Abstract
Many African Americans experiencing serious illness rely on their faith or spirituality to navigate the complex systemic inequities of the United States healthcare system. Yet, African American patient's faith affirmations, beliefs, and spirituality are seldom explored or understood by their clinicians. Despite the urgent need to improve palliative care utilization by this underserved and understudied patient demographic, limited research has been performed to operationally define and quantify how religious belief and/or spirituality affect medical decision-making in African American patients. While a literature search for a tool to measure the concept of African American religiosity or spirituality in medical decision-making produced no results, this review examines three valid and reliable instruments, the DUREL, the RBEC, and the FACIT-Sp-12, that palliative care clinicians and researchers may adapt or supplement with Patient Centered Outcome Research developed items to investigate the influence of faith, spirituality, and religious belief in medical decision-making within the African American patient population.
Keywords
Introduction
Many African American adults have not benefitted equitably from recent advances in medicine and in the field of palliative care. They are more likely to be diagnosed with chronic disease at earlier ages than whites, less likely to have their chronic illnesses managed as well as whites and are more likely to suffer from poorer health outcomes throughout their lifespan until they die (Aaron et al., 2021). These inequitable outcomes are indicative of a healthcare system that still struggles with the long legacy of systemic racism (Macias-Konstantopoulos et al., 2023). As a result, many African Americans, 97% of whom believe in God or a higher power that is intimately involved in their lives (Mohamed et al., 2021), rely on their faith or spirituality to navigate the toxic stress produced by the inadequate access to timely and responsive care, racist interactions, and unconscious bias they often encounter while pursuing treatment (Aaron et al., 2021). African American patients’ reliance on their spirituality and the resilience they achieve through their spiritual orienting systems and spiritual coping strategies remain understudied and underappreciated by palliative care clinicians and researchers despite the guidelines that govern their practice (Siler et al., 2021).
The National Coalition for Hospice and Palliative Care's Clinical Practice Guidelines for Quality Palliative Care's fifth and six domains outline the need for providing culturally relevant care that is cognizant of and responsive to patient's spiritual, religious, and existential concerns. However, African American patient's faith affirmations, beliefs, and spirituality are too often dismissed, ignored, and seldom understood (Gazaway et al., 2023) by clinicians who are less likely to offer person centered communication and less likely to provide care consistent with their expressed preferences (Ashana et al., 2022).
While researchers and clinicians often lament the relative underutilization of palliative care treatment modalities in favor of inpatient intensive care by African American patients experiencing serious illnesses during the last six months of life as compared to whites (Aaron et al., 2021), little research has been conducted into how a clinician's understanding of African American spirituality or religious belief may contribute to better patient-provider communication and goal concordant care at end of life (EOL) (Siler et al., 2021). Since the voices of African Americans are often silenced in healthcare settings, research on how spiritualty and/or religion affect African American patients’ end-of-life decision making is critical (Siler et al., 2021). The use of valid and reliable tools to measure decision-making is especially important when capturing the views of underrepresented groups (Calvert et al., 2022): even more so when exploring aspects of religion and spirituality. Thus, the focus of this paper will be on reviewing measurement tools appropriate for developing a better understanding of the influence of spirituality and/or religion in medical decision-making in African American populations.
Literature Review
Ethical Considerations
Palliative care clinicians and researchers must uphold the core ethical principles of “anonymity, autonomy, confidentiality, consent, privacy, and risk” (Buchanan & Hvizdak, 2009, p. 37) when designing and conducting surveys. This methodological mandate becomes especially important when interrogating the historically marginalized older African American patient population concerning such sensitive issues as the influence of faith and spirituality in end-of-life medical decision-making. The fundamentals of Patient Centered Outcome Research (PCOR) demand that investigators (Carpenter et al., 2021) involve stakeholders in both study design and implementation. Researchers must also consider the particular vulnerability of palliative care patients as so-called “captive audiences” (Raudonis, 1992 as cited in Addington-Hall, 2002, p. 221) and make every effort to reduce the physical and/or cognitive burden of participation by utilizing clear, concise, and brief survey instruments and recruiting patient family members—caregivers who can speak to the patient's experience when they are unable.
