Abstract
Advancements in surgical, interventional, and intensive-care medicine have significantly increased the life expectancy of individuals born with congenital heart disease (CHD). As a result, growing numbers of affected children now reach adulthood. Despite medical progress, CHD remains a lifelong condition that influences how individuals perceive and shape their lives. This qualitative study explored ideas of a good life among 14 young adults aged 18–29 years living with CHD. Data were gathered through semi-structured phenomenological interviews and analyzed using interpretative phenomenological analysis. The pursuit of a “normal” life, characterized by equal developmental opportunities compared to peers without CHD, emerged as a central pattern. This experience was reflected in four key themes: “My Whole Life I Have to Fight for Normality,” “Being Treated Normally by Others Is Part of a Good Development,” “Normal Development Includes Lightheartedness,” and “I Need to Stand on My Own Two Feet.” These findings carry important implications for healthcare providers, particularly regarding the promotion of normality and autonomy among individuals with CHD. Patients should be supported in adopting this perspective—as should their parents, since they significantly shape the lives and well-being of patients during their formative years, playing a crucial role in laying the foundation for healthy development and a good life. At the same time, healthcare providers should avoid paternalistic attitudes that risk replicating patterns of parental overprotection. Finally, our findings point to the importance of future research exploring how gender and cultural background shape ideas of a good life with CHD.
Keywords
Introduction
Congenital heart disease (CHD) is one of the most common congenital conditions, affecting approximately 12 million individuals worldwide in 2017 (GBD 2017 Congenital Heart Disease Collaborators, 2020). The term refers to structural anomalies of the heart, ranging from mild forms like ventricular septal defects to moderate conditions such as repaired tetralogy of Fallot, and defects that are more complex, including transposition of the great arteries (Baumgartner et al., 2021). Advances in surgical, interventional, and intensive-care medicine have significantly improved survival rates in individuals with CHD: More than 90% of those born between 1990 and 1992 now reach adulthood, compared to 82% of those born before 1980 (Baumgartner et al., 2021; Mandalenakis et al., 2020). However, many patients continue to experience physical limitations and symptoms, such as dyspnea, tiredness and fatigue, or cyanosis, requiring ongoing medication or repeated medical procedures (Zomer et al., 2011).
The impact of health status on an individual’s life is commonly assessed through subjective evaluations, for example, by measuring quality of life (QoL). QoL is originally defined as “individuals’ perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards and concerns” (The WHOQOL Group, 1995, p. 1403). In medical contexts, however, QoL is commonly conceptualized as health-related QoL (HRQoL), which encompasses an individual’s perceived well-being, symptom burden, and functional status across physical, mental, and social domains.
Although HRQoL in CHD has been studied for five decades, findings remain inconclusive (Moons & Luyckx, 2019). While some studies report no significant differences in HRQoL between adults with CHD (ACHD) and the general population, others indicate lower HRQoL among ACHD (Kovacs et al., 2005). Moons and Luyckx (2019) attribute these inconsistencies to methodological and conceptual issues: ACHD tend to report QoL levels comparable to those of healthy controls when assessed in terms of life satisfaction rather than HRQoL. While HRQoL primarily reflects functional aspects of well-being, life satisfaction captures an individual’s subjective evaluation of their overall life experience (Pavot & Diener, 1993). In this sense, it aligns more closely with the broader concept of QoL, encompassing individuals’ perceptions of what constitutes a good life. The notion of a good life has its roots in philosophical discourse and addresses the fundamental question of how individuals strive to lead a meaningful and fulfilling life (Steinfath, 1998). In the context of chronic illness—characterized by experiences of suffering as well as diminished physical, mental, and social well-being and functioning—individuals may affirm their lives by actively engaging in meaning-making processes, striving to make sense of their experiences, pursuing personally significant goals, or enacting deeply held values. Beyond the specific context of CHD, recent empirical studies focusing on young and middle-aged adults with chronic, and mostly acquired, heart disease have shown that a fundamental bodily trust, self-determined life conduct, and authentic relationships represent essential cornerstones of a good life (Broschmann et al., 2025; Nebel et al., 2025). Furthermore, some adults reported that the confrontation with their heart condition—and the resulting heightened awareness of their own vulnerability—opened up opportunities to cultivate a renewed modesty toward life as well as gratitude for life itself (Broschmann et al., 2025; Broschmann & Herrmann-Lingen, 2023).
Previous research with adolescents and ACHD highlights a profound sense of otherness, shaped by biographical experiences of growing up with a congenital condition (Claessens et al., 2005). The perception of being different is rooted in specific, illness-related experiences, such as frequent hospital visits, surgeries, and extended recovery periods (Tong et al., 1998). Visible scars serve as constant reminders of their condition, while limited physical stamina and breathlessness often hinder participation in activities with peers (Claessens et al., 2005). These challenges foster a strong desire to feel and be perceived as normal (M. Berghammer et al., 2006; Claessens et al., 2005; McMurray et al., 2001; Tong et al., 1998). In striving for normality, ACHD sometimes conceal symptoms or exceed physical limits to align with societal expectations (Claessens et al., 2005; McMurray et al., 2001). Parental overprotection can influence their sense of self, potentially leading to prolonged dependency (Claessens et al., 2005; Kokkonen & Paavilainen, 1992), while physical limitations may result in exclusion or bullying (Horner et al., 2000; McMurray et al., 2001). Adulthood brings additional challenges, including career entry, relationships, family planning, and concerns about health deterioration (Horner et al., 2000). In this context, worries about healthcare coverage may also arise—particularly in systems where access to care is not universally guaranteed—further amplifying anxieties related to potential health decline. ACHD report ambivalence, balancing fears of premature death with resilience and determination (Berghammer et al., 2006; Verstappen et al., 2006). Despite hardships, they experience personal growth, confidence, and spiritual insights (Berghammer et al., 2015; Verstappen et al., 2006).
While previous research has provided valuable insights into the lived experiences of adolescents and ACHD, including their sense of otherness, striving for normality, and the challenges they face in different life domains, it has not explicitly been examined how young ACHD conceptualize a meaningful and fulfilling life.
