Abstract
Employers sometimes hinder the appropriate reporting of claims to workers' compensation, a phenomenon termed claim suppression. While the magnitude of claim suppression is difficult to quantify, various reports have identified it as a significant concern. In response, several Canadian jurisdictions, such as Ontario in 2015, introduced legislation addressing claim suppression. This article first discusses the legislative and policy context that influences claim suppression in Ontario, including concerns concerning the scope, interpretation, and enforcement of the law. It then presents qualitative findings from a community-based study with members of the Toronto Bangladeshi immigrant community that documented varied forms of employer claim suppression in precarious work, as well as facilitators of claim suppression within the workers' compensation and health care systems. Our findings and those of other research suggest that the scope of claim suppression is broader than that contemplated by the legislation. Our article proposes recommendations for the conceptualization of claim suppression and for legislation, policies, practices, and interventions that are grounded in workers' lived experiences.
Keywords
Introduction
Claim suppression is generally defined as the phenomenon whereby employers hinder the appropriate reporting of work injury and illness claims to workers' compensation.1,2 In Canada, workers' compensation boards are provincial and territorial employer-funded systems that provide workers with benefits and services in the event of a work injury of illness. 1 Employers engage in claim suppression to reduce or avoid increases in their workers' compensation premium costs. In the 1970s and 1980s, compensation boards in Canada and other countries introduced and expanded experience-rated premium plans. These plans compared similar work and issued employers premium rebates or assessed them surcharges for lower- or higher-than-average workers' compensation costs.3,4 While this approach was intended to create an economic incentive for employers to make workplaces safer, critics have argued that experience rating instead resulted in aggressive claim suppression by employers to reduce premium costs.3,5,6 The financial incentive to suppress claims is greater for claims that involve a work absence (known as lost-time claims), which more significantly impact costs. Concerns with the perverse effects of experience rating of employer premiums have been expressed for decades by researchers,3,7,8 unions,9–11 injured workers' advocates,12,13 and experts appointed to review workers' compensation systems. 14
Employer claim suppression takes several forms. It may involve failing to report, actively blocking a claim, or understating an injury or illness' severity or duration.1,2 Actions may be overt, such as making threats, or subtle, such as offering workers wages in lieu of benefits they would receive if they submitted a claim.1,7,9,10,15 The currently accepted defining feature of claim suppression is the intent by employers to prevent appropriate reporting.2,7 As such, claim suppression is distinct from worker underclaiming (nonclaiming or abandoning claims) and employer underreporting (nonreporting or misreporting claims). Without employer intent, these events are not typically considered claim suppression.2,7
Underclaiming by workers and underreporting by employers are common occurrences. 2 In Canada, high rates of nonclaiming ranging from 40% to 54% have been found, with claiming rates lower among those who experience less severe injuries or lack knowledge about occupational health and safety rights.15–18 At the same time, two Canadian surveys have estimated the incidence of employer nonreporting at approximately 7–8% of compensable injuries and illnesses.19,20 Studies have also found that up to 35% of no-lost-time claims may be incorrectly reported as such by employers to minimize the premium surcharge costs.1,15,17 These and related findings 21 indicate that a large number of work injuries and illnesses are underclaimed or underreported. The magnitude of claim suppression and its contribution to these statistics are difficult to assess due to the fact that it is a phenomenon intended by employers to be hidden.1,2 A 2020 British Columbia study based on a survey of 699 workers with a self-reported work injury or illness within the past 3 years estimated the incidence of claim suppression to be between 3.7% and 13%. 17 In Manitoba, a survey of 200 workers found that 11.5% had experienced or were aware of overt claim suppression practices by employers. 15
For decades, qualitative occupational health research in Canada and other countries has discussed the pressure on workers from employers not to report injuries or illnesses to workers' compensation.22–27 Research has outlined specific employer strategies, both overt (terminating employment, threatening repercussions, etc.)9,28–31 and subtle (paying wages in lieu of filing a claim, using return-to-work schemes to avoid claims or reduce costs, etc.).7,9,25,30–33 Studies have also identified “gaming the system” employment strategies, such as hiring workers through temporary employment agencies, which are typically considered the employer and thus responsible for workers' compensation premiums,30,34 and the misclassification of workers as independent contractors, who are responsible for their own premium costs, as forms of claim suppression. 31
Claim suppression also has important equity dimensions, as evidence suggests that underclaiming/reporting are commonly or disproportionately experienced by workers with less power and fewer resources. These include new and young workers, immigrant and migrant workers, workers who experience language barriers, and workers with a high school education or less.2,15,18,31,33,35–39 These workers are also at higher risk of work-related injury or illness,38,40 perpetuating a cycle of unsafe working conditions, poor health, and financial insecurity. Claim suppression may also be more common in certain industries such as manufacturing, road transportation, food services, and construction, 1 as well as in non-unionized workplaces 18 and in precarious, temporary, or part-time employment.17,18,41 These experiences may also be more widespread for certain types of injuries and illnesses, such as those that are “invisible” (e.g., back pain) or that involve work absence. 2
The Ontario Context
In response to concerns about claim suppression, several Canadian jurisdictions have introduced legislation.42,43 In 2015, the Ontario Government introduced Bill 109, which made claim suppression a prohibited activity for which a monetary penalty, or a prosecution in more severe cases, may be pursued. Specifically, Section 22.1 states that “no employer shall take any action … in respect of a worker with the intent of discouraging or preventing the worker from filing a claim for benefits or influencing or inducing the worker to withdraw or abandon a claim ….” 44 Despite this, the injured worker community has continued to express concerns about claim suppression and the system that motivates it.12,13 A new rate framework that came into effect in 2020 has been argued to retain the key flaws of experience rating, namely that safety is still measured by claim costs which begin to accrue the day after the injury. 45 At the same time, some concerns relate to the scope of the 2015 law, as only overt actions by employers are explicitly described, despite evidence suggesting that most claim suppression is subtle, 15 and as the law does not address actions or inactions by stakeholders within the workers' compensation and healthcare systems that may contribute to employer claim suppression or otherwise result in the hindering of claims. There are also concerns about the interpretation of the law, namely concerning what constitutes intent and evidence thereof, with a recent reversal of a claim suppression monetary penalty on appeal over this question 46 indicating the need for further guidance. Lastly, concerns exist regarding case detection and enforcement. Since 2018, the Workplace Safety and Insurance Board (WSIB), Ontario's workers' compensation system, has conducted audits of employers identified through a risk matrix. The objective of 300 audits per year, out of approximately 300,000 employers, 47 has been characterized as insufficient.12,48 Between 2019 and 2023, only 73 claim suppression penalties were assessed against 33 employers. Court convictions are also rare, with only 6 convictions for claim suppression for the same period. 3
Current measures have thus far been ineffective at curbing claim suppression. Accordingly, there is a need to better understand the lived experiences of claim suppression for different workers and contexts, to ensure that laws, policies, practices, and interventions are grounded in and reflective of those experiences. 49 The current article contributes to this understanding by exploring mechanisms of claim suppression among precariously employed immigrant workers, a group at heightened risk. In addition to workplace factors, it considers the ways in which the workers' compensation and healthcare systems facilitate employer claim suppression.
