Abstract
This study examined the functional relation between the Teach-Model-Coach-Review (TMCR) instructional approach and Brazilian parents use of Enhanced Milieu Teaching with Phonological Emphasis (EMT-PE) strategies with their child with nonsyndromic cleft palate. A single-case multiple baseline across behaviors experimental design replicated across three parents was utilized. The Teach-Model-Coach-Review approach was applied to teach EMT-PE strategies (use of speech and language targets within balanced turns, use of speech recasting and/or language expansions, and use of communication elicitation procedures). The intervention was short term (2–3 months) and delivered in an in-person and hybrid in-person + telehealth model. Children’s expressive language outcomes were measured, and social validity data were collected. A functional relation between the TMCR intervention and parent’s use of EMT-PE strategies was found for the three dyads. All children showed improvement in their expressive language. Parents reported that the intervention approach was effective. Brazilian clinicians rated the approach as culturally valid.
Around one in 1,000 children globally are born with an oral cleft (cleft lip, cleft palate, or cleft lip and palate; Salari et al., 2022). A meta-analysis found that children with nonsyndromic cleft lip and/or palate (NSCL/P) in the United States have lower expressive and receptive language skills and are more likely to present with speech production difficulties when compared with their peers without NSCL/P (Lancaster et al., 2020). These differences are likely to persist throughout early childhood and are greater for younger children (i.e., 2-year-olds with NSCL/P are further behind their peers than 8-year-olds with NSCL/P). Children in Brazil with NSCL/P are similarly impacted. In one study, 48% of 4- to 5-year-old children with NSCL/P in Brazil were identified as at risk for language delays, and 15% showed significant expressive and receptive impairments when compared with a sample of children without NSCL/P (Jurado et al., 2021). Another study, examining the language development of younger children, found that children aged 12 to 36 months with NSCL/P in Brazil had significantly lower expressive and receptive language skills than their peers without NSCL/P (Lamônica et al., 2016).
Early intervention is effective and recommended for children with clefts to monitor for disordered speech, increase children’s speech sound repertoire, and support early vocabulary development (Kaiser et al., 2017; Scherer et al., 2021; Scherer & Kaiser, 2007). Children with NSCL/P present with speech sound disorders at a higher rate than their typically developing peers (Hardin-Jones & Jones, 2005). A smaller subset of these children develop cleft-related speech errors (e.g., glottal stop substitutions), and the majority develop phonological errors (Hardin-Jones & Jones, 2005; Lien et al., 2023). Speech and language development are deeply interconnected, with each domain influencing the other in a reciprocal relationship. Speech development impacts language acquisition, and language development in turn influences the phonemic inventory (Lien et al., 2023; Scherer et al., 2021).
Two studies have demonstrated the benefits of Enhanced Milieu Teaching with Phonological Emphasis (EMT-PE) delivered by a speech-language pathologist (SLP) on children’s speech and language outcomes for children under 3 with NSCL/P (Kaiser et al., 2017; Scherer et al., 2021). Enhanced Milieu Teaching (EMT; Kaiser & Hampton, 2017) uses environmental arrangement, responsive interaction strategies, language modeling and expansions, and prompting procedures to elicit communication. In addition, for children with NSCL/P, the intervention includes a PE in which language modeling specifically focuses on targeted speech sounds and includes recasting as a responsive strategy (Kaiser et al., 2017).
In one small randomized clinical trial in the United States, 19 children aged 15 to 36 months with NSCL/P participated and were randomized to a control group (N = 8) or the EMT-PE intervention group (Kaiser et al., 2017). The intervention was 48 EMT-PE sessions completed at a university clinic in the United States and delivered by an SLP in English. At the end of the intervention, the children who had participated in the treatment group had significantly higher expressive vocabulary as reported by their parents on the MacArthur Bates Communicative Development Inventories (MB-CDIS; Fenson et al., 2007) and higher receptive language on the Preschool Language Scale, Fourth Edition (PLS-4; Zimmerman et al., 2002). In addition, children in the treatment group had significantly less consonant errors on the Profiles of Early Expressive Phonological Skills (PEEPS; Stoel-Gammon & Williams, 2013).
A replicated randomized control trial of EMT-PE in Brazil and adapted to Brazilian Portuguese enrolled 24 children with NSCL/P from 20 to 34 months old (Scherer et al., 2021). In this study, 12 children were assigned to the intervention group and 12 to the control group. The intervention consisted of 24 EMT-PE sessions in Brazilian Portuguese delivered by an SLP in a hospital clinic. At the postintervention testing, children in the treatment group had significantly higher expressive vocabulary on the MB-CDIS adapted to Brazilian Portuguese (Teixeira, 2019) and receptive language on a standardized test (Avaliação do Desenvolvimento da Linguagem (ADL); Menezes, 2004). In addition, children in the treatment group used more words during an observational language sample at posttesting and in a 3-month follow-up. Children in the treatment group had fewer consonant errors in the 3-month follow-up on the PEEPS adapted to Brazilian Portuguese (Scherer et al., 2020). Children in the treatment group were more intelligible at the 3-month follow-up based on parent report on the Intelligibility in Context Scale (ICS; McLeod et al., 2015). Importantly, neither of these studies included a parent coaching component; the intervention was solely implemented by therapists in a university or hospital clinic, directly with the child.
Application of Parent-Implemented Early Language Intervention in Brazil
During the early years, parents and other caregivers serve as children’s language teachers by structuring children’s experiences and their environment (Adamson et al., 2020). Thus, many early intervention approaches are delivered as parent-implemented interventions via parent coaching. The “Teach-Model-Coach-Review” instructional approach (TMCR) has been utilized in various studies (e.g., Peredo et al., 2022; Roberts et al., 2014; Roberts & Kaiser, 2015). Two randomized control trials of this approach have demonstrated effectiveness on children’s receptive and expressive language for English and Spanish-speaking children in the United States with developmental language delays (Peredo et al., 2022; Roberts & Kaiser, 2015). In addition, English-speaking parents applied and maintained EMT-PE strategies with their young children with NSCL/P when taught the strategies via telehealth using TMCR (Philp et al., 2021).
To our knowledge, given the novelty of early intervention and parent coaching in Brazil, no other studies or programs have systematically coached parents to support their young children’s speech and language for children with NSCL/P. Parent coaching might be especially relevant in Brazil and other Latin American contexts. Latin American parents report a desire to be involved in their child’s intervention and to be taught how to apply strategies at home (DuBay et al., 2018; Hampton et al., 2022). Furthermore, in a study of 350 Brazilian mothers of children 3 and under, mothers reported that providing their child with stimulating opportunities and talking a lot to their child was of great importance (Viera et al., 2010). Given the variability in the developmental trajectory of speech and language for children with NSCL/P, for some an early, efficient, parent-implemented intervention could ameliorate early differences in language and academic outcomes; for others, this approach can be an initial early intervention approach to bridge to ongoing and clinician-based longer-term intervention.
Current Study
This study utilized an experimental single-case multiple baseline across behaviors design (Gast et al., 2018) to test the initial effects of teaching Brazilian parents to implement EMT-PE with their toddlers with NSCL/P. A systematic coaching protocol (TMCR) was utilized to teach parents how to apply EMT-PE strategies with their child. The following research questions were addressed: (a) Is there a functional relation between the TMCR intervention and parent’s increased use of EMT-PE strategies with their child with NSCL/P? (b) Do parents continue to use these strategies in a similar but uncoached book and play context? (c) Are there changes in children’s expressive language over the course of the intervention? (d) How do parents and providers judge the acceptability and effectiveness of the approach?
Method
Study procedures were approved by the research ethics committee at the university hospital in Brazil, where the study was conducted, and data analysis and sharing were also approved by the IRB at the first author’s home institution.
Experimental Design
A single-case multiple baseline across behaviors within a parent (Gast et al., 2018) replicated across three parents was utilized. The single-case experimental design focuses on within-subject comparisons and allows for systematic individualization of the intervention for the parent based on the child’s developmental needs.
Participating parents were taught three sets of EMT-PE strategies independently from each other in a time-lagged fashion, where the next set of strategies was introduced once the parent showed a stable increase in the use of the targeted behavior. Sets of EMT-PE strategies taught to parents are described in detail in Table 1. They were (a) use of phonological targets and other language targets in balanced turns, (b) use of recasting and/or expansions, and (c) use of communication elicitation strategies (nonverbal choice, question asking in books). All baseline, generalization, and intervention sessions were video recorded, coded, and graphed in GraphPad Prism v10 (GraphPad Software, LLC, 2023) for visual analysis. Two parents received the intervention in a hybrid (in person + telehealth model) and one parent received the intervention fully in person. Differences in delivery approach were based on parent preferences and the need for accurately capturing speech sounds. The study budget limitations did not allow for proper audio equipment to capture child speech sounds via telehealth.
