Abstract
Assistive technology (AT) and artificial intelligence (AI) are topics that are becoming increasingly important in the context of long-term care (LTC). The literature discusses various so-called intelligent assistive technologies (IATs) in relation to persons with disabilities, people with chronic diseases and people with mental health problems. These technologies aim to improve the quality of life of those affected. The aim of this paper is to provide an overview of IATs used by service users in the LTC sector and to identify emerging issues related to the use of these technologies. To achieve this, a systematic literature review was conducted. The findings show that IATs are increasingly recognized for their role in enhancing quality of life for users and supporting caregivers in LTC, but their deployment raises critical issues such as ethics, privacy, and responsible innovation. The literature highlights the need for updated policies to address technical, regulatory, and practical challenges, while also identifying gaps in long-term impact research and technology integration strategies.
Introduction
The field of intelligent assistive technologies (IATs) in the long-term care (LTC) sector is rapidly evolving, with a focus on improving independence, safety, and quality of life for service users while also supporting caregivers.1–3 IAT is offering significant benefits to persons with disabilities, people with chronic illnesses and people with mental health problems. Examples for IAT include robotic assistants, AI-powered monitoring systems, predictive analytics for health deterioration, and personalized care systems.2,3
IATs have the potential to improve the user’s quality of life. 4 On the other hand, AI-driven health monitoring systems provide real-time monitoring and early detection of health issues, enabling timely intervention and improving user’s outcomes. These systems also enhance communication and collaboration among healthcare professionals, leading to better care coordination and more accurate diagnoses. 5 IATs in LTC integrate smart home systems or ambient assisted living systems that automate lighting, temperature, and movement monitoring to enhance safety and comfort. Wearable devices track vital signs and activity levels, providing real-time feedback to caregivers and health professionals. AI-driven medication management systems ensure adherence by reminding care-users to take their medications and notifying caregivers of missed doses. Communication tools, including voice-activated assistants and smart devices, facilitate seamless interaction between care-users and caregivers. Advanced behavioral and mood monitoring analyses speech, facial expressions, and physiological signals to detect emotional or cognitive changes, enabling timely interventions. Predictive analytics leverage historical data to forecast health issues, allowing for early detection and management. Telehealth solutions enhance remote healthcare through improved diagnostics and care-user monitoring via video conferencing. Robotic assistive technologies aid in physical tasks, promote mobility, and offer companionship, helping to reduce isolation and improve overall well-being in LTC settings. 6
Despite this promising landscape, the rapid expansion and multidisciplinary nature of IAT applications in LTC has resulted in a fragmented body of knowledge, with studies varying widely in focus, methodology and outcomes. A systematic literature review (SLR) is therefore essential to synthesize existing evidence, assess the effectiveness and limitations of current techniques, and guide future research and policy. Therefore, the following paper utilizes a systematic literature review (SLR) to assess ethics and policy (in section 4.1), types of AI-powered ATs in LTC (in section 4.2) and the impact of AI-driven ATs on quality of life in LTC (in section 4.3). The methodology and search strategy for the SLR is described in Chapter 3, results are presented in Chapter 4 and finally Chapter 5 summarizes and concludes the findings.