Methods
This study investigated experiences of work, health, workers' compensation, and return-to-work among precariously employed Bangladeshi immigrants in Toronto, Canada. It was co-led by a McMaster University researcher and South Asian Women and Immigrants' Services (SAWIS), 4 a small nonprofit organization that is run by and works primarily with Bangladeshi immigrant women in the Toronto neighborhood of Oakridge-Crescent Town. A community-engaged approach was adopted whereby McMaster and SAWIS were equally involved in all aspects of the research process, including the design, analysis, and dissemination of the data. The project was conducted by peer researchers, Bangladeshi immigrant women with lived experience of precarious employment. Throughout the research process, we provided training and support to peer researchers to build research capacity at the community level.
Between August 2020 and August 2021, a period that overlapped with the second and third waves of the COVID-19 pandemic in Ontario, we conducted 31 semistructured interviews with workers and four focus group discussions (14 participants total, three to four in each group). The samples included Bangladeshi immigrant workers who were currently working or had last worked in a precarious job and self-reported a physical and/or mental illness or injury due to work. Precarious work was defined as insecure or unstable employment, such as work that is temporary, gig-based, on-call, involuntarily part-time, or informal. In line with the definition from the Law Commission of Ontario, we posited low wages as a necessary condition of precarious employment. 50 Workers were recruited through SAWIS contact lists, Facebook groups for the Toronto Bangladeshi immigrant community, and snowball sampling. In addition, eleven key informants with knowledge of the Toronto Bangladeshi immigrant community, who were identified through our networks and snowball sampling, were individually interviewed. Workers were asked about their immigration and work experiences, their work-related injury or illness, and their experiences post-injury or illness (e.g., Did you tell your employer that you got hurt or sick? How did they respond? Did you or someone else file a WSIB claim? Why/why not? If you went back or continued to work with that employer, did they help you, e.g., with accommodations?). We also asked workers about the impacts of their injury or illness and about what could be done to address the difficulties they faced. Key informants were asked about the trends they observed with regard to precarious work and work-related injuries and illnesses (e.g., What are some typical trajectories for workers in precarious jobs who get hurt or sick at work?). We also asked key informants about the resources and supports currently available and the impacts and solutions of the challenges discussed.
Interviews and focus group discussions each lasted around 2 hours, were conducted remotely by phone or Zoom, and were audiorecorded. Workers were compensated with a $45 honorarium. Prior to data collection, all participants were provided with a consent form. Worker consent forms were available in English and Bangla. Consent was obtained in writing, or verbally and recorded in a consent log. All interviews with key informants were conducted in English, while all worker interviews were conducted in Bangla, with workers having varying levels of English language proficiency. Bangla audio files were translated into English and transcribed in a single step by peer researchers who had high proficiency in both languages. The decision to translate data before analysis was made to ensure all team members could participate in the analysis. Using NVivo software, interview transcripts were each coded by a team member using a mixed coding strategy, whereby some codes were defined a priori while others emerged from the data. Team members worked collectively on the coding framework and on the development and analysis of themes. Ethics approval was obtained from the McMaster University Research Ethics Board. All names are pseudonyms, and details have been changed as appropriate to protect the anonymity of participants.
Our project adopted an equity lens. While a growing body of research has documented inequities in health and safety experiences and outcomes, 51 there continue to be gaps in research, namely with regard to how these inequities are produced and how to reduce them. 52 Existing explanations for inequities have largely focused on individual rather than systemic factors, with language barriers and cultural differences commonly cited to explain inequities between immigrant and nonimmigrant workers. 52 As Flynn et al. (2021) have argued, however, addressing inequities requires a holistic approach that accounts for the broader structures within which these patterns are produced. 51 Microlevel experiences of claim suppression and related inequities are thus understood to arise not from a few “bad actors,” but from the rules of prevention and compensation systems, which are in turn informed by broader political and macroeconomic conditions.3,23,53,54 More broadly, our study employs a systems approach to work injury and disability by identifying barriers to claims within the workplace, insurance, and health systems. 55
Results
Demographic Characteristics of Participants
Worker characteristics are presented in Table 1. Workers were almost equally distributed in the 31–40, 41–50, and 50+ age categories. A large majority of participants were women (31/45), and almost all had been in Canada for 10 years or fewer (38/45). Almost all had a postsecondary education, with 25 of the 45 workers holding a master's degree. Despite this, workers labored in low-wage jobs in factories, retail, restaurants, childcare, and security. Data on whether participants worked in formal or informal employment was not collected. Workers experienced a wide range of physical and psychological health problems due to work, including musculoskeletal pain, traumatic injuries, high blood pressure, anxiety, and depression (data not shown). Several workers had experienced injuries and illnesses in more than one precarious job. Only eight of the 45 workers in our study had filed a workers' compensation claim.
Characteristics of Worker Participants.
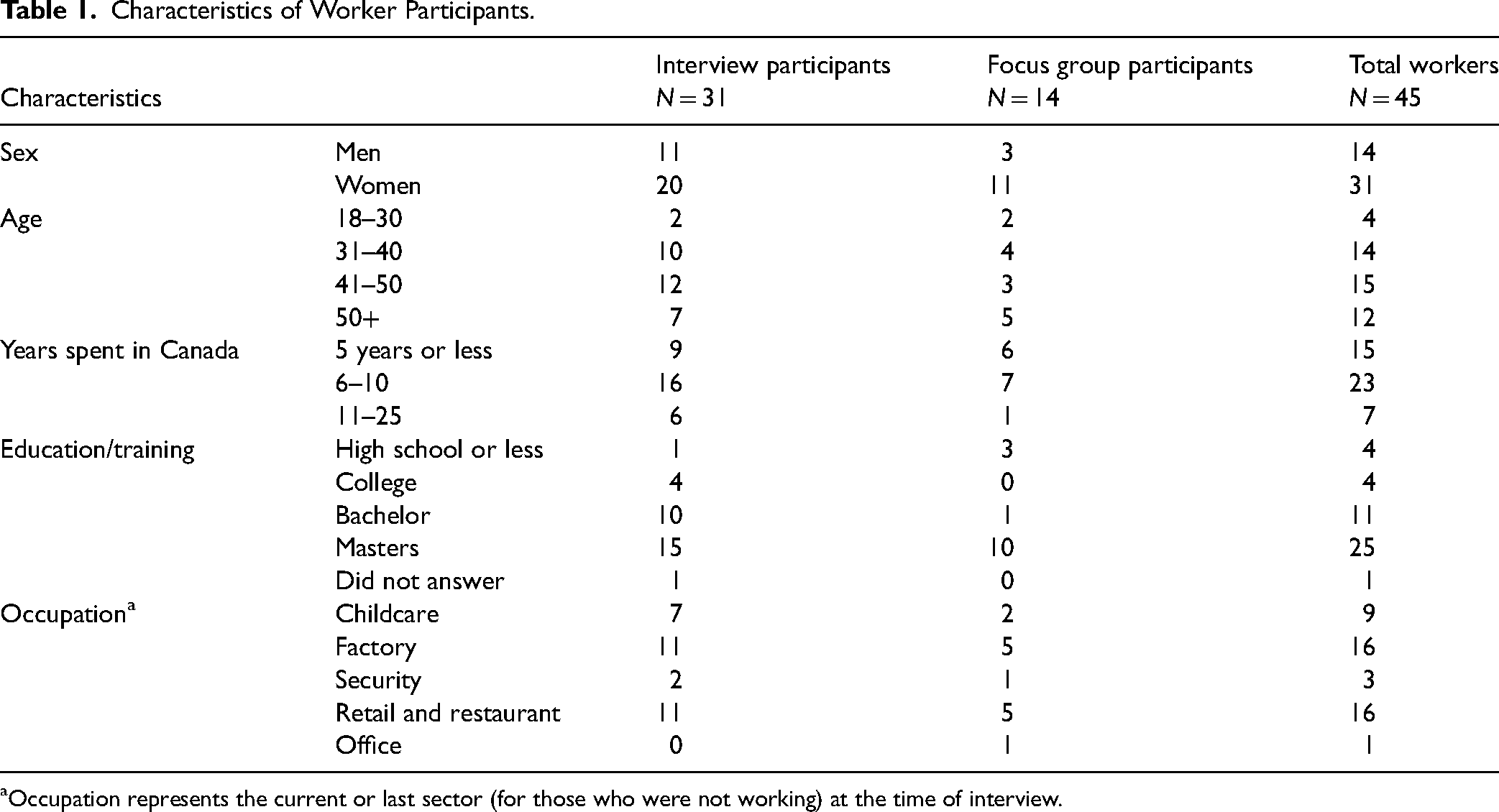
Occupation represents the current or last sector (for those who were not working) at the time of interview.
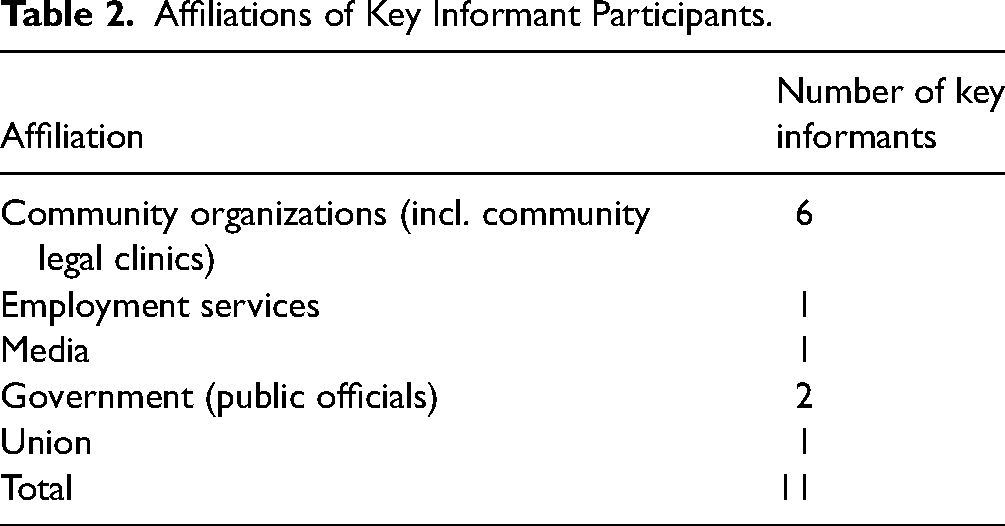
Key informant affiliations are presented in Table 2. They included representatives from community organizations, employment services, unions, government, and the media.
Affiliations of Key Informant Participants.
Mechanisms of Employer Claim Suppression
All workers spoke at length about their experiences with and knowledge of employer claim suppression. Their narratives revealed varied forms of claim suppression in precarious work, including employers reacting negatively to health problems, retaliating or threatening to retaliate, contributing to and exploiting information gaps, engaging in illegitimate return-to-work schemes, and hiring through temporary employment agencies and/or misclassifying workers as independent contractors.
Reacting Negatively to Health Problems
Employers reportedly reacted with annoyance and anger at workers' health problems, specifically their potential to reduce productivity or require time off and/or to result in a workers' compensation claim. Descriptions of employer reactions revealed intolerance for any reduction in productivity at work. This was evident across several stories of workers being required to continue to work after reporting a work-related injury or illness. Ranu, who at the time of the interview was a coffee shop worker in her 30s, described how she injured her finger in her previous job in a factory. She recounted the lack of care shown by her employer at the time when she requested a different task due to her injury: I told them that I cannot work, my finger got cut, and I can't work in this line and that they should give me something else to do. They didn't give me anything, and they didn't give me medicine or a band-aid or anything. I said fine, I don't need medicine or a band-aid, I'll treat it when I go home. I used a tissue to apply pressure and put on gloves and went back to work. But I didn't get to leave the line, I had to continue working in the line.
Similarly, several participants described a lack of tolerance by employers for workers taking time off. As a result, most workers were afraid to take time off, and many never did despite experiencing health problems typically requiring it. In the absence of financial support in the form of workers' compensation, paid sick leave, or other, taking time off resulted in both a negative impact on the relationship with the employer and an immediate loss of income. Shaila, a cashier in her 20s, characterized the unsupportive attitude of employers with regard to time off as oppression: But if I ever called and said I was really sick and I wasn't feeling good, then what more can they do? A positive approach like saying ‘It's okay, take care.’ That rarely happened. In four to five people, maybe one person would be nice and tell me to take care. But everyone else would say something like ‘Oh you're letting us know now? What do you expect us to do?’ But I'm sick, you should understand that. They would not understand. It's like … oppression. It's not called that, but you would definitely feel it.
Employers were thus described as intolerant of health issues that could impact workers' productivity at work and need to take time off from work, and this was particularly true for chronic health issues and longer-term absences. Several participants described a limited tolerance by employers for infrequent, temporary issues (e.g., fever), and a complete intolerance for chronic health conditions (e.g., back pain). This lack of tolerance for health issues was embedded in the workplace culture and discouraged workers from reporting any health condition.
When health problems were compensable work-related conditions, employers were additionally described as trying to avoid responsibility by ignoring or delaying responding to workers' reports or claims, or by interrogating and blaming them for their conditions. Several workers and key informants, including Jerry, a community service provider, described “the culture of denial” which regards injured or ill workers as “criminals”: The first thing they ask you, was there any witness? Treating you like a criminal, right? And why didn't you report it? Well, because there were no witnesses, right? Why didn't you report it? Well, because there is nothing shown, right? So, this culture of denial is not just something that happens at the end of the story … So why did the claim get denied? Because there is a culture of denial. Why didn't the claim get filed? Because there is a culture of denial.
Negative reactions by employers thus discouraged workers from reporting their health problems or submitting a workers' compensation claim and encouraged workers to continue to work despite injuries and illnesses.
Retaliating, or Threatening to Retaliate
Underlying employers' negative reactions was the explicit or implicit threat that reporting an injury or illness or filing a claim would lead to negative consequences for employment—or the promise that not filing a claim would produce positive employment outcomes. Workers feared retaliation in the form of loss of employment, work hours, future work, or opportunities for promotion or permanence, a theme consistently present across workers' stories. For instance, Lima, a factory worker in her 30s, explained how concerns over future employment motivated her decision not to submit a claim: I consulted with my husband and reached a decision that I will not claim as I want to work there in the future. I thought that if I make a claim, in the future they will not hire me again. They will have a document or a report that this woman was injured here and she made a claim … Often we don't want to do this.
Workers' fear of retaliation was based on employers' negative reactions to health problems as described above, as well as on direct experience with, or awareness of threats to employment. This was illustrated by Tahira, a factory worker in her 30s, who described how she was made to understand that her pain was incompatible with her continued employment: When I realized my hands were swelling, I informed my supervisor. She said, ‘we do not have any extra workers to replace you, so if you think that this work is painful for you, do not come tomorrow.’ Then, I stepped back and did not argue, and I continued my work.
Several key informants noted that immigrant workers in precarious jobs regularly lost employment in response to their reports of or claims for work-related injuries or illnesses, with those employed through temporary employment agencies typically dropped from agencies' call lists. In the context of precarious work, knowledge of or direct experience with threats to employment was effective in discouraging workers from submitting claims.
Contributing to and Exploiting Information Gaps
Lack of knowledge of and information about workers' compensation were described by several workers and key informants as widespread in the Bangladeshi immigrant community and played an important role in workers not submitting claims. Arif, a taxi driver in his 50s, described how he first learned about workers' compensation after almost 20 years working in Canada: Since the time I started to work in 1998, the first time I came to know about WSIB was in 2017 when I just started to drive a taxi. One day I picked up the passenger who was in a contract with WSIB. I asked him what WSIB is. Then they explained to me what you just told me now. At that time, I first came to know about WSIB. I don't think a lot of Bangladeshis know about WSIB.
Few workers were aware of the workers' compensation system, and those who were aware typically had incomplete or incorrect information about its eligibility criteria and process. While some of the reported health conditions, such as anxiety due to the instability of employment, are not covered under Ontario workers' compensation, workers generally did not know the eligibility status of their work-related condition. These information gaps, in turn, were rooted in workers' relative newness in Canada and their experiences of language barriers, but also in the fact that despite a legislative requirement,
5
few employers provided workers with information about the role of the workers' compensation system. Several workers and key informants additionally reported that employers at times directed workers to other income support systems, thus exploiting their information gaps. On a more general level, workers' lack of information, combined with language barriers, allowed employers to work the system in their favor, as illustrated through the words of Faruk, a factory worker in his 30s: I don't remember, I think they did that (got a signature from him about the incident). I was not aware of that, they did what they wanted to do at that time. I followed that … that time I couldn't understand. I came here new, I don't know any way out … That's why I didn't go there (to WSIB). So, after I got well a little bit, I rejoined the work. I closed that chapter.
Information gaps, at times produced and exploited by employers, thus contributed to the invisibility of work injuries and illnesses from workers' compensation.
Engaging in Illegitimate Return-to-Work Schemes
Several workers described pressure or schemes to avoid lost-time claims or push an early return to work. For instance, Shurovi, a factory worker in her 40s, explained that she was offered money by her employer to sit at work as an alternative to filing a claim: HR offered that if you stay home, the pay you'll receive from WSIB will be very little. But if you come here daily just to sit, the money you are getting now monthly on an hourly basis we will give you the same money.
A few workers described being offered modified or accommodated work to return to work, though in all cases the modifications or accommodations were either not provided upon workers' return or eventually removed. Sabiha, a childcare worker in her 50s, described being pressured to come back to work with the promise of modifications which were never implemented: But what made me feel bad was that they were pressuring me to come into work. But even the doctor said I can't work. I had a doctor's note. But despite this, they pressured me. After 2 weeks, they kept trying to get me to come in and do modified work. They did not ask me ‘Are you ok right now or not … Could you do work or not?’ Nothing. Just started to give me work as a normal employee. So, I have started the work again.
Rather than supporting workers reintegrating into the workplace after an injury or illness, return-to-work represented a strategy used by employers looking to minimize the costs of claims.
Hiring Through Temporary Employment Agencies and/or Misclassifying Workers
Employers were reported by some key informants to hire workers through temporary employment agencies to suppress claims. In Ontario, in a triangular employment relationship, the temporary employment agency is considered the employer and responsible for workers' compensation premiums.
6
Our analysis revealed that temporary employment agencies used the same strategies as employers, as described above, to evade or minimize the costs of claims. For instance, Rubina, who at the time of the interview was a childcare worker in her 40s, described the pain she developed in her previous factory job and the reaction from the temporary employment agency: I finished the day job anyway only to find out later that I cannot move my hand due to pain … The next day … I went to their office (of the temporary employment agency) and told them, complained about the fact, and told about the problem … They told me ‘It's not a problem. You keep doing the job. We will change your posting.’ … I still clearly remember that I took medicines for the pain and I worked there for 4 days … .they did nothing to change my posting. Then I went to their office and told them that if they do not change my posting, then I will quit the job. They told me ‘If you do not want to work there … at present, we have manpower shortage in that section (referring to a different section).’ It was actually a man's job. They told me ‘ … If you do not want to work there, then it's up to you.’ They meant it was my choice. ‘Then you can quit the job.’ I did not have any other choice as my hand was involved … Then I quit.
In addition, employers sometimes classified workers as independent contractors to avoid responsibility for work injuries and illnesses. That the system allowed employers to evade claims in this way was described by Donna, a public representative, as corruption: Those who are working in the factory they work as contract staff so it means they are self-employed so if something happens in the factory the factory is not responsible for that so far I know because you're working as a contractor so that is a very dangerous thing … This is bullshit and this is very dangerous systemic corruption I would say, I say corruption and it should be stopped.
Systemic Facilitators of Employer Claim Suppression
Various features of the workers' compensation system facilitated employer claim suppression by helping discourage workers' claims. The reputation of workers' compensation in the community as a difficult to navigate organization played a central role in workers' reluctance to submit a claim. Participants described the process of obtaining compensation as lengthy and complex, necessitating workers to invest time, effort, and money to get their claim accepted. For instance, Shobuj, a construction inspector in his 60s, described the complicated process of having the cost of orthopedic shoes approved by the WSIB: I did my own research. There are three types of orthopedic shoes available on earth. One is Japanese, one is European, and the last one is American. I called the American companies that manufacture those shoes. I told them the size of my shoes … I asked for papers from them. I made a summary of those papers. I submitted that summary to the appeal division of WSIB. I wrote the summary in light of tort law. The appeal approved my claim … Accordingly, my problem was solved. They have created many obstacles like this one.