EMT-PE in Brazilian Portuguese Strategies.
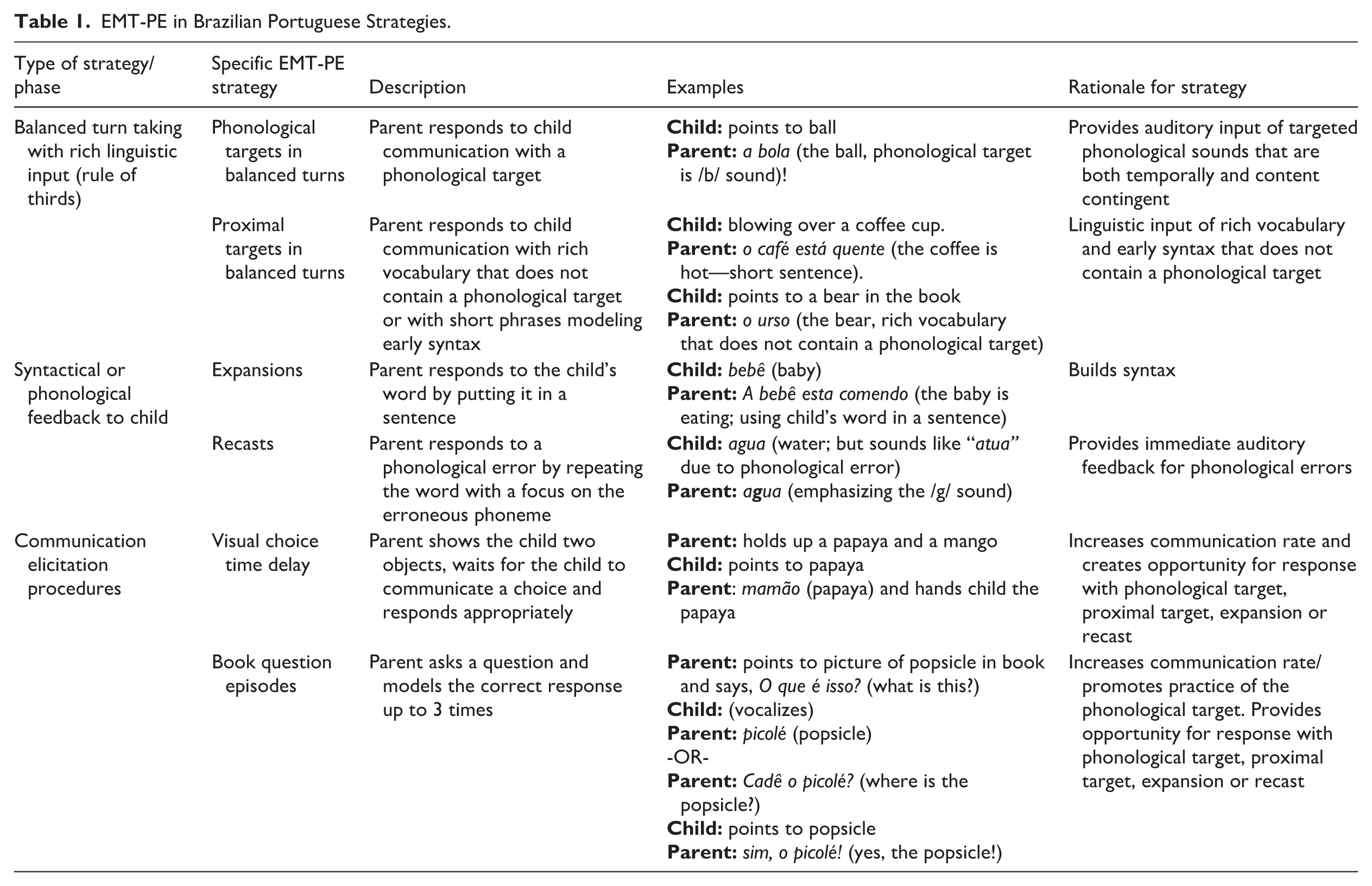
Participants
Participants were recruited via email from the hospital database. Interested parents received a phone call to discuss the study and were consented in person during the first visit. Three parents participated in the study. They were eligible to participate if they had a child between 20 and 36 months old at the time with a cleft palate (with or without cleft lip) and were concerned about their child’s speech and/or language. Parents had to be willing to participate in biweekly sessions to learn and practice the intervention strategies. The child needed to have had their palatoplasty completed by 18 months of age and be showing delays in their speech and/or language acquisition. Children under 3 were selected because the strategies in this early intervention approach are designed for children who are acquiring early vocabulary through early syntax. The strategies have been shown to improve speech and language outcomes in Brazilian children in this age range with cleft palate when delivered by an SLP (Scherer et al., 2021). Standard recommendations in Brazil are for palate repairs to be completed between 12 and 18 months, (HRAC-USP, 2018), thus, we aimed to enroll children who followed this typical trajectory and not those with more intensive health care needs.
All three participants were Brazilian mothers. Participant 1 had a doctoral level of education. She was in her mid-30s. Her daughter was an only child who was born with a cleft lip and palate and was 21 months old at the time of the study. They lived in a two-parent household as a nuclear family. Participant 2 had the equivalent of a high school education. She was in her early 40s. She lived in a multigenerational household with her mother-in-law, her husband, and two children. Her son was born with a cleft palate and was 26 months old at the start of the study. Participant 3 was in her early 40s and had the equivalent of a college degree. She also lived in a multigenerational household with her two children, her husband, and her mother. Her daughter was born with a cleft palate and was 31 months old at the time of the study.
The three children in the study were representative of the broader population of children with NSCL/P with varying speech and language abilities. One child had a mild to moderate receptive and expressive language delay, one child had severe receptive and expressive language delays, and one child had no language delays but significant phonological errors. Child characteristics are summarized in Table 2.
Child Characteristics.
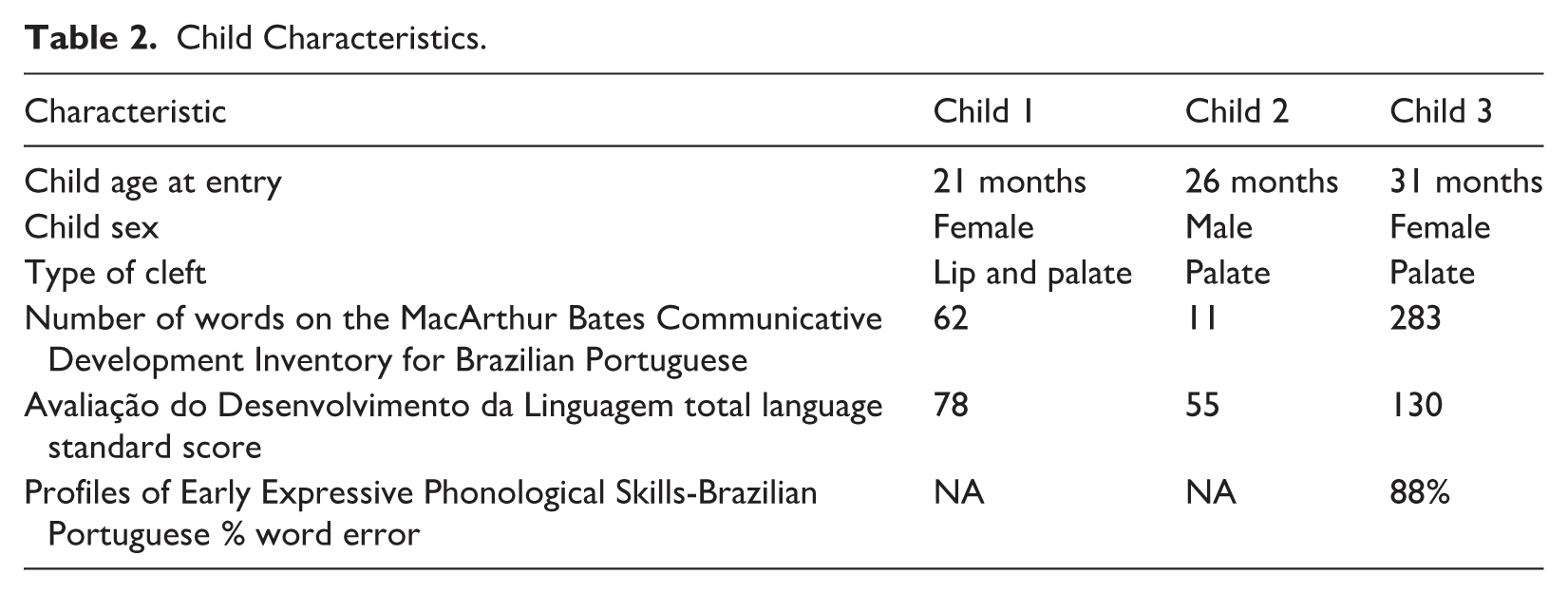
Setting and Materials
Sessions occurred in a hospital clinic and in participants’ homes via telehealth. Toys and books were utilized during the sessions. For the visits in the clinic, five books were chosen based on the following criteria: the books contained at least three opportunities for vocabulary with the phonological targets per page; the books were developmentally appropriate and engaging for young children (e.g., including sensory component, song lyrics, and simple story lines); the topics/storyline aligned with Brazilian culture and they were written by Brazilian authors or translated to Brazilian Portuguese (Bibo na Praia by Silvana Rando (2012a), Bibo no Mercado by Silvana Rando (2012b), O Pato by Vinicius de Moraes (2023), Pintinho um livro-squeaky by Mammoth World (2022), Baleia na Banheira by Susanne Straber (2020)). Five Brazilian clinicians, including the first and last author, reviewed the books for cultural relevance and appropriate speech and language targets. Toys included a ball, a playhouse, dolls, food and cooking utensils, cars, and trucks. For telehealth sessions, the coach and parent selected similar materials (dolls or stuffed animals, blocks, pretend foods, and vehicles) and books the child had in the home. All families had materials available to them.
