Abstract
Objective:
Life can be challenging for children with a visible difference due to a medical condition, and they might be at risk for emotional and behavioral problems. This study examines emotional and behavioral problems in children with a cleft lip with or without palate (CL ± P) or an infantile hemangioma (IH) in relation to the visibility of the condition, the presence of additional condition-related problems, and parental affect.
Setting:
This cross-sectional study took place in an academic medical hospital in the Erasmus MC Sophia Children’s Hospital, the Netherlands.
Participants:
A total of 309 parents (mean age = 40.34, 44.00% male) of 182 children with CL ± P and 48 parents (mean age = 39.21, 37.50% male) of 33 children with an IH completed questionnaires. Children were 1.5 to 12 years old.
Results:
Parents reported fewer child emotional and behavioral problems compared to normative data. Problems reported were mainly related to learning difficulties and parent gender, while visibility of the condition had no significant influence. Parental negative affect was related to child internalizing problems. Parental positive affect was not related to any of the outcome measures.
Conclusions:
Parents reported fewer problems for their children compared to normative data. This is inconsistent with previous research, showing similar or worse scores for these children compared to peers. Our findings may be explained by a protective parenting style, a response shift in parents, or problems developing at a later point in life.
Keywords
Introduction
In societies that place high demands on physical appearance, coping with a visible difference due to a medical condition, such as cleft lip with or without palate (CL ± P) or an infantile hemangioma (IH), can be challenging. Children with a visible difference that is present from birth or early infancy are at risk for negative social interactions, including stigmatization and bullying (Ablett & Thompson, 2016). These social interactions may be associated with emotional and behavioral problems and can negatively impact the overall quality of life of children with a visible difference (Hunt et al., 2006; Masnari et al., 2013).
Cleft lip with or without palate is one of the most common craniofacial anomalies with 1 occurrence per 700 to 1100 live births (Goodacre & Swan, 2008; Mai et al., 2014). Infantile hemangioma is the most common vascular tumor with an estimated incidence of 2.0% to 4.5% in infants, often located in the head and neck area (Dickison et al., 2011; Munden et al., 2014; Anderson et al., 2016). Both conditions are visible from birth or shortly after, may cause significant functional problems during infancy, and leave permanent scars (Goodacre & Swan, 2008; Léauté-Labrèze et al., 2017). Nonetheless, the nature of the visible differences and functional problems may be different, potentially associated with variation in emotional and behavioral functioning.
A range of findings have been reported regarding emotional and behavioral problems in children with CL ± P (Hunt et al., 2005). Some studies report an increased number of psychological difficulties in children with CL ± P compared to children from the general population (Murray et al., 2010; Snyder & Pope, 2010; Zeraatkar et al., 2019; Pinckston et al., 2020), while other studies suggest that children with CL±P do not have more psychological difficulties (Berger & Dalton, 2009; Brand et al., 2009; Feragen & Stock, 2014). The nature and the extent of emotional and behavioral problems vary according to the child’s age and gender (Pope & Snyder, 2005; Snyder & Pope, 2010; Pinckston et al., 2020). Furthermore, emotional and behavioral problems may be more prevalent in children with visible cleft as opposed to children with a nonvisible cleft (Hunt et al., 2007).
Previous studies suggest that children with IH have an average or a better quality of life than children without IH (Hoornweg et al., 2009; Cohen-Barak et al., 2013). Nonetheless, parents report that their school-age children with IH exhibit more negative emotions compared to peers (Hoornweg et al., 2009). In addition, children with an IH experience negative observer responses such as staring, when the IH is at a visible location or medically complicated (Hoornweg et al., 2009). Yet, research has not found elevated levels of emotional or behavioral problems in children with IH (Dieterich-Miller et al., 1992; Masnari et al., 2012; Moyakine et al., 2017). However, small sample sizes may have led to inconclusive results. Furthermore, associations between emotional and behavioral problems and visibility or additional medical problems were not explored.
Given concerns about the impact of the visible medical conditions CL ± P and IH, an investigation of emotional and behavioral problems in these patient groups is highly relevant. Conclusions about why some patients with CL ± P or IH, but not others, experience mental health problems are hard to draw (Pope & Snyder, 2005; Feragen & Stock, 2017). Adjustment to living with a visible difference involves a complex interplay of physical, sociocultural, and psychological factors (Clarke et al., 2014; Gee et al., 2020). It is commonly assumed that the degree of visibility of a medical condition is directly associated with mental health problems in children with visible differences. However, results in the literature are variable (Feragen & Stock, 2016). It has been suggested that the relationship between visibility and mental health problems follow an inverted U shape, with individuals with minor or major visibility experiencing less stress (Moss, 2005). Additionally, parent-reported or child-reported subjective visibility of a child’s medical condition may be a more appropriate indicator of a child’s emotional and behavioral problems than clinician-reported visibility of a child’s medical condition (Moss, 2005; Feragen et al., 2010).
