Abstract
Keywords
Obsessive-Compulsive Disorder (OCD) is a chronic illness with 12-month prevalence in the United States of 1.2% (American Psychiatric Association, 2022) and a lifetime prevalence of 2–3% (Ruscio et al., 2010). Furthermore, the World Health Organization has designated OCD as one of the most debilitating global diseases (Mathews, 2021). Ruscio et al. (2010) found subclinical OCD symptoms are more prevalent than previously expected, which indicates OCD might cause a more significant public health burden than the prevalence rates would suggest. Even so, OCD has been found to have a considerable socioeconomic burden on society, impairments in quality of life, and impacts on family functioning (Hollander et al., 2016). Furthermore, in the 5th edition of the American Psychiatric Association's Diagnostic and Statistical Manual of Mental Disorders (2013), OCD was removed from anxiety disorders chapter and assigned a separate chapter, which exemplifies its growing clinical significance in practice and research.
Hollandar et al. (2016) examined the costs of OCD and uncovered a considerable socioeconomic burden to society, impairments in occupational domains, and comparable degrees of impairment in family functioning and quality of life to that of schizophrenia. Greater than 30% of individuals with OCD are underemployed or unemployed (Mathews, 2021), which further contributes to impairments in quality of life, burdens on caretakers and family, and the growing direct and indirect societal costs of OCD. Furthermore, in the United States, an annual estimated $40 billion USD is spent by employers on sick pay for employees with OCD who are unable to work (Hollandar et al., 2016). In comparison, a total of $10.6 billion USD is spent on OCD-specific treatment annually (Hollandar et al., 2016). This apparent gap in spending displays a trend of the socioeconomic impacts of OCD and the lack of engagement in effective treatment.
Background on Exposure and Response Prevention
Exposure and Response Prevention (ERP) is a cognitive-behavioral research-based practice for the treatment of OCD that entails systematic, repeated, and prolonged interaction with stimuli that induce distress and the urge to engage in compulsive rituals (Abramowitz et al., 2009). In conjunction with this exposure component of ERP, the imperative response prevention component entails abstaining from compulsive rituals which serve as a maladaptive coping mechanism (Bornheimer, 2015). This form of treatment is a highly collaborative experience between clinician and client. Rigorous randomized controlled trials have added to ERP's effectiveness, which is how ERP earned its standing as the gold standard treatment for OCD (Abramowitz, 2006; Abramowitz et al., 2009). Meta-analyses examining the effectiveness of ERP in the treatment of OCD display its overall efficacy and superiority over alternative therapeutic modalities, including relaxation training and nonexposure-based approaches (McKay et al., 2015). Patient response rates to ERP have been demonstrated as high as 86% (Franklin et al., 2000), ERP has shown effectiveness at reducing OCD symptom severity by 50–60% and has produced sustained improvements lasting for more than two years after treatment (Abramowitz et al., 2009).
Despite that ERP is the research-supported recommended treatment for OCD, those suffering from OCD often do not receive any treatment, or when they do, they receive treatments other than ERP (Schwartz et al., 2013). A seminal study on the impacts of OCD found, on average, individuals with OCD do not receive OCD-specific treatment until 17 years after the onset of their symptoms and 11 years after meeting full diagnostic criteria for the disorder (Pinto et al., 2006). Subsequent exploration into the duration of untreated illness (DUI) refined the average to 7–11 years and exemplified high rates of undertreatment and prolonged suffering of individuals with OCD (Altamura et al., 2010; Dell’Osso et al., 2010, 2015, 2019). There are effective research-based psychotherapy and pharmacotherapy treatments available for OCD, although many who suffer from this disorder experience it as a chronic and debilitating illness, often due to low availability of effective treatment (Abramowitz et al., 2009; Franklin & Foa, 2021). Of treatment-seeking individuals with OCD, only 10–30% receive research-based psychotherapy, such as ERP (Schwartz et al., 2013). Fewer than one-third of community mental health providers report providing exposure-based methods to clients with anxiety disorders (Hipol & Deacon, 2013). Despite substantial evidence of ERP's effectiveness in treating OCD (Abramowitz, 1997; Franklin & Foa, 2021; Ojalehto et al., 2020; Olatunji et al., 2013), it is underutilized, and when utilized, is often delivered in suboptimal ways (Deacon et al., 2013; Pittig et al., 2019).
Negative Beliefs and Attitudes Toward ERP
Pittig et al. (2019) studied an association between the underutilization of exposure therapy with negative beliefs and perceived practical barriers among a population of outpatient psychotherapists in Germany with training in behavioral therapies, such as exposure-based interventions and cognitive-behavioral therapy. Therapist-held feasibility issues and therapist willingness to use exposure therapy were significant barriers to the dissemination of this research-based practice (Pittig et al., 2019), which can contribute to the underutilization or suboptimal use of exposure therapy. Similarly, clinicians who report global negative beliefs about exposure therapy are less likely to use ERP in the treatment of OCD (Deacon et al., 2013; Deacon & Farrell, 2013; Farrell et al., 2013; Hipol & Deacon, 2013; Keleher et al., 2020; Pittig et al., 2019; Richard & Gloster, 2007). Commonly held negative beliefs by mental health professionals are that the client will decompensate, symptoms will worsen, the client will be psychologically harmed, the therapist will experience vicarious trauma, and the therapist could face malpractice litigation (Deacon et al., 2013). Furthermore, many therapists view exposure-based therapies as inherently unethical and unacceptably aversive to clients (Deacon et al., 2013). Further, some therapists view exposure as insensitive to a client's unique needs and require simultaneous relaxation strategies to make exposure safe and tolerable, which is a form of less effective and nonresearch-based exposure therapy (Deacon et al., 2013).
Beliefs and attitudes toward a behavior are fundamental components of Theory of Planned Behavior (TPB) (Ajzen, 1991). This theory hypothesizes that intentions to perform specific behaviors are the strongest predictor of a behavior. As it relates to ERP, intention refers to a clinician's reported willingness to implement ERP among their patients with OCD. In turn, intentions are predicted by understanding one's attitudes toward the behavior, subjective norms, and perceived behavioral control (Ajzen, 1991). In addition to perceived behavioral control, defined as behavior under volitional control that a person can decide to enact or not, the remaining two behavioral determinants influencing behavioral intention are one's attitudes toward the behavior and subjective norms (Ajzen, 1991). Examples of how these factors relate to the use of ERP are the following. A favorable expectation and belief in the mechanisms of ERP would exhibit a positive attitude, the expectations that professional peers use and favorably support the research-base of ERP implicates the impact of shared social norms, and a clinician's views on their practical ability to use ERP showcases their perceived behavioral control to do so.
Much of the work conducted by Deacon et al. (2013) and Pittig et al. (2019) examined attitudes and beliefs determinants of behavioral intentions. Pittig et al. (2019) additionally explored what TPB would consider some of the nonmotivational factors. These factors comprise requisite opportunities and resources, including time, finances, skills, and cooperation of others (Ajzen, 1991). Theory of Planned Behavior further elaborates that to the extent an individual has these nonmotivational factors and resources and they intend to perform the behavior, then they are expected to succeed in following through on the specific behavior (Ajzen, 1991). Therefore, behavioral intention is exemplified as a measure that accurately predicts the performance of a behavior.
The literature concerning the general use of research-supported practices by clinical social workers displays a trend of negative attitudes and beliefs, resulting in underutilization and barriers to implementing EBPs (Bellamy et al., 2006; Tennille et al., 2016). Bellamy et al., (2006) reports that some social workers believe research-based practices are too broad and incongruent with a client's cultural needs. Other social workers experience a degree of suspicion toward research-based practices as a cost-cutting tool that does not consider a client's unique presentation and maintain perceptions on implementation challenges in their clinical work settings (Bellamy et al., 2006). This finding is amplified by The Substance Abuse and Mental Health Services Administration report displaying clinical social workers as predominant providers of psychotherapy in treating mental illnesses in the United States (Bellamy et al., 2006). As predominant providers of psychotherapy, it is imperative to be cognizant of their clinical intentions toward ERP and the treatment of OCD. Social workers can be found in a diverse array of clinical settings and therefore will routinely encounter individuals presenting with symptoms of OCD. Thus, furthering the importance of understanding their intentions, attitudes, shared norms, and knowledge of ERP and OCD.
The trends in negative beliefs and attitudes about research-based practices, in addition to the knowledge required to implement them, highlight some of the issues regarding their degree of utilization in the field of behavioral health (Mah et al., 2020; Shafran et al., 2009; Tennille et al., 2016). The awareness of ERP as a research-based practice for the treatment of OCD is far from new information in the field of clinical social work (Steketee, 1987). However, in-depth education and training on OCD and research-based modalities, such as ERP, are not commonplace in social work courses. Academic calls for clinical social workers to seek out formalized training in ERP have been made (Bornheimer, 2015) in response to the growing awareness of the significant impacts OCD can have on quality of life, as well as the lack of specialists trained in ERP to provide care to the large prevalence of individuals living with OCD. Self-guided clinical handbooks are accessible to clinical social workers, and more structured training opportunities are available through the International OCD Foundation, Massachusetts General Hospital Psychiatry Academy, and the Center for the Treatment and Study of Anxiety at the University of Pennsylvania. While social workers can gain training and experience through these avenues, there is a gap in research concerning clinical social workers and their specific intentions to use ERP in treating OCD. It is this gap that this novel study sought to explore and add knowledge to the literature on OCD and social work practice.
To reduce the trends of ineffective treatment of OCD and negatively held beliefs and norms about exposure-based therapy, it is essential to understand the intentions of clinical social workers that direct their choice to use ERP. Previous research has explored the impact of negative attitudes and perceived practical barriers to implementing ERP, but a gap remains in the literature concerning the degree to which clinical social workers and their specific attitudes, norms, perceived behavioral control, and knowledge explain their intentions to use ERP in treating OCD. Guided by TPB, we explored the following 11 hypotheses:
Clinical social workers who endorse more positive attitudes, greater perceived behavioral control, and more influential subjective norms would have greater behavioral intentions of using ERP to treat OCD. Clinical social workers who used ERP within the past year would have more favorable attitudes toward ERP than those who did not. Clinical social workers who used ERP within the past year would have greater perceived behavioral control to use ERP than those who did not. Clinical social workers who used ERP within the past year would have more influential subjective norms toward ERP than those who did not. Clinical social workers who used ERP within the past year would have greater behavioral intention to use ERP than those who did not. Clinical social workers who used exposure therapy within the past year would have more favorable attitudes toward ERP than those who did not. Clinical social workers who used exposure therapy within the past year would have greater perceived behavioral control to use ERP than those who did not. Clinical social workers who used exposure therapy within the past year would have more influential subjective norms toward ERP than those who did not. Clinical social workers who used exposure therapy within the past year would have greater behavioral intention to use ERP than those who did not. Clinical social workers who used ERP within the past year would have greater knowledge than those who did not. Clinical social workers who used exposure therapy within the past year would have greater knowledge than those who did not.
Methods
Parent Study
The parent study of this investigation was a randomized controlled trial conducted online, using a randomized distribution implemented by Qualtrics. Research participants randomly assigned to experimental group were provided with an informational fact sheet on ERP's effectiveness in treating OCD before the administration of study measures. Control group participants were administered study measures at the onset before they were provided the informational fact sheet. The control group received the same experimental intervention but at a delay and after all outcome measures were obtained. The fact sheet contained diagnostic information on OCD, defining characteristics of what ERP is and how it works, information on efficacy of ERP, and therapeutic benefits of ERP. For purposes of answering the research questions for the present analyses, the respondents for both conditions were combined. Moderation sensitivity analysis was conducted to ensure the two groups from the parent study could be combined. Group assignment was nonsignificant and the fact sheet was not associated with any differences in constructs evaluated in the study (attitudes [t(156) = 1.31, p = 0.19], behavioral control [t(163) = 0.70, p = 0.48], subjective norms [t(165) = −0.76, p = 0.45], behavioral intentions [t(157) = 0.70, p = 0.48], or knowledge [t(158) = 0.90, p = 0.37]). Accordingly, for purposes of the present analyses, both groups were combined into one, but experimental/control condition was included as a covariate. The Institutional Review Board at the University of Pennsylvania approved the study. The authors had no conflicts of interest or funding for this research.
Sampling
Recruitment began in January 2024. Eligible participants were clinical social workers in the United States with a master's degree or higher in social work. Using an IRB-approved flyer, participants were recruited through social media and professional listservs. Participants completed informed consent and surveys of intentions, attitudes, social norms, behavioral control, and knowledge about ERP. All participants were offered the opportunity to enter a raffle for one of four $50 Amazon gift cards. Recruitment closed after 10 weeks with a study population of 168.
Measures
The Intention Scale for Providers-Direct Items (ISP-D14) was used to measure TPB components. The ISP-D14 is a revised and abbreviated psychometric measure from the 70-item ISP developed to measure constructs of TPB in the context of mental health clinicians using research-based practices (Burgess et al., 2017). The ISP-D14 has four subscales measuring attitudes, subjective norms, perceived behavioral control, and behavioral intention. The ISP-D14 demonstrated convergent validity patterns with the Evidence-Based Practice Attitude Scale (EBPAS) (Hill et al., 2021), which is the most well-tested psychometrically sound measure employed to evaluate therapist attitudes toward using research-supported treatments (Mah et al., 2020). However, the EBPAS does not specifically assess the remaining three constructs of the TPB (e.g., perceived behavioral control, social norms, and behavioral intentions) as the ISP-D14 does (Mah et al., 2020). The ISP-D14 is a newly constructed measure with varying reliability and has only recently been utilized in empirical studies, including the psychometric evaluation by Mah et al. (2020) employing a multidisciplinary population of public sector youth mental health therapists in Hawaii to evaluate research-based practices in general. Cronbach's alpha coefficients were calculated for the four subscales of the 14-item ISP-D14 to test its reliability. The behavioral intentions subscale (α = .84) met the benchmark for good reliability, the attitudes subscale (α = .75) and subjective norms subscale (α = .72) both had acceptable reliability, and the perceived behavioral control subscale (α = .63) qualified for questionable reliability (0.6 ≤ α < 0.7) (Mah et al., 2020). Its strength in directly measuring the constructs of TPB in a brief manner that did not overburden participants determined its selection.
Cronbach's alpha reliability was calculated for this study sample on the four subscales of the ISP-D14. Reliability of attitudes scale had Cronbach's alpha = 0.59, which is considered unacceptable; behavioral control scale was Cronbach's alpha = 0.46, considered unacceptable; subjective norms scale Cronbach's alpha = 0.70, considered acceptable; Behavioral intention scale was Cronbach's alpha = 0.88, considered good.
The knowledge variable was measured by a novel knowledge quiz on ERP's effectiveness in treating OCD, developed by the first author of this study. Five mental health professionals reviewed the knowledge quiz during development to evaluate it for clarity and understanding. Knowledge was scored as a summation of 10 questions which were based on information presented in the ERP fact sheet. Reliability of the knowledge scale was Cronbach's alpha = 0.76, which is considered acceptable. Additional information was obtained, including previous clinical experience using ERP or exposure-based therapies in general as well as sociodemographic information, such as age, gender, race, years of clinical experience, and education.
Data Analysis
The data were analyzed using IBM SPSS Statistics version 29. Initial descriptive statistics were conducted. A multiple regression analysis model was used with behavioral intention to use ERP as the dependent variable. Independent variables were social norms, perceived behavioral control, attitudes about ERP, age, clinical experience, use of ERP, and use of exposure therapy. Group assignment (treatment or control) was included as a covariate.
Independent t-tests were used to compare mean scores of each dependent variable based on the use of ERP and exposure-based modalities in the previous year and to test the impact of knowledge on behavioral intention.
Results
Sample Characteristics
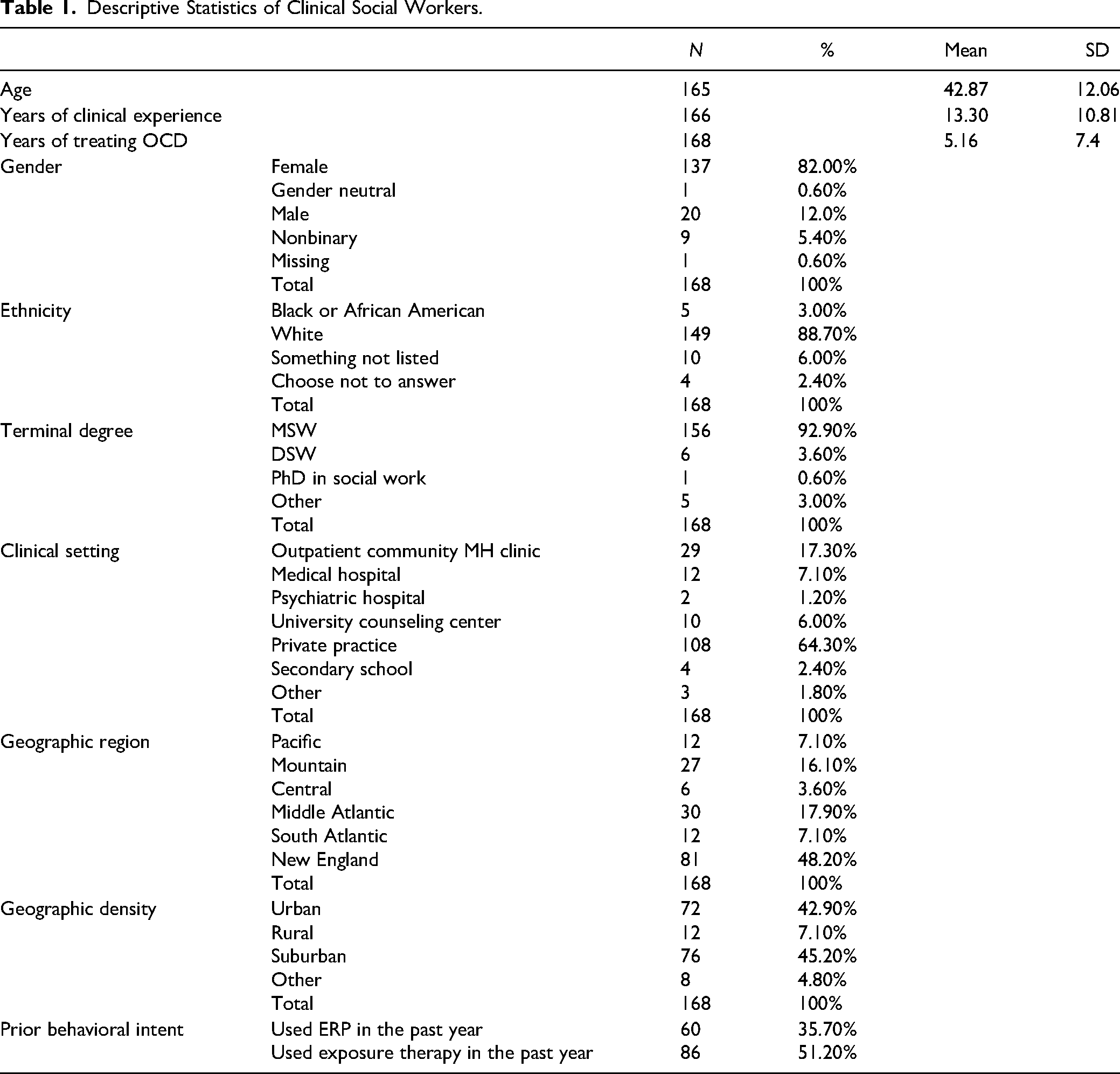
Participants were primarily women (n = 137, 82%), and almost all reported their race as White (n = 149, 89%), and the median age was 41 (SD = 12.06), with 13 years (SD = 10.81) of clinical experience, and mean of 5 years (SD = 7.4) of experience treating clients with OCD (see Table 1). The majority of participants were clinicians in private practice (n = 108, 64%), followed by clinicians working in outpatient community mental health clinics (n = 29, 17%), and about one-third (36%; n = 60) reported using ERP within the past year, and half (51%; n = 86) reported to have used exposure therapy in the past year. Almost half of the participants work in New England (n = 81, 48%), followed by 18% in the Middle Atlantic region (n = 30). The overwhelming majority of participants (n = 148) work in either suburban (n = 76, 45%) or urban (n = 72, 43%) settings (see Table 1 for details).
Descriptive Statistics of Clinical Social Workers.
Influences on Behavioral Intention
Multiple regression analysis explained 56% of the variance in behavioral intention with attitude, behavioral control, and subjective norms all significantly predicting changes in behavioral intention at a confidence interval of 95% (α = .05) (see Table 2). For every additional point in attitude, behavioral intention increased by ∼½ a point (B = 0.48, p = 0.01; β = 0.35), which equates to a medium effect size (Cohen, 1988). For every additional point in behavioral control, behavioral intention increased by ∼½ of a point (B = 0.41, p < 0.001; β = 0.25), which equates to a small effect size (Cohen, 1988). For every additional point in subjective norms, behavioral intention increased by ∼½ a point (B = 0.51, p = 0.01; β = 0.50), which equates to a large effect size (Cohen, 1988). These findings support hypothesis 1.
Multiple Regression Analysis of Behavioral Intention Among Clinicians.
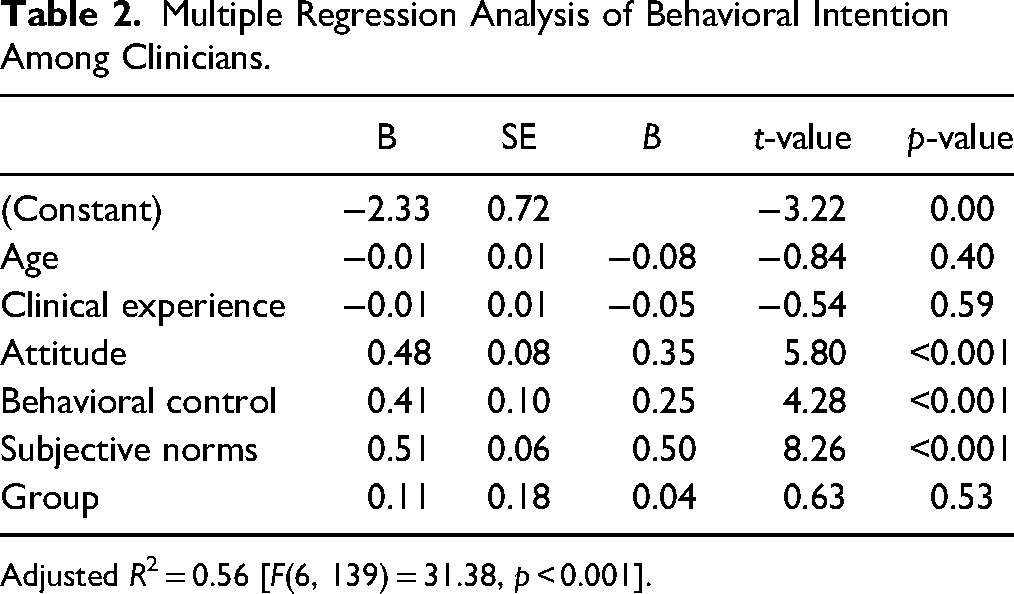

Adjusted R2 = 0.56 [F(6, 139) = 31.38, p < 0.001].
Impacts of Previous Behavior
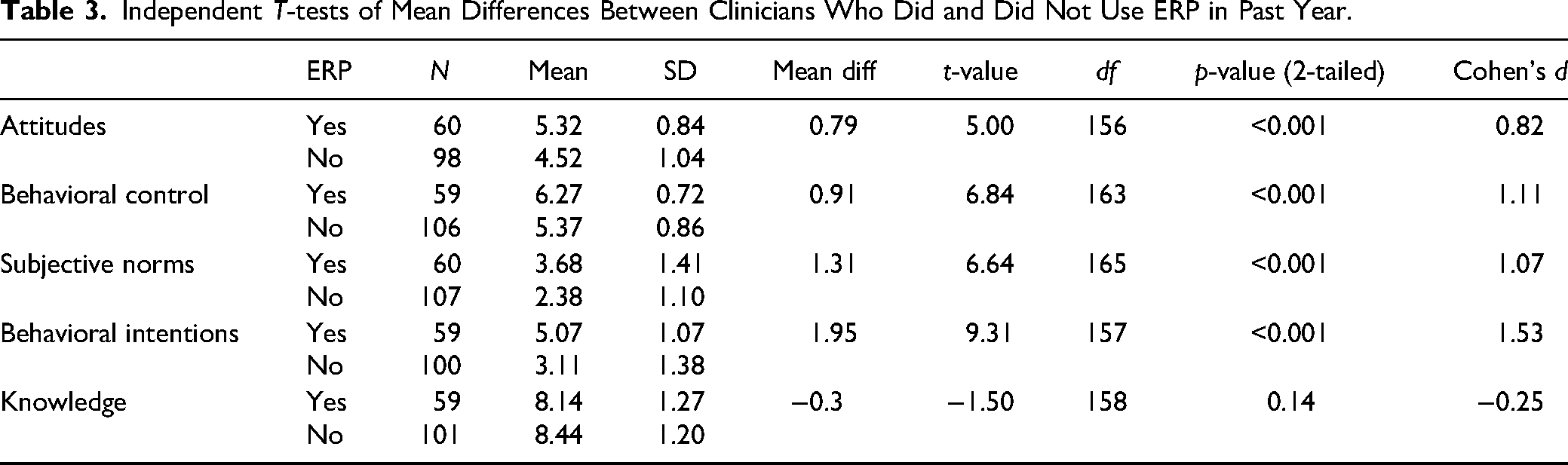
Social workers who reported using ERP in the past year (36%, n = 60) reported higher scores on attitudes [5.32, 0.84; 4.52, 1.04; t(156) = 5.00, p < 0.001], which supports hypothesis 2. Social workers who reported using ERP in the past year indicated greater perceived behavioral control [6.27, 0.72; 5.37, 0.86; t(163) = 6.84, p < 0.001], which supports hypothesis 3. Social workers who reported using ERP in the past year reported more influential subjective norms [3.68, 1.41; 2.38, 1.10; t(165) = 6.64, p < 0.001], which supports hypothesis 4. Social workers who reported using ERP in the past year indicated greater behavioral intentions [5.07, 1.07; 3.11, 1.38; t(157) = 9.31, p < 0.001] than those who did not use ERP in the past year, which supports hypothesis 5 (see Table 3).
Independent T-tests of Mean Differences Between Clinicians Who Did and Did Not Use ERP in Past Year.
Social workers who reported using exposure therapy in the past year (51%, n = 86) indicated higher scores on attitudes [5.12, 0.94; 4.50, 1.05; t(156) = 3.86, p < 0.001], which supports hypothesis 6. Social workers who reported using exposure therapy in the past year determined to have greater perceived behavioral control [6.11, 0.78; 5.26, 0.86; t(163) = 6.66, p < 0.001], which supports hypothesis 7. Social workers who reported using exposure therapy in the past year indicated more influential subjective norms [3.35, 1.38; 2.32, 1.15; t(165) = 5.22, p < 0.001], which supports hypothesis 8. Social workers who reported using exposure therapy in the past year had greater behavioral intentions [4.71, 1.28; 2.87, 1.31; t(157) = 8.91, p < 0.001] than those who did not use exposure therapy in the past year, which supports hypothesis 9 (see Table 4).
Independent T-tests of Mean Differences Between Clinicians Who Did and Did Not Use Exposure Therapy in Past Year.
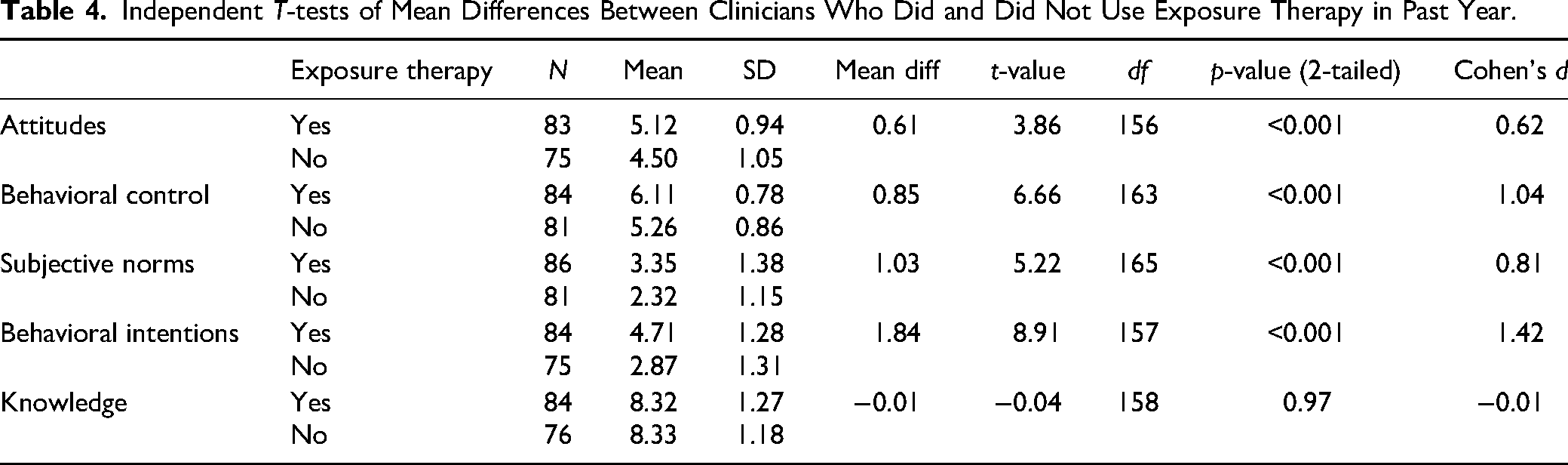
Independent t-tests found no significant difference between social workers who reported using ERP in the past year and those who did not on knowledge [t(158) = −1.50, p = 0.14], which does not support hypothesis 10. Independent t-tests found no significant differences between social workers who reported using exposure therapy in the past year and those who did not on knowledge [t(158) = −0.04, p = 0.97], which does not support hypothesis 11.