Study Focus and Aim
To address this gap, the present study investigates the perspectives of young ACHD on what constitutes a good life, aiming to deepen our understanding of their aspirations, values, and sources of meaning beyond traditional health-related measures. The research question was formulated as follows: What ideas do young ACHD, aged 18–29 years, have about leading a good life with their congenital conditions?
Methods
Sampling Approach
This study was conducted in accordance with the Declaration of Helsinki, approved by the local ethics committee, and registered in the German Clinical Trials Register (DRKS00028096).
Following a purposeful sampling strategy aimed at ensuring homogeneity of the sample with respect to key characteristics of the phenomenon under study (ideas of a good life with CHD), and to enable a detailed, nuanced exploration of shared lived experiences, eligible individuals were approached through flyers and participant information sheets distributed at a university hospital and a specialized outpatient clinic for ACHD, and through nationwide patient organizations. Recruitment took place between October 1, 2023, and July 15, 2024. ACHD were included if they were aged 18–29 years and had a diagnosed CHD that had significantly impacted their lives since childhood. This criterion aimed to include individuals who had consciously experienced the impact of their condition in their everyday lives over the course of their life. Since some CHDs cause few or no symptoms and may remain largely unnoticed by those affected, the criterion helped differentiate between abstract diagnosis and lived experience. The assessment of impact was made both by medical expertise and validation by the individuals themselves during the recruitment process. Exclusion criteria included insufficient proficiency in the German language, cognitive impairments that hindered participation in interviews, and severe mental health conditions such as severe depression, addiction, or schizophrenia.
As part of the recruitment process, a personal or telephone-based informed consent conversation was held with each participant, explaining the study’s aims, procedures, potential risks, benefits, and their rights. To address potential risks, participants were informed that discussing past life events and medical experiences could cause emotional distress, although many also find value in such reflection. Participation was voluntary, and participants could pause or withdraw at any time without consequences for their medical care. Following the provision of written informed consent, an interview appointment was scheduled. Throughout the interviews, the researcher remained attentive to participants’ emotional responses and offered breaks or follow-up support when needed. All interviews were recorded with consent, and personal data were pseudonymized or anonymized before transcription. Team members were bound by confidentiality, and data were stored securely according to institutional data protection policies.
Participants
During the recruitment phase, we contacted 15 eligible young ACHD. After having accepted the invitation to the briefing, one woman did not respond to further contact attempts. Thus, the final study sample comprised 14 young ACHD aged 18–29 years (median age: 24), with an even distribution of women (n = 7) and men (n = 7). Participants were geographically distributed across various regions of Germany. One-third of the sample had completed a general higher education entrance qualification or held a higher academic degree. Only one participant had a migration background.
List of Pseudonyms Assigned to All Study Participants, Organized by Gender
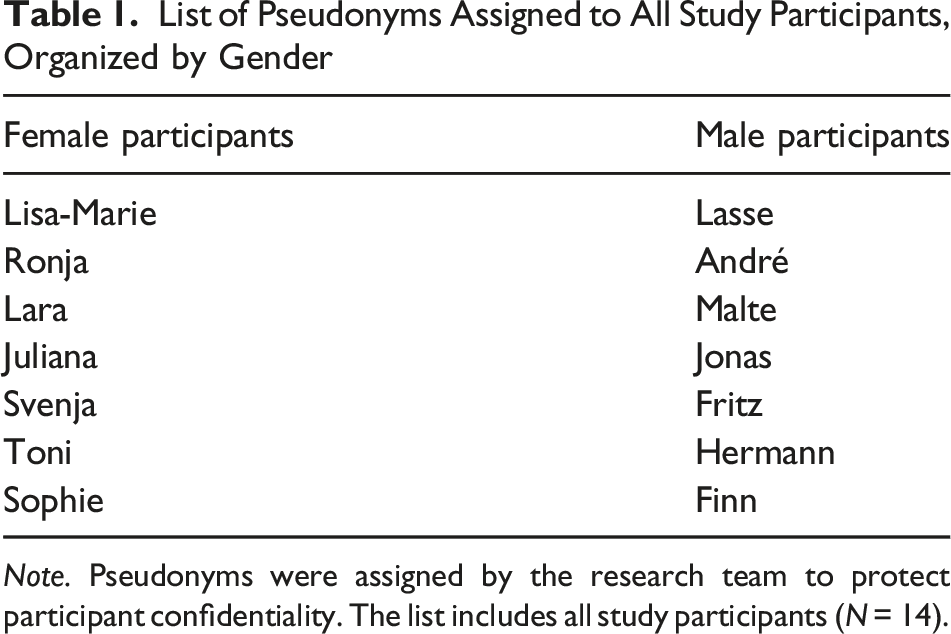
Note. Pseudonyms were assigned by the research team to protect participant confidentiality. The list includes all study participants (N = 14).
Procedure and Interview
Semi-structured individual interviews were conducted by a trained member of the research team—either a 36-year-old male physician (DB) or a 29-year-old female psychologist (LN)—both of whom were equally involved in data collection and analysis. Since ACHD were recruited from a department separate from the one in which the study team worked, neither interviewer had any clinical involvement in their care. Owing to the nationwide sampling strategy, participants who were unable to attend in-person interviews at the university hospital were offered the option to participate remotely, either via telephone or through Sprechstunde Online, a GDPR-compliant (General Data Protection Regulation), secure video-conferencing platform specifically designed for medical consultations, which allows for real-time audio-visual communication between participants and interviewers. Interviews lasted between 35 and 79 minutes (
The interview schedule (see Appendix) was developed based on an in-depth review of relevant literature, followed by reflective discussions within the research team to identify key thematic areas. It was pilot-tested to ensure clarity and relevance.
Interviews commenced with open-ended prompts to encourage participants to share their lived experiences with CHD (e.g., “Would you like to start by telling us about your heart disease?” or “How does heart disease influence your life?”). This open and flexible approach facilitated rapport-building and fostered a trustworthy atmosphere, enabling participants to share their perspectives in a non-directive, participant-centered manner. As the interviews progressed, more focused questions were introduced, addressing participants’ ideas of a good life (e.g., “What is important to you in your life?” or “What does a good life mean to you?”). Follow-up prompts such as “Tell me more about this” or “Can you give me an example for this?” were used to elicit deeper insights. Trustworthiness was enhanced by posing concrete questions, encouraging elaboration, and seeking clarification when needed.
Analytic Approach
The interviews were analyzed using interpretative phenomenological analysis (IPA; Smith et al., 2022), a qualitative method frequently employed in health research to explore lived experience (e.g., Arroll & Senior, 2008; Collins et al., 2023; Eisenberg & Josselin, 2024). IPA draws on phenomenological, hermeneutic, and idiographic traditions, facilitating the identification of shared experiential patterns while simultaneously accounting for individual nuances.
Phenomenology and hermeneutics constitute two distinct yet complementary philosophical frameworks for understanding human experience. In the context of IPA, these traditions are brought together in a way that emphasizes both the detailed exploration of lived experience and the interpretative processes through which meaning is co-constructed by participants and researchers. Phenomenology, particularly in its descriptive form as grounded in the work of Husserl (2009), emphasizes the investigation of lived experience from a first-person perspective, seeking to bracket preconceptions in order to approach phenomena as they present themselves. Phenomenology has evolved into more interpretative and existential directions, as developed by philosophers such as Heidegger (1927/2006) and Merleau-Ponty (1966/1974). Each of these scholars contributed to a broader understanding of lived experience as always embedded in a world shaped by language, embodiment, relationships, and historical context. Their approaches underscore the situated and meaning-laden nature of human existence and align closely with the epistemological foundations of IPA.
In contrast, hermeneutic philosophy, as advanced by scholars such as Gadamer (2010) and Ricœur (1984), foregrounds interpretive engagement, where meaning arises through interaction with texts, language, or other people, acknowledging the productive role of pre-understandings in shaping meaning. While the phenomenological orientation in IPA aims to access the insider’s perspective of those experiencing a phenomenon, the hermeneutic component allows for a reflective interpretative stance, through which researchers make sense of participants’ accounts in context.
Following each interview, the interviewer recorded their initial impressions and highlighted relevant passages in a separate Word document. Subsequently, the other member of the research team reviewed the interview, providing additional notes on the interview process and possible interpretations to the same Word document.
Once the transcripts were completed, they were transferred to the software MaxQDA for analysis. The analytical process involved the following steps of IPA: (1) Reading and re-reading: DB and LN independently read the first transcript to develop an initial understanding of the interview as a whole. (2) Initial noting: While reading, they noted linguistic and conceptual particularities. (3) Constructing experiential statements: DB and LN then independently identified aspects relevant to the participant’s ideas of a good life and formulated experiential statements that closely reflected the participants’ language and meaning. (4) Searching for connections across experiential statements and (5) naming the Personal Experiential Themes (PETs): Experiential statements were transferred to a separate Word document and clustered into overarching themes using strategies such as subsumption, abstraction, and comparative analysis of similarities and differences. (6) Moving to the next case: Steps (1) to (5) were repeated for each subsequent transcript. (7) Developing Group Experiential Themes (GETs): The resulting individual PETs were compiled in another separate Word document and examined for recurring patterns across transcripts to develop GETs. In a final step, all GETs were validated against the original data, following the logic of the hermeneutic circle. Throughout the analysis, weekly meetings were held to resolve discrepancies in the development of statements and themes. CHL and TLB supervised the process, providing a more distanced, third-party perspective. These supervision sessions regularly included reflections on the researchers’ own backgrounds and positionalities, creating space to critically examine how individual assumptions and prior experiences might influence the interpretation of the data.
Research Team Reflexivity
Both researchers involved in data collection and analysis had prior experience in qualitative research; the physician also brought several years of professional experience in psychiatry and psychosomatics. Although neither interviewer was involved in clinical care and participants were recruited from a different department, we acknowledge that the researchers’ professional backgrounds may have influenced the interview dynamic—particularly in terms of perceived authority, expertise, or expectations. Throughout the research process, the interviewers engaged in continuous reflexive practice, considering how aspects such as their professional roles, gender, age, ethnicity, and education might have shaped data generation and interpretation. These reflections were documented in a shared research diary, in which the authors recorded and examined their personal reactions, assumptions, and interpretations. In addition, reflexive discussions were systematically integrated into team meetings and supervision sessions, which included TLB, a bachelor’s student in public health with prior training in qualitative methods but no professional background in cardiology, and CHL, who brought extensive experience in psycho-cardiology research and clinical practice but had less familiarity with qualitative research approaches.
Results
The analysis identified four key themes that emphasize the constant struggle for a good life experienced by ACHD: “My whole life I have to fight for normality,” “Being treated normally by others is part of a good development,” “Normal development includes lightheartedness,” and “I need to stand on my own two feet.” While these theme titles often closely reflect participants’ own expressions or direct quotes, they also incorporate interpretive elements by the researchers to capture the underlying experiences in relation to the research question. Themes are illustrated with participant quotes, translated from German into English in accordance with the guidelines of the American Psychological Association. Ellipses indicate minor omissions that do not alter the original meaning of the quotes. Additions or modifications made to ensure pseudonymization are marked with square brackets.
My Whole Life I Have to Fight for Normality
Throughout their development, individuals with CHD repeatedly encounter situations that reinforce their sense of being different from others. This perception of otherness shapes their idea of a good life as one that is “normal.” Thus, growing up with CHD involves a continuous struggle for normality.
The sense of being different is rooted in a bodily experience that individuals with CHD face: a constant latent existential threat that impairs the development of trust in their own bodies. In the striving for what they perceive as a good development, this existential fear is often suppressed or countered to avoid confronting the awareness that symptoms could suddenly become life-threatening—an awareness that could otherwise disturb their fundamental sense of safety and embodied stability. Yes, because the risk is always there. … And something could always be wrong. [The physician] said, “You can be fit as a fiddle today—you can work out or whatever—and then later, you think you will just go to bed, but you do not wake up the next morning.” That is normal, he said. Even healthy people have that risk. But for me, for us children with congenital heart disease, the risk is just higher. And when it comes to disease and things like that, we can get sick more easily, or a fever can be dangerous—anything, really. There is always something that could happen. (Lisa-Marie)
Referring to “something that could happen,” be wrong or dangerous, Lisa-Marie highlights the existential threat posed by her CHD. This threat is ever-present, even in routine occurrences, such as an infection, which healthy peers would typically recover from more easily. Notably, in an effort to cope with this existential threat, both the treating physician and Lisa-Marie, by recalling his statement, relativize her experience in comparison to those of healthy peers: “Not waking up the next morning” is framed as a normal condition of life, yet in the case of CHD, it becomes more probable. Having survived into adulthood without requiring further interventions represents an accomplished sense of normality for Lisa-Marie—one that she takes pride in.
