Abstract
Introduction:
Transgender and gender-diverse (TGD) individuals face health disparities and workplace discrimination, yet the job and health outcomes of TGD nurses remain underexplored.
Purpose:
To investigate how gender identity affects job and health outcomes.
Methods:
This cross-sectional observational study included 52,491 nurses (52,455 identifying as cisgender and 36 as TGD) in New York and Illinois surveyed in 2021. Job outcomes were burnout and job dissatisfaction. Health outcomes were depression, anxiety, and overall health ratings. Propensity score weighting was used to address confounding factors. Doubly robust methods were applied to refine estimates.
Results:
Compared with cisgender nurses, TGD nurses had higher odds of high burnout (adjusted odds ratio [aOR] = 2.60, p = .036), job dissatisfaction (aOR = 2.21, p = .044), poorer overall health (aOR = 3.98, p < .001), and more depressive (b = 0.82, p = .013) and anxiety symptoms (b = 0.76, p = .044).
Conclusions:
TGD nurses reported poorer job and health outcomes than cisgender nurses, underscoring the need to identify workplace factors associated with these disparities.
Introduction
Burnout remains a persistent challenge in the nursing workforce and has been further exacerbated by the COVID-19 pandemic (Shah et al., 2021). Extensive research demonstrates that organizational conditions play a central role in shaping nurses’ job outcomes (Gershon et al., 2007). Nurses from historically marginalized groups, particularly racial and/or ethnic minority nurses, experience disproportionately higher levels of burnout, reflecting the cumulative effects of structural inequities embedded within health care organizations (Brooks Carthon, Brom, et al., 2024; Brooks Carthon, Nikpour, et al., 2024). These findings underscore that burnout is not merely an individual-level phenomenon, but one that is produced through institutional and social contexts.
Despite growing attention to equity in the nursing workforce (American Nurses Association, 2024), gender identity has been largely absent from empirical investigations of job and health outcomes among nurses. Although lesbian, gay, bisexual, transgender, queer or questioning, and other sexual and gender-diverse (LGBTQ+) employees experience higher levels of workplace mistreatment than their non-LGBTQ+ peers (Human Rights Campaign Foundation, 2023), most national nursing surveys, including the National Sample Survey of Registered Nurses (Health Resources & Services Administration, 2024), do not systematically collect information on gender identity or sexual orientation. As a result, the experiences of transgender and gender-diverse (TGD) nurses remain largely invisible in workforce research, limiting understanding of how organizational environments may differentially affect their well-being.
Gender identity is not an isolated personal attribute but a socially situated characteristic that shapes, and is shaped by, workplace structures, norms, and policies (Nagoshi et al., 2012). For TGD nurses, interactions within health care organizations may involve heightened exposure to misgendering, exclusion, and lack of institutional support, which can accumulate over time to affect job-related stress and mental health (Yu, Tibbitt, et al., 2025). Evidence from broader workforce studies indicates that TGD employees are more likely than cisgender workers to encounter hostile or invalidating workplace climates (Human Rights Campaign Foundation, 2023). However, nursing-specific research has not adequately examined whether and how these organizational dynamics translate into measurable differences in burnout, job dissatisfaction, and health outcomes. This study addresses a critical gap in nursing workforce research by moving beyond descriptive accounts of marginalization to quantitatively examine the association between gender identity and job and health outcomes among nurses, providing empirical evidence on the occupational well-being of TGD nurses and clarifying how gender identity functions as a structurally relevant factor shaping workforce outcomes.
Conceptual Framework
This study is guided by the Systems Model of Clinical Burnout and Professional Well-being developed by the National Academy of Medicine’s Action Collaborative on Clinician Well-Being and Resilience (National Academies of Sciences, Engineering, and Medicine, 2019). The model conceptualizes burnout and well-being as emergent outcomes of interactions across three interrelated levels: frontline care delivery, health care organizations, and the external environment. Organizational policies, workplace norms, staffing structures, and leadership practices shape job demands and resources at the point of care, while broader sociopolitical and regulatory environments influence the degree of institutional support or marginalization experienced by clinicians. Individual characteristics do not operate in isolation but rather condition how clinicians are exposed to, and affected by, these multilevel forces (National Academies of Sciences, Engineering, and Medicine, 2019).
Within this framework, gender identity is conceptualized as a structurally situated factor that influences nurses’ exposure to organizational stressors and supports, rather than as an intrinsic risk factor. For TGD nurses, gender identity may modify how organizational policies, workplace climates, and external sociopolitical conditions are experienced, thereby shaping job outcomes, such as burnout and job dissatisfaction and downstream health outcomes, including depression, anxiety, and overall self-rated health. Guided by this framework, we examined whether TGD nurses experience poorer job and health outcomes than cisgender nurses, interpreting observed differences as reflective of differential exposure to organizational and systemic conditions rather than individual vulnerability. This framework also informs interpretation of the findings by situating observed disparities within modifiable workplace and organizational contexts.
Method
Ethical Considerations
All study procedures received approval from the University of Pennsylvania Institutional Review Board, which determined that the study qualified for expedited review (IRB protocol number: #834307).
Participation involved minimal risk to participants and consisted of completion of a voluntary, anonymous survey. Prior to participation, nurses were provided with information describing the purpose of the study, the voluntary nature of participation, and assurances of confidentiality and anonymity. No identifying information was collected. Informed consent was implied through completion of the survey.
