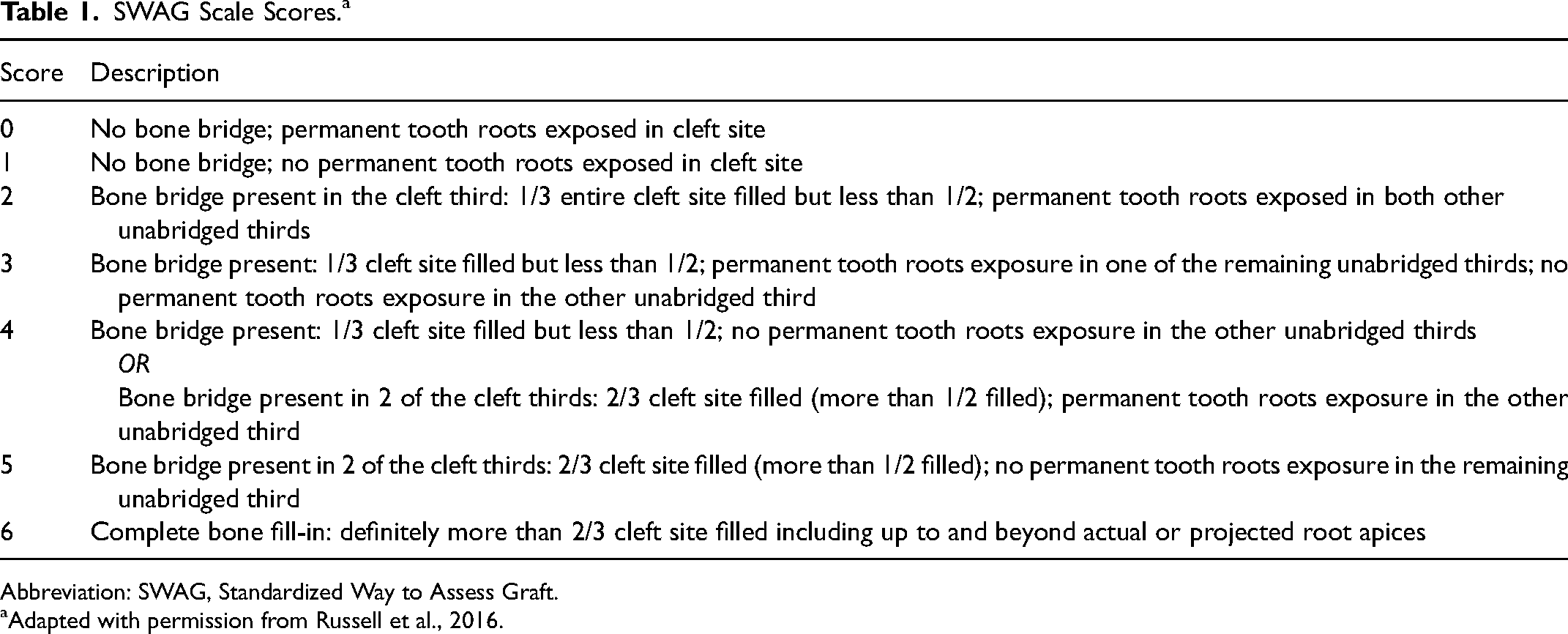
Abbreviation: SWAG, Standardized Way to Assess Graft.
Adapted with permission from Russell et al., 2016.
If complete bone fill is not achieved, the score is determined by assessing the presence (score 0) or absence (score 1) of exposed permanent tooth roots within the cleft site. The final SWAG score is obtained by summing the scores for each third, resulting in a range of scores from 0 to 6. This scoring system provides an indication of the extent of bone fill and, if incomplete, identifies the location (apical, middle, or coronal) of residual defects. It also offers insights into the prognosis for regrafting without tooth loss, due to identification of root coverage with bone.
Radiographic Analysis
Maxillary occlusal radiographs were scanned and digitally enhanced, as necessary. All patient and center identifiers were carefully removed from the radiographs. The radiographs were then assigned random numbers and arranged in a random order for evaluation. To facilitate the rating process, the radiographs were projected in a PowerPoint format (v. 14.4.9, Microsoft, Redmond, WA) and assessed by 6 trained and calibrated raters using the SWAG Scale. The raters consisted of a group of 1 oral and maxillofacial surgeon, 1 plastic surgeon, and 4 orthodontists. All raters were blinded to the identity and origin of the radiographs throughout the rating process. After a 24-hr interval following the initial rating, the radiographs were randomly rearranged, renumbered, and subjected to a second round of assessment by the same group of raters.