The management of illness-related risks involves regular medical appointments, interventions, and medication—necessities that ACHD perceive as “normal” aspects of life. However, efforts to prevent disease decompensation can sometimes hinder individuals with CHD from taking developmental steps similar to their peers without CHD. When it came to sports, many people said: “You cannot do it, do not try, it is too much for you.” The doctors told me I should do sports, but everyone around me said: “You cannot do sports, it is too exhausting, do not do it, stop.” Well, … with cycling, for example. Nobody wanted to teach me, so I just did it completely on my own. Or when I was rollerblading: “You could break something. You might get dizzy and fall and hurt yourself,” or something like that. And still, I pushed through and somehow managed to do it. So, in the end, I mostly succeeded. (Ronja)
Concerned that Ronja might harm herself through physical exertion, her parents restricted her participation in physical activities. However, Ronja fights to achieve her goals and pushes herself beyond expected limits, striving to be perceived as “normal” by others and to experience a sense of normality for herself. Similar to Lisa-Marie, achieving this sense of normality fills her with pride.
While Ronja perceives “normality” as achieving the same developmental milestones as her peers without CHD, Toni experiences a sense of accomplished normality through her positive attitude toward her scar. I used to act in theater, and once, they covered up my scar with stage makeup, and you could not see it at all. I felt really strange, though, like I was not myself because I could not see it anymore. It felt really uncomfortable when it was not there. I mean, it is not nice when people look at you, and the scars from the drainage tubes, well, they fade, but they are not exactly pretty. But the scars are part of it. I really do not have a problem with them. (Toni)
With her scar covered, Toni felt “strange” and “uncomfortable,” alienated from herself. However, by emphasizing her ability to accept the scar as part of her biography and identity, she seems to view it as a positive marker of her uniqueness. Between the lines, a sense of pride emerges in her ability to cope with the burden of a congenital condition—a process of suffering and fighting, which is made visible through the scars. Despite the pride reflected in her positive attitude toward the scar and her identity’s connection with the illness, Toni experiences her condition as profoundly unjust. Sometimes, it just feels unfair. I really ask myself, why? Why can’t I just be normal? (Toni)
Fritz, too, describes the ongoing emotional effort required to navigate the tension between accepting his condition and perceiving it as disadvantageous in comparison to others without CHD: I still catch myself making those comparisons, even though I know I should not—and really cannot—because we are two different people with different backgrounds, traits, abilities, and so on. But it is something I have struggled with a lot in the past, and I still do to some extent. It’s not completely gone, but it has gotten better. … I think that at 27—almost 28—other people are just further along in terms of where they are in life. And I don’t think that’s something you can really deny. The truth is, with all the hospital stays over the years, there are just certain parts of development that I’ve kind of missed out on. (Fritz)
The continuous struggle for a sense of normality and the ability to achieve the same developmental milestones as their peers is a fundamental life theme for ACHD. This struggle is reflected in their pursuit of independence, educational and career opportunities, and, for some women, the aspiration to experience successful motherhood. It is accompanied by ambivalence between accepting one’s condition, thereby acknowledging one’s otherness, and striving for “normality,” which at times involves denying individual illness-related needs and limitations.
Being Treated Normally by Others Is Part of a Good Development
Relationships are considered an important aspect of a good life by all participants. Especially close relationships with family, partners, and friends are seen as crucial components. However, relationships can also be a source of the otherness perceived by ACHD. For instance, Toni recalls how others’ reactions to her scar changed over time, making her feel increasingly uncomfortable. I mean, kids just ask. I have a long scar, and of course, everyone always asks me, “What is that?” or “What is this?” and “Why?” With time, there comes an age when people start avoiding the question, and they do not dare to ask. I actually find that much harder. (Toni)
While Toni does not feel bothered by an honest and interested approach toward her scars, avoidance and concealment reinforce her feeling of being different in a burdensome way compared to others. With all other scars, it is kind of okay to ask, “Hey, what is that?” and people talk about it openly. But when it is that scar, people look at you, and I can tell they are thinking about it but do not dare to ask. And I am left wondering, what is the problem? What is so different about that, compared to having a scar on my knee or my back from, I do not know, an accident? It is frustrating. (Toni)
Toni believes people stop asking about the scar on her chest because they associate its location with a serious medical condition. However, based on her lived experience, she does not perceive this reluctance to address such existential topics as an expression of care but rather as a subtle form of discrimination. In contrast, participants emphasized that open communication about their CHD not only enables a humorous or lighthearted approach to coping but also creates opportunities to prepare others for potentially threatening situations—thus fostering a sense of agency and shared resilience. Additionally, other participants report that treatment-related school absences, disease-related limitations in physical performance, and visible physical traits, such as cyanosis or surgical scars, have led to experiences of exclusion, bullying, or social stigma. For instance, while Toni expresses frustration about her peers’ avoidant behavior regarding her scar, Lisa-Marie describes a contrasting experience of being openly bullied because of her cyanosis and visible scar—particularly in situations where teachers had to draw attention to her condition: I just grew up with it—my family was always very open about my condition. Even in kindergarten, they would explain to others: “Be careful, she has a heart defect. If she turns blue, call an ambulance. Watch her closely if she has a fever.” So it was just normal for me pretty early on. I was like, okay, this is just part of my life, whatever. But then, around the end of elementary school, things started to change. I started wanting to hide it. That’s when the bullying started—like “Ew, what’s that?” or people making a big deal about it, giving me all this unwanted attention. And I was like, I’ve had this scar since I was a kid. I didn’t choose to have this giant scar. But people acted like I did, and treated me accordingly. (Lisa-Marie)
However, while experiences of peer avoidance or negative attention may be unsettling and burdensome for the participants, it is the family’s approach to CHD that fundamentally influences the patients’ experience, as it shapes early relational experiences and contributes to the formation of their sense of self. Half of the participants report that their parents were overprotective, which hindered them from achieving developmental goals or exacerbated their anxiety. Ronja, for example, who described how her parents prevented her from cycling and rollerblading, illustrates this point clearly: For me, a good life means being able to have fun—taking care of myself, sure, because there is something there—but still living my life and enjoying it without feeling restricted all the time. There are limitations I have to deal with. But then there are things where other people limit me—because they do not think I can handle them. (Ronja)