Methodology and search strategy
The study is based on a SLR using the Population, Intervention, Comparison, Outcome, and Context (PICOC) 7 method for computer science research.7–9 Generally, the SLR is conducted to categorize and compile extensive sources of information on a specific topic. The primary objective of this method is to use the results of the SLR in an analytical manner to address a specific research question. 8
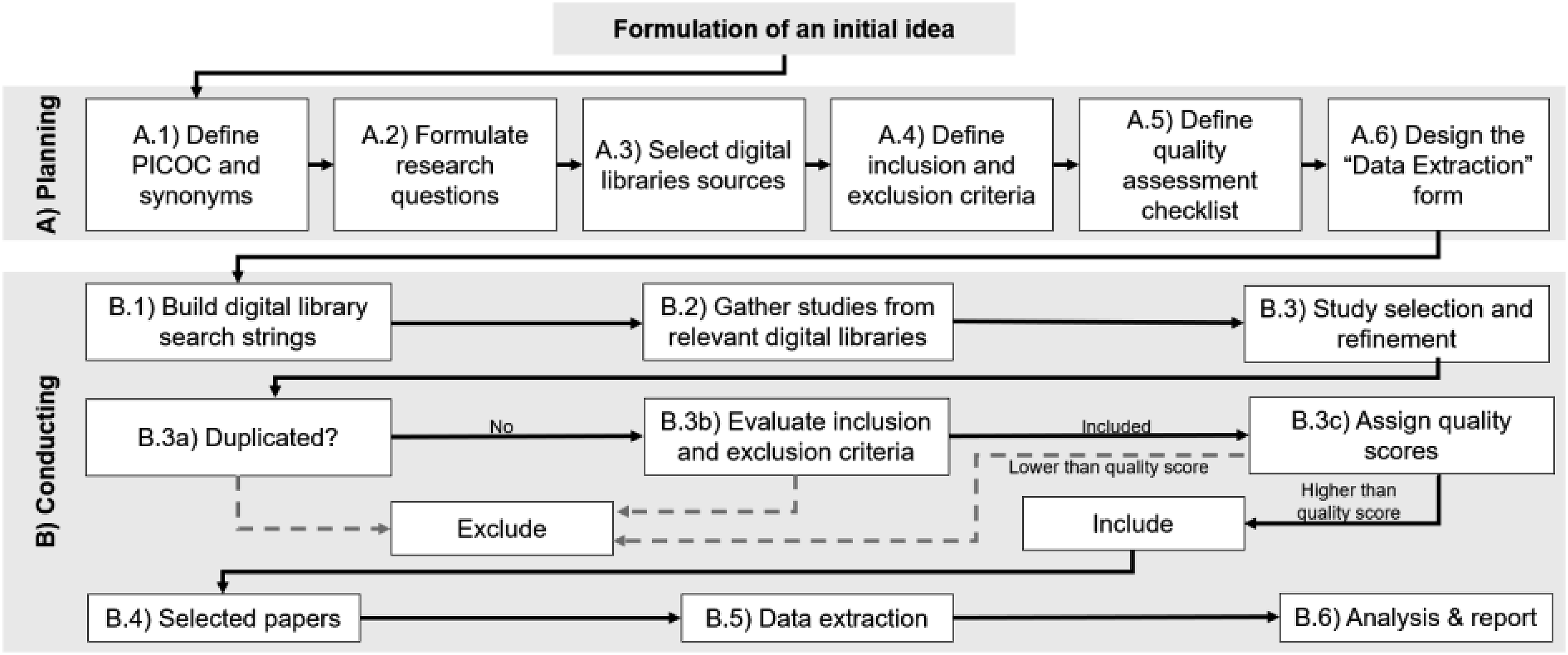
Figure 1 illustrates the process of conducting a SLR using PICOC. Quick guide for computer science research (own representation according to Carrera-Rivera, 2022
7
).
Definition of PICOC keywords and search string(s); source: own presentation.

Search query, source: own presentation.

Based on the PICOC criteria, research questions were formulated. ➢ What types of assistive technologies using artificial intelligence are described in the literature as being used in long-term care for persons with disabilities? ➢ How does the existing literature address the effect/ impact of assistive technologies using artificial intelligence on the quality of life of persons with disabilities in long-term care settings?
Then, a search query was constructed focusing on the topics of LTC and AT using AI, with a special emphasis on persons with disabilities. This SLR follows the guidelines for conducting SLRs in Software Engineering.7,10
Afterwards, appropriate digital library sources such as Web of Science, ACM Digital Library, Springer eBooks Computer Science and IEEE Digital Library were selected. These databases were selected due to their scientific level as well as their access to peer-reviewed and full-text articles in the relevant fields of AT, information and communication technologies (ICT), and LTC. Inclusion and exclusion criteria were established to determine the relevance of studies within the pre-screening phase. Studies published before 2014 were excluded to ensure relevance to current research. For enhanced international traceability only articles written in English were considered, while those in other languages were excluded. Grey literature, including reports, theses, policy documents, unpublished research such as preprints and working papers, editorial material, letters, and magazines, was not included. Studies had to be accessible through databases or institutional resources; those that were not available were excluded. Research had to focus on persons with disabilities in LTC settings, with studies outside this scope being omitted. Then, articles were included or excluded in a further screening based on their abstracts and primary bibliographic information. The Quality Assurance Assessment (QAA) Checklist for final selection evaluated studies based on key criteria to ensure relevance and rigor. The checklist included whether the study discusses limitations and reliability, clearly states research aims, goals, and objectives, and defines research questions. It also assessed the focus on LTC, target groups being persons with disabilities, and whether the study addresses AT using AI, including their evaluation and the user perspective. A distinction between sample sizes, qualitative or quantitative study design, longitudinal studies had not been undergone which may cause a bias in the significance and capacity of results.
Finally, a data extraction form within a spreadsheet was designed to collect relevant information during the review. It was designed to systematically collect and organize key information from selected studies and is divided into several structured sections to ensure consistency in data collection.
In the conducting phase, the process began with the construction of search strings based on the identified keywords and synonyms. Studies were then collected from the selected digital libraries. These studies went through a three-step refinement process. First, duplicate studies were identified and removed. Second, the remaining studies were assessed against the pre-defined inclusion and exclusion criteria to determine their relevance for this study. Thirdly, the quality assurance assessment excluded studies which were not relevant or did not reach the expected quality. The selected studies then proceeded to the data extraction stage, where relevant information was systematically collected using the pre-designed form. Finally, the extracted data were analyzed and the results were reported as part of the review.7,10
Results
The search across the four academic databases initially yielded a total of 943 results. After applying pre-screening criteria, the dataset was reduced to 521 studies. A further QAA was conducted to ensure methodological rigor and relevance, ultimately narrowing the selection to 17 papers for detailed analysis (Figure 2). Search results; source: own representation.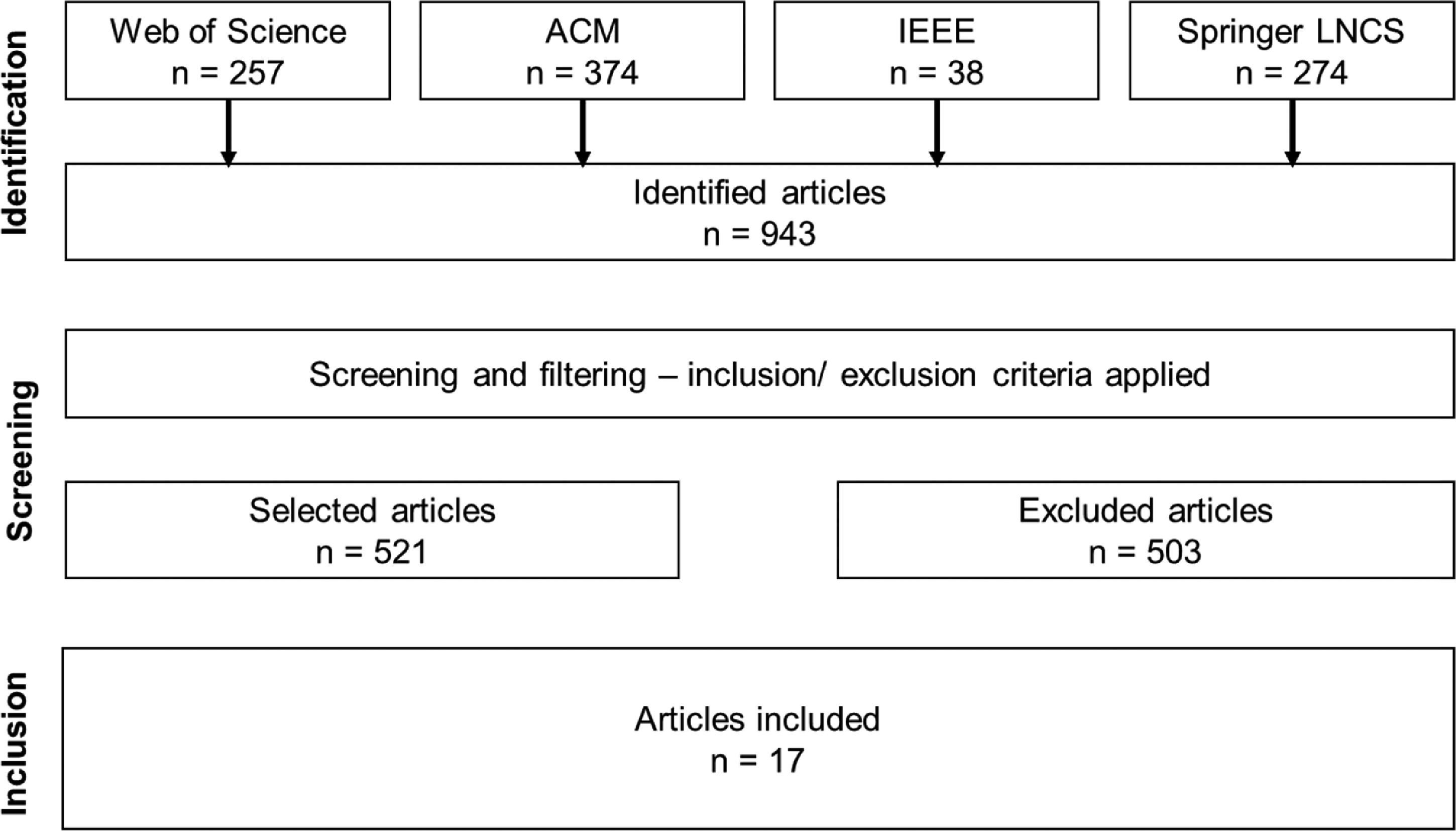
Included studies, source: own presentation.
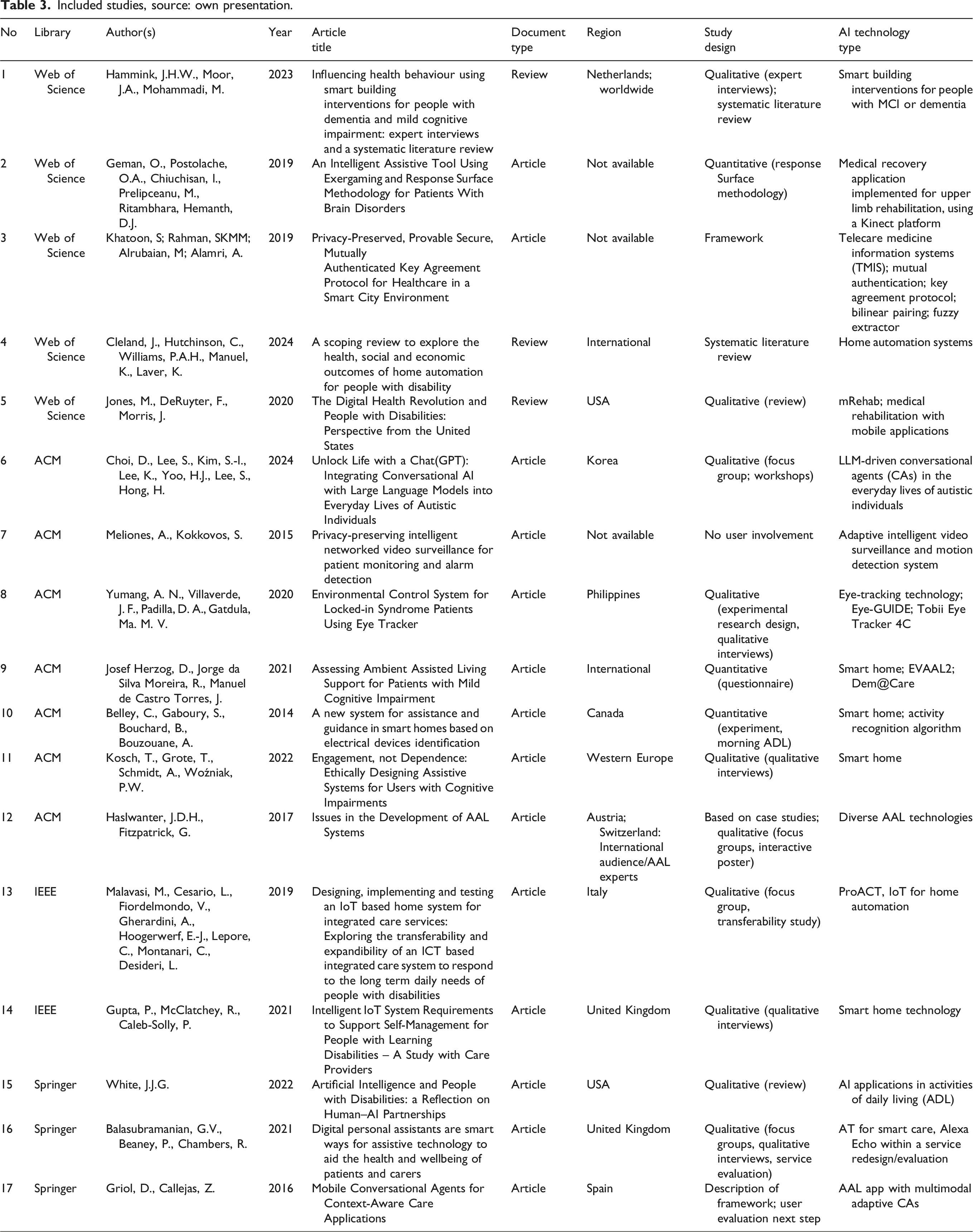
Four results had an international focus, and four were conducted in the form of (systematic literature) reviews. A potential bias within the identified results exists regarding the regional distribution as numerous results focus on Europe. Overall, user groups were diverse, samples relatively small, maybe due to qualitative approaches which can cause a bias related to the significance of findings. The scope of AI presented was wide but targeted within this systematic literature review which aims to present IATs in relation to persons with disabilities, people with chronic diseases and people with mental health problems in LTC. As this is a relatively young topic, small samples and qualitative study designs were expected. Future research with larger samples, selection of further online libraries and enhanced global distribution is desired.
Ethics and policy
The results demonstrate that ethical, regulatory or legal issues had been considered and discussed with LTC and AAL experts.11,12 Privacy and user records are provided by anonymous or unlink-able authentication, key agreement protocols in Telecare Medicine Information System (TMIS). 12 One paper describes in detail how they base their service on frameworks in order to keep ethical, legal and regulatory standards. 13 Studies within an identified literature review describe about increased independence and autonomy because of home automation, yet nothing about ethical or legal standards to support privacy. 14 Interestingly, few papers describe their ethical approach and how their systems are based on legal frameworks. Also, a discussion about privacy of service users has not been a topic in any study identified. Future research and literature reviews should take this into account.
Types of AI-powered assistive technologies in long-term care
The existing literature describes several types of IATs that are applied in LTC for persons with disabilities. These technologies encompass various functions aimed at enhancing independence, communication, and overall quality of life.
Smart homes/ambient assisted living and ubiquitous health supervision
Smart homes and ambient assisted living (AAL) systems including Internet of Things (IoT) environments and ongoing ubiquitous health supervision are facilitated by means of AI which helps to create a seamless and intelligent living environment for users at home, including those with mild cognitive disabilities. 15 The system assists individuals with cognitive disabilities by delivering prompts to support them in daily activities. It evaluates the most effective method for conveying these prompts, choosing between video, verbal communication, or light signals, based on the user’s needs and preferences. 16 Moreover, AI integrates contextual information to optimize system performance within AAL environments. Research conducted in sheltered living facilities indicates that feedback delivered through audible prompts is effective in helping individuals with dementia adjust their Activities of Daily Living (ADL). However, the caregivers’ involvement remains strongly preferred. 17
AI in telecare and smart cities
The concept of smart homes in a smart city environment has evolved from integrating medicine, home automation, and information systems. These smart homes are crucial for developing care-user-centred telemedicine and telecare services. 12
The Telecare Medicine Information System (TMIS) connects healthcare providers with care-users for remote consultations, verifying legitimacy through mutual authentication and biometric data. AI-driven technology enhances smart homes with advanced monitoring, predictive analytics, and personalized care, analysing data to detect patterns, predict health issues, and alert caregivers in real time. 18
A literature review on health, social, and economic outcomes experienced by persons with disabilities using home automation tools emphasizes the potential benefits of these systems. Wearable sensors, in-home environmental monitors, and cloud computing, enhanced by AI, support mobile rehabilitation. AI algorithms combine movement and activity sensor data to provide accurate assessments of individual well-being while receiving mobile rehabilitation. 14
Smart homes, telecare, and privacy
An adaptive, intelligent video surveillance and motion detection system for care-user monitoring and alarm detection can preserve care-user privacy by processing motion information instead of actual images. The intelligent system identifies motion events, stores them, and prevents the cancellation of older records from the database of stored events. The system acts when multiple cameras detect a motion event, facilitating the effective provision of extensive camera networks and integrating a comprehensive application within compact, cost-effective computing devices. 12 Gamification and affordable technology costs are suggested to ease the start with the devices, to intensify practical exercises and the usage rate of mobile rehabilitation applications. At the same time ethical and privacy issues arise when dealing with user data or implementing reimbursement. 13
Assistive technologies using AI for accessibility and independence
IATs enhance accessibility and independence for individuals with disabilities through various applications. Automatic captioning transcribes spoken language into text, improving communication for those who are deaf or hard of hearing. Autonomous vehicles provide mobility solutions for individuals unable to drive, increasing freedom of movement. Image and facial recognition assist those who are blind or visually impaired by identifying environments, persons and key details in daily life. Language generation and AI-based text simplification make information more accessible for individuals with cognitive or learning disabilities by converting complex texts into simpler language. Speech recognition enables users to interact with devices through voice commands, promoting ease of use and independence. Wearable devices equipped with AI support navigation, medication reminders, and emergency alerts, helping individuals manage their daily routines more effectively. 19
Another study focuses on the improvement of accessibility and independence of people with the locked-in syndrome, who are awake and aware but can only move their eyes. An AI application involves developing an AT system that uses eye-tracking data to enable users to control electronic devices and appliances. The core AI component includes processing the eye gaze signals captured by the Tobii Eye Tracker 4C to accurately interpret user intents, such as selecting or turning on/off appliances. The system functions through the integration of computer vision techniques to detect the user’s gaze point on a digital interface, determining which control element—such as a button for a specific appliance—is being fixated upon. To ensure reliability and reduce the risk of unintentional activation, the AI employs decision-making mechanisms that assess gaze patterns using parameters like dwell time and gaze stability. Once an intent is confirmed, the interpreted command is transmitted via wireless communication technologies, such as Bluetooth, to a control module that actuates the desired device function, such as turning an appliance on or off. This approach exemplifies how AI can enhance accessibility and autonomy for users with severe physical limitations. 20
AI in integrated care systems
One paper outlines the design, development, and testing plan for the transferability of the Integrated Technology Systems for ProACTive Patient Centred Care (ProACT) system, an ICT-based solution for integrated care. Initially optimized for older adults with multimorbidity, ProACT aims to support a wider range of users and needs. Multimorbidity increases healthcare use, worsens self-reported health, and reduces functional capacity. AI-driven insights could enhance self-management of chronic conditions. 21 The ProACT system integrates IoT technologies to support integrated care for (older) individuals with multiple chronic diseases, ensuring user-centred design that considers aspirations, needs, and preferences. This approach enhances self-management and independent living among older adults. 22
AI-driven mood and behavioural influence systems
AI-driven systems in smart buildings can influence the mood and health behaviour of people with dementia or mild cognitive impairments (MCIs). Smart floors, smart walls, and smart rooms provide personalized feedback and guidance through visual and auditory cues, aiding individuals in completing daily tasks. These systems offer step-by-step visualizations of activities, improving task completion and independence. However, current literature lacks robust evidence on the effectiveness of smart home solutions in significantly improving health outcomes and behavior in individuals with MCI or dementia. 23
Conversational agents and dialogue systems
IATs can include dialogue systems that enable natural communication between care-users and caregivers, supporting tasks such as medication reminders and emotional support. Chatbots and virtual assistants provide companionship, health-related information, and scheduling assistance. Robotics assist with mobility, daily tasks, and social interaction, while context-aware systems use sensors and AI to monitor environments, detecting falls or unusual activities and alerting caregivers. Cognitive training tools offer personalized exercises to enhance cognitive functions. 24
Conversational agents (CAs) like ChatGPT and other large language models (LLMs) can support people with autism spectrum disorders in, for example, managing daily tasks, handling bullying at school, or addressing anxiety and depression. Voice-based CAs can serve as conversational partners, help users practice conversation, and enhance social interaction. 25
AI-enhanced rehabilitation and exercising-gaming tools
An intelligent exercising-gaming tool has been designed to measure various angles of movement, such as neck, hand, and shoulder inclination, generating a score based on the user’s performance. This score tracks progress in medical rehabilitation, particularly for older people with brain disorders like Alzheimer’s during upper limb rehabilitation. The tool focuses on cognitive stimulation and reducing neurological decline through real-time feedback from sensors measuring limb inclination. AI analyses the collected data, linking it with previous records to predict the rehabilitation process. 4
Assessing the impact of AI-driven assistive technologies on quality of life in long-term care and identified improvements in the literature
The existing literature highlights several ways in which IATs positively impact the quality of life of persons with disabilities in LTC settings.
Enhanced communication and independence
IATs improve communication between care-users and caregivers, creating a supportive environment where individuals can express their needs freely. This reduces isolation and increases overall satisfaction. These technologies also promote independence by automating tasks like medication reminders and personal care routines, allowing users to manage their daily lives with greater autonomy. Emotional support and companionship features help reduce anxiety, as some users feel more comfortable discussing sensitive topics with AI. Cognitive training tools offer personalized exercises that help maintain cognitive functions and delay cognitive decline. Personalized AI-driven care ensures adaptation to individual needs, improving quality of life. 24 AI-driven CAs enhance independence and self-determination by helping individuals manage daily routines, reducing reliance on caregivers. These agents provide emotional support, assist users in handling challenging social interactions, and encourage problem-solving skills. AI-supported CAs can be integrated into LTC environments to offer ongoing personal assistance, helping users maintain autonomy while improving overall well-being. 25 Additionally, AI-driven monitoring systems enhance safety by detecting health risks and alerting caregivers, offering peace of mind to users and their families. 24 Additionally, AAL systems and wearable devices improve safety by continuously monitoring well-being and detecting emergencies, ensuring quick responses. AI-powered communication tools and virtual companions combat loneliness by encouraging social interaction, especially in LTC settings. By analyzing individual health data, AI enables personalized care, leading to improved outcomes and satisfaction. Caregivers benefit from increased efficiency as AI automates tasks and provides insights, allowing for more meaningful interactions. Continuous health monitoring and predictive analytics help detect health risks early, enhancing overall well-being. 6
AI for accessibility: supporting individuals with disabilities through smart technologies
Advancements in AI improve communication for individuals with hearing or speech impairments through automatic captioning and speech recognition, fostering social inclusion. Autonomous vehicles and smart home technologies grant greater independence to those with mobility limitations by reducing reliance on caregivers. AI-powered tools simplify text, offer speech-to-text capabilities, and improve access to information for individuals with cognitive disabilities, enabling active participation in decision-making. Wearable AI systems enhance safety by monitoring health metrics and alerting caregivers in emergencies. AI-driven personalized care interfaces optimize interventions, improving care-user satisfaction. Additionally, AI fosters inclusion by enhancing access to education and job opportunities, improving overall quality of life. 19
Ambient assisted living (AAL) and AI: improving monitoring and personalized care
Caregivers recognize the potential of AI-based AAL to improve care-user monitoring and support. AI-enhanced AAL environments integrate ubiquitous perception, reasoning, acting, communicating, and interacting, enabling real-time assessment of ADLs. By continuously monitoring vital signs, detecting the need for medical interventions, and reminding users about medication intake, AI-powered AAL systems enhance care quality. These technologies contribute to better user support and more efficient caregiver workflows. 17
Smart buildings and assistive environments: supporting health and well-being
Smart buildings featuring smart floors, walls, and adaptive prompts contribute to increased independence, improved sleep quality, and positive user experiences. However, while short-term benefits are evident, the long-term impact remains unclear due to limited studies. Further research is necessary to assess their sustained effectiveness, particularly in adapting to progressive conditions like dementia. Personalization of AI-driven prompts and feedback remains crucial to ensuring usability over time. 23
AI-driven exercising-gaming and cognitive rehabilitation for physical and mental health
Intelligent exercising-gaming tools significantly impact physical rehabilitation by providing engaging and effective home-training solutions. Exercising-games help individuals with motor impairments or neurodegenerative disorders maintain physical activity while tracking progress, increasing motivation, and reducing stress. Similarly, serious games for cognitive stimulation help slow cognitive decline in care-user with neurodegenerative diseases, improving their quality of life. These AI-driven interventions promote active ageing by enabling elderly individuals to participate in social activities, volunteer work, and intergenerational knowledge-sharing, reinforcing their sense of purpose. 4
Summary and conclusion
Assistive technologies using AI are becoming an increasingly important topic in the field of LTC. Numerous articles engage with the subject and emphasize the significance of IATs in enhancing the quality of life for persons with disabilities in LTC.
Nevertheless, ensuring the ethical deployment and use of these technologies is critical to addressing privacy concerns, informed consent, and the autonomy of users. 26 Literature discusses the societal impacts of AI, including the potential for reducing caregiver burden and addressing workforce shortages. Additionally, frameworks and approaches are addressed to ensure responsible innovation in AI technologies, emphasizing key principles for ethical AI deployment, stakeholder involvement, and ensuring transparency and accountability.2,3 Additionally, AI-based situation-aware AT is discussed as counselling systems, referring to the users’ flexible decision-making processes, a combination of flexibility features, environmental aspects, and the users’ physical and cognitive resources. 27
Challenges and barriers to the implementation of IAT are addressed by literature, including technical, regulatory, and practical challenges. The barriers encompass, for example, costs, interoperability issues, and resistance from caregivers or users.2,3
Policy and regulatory considerations are discussed in literature, highlighting the need for updated policies and regulations to govern the use of AI in LTC. Recommendations for policymakers should aim to support innovation while safeguarding service users’ rights and welfare. Only a few describe on which and how they base their work on the various frameworks. Further gaps in the current literature include long-term impacts, cross-cultural applicability, and technology integration strategies.2,3,13
AI-driven AT are shaping a shift toward more adaptive and personalized care, improving the independence and quality of life for individuals with disabilities in LTC. These innovations leverage AI to enhance ADLs and support needs. However, ethical concerns, including transparency, bias, and autonomy, remain ambiguous, and ensuring privacy and data security is crucial for responsible implementation. Moreover, the literature reflects a promising landscape for AI in LTC, with various improvements that enhance the quality of life for people with disabilities through personalized, engaging, and efficient services. These advancements not only positively affect the individuals receiving care but also alleviate some of the burdens experienced by caregivers and health professionals. 24
AI applications have the potential to greatly enhance the lives of individuals in LTC by improving accessibility, assisting with ADLs, and fostering greater independence. By enabling more personalized and responsive support, these technologies can contribute to better quality of life and well-being. However, their development and implementation must carefully address ethical concerns, such as privacy, bias, and user autonomy, while ensuring they meet the diverse needs of individuals in care settings. 6
The literature highlights that the design and implementation of these AI technologies must prioritize ethical and legal considerations, user-friendliness and the active involvement of people with disabilities/users in the development process in order to fully realize their potential benefits. The improvements identified encourage continued research and innovative approaches to ensure that AT make a positive contribution to the lives of people in LTC. 19
To conclude, IATs are emerging as a vital and transformative force in LTC, with a growing body of literature highlighting their potential to improve the quality of life for persons with disabilities. These technologies have the potential to offer personalized, adaptive and efficient support, promoting greater independence and reducing the burden on carer-givers and healthcare providers. However, the successful deployment of IATs depends on addressing key ethical, legal and practical challenges – including privacy, informed consent, user autonomy, cost and interoperability. The literature consistently calls for responsible innovation frameworks that prioritize stakeholder engagement, transparency and accountability. In addition, updated policy and regulatory frameworks are needed to ensure ethical implementation while fostering innovation. Despite promising developments, significant gaps remain, such as understanding long-term impacts, ensuring cross-cultural applicability, and effectively integrating technologies into care systems. To fully realize the potential of AI in LTC, ongoing research and inclusive design practices must ensure that technologies are developed with and for the users they are intended to support. Ultimately, the way forward is to balance technological advancement with ethical responsibility to create meaningful, equitable and sustainable improvements in LTC.
Footnotes
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work has been carried out as part of the Care4Skills project under the Erasmus+ programme. The project is funded by the European Union under proposal number 101140263, within the framework of the call ERASMUS-EDU-2023-PI-ALL-INNO (Partnerships for Innovation – Alliances). The content of this publication reflects the views of the authors only, and the European Union cannot be held responsible for any use which may be made of the information contained therein.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data are available from the corresponding author upon reasonable request.