Study Design and Data Source
This cross-sectional observational study utilized the 2021 RN4CAST–NY/IL survey data from registered nurses in New York and Illinois, collected during the pandemic between April 13, 2021 and June 22, 2021 (Aiken et al., 2023), to examine job outcomes and working conditions. All actively licensed registered nurses in these states were invited to participate in an online survey, resulting in a data set of 70,072 nurses.
Study Sample
Survey respondents reported their employment status, indicating whether they were currently employed in health care, employed outside of health care, not currently employed, or retired. Given that burnout is an occupational phenomenon stemming from chronic workplace stress characterized by emotional exhaustion, cynicism toward one’s work, and reduced professional efficacy (World Health Organization, 2019), a subset of 52,833 staff nurses employed both in health care and non-health care settings, excluding those who were not working or retired, was used to evaluate job outcomes and health outcomes.
From the initial pool, we included both cisgender and TGD nurses. The gender question, “What is your gender?” offered three response options: “Man,” “Woman,” and “Other (please specify).” Nurses who selected “Other” had the opportunity to specify their gender. We initially excluded 287 nurses who did not respond to the gender question. In addition, we excluded 55 nurses who chose “Other” but either did not provide a written response or provided an invalid response. As a result, the final sample comprises 52,491 nurses, including 52,455 cisgender nurses who selected the response options “Man” or “Woman” (47,198 women and 5,257 men) and 36 TGD nurses who specified their identities in written responses as “Transgender” (n = 10), “Non-binary” (n = 19), “Genderqueer” (n = 5), and “Agender” (n = 2; Figure 1).
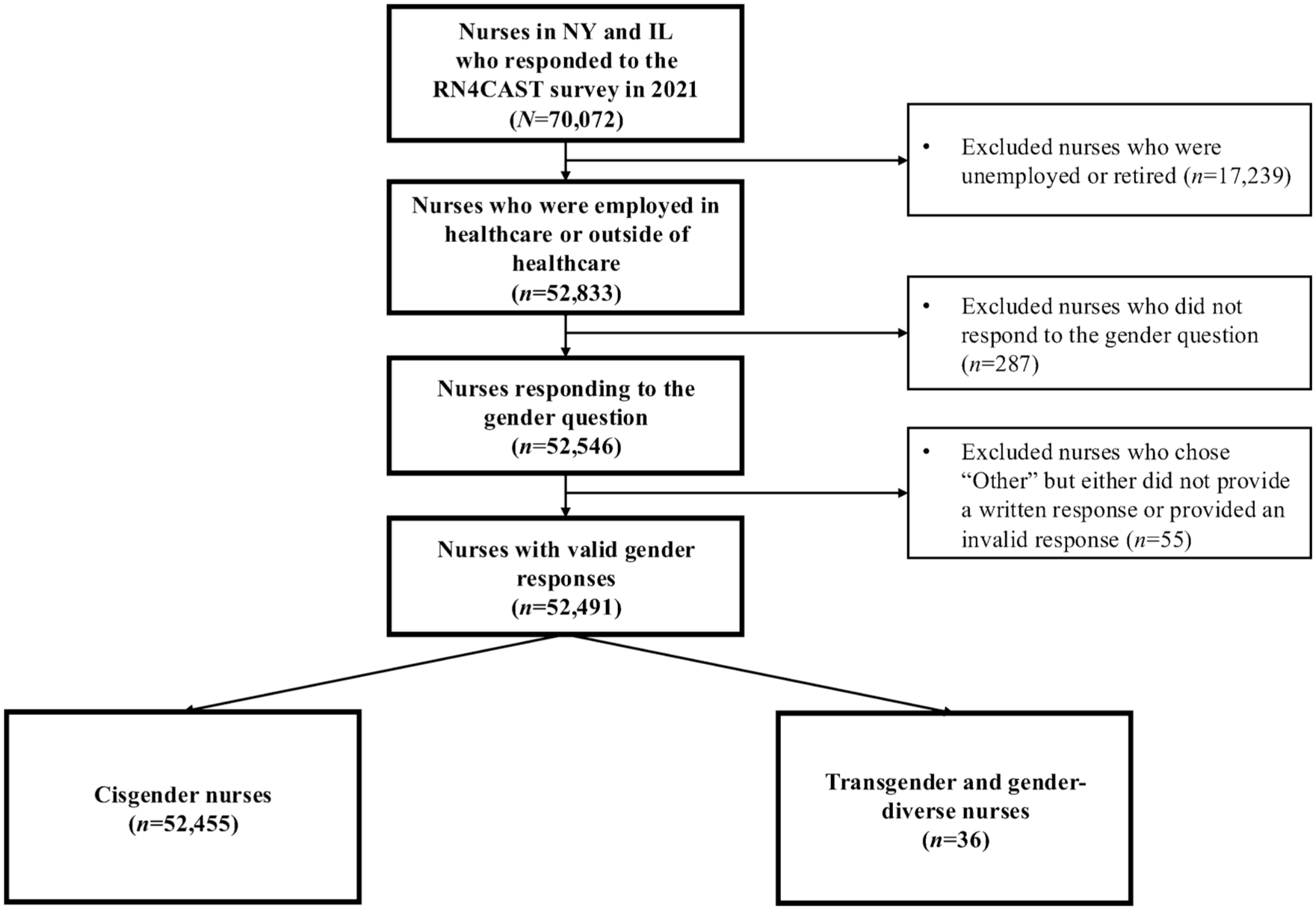
Subject Inclusion Diagram.