Statistics
All statistical analyses were performed using SPSS version 22.0. To assess reliability among raters, both intrarater and interrater reliabilities were evaluated using weighted kappa statistics to measure the consistency of SWAG score measurements. The SWAG score, which encompasses the apical, middle, and coronal thirds of the alveolar cleft, as well as the overall SWAG score, was compared between centers using the Kruskal–Wallis test. Post-hoc analyses were conducted using Dunn's test with Bonferroni correction to identify specific pairwise differences among centers.
Additional analyses were performed to evaluate demographic and follow-up time differences across centers. Age differences were assessed using the Kruskal–Wallis test, followed by Dunn's post-hoc test with Bonferroni correction to identify specific center comparisons. Gender distribution differences across centers were analyzed using the Chi-square test. Radiographic follow-up times were also compared across centers using the Kruskal–Wallis test, with post-hoc pairwise comparisons where applicable.
To explore the relationship between age at the time of ABG and SWAG scores, Spearman's rho correlation analysis was used to evaluate associations between age and the overall SWAG score, as well as each of the apical, middle, and coronal thirds. A significance level of P < .05 was used to determine statistically significant differences in all analyses.
Results
A total of 53 patients met the inclusion and exclusion criteria from the 4 North American cleft centers. Center 1 (n = 23) used a CBG for nasal floor reconstruction, while Center 2 (n = 10), Center 3 (n = 10), and Center 4 (n = 10) did not (Table 2). Most patients received their postoperative radiograph at 6 months, with a smaller proportion of patients receiving their postoperative radiograph at later time points, up to 18 months postoperatively.
Demographics and Treatment Protocols for Patients at the 4 Study Centers.
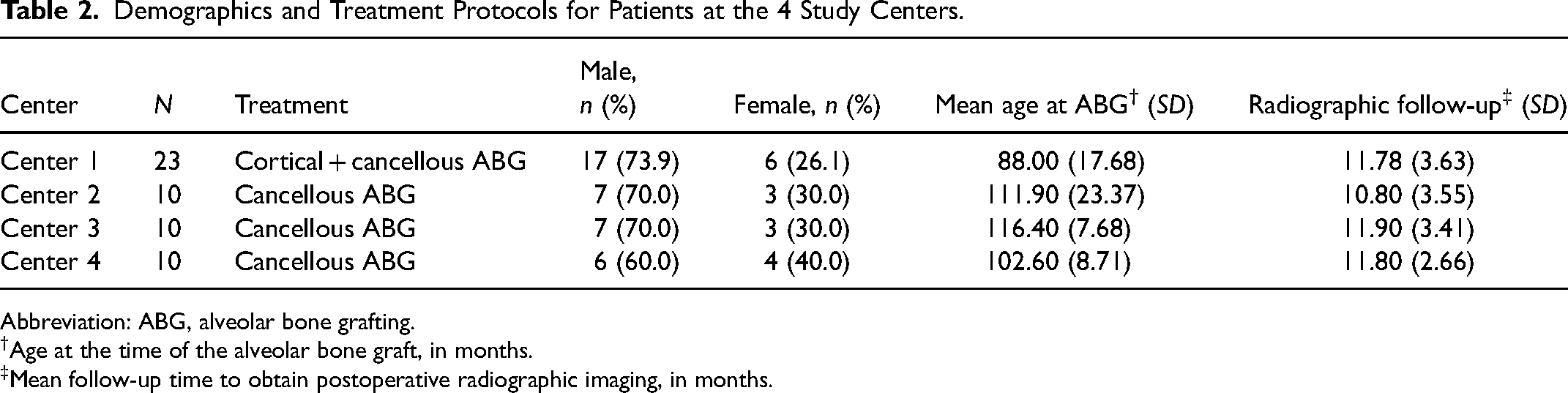
Abbreviation: ABG, alveolar bone grafting.
Age at the time of the alveolar bone graft, in months.
Mean follow-up time to obtain postoperative radiographic imaging, in months.
Demographics and Follow-Up
The demographic characteristics of each center are summarized in Table 2. A Kruskal–Wallis test indicated a statistically significant difference in age distribution across centers (H = 24.043, P < .001). Post-hoc pairwise comparisons using Dunn's test with Bonferroni correction revealed that Center 1 had a significantly younger population than Centers 2 (adjusted P = .013) and 3 (adjusted P < .001). Center 1 also differed in age from Center 4, but this difference was not statistically significant after adjustment (adjusted P = .221). Additionally, a Chi-square test for gender distribution showed no statistically significant difference among centers (P = .887). A Kruskal–Wallis test indicated no statistically significant differences in radiographic follow-up time in months across centers (H = 0.520, P = .914). Pairwise comparisons with Dunn's test also revealed no significant differences between any centers.
SWAG Score Reliability
The intrarater reliabilities demonstrated very good agreement, with a weighted kappa value of 0.858. Interrater reliabilities also showed good agreement with a weighted kappa value of 0.717. These results indicate consistent and reliable assessments of the SWAG scores within the same rater and reasonable agreement between different raters.
SWAG Score Comparisons
Center 1, utilizing cortical and CBG, achieved a mean overall SWAG score of 5.16 ± 0.99, while Centers 2, 3, and 4 achieved mean overall SWAG scores of 4.48 ± 1.37, 4.58 ± 1.44, and 3.72 ± 0.65, respectively (Figure 3). Pairwise comparisons demonstrated that Center 4 had significantly lower overall SWAG scores compared to Center 1 (adjusted P = .001) but was not significantly different from Centers 2 and 3 (adjusted P = .420 and P = .357, respectively). No significant differences were observed among Centers 1, 2, and 3 for overall SWAG scores (adjusted P = .765 for Center 2 vs. Center 1 and P = .902 for Center 3 vs. Center 1).
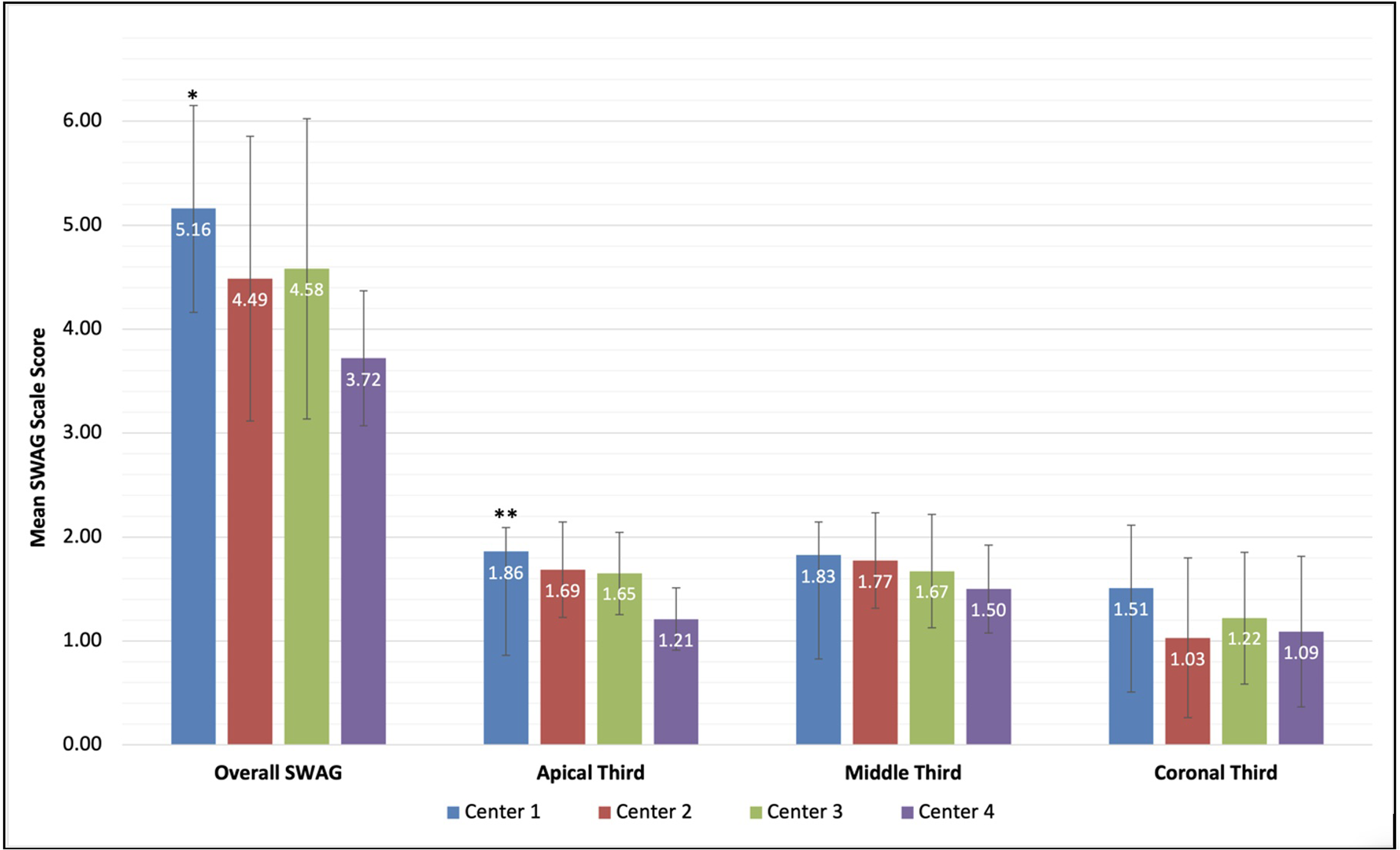
Mean SWAG scores across the 4 surgical centers.
At the apical third, Center 1 achieved a bony bridge in 96% of cases, while Centers 2, 3, and 4 exhibited proportions of 80%, 70%, and 20%, respectively (Table 3). Center 1 achieved a mean apical SWAG score of 1.86 ± 0.23, while Centers 2, 3, and 4 achieved mean apical SWAG scores of 1.69 ± 0.45, 1.65 ± 0.40, and 1.20 ± 0.40, respectively. Pairwise comparisons indicated that Center 4's apical scores were significantly lower than those of Center 1 (adjusted P < .001) but did not differ significantly from Centers 2 or 3 (adjusted P = .053 and P = .184, respectively). No significant differences were observed among Centers 1, 2, and 3 for apical scores (adjusted P = .330 for Center 3 vs. Center 1 and P = 1.000 for Center 2 vs. Center 1).
Apical Bony Bridges Present for Patients in Each Study Center.
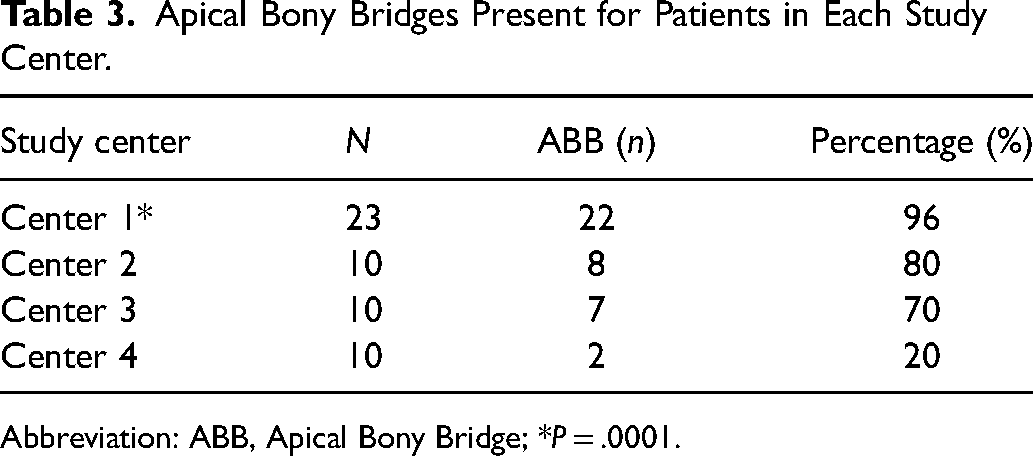
Abbreviation: ABB, Apical Bony Bridge; *P = .0001.
No statistically significant differences were observed in SWAG scores for the middle (P = .055) or coronal (P = .131) thirds of the cleft across all centers. The mean middle third SWAG scores ranged from 1.75 ± 0.18 (Center 1) to 1.53 ± 0.34 (Center 4). For the coronal third, the mean scores ranged from 1.55 ± 0.18 (Center 1) to 1.20 ± 0.33 (Center 4).
A sensitivity analysis excluding Center 4, identified as having notably lower outcomes, revealed no statistically significant differences among Centers 1, 2, and 3 in either overall SWAG scores (P = .135) or apical SWAG scores (P = .071). Again, no significant differences were observed in the middle (P = .479) or coronal thirds (P = .122) after excluding Center 4.
Correlation of Age With SWAG Scores
A Spearman's rho correlation analysis revealed a significant negative correlation between age at the time of ABG and the overall SWAG score (ρ = −0.397, P = .003) and the coronal SWAG score (ρ = −0.471, P < .001). No significant correlations were observed between age and the apical SWAG score (P = .063) or the middle SWAG score (P = .241).
Discussion
This study evaluated the use of cortical and CBGs for nasal floor reconstruction in secondary ABG for patients with nonsyndromic CUCLP. CBGs have been proposed to improve bony bridge formation and optimize nasal floor reconstruction by placing a thin cortical sheet over the cancellous graft.20–22
Our findings show that cortical and CBGs achieved similar bony bridge formation to cancellous grafts alone. Center 1, which used CBGs, demonstrated high apical bony bridge rates, but comparable outcomes were observed at Centers 2 and 3 with cancellous grafts alone. While Center 1 showed a trend toward higher apical scores, it was not statistically significant. Sensitivity analysis excluding Center 4—where outcomes were notably lower—revealed no significant differences in apical bony bridge formation or overall SWAG scores among Centers 1, 2, and 3.
Consistent with prior research, achieving reliable bone formation in the apical portion of alveolar clefts remains challenging.1,5,22 While CBGs have been proposed to provide structural support for cancellous bone and separate the graft from the nasal mucosa,5,22 our findings showed comparable apical outcomes in Centers 2 and 3 using cancellous grafts alone. Prior studies using both 2D and 3D imaging techniques have similarly noted reduced bone formation in the apical region, which may reflect the region's geometry and limited accessibility.23–25
Age at the time of ABG was found to negatively correlate with overall and coronal SWAG scores, suggesting a trend toward improved bone formation in younger patients. However, no significant correlations were observed for the apical or middle thirds. These findings should be interpreted with caution, as the small sample size may have limited the ability to identify consistent trends across all regions.
CBG may help seal the interface between cancellous bone and nasal mucosa, reducing the risk of oral-nasal fistulas, while providing adequate bone stock for tooth development and orthodontic movement.15,26 However, results from Centers 2 and 3 suggest cancellous bone alone can also be effective. The lower apical bony bridge formation at Center 4 likely reflects center-specific factors such as surgical technique, patient demographics, or postoperative management, underscoring variability in multicenter studies.
This study has limitations, including its retrospective design, small sample size, and use of 2D occlusal radiographs. While the SWAG scale is a validated tool for assessing graft outcomes, it may underestimate bony bridge formation compared to CBCT, which could provide a more comprehensive evaluation of graft integration.17–19,27 The study period (2000-2008) limited imaging options, and differences in age across centers, surgical technique, flap design, and orthodontic protocols may have influenced outcomes. Future studies with larger sample sizes, standardized protocols, and three-dimensional imaging such as CBCT are needed to better identify factors contributing to successful graft integration and further validate the SWAG scale.
Cortical and cancellous bone grafts in secondary ABG achieved similar apical bony bridge formation to cancellous-only grafts. While Center 1, which used CBG, showed a trend toward higher apical scores, this was not statistically significant. The established effectiveness of cancellous grafts in achieving apical bone fill remains evident. Future studies with larger sample sizes and three-dimensional imaging are needed to further compare the outcomes of cortical and cancellous grafts to cancellous-only grafts in secondary ABG.
Conclusion
Combining cortical and CBG in secondary ABG demonstrated comparable apical bony bridge formation to cancellous-only grafts. While CBG showed a trend toward improved apical outcomes on the SWAG scale, this was not statistically significant. The established success of cancellous grafts remains evident, though the potential advantages of CBG merit further investigation. Larger studies with three-dimensional imaging are needed to confirm these findings and explore their long-term clinical implications.
Footnotes
Acknowledgments
The authors would like to acknowledge Nicholas Emanuele, DDS, BSc; Jennifer Kearns, DDS; Patricia Beals, DMD, MS; Stephen Beals, MD, FACS, FAAP; Michelle Kornbluth, BSc, DMD, MSc, FRCDC; Thomas J. Sitzman, MD, MPH; and Richard E. Campbell, DMD for their contribution.
Author Note
This article was presented, in part, at the American Cleft Palate—Craniofacial Association 74th annual meeting in Colorado Springs, CO, March 2017.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded in part by the 2014 Subtelny Orthodontic Clinical Research Grant from the Cleft Palate Foundation and by a Faculty Research Grant from the Faculty of Dentistry, Dalhousie University, Halifax, Canada.