Discussion and Applications to Practice
We hypothesized that clinical social workers who endorsed higher levels of perceived behavioral control, more positive attitudes, more influential social norms, and greater knowledge would have higher behavioral intentions of using ERP to treat OCD when controlling for experimental/control conditions. Furthermore, we hypothesized that social workers with prior behavioral intent, as measured by the reported use of ERP and exposure therapy in the past year, would have greater behavioral intention to use ERP to treat OCD than those who did not. This study found significant findings on the influence of perceived behavioral control, attitudes, subjective norms, and past behavioral intent on behavioral intention of using ERP to treat OCD among a population of clinical social workers. There was no significant influence of knowledge on behavioral intention to use ERP.
The results of this study support the findings by Deacon et al. (2013) and Pittig et al. (2019), such that more favorable attitudes about ERP and lower practical barriers correlated with greater utilization of ERP to treat OCD. Additionally, the study found that the influence of social norms produced a large effect on behavioral intention to use ERP. However, study findings provide unique information about the specified population of clinical social workers, and more specifically, measured behavioral intention in addition to the remaining TPB components, which is relevant for filling gaps in research knowledge on the implementation of ERP and exposure-based modalities in the treatment of OCD and anxiety disorders. Findings on the influence of TPB factors on these clinical social workers’ behavioral intention to use ERP in treating OCD fill this important gap in the literature.
Previous behavior was measured within the sample to establish a behavioral baseline of those who have used ERP or an exposure-based modality within the past year. Collecting this information was essential to understanding participants’ clinical decision-making and influences of prior behaviors. A larger percentage of participants reported using general exposure therapy than those who used ERP in the past year. Findings indicate that participants who used ERP in the past year had more favorable attitudes, influential social norms, and greater perceived behavioral control when compared to those who, in the past year, reported they did not use ERP. Therefore, participants who, within the past year, used ERP, can be viewed as having previous behavioral intent, and had significant differences in this influential component of TPB. These findings provide a few essential points to understand. First, it not only displays a trend of clinical social workers who have used ERP in the past year as having more influential components of TPB but it predicts a trend in clinical decision-making that those who have used ERP within the past year are planning to continue using ERP. Past behavior does not always predict future behavior. Still, the responses from these clinicians exemplify their favorable views toward ERP and their sense of self-agency in treatment planning and implementing this research-based modality. Findings further suggested that clinical social workers who have used ERP within the past year not only have favorable attitudes and perceived behavioral control to use this research-based modality but are also in contact with colleagues who have favorable views, as evidenced by social norm scores for study participants. These findings suggest an overlap between intrapersonal and interpersonal influences on clinical decision-making. These clinicians endorsed having intention to use ERP to treat OCD and having the belief that their professional peers’ support will encourage them to use ERP, as indicated in the significant and large effect of social norms.
Furthermore, the study findings on clinicians who used general exposure therapy in the past year as having more influential components of TBP, including behavioral intention to use ERP, is another important discovery. These clinicians have made the previous choice to use general exposure therapy while also having significantly greater behavioral intention to use ERP than those who did not use general exposure therapy. These findings are significant in understanding a subgroup of clinicians who could be open to implementing the research-based practice of ERP but presently fall short of making the treatment decision to implement this therapeutic modality.
Results align with the theoretical foundation of TPB and further affirm the relevance of understanding how these components impact social workers’ clinical decision-making and behavioral intentions when assessing and intervening with OCD client populations. This information is highly relevant to clinical practice because it provides an empirical understanding of both utilization and underutilization of this research-based practice that can impact the chronicity and severity of OCD, which otherwise could be more effectively treated to reduce the prolonged pain and suffering of individuals who go untreated or undertreated.
This study expands the literature on the utilization of the research-based practice of ERP in the treatment of OCD. The study adds specificity to this growing area of research by narrowing its focus to the field of clinical social work. Clinical social workers in various geographic and clinical settings participated in this research study, which uncovered relevant and applicable information on clinical decision-making and behavioral intentions. The specificity of this population supported the enhancement of the knowledge base and empirical literature on social workers’ clinical decision-making in the treatment of OCD.
The study aimed to examine the extent to which TPB components influence a clinical social worker's behavioral intention to use ERP in treating OCD. As Ajzen (1991) theorized, the greater one's intention is to enact a behavior, the greater the likelihood that the behavior will be implemented. Having an empirical understanding of the ways that the TPB mechanisms influence the use of the research-based modality of ERP to treat OCD is valuable knowledge for clinical practice settings. This information can be impactful in clinical settings, including outpatient community mental health clinics and private practice, as well as in educational settings, including social work courses and professional continuing education agencies. The findings on the influence of interpersonal and intrapersonal factors on the use of ERP to treat OCD hold the potential to make meaningful impacts. For example, the large effect found in the influence of subjective norms could sway social workers in outpatient group practices or private practices who hold negative attitudes toward ERP. If these clinicians were engaged in clinical consultation with colleagues who hold more favorable attitudes toward ERP, this could influence the belief system and behavioral intention of those who had previously been uninterested or opposed to utilizing ERP. This shift could disrupt the perpetuation of the trend of underutilization of this research-based practice. Similarly, if continuing education agencies could introduce alternative ways of viewing the practice of ERP, this could counter the negative attitudes toward ERP, such as it is unethical and unnecessarily adverse to the client, and it could influence practitioners’ belief system toward ERP, resulting in the potential of shifts in utilization rates.
Clinical practice classes that provide a cursory overview of research-based practice for common mental health disorders found in children and adult populations are commonplace in MSW programs. However, what is less typical is in-depth elective courses that go beyond Cognitive-Behavioral Therapy and provide MSW students with more specialized information and knowledge about ERP. Taking the findings from this study, such as the interplay among TPB factors and their impact on behavioral intentions, and integrating them into the curriculum of MSW programs could facilitate meaningful changes in the awareness and utilization of ERP to treat OCD. As previously discussed, the DUI is staggering, and like many mental health disorders, early intervention can create a profound impact on the chronicity and severity of OCD. Therefore, if MSW students had the opportunity to take a course that provides objective evidence and research on ERP, this could shift the influential factors on behavioral intention by intervening at this pivotal stage in their professional and educational development. In doing so, there could be more widespread benefits for individuals suffering from the debilitating symptoms of OCD.
This present study provided valuable knowledge to the clinical social work field and the growing literature base investigating trends of underutilization of exposure-based therapies. The findings epitomize the significant influence attitudes, perceived behavioral control, and social norms have on behavioral intention in the context of clinical decision-making in the treatment of OCD. These findings align with the theoretical foundation of TPB and further affirm the relevance of investigating the extent to which these components impact social workers’ clinical decision-making and behavioral intentions when assessing and intervening with OCD client populations, which routinely occurs given the prevalence rates of the disorder and the predominant role social workers play in the landscape of psychotherapy services in the United States. This present study exemplifies that in the growing research field exploring implementation barriers in the use of exposure-based modalities and implementation science, TPB constructs are highly relevant in understanding the behavioral intentions of clinical social workers when treating OCD. Until this present research study, clinical decision-making on the use of ERP to treat OCD has not been researched in an exclusive population of clinical social workers.
There were a few study limitations. First, the parent trial was designed to evaluate the impact of a fact sheet on knowledge and TPB constructs; the fact sheet was not associated with differences in key constructs, though it is possible the collapsing across both groups might have altered the pattern of findings. The nonsignificant findings on knowledge are a likely result of a poor measure. The average knowledge score was high, which indicates it was an ineffective measurement tool. Future studies can examine means of developing a more challenging knowledge quiz, which could be a more accurate way of measuring participant knowledge of OCD and ERP.
In addition, most of the participants identified as White women from New England who worked in private practice, which limits the generalizability of the study. The research was designed to evaluate the beliefs of social workers, who are a critical mass of clinicians in the mental health sector, but as a result, findings might not translate to other professionals.
Another study limitation was the weakness found in Cronbach's alpha reliability scores of the ISP-D14. Findings from the study come with caution because of the varying levels of reliability. The psychometric evaluation by Mah et al. (2020) depicted this measurement tool as an effective and promising way of evaluating the specific components of the TPB, which were not fully measured in more established measurement tools, such as the EBPAS. However, the specific application of the ISP-D14 proved less reliable than anticipated. Future research could explore ways to strengthen the reliability and construct validity of the ISP-D14. Altering low-reliability items and adding new items can progress the exploration of the components of the TPB in the context of clinical social workers’ behavioral intention to use ERP to treat OCD. Further exploration into an improved measure that can reliably measure these concepts is another point of exploration for future research.
Another potential limitation was the chance of biased recruitment of participants. The recruitment flyer informed prospective participants that the study sought to learn more about the role of clinicians’ intentions and influences on their clinical decision-making in the treatment of OCD. As a result, prospective participants who were initially interested in OCD might have been disproportionately drawn to the study.
Conclusion
Greater perceived behavioral control, favorable attitudes, and shared social norms increased social workers’ behavioral intention to use ERP when treating OCD. Those who reported using ERP or exposure therapy within the past year scored higher on all of these influential factors impacting behavioral intention to use ERP compared to social workers who did not use these therapeutic interventions. Future research directions include testing the theoretical framework with more diverse populations to continue examining implementation barriers to the use of ERP to treat OCD. An additional direction for future research is to investigate further the subgroup of clinicians who expressed influential components of TPB, including the behavioral intention to use ERP, but in the past year elected to use general exposure therapy instead of this research-based practice.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