We collapsed these identities into a single TGD category for analytic purposes based on both conceptual and methodological considerations. Conceptually, these identities share common exposure to gender-related marginalization in health care workplaces, such as misgendering, exclusion from gender-normative organizational structures (Huffman et al., 2021), and limited institutional recognition, which are theorized to affect job stress and health outcomes. Methodologically, the small number of respondents in each gender-diverse subgroup precluded stable estimation of separate effects and increased the risk of sparse-data bias and unstable propensity score (PS) weights. This approach enabled a more robust examination of whether nurses whose gender identity falls outside the cisgender binary experience systematically different job and health outcomes, while acknowledging heterogeneity within the TGD population that could not be examined in this study.
Study Variables
Job Outcomes
Burnout was measured using the nine-item Emotional Exhaustion Subscale from the Maslach Burnout Inventory (Maslach et al., 1997). Participants rated each item on a 7-point Likert-type scale, where responses ranged from “0 = never” to “6 = every day.” Sum scores were calculated, with possible scores ranging from 0 to 54. Cronbach’s alpha for this scale in our analytic sample was .95. A score of 27 or above was classified as indicating high burnout (Maslach et al., 1997). The variable was dichotomized as follows: 0 = no high burnout (<27) and 1 = high burnout (≥27).
Job dissatisfaction was evaluated using a single-item measure. Participants indicated their overall job satisfaction by answering the question, “Overall, how satisfied are you with your job?” on a 4-point Likert-type scale, with responses ranging from “1 = very satisfied” to “4 = very dissatisfied.” The responses were then dichotomized: 0 = satisfied (combining “very satisfied” and “moderately satisfied”) and 1= dissatisfied (combining “very dissatisfied” and “moderately dissatisfied”).
Health Outcomes
Overall health was evaluated using a single-item measure initially recorded on a 5-point Likert-type scale. Participants rated their overall health by responding to the question, “Over the past 4 weeks, how would you rate your overall health?” with options ranging from “1 = excellent” to “5 = very poor.” The responses were subsequently dichotomized: 0 = excellent or good health (combining “excellent” and “good”) and 1 = fair or poor health (combining “fair,” “poor,” and “very poor”).
Depression was measured using the Patient Health Questionnaire-2 (Kroenke et al., 2003). Participants rated their experiences on a 4-point Likert-type scale, ranging from “1 = not at all” to “4 = nearly every day.” Cronbach’s alpha for this two-item scale was .87. Scores were obtained by summing the responses to each item, with higher scores indicating greater depressive symptoms.
Anxiety was measured using the Generalized Anxiety Disorder-2 (Kroenke et al., 2007), with participants responding on the same 4-point Likert-type scale as the depression scale. Cronbach’s alpha for this two-item scale was .88. Scores were determined by summing the responses to each item, with higher scores indicating greater levels of anxiety symptoms.
Nurse Characteristics
We selected covariates for the PS model based on prior theory and empirical evidence. We were also mindful of the risk of overadjustment and collider bias, particularly given the extremely small number of TGD nurses. To mitigate these risks, we intentionally restricted covariates to characteristics that are largely antecedent to both TGD identification and outcomes, rather than variables likely to lie on the causal pathway between gender identity and job or health outcomes. Specifically, we included age (Gómez-Urquiza et al., 2017; Hatch et al., 2018), race and ethnicity (Brooks Carthon, Brom, et al., 2024), years of experience at the current hospital (Dyrbye et al., 2019), highest nursing degree, entry level of nursing education (Hayes & Bonner, 2010; Jansen et al., 1996), job role (Brayer & Marcinowicz, 2018), and employment in hospital settings (Robat et al., 2021). These variables capture stable sociodemographic and professional characteristics that shape nurses’ work contexts, opportunities, and health risks and have been shown in prior research to be associated with both workforce outcomes and differential experiences among gender-diverse individuals.
Age and years of experience at the current hospital were treated as continuous variables and did not exhibit high correlation with each other (Pearson’s r < .5), suggesting that each captures distinct dimensions of career stage and tenure rather than redundant information. Race and ethnicity were included given well-documented structural inequities in nursing employment, workplace treatment, and health outcomes that may intersect with gender identity (Yu et al., 2026). The race question included options, such as American Indian or Alaskan Native, Asian, Black or African American, Native Hawaiian or Other Pacific Islander, and White. The ethnicity question had two choices: Hispanic or non-Hispanic. These two variables were combined to create a binary race and ethnicity measure of non-Hispanic White versus racial and/or ethnic minority to align with the National Institute on Minority Health and Health Disparities definition of health disparity populations and to reduce sparsity and avoid unstable estimates given the small number of TGD nurses in the sample (National Institute on Minority Health and Health Disparities, 2025).
Educational attainment and job role were included because they reflect professional positioning within health care organizations, which may influence exposure to job stressors, autonomy, compensation, and health risks, and may also differ systematically by gender identity due to barriers in career advancement. The entry level of nursing education and the highest nursing degree had four options: diploma program, associate degree program, baccalaureate degree program, and graduate program. These were then dichotomized into two groups to capture meaningful distinctions in professional preparation: associate degree or diploma program and baccalaureate degree or higher. These degree variables did not exhibit high correlation (Pearson’s r < .5). The job role question had four options: staff nurse or direct care nurse, nurse manager, advanced practice nurse, and other (please specify). After reviewing all written responses, we dichotomized these roles into direct patient care (e.g., staff nurse and advanced practice nurse) and non-patient care roles (e.g., management, education, and administration), reflecting differences in clinical exposure and work demands. Employment in hospital settings was included to ensure comparability of organizational context, given that job demands and health risks differ substantially between hospital and nonhospital settings. This variable was recorded as a binary indicator with response options of yes or no.