Children develop within the broader context of their family. Parents may also be emotionally affected by having a child with a visible difference (Gee et al., 2020). In turn, parental emotions may influence emotional and behavioral problems in their children. For example, children of parents with psychopathology have an elevated risk for developing psychiatric symptoms (Wesseldijk et al., 2018). Similarly, parenting stress is associated with increased parent-reported emotional and behavioral problems in children with CL ± P or IH (van Dalen et al., 2021). On the other hand, parental positive affect promotes child development (Stifter et al., 2020).
Additional medical difficulties could also play a role in emotional and behavioral problems of children with CL ± P or IH (Hoornweg et al., 2009; Feragen & Stock, 2016). Infantile hemangioma may be life- or function-threatening during infancy, obstructing vital organs and causing feeding difficulties (Léauté-Labrèze et al., 2017). Feeding problems in infants can impact parent–child interaction and indirectly contribute to infant mental health (Tyler et al., 2013). At school age, speech problems and academic problems in children with CL ± P, such as learning disability, low academic achievement, and grade retention, are also associated with emotional and behavioral problems (Wehby et al., 2014; Feragen et al., 2017).
Finally, child behavioral problems vary according to a child’s age, gender, and socioeconomic status (Verhulst & van der Ende, 2013). Parental characteristics, such as parent age and gender, also play a role in the assessment of child emotional and behavioral problems (Achenbach & Rescorla, 2000; Zondervan-Zwijnenburg et al., 2020). Therefore, these variables have to be taken into account as covariates when identifying the association between emotional and behavioral problems and the visibility of CL ± P or IH, parental affect, and condition-related difficulties.
Our aim was to answer the following 2 research questions: Do children with CL ± P or IH experience different levels of emotional and behavioral problems compared to children in the general population? Which factors are associated with emotional and behavioral problems in children with CL ± P or IH?
We expect that parent-perceived visibility of the medical condition, parental affect, and additional condition-related difficulties (ie, feeding problems, eating problems, learning difficulties, and psychosocial problems) are associated with emotional and behavioral problems in children with CL ± P or IH, when corrected for child age, child gender, parent age, parent gender, and socioeconomic status.
Method
This study was part of a larger project assessing parental well-being as described in van Dalen et al. (2021). Ethical approval for this study was obtained from the Medical Ethics Review Committee Erasmus MC, Rotterdam, the Netherlands (MEC-2006-185 and MEC-2008-191). This study was conducted in accordance with the Declaration of Helsinki (World Medical Association, 2013). This article was written in accordance with the STROBE guidelines (Von Elm et al., 2014).
Sample and Procedure
Recruitment took place at the Department of Dermatology in the Centre of Paediatric Dermatology and the Department of Oral and Maxillofacial surgery of the Erasmus MC Sophia children’s Hospital. Recruitment took place from 2008 until 2011, and data were later analyzed and reported in 2019 and 2020 by a PhD student. Parents were included in the study if they (1) had sufficient knowledge of the Dutch language and (2) had a child between 0 and 12 years of age with CL ± P (isolated cleft palate excluded due to the nonvisible nature) or an IH (regardless of the location on the body). This age range was chosen as in the Netherlands children often make the transition to secondary education at age 12. For many parents and their children, this is seen as the end of childhood and the start of adolescence. There were no additional exclusion criteria. For our analyses, children younger than 1.5 years were excluded.
Each family was sent an informed consent letter, 2 questionnaires, and a prepaid envelope. Parents were explicitly asked to fill out the questionnaires independently from their partner. Children did not complete any questionnaires. As an incentive, parents received a small gift for their child. Reminders were sent after approximately 1 month and after 3 months.
Medical Care at the Erasmus MC Sophia Children’s Hsopital, the Netherlands
Cleft care was provided at the [HOSPITAL], [COUNTRY] by multidisciplinary teams with average cleft lip surgery at an age of 3 months and cleft palate closure at an average age of 12 months. The alveolar cleft is closed around 9 to 12 years of age. Access to speech therapy is guaranteed through the treating hospital. Patients are followed up regularly by the multidisciplinary team until age 22.
Medical care for patients with an IH was provided at the Centre for Vascular Anomalies at the Erasmus MC. Treatment (such as propranolol topical/systemic, prednisone, system/intralesional, surgery) was administered to children with IH. All treated IHs were either potentially life-threatening or had functional risk, local discomfort, or severe cosmetic consequences. In case of treatment, follow-up is until the end of systemic treatment. If cosmetic surgery is a suspected possibility, the IHs or its residuals are reevaluated at about age 3.
Instruments
Parent and child demographic characteristics
Demographic and participant characteristics were obtained using questionnaires and included age and ethnicity of children and parents and parental educational level as a proxy measure of socioeconomic status. Parental education was divided into low, middle, and high, based on the International Standard Classification of Education guidelines (CBS, 2011).
Child emotional and behavioral problems
Validated Dutch versions of the Child Behavior Checklist, designed for ages 1½ to 5 (CBCL 1½-5; Achenbach & Rescorla, 2000) and ages 6 to 18 (CBCL 6-18; Achenbach & Rescorla, 2001), were used to assess child emotional and behavioral problems, as reported by parents. The CBCL 1½-5 consists of 100 items and the CBCL 6-18 has 120 items, both scored on a 3-point scale ranging from 0 (not true) to 2 (very true or often true).
For this study, the Total Problems scale and the Internalizing and Externalizing scales were used. The Total Problems scale is the sum of all items. To calculate the Internalizing scale for the CBCL 1½-5, the syndrome scales Emotionally Reactive, Anxious/Depressed, Somatic Complaints, and Withdrawn Behavior were used. For the CBCL 6-18, the syndrome scales Anxious/Depressed, Withdrawn/Depressed, and Somatic complaints were summed. The Internalizing scale measures problems that are present mainly within the child. To calculate the Externalizing scale on the CBCL 1½-5, the syndrome scales Attention Problems and Aggressive Behavior were summed. For the CBCL 6-18, the syndrome scales Rule Breaking Behavior and Aggressive Behavior were summed. The Externalizing scale measures problems with regard to conflicts with others and the conflicts in the expectation others have of the child.
Raw scores can be converted to T scores based on age (and gender for the CBCL 6-18). T scores are normally distributed with a mean of 50 and an SD of 10. T scores of 60 to 63 (84th-90th percentile) are considered borderline clinical range, and scores above 64 are in the clinical range.
Internal consistencies for the scales range from α = .89 to α =.99 (Achenbach & Rescorla, 2000, 2001). In the present study, Cronbach alpha ranged between α = .84 and α = .98 for the CBCL 1½-5 and between α = .86 and α = .98 for the CBCL 6-18.
Parental positive and negative affect
To measure parental affect, the Dutch version of the Positive and Negative Affect Schedule was used (PANAS; Watson et al., 1988). The PANAS consists of the subscales Positive Affect (PA) and Negative Affect (NA). Positive Affect refers to the extent to which a person feels enthusiastic, active, and alert. High scores reflect a state of high energy, full concentration, and pleasurable engagement. In contrast, NA refers to a general dimension of subjective emotional distress and includes a variety of aversive mood states, including anger, anxiety, and disgust. High scores on the NA scale indicate more distress. Both scales consist of 10 items, using a 5-point Likert scale ranging from 1 (very slightly or not at all) to 5 (very much). Parents were instructed to indicate how they had been feeling during the last 2 weeks. Scale scores are obtained by summing the item scores.
The PANAS has good psychometric properties, with α = .89 for PA and α = .85 for NA (Crawford & Henry, 2004). In the present study, Cronbach alphas were α = .89 and α = .85 for the PA and NA scales, respectively.
Visibility
To assess the visibility of the condition, parents were asked two questions, both measured on a 5-point Likert scale: (1) “To what extent do you think your child’s condition is visible?” and (2) “To what extent do you experience that bystanders look at your child’s condition?” (both ranging from “not at all” to “very much”). Item scores were added to derive a total visibility score. The items correlated significantly (r = .59, P < .001), and the scale was reasonably reliable (α = .72).
Additional condition-related difficulties
Three additional questions measured other problems related to the medical condition. Questions were asked on feeding problems (eg, “Does your child have feeding problems?”), speech problems, and learning difficulties. All items were rated on a 5-point Likert scale.
Statistical Analysis
Statistical analyses were performed using Rstudio version 1.3.959 (RStudio Team, 2020). Missing data were handled using multiple imputation. Multiple imputation was performed using the MICE package (van Buuren & Groothuis-Oudshoorn, 2011) in R.
The frequency of scores on the CBCL in the subclinical and clinical ranges was calculated. For children where both parents completed the questionnaires, a Pearson correlation was calculated to assess concordance. Additional analyses were run for parents’ PANAS scores, comparing parents’ scores to normative data. These are reported in the Supplementary Materials.
The first research question was tested using one-sample t tests to compare T scores on the CBCL Total Problems, Internalizing, and Externalizing scales to normative data. The T scores were compared to a mean T score of 50 with an SD of 10. As one-sample t tests do not account for clustering in the data (ie, 2 parents reporting on the same child), separate analyses were conducted for mothers and fathers.
The second research question was tested using linear mixed models (LMMs). In cases where both mother and father participated, there were 2 parent reports for the same child. The LMM account for this clustering in the data, so both parent reports can be analyzed in the same model. Three models were calculated. One for the Total Problems scale, one for the Internalizing scale, and one for the Externalizing scale. Type of condition (CL ± P or IH), parent-perceived visibility of the condition, parental affect, feeding difficulties, speech difficulties, and learning difficulties were entered as predictors. To assess whether visibility was associated with a possible U shape, as described by Moss (2005), visibility was entered into the model with 2 splines. In addition, to test whether the predictors differed depending on the type of condition, an interaction term with condition was entered for all predictors. Child age, child gender, parent age, parent gender, and socioeconomic status were entered as covariates. A model with all covariates was computed, after which a second model was calculated excluding the nonsignificant predictors. Both models were subsequently compared using a likelihood ratio test to assess which model had a better fit to the data.
To account for multiple testing, the false discovery rate method as proposed by Benjamini & Hochberg (1995) was used. All P values were 2 tailed and were compared to α = .05.
Results
Participants
A total of 337 families with a child with CL ± P and 72 families with a child with IH were approached. Four parents with a child with CL ± P and 4 parents with a child with IH indicated that they did not have sufficient knowledge of the Dutch language. The response rate was 45.7% for CL ± P and 34.0% for IH. A total of 357 questionnaires of parents of children older than 1.50 years were returned and analyzed. Detailed sample characteristics are shown in Table 1. Overall, 203 mothers and 154 fathers of 215 children participated. Concerning CL ± P, 40 (22.98%) children had an isolated cleft lip and 142 (78.02%) had a combined cleft lip and palate. Most clefts (N = 137, 75.69%) were unilateral. Concerning IH, 26 children (78.79%) had hemangiomas located on the face or the head, 4 (12.12%) on the face and the body, and 3 (9.09%) on the body. Parents’ concordance between Total, Internalizing, and Externalizing scores on the CBCL ranged from r = .62 to r = .67.
Descriptive Statistics.
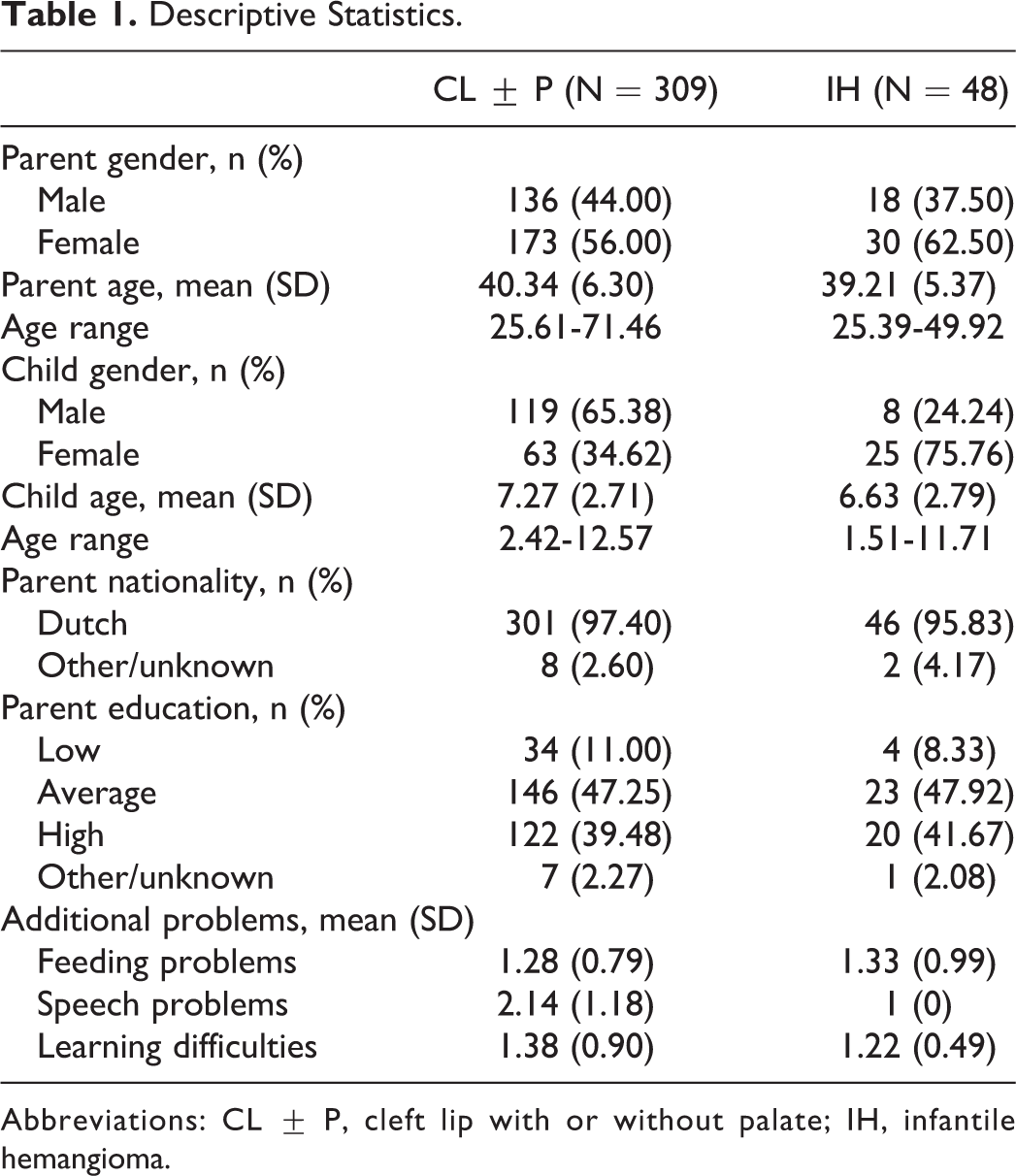
Abbreviations: CL ± P, cleft lip with or without palate; IH, infantile hemangioma.
As seen in Supplemental Tables 1 and 2, all the parents in this study had significantly less negative affect than adults in the norm group. Parental positive affect did not differ from the norm group, except for a small effect size of lower positive affect for fathers of a child with a cleft.
Comparison to Norm Group
Overall, 8.8% to 16.4% of children with CL ± P were rated by their parent as experiencing (sub)clinical problems. In children with IH, this percentage was 0% to 5.6%. The breakdown of children experiencing subclinical or clinical problems is shown in Tables 2 and 3.
Comparison of Children With CL ± P to Normative Data (One-Sample t Tests).
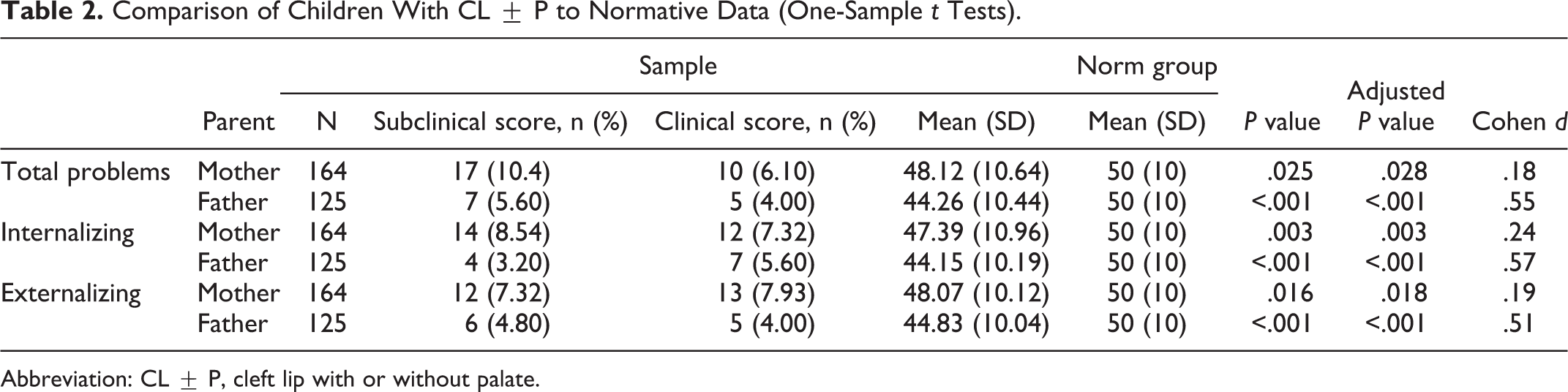
Abbreviation: CL ± P, cleft lip with or without palate.
Comparison of Children With IH to Normative Data (One-Sample t Tests).
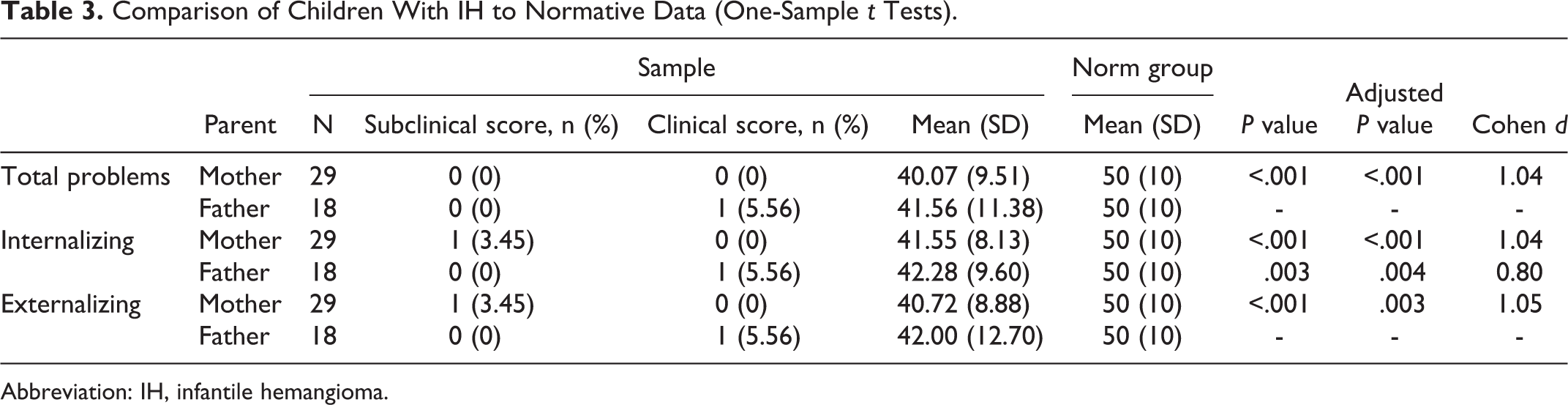
Abbreviation: IH, infantile hemangioma.
To assess whether children with CL ± P or IH experience more emotional and behavioral problems than children in the general population, their scores on the CBCL were compared to the normative data. Results are shown in Tables 2 and 3.
Analyses were not performed for total and internalizing problems for fathers of children with an IH, as these variables were not normally distributed and had a very low N. Nonparametric tests were not performed due to the low N.
Overall, parents of children with CL ± P and IH reported less emotional and behavioral problems regarding their children than parents of children in the norm group. For parents of children with CL ± P, the effect sizes ranged from small to medium (δ = 0.18 to δ = 0.57; Cohen, 1992). For parents of children with IH, the effect sizes range could all be classified as large (δ = 0.80 to δ = 1.05; Cohen, 1992).
Predictors and Correlates of Emotional and Behavioral Problems
To assess what variables are related to the scores for total, internalizing, and externalizing problems, LMMs were computed. For all 3 outcomes, the condition, parental positive affect, child age, child gender, parental age, and socioeconomic status (parental education) did not add significantly to the model. None of the interaction terms were significant, meaning that the type of condition (CL ± P or IH) did not influence the relation between the predictors and the CBCL scores. Results can be seen in Table 4.
Determinants of CBCL Problem Scales Scores: Results of Linear Mixed Models.
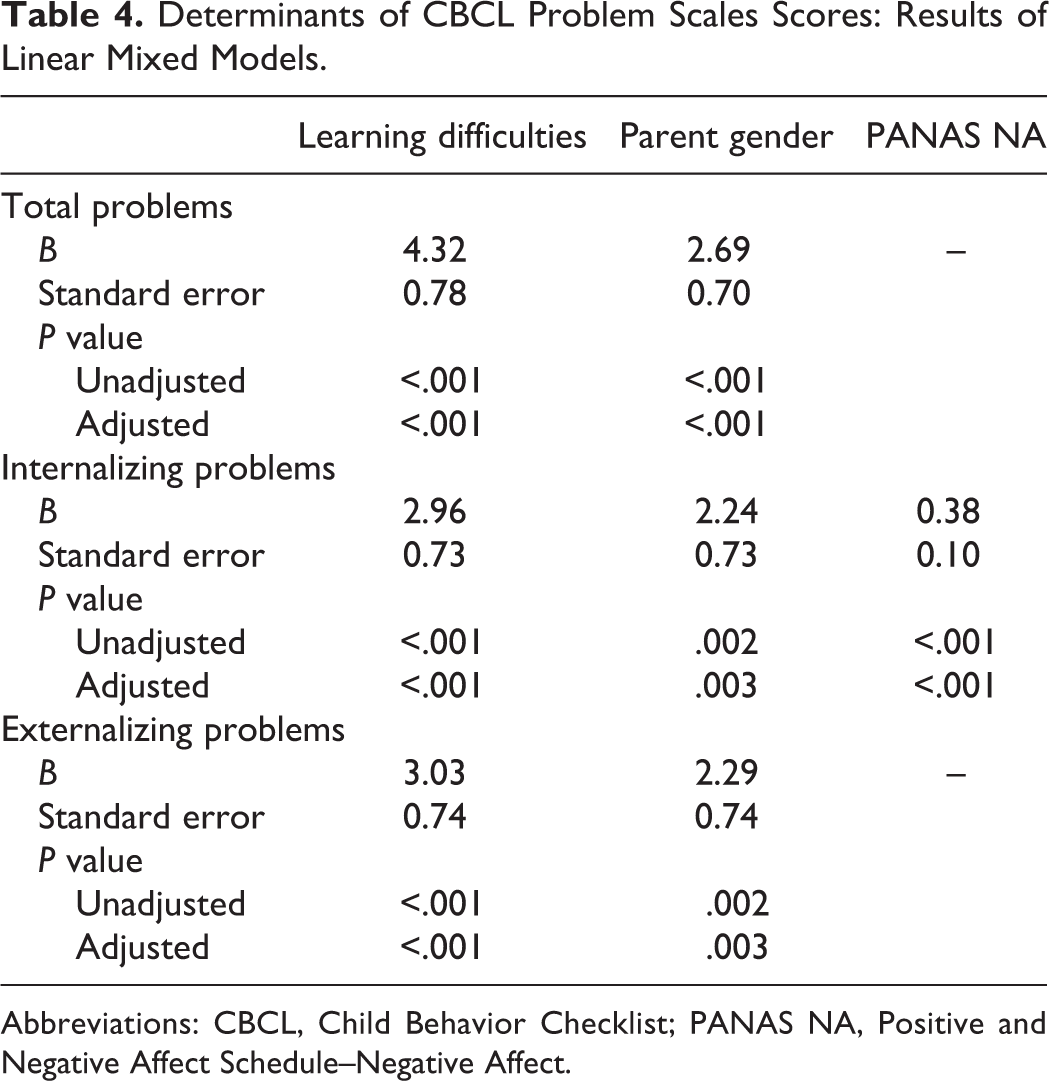
Abbreviations: CBCL, Child Behavior Checklist; PANAS NA, Positive and Negative Affect Schedule–Negative Affect.
The model that best predicted total problems included learning difficulties, t(106.62) = 5.51, P adjusted < .001, and parent gender, t(4126.41) = 3.83, P adjusted < .001. Hence, parents reported more problems when the child had more learning difficulties and when the mother completed the questionnaires.
The model that best predicted internalizing problems included the variables learning difficulties, parent gender, and parental negative affect. Parents reported more internalizing problems for their child when the child had more learning difficulties and when the parent themselves experienced more negative affect. Furthermore, fathers reported significantly less internalizing problems than mothers.
The model that best predicted externalizing problems included the variables learning difficulties, t(352.29) = 4.07, P adjusted < .001) and parent gender, t(20,424.90) = 3.11, P adjusted = .003. Both variables were significantly related to externalizing problems. Hence, parents of children with more learning difficulties and mothers reported more externalizing problems.
Discussion
This study assessed parent-reported emotional and behavioral problems in children with the visible conditions such as CL ± P or IH aged 1.5 to 12 years old. We expected more emotional and behavioral problems in both patient groups when compared to normative data of same-aged peers. Contrary to this expectation, the results of the current study indicated significantly fewer emotional and behavioral problems in children with CL ± P and IH when compared to normative data. In the CL ± P group, 8.8% to 16.4% of children experienced subclinical or clinical problems. In the IH group, this percentage was 0% to 5.6%. As these represent scores in the 84th percentile or higher (Achenbach & Rescorla, 2000, 2001), our sample had less children in the subclinical or clinical range than might be expected.
The current results are inconsistent with findings from some previous studies, which found either no significant differences with norm data (Berger & Dalton, 2009; Brand et al., 2009; Masnari et al., 2013; Stock & Feragen, 2016; Moyakine et al., 2017) or significantly more emotional and behavioral problems in children with a visible difference (Pope & Snyder, 2005; Kenny et al., 2016). The only previous study on Dutch children with an oral cleft found no differences in emotional and behavioral problems when compared to normative data (Hoek et al., 2009). It remains unclear whether children with a visible difference are at risk for experiencing emotional and behavioral problems.
This study’s current findings can be explained in several ways. A first explanation may be that children with CL ± P or IH grow up in a protective environment. Parents may perceive children with a visible difference as more vulnerable, which could elicit a protective parenting style. Such overprotection has previously been shown in a meta-analysis including parents of children with a chronic medical condition (Pinquart, 2013). Appropriate protection may facilitate positive emotional and behavioral development throughout childhood. Nonetheless, appropriate protection also includes a certain amount of autonomy support, which was recently associated with better child quality of life, less externalizing behavior, and less anxiety in a meta-analysis (Crandell et al., 2018). A second explanation is that emotional and behavioral difficulties in children with CL ± P or IH are less prevalent during childhood than in puberty. This may be due to methodological differences between studies, with research in young children often using parent/caregiver reports, while research in adolescent populations often use self-reports. Moreover, body image plays a more prominent role in well-being during adolescence (Smolak, 2012). Indeed, studies have shown that the majority of adolescents in the general population experience body dissatisfaction (Dion et al., 2015). Body dissatisfaction has been linked to negative outcomes such as social anxiety and school avoidance (Vannucci & Ohannessian, 2017) and depressive symptoms (Flores-Cornejo et al., 2017) and could thus play a vital role in the origin of emotional and behavioral problems. Its role in people with a visible difference remains unclear, but there are indications that satisfaction with appearance decreases with age for people with CL/P (Stock & Feragen, 2016). A third possibility is that parents of children with CL ± P or IH may exhibit a response shift. Response shift is a shift in an individual’s perception of health and well-being, which can occur due to potentially challenging circumstances (eg, parenting a child with a visible condition; Sprangers & Schwartz, 1999). Possibly, parents of children with CL ± P or IH have a more positive or a milder perception of emotional and behavioral problems than other parents and evaluate their child’s behavior in a more positive way.
The second research question involved an investigation of factors associated with emotional and behavioral problems in children with CL ± P or IH. Our analyses led to 3 major results. First, learning difficulties and parent gender were related to all emotional and behavioral problem areas (ie, total problems, internalizing problems, and externalizing problems). Second, parental negative affect was associated with the child’s internalizing problems, but not with the child’s externalizing or total problems. Third, parent-reported subjective visibility was not associated with any of the emotional and behavioral problem areas. Lastly, the type of condition (CL ± P or IH) did not influence the relation between the predictors and CBCL scores.
Consistent with our results, learning difficulties have previously been recognized as a risk factor for emotional and behavioral problems and psychopathology (Castro et al., 2020; Visser et al., 2020). In this study, the role of parent gender was similar to the general population, as described in the CBCL manual: Mothers reported more child problems than fathers (Achenbach et al., 1987; Verhulst & van der Ende, 2013). Possible explanations are a different parent–child interaction and differences between the roles of fathers and mothers within the family (Verhulst & van der Ende, 2013; Alakortes et al., 2017).
Our finding that parental negative affect is associated with child internalizing problems can be linked to previous research showing a relationship between parental stress and child emotional and behavioral problems. However, this relationship was not specific to internalizing problems (Spijkers et al., 2013; van Dalen et al., 2021). The association found in the current study may reflect the familial aggregation of anxiety and depression. Although the major source of familial anxiety and depression seems genetic, parenting practices, including parental control, are also related to childhood anxiety (Hettema et al., 2001; van der Bruggen et al., 2008). Theoretical models including social learning theory (Dishion et al., 1994) and attachment theory (Ainsworth et al., 1974) emphasize the role of parenting in child development (McLeod et al., 2007). Furthermore, common method variance may have played a role in the current study. The same informant completed questionnaires about both their parental affect and their children’s emotional and behavioral problems. Parents with a more negative affect could have reported more emotional and behavioral problems in their children. Similarly, parents with internalizing problems are prone to observe internalizing problems in their children (Miller et al., 2020). Any correlations between informants (ie, between the mother and father of the same child) were adjusted for in our statistical analyses.
Concerning the visibility of CL ± P or IH, previous results on the association between visibility of a medical condition and emotional and behavioral problems have been mixed. Possibly, children and parents are used to the always present visible nature of CL ± P or IH. This may not impact functioning as much as repeatedly recurring problems related to the medical condition.
The current study includes some strengths and limitations. Strengths of the current study were the sample size (n = 357) and the number of fathers participating (n = 154). Fathers are often not included in other studies, especially when the target group involves children below the age of 3 (Alakortes et al., 2017). Mothers and fathers each provide a unique view of their child’s development. This unique point of view was highlighted in the current study, in which mothers appointed different scores to their child’s emotional and behavioral functioning than fathers. Hence, multi-informant research is important in obtaining a detailed view of the child’s development.
The current research involved a few limitations. First, this study was limited due to a low response rate of both patient groups (45.7% for children with CL ± P and 34.0% for children with IH). Second, our sample was selected from a tertiary health care center, which could entail more severe cases of IH. Furthermore, our sample mostly involved highly educated parents. Therefore, parents in our study may have access to more resources to help their children with emotional or behavioral problems, compared to a more evenly distributed or lower educated group of families. Third, parents could have been influenced by a social desirability bias and completed the questionnaires to encompass less problems than they actually experienced. However, questionnaires have a lower social desirability bias than other methods such as a face-to-face interview (Bowling, 2005). Fourth, despite requesting parents to complete the questionnaires independently from each other, we cannot guarantee that all parents complied with these instructions, as the questionnaires were completed without supervision of the research team. Hence, some parents could have influenced each other during completion of the questionnaires. Fifth, this study was limited by the lack of a standardized measure of the functional impact of children’s CL ± P or IH diagnosis. Finally, treatment status was not accounted in the analysis.
To address the abovementioned limitations, we advise future research to include children from multiple health care settings, have a representative group of parents across a wider range of educational attainment, gather information about treatment status, and construct standardized measures to capture the impact of diagnoses. Furthermore, qualitative research is needed to assess specific concerns that might not have been addressed in our questionnaires. These studies can also help to indicate what factors, such as parenting style or a response shift, play a role in the etiology of the current findings. In addition, replication across countries and cultures is needed.
In conclusion, this study showed that parents of children with CL ± P or IH report less emotional and behavioral problems in their children compared to the general population. Nonetheless, some children appear to be at risk. These include children with increased learning difficulties and children of parents with heightened negative affect. To identify patients most at risk, we advise clinicians to use screening questionnaires in clinical follow-up. These can be used to offer timely psychological support.
Supplemental Material
Supplemental Material, sj-pdf-1-cpc-10.1177_10556656211031411 - Emotional and Behavioral Problems in Children With a Cleft Lip With or Without Palate or an Infantile Hemangioma
Supplemental Material, sj-pdf-1-cpc-10.1177_10556656211031411 for Emotional and Behavioral Problems in Children With a Cleft Lip With or Without Palate or an Infantile Hemangioma by Marije van Dalen, Mireille M. Hermans, Willem H. Leemreis, Vivian Kraaij, Peter C. J. De Laat, Suzanne G. M. A. Pasmans, Sarah L. Versnel, Maarten J. Koudstaal, Manon H. J. Hillegers, Elisabeth M. W. J. Utens and Jolanda M. E. Okkerse in The Cleft Palate-Craniofacial Journal
Footnotes
Authors’ Note
The data that support the findings of this study are available from the corresponding author, J.M.E.O., upon reasonable request.
Acknowledgments
First, we thank Prof. Dr Oranje, the initiator of the present study who regretfully passed away during the writing of this article. Furthermore, we thank Gerard Madern, Claartje Plaisier, and Ditta van Dijk for their collaboration in the study design and data gathering.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by “Stichting In Face”.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