Description of the Intervention
EMT-PE strategies adapted to Brazilian Portuguese (Scherer et al., 2021) were taught to parents using the TMCR approach (Roberts et al., 2014). During the “teach” component, the coach explains the strategies that will be targeted for the session and the rationale for each strategy. In “model” (5 min), the coach demonstrates how to use the strategy with the child and narrates what she is doing for the parent (video examples and role-plays with the parent are used in telehealth). The parent practices the strategies with the child with guided feedback from the coach for 8 min during “coach.” Finally, during “review,” the parent and coach discuss how the session went and plan for the next practice. Parents were taught strategies (see Table 1) in three phases. All sessions were conducted by a parent coach who is Brazilian and a native speaker of Portuguese (first author). The coach is a doctoral-level developmental psychologist with over 15 years of experience and expertise in language intervention, parent coaching, and EMT strategies.
Procedures
Baseline, intervention, generalization, and maintenance sessions were video recorded and coded for dependent variables (described in detail in measures).
Baseline
Baseline sessions occurred in the clinic over 2 days, along with the administration of assessments. The visit lasted between 30 and 45 min, with the baseline sessions lasting 8 min each. The participating parent was told to interact with the child for 8 min with a set of toys and books. The parent was asked to spend 2 min interacting with books. The coach did not provide any feedback during the interaction. Each family completed three baseline sessions because all showed a stable trend in their data for the targeted intervention behaviors. It was important to move families on to the intervention phase both practically due to the coach having limited time in country and ethically to provide families with strategies without a long withholding period.
Intervention Sessions
Participants received the intervention sessions in a rapid coaching model where two cycles of TMCR (independent variable) were completed per session to build on the next strategies to give the child access to the full intervention within a shorter time. Parents 1 and 2 received the intervention in a hybrid model where they began sessions in the clinic in person and then moved to a telehealth format via Zoom (version 5.13.7), and parents were able to practice the strategies in their homes. This decision was made based on family preferences. Parent 1 lived far away from the clinic and Parent 2 did not drive and depended on other family members to take her and her child to the clinic. Based on expert advice, the move from in-person to hybrid happened only after a stable trend in the targeted behavior was observed and never during a phase change (J. R. Ledford, Personal Communication, April 18, 2023). Parent 3 received all sessions in-person and in the clinic. Parent 3 lived close to the clinic, and her schedule allowed for bi-weekly sessions in the clinic.
In the first phase, all three participating parents were taught to increase their use of phonological targets (i.e., words containing specific targeted speech sounds for each child) in balanced turns. This was the behavior in which phase change decisions were made. In addition, parents were also taught proximal targets (i.e., rich vocabulary that did not contain a phonological target or short sentences) in balanced turns and to reduce their use of nontarget/nonbalanced language (i.e., questions, behavioral directions, talking without pausing). Parents were taught to balance their linguistic input to the child by attending to the “rule of thirds” where one-third of the time they should aim to use a phonetic target in balanced turn, one-third of the time they should aim to utilize a proximal target in a balanced turn, and the remaining third they can use other language such as questions, directions, words of affect, playful sound effects or songs. In the second phase, Parent 1 and Parent 3 were taught expansions and recasting. Parent 2 was taught communication elicitation procedures (time delay choice, and receptive book question) in Phase 2. Child 2 was not using words consistently yet in Phase 2, so his mother was taught these strategies to increase his rate of communication and give her more opportunities to model target-level language. Expansions and recasting are not appropriate strategies for children who are not consistently using words because these strategies require repeating the child’s word or putting it in a sentence. In Phase 3, Parent 1 was taught time delay choice and book questions, Parent 2 was taught book questions, and Parent 3 was taught expansions. Child 1 could benefit from both types of elicitation procedures to practice her phonological targets. Child 2 had begun using around five words in the 8 min sessions during Phase 2 which made it appropriate to teach his mother expansions in Phase 3. He was not showing any phonological errors in the early words he produced, so recasting was not taught. Child 3 was a high-rate communicator and consistently used specific words and phrases in requesting, so time delays would not be an effective strategy for her. She did benefit from the question asking sequence in books which allowed her up to three opportunities to practice specific phonological targets and gave her mother an equal number of opportunities to recast or expand.
Strategies were introduced at the beginning of each phase in an individualized 15-min PowerPoint workshop which explained how to use the strategy, the rationale for the strategy, and showed video examples of the strategy use in Portuguese with Brazilian children with NSCL/P. Each in-person cycle of TMCR lasted about 20 min (5 min review of strategies, 5 min of modeling, 8 min of coaching, and 2 min of review). The 8 min of coaching during each cycle were utilized for collecting and monitoring data on the participating parents’ use of EMT-PE strategies. Families received two cycles of TMCR per visit so each visit lasted about 45 min.
Generalization and Maintenance Sessions
Generalization and/or maintenance sessions were uncoached and lasted 8 min. Parents were instructed to attempt to engage their child with a book for at least 2 min of the interaction and use the remaining time to play like they normally would with toys. The procedures for maintenance sessions were identical to generalization sessions; however, maintenance sessions occurred about one month after the coaching sessions concluded.
Treatment Fidelity
Treatment fidelity on 30% of randomized sessions of the parent coach’s implementation of TMCR procedures was rated from videos by a master’s student with native fluency in Spanish and understanding/conversational skills in Portuguese. She was trained on the EMT-PE specific scripted explanations of strategies. The first author was available to translate if there was any portion of the coaching video she did not understand; however, there were no instances of this happening. The student research assistant was not involved in the study in any other way. The fidelity checklist included the following items: (a) coach asks parent how practicing the intervention strategies at home is going; (b) coach explains strategies and rationale for strategies to be practiced (scripted); (c) coach asks parent if she has any questions; (d) coach helps parent set up the environment to optimize child engagement (e.g., face to face, limiting distractions); (e) parent–child coached interaction lasts exactly 8 min; (f) coach provides at least four instances of specific coaching/guided feedback during parent–child interaction; and (g) coach summarizes how the parent used the targeted strategies in the session. The parent coach’s adherence to TMCR procedures ranged from 91% to 100% and averaged 97%.
Descriptive Measures
Demographics Survey
All participating parents completed a demographics and child health history survey. Demographic information collected in this survey included participating parents' relationship to the child, parents' educational level, parents' occupation, and household composition. Child health history information collected included prenatal and birth history, birth weight and height, type of cleft (palate and lip or palate only), hearing screening results, history of ear infections, any other health-related concerns, and child therapy history.
PEEPS:BP
The Profiles of Early Expressive Phonological Skills (PEEPS; Stoel-Gammon & Williams, 2013) is a play-based measure of phonological features for children 18 to 36 months old. The PEEPS was adapted to Brazilian Portuguese (PEEPS:BP) for use with Portuguese-speaking Brazilian children ages 18 to 36 months (Scherer et al., 2021). The goal of the PEEPS:BP is to descriptively assess speech production skills to identify children who may need to be referred for early intervention services and for treatment planning. The assessment includes 36 commonly acquired early words with a variety of Brazilian Portuguese consonants across all places, voice, and manner categories of sound production, and with different syllable structures.