Ronja explicitly distinguishes between the limitations imposed by her disease and those imposed by others who perceive her as ill and restricted. While Ronja expresses her frustration with being overprotected quite openly, André takes a more reserved approach. He initially emphasizes his ambivalence toward the care others show him before eventually articulating his sense of discomfort. I think it is kind of nice that people look out for me a little—like, making sure I do not overdo it or that nothing happens. But at the same time, it also kind of bothers me, because it feels like they do not really have trust in me right away. (André)
In contrast, Toni—like the other half of the participants—felt that she was treated no differently. For her, this is evident in the fact that the same expectations regarding household chores and education applied to her as to her siblings without CHD. However, she acknowledges that her parents held a different perspective, noting that they took her to the doctor more quickly and granted her certain leniencies, such as allowing her to watch television for longer periods. Nevertheless, Toni considers her perception of being treated normally as essential for developing a sense of bodily trust. I believe that was beneficial and the right approach. It probably led me to believe for a long time that the problem was solved, that everything was fine. However, I feel it allowed me to grow, making me more carefree than I would have been if it had always been an issue. Overall, I do not let it restrict me too much, and I am not particularly afraid of making mistakes. (Toni)
Although being treated normally by her parents has given Toni a distorted perception of her condition, she places greater value on the positive developmental opportunities it has afforded her.
Normal Development Includes Lightheartedness
Like Toni’s and Ronja’s previous statements indicate, good development includes the ability to act spontaneously and without caution in order to feel unburdened and “normal.” In contrast, restrictions and rules aimed at preventing decompensation of the CHD often reinforce the feeling of being different. For instance, Ronja recalls her time in kindergarten as highly restrictive due to behavioral rules meant to prevent her pacemaker leads from breaking. When the other kids were playing, I could not always join in the same way. There were these poles you could spin around on, but I was not allowed to do that because my pacemaker was in my stomach area, and the lead could have snapped. Bending over chairs or doing certain movements was not okay either. That is when I really started to realize that something was limiting me. … To be honest, I did not always follow the rules. My pacemaker leads tend to break pretty easily. … But as a kid, it did not bother me that much. I just lived my life like any other child. The only thing that really annoyed me was being in the hospital—I think no child likes being in the hospital. (Ronja)
To feel included and “normal,” Ronja behaved like the other children in her kindergarten. Although this often led to dangerous episodes of syncope and required the replacement of her pacemaker, she placed significantly greater value on achieving what she perceived as good development. In this context, good development is equated with “normal” development, understood as a relational and identity-shaping experience grounded in the desire to align with socially shared standards of age-appropriate behavior. Rather than referring to a biomedical ideal, “normal” development here reflects a socially situated sense of belonging and inclusion.
For Jonas, it was also important to be able to be lighthearted and have fun with his friends from time to time. However, unlike Ronja, he differentiates between “shenanigans” and real danger—situations that could cause long-term harm to his health. So, with some things where I was out with friends or doing silly stuff I probably should not be doing, I had a mind of my own. But when it came to things like, “Okay, my friends are going to play sports again” or do something risky where something might happen, I thought at that moment: “Yeah, maybe sit this one out and stay out of trouble.” Not trouble exactly, but like avoid anything that could affect my heart or put me at risk. … Because whenever something did happen, it always meant I was missing out for a long time—no matter what it was. And I really just wanted to avoid that. (Jonas)
For Jonas, then, good development does not mean participating in all typical adolescent activities regardless of the risks involved, as it does for Ronja. Rather, it means finding a shared experiential space with peers that respects his health limitations while still allowing for inclusion and a sense of ease. While not equal to the good life itself, lightheartedness fosters a sense of belonging and thus becomes an important expression of agency and everyday normality within the lived constraints of chronic illness.
In contrast to Ronja and Jonas, Lara tended to fully comply with imposed restrictions. She describes that she now experiences a sense of inferiority when confronted with boundaries, which she explicitly attributes to the parental overprotection she encountered during childhood and adolescence. It makes me a little angry (laughs). Like, I get kind of frustrated because it makes me feel like I am not as good as other people. … Maybe it has to do with [pause] I do not know, maybe because I was taken care of more? … Because my parents were probably afraid—and even more so because of my history—I was always more careful to avoid dangerous situations. Even now, I tend to be extra cautious about a lot of things, and sometimes I wish I could be braver and just go for it. Like, for example, jumping over something or whatever—just little things like that. (Lara)
The courage Lara longs for is embodied by Juliana, who describes taking risks as an essential part of good and “normal” development—even during times of medical instability: Yeah, you will always have to take steps in life, even if you are dealing with disease. If you do not, you will end up regretting it—or it will just be something left in your past. And that is just the kind of person I have always been. Even when my heart was in bad shape, I still took the riskiest steps. And I am still here. I am doing fine. Yeah. I do not have the same doubts I used to. (Juliana)
Taking risks and exploring her own limits was important for Juliana in developing a certain level of trust and dispelling doubts. For good development, she had to fight with her concerned parents to be allowed to take the same steps as her siblings and peers, such as going to parties, working, and moving out. She recalls being taught how to properly manage her illness. However, she admits that she did not always adhere to those recommendations. I was told how to take care of myself and what I should not do. I was even told not to buy alcohol, soda, or anything like that. And yeah [pause] but I do all of it. For example, I smoke. And I never drink water—almost never. I either have apple spritzer, soda, or Sprite, but never water. (Juliana)
These conscious acts of non-compliance were not simply rejections of medical norms but expressions of autonomy and identity. By prioritizing life experiences shared with peers over strict compliance with clinical recommendations, Juliana reclaims a sense of agency and normality. This enables her to envision and live a good life with CHD—one in which lightheartedness becomes a form of embodied confidence rather than recklessness, and in which a “normal” development is a felt achievement, not a medical status.