While Shabuj was able to navigate the system, many workers found the process too daunting, particularly given language barriers. At the same time, several workers related direct experiences or had heard stories about the WSIB whereby workers were not believed and had their claim denied, and many expressed the belief that their word would be insufficient to support their claim. Participants, like Amena, a community service provider, described the WSIB's culture of suspicion, scrutiny, and denial of workers' claims: It looks like the WSIB is an insurance board, it's working on behalf of the employers. It's not a compensation board that's ‘OK. I'm going to be lobbying for my workers to benefit.’ It looks like they're trying to save the employer profit because if you have more accidents in your workplace your insurance is going high. That kind of thing are some sort of mentality to minimize all of this claim.
Indeed, even when injured or ill workers were aware of workers' compensation, when unable to work they often pursued other income supports due to the perceived complexity and low chances of success of a claim.
In addition, participants described concerns about the temporary nature of benefits, the low level of income replacement (85% of net income), and the potential delays in obtaining payment as important factors in their decision not to submit a claim. Staying employed, albeit in a precarious job, was preferable to the potentiality of obtaining temporary and insufficient benefits from workers' compensation. This was expressed by Hasina, a childcare worker in her 50s: We need that job, right? And in this precarious sector, there is no job security at all. Though you do your best, there is no job security. In this situation, we can't lose our (future) whole year's work for only 10 days because of WSIB!
Workers' compensation claims were also discouraged by policies and practices that complicated access for workers, particularly those who experienced language barriers and/or were in precarious work. For example, while the WSIB provided free interpretation and translation services, they were typically unknown to workers or described as inadequate to navigate the complexity of a claim. As well, some key informants noted confusion surrounding the identification of the employer when there were multiple concurrent or subsequent employers, or when in a triangular employment relationship. In sum, while experience rating motivated claim suppression, our findings suggest that other features of the workers' compensation system facilitated it by contributing to workers' reluctance to claim, which in turn benefitted employers. In fact, several key informants reported that employers often emphasized the difficulties of obtaining benefits from workers' compensation and the 85% income replacement rate in their attempt to discourage claims.
Our analysis similarly identified factors within the healthcare system that enabled employer claim suppression. Some healthcare providers were described as helpful in guiding and supporting injured or ill workers through the process of workers' compensation. However, our interviews revealed that workers sometimes found it difficult to find a provider, especially in the context of language barriers. As well, while many healthcare providers were described as helpful, others were said to be uninformative or unsupportive with regard to workers' compensation claims. Nahida, a factory worker in her 30s, described her experience with health care after her work injury: I was sent directly to the emergency. They did not give me such information or documents from emergency. They just told me that I do not have any fracture, but I have some bruises. They put some bandage on that so that I do not move my hand. But they did not tell us anything about filing a claim at WSIB.
The lack of support and information from some healthcare providers may be attributed to a lack of knowledge of the system, language barriers, or a reluctance to engage with workers' compensation due to the high workload and relatively low remuneration involved. This, in turn, left some workers without an important source of information and support and therefore more vulnerable to employer claim suppression.
Impacts of Claim Suppression
Employer claim suppression, within the context of a system that motivated and facilitated it, had a significant negative health, social, and economic impact on workers, families, and communities. Workers typically self-managed their health problems by avoiding disclosing to their employer or agency health issues that could impact their work in the short and long term. In most cases, there was no time off, though workers who were able to take time off for work injuries and illnesses and return to work often continued to struggle after returning as modifications and accommodations were removed, if provided. Workers generally continued to work through pain or discomfort, which often exacerbated the health condition and sometimes led to permanent disability. When work with an employer was no longer possible, some workers moved to other jobs while others exited the labor market temporarily or permanently. Work injuries and illnesses thus heightened workers' employment and financial precarity. In several cases, injured workers were forced to rely on government support programs, many of which offered lower levels of support compared to workers' compensation. Importantly, the eligibility criteria for various government support programs were described by several participants as difficult to meet, and so the financial burden of work injuries and illnesses burden often rested on families. Jack, a community legal worker, described those impacts: In the long run, it becomes problematic for the family if the breadwinner can't get back to work. For a while, there's a lot of support, but then tensions build because … they were supporting a spouse at home, then the spouse needs to go out and get work. In some cases, in a lot of families, we see where the children are in their teenage years, they end up having to go to work as much as possible to support the family which also creates tensions … There's been research done about the impact on relationships, families break down and split up.
The mental health impacts of injuries and illnesses, and of claim suppression and its ramifications, were also significant. Renuka, a security officer in her 30s, described the mental health effects of her injury and subsequent need to support her family with the help of government support: I had a hope, but this injury has ruined all my hopes. I don't know what my future is. Sometimes I even thought that I'll take Ontario Student Assistance Program (OSAP), but I couldn't mentally agree with that, because I had the belief that I can do something. I had dreams too. So, the thinking of maintaining my family with OSAP was distressing.
The impacts on mental health of claim suppression itself were evident in several workers' stories, which decried their disposability and the dehumanizing nature of their experience. This was illustrated through the words of Nahida, a factory worker in her 30s: Like, when I had the accident, they could have told me ‘Please take rest. Don't worry. Take 2 weeks. We will pay you for that.’ But in reality, they did not pay me for that. I was disappointed at that … The accident would not have occurred if they had tightened that screw. They do not consider us as workers. They consider us products like the products that they manufacture.
As the health and economic impacts of work injuries and illnesses reverberated through various aspects of life, the costs of work injuries and illnesses were shifted through the process of claim suppression from employers to workers, families, communities, and society.
Discussion
Our study, based on qualitative interviews with 45 precariously employed Bangladeshi immigrant workers and 11 key informants, documented diverse forms of claim suppression in the Toronto precarious labor market. Our results suggest that the avoidance of employer responsibility for work-related injuries and illnesses, including the undesirability of workers' compensation claims, was embedded in a “culture of denial” that spanned sectors and jobs. More specifically, employer claim suppression involved a range of actions and inactions that workers and key informants understood as attempts to prevent the appropriate reporting of work-related injuries and illnesses to workers' compensation. These included employers reacting negatively to health problems, retaliating or threatening to retaliate, contributing to and exploiting information gaps, engaging in illegitimate return-to-work schemes, and hiring workers through temporary employment agencies and/or misclassifying them as independent contractors.
These findings support those of other studies that have documented similar employer strategies to suppress work injury and illness claims26,28,31,33,34,39 and similar impacts on workers and their families of employers' and workers' compensation’ inadequate and unjust responses to their injuries and illnesses.56,57 Like most of these studies, ours did not seek out to investigate claim suppression; instead, it focused more generally on experiences post-injury or illness among a sample of precariously employed immigrant workers in Toronto. As such, our study could not capture all forms of claim suppression present in the precarious labor market. Other studies conducted among precariously employed immigrant and migrant workers in various contexts have identified additional strategies to suppress claims such as deportation,58,59 drug testing, 33 and the use of internal medical providers to discourage claims, 60 with data suggesting that experiences vary by context and population. 33 However, while it is possible that some mechanisms of claim suppression documented in our study may be more prevalent in precarious work that disproportionately employs immigrant workers, there are no indications that any of the findings are specific to the Bangladeshi community.
Our study adds to the literature by documenting the role of the workers' compensation and healthcare systems in the suppression of work injury and illness claims. Some of the features described in our study, such as the institutional mistrust of injured workers, are features of the broader system that manifest in part by discouraging claims. 61 We found that the reputation of workers' compensation as a lengthy and complicated process that requires considerable effort to navigate, and as a pro-employer organization that views workers' claims with suspicion, played a major role in discouraging workers from engaging with the system. Workers were additionally discouraged by the temporary nature of benefits, the level of income replacement, which was insufficient given workers' low wages, and the potential delays in obtaining compensation. As well, workers' compensation improperly accounted for the reality of language barriers and precarious employment, which may complicate access for precariously employed immigrant workers62–64 and thus benefit employers looking to avoid or minimize claims. Workers were also left vulnerable to claim suppression by their lack of access to healthcare providers who were, in some cases, important sources and information and support, as they were by their interactions with providers who were uninformative and unsupportive. Together, these elements contributed to a context whereby the potential benefits of submitting a claim in most cases did not outweigh the effort required nor the challenges and risks involved. These systemic facilitators of claim suppression are not exhaustive, and other system-level factors, such as policies and practices that deem workers employable and cut their benefits even if they are not employed 3 or push them to return to work early, 65 or that ignore or deny claims with missing documentation without proper inquiry, may also help suppress claims. Each year, about 40,000 incidents registered at the WSIB based on a health professional's report (Form 8) alone are neither properly investigated nor adjudicated. 7
The broad scope of claim suppression as documented in this and other studies exceeds that contemplated by the Ontario legislation, which states that “no employer shall take any action … in respect of a worker with the intent of discouraging or preventing the worker from filing a claim for benefits or influencing or inducing the worker to withdraw or abandon a claim … ” 44 Prohibited actions outlined under Section 22.1, include but are not limited to dismissal or threat of dismissal; disciplining or suspending, or threatening to discipline or suspend a worker; imposing a penalty upon a worker; or directly or indirectly intimidating or coercing a worker with threats, promises, persuasion or other means. 44 While claim suppression is not limited to these actions in the legislation, the focus is on overt employer actions directed at workers to pressure them not to claim or underclaim, which is in line with some definitions of claim suppression.7,17 This is at odds with evidence suggesting that most claim suppression is subtle, 15 and with our findings of veiled and sometimes indirect employer claim suppression strategies, such as engaging in disinformation or hiring through temporary employment agencies—though we note divergence about what constitutes overt and subtle claim suppression, with some, for instance, classifying disinformation as overt. 15 As well, while the legislation exclusively emphasizes actions taken by employers, it does not consider scenarios where a lack of action (e.g., not providing information) serves to suppress a claim, nor does it contemplate the role of nonemployer factors in the suppression of work injury and illness claims.
The interpretation of the law is also problematic, as intent is difficult to establish, particularly when involving subtle forms of claim suppression. For instance, it may be challenging to determine employers' intent in not providing workers with information about the workers' compensation system, though the pattern of suppressing claims in jobs characterized by precariousness and immigrant labor suggests that at least some of the information gaps are intentionally produced. The challenge concerns the threshold and evidence needed to establish intent. In other words, at what point does misinformation become disinformation, and how does one prove this? This vagueness has hindered both the development of knowledge on claim suppression1,2 and the application of claim suppression legislation. 46 Currently, no policy regarding the threshold and evidence needed to demonstrate intent in claim suppression cases exists in Ontario. Due to difficulties proving intent, suspected cases are typically handled as late or nonreporting, which commands lower fines ($1,000 vs $5,000). These various limitations and challenges underline not only the inability of legal mechanisms to address claim suppression but also their role in facilitating it. Thus, rather than protect workers from claim suppression, current legislation, as written and implemented, largely shields employers from penalties while ignoring the contribution of other systems to the suppression of work injury and illness claims.
These issues raise questions about the underlying conceptualization of claim suppression as necessarily involving actions by employers intended to suppress claims.2,7 It may be argued that policies and practices in workers' compensation, health care and other domains that hinder the appropriate reporting and compensation of work injury and illness claims should be conceptualized as nonemployer forms of claim suppression rather than as facilitators since they work to suppress claims even in the absence of employer claim suppression. It may also be debated whether intent is a useful concept for understanding and addressing claim suppression. The conceptual boundaries of claim suppression must encompass how various systems, including the workplace, workers' compensation, health care, and legal systems, work to suppress claims, in outcome if not intent. Conceptual and empirical work is needed to understand the range of mechanisms at play and the ways experiences vary in intersecting ways according to context, population, and other factors. The lack of consistent conceptualization and terminology regarding claim suppression—alternatively called “concealment of claims,” 7 “claims avoidance,” 66 and “claims management” 4 —has represented a barrier to establishing a body of evidence around the issue, as has the fact that little qualitative research has looked directly at claim suppression, instead, like ours, documenting it as part of larger investigations.
Beyond a need to consider, in light of diverse lived experiences, the scope and interpretation of the law, and the underlying questions with regard to the conceptualization of claim suppression, several solutions have been proposed by labor unions, 9 injured workers' advocates, 12 and experts tasked with reviewing the workers' compensation system. 48 These have included abolishing experience rating, which has, according to Mansfield et al. (2012), transformed “collective responsibility for occupational health into deregulated, individualized responses.” 4 p 20 Before experience rating came into effect in Ontario, there was collective liability based on industry groups, so rates did not fluctuate for individual employers based on their own workers' injuries and illnesses. At the time, claim suppression was rare (see Endicott in this special issue). For this reason, the incentivization of claim suppression through experience rating has been labeled a “moral crisis” in the 2012 Funding Fairness report to the WSIB. 14 p 81 There have also been calls to put in place appropriate controls, sanctions, and enforcement for claim suppression activities as a necessary prerequisite to experience rating. 67 These include recommendations for the WSIB to conduct a significant number of employer audits, impose larger penalties on employers as disincentives, follow up on claims that are abandoned, delayed or missing documentation, and increase employer and worker education, starting in schools. Recommendations have also highlighted the importance of any effective strategy to properly address the complex challenges present in various intersecting contexts of vulnerability, such as those of language barriers, im/migration, and precarious work.
Importantly, our findings point to the need to reform the temporary employment agency sector in Ontario, to which employers can outsource the risk of workplace injuries and illnesses. Temporary employment agencies, in turn, have been shown to use a range of strategies to avoid financial risk, beyond those documented in our study, such as shutting down and reopening. 34 In April 2018, the former provincial Liberal government drafted new regulations under the Workplace Safety and Insurance Act, titled Section 83(4), which ensures that client companies of temporary employment agencies are liable for WSIB premiums; however, the regulations were never put into effect as the Progressive Conservative government came to power in June of that year. 68 While researchers and community and labor activists have asked for regulation that holds the client company liable,34,68 the government instead amended the legislation to place temporary employment agencies into the same classification as the client company, 8 so that agencies will pay higher premiums where the workers they supply work in industries that are more dangerous. In other words, these changes have done nothing to address the problem of claim suppression driven by experience rating, instead further incentivizing temporary employment agencies to suppress claims. Research is needed to determine how these changes will affect behavior on the ground, including with regard to prevention, which is the shared responsibility of the employment agency and the host employer in Ontario. 69 Additionally, while employee misclassification is prohibited under the Ontario Employment Standards Act and carries the risk of legal and financial penalties, 9 more work is needed to prevent the practice among employers. More broadly, reducing precarity, such as by putting in place limits on the use of temporary workers, increasing the minimum wage, supporting greater unionization, and establishing a permanent employer-paid sick leave program, would help minimize workers' exploitation and the effectiveness of employer claim suppression.
Finally, our findings point to the need to address factors beyond the workplace, such as making the workers' compensation process easier and more intuitive, including for workers who experience language barriers, 62 and fundamentally transforming the WSIB's ethos of helping employers first. As Barnetson (2010) has argued, a central objective of workers' compensation is to contain employer claim costs. 3 This is highlighted by the fact that the WSIB has reduced employer premiums by $8.5 billion since 2018, 70 rather than putting the excess funds toward helping injured workers. Our results further support the need for workers' compensation to provide low-wage injured and ill workers with 100% of their net pay and to identify and address other workers' compensation policies and practices that may produce or contribute to claim suppression, including the lack of recognition of certain work-related conditions. At the same time, our study highlights the need to improve access to doctors, enhance their training on health and safety and workers' compensation, and increase their remuneration for workers' compensation cases, to ensure that injured and ill workers may benefit from this important source of support.
Conclusion
Our findings document the persistence of claim suppression in the precarious immigrant labor market in Toronto despite legislation making it an offense in Ontario since 2015. For precariously immigrant workers who are injured or become sick due to their jobs, there is no time off, compensation, or proper return to work. The health, economic, and social impacts of claim suppression on workers, communities, and society are, in turn, significant. Importantly, claim suppression contributes to a cycle of unsafe work, as prevention actions and policies are predicated on injury and illness rates based on workers' claims.8,71 In bringing to light the various mechanisms for claim suppression in precarious work, our findings repudiate the “bad actor” discourse and instead position claim suppression as a systemic problem motivated, facilitated, and enacted by multiple systems.
Supplemental Material
sj-pdf-1-new-10.1177_10482911241312387 - Supplemental material for Claim Suppression of Occupational Injuries and Illnesses Among Precariously Employed Immigrant Workers in Ontario
Supplemental material, sj-pdf-1-new-10.1177_10482911241312387 for Claim Suppression of Occupational Injuries and Illnesses Among Precariously Employed Immigrant Workers in Ontario by Stephanie Premji, Momtaz Begum and Kishower Laila in NEW SOLUTIONS: A Journal of Environmental and Occupational Health Policy
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by the Social Sciences and Humanities Research Council of Canada and the Canadian Institutes of Health Research through the Government of Canada (PWP-159064).
Notes
Correction (September 2025):
Article updated with the addition of online supplemental material.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