Statistical Analysis
All data analyses were conducted using R version 4.5.1. Initially, we performed descriptive statistics to examine unadjusted difference in job and health outcomes by TGD status. Following this, we utilized PS (Rosenbaum & Rubin, 1983) and doubly robust methods (Bang & Robins, 2005) to evaluate the extent to which differences in job and health outcomes could be attributed to TGD status versus measured confounding factors.
PS methods are preferred over traditional regression models when comparing groups that differ significantly on some confounders. For example, PS weighting provides less biased estimates of the association between job and health outcomes and TGD status by addressing issues related to linearity assumptions and model specification sensitivity inherent in traditional regression. The PS represents the conditional probability of a nurse being TGD versus cisgender given the observed confounding factors. We used this probability to create weights (McCaffrey et al., 2004) for cisgender nurses. Cisgender nurses with characteristics similar to TGD nurses received higher weights (up-weighted), while those with dissimilar characteristics were given lower weights (down-weighted).
We fitted the PS model using the twang R package, which employs generalized boosted models rather than traditional logistic regression and targets the average treatment effect on the treated (ATT; Ridgeway et al., 2025). Given the substantial imbalance in group sizes between TGD nurses and cisgender nurses, we conducted extensive diagnostics to assess PS overlap, weight stability, and the plausibility of the positivity assumption. To evaluate overlap, we examined the distribution of PSs for TGD nurses and cisgender nurses using density plots and boxplots and confirmed substantial overlap between groups. The observed ranges of PSs were nearly identical for the TGD and cisgender groups, indicating no evidence of non-overlap. We further assessed weight stability by inspecting the distribution, mean, and variance of the ATT weights and found no extreme or influential weights. Covariate balance was evaluated using standardized mean differences, Kolmogorov–Smirnov (KS) statistics, and balance plots, all of which demonstrated adequate balance after weighting. KS statistic values greater than 0.10 were used to indicate potential imbalances (McCaffrey et al., 2013). When covariates contained missing values, twang balanced the rates of missingness between the cisgender and TGD groups during weight construction. Therefore, observations with missing covariate data were not excluded from the PS weighting procedure (Ridgeway et al., 2025).
Although PS weighting addressed most imbalances, small imbalances remained, necessitating the use of doubly robust methods. Doubly robust methods minimize bias from small confounder differences (Golinelli et al., 2012). We obtained doubly robust estimates by fitting a PS-weighted logistic regression for burnout, job dissatisfaction, and overall health rating, and a PS-weighted linear regression for depression and anxiety, including all confounding variables from the PS model and the TGD status indicator. Both the PS-weighted logistic and linear regressions were fitted using the survey R package to account for the design effect induced by the PS weights. The standard errors produced by the svyglm command are robust standard errors derived via the Taylor linearization method and are reported in Tables 3 and 4.
Results
The overall nurse participant characteristics are detailed in Table 1. Cisgender nurses had a mean age of 47.6 years with a standard deviation (SD) of 13.4, while TGD nurses had a mean age of 36.2 years (SD 9.7). Among cisgender nurses, 64.2% were non-Hispanic White, compared with 72.2% of TGD nurses. Baseline characteristics before and after PS weighting are also presented in Table 1. After applying PS weighting, the KS statistics for most confounding factors fell below 0.02 indicating that the PS weighting effectively balanced the distribution of these confounding factors between the cisgender and TGD groups.
Baseline Characteristics Before and After Propensity Score Weighting.
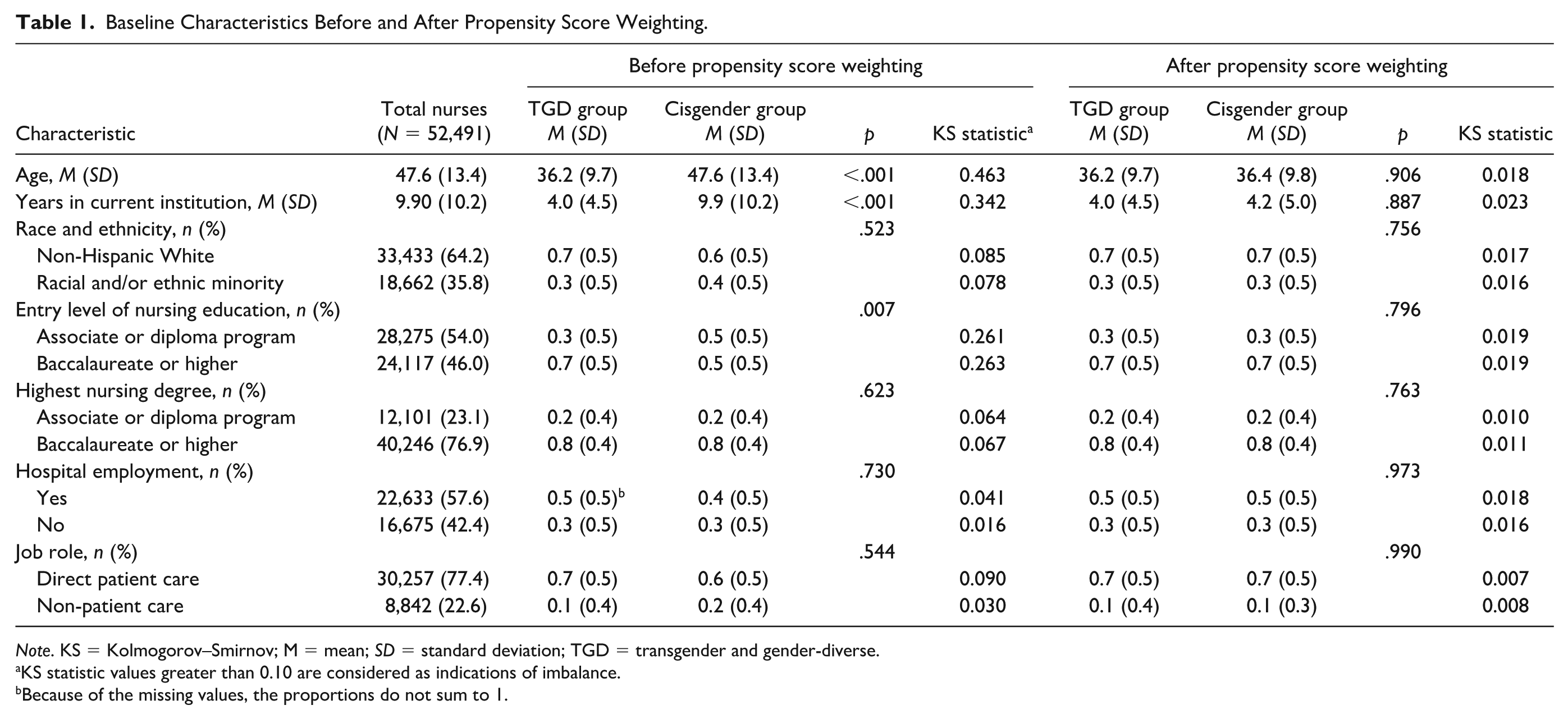
Note. KS = Kolmogorov–Smirnov; M = mean; SD = standard deviation; TGD = transgender and gender-diverse.
