Abstract
Family systems theory explains how post-traumatic stress disorder (PTSD) in the family affects family members who must cope with disturbing behaviors from the military member. Although military-related PTSD has been studied in the United States for over a decade, Canadian research is in its infancy. This article focuses on the challenges military families face for both active military members and retired veterans. Corbin and Strauss’ (2015) grounded theory was used to guide this study. Following theoretical sampling, semi-structured in-depth interviews were conducted with 21 non-military parents and 4 adult children in Alberta. The findings have important implications for military families, as well as practice, policy, and research on the topic. Further research could expand the sample to include military members/veterans and families across Canada.
Introduction/Literature Review
Although there is growing research on the impact of military-related post-traumatic stress disorder (PTSD) on individual military parents, much of the research on military-related PTSD has focused on the U.S. armed forces (Cramm et al., 2015). The United States first recognized the impact on military parents 25 years ago, while Canada lagged behind significantly (Cramm et al., 2015). However, there are several differences between the armed forces in Canada and the United States and the experience of military parents in the Canadian and the United States are considered to be significantly different (Cramm et al., 2019). For example, family members of Canadian military parents do not receive care from the military medical system, whereas U.S. military families have the option of being served through the military medical system (Cramm et al., 2019). Canadian families of serving members as military families are four times less likely to have a family doctor than civilians, resulting in many underserviced health needs (Rowan-Legg, 2017). The needs of Canadian military families within their social contexts have rarely been explored and thus are often overlooked.
In 2021, there were 97,625 military members who were serving in the Canadian Armed Forces (CAF; Statistics Canada, 2022). In other words, these members are actively in the military, whereas veterans are considered retired or out of the military. There were 461,240 Canadian veterans in 2021 (Statistics Canada, 2022).
Although exposure to trauma is common within the general population, not everyone exposed to a traumatic event develops PTSD. One of the most recent population-based study in Canada found that while 76.1% of individuals have been exposed to trauma over a lifetime, only 9.2% of the general population met the diagnostic criteria of PTSD (Van Ameringen et al., 2008). However, rates of military-related PTSD vary for those servicing and those who are no longer serving (veterans). For example, an epidemiological study by Zamorski and Boulos (2014) found rates of military-related PTSD to vary between 8% and 20% in serving CAF members following deployment to Afghanistan. According to a study completed by van Til et al. (2017), post-9/11 rates of PTSD among Canadian military veterans were at a rate of approximately 16%.
Anecdotal evidence, and some family theorists, supports the belief that the experiences of families and individual family members are affected by military-related PTSD (DeVoe et al., 2018). Although a child or non-military parent was not part of the original trauma, they may take on symptoms of PTSD in response to being exposed to the military parent’s PTSD (Banneyer et al., 2017; Canfield, 2014). PTSD negatively impinges on the ability to engage with the family, and contributes to the disruption of interpersonal bonds, effective communication, and coping skills (Banneyer et al., 2017; Harrison & Albanese, 2016), making a family focus important (Canfield, 2014).
Military Families
In 2017, more than half were under the age of 35 (54%) and 56% were married or living common-law (Manser, 2020a). Moreover, approximately 57,640 children are currently growing up in Canadian military families (Manser, 2020a), not including the children of the 461,240 Canadian veterans (Statistics Canada, 2022).
There has been extensive research in the United States on the impact of military families residing with a military member diagnosed with PTSD (i.e., Dekel & Monson, 2010; Renshaw et al., 2011). Despite the growing attention on military-related PTSD, research on military children and families remains scarce, particularly in Canada (Sullivan et al., 2018). For example, a scoping review by Cramm et al. (2016) noted that out of 660 articles related to military-related PTSD, only 21 Canadian articles mention the impact on families. Moreover, studies within Canada that focus on the perception of military partner’s relationship and the relationship of the children and the military parent with military-related PTSD are not as prevalent as those derived from the perception of military parents (McGaw et al., 2020). Many Canadian studies on family relationships have been derived from self-reports of veterans rather than from family members (Norris et al., 2018), eclipsing the voice of the family. This is a significant gap despite the relationship between parental mental health and child development. Specifically, the family systems theory suggests that the well-being of an individual in the family is intricately linked with that of the rest of the family (DeVoe et al., 2018; McGoldrick et al., 2005; Satir, 1964), and individual difficulties ripple throughout the family (Sullivan et al., 2016). Family system theory further asserts that families do not live in isolation and that each member is affected by the behaviors of other family member (Carter & McGoldrick, 2005). With the limited research on military children and youth in Canada, research is needed to further understand and meet their needs (Manser, 2020b).
This paper looks at the gap in qualitative studies to provide a better overview of the experience of children and non-military parents as a consequence of their military parent’s PTSD by answering the question
Research Question 1 (RQ1): What are the challenges faced by family members when residing with a military parent (both serving and retired veterans) experiencing military-related PTSD in Canada?
The question is supported by family systems and ecological systems theory.
Ecological and Family Systems Theories
The core of ecological systems theory proposes that life unfolds through a series of environmental transactions (Bronfenbrenner, 1979). Difficulties are thought to evolve in response to problematic transactions between individuals and larger systems. Military parents and their families are embedded in a unique set of social systems that affect their lives including families and support systems (Everson & Camp, 2011). The challenge is to capture relationships between persons and their environment and intervene at appropriate levels to promote change (Gitterman & Germain, 1980/2008). In relation to military-related PTSD, systemic influences have an enormous impact on military parents’ lives and well-being yet are not readily studied in Canada.
Military parents and their families are therefore best understood within their social and environmental contexts including schools, the military environment (both with interaction with military peers and culture), family relationships, the community, and larger socio-policy-legal infrastructures. A sole focus on micro and individual level transactions limits understanding, since it fails to recognize the holistic set of systemic influences that shape life (Gray, 1972). Practice with families living with someone experiencing PTSD must be cognizant of the influence of military culture on individuals and families including interactions between individuals, family systems, military systems, and larger bureaucratic systems (Marquez, 2012).
Family systems concepts guide how helping professionals understands family functioning (De Shazer, 1983), specifically military families. The foundation of family systems theory is the recognition that members of a family are mutually dependent and connected to systems external to the family (Bowen, 1971). In addition, change in one part of the family affects the rest of the family (Bowen, 1971). Based on these concepts, this paper focuses on the understanding of challenges faced by military families residing with military-related PTSD.
Method
In this research, we adopted the grounded theory method developed by Corbin and Strauss (2015) to cultivate a theoretical understanding of the research question. The research question explored how families navigated their challenges when they resided with a military parent experiencing military-related PTSD. We were looking to understand how families perceived their experiences of living with a family member diagnosed with military-related PTSD. Delving into this question was essential to ensure that military parents’ needs and those of family members were being met adequately.
Ethics approval was obtained through the University of [anonymized] Research Ethics Board. The first author interviewed and collected the data. Participants completed an informed consent in order to participate, which outlined limits to confidentiality and ensured that anonymity would be maintained. The researcher informed participants that every effort would be made to ensure that participation in the research would be kept anonymous and that their identity would be confidential, and that their participation was voluntary.
Analysis
Criteria described by Corbin and Strauss (2015) to strengthen the quality of this research study included ensuring that the research “fit” or resonated with participants and those who read the research and “variation” (Corbin and Strauss, 2015). Since data collection and analysis occurred concurrently; we utilized a modified version of member checking. For instance, following the completion of the interview, we shared some key points that the participant made during the interview and allowed the participant to expand or clarify any points. We also discussed any descriptive themes that appeared to arise from the interview and allowed the participant to expand upon or refute. Participants were all in agreement with themes.
To ensure variation, a sampling matrix was used to capture the diversity of the research participants. The sampling matrix consisted of information such as the participant’s ID, age, ethnicity, the age of ethnicity of family members, number and locations of deployments the military parent had undergone, and the length of relationship. As concepts and categories emerged, variations were also noted among concepts and categories as well as between participants.
During coding, the primary data analysis technique is constant comparison, which involves breaking down data into manageable parts to explore similarities, differences, and consistencies within the data (Turner & Astin, 2021). Constant comparison unfolded first by comparing narratives from the same participant, and later, by comparing passages from one participant to another to extract similarities and differences. Text from one participant was compared with text from another participant to determine whether they were experiencing and responding to the same issue. If the chunks of text were different, unique codes were assigned. Similar texts were assigned the same codes. One example appeared between two different participants whose code was labeled “responding angrily towards children” when one articulated that “he is very quick to anger with the kids.” The other participant indicated that “he will start screaming at the kids when he is mad.” Through constant comparison, a description and analysis of emergent themes were generated and recorded, backed up with supportive quotes to reflect upon challenges families experience when they reside with a military parent diagnosed with PTSD.