The first author administered the PEEPS:BP. During the administration, the child was allowed to select different toys/materials from a bin one by one that contained items/toys for the targeted words (e.g., a toy house for the target “casa”). The child was given an opportunity to spontaneously label the item, and after a few seconds, the parent coach would say, “What is it?.” If the child still did not name the object, two other prompts followed in hierarchical fashion including a model “It’s an X” with a pause and a direct say prompt, “Say X.” The assessment was phonetically transcribed from video by a Brazilian fourth/final year speech-language pathology student at the university in which the study was conducted. This yields a consonant inventory and percent correct consonant (PCC). Scoring was verified by the third author, a doctoral-level cleft specialized certified SLP in Brazil.
Avaliação do Desenvolvimento da Linguagem [Evaluation of Language Development]
A language assessment for early language development in Brazilian Portuguese, the ADL (Menezes, 2004), was utilized. This is a play-based norm-referenced assessment that yields raw and standard scores in receptive language, expressive language, and total language (M = 100; SD = 15). It was the only available language measure in Brazilian Portuguese for children in this age range and has been utilized in other studies with this population (e.g., Scherer et al., 2021). The test was administered by a fourth-year speech-language pathology student who was previously trained in the assessment.
MacArthur Bates Communicative Development Inventories
The MacArthur Bates Communicative Development Inventory adapted for Brazilian Portuguese (Teixeira, 2019) is a vocabulary checklist of over 500 early words in Brazilian Portuguese-speaking children. Parents checked off all the words their child utilized (understands and says).
Parent Perception of Intervention (Social Validity Survey)
Parents completed a survey of their perception of the intervention after their last intervention session. The survey was completed online via a Vanderbilt REDCap (Harris et al., 2009) link. Survey questions included (a) what part of TMCR parents thought was most helpful in their learning of the strategies, (b) was the coaching time sufficient for them to learn the strategies (c) did parents teach EMT strategies to another family member/parent, (d) if the parent practiced EMT strategies in other routines besides play and book and if so which one/s, (e) how many hours weekly did the parent estimate practicing the strategies with her child, and (f) did the parent think the intervention helped their child and if so how.
Clinician Survey (Social Validity)
SLPs and students at the hospital where the study was conducted were invited to a presentation of TMCR and EMT-PE. After watching the presentation, professionals used a QR code to access a REDCap survey. The brief survey asked: (a) In your opinion, is early speech and language intervention important for children with cleft palate? (b) In your opinion, are the EMT-PE strategies culturally appropriate for Brazilian children? and (c) In your opinion, is TMCR culturally appropriate for Brazilian caregivers? Response options were yes, no, and not sure.
Dependent Variables
All dependent variables were coded from videos following a code developed for this study by the first and second authors (both fluent in English, Spanish, and Portuguese); the second author is an SLP who specializes in clinical treatment for children with clefts. The SLP was naïve to the parent phase of parent training. She transcribed parent and child utterances in Excel and rated them for the behaviors described below. A total count or ratio of each behavior was calculated from the Excel datasheets and graphed for visual analysis (code available by request).
Phonological Targets in Balanced Turns
Information from the PEEPS:BP assessment was utilized in choosing the phonetic targets for Child 3. Results from the PEEPS:BP revealed a phonological disorder with frequent fronting of velars /g/, /k/ to alveolar-dental /d/, /t/. In Brazilian Portuguese, stops /d/, /t/ are typically acquired by age 3;0 with the phonological process of fronting eliminated by 3;0 to 3;5 (Ceron et al., 2017; Martins et al., 2021). While Child 3’s receptive and expressive language skills were not impacted, she was judged to be unintelligible by both familiar and unfamiliar speakers. In addition, her velar fronting was pervasive at an age where some remaining errors might be considered typical, but not at the frequency observed within her speech. Based on results of the PEEPS:BP, the decision was made to address targets /g/, /k/ throughout the intervention period.
Children 1 and 2 did not attempt any of the prompts on the PEEPS:BP, which is unsurprising given their small lexical repertoire at baseline. For these two children, early emerging sounds for Brazilian Portuguese were chosen as their phonetic targets (i.e., /p/, /b/, /t/, /d/, and /m/).
The parent’s use of single words that contained the phonetic target which was either (a) in response to child communication or (b) descriptive of what the child and parent were doing were considered balanced targets. A total count of utterances that were both balanced and contained a phonetic target was used as the variable monitored to determine when to change phase.
Proximal Targets in Balanced Turns
Proximal targets were single words that did not contain phonetic targets and short sentences that were in response to child communication or descriptive of what the parent and child were doing together. A total count of utterances that were both balanced and contained a proximal target was analyzed.
Nontarget/Unbalanced Language
Examples of utterances that were considered nontarget and/or unbalanced included: (a) when the parent took more than two consecutive conversational turns without pausing to give the child an opportunity to take their communication turn; (b) use of questions and behavioral directions (play directions were considered balanced and target if they were contingent with what the parent and child were doing together); and (c) making sound effects, singing, counting, reciting the alphabet. A total count of unbalanced and/or nontarget language was utilized in the data analysis. A decrease in this behavior was the aim of the intervention.
Expansions
Expansions were phrases used by the parent that contained the child’s word and were temporarily contingent responses. For example, the child says “abelha [bee]” while pointing to a picture of a bee in a book and the parent responds with “a abelha está voando [the (feminine/singular) bee is flying].” Expansions were coded as a ratio of expandable utterances made by the child to correctly expanded by the parent and graphed as such. Utterances by the child that contained a phonetic target with a phonological error were not considered expandable, as a speech recast described below would be the most appropriate response.
Speech Recast
A speech recast was a temporarily contingent response by the parent repeating the child’s word which contained a phonological error while emphasizing the omitted or erroneous speech sound. Importantly, the parent was only taught to recast the specific speech sounds that were identified as the child’s phonological targets. Developmentally appropriate phonological errors were not the emphasis for recasting. Like expansions, recasts were coded as a ratio of utterances by the child that contained a phonological error of a targeted sound to correctly recast responses by the parent.
Communication Elicitation Strategies
Communication elicitation strategies included a time delay choice in play in which the parent provided a visual choice and waited for the child to communicate by pointing or saying a word. These strategies focus on child requests (e.g., the child wants something) and are more appropriate for play. In books, parents were taught a question episode in which they prompted the child to either receptively identify a phonetic target (“Where is the dog?”) or to use a phonetic target in the book (“What is this?”) in a specific teaching sequence. These prompts are for commenting on vocabulary in the book (e.g., the child does not want the dog in the book, they are commenting/sharing about the book “here is a dog!”). For both types of elicitations, the parent was taught to model the prompted target again if the child did not respond and continue playing/sharing books.
Child Outcome Variables (Secondary, Descriptive Outcome)
Child outcomes were also coded from video of the 8-min parent–child interactions. Only variables that were appropriate for the child’s current speech and language abilities were calculated for that child. Total number of words said in the 8 min interactions and the number of different words (removing any word said multiple times) were calculated for Children 1 and 2 throughout baseline, intervention, and generalization sessions. Correct consonant use for the /g/ and /k/ sounds was calculated for Child 3.
Data Analysis
All data were coded immediately following sessions and graphed utilizing GraphPad Prism v10 for visual analysis of the data. All coded and graphed sessions including baseline, intervention, and generalization lasted exactly 8 min. The first author determined when to change phases based on the visual analysis. In addition, a log response ratio (LRR; Pustejovsky, 2018) was utilized as an effect size index to quantify the magnitude of the functional relation between the TMCR intervention and the parent’s use of EMT-PE strategies. LLRs are used in single-case design studies to quantify functional relations based on the natural logarithm of the proportional change between phases (Pustejovsky, 2018). It is an appropriate effect size index for behavioral observational data expressed as frequency counts or percentages of a behavior. The two versions of LRR are LLRi, where positive values denote improvements and LRRd where negative values denote improvements. An online calculator (https://jepusto.shinyapps.io/SCD-effect-sizes/; Pustejovsky et al., 2023) was utilized to compute these effect sizes. For the behaviors in which parents had a zero or near-zero baseline, LLR was not calculated to avoid reporting inflated effect sizes.
Interrater Reliability
Twenty-nine percent of all sessions were consensus coded by the first author and second author. The second author is a trilingual cleft specialist SLP who was naïve to the training phase. Of the remaining sessions coded by the first author, 13% were randomized and coded for reliability by the SLP. Interrater percent agreement averaged 88.5% to 100% across all coded behaviors. The SLP coded 100% of speech sound productions for Child 3.