KS statistic values greater than 0.10 are considered as indications of imbalance.
Because of the missing values, the proportions do not sum to 1.
Table 2 presents unadjusted differences in outcomes between cisgender and TGD nurses. Supplemental Material 1 presents PS-weighted differences in outcomes. High burnout was reported by 39.4% of cisgender nurses and 66.7% of TGD nurses (p = .012). Job dissatisfaction was reported by 21.4% of cisgender and 41.7% of TGD nurses (p = .019). In addition, 25.5% of cisgender nurses and 61.1% of TGD nurses rated their health as fair or poor (p < .001). Mean depression scores were 1.0 (SD = 1.5) for cisgender and 2.0 (SD = 1.8) for TGD nurses (p = .001). Mean anxiety scores were 1.4 (SD = 1.7) for cisgender and 2.5 (SD = 2.0) for TGD nurses (p = .001).
Unadjusted Differences in Outcomes Between Cisgender and Transgender and Gender-Diverse Nurses.
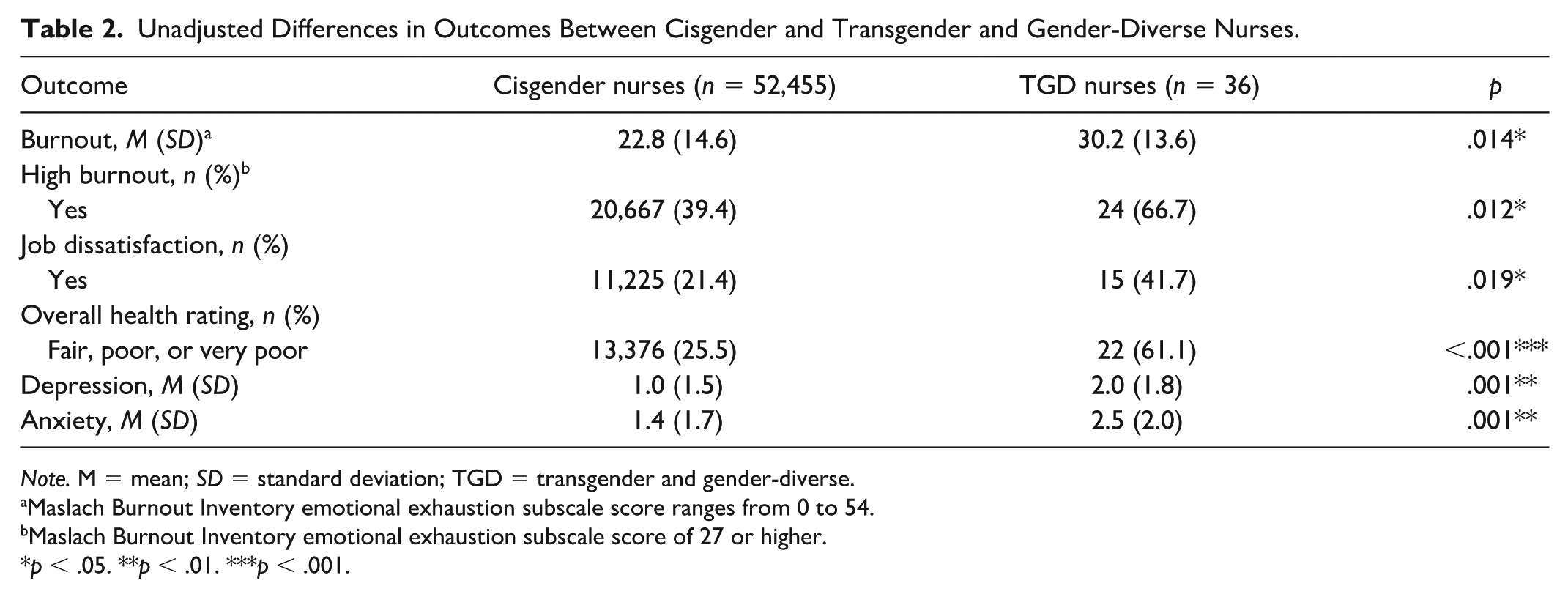
Note. M = mean; SD = standard deviation; TGD = transgender and gender-diverse.
Maslach Burnout Inventory emotional exhaustion subscale score ranges from 0 to 54.
Maslach Burnout Inventory emotional exhaustion subscale score of 27 or higher.
p < .05. **p < .01. ***p < .001.
The results of the PS-weighted logistic regression for burnout, job dissatisfaction, and overall health rating are presented in Table 3. Compared with cisgender nurses, TGD nurses were approximately 2.6 times more likely to experience high burnout (adjusted odds ratio [aOR] = 2.60; 95% confidence interval [CI] = 1.06, 6.34). TGD nurses were also about two times more likely to be dissatisfied with their job (aOR = 2.21; 95% CI = 1.02, 4.78) and nearly four times more likely to rate their health as fair or poor (aOR = 3.98; 95% CI = 1.80, 8.81).
Weighted Logistic Regression Results.
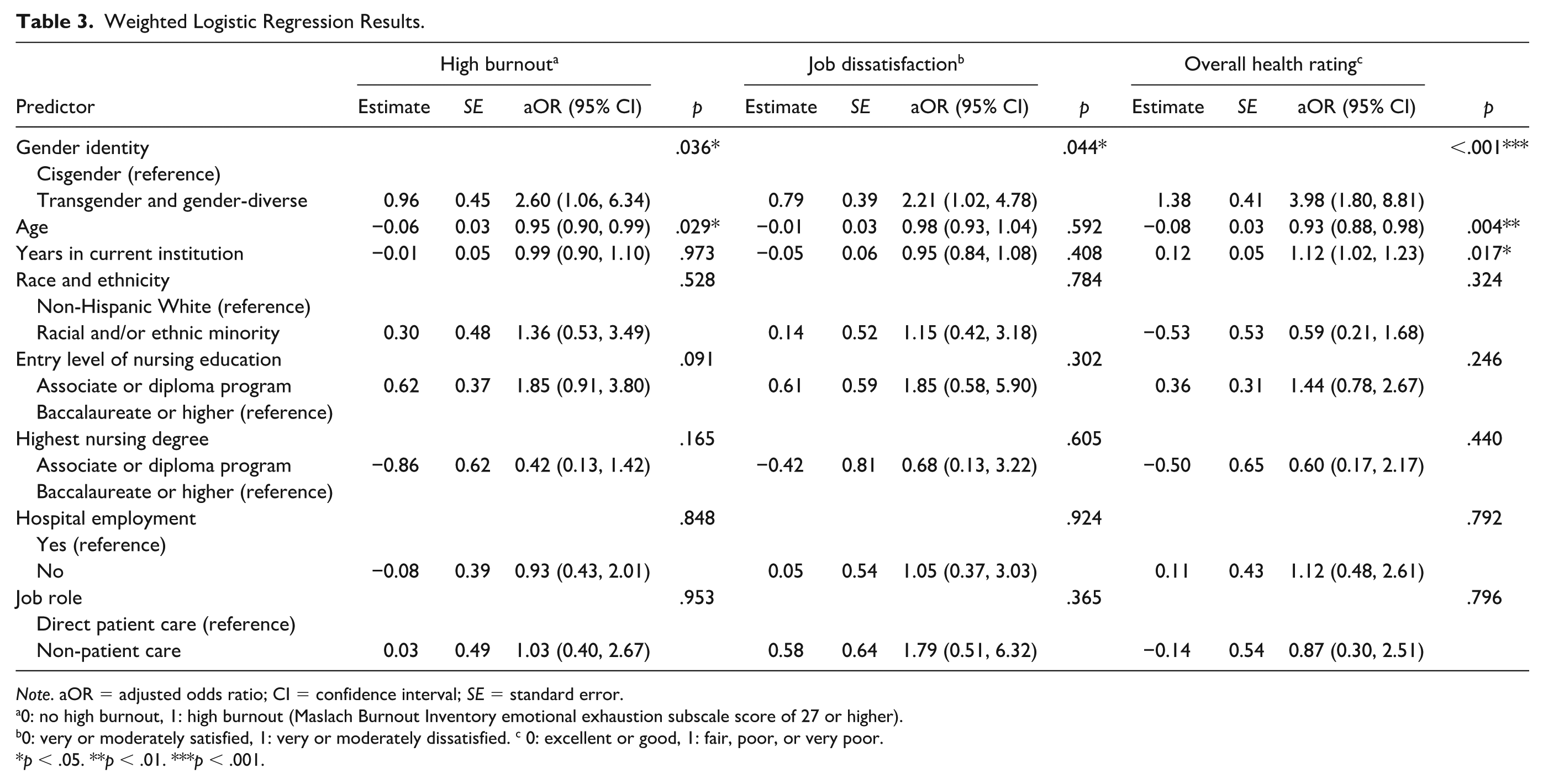
Note. aOR = adjusted odds ratio; CI = confidence interval; SE = standard error.
0: no high burnout, 1: high burnout (Maslach Burnout Inventory emotional exhaustion subscale score of 27 or higher).
0: very or moderately satisfied, 1: very or moderately dissatisfied. c 0: excellent or good, 1: fair, poor, or very poor.
p < .05. **p < .01. ***p < .001.
The PS-weighted linear regression results for depression and anxiety scores are shown in Table 4. Compared with cisgender nurses, TGD nurses reported experiencing depressive symptoms more frequently (b = 0.82; 95% CI = 0.17, 1.47) and anxiety symptoms more frequently (b = 0.76; 95% CI = 0.02, 1.50).
Weighted Linear Regression Results.
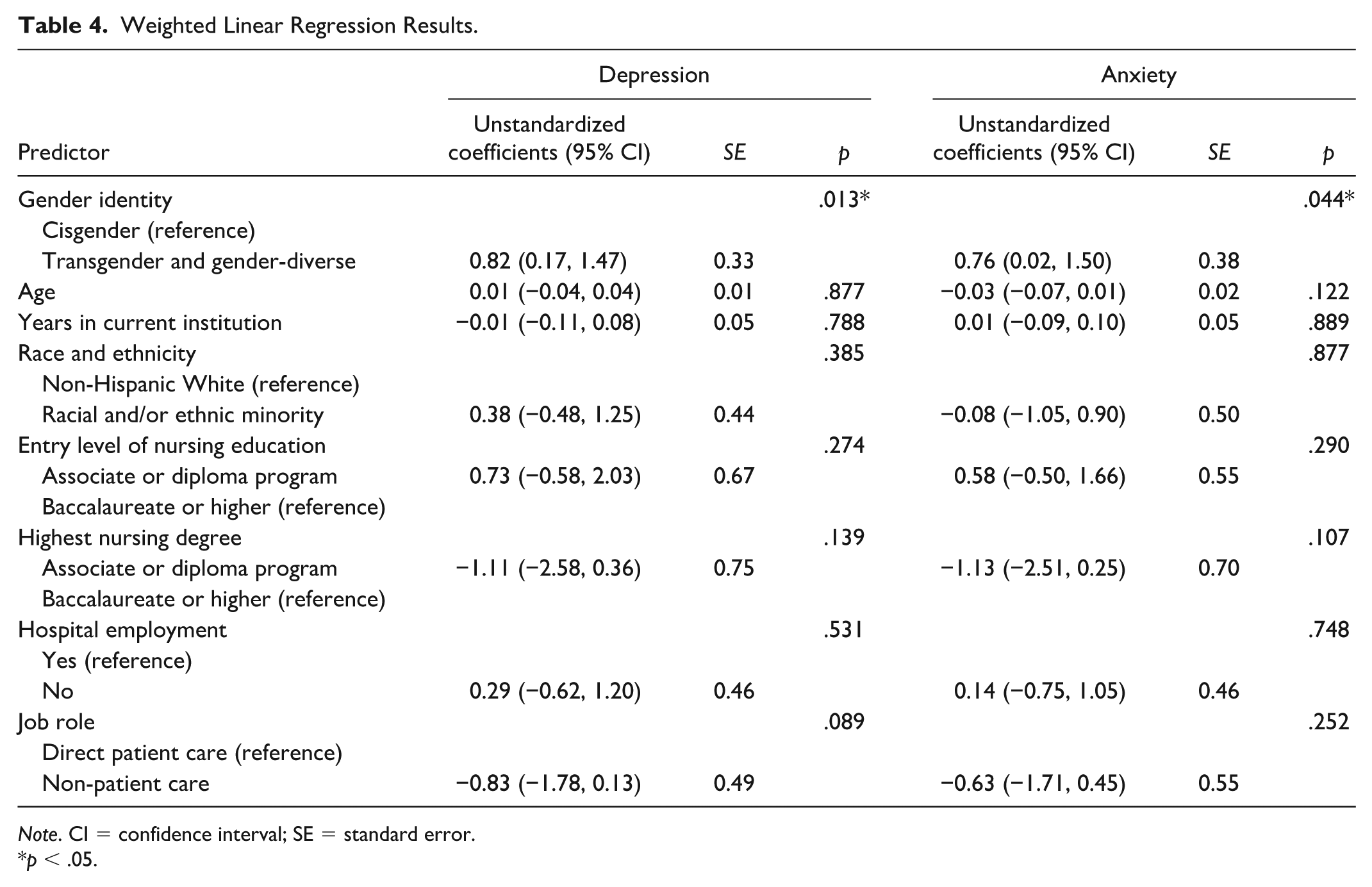
Note. CI = confidence interval; SE = standard error.
p < .05.
Discussion
This study examined job and health outcomes among TGD nurses, a critically understudied population in health care research, as no prior studies have specifically focused on job outcomes of TGD nurses. Our findings reveal that TGD nurses are more likely to experience higher levels of burnout, greater job dissatisfaction, and poorer health outcomes, including increased depressive and anxiety symptoms. TGD nurses face significant challenges in their work environments, such as unfair treatment and workplace discrimination (Yu, Tibbitt, et al., 2025), potentially leading to poor job and health outcomes. These results underscore the need for tailored interventions to support TGD nurses and promote more inclusive and supportive workplace environments.
The findings regarding poorer job and health outcomes among TGD nurses compared with cisgender nurses are consistent with a growing body of literature documenting the adverse occupational consequences of marginalization among TGD individuals across health care professional contexts (Wolfe, 2023), including physicians (Reece-Nguyen et al., 2022; Streed et al., 2024). Prior research suggests that these disparities arise not from individual characteristics alone but from structurally embedded workplace conditions, such as discriminatory organizational climates, limited institutional support, and persistent stigmatization (Reece-Nguyen et al., 2022; Streed et al., 2024; Yu, Tibbitt, et al., 2025). In health care settings, such conditions may include the absence of gender-affirming workplace policies, limited access to gender-neutral restrooms, inconsistent use of correct names and pronouns, and the lack of clear or trusted mechanisms for reporting gender-related mistreatment (Reece-Nguyen et al., 2022; Streed et al., 2024; Yu, Tibbitt, et al., 2025). Although these organizational factors were not directly measured in the present study, they represent plausible contributors to the elevated burnout, job dissatisfaction, and mental health symptoms observed among TGD nurses.