Participants
In total, 25 participants, including 21 partners and 4 adult children were interviewed on one occasion. Primary data collection included either face-to-face or telephone interviews (depending upon participant preference). Interviews were semi-structured and in-depth and were guided by a review of the literature and noticeable gaps. Semi-structured interviews enabled consistency of concepts over the course of the interviews with the concepts, ensuring that the same concepts were covered in each interview. Interviews were approximately 30 min to 1 hr. Data collection took place from December 2018 to December 2020.
Initial data collected were analyzed, starting at 1-week post interview. Participants were asked about their experiences and challenges they encountered. At the same time, after the slate of questions was covered, participants were invited to add their thoughts on the subject matter. Nineteen non-military parent participants were white, and 2 were Indigenous; and all four adult children were white. The partners’ age ranged between 27 and 53; whereas the adult children aged between 18 and 24. Except one partner and one adult child identified themselves as male, all other participants were female. The numbers of deployment of military parent ranged between one and five. The numbers of children among the participant ranged between one and four.
Findings
Family stressors increased as challenges became more evident. In response to the stressors, several presenting concerns and challenges emerged. The findings are broken down into presenting challenges experienced by the military parent, non-military parent, children, and the family as a whole.
Military Parent Presented Challenges
Deteriorating Self-Care
As military-related PTSD symptoms amplified, some military parent’s self-care deteriorated. For example, Laura shared that “he was not managing day to day. He did not remember to have a shower without me telling him to.” Although not all military parent’s self-care deteriorated, for some military members, their hygiene changed drastically from before they developed military-related PTSD. Zoey indicated “his hygiene went down a lot. He wasn’t showering regularly and to be honest it was too much.” This deterioration in self-care occasionally resulted in challenges in the intimate relationship. Some non-military parents no longer found the military parent to be as attractive as they once were. Zoey went on to state, “I was finding that I was not as attracted to him as I used to be. I had to be blunt with him and share this with him and talk to him about taking care of himself better.” The deteriorating self-care resulted in Zoey having a difficult conversation with the military parent about caring for his hygiene.
Increasing Anger Outbursts
All of the participants revealed that there was an escalation in anger over time displayed by the military parent toward family members, community members, and external systems. Increasing anger outbursts were the most common emotion shared by participants. When asked what anger looked like for the military parent, Kristy disclosed, there’s been a few incidents like we were crossing the crosswalk at Walmart, and someone was like revving their engine at us. When we are like going and then [the person] actually did move the car towards us and I was pregnant, carrying one, and holding another child. And anyway, we were in separate vehicles, and he went after the guy. Yep, got in his truck and followed, buddy. I was like, oh, he’s going to kill him.
All of the adult children and non-military parents revealed that the military parent displayed anger as a prominent behavior. Military parents were easily angered and took it out on their families, including children. For example, Barb expressed “So, they are impacted by being yelled at instead of communicated at.” Occasionally, children were targets of the military parent’s anger. Beverly echoed Barb’s sentiment, reporting that her husband frequently displayed anger toward the children, “He was always angry at the kids over nothing. . . like, nothing at all.” Anger outbursts were also observed by children. Adult child, Janine, shared an example of her military parent’s anger, I’d say the first time I personally really noticed a change in my dad would be when my dad, who I had in my entire life before I was a teen . . . who I had never heard yell once, over the course of a weekend, lost his temper over the smallest things five or six times. I don’t really understand what happened to him.
It was not uncommon for the military parent’s anger to escalate, creating confusion and misunderstanding. For family members who were not used to this eruption in anger, this could come as a surprise. The explosive anger added an additional layer of stress to the family. The regular presentation of anger toward children created tension between the military parent and child. The sense of safety of family members decreased as family members often became targets of anger. As discussed below, in response to increased anger, non-military parents began to display mental health concerns while children became emotionally dysregulated. The family also began to lose intimacy as the military parent isolated more.
Non-military Parent Presented Concerns
Increasing Safety Concerns
When the military parent’s mental health condition deteriorated, family members became worried for the military member or themselves as safety concerns emerged. Safety concerns became the paramount issue that families had to deal with instantly. They were forced to immediately address these safety concerns. Kelly shared that her husband has been “hospitalized against his will. I said to the psychiatric ward that he kept saying that he wants to kill himself and that he should just die.” Families took immediate action during a major breakdown. For example, Sydney identified that she became more vigilant to everyone safety in the family.
After he was hospitalized for trying to kill himself, I felt like I could no longer trust that he wouldn’t hurt himself. I couldn’t trust him to take care of the kids, so I had to always be there to make sure everyone was okay.
As the family went into crisis mode, mental health concerns of the non-military parent emerged.
Displaying Mental Health Concerns
As the military parents’ functioning deteriorated, the non-military parents also faced challenges. They talked about developing mental health issues. Some mental health issues were directly connected to the military parent’s military-related PTSD, such as when a non-military parent developed secondary PTSD. Other mental health issues were further exasperated by the military parent’s military-related PTSD. Non-military parents reported feelings of helplessness, such as Ashley who claimed, “it also impacts you so trying to keep connection in the relationship because nothing I was doing was working. I could not fix it. It impacts my mental health because nothing I was doing was working.” Michelle expanded on the devasting impact on her mental health.
I was diagnosed with vicarious trauma. It was then confirmed again by another psychologist. It is not just a burned-out caregiver. I was no longer thinking right. My cognitive abilities. . .. that’s one of the things that bothered me the most. I used to feel like a somewhat intelligent person, and I couldn’t hold a job. I didn’t feel like I could have an intelligent conversation anymore. Something like going back to school terrified me because I couldn’t read a whole page of a book any longer.
As evident by the quotes, the challenges experienced by the military parent also had grave impacts on the non-military parent, marked by a deterioration in their well-being. As both parent’s well-being declined, many children also concurrently experienced challenges.
Challenges Experienced by Children
Child Dysregulating
Children were sensitive to the parents’ own issues and responded to their with their own emotional dysregulation. It was challenging for children to remain regulated and calm when those closest to them struggled. Amber shared, When my husband and I both had a hard time, my son would also get upset and either spend more time in his room or cry. This made it even harder for me. I almost felt like I was in a rut because everyone wasn’t doing so good, and when they weren’t we just kinda got worse.
The interconnection between individual and family functioning. Congruent with family systems theory, as one member struggled, so did others in the family. As parents struggled so did the children. One of the non-military parents, Merel, indicated that, the children are also sensitive to what is going on around them and get upset when we are upset but didn’t get it [PTSD]. They take it all in even when we think they don’t hear. They are easily frustrated or upset more it seems when things aren’t going well at home.
As challenges are present by the parents, the children also become more dysregulated. They are no longer able to function as they normally would. Children became more easily upset as they took in what was happening in their surroundings. The children may have also had difficulty understanding the PTSD.
Child Take on Adult Roles
Interpersonal boundaries shifted as children were expected to function beyond their developmental age to protect their non-military parent. As parent–child boundaries altered, so did the rules as to what behaviors were appropriate. One of the non-military parents, Christina, indicated that, the children are sensitive to my emotions and try to support me, sometimes by just giving me a hug after fighting with their dad. I try for them not to hear what is going on, but they often do. They see that I am hurting and try to comfort me.
When children adopted the role of comforting their parent, the family life cycle was disrupted. Children could not go through normal developmental milestones. Instead, children were expected to mature beyond their years to comfort and support their parents. Dixon also shared how his children would comfort their mother.
The kids will ask what’s wrong. And she will tell the kids that she is just sad, and they go hug her and tell her it’s okay. Our son is only six and he is asking his mom if she is alright.
This revelation demonstrated how the intergenerational roles shifted in an attempt to comfort and help their non-military parent. These children became parentified. They had to help their parents feel better as opposed to adhering to normal development where their parents were responsible for comforting them.
Overall Challenges as a Family
With military-related PTSD looming over the family, stress continued to amplify disruptions in the family unit as the military parent began to isolate from their family by spending more time alone or disengaging from others. Family dynamics were challenged as relationship tensions escalated.
The Family Became Further Distanced
Individuals with military-related PTSD typically isolated from other family members, which often involved them spending time alone. Isolation and withdrawal shifted family dynamics and affected relationships, transforming individuals from being involved and engaged in family activities to spending time alone away from the rest of the family. Dixon explained how his wife’s isolation affected their relationship.
She just started to become more introverted. Didn’t really do as much as we used to. We’d always go out on dates before PTSD. Now, I go out and do things with other people and for her it’s like a chore. So, it was hard for her to go out in different social situations.
In another example, the military parent resisted participating in activities they had been involved with in the past, further straining the family relationships. Mary, an adult child, disclosed that her father transformed from being family-oriented to detaching from family engagement.
He was always very close to me, like I was daddy’s little girl. He coached me in soccer and everything all the way until I was grown up. And then when he came back from Afghanistan, he started becoming more and more separated from us. He just started to isolate away from us. He was not really spending much time at home. He was sleeping in his truck. He’d like to go for days or weeks at a time, not being in touch with my mom or anybody else.
The pain and functioning of one family member reverberated throughout the family. Thus, the military parent’s expressed emotions affected family’s connectedness.
Escalated Family Tension
When the military parent or family member felt misunderstood, further family tension developed. Participants revealed that family dynamics shifted when either the military parent or family members felt misunderstood. Kelly shared how tension amplified when her partner believed that she did not understand what he was going through. “You don’t know what I’m going through. You’re not listening to me. You’re like, you’re the worst he would say.” Christina revealed similar challenges. “In his view I wasn’t supporting him. So, if he was blowing up, I was blowing up too.” Such escalated family tension could result in further family dysfunction.
Lacking Needed Support
Family tension was high and family functioning further waned as family members faced barriers to accessing supports. The lack of supports further affected family functioning. Zoey, as a non-military parent, felt insignificant and invisible in the military-related PTSD healing journey. She did not feel that her issues mattered.
They just look at the veteran and their needs. You have to prove how helping the kids and I would benefit him, and even then, it’s really difficult to prove. Even now I’m still not covered so I pay $180.00 each time out of my own pocket for personal counseling. I have not got that funding yet. It’s been a year. I’ve been paying for counseling for a year at least once a month. I’m not a veteran so I can’t deal with his caseworker. So, I’m dealing with him to get him to talk to his caseworker get all of the paperwork.
Dixon, a non-military parent and also a military member, offered his perception of the challenges with accessing support in the military.
Its not really health services from my point of view who are failing. It’s the chain of command. There’s still stigma on people trying to access healthcare for mental health. There’s still this misunderstanding from the military. When someone has PTSD, the military goes and says, they can’t be in a group environment and kicks them out but doesn’t always tell people where to get help.
Without being able to access supports, military parents’ functioning continued to deteriorate, alongside their ability to regulate their emotions.
Discussion and Implications
Family life unfolds within a social context. The military context is unique. Families do not exist in isolation. Family members are affected by one another and by external social systems. Table 1 summarizes the identified challenges experienced by families reported military-related PTSD.
Summarized Themes.
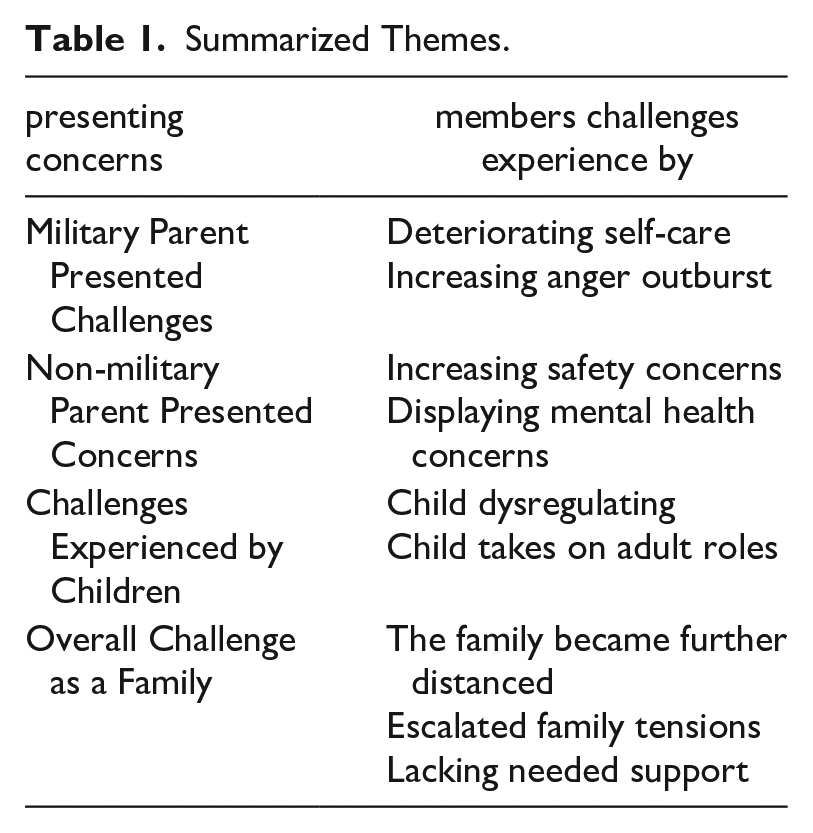
Even though some individual themes are not new, for example, increasing anger outbursts (Gerlock et al., 2014), displaying mental health concern of the non-military parent (Vasterling et al., 2015), and child taking on adult roles (Harrison et al., 2014), escalated family tensions (Creech & Misca, 2017), when these individual’s and familial challenges are combined and are not addressed with needed support services, families’ needs are not adequately met. Implications including prevention and intervention for military families and policy implications, specifically enhancing policies and improving communication are discussed.
Understanding of Military Families
Despite the evident impact of military-related PTSD on military families, more remains to be learned (Cramm et al., 2021). The lack of studies on military family challenges within a Canadian context underscores the importance of further research on how families and the military parent heal (DeVoe et al., 2018; Sullivan et al., 2018). It is important for military parents and their families to understand that they are not alone and to be able to understand what is going on for themselves and the family. Some participants shared that there was a lack of understanding about what was happening regarding their own emotions and the military parents. In response, prevention, intervention, policy and research implications for military families are discussed below.
Practice Implications
Prevention for Military Families
A wealth of studies point out that individually focused interventions often fail to accommodate a military member’s (both serving and retired veteran) systemic context. Without understanding the social context of individual problems, interventions will have limited impact on how families face challenges (DeVoe et al., 2018). This study extended previous research by identifying the challenges that exacerbate stress, such as enhanced tension from emotions running high in the family. Focusing on family interactions affected by trauma and contextual issues, capitalizes on helping professional’s expertise as person-in-environment specialists.
Interventions for Military Families
Family members can be helped to understand what is happening in their family. They can also work with helping professionals to alleviate potential secondary trauma. The non-military parent can also be supported so the children are not emotionally dysregulated in response to their parent’s challenges. Broader education among support systems, both formal and informal, can ease the stigma of military-related PTSD and enable these supports to be of benefit to military families.
Services can support families to better handle emerging stressors placing emphasis on the centrality of the family and acknowledging the interconnectedness of the military parent’s well-being and that of the family. The military parent with military-related PTSD will be helped when the family is functioning well. To support these families, they can be offered a menu of services upon the military parent’s return from a war front and the military-related PTSD diagnosis. Workshops and training can target service providers within the community. They can also target helpers involved in working with military-related PTSD and reinforce the importance of involving couples and families in their healing journey.
Policy Implications
Implications of this study are also at higher levels including at a policy level. The findings from this study, has implications on improved communication with families.
Enhancing Policies
Given that the military-related PTSD-inducing event(s) occurred as a result of military service, it is concerning that many participants continued to experience challenges as a result of the diagnosis. It is hoped that these findings will play an important role in shaping policies so that services are more “family friendly.” This includes an affirmation by the military of the importance of families and the impact that one member has on others. Despite the importance of families, current policies require that family members provide evidence that their formal support would benefit the military parent in order to receive funding to receive services. Given that research on the impact of military families on alleviating PTSD symptoms is in its infancy, how are families expected to address that while researchers are only now beginning to uncover? Often the military parent’s formal support such as a psychiatrist or therapist is needed to provide this evidence. “Family friendly” policies would recognize that it is apparent that a strong family means a stronger military parent, and thus, not force families to prove that the military parent’s well-being is connected by jumping through these tiring hoops, often resulting in families giving up fighting for supports.
Improved Communication With Families
Challenges presented trickle to all family members. Without the needs being meet of these families, they are at risk of long-term issue. These challenges can result in a breakdown in the family unit. Although one recommendation in On the Homefront: Assessing the Well-being of Canada’s Military Families in the New Millennium (Special Report to the Minister of National Defense, 2013) was to focus more on military families, a lag in military support for them remains. The Office of the Ombudsman, National Defence and Canadian Forces, recommended that the Department of National Defence (DND) take steps to “communicate more coherently, consistently, and forthright to, and with military families” (Daigle, 2013, p. 17). Statistics Canada (2018) revealed that military partners have challenges understanding the available supports for them and the military parent. More transparency is needed on what is available to address these challenges identified by participants. Case managers should be encouraged to be up to par on services to provide a comprehensive list of available resources to families.