I Need to Stand on My Own Two Feet
Despite the challenges that come with growing up with CHD, the participants are grateful to be alive. As they age, limitations, though still painful, become easier to accept, because the participants instead focus on their possibilities. For instance, to maintain his confidence after heart transplantation, Lasse constantly reminds himself that his situation could be worse. Well, I would not say that I have the best life in the world right now. Sometimes, especially in situations like this, where things have been really tough for me lately, you think to yourself, “No one has it as bad as I do.” But then you also think, “There are people who cannot even walk.” That is tough too. (Lasse)
Similarly, Ronja strives to focus on the positive aspects of her situation. When asked what gives her life meaning, she responds: PUH! Well, really, it is that I am ALLOWED to live. That I can almost do whatever I want. I can live my life without being completely dependent on everything all the time. The pacemaker makes me more independent than if I had other problems. For me, the meaning of life is that I am allowed to live and have the freedom I do. Of course, there are limitations too. There are always pros and cons, no matter what. (Ronja)
However, the autonomy once achieved is fragile. Health setbacks reinforce actual dependency and the concerns of family members, whose caregiving behavior is experienced by ACHD as overprotective and limiting. Following a significant decline in health, Ronja observes her family and boyfriend becoming more cautious. I do have a driver’s license, but no one will let me drive at the moment because I might get dizzy. I get it, but on the other hand, I still rely on the car for some things, and that means I always need someone to drive me. And that freedom I used to have, the one I worked for, is just gone because I am dependent on others. It is frustrating. (Ronja)
Due to the acute deterioration of her physical condition, Ronja experiences the loss of her hard-won autonomy. Having to accept that she is once again more dependent on the help of others in her current situation is difficult for her to endure.
The freedom experienced through independence, which the participants worked hard for, is particularly vividly described by Juliana: Starting at the age of 16, I began doing what my other sisters were doing. I sat down with my parents and told them that eventually, they would not always be around, and I would have to stand on my own two feet. I realized I needed to plan for the future … because, if something happened to them, I would be left alone. My siblings each have their own lives, and I did not want to burden them with my illness. … Once I was standing on my own two feet, it became easier for me and lighter on my heart. … I no longer felt sick, I always felt free. I was not being watched or protected by my parents anymore, like someone was always behind me, ready to catch me. I could finally say, “It feels good to stand on my own two feet and walk my own path.” (Juliana)
Being able to stand on her own two feet gives her a sense of no longer being sick, which she considers a significant accomplishment of positive development. Furthermore, her independence enabled Juliana to move out of her parents’ home and start her own family with her husband—a developmental milestone that she considers an integral part of a good life. [The physician] told me, very clearly, even back then: “You and children—no way.” I simply replied, “But I still have the desire to have children in my heart.” After that, she made a plan for me to undergo my third cardiac catheterization. Thankfully, the doctor who performed the procedure also arrived and said, “Yes, you can have children.” The next day, I was discharged. We had already started preparing for the pregnancy. And then I became pregnant. (Juliana)
Despite the initial medical assessment that pregnancy was contraindicated due to Juliana’s heart condition, she did not give up on her desire, accepting the risks to her own life and that of her future child. Motherhood now provides her with a strong sense of meaning.
Her story reflects a broader theme that emerged in the study: the aspiration to start a family despite medical risks. Family planning was discussed by nine participants—six women and three men—suggesting that the topic may carry particular significance for women with CHD. For some women, becoming a parent symbolized reclaiming control over their body and future. In contrast, other participants—both men and women—explicitly rejected the idea of having children, primarily due to fears of passing on their condition or concerns about a child’s well-being. These contrasting perspectives reveal the emotional complexity surrounding reproductive decisions among ACHD, entangled with questions of autonomy, identity, and responsibility.
Discussion
This study examines young adults’ ideas of a good life with CHD, focusing on fundamental life themes, aspirations, and values that shape their understanding and pursuit of a fulfilling life.
Our findings suggest that a good life for ACHD is, above all, a “normal” life—one that offers the same developmental opportunities as their peers without CHD. The notion of normality thus refers to the average norm rather than to an ideal norm. This desire stems from a biographical sense of being different, making the pursuit of normality a central life theme. Despite illness-related challenges, often described as traumatic experience such as repeated hospitalizations and medical interventions (Freiberger et al., 2023), ACHD strive to navigate the same developmental milestones as their peers. They view being treated as normal as essential to building confidence in their own abilities. Overcoming parental overprotection, testing personal limits, and pursuing desired hobbies, careers, or life goals despite their condition are sources of pride. At the same time, engaging in moments of carefreeness—even acting unreasonably—emerges as a crucial skill, allowing ACHD to push their condition into the background, avoid demoralization, and experience independence. Independence itself becomes the ultimate goal, enabling them to shape and affirm their lives on their own terms. For some young women with CHD, autonomy is also a prerequisite for having children—an aspiration that, despite the risks, represents a powerful symbol of normality. However, the hard-won independence remains fragile, subject to being lost and regained throughout their lives.
The profound sense of being different and the resulting drive for normalization are well-documented in previous qualitative research on adolescents and young ACHD (Berghammer et al., 2006; Claessens et al., 2005; McMurray et al., 2001; Tong et al., 1998). Similar to our results, Berghammer et al. (2006) describe this tension as ambivalence: ACHD’s unique medical needs stand in direct contrast to their desire for normality, shaping a conflicted self-image. However, in a later phenomenological-hermeneutic study, Berghammer et al. (2015) found that young adults with a surgically treated Fontan circulation identified more strongly with healthy peers than with other ACHD, viewing their condition as part of their identity rather than as an illness. This aligns with McConville’s (2021) analysis of the phenomenology of congenital illness, which challenges Svenaeus’ (2011) argumentation that chronic illness and a sense of homeliness in one’s own body exclude each other. Drawing on his own experiences with CHD, McConville suggests that for individuals with congenital conditions, uncertainty about health and bodily integrity is not an intrusion into normality but an inherent part of it. Our findings support this perspective, yet they also indicate that ACHD experience tangible losses—such as setbacks in autonomy—making their pursuit of normality both fragile and dynamic.