Results
Parent 1
Results for Parent 1 are shown in Figure 1. In Phase 1, parent use of balanced turns that contained a phonological target as a total count within 8 min sessions showed a clear shift in level from baseline (range 1–5, M = 3) to intervention (range 13–39, M = 25). Her level of this behavior in baseline was low with minimal variability. Change in level was observed immediately following the intervention and remained stable. The effect size for this behavior was large, LRRi = 1.96 (SE = 0.37). Her use of balanced turns that contained a proximal target also showed a clear increase in level immediately following the introduction of the strategy and showed a slight accelerating trend throughout intervention. In baseline, her use of balanced turns that contained a proximal target ranged from 3 to 8, with a mean of 4 utterances. In intervention, the range was 16 to 64 with a mean of 41. The effect size for use of balanced proximal targets was also large, LRRi = 2.20 (SE = 0.52). A therapeutic decelerating trend in her use of nonbalanced/nontarget language was also observed in Phase 1 from baseline (range 180–208, M = 190) to intervention (range 7–74, M=30), there was also a large effect size of the intervention on this behavior, LRRd = 1.63 (SE = 0.10).
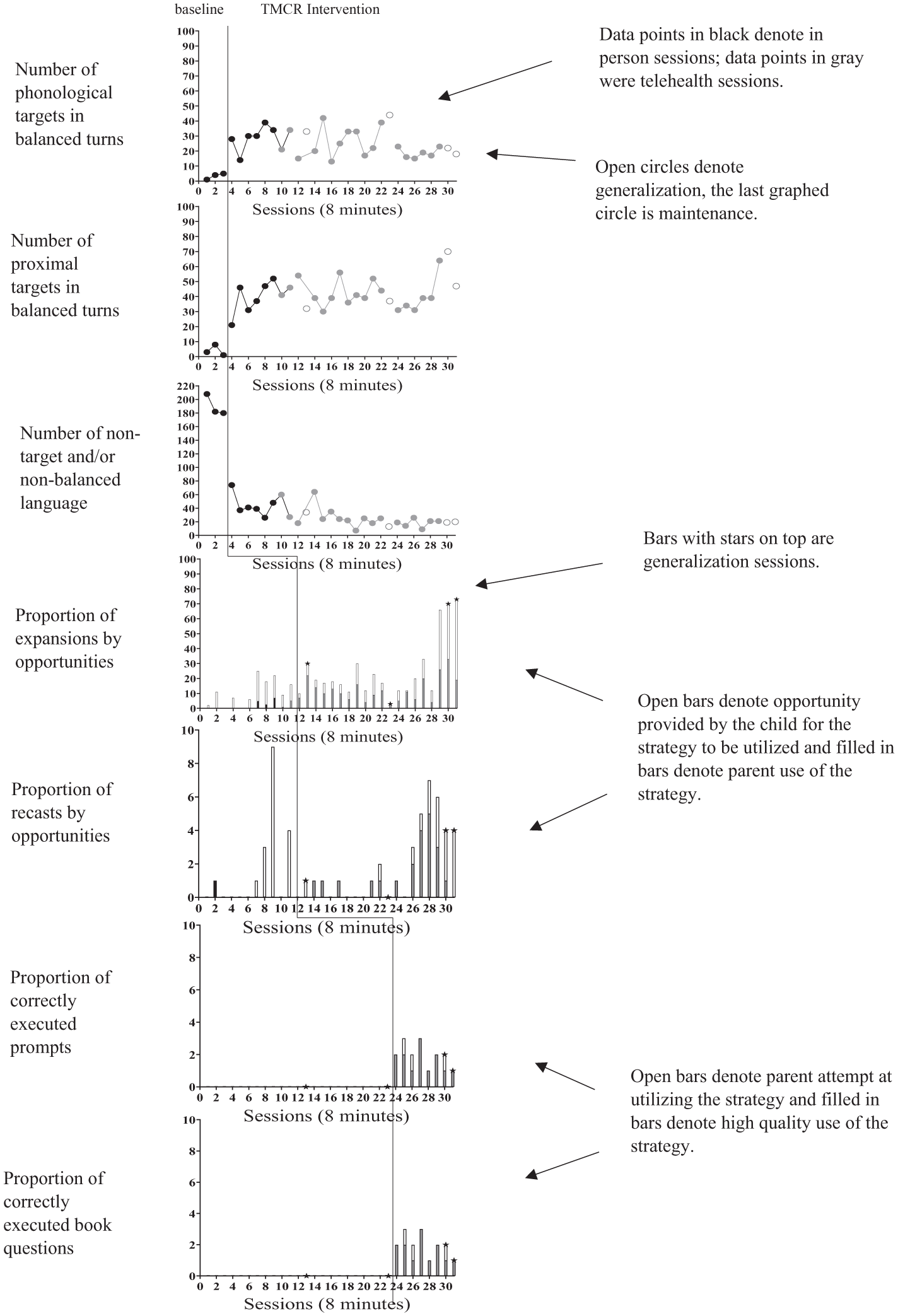
Parent 1 Use of EMT-PE Strategies.
Phase 2 targeted expansions and speech recasting. During baseline use of expansions ranged from 0% to 32% of opportunities with an average of 9% completed expansion by opportunity. The range for use of expansions in the intervention phase ranged from 30% to 92% of opportunities and averaged 55%. The effect size was large LRRi = 1.71 (SE = 0.42). Parent use of speech sound recasting was also calculated in the same ratio format. During baseline, the parent's use of recasts was 0% of opportunities in all but one baseline session, in which it was 9%, the average use of recasts in baseline was less than 1% of opportunities (a near 0 baseline frequency). During intervention, the use of recasting ranged from 50% to 100% of opportunities with a mean of 90%.
In Phase 3, Parent 1 was taught two communication elicitation procedures (a) a time delay prompt to set up a request with a phonetic target and (b) a book question sequence using a test question (e.g., what is this?) to probe for vocabulary words containing a phonetic target. Parent 1 was not attempting either of these strategies at baseline (0 occurrences/attempts). During intervention, she correctly utilized 0% to 100% of time delay attempts (M = 20% correct use). Book question correct episodes ranged from 50% to 100% of attempts with a mean of 75% correct use.
Generalization and Maintenance
Parent 1 generalized and maintained (1 month after intervention) to an uncoached context use of balanced targets (range 18–44, M = 29), proximal targets in balanced turns (range 32–70, M = 46), expansions (range 26–100% of opportunities, M = 61%), and book questions (range 50–100%, M = 75%).
Child Outcomes (Descriptive)
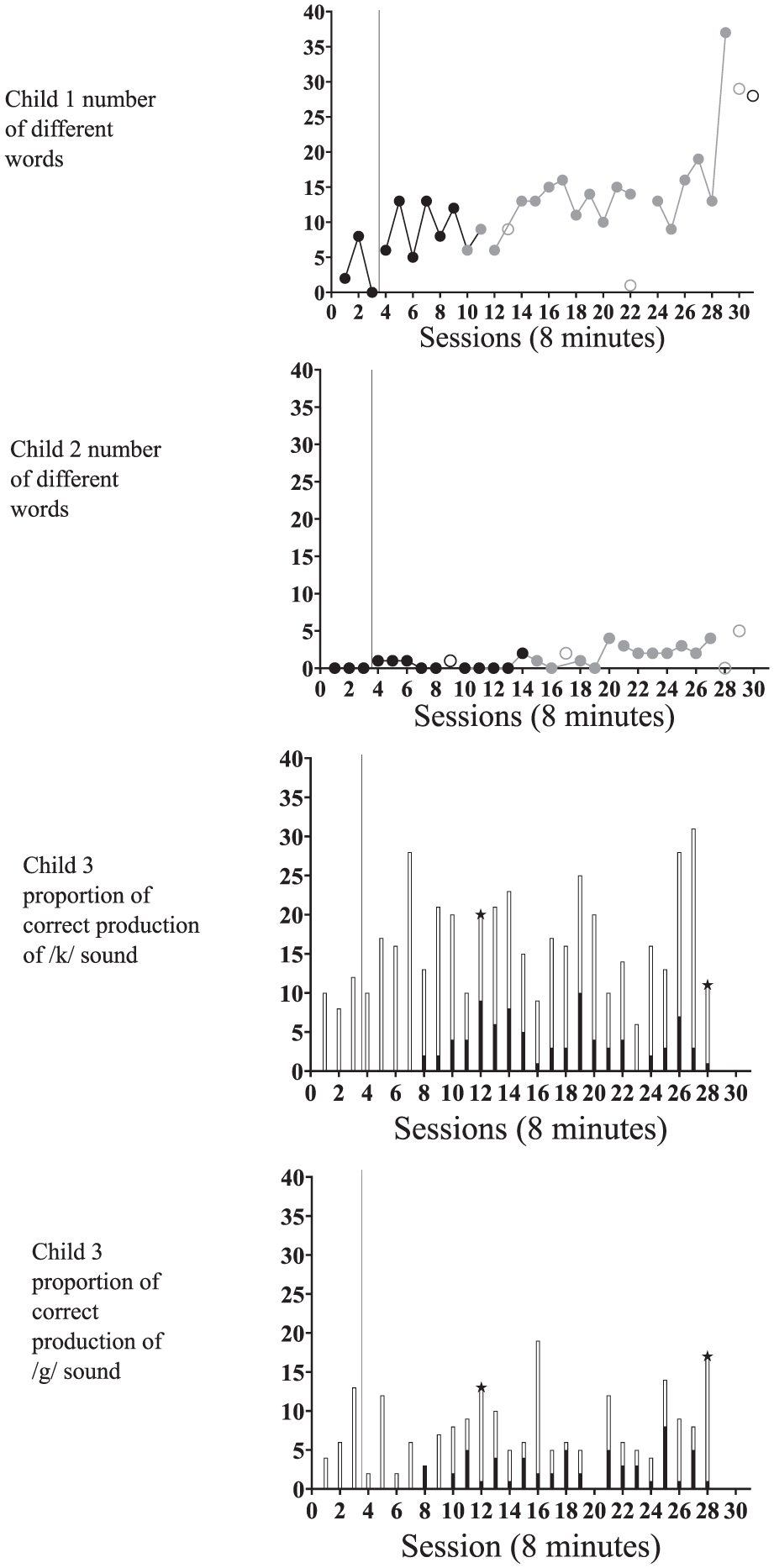
Child 1 used on average four total words and three different words during the 8-min baseline sessions (ranges 0–12 and 0–8, respectively). She did not utilize any phrases or word combinations during baseline. In intervention, she used on average, 12 different words (range 6–37) during the 8 min sessions (Figure 4).