Limitations and Future Research
There are two main limitations to this study, including the study being focused on limited inclusion criteria for children and having a homogeneous population.
Limited Inclusion Criteria for Children
The inclusion criteria for adult children limited sampling possibilities resulting in a small number of adult child participants. The inclusion criteria included an adult child, between the age of 18 and 25, who resided with a military parent for at least 6 months and had not moved outside of the military home for >2 years. Only four adult children were interviewed. Ideally, adult children’s numbers being equivalent to partners’ numbers would be beneficial to ensure that their voices are adequately included. Younger children are vulnerable population, and were therefore excluded. However, if sufficient protections for children were put into place, future research could include them.
This study looked at the intimate life of families experiencing military-related PTSD. It gave voice to its forgotten victims—families. The voices of children are important to understand the impact of military-related PTSD and family healing journey and future research can place more emphasis on military children. Specifically, intimate partners are the primary support for military parents (Skomorovsky et al., 2019). Therefore, it is critical that the well-being of intimate partners is maintained as well. A more in depth look at the couple relationship would uncover more detail about relational stressors. The marital relationship is the foundation of the family. However, children are often overlooked with most services focusing on the couple relationship (Rowan-Legg, 2017; Stelnicki, 2018). In addition, child and youth mental health is a growing concern in Canada and beyond (Alberta Health, 2017; Mental Health Commission of Canada, 2015; World Heath Organization [WHO], 2020). Proper prevention and intervention on military-related PTSD within the families certainly will help these young generations to developmental wellness. Therefore, more future research is needed to be conducted on military children and the challenges they experience.
Homogeneous Population
Although there were attempts to capture diverse populations, overall, the sample was homogeneous, limiting the scope of the findings. Initially only one adult child participated in the study. To recruit more adult children and ensure that data was richer, a modification was made to ethics to also recruit participants online through the Military Family Resource Centre’s (MFRC) newsletters and Facebook page across Alberta. Following the shift to recruiting online, three more adult children participated in addition to 16 non-military parents.
One notable critique of family military studies is that existing research has often been confined to two parent heterosexual couples (Gribble et al., 2020). This study was limited to a predominantly two parent, heterosexual families, with males most often being the military parent. Nevertheless, diversity is prevalent in the military. As an example, 14% of Canadian regular forces with children are single parents and 1,750 military parents also have other dependents (which can include anyone who is financially dependent on another member) in the home, including parents or siblings (Manser, 2020a).
The only other ethnicity other than white represented in this study was Indigenous. All of the partners interviewed reported being in a relationship with the military parent whom they identified as white, except for one who indicated that her military partner was Indigenous. Although this is not surprising given that in 2016, the Canada Department of National Defense, Employment Equity Report 2015-16 reported that 2.6% of military parents were Indigenous and 8.3% identified as a visible minority, future studies would be beneficial that look at diversity and other family compositions.
Participants who identified as female were also the predominant gender. There was one adult child and one non-military parent who identified as male. Despite efforts to recruit females in the CAF, males represent the majority of members serving and retired. In 2019, just under 15% of serving CAF members were women (Statistics Canada, 2020).
Conclusion
Military families face a unique set of challenges that strain family resources beyond those of civilian families. The challenges of military-related PTSD exacerbate this strain. The lives of the military family and military culture are intimately intertwined, making their unique constellation of issues amenable to a systemic analysis (Everson & Camp, 2011). It also means that we need to examine the adaptation and fit of the military family with its environment (Gitterman & Germain, 1980/2008). With ongoing knowledge and targeted intervention at family and larger macro system levels, military families will be better able adapt to the challenges of military-related PTSD.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Dr. Collins’s dissertation research was funded through the Centennial Flame Research Award and Wounded Warrior and Canadian Institute for Military Research and Health.
Disposition editor: Cristina Mogro-Wilson
Ethics Approval
Ethics approval was obtained through the University of Calgary Conjoint Faculties Research Ethics Board.