The feeling of being different is not solely attributable to having CHD itself but also to the way ACHD perceive treatment by others—an aspect previously reported in the literature (Berghammer et al., 2006; Claessens et al., 2005; Gantt, 1992; Horner et al., 2000; McMurray et al., 2001; Tong et al., 1998). Our participants similarly described how others, aware of their heart condition, often acted with excessive caution, which reinforced their sense of otherness. Some reported becoming more cautious and anxious themselves as a result of this protective behavior, while others pushed their limits to counteract the perceived deviation from their peers. This tendency to “live beyond one’s own capacity” (p. 343) aligns with the findings of Berghammer et al. (2006). Moreover, an ambivalence emerges regarding how ACHD navigate their condition—equally echoing Berghammer et al.’s (2006) observations. While the young adults in our study strongly advocate for equal treatment, they also emphasize the importance of transparency about their condition. Beyond affirming their identity, openness serves a practical function: preparing others for potential medical emergencies. Transparency appears to mitigate stigma, facilitating a more relaxed and even humorous approach to their condition. Claessens et al. (2005) similarly identified a desire for open communication about CHD in their sample. Furthermore, the authors argue that parents who encourage their children to participate in peer activities despite their heart condition play a key role in promoting healthy development. Such parental support helps children and adolescents with CHD to better understand and assess their own limits, while also reducing feelings of being different from their peers. Framing CHD as a challenge rather than a restriction reduces feelings of stigma and fosters a greater sense of normality. In both our study and that of Berghammer et al. (2015), normality is closely linked to a sense of belonging.
Notably, the complex tension between the desire to feel and be treated as normal, on the one hand, and the simultaneous wish for others to show genuine interest in the condition, on the other, challenged our own preconceptions of what constitutes a good life with CHD. Rather than viewing these desires as opposed, participants integrated them into a nuanced understanding of social recognition and identity, revealing the dialectical nature of their lived experience.
A notable and somewhat unexpected finding in our study, which also challenged our preconceptions of a good life with CHD, is the significance participants placed on a lighthearted attitude as part of a good life with the condition. Previous studies have documented positive psychological consequences of living with CHD, such as personal growth, deeper social relationships, and an increased awareness of priorities (Berghammer et al., 2015; Verstappen et al., 2006). Among these, Berghammer et al. (2015) identified ACHD’s determination to embrace life fully and seek enjoyment. Both themes can be understood as positions along with the ambivalence of acceptance proposed by Berghammer et al. (2006): On the one hand, ACHD acknowledge the limitations imposed by their condition, while on the other, they strive to move forward and live life as fully as possible. This ability to reconcile these seemingly contradictory positions has been described in the literature as existential maturity (Berghammer et al., 2015; McConville, 2021). In pursuit of self-determination and normality, ACHD occasionally choose to set aside concerns about their heart condition, which allows them to experience greater agency.
Agency—the feeling of being able to actively shape one’s own situation—is closely tied to our fourth finding: ACHD’s strong aspiration for autonomy. Standing on their own two feet emerges as a prerequisite for shaping their lives on their own terms. Breaking free from overprotection, taking responsibility for themselves, and managing their CHD both emotionally and practically provide participants with a sense of normality. The struggle for independence has been reported in previous studies (Claessens et al., 2005; Tong et al., 1998). However, our findings highlight not only the emotional strain associated with this struggle but also its profound significance for life satisfaction. Beyond these well-established aspects of autonomy, our study identifies an additional dimension: the fight for autonomy against one’s own body. This is particularly evident in the aspiration to start a family despite medical risks. While not all participants addressed the issue, discussions of reproductive choices surfaced across genders—most notably among women, for whom parenthood often carried particular symbolic and existential weight. For some, the wish to have children was tied to a sense of bodily agency and a desire to overcome medical limitations. Others, by contrast, voiced strong reservations or rejected parenthood altogether, citing fears of genetic transmission or concern for a future child’s QoL. These divergent perspectives underscore the ethical, emotional, and identity-related tensions that accompany reproductive decision-making in the context of CHD (Nebel et al., in press).
Previous research suggests that women with CHD may experience a diminished sense of feminine identity due to the lack of unrestricted reproductive choices (Gantt, 1992). As a result, pregnancy itself becomes a means of asserting autonomy over one’s body (Flocco et al., 2020), symbolizing a deeply personal victory in the struggle for self-determination. In this context, it is not surprising that mothers with CHD report significantly higher scores for functional illness identity states than for maladaptive ones in self-assessment measures (Freiberger et al., 2022).
Strengths and Limitations
Our study has several strengths that enhance the validity, depth, and quality of our findings in line with established general criteria for qualitative research (Cena et al., 2024) and specific criteria for IPA (Nizza et al., 2021). First, with 14 participants, our sample size is relatively large for an IPA, allowing for a nuanced exploration of young ACHD’s perspectives. We initially conducted in-depth case analysis, closely aligned with the participants’ words, before developing PETs and cross-case GETs, ensuring both analytic rigor and sensitivity to convergence and divergence within the data. For example, while certain aspirations, such as the desire to feel “normal” and be treated as such, were widely shared, participants’ experiences diverged in how they navigated interpersonal relationships and engaged with their condition. Lisa-Marie, for instance, described being openly bullied due to visible signs of her condition, whereas Toni expressed frustration about others’ avoidance and silence. In family contexts, Ronja critically reflected on her parents’ overprotectiveness, while André adopted a more reserved stance, also highlighting positive aspects. Similarly, notions of lightheartedness ranged from risk-taking behaviors in Ronja and Juliana, to a more balanced view in Jonas, and a strongly risk-avoidant attitude in Lara. These variations underscore how individual priorities, relational experiences, and temperamental dispositions shape diverse understandings of what it means to live well with CHD.