Palliative care researchers must be prepared for the potential psycho-spiritual and emotional burdens associated with their survey topic(s) even during the participant recruitment phase. Recruitment media should inform prospective participants that their participation is completely voluntary, highlight the potential risks and benefits of participation and outline any other pertinent information to afford informed consent. The dissemination of this and other descriptive information concerning the study's treatment rationale may burden and discomfort prospective participants. An offer of supportive services should therefore be included with all recruitment media for those experiencing existential distress due to the sensitive nature of the survey's focus.
Ultimately, the potential for harm due to the sensitive nature of the influence of African American religion and spirituality in the context of complex medical decision-making and EOL concerns should not deter researchers from engaging in this important work. Researchers should anticipate the possibility that survey participants may become distressed while completing the survey because they are asked to reflect on their experience of illness, disease progression or encounters with their palliative care or other medical providers. Researchers can mitigate these negative outcomes by first engaging African American stakeholders in survey design, then by avoiding misleading information or intentionally embarrassing questions and finally by utilizing culturally sensitive and respectful language that does not convey bias. This stakeholder participation will undoubtedly contribute to the development and appropriate use of a well-developed, reliable, and valid measurement tool.
Importance of Reliable and Valid Tools
A reliable and valid measurement tool must demonstrate stability of measurement, across intervals and between different observers, while consistently measuring what it claims to measure. The ability to operationally define and quantify an abstract construct like how religious belief and/or spirituality affects medical decision-making in African Americans can only be inferred from observations of behaviors, practices or phenomena that are thought to serve as indicators of it (Kimberlin & Winterstein, 2008).
Methods
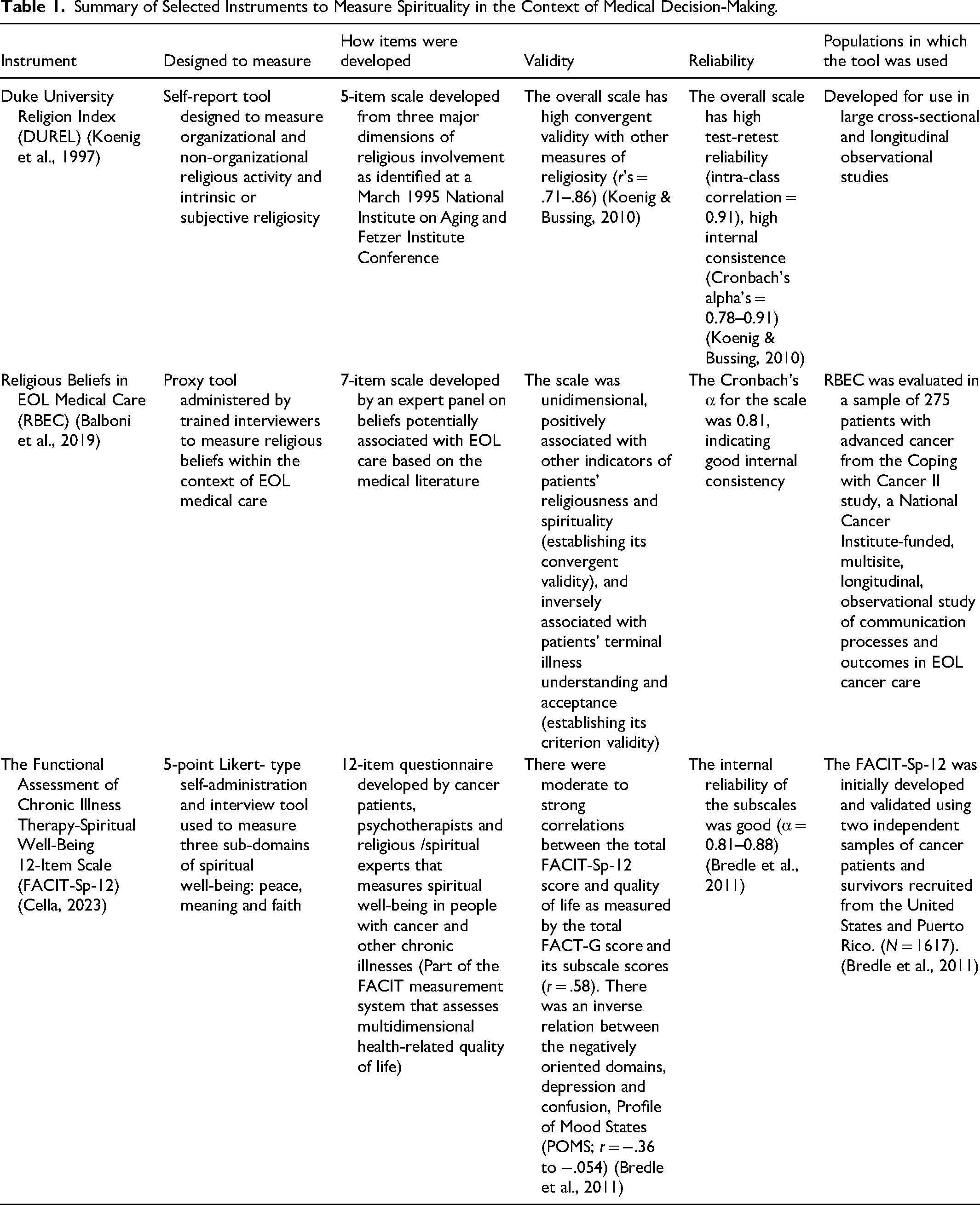
An initial search of PubMed, Google Scholar, and CINAHL was conducted during September 2023 using the Boolean/Phrase search mode of the terms (“African American religiosity,” “African American spirituality”) AND (“measurement,” “measure,” “tool,” “survey”) AND (“medical decision-making,” “medical decisions”). No results emerged for a tool to measure the concept of African American religiosity or spirituality in medical decision-making. However, several tools that measure patient religiosity/spirituality emerged once the racial identifier African American was removed from the search parameters. The inclusion criteria were articles that reported on or psychometrically tested quantifiable measures of spirituality, religiosity, faith, or belief preferably in the context of medical decision-making. The exclusion criteria were publications not written in the English language. Three tools were selected for review based on relevance to the role of spirituality in the context of medical decision-making. None of the instruments were specifically designed for African Americans. Refer to Table 1 for a summary of the tools selected for this review.
Summary of Selected Instruments to Measure Spirituality in the Context of Medical Decision-Making.
Findings
Duke University Religion Index (DUREL)
The DUREL was developed by Koenig, Parkerson, and Meador in 1997 to provide a comprehensive, brief, non-offensive, low-burden measure of an individual's religious involvement, activity an individual participates in as an expression or celebration of what they consider sacred or divine, readily available for easy inclusion in large cross-sectional and longitudinal studies (Koenig & Bussing, 2010). The 5-item questionnaire was developed to measure three different dimensions of religious involvement as determined by a consensus meeting of National Institute on Aging researchers in 1995. These measured sub-scales are organizational religious activity (ORA), non-organizational religious activity (NORA), and intrinsic religiosity (IR). ORA consists of public religious activities such as attending religious services or participating in other organized activities such as group prayer or group scripture study. NORA consists of individual religious activities such as meditation, private prayer, private scripture study, watching religious television, or listening to religious radio. IR involves pursuing religion as an ultimate end in itself as opposed to possible extrinsic motivations such as financial gain, social status, or social interaction. The first 2 items of the index, ORA and NORA were taken from large National Institutes of Health (NIH) community and clinical studies conducted in North Carolina. The ORA and NORA subscales are each 1-item Likert-type measures where respondents are asked to select one of the six following measures of frequency: (1) Never; (2) Once a year or less; (3) A few times a year; (4) A few times a month; (5) Once a week; (6) More than once a week. The IR subscale is a 3-item Likert-type measure of intrinsic value taken from the 10-item Hoge IR scale. Respondents are asked to select one of the five following measures of agreement: (1) Definitely not true; (2) Tends not to be true; (3) Unsure; (4) Tends to be true; (5) Definitely true of me. The overall scale has high test-retest reliability (intra-class correlation = 0.91), high internal consistence (Cronbach's α = 0.78–0.91), and high convergent validity with other measures of religiosity (r's = 0.71–0.86) (Koenig & Bussing, 2010).
Each subscale is intended to serve as an independent measure; therefore, the summing of all subscales into a total religiosity score is not recommended by its authors because multiple collinearity between subscale scores could interfere with accurate estimate of effects for each subscale. Also, the combining of all three subscales could result in subscale scores canceling out the effects of each other. The DUREL was developed to measure religiosity in Western religions and may not provide as accurate an assessment of religiosity in Eastern religious traditions (Koenig & Bussing, 2010). However, researchers have assessed the DUREL in varying contexts and 20 languages, providing evidence of strong cross-cultural measurement invariance despite the representation of many different religions (Toscanelli et al., 2022).
Religious Beliefs in EOL Medical Care (RBEC)
The RBEC was developed, introduced, and evaluated to assess patient's religious beliefs within the context of EOL cancer care (Balboni et al., 2019). The 7-item measure was developed by an interdisciplinary research team of experts with varying backgrounds in causal methods, EOL care, epidemiology, measure development, oncology, palliative care, psychosocial oncology, religion and spirituality. The team did not engage patients or any other stakeholders in the development of the tool but based its formulation on a thorough review of pertinent medical literature. The research team sought out to capture seven beliefs within four thematic constructs of religious belief associated with influencing EOL medical decision-making: (1) God's sovereignity; (2) the sanctity of life; (3) miracles; and (4) sanctification through suffering (Balboni et al., 2019). The seven beliefs were measured by study participants indicating their degree of agreement with the following statement on a 5-point Likert-type scale: To what degree do you agree with the following statement? (1) not at all; (2) a little; (3) somewhat; (4) quite a bit; and (5) a great deal. The research team assessed patient illness understanding and the study participants were also asked to characterize their religiousness and spirituality using questions from the Multidimensional Measurement of Religiousness/spirituality for Use in Health Research.
The 275 initial study participants were recruited from a National Cancer Institute funded prospective cohort of the Coping with Cancer II Study between November 2010 through April 2015 from the outpatient facilities of nine cancer centers in the United States. The eligibility criteria included being of the white or black race; being aged 21 years or older; having stage IV gastrointestinal, gynecologic, or lung cancer: or oncologist determined incurable or poor prognosis stage III cancers; an oncologist estimated life expectancy of less than 6 months; and disease progression after at least one chemotherapy regimen or, for patients with colorectal cancers, disease progression after two chemotherapy regimens. Patients were excluded if they were determined to be cognitively impaired, were too weak to perform the interview or they were receiving hospice or palliative care.
The mean age of the study participants was 60.1 years (standard deviation, 10.4 years). About 68% were female, 78.2% self-identified as white and 87.6% as non-latino. The largest religious tradition represented was Catholic (40.7%) followed by Protestant (20.4%) and Baptist (16.7%). The Cronbach's α for the scale was 0.81 indicating good internal consistency. A principal component factor analysis of the RBEC scale items, only the first component factor (eigenvalue λ1 = 3.25, variance explained = 46%) had an eigenvalue greater than 1, indicating that underlying RBEC construct is unidimensional and adequately represented by an item sum, or equivalently an item average, aggregate measure. The RBEC scores were found to be strongly associated with patient spirituality, daily spiritual experiences, and spiritual care from religious communities, thereby supporting the scale's convergent reliability.
Functional Assessment of Chronic Illness Therapy-Spiritual Well-Being 12-Item Scale (FACIT-Sp-12 -Version 4)
The FACIT-Sp-12 was developed in the 1990s by health outcomes researcher David Cella. It is one of the many subscale measures that comprise the FACIT system which evolved from Cella's Functional Assessment of Cancer Therapy (FACT) measure (Bredle et al., 2011). Each of the FACIT system questionnaires were developed and created with input from patients and clinicians. The FACIT Sp.-12 is a 12-item Likert-type questionnaire designed for the exploration of three subscales of spiritual well-being: meaning, peace, and faith in patients experiencing chronic illness. Each subscale measurement consists of four interspersed statements for each of which respondents are asked to indicate their degree of agreement when recalling the prior seven days by circling or marking one of the following: (0) Not at all; (1) A little bit; (2) Somewhat; (3) Quite a bit; (4) Very much. The survey was initially developed for self-administration at a fourth grade reading level. Unlike the DUREL and RBEC developers, the FACIT Sp.-12's developers specified that it can be completed by interview when necessary to reduce patient burden (Bredle et al., 2011). It has been translated from English into 39 other languages, has a 23-item expanded version, FACIT-Sp-EX, as well as palliative care, FACIT-Pal, and non-illness, FACIT-SP-NI, related measures. The FACIT system is copyrighted and available for licensure through the FACIT website: https://facit.org. The FACIT-Sp-12 was initially validated using two independent samples of 1617 mostly cancer patients and survivors recruited from the United States and Puerto Rico (Bredle et al., 2011). The first study's participants were administered the FACIT-Sp-12 and other health related and quality of life measures (HRQOL). The internal reliability of the subscales was good (Cronbach's α = 0.81–0.88). There were moderate to strong correlations between the total FACIT-SP-12 subscale score and the other HRQOL instruments, including the FACT-G scale (r = .58), Vigor domain of the Profile of Mood States (POMS) (r = .42), and the negatively oriented domains of the POMS: Depression and Confusion (r = −.36 to −.54). The second study analyzed data from 131 participants in a larger study investigating fatigue and HRQOL in patients beginning chemotherapy. Internal validity was comparable to the first study and the FACIT-Sp correlated moderately to strongly with the Cancer Patient Behavior Survey Satisfaction with Religion (r = .25), Spiritual Beliefs Survey (r = .48), and four other measures of spiritual well-being and religion thereby supporting the scale's convergent reliability.
Discussion
Understanding how religion and or spirituality influence medical decision-making is an integral part of providing culturally sensitive and patient-centered communication and care (Balboni et al., 2019). While only one of the measurement tools, the RBEC, specifically identifies how a patient's religious or spiritual beliefs may influence their medical decision-making, all three provide palliative care clinicians and researchers with valid and reliable means of capturing their patient's religious or spiritual beliefs. This is an essential first step in developing an understanding of how these beliefs may influence their African American patient's medical decision-making. All three measures have been developed through collaborative interdisciplinary efforts, have demonstrated reliability and validity, and, when used as a starting point for further investigation, can offer insights into the interplay between religion, spirituality, and medical-decision-making; yet only one, the FACIT-SP-12, involved patients in the initial stage of its development. This commitment to the principles of PCOR through which patients, who have a vested interest in a clinical decision and the evidence that supports that decision, participate in a measure's development (de Forcrand et al., 2021), likely contributed to the FACIT-Sp-12's strong psychometric properties, eventual translation into 39 different languages and widespread acceptance as a non-biased instrument capable of measuring meaning, peace, and faith in diverse religious and cultural contexts. While PCOR principles certainly offer a pathway to establishing content validity through the reflections and critical analysis of patients as participant stakeholders, there are no formal empirical tests for content validity and therefore no substitute for the contribution of subject matter experts.
The subject matter experts who contributed to the development of the FACIT-Sp-12 were focused exclusively on the spiritual well-being of patients experiencing chronic illness as a component of health-related quality of life (Bredle et al., 2011). The measure's original factor analysis does, however, substantiate faith as an integral component of spiritual well-being. In doing so, and because of its widespread adoption, the FACIT-SP-12 allows researchers interested in the role of religion and spirituality in medical decision-making to capture pertinent data that allows for normative comparisons with many other populations (Switzer et al., 1999). In the same manner, the DUREL can serve as source of pertinent data for normative comparisons having been translated into 20 languages and validated in 27 nations as of 2022 (Toscanelli et al., 2022).
The DUREL's three dimensions of religious involvement, ORA, NORA, and IR subscales, were determined by a consensus of subject matter experts on aging. Motivated by what they considered a lack of well-designed and theoretically grounded studies on the religion-health relationship (Koenig & Bussing, 2010), the DURELs developers emphasized brevity in the measure's 5-item design to assist epidemiologists conducting cross-sectional longitudinal studies with a brief measure capable of identifying the three dimensions of religiosity, ORA, NORA, and IR, of their study subjects.
Using a pragmatic approach in the measures’ development, the researchers leveraged two existing survey instruments as resources from which they gleaned the 5 items after conducting thorough psychometric analyses. The 3 items measuring IR were adapted from Dean Hoge's 10-item IR Scale and ORA and NORA were taken from NIH studies (Koenig & Bussing, 2010). While some may be challenged to accept the plausibility of 1-item subscales, ORA and NORA were established 1-item measures that had been widely adopted at the time of their inclusion. A more robust criticism is justifiably made of a development process that abandoned any pretense of supporting PCOR principles by circumventing any patient participation whatsoever. However, the DUREL's high test-retest reliability, internal consistence, and convergent validity demonstrate its utility as a brief, comprehensive, and easily used measure of religiosity (Koenig & Bussing, 2010). Subsequent researchers have not only validated the measure in 27 cultural contexts, but they have demonstrated psychometric support for using an aggregate total score of the 3 items when measuring health outcomes in diverse cultural contexts despite the original authors’ admonition against doing so (Toscanelli et al., 2022). This psychometrically validated use of an aggregate score may offer researchers additional motivation for using such an invaluable tool for measuring the role of spirituality in African American's medical decision-making; first, because of the measures ability to quantify three vital components of religiosity and/or spirituality individually and in the aggregate; second, because of the measure's brevity; finally, because of its validation with religions and cultural contexts far beyond the Western theological bias (Koenig & Bussing, 2010) that informed its development. Despite these quality attributes, there is only one instrument developed by clinicians and subject matter experts for the explicit purpose of measuring the influence of religious beliefs in medical decision-making: The RBEC.
The RBEC's developers relied on the clinical and research expertise of the professionally diverse panel of experts who designed it. These experts hypothesized that religious beliefs in end-of-life care would be related to patient religiousness, daily spiritual experiences, and spiritual care from religious communities (Balboni et al., 2019). They further hypothesized that patients who strongly endorsed RBEC would have lower levels of terminal illness understanding. The latter determination was based on previous associations of lower rates of terminal illness acknowledgement with a patient's degree of religious coping (Balboni et al., 2019). But the researchers did not engage patients during the measures’ development to evaluate their assumption concerning the relatedness of illness acknowledgement and illness understanding. The researchers acknowledged the potential influence of religious communities in deterring hospice enrollment and raising the incidence of more intensive medical interventions at EOL, but they did not engage religious communities when designing the measure. These omissions, a failure to engage patients and religious communities, are indicative of a failure to embrace PCOR principles. In addition, the decision to exclude hospice and palliative care patients from participating in the initial study of an instrument designed to assess religious beliefs solely in the context of end-of-life medical care may further limit the measures adoption by palliative care clinicians and researchers. First, the absence of PCOR principles in its design may cause some to question the face validity of the measure despite its relatively strong psychometric values of internal consistency and convergent and criterion validity and next it may be of limited use for those investigating the influence of religious beliefs in medical decision-making upon diagnoses or during earlier stages of disease progression.
Conclusion
While each of the measurement tools reflect the value and efficacy of the interdisciplinary processes that contributed to their development, they measure what they are intended to measure in a reliable manner, they also reflect a cultural bias within the medical research community. Only one of the measures’ development reflected an inclusive approach to research design according to PCOR principles. Further, the available literature provides no indication that any investigation has been performed to determine whether the measures were culturally relevant or resonant with African American patients. Despite the evidence illustrating the significance of spiritual orienting systems, spiritual coping strategies and religious beliefs in African American culture (Siler et al., 2021), the instruments designed to measure these outcomes may not be entirely valid and/or reliable for this subset of the population due to the lack of stakeholder participation in development. Ultimately, until the influence of faith, spirituality, and religious belief in medical decision-making within the underserved African American patient population becomes the focus of more clinical research investigation, palliative care researchers must adapt or supplement the available psychometrically validated instruments with PCOR developed, culturally relevant and resonant items to improve provider understanding and patient-provider communication in medical decision-making.
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