Parent 2
Results for Parent 2 are shown in Figure 2. Parent 2, like Parent 1, demonstrated a clear shift in level from baseline (range 1–2, M = 1.3) to intervention (range 14–42, M = 29) on her use of phonological targets within balanced turns (Phase 1). Her baseline use of this strategy was near 0 with no variability. An immediate increase in level was seen when the strategy was introduced which remained stable. The effect size for the shift in this behavior was large, LRRi = 3.06 (SE = 0.26). Similarly, there was an immediate and clear shift in her use of proximal targets within balanced turns from baseline (range 0–2, M < 1) to intervention (range 6–56, M = 41). A therapeutic accelerating trend was noted during intervention and a large effect size was found, LRRi = 3.62 (SE = 1.00). A clear shift in level in her use of nontarget and/or nonbalanced language was also observed from baseline (range 124–146, M = 137) to intervention (range 5–64, M = 22). A therapeutic decelerating trend was observed in intervention and a large effect size was found (LRRd = 1.83, SE = 0.16).
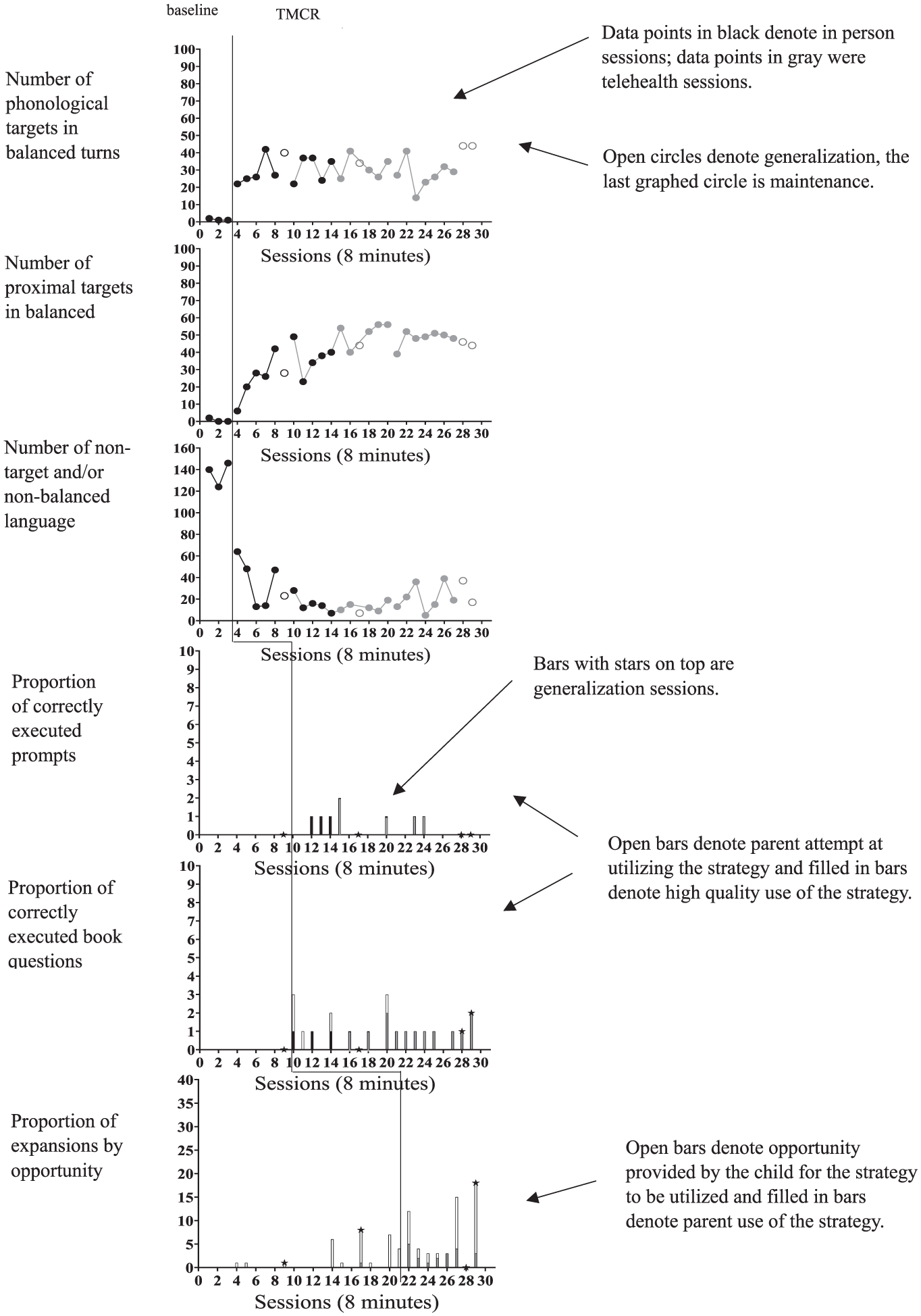
Parent 2 Use of EMT-PE Strategies.
Parent 2 was taught time delays and receptive question asking in book in Phase 2. She had a zero baseline of use of a visual choice to elicit child communication and a zero baseline of use of receptive question asking in book sharing. During intervention, she applied a choice time delay correctly 100% of attempts and applied the book sharing receptive question asking sequence correctly an average of 81% of attempts (range 0%–100% correct question episodes).
Expansions were targeted in Phase 3. During baseline, Parent 2 did not use any expansions (0% of opportunities). In intervention, her expansion use increased to an average of 45% of opportunities (range 0%–67%).
Generalization and Maintenance
Like Parent 1, Parent 2 generalized and maintained to an uncoached context use of balanced targets (range 34–44, M = 40) and proximal targets in balanced turns (range 28–46, M = 40). She correctly implemented 100% of attempted book question episodes during the generalization and maintenance sessions that occurred after the strategy was taught. Her use of expansions was 16% of opportunities in the maintenance session.
Child Outcomes (Descriptive)
Child 2 used zero words during baseline. During intervention, his word use ranged from 0 to 15 (M = 2) and his number of different words ranged from 0 to 4 (M = 1; Figure 4).
Parent 3
Results for Parent 3 are shown in Figure 3. Parent 3 did not complete the maintenance session and only completed two generalization sessions. The child was the last enrolled participant and had tonsil surgery during the study period. Due to the study period/coach’s time in the country ending, completing the three phases of the intervention was prioritized. As with Parents 1 and 2, Parent 3 showed an immediate increase in the level of her use of phonetic targets and proximal targets in balanced turns from baseline (range 2–5, M = 3; range 7–16, M = 12) to intervention (range 4–34, M = 19, and range 18–62, M = 42, respectively). Level of both behaviors were very low at baseline with minimal variability. Her use of phonological targets in balanced turns shifted in the second coaching session and remained stable throughout intervention. Her use of proximal targets in balanced turns showed a slight accelerating trend in baseline and a therapeutic accelerating trend throughout intervention. She also had a clear decrease in the level of her use of nonbalanced and/or nontarget language from baseline (range 122–179, M = 148) to intervention (range 11–113, M = 49). A decelerating trend was noted for this behavior. LRR effect sizes were large for the three targeted behaviors (increase in use of targets in balanced turns LRRi = 1.27, SE = .23, increase use of proximal targets in balanced turns LRRi = 1.11, SE = .14, decrease in use of nontarget/nonbalanced language LRRd = 1.11, SE = .14).
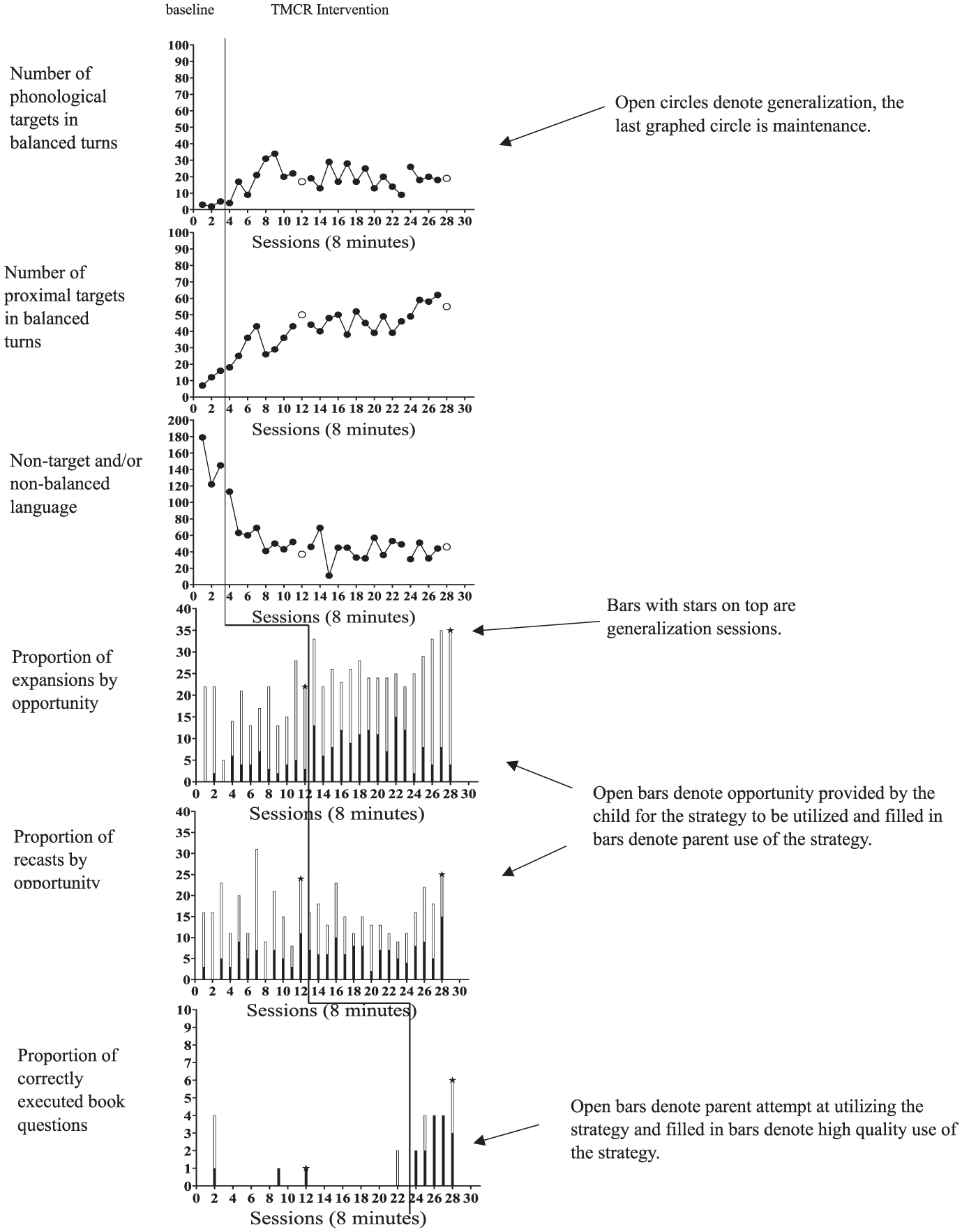
Parent 3 Use of EMT-PE Strategies.
Child Outcomes (Descriptive).
There was a medium effect of the TMCR intervention on Parent 3’s use of expansions (LRRi = .59, SE = .25) and speech recasting (LRRi = .53, SE = .20) in Phase 2. Prior to being taught these two strategies, Parent 3 utilized expansions on average 19% of opportunities (range 0%–40%). After being taught the strategy, Parent 3 utilized expansions on average 35% of opportunities (range 8%–54%). During baseline, her use of recasting averaged 26% (range 0%–45% of opportunities). In intervention her use of this strategy ranged from 15% to 55% of opportunities and averaged 45%.
There were three sessions prior to being taught the book question sequence (Phase 3) in which Parent 3 utilized this strategy. In these sessions she correctly used the strategy one out of four attempts in one session, one out of one attempt in another session, and zero out of two attempts in the third, averaging 41% correct use of the strategy before it was formally introduced. After the strategy was introduced, Parent 3 averaged 87% correct use of the strategy (range 50%–100%).
Generalization
Parent 3 demonstrated generalized use of phonetic targets (range 17–19, M = 18) and proximal targets (range 50–55, M = 52) in balanced turns, and speech sound recasting (60% of opportunities).
Child Outcomes (Descriptive)
Child 3 correctly used the /k/ sound on average 0% in baseline and 18% in intervention (range 0%–40%). Her correct use of the /g/ sound was on average 0% in baseline and 35% in intervention (range 0%–83%). See Figure 4.
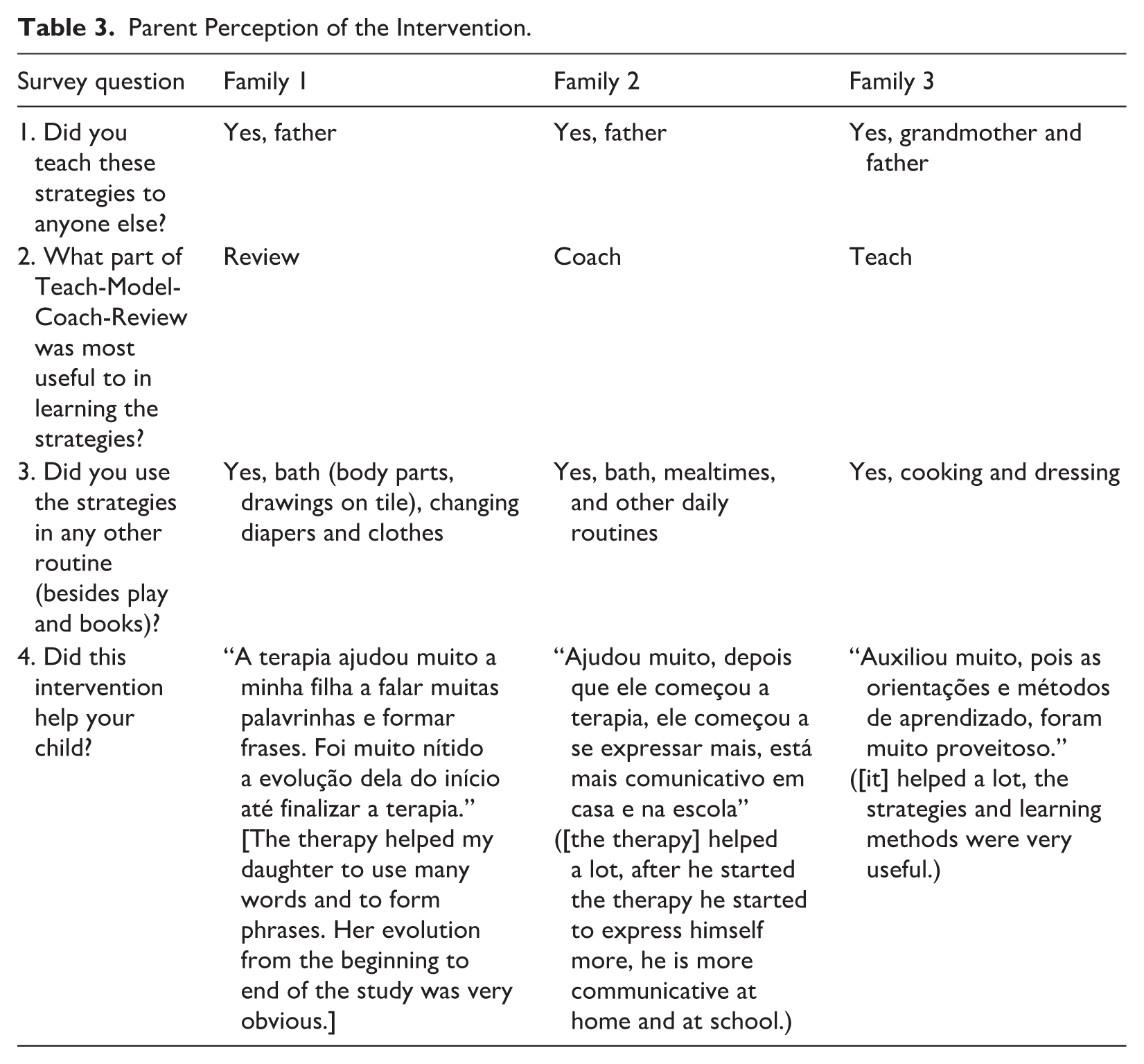
Social Validity
Table 3 outlines the participating parents’ perceptions of the intervention. All three participating parents reporting teaching the strategies to another caregiver and using them in other home routines. All perceived the intervention as effective for their child. In addition, anonymous survey data were collected from 26 Brazilians who work with children with CL/P including 17 SLPs, six students, and four individuals who identified as other professionals. Experience working with this population ranged from 1 to 40 years. Ninety-six percent reported a need for early speech and language intervention for children with CL/P and 96% thought a parent-mediated intervention was appropriate. Ninety-six percent thought the EMT-PE strategies were culturally appropriate and 100% of respondents thought the TMCR approach to teaching parents was culturally appropriate.
Parent Perception of the Intervention.
Discussion
This study adds to the plethora of studies that show TMCR is effective in increasing parents use of naturalistic language support strategies in interactions with their young children (e.g., Peredo et al., 2018, 2022; Philp et al., 2021; Roberts et al., 2014; Roberts & Kaiser, 2015). Notably only one prior study utilized TMCR with parents of children with NSCL/P and in that study parents lived in the United States and spoke English (Philp et al., 2021). This study is unique in that it focused on coaching parents on the implementation of strategies in a Brazilian social cultural and linguistic context.
All three parents applied use of targets and proximal targets within balanced turns, expansions, and/or recasting, and book question episodes with their toddler with NSCL/P. Like with Latino and Spanish-speaking parents residing in the United States, the time delay choice strategy was not generalized or maintained (Peredo et al., 2018, 2022); however, utilization of a book question episode in book sharing to elicit child understanding or use of a phonological target was generalized by all three parents in this study. This suggests that perhaps this more directive and structured strategy for communication elicitation within book sharing may be a better fit for Latino parents, including Brazilian parents.
There were very large effects of the intervention within a relatively short amount of time on the parents’ use of phonological and proximal targets in balanced turns for all three parents, with a notable reduction in conversational turns that are unbalanced and/or do not contain a target. The high numbers of unbalanced/nontarget language observed in baseline may reflect a more directive parenting style observed in Latino families in general (e.g., Domènech Rodriguez et al., 2009; Peredo et al., 2020) and the cultural belief of Brazilian parents that talking a lot to very young children is very important (Viera et al., 2010). Balancing input using the “rule of thirds” may not be a strategy that Brazilian parents use intuitively, but once taught, it can become a natural and effective way to respond and communicate with their child. Without coaching, Brazilian parents may not provide the necessary dosage of contingent responsive speech and language models with conversational pauses to support the development of their children with identified disabilities.
EMT-PE strategies have been shown to be effective for English and Brazilian Portuguese-speaking children with NSCL/P when applied by an SLP (Kaiser et al., 2017; Scherer et al., 2021). In this study, there were notable changes in all three children’s expressive language from baseline to intervention, and in Child 3’s speech intelligibility. Although maturation cannot be controlled for in this study, given the short length of the intervention (2–3 months), it is unlikely that maturation alone would account for the changes. This suggests that the increase in the parents’ use of EMT-PE strategies in their interactions with their children was positively associated with the changes in children’s expressive language. Importantly, all three parents attributed a change in their child’s speech or language to the intervention.
Limitations and Future Directions
As a single-case design study with only three participating families, further research is needed to test the effectiveness of parent/caregiver-implemented EMT-PE for Brazilian children with NSCL/P. Two strengths of this study were the use of an expert-level coach and the ability to tailor and individualize the intervention for each family/child while maintaining the integrity and fidelity of the intervention components. However, these strengths are also limiting in terms of expanding access both in research and in clinical practice to the intervention.
Although the flexibility in teaching strategies in a different order and individualizing for child language needs is important clinically, there is a trade-off in methodological rigor for a single-case design. Notably, all parents were taught the foundational strategies of targets in balanced turns in the first phase and in the same fashion. These strategies are thought to be the active ingredient for child language outcomes in other EMT studies (Dillehay, 2023). In addition, the order of when strategies were taught did not seem to systematically impact parent use of those strategies differentially.
There were also budgetary and time limitations that impacted this study. Each family completed only three baseline sessions. Only one coder completed fidelity of coaching sessions due to inability to hire multiple coders who had Portuguese language skills. The social validity data from parents is limited to a short survey they completed online. With more time and more research funding, richer data could be collected via parent and provider interviews, analyzed qualitatively. The hybrid telehealth option was not available for participant 3 because of the inability of Zoom audio to accurately capture her daughter’s speech sounds. This issue could be resolved with better video and audio technologies (e.g., microphones to capture child audio) which were not feasible within this study’s budget.
Another limitation is related to the variability in parent and child behaviors and the impact on visual analysis. Some parent behaviors are very high frequency (e.g., nontarget/nonbalanced talk in baseline), and to capture these alongside less frequent behaviors required different scaling for graphing. This is also true for some behaviors that are intended to be used at higher frequencies (e.g., phonological targets in balanced turns) and some that are meant to be used sparingly (e.g., time delays). It is also challenging to capture the variability of child language (e.g., number of different words) within the same scales and variables when some children are not using words and some are using multi-word utterances.
Future studies should focus on training Brazilian clinicians as parent coaches and in creating systematic and manualized individualization strategies for children with different speech and language profiles. Longer-term studies which would allow for follow-ups at least 6 months following intervention, would provide better evidence of parents continuing use of strategies and how longer-term EMT-PE strategy use by the parent impacts child language outcomes. In other parent-implemented EMT studies, the largest effects on children’s language are found at the 6-month follow-up which is hypothesized to be due to the parent’s continuing use of the strategies once the coaching sessions are completed (e.g., Peredo et al., 2022; Roberts & Kaiser, 2015).
Conclusion
These initial pilot data show that short-term coaching using TMCR delivered in person or in a hybrid in person + telehealth model is effective in increasing Brazilian parent’s use of EMT-PE strategies with their children with NSCL/P. Parent-implemented EMT+PE could be a promising approach to ameliorate early speech and language difficulties for Brazilian children with NSCL/P. The intervention can be delivered as an efficient short-term model as a hybrid, in-person, or telehealth-only approach to match the needs of families. Additional research is needed involving more parents and caregivers with more varying socio-economic status in Brazil to ensure equitable access to this type of intervention, including examining how a similar approach could work for families in rural and remote areas of the country. EMT-PE delivered as parent-implemented intervention could be a scalable and cost-effective approach to provide children with early speech and language support.
Footnotes
Ethical Considerations
This study was approved by the research ethics committee at the Hospital for Rehabilitation of Craniofacial Anomalies (HRAC), University of São Paulo (# 67173623.0.0000.5441), and the Vanderbilt University Institutional Review Board (IRB # STUDY00000051). All parent participants provided written informed consent to participate.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Fulbright U.S. Scholar Program, sponsored by the U.S. Department of State and the Fulbright Commission in Brazil, provided funding for this study. Additional financial support for some data coding was provided by a Vanderbilt University Rapid-Advancement MicroGrant Program award. The contents of this article are solely the responsibility of the authors and do not necessarily represent the official views of the Fulbright Program, the Government of the United States, the Fulbright Commission in Brazil, the University of São Paulo, Phoenix Children’s Center for Cleft and Craniofacial Care, or Vanderbilt University.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The datasets generated and analyzed for this study are available upon request by contacting the first author.