In terms of transparency, the study was pre-registered in the DRKS (Deutsches Register Klinischer Studien, engl. German Clinical Trials Register) registry and reported in accordance with COREQ (Consolidated Criteria for Reporting Qualitative Research) criteria. Our IPA approach facilitated integration of the experiential “insider” perspective of young ACHD with the professional “outsider” view of the researchers, allowing us to construct a compelling existential narrative of what it means to live a good life with CHD. This narrative unfolded from the participants’ shared sense of being different to their search for normality and lightheartedness, culminating in their pursuit of autonomy.
Reflexivity, a core tenet of IPA, was practiced through regular team discussions and the use of a research diary, critically engaging with how our disciplinary backgrounds, gender, and professional roles shaped data interpretation. The balanced gender distribution ensures that both male and female voices are equally represented.
Moreover, although the sample is homogeneous in terms of its shared diagnosis of CHD, the diversity within this group—including a broad age range, various types and severity levels of CHD, as well as different treatment histories—provides a rich foundation for understanding the varied experiences and perspectives related to living a good life with CHD.
Additionally, we ensured methodological rigor by employing a manualized analysis approach and systematically accounting for potential biases related to the researchers’ gender, age, disciplinary background, and sociocultural perspectives through regular reflexive team meetings and the use of a research diary.
Finally, ethical standards were strictly adhered to throughout the research process, including informed consent, transparency about the study’s aims, and pseudonymization to protect participants’ identities.
Despite these strengths, several limitations must be acknowledged. Although our sample is representative of the general German population in terms of education, it is not representative in terms of cultural diversity: In addition to 13 individuals with a Western European background, the sample included only one participant with a migration background, which limits the generalizability of our findings.
Furthermore, while the internal diversity of our sample is a strength in terms of breadth, it also poses methodological challenges. The variation in age, diagnosis type, severity, and treatment history may limit the comparability of individual accounts and complicate the identification of overarching patterns. To make the complex material analytically accessible, it was necessary to reduce and synthesize the data, which may have led to a simplified representation of particular aspects relevant to specific subgroups—for example, differences related to CHD type or severity. Future research with more targeted subsamples could provide deeper insights into these variations.
Our study contributes to the existing research on QoL in young ACHD by shifting the focus from standardized assessments of well-being to an in-depth exploration of how ACHD themselves define and pursue a good life. While previous studies have primarily examined QoL through quantitative measures, often emphasizing medical and psychosocial risk factors (e.g., Kamphuis et al., 2002; Moons et al., 2005), our findings highlight the subjective aspirations, values, and coping strategies that shape ACHD’s lived experiences. In doing so, we expand on prior qualitative research that describes the ambivalence between illness-related limitations and the pursuit of normality (Berghammer et al., 2006, 2015) by illustrating how autonomy, identity negotiation, and the ability to experience carefreeness play a central role in achieving a fulfilling life. While qualitative studies from Sweden, the United States, the United Kingdom, and Belgium already provide valuable insights, our findings replicate these international studies within a German sample, marking the first qualitative investigation of these themes among young ACHD in Germany. Furthermore, our results underscore the dynamic and fragile nature of autonomy, particularly in the context of medical dependency and evolving life circumstances. By offering a phenomenological perspective, our study provides a deeper understanding of what makes life meaningful for young ACHD—insights that could inform patient-centered care approaches and psychosocial support interventions. Based on our findings, interventions that empower individuals in their pursuit of autonomy and support them in pushing their boundaries while building self-confidence emerge as particularly valuable.
Conclusion
Our study provides new insights into how young ACHD conceptualize a good life, highlighting the central role of autonomy, normalization, and identity negotiation. While previous research has primarily focused on QoL in terms of medical outcomes and psychosocial risk factors, our findings emphasize the subjective aspirations and coping strategies that shape ACHD’s pursuit of fulfillment. The desire to stand on one’s own two feet reflects a deeper need for self-determination, which is not only challenged by external factors such as overprotection but also by the limitations imposed by their own bodies. At the same time, our results show that moments of carefreeness and a lighthearted approach to their condition are crucial for maintaining agency and well-being.
These findings have important implications for clinical practice and psychosocial support. A more nuanced understanding of ACHD’s lived experiences can help healthcare providers foster autonomy, encourage open communication, and create interventions that acknowledge both the challenges and strengths of this group. Future research should explore the diverse influences on ACHD’s life perspectives in more culturally and socially diverse samples and examine how individual trajectories shape long-term well-being.
Footnotes
Acknowledgments
We sincerely thank the participants for their willingness to share their personal experiences and contribute to this study. Our appreciation also goes to the supporting departments and the patient organizations involved in the recruitment process, whose assistance was invaluable. Lastly, we gratefully acknowledge the insightful discussions and collegial input provided by members of the DFG Research Group 5022, which enriched the development of this work.
Ethical Considerations
Our study was approved by the Ethics Committee of the University Medical Center Göttingen (approval no. 18/8/20). Participants provided written informed consent prior to study enrollment. The study protocol was drafted in accordance with the Declaration of Helsinki and approved by the responsible ethics committee on 19.01.2022. Registration took place on 18.02.2022 at the German Clinical Trials Register (DRKS; project no. DRKS00028096).
Author Contributions
C.H.-L. and D.B. contributed to study conception and design. D.B. and L.N. recruited participants, and collected, analyzed, and interpreted the data. L.N. drafted the manuscript. All authors critically revised it and gave final approval.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This publication was created as part of the Research Group 5022 “Medicine, Time and the Good Life” (Speaker: Claudia Wiesemann, University Medical Center Göttingen), funded by the German Research Foundation (DFG), project number 424883170. Open Access funding was enabled and organized by Project DEAL.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: C.H.-L. has received personal royalties for the German version of the Hospital Anxiety and Depression Scale from the publisher Hogrefe-Huber, personal lecture fees from Novartis, as well as from sponsors of non-industry-dependent training events, and institutional research funding from the BMBF, DFG, and EU Commission over the past 3 years. The other authors declare that they have no competing interests.