The elevated risk of burnout among TGD nurses likely reflects the cumulative impact of these gender-related workplace stressors in combination with well-established nursing-specific drivers of burnout, such as poor work environments and inadequate staffing (Muir et al., 2024). Prior research indicates that TGD employees across sectors frequently encounter microaggressions, misgendering, exclusion from professional networks, and organizational indifference to gender-related concerns (Davis & Yeung, 2022). Such experiences contribute to chronic stress and emotional exhaustion, which over time can manifest as burnout and job dissatisfaction (Corby et al., 2024; Schaufeli & Bakker, 2004). Importantly, when organizations lack formal policies, leadership accountability, or responsive reporting structures to address gender-related mistreatment, these stressors may be amplified (Köllen, 2016). Evidence further suggests that TGD employees are less likely than cisgender workers to perceive their employers as supportive of TGD individuals (Human Rights Campaign Foundation, 2023), reinforcing a cycle in which insufficient organizational protections erode morale and undermine workforce well-being.
Addressing these risks requires institutional-level action rather than reliance on individual coping strategies. Feasible system-level approaches include routine workforce climate assessments that explicitly measure gender identity and inclusion, leadership accountability metrics tied to equity and inclusion goals, and standardized onboarding and continuing education modules that establish expectations for respectful communication (Yu et al., 2023), correct use of names and pronouns, and psychological safety in the workplace (Huffman et al., 2021; Yu, Ancheta, et al., 2025; Yu et al., 2024; Yu, Tibbitt, et al., 2025). Such strategies align with organizational responsibility for creating inclusive environments and may help mitigate burnout among TGD nurses while strengthening overall workforce resilience. These proposed strategies are informed by prior literature and established workforce best practices and were not directly evaluated or tested in the present study.
Given the significant mental health disparities faced by TGD individuals, including higher rates of depression and an increased risk of suicide compared with cisgender individuals (Pellicane & Ciesla, 2022), this concern is further amplified by evidence that nurses, as a professional group, have a higher suicide risk than many other health care workers (Olfson et al., 2023). The disparity in burnout observed in this study therefore underscores the urgent need to explore the underlying drivers of burnout and to develop tailored interventions and support systems for TGD nurses. Potential strategies include access to confidential employee assistance programs staffed by clinicians trained in gender-diverse care, the development of peer support or affinity groups for gender-diverse staff, and supervisor training focused on psychological safety, inclusive leadership, and supportive management practices (Huffman et al., 2021; Yu, Tibbitt, et al., 2025). As more LGBTQ+ inclusive hospital policies are associated with improved nurse job outcomes and patient outcomes (Yu, Bauermeister, et al., 2025; Yu, McHugh, Bauermeister, Hanneman, & Brom, 2025; Yu, McHugh, Bauermeister, Hanneman, & Lasater, 2025) addressing burnout among TGD nurses is not only a matter of workplace equity but also a critical component of ensuring a resilient and diverse nursing workforce capable of delivering high-quality, inclusive patient care.
Overall, our findings should be viewed as a foundation for future inquiry rather than evidence of intervention effectiveness. By identifying disparities in job and health outcomes among TGD nurses, this study highlights the need for longitudinal and intervention-based research to determine which organizational strategies most effectively promote psychological well-being, job satisfaction, and workforce retention among gender-diverse nurses. These findings also offer an opportunity to catalyze critical discussions and policy changes within the nursing profession. This is particularly significant given the current federal-level hostility toward transgender health, rights, and research (Harvard Law School Forum on Corporate Governance, 2025; Sandhu et al., 2025). In this increasingly hostile environment, the nursing profession must take proactive steps to safeguard the well-being and rights of TGD individuals, both within the nursing workforce and among the broader patient population. In addition, nurse leaders should actively engage in policy advocacy at local, state, and federal levels, championing legislation that protects TGD health care access, employment rights, and research funding.
Strengths and Limitations
The strengths of this study include the use of PS weighting to address potential confounding factors and its focus on a significantly understudied population within health care. However, there are limitations. First, the survey’s gender question offered limited response options and relied on open-text specification for gender-diverse identities, which may have constrained how participants reported their gender and influenced both the representation of TGD nurses in the sample and the interpretation of findings. This measurement approach predates best practices recommending a two-step method that separately assesses gender identity and sex assigned at birth (National Academies of Sciences, Engineering, and Medicine, 2022). Future studies should employ more inclusive and standardized measures of sex and gender. Second, overall health and job dissatisfaction were measured using single-item indicators, which may not fully capture the multidimensional and dynamic nature of these constructs. Third, we did not adjust for factors, such as sexual orientation, workplace discrimination, shift work, income, or relationship status due to data unavailability. Although these variables may be associated with both gender identity and job and health outcomes, they are also plausibly downstream consequences of gender identity or mechanisms through which structural inequities operate. Adjusting for such variables could block meaningful causal pathways and bias effect estimates toward the null. Next, the sample is limited to registered nurses in New York and Illinois, states known for relatively progressive LGBTQ+ policies, which may limit generalizability. The cross-sectional design restricts causal inference, and the small number of TGD participants may limit statistical power. Finally, excluding nurses who did not report their gender may introduce bias if their experiences differ from those included in the analysis.
Conclusion
TGD nurses may face significantly higher levels of burnout, job dissatisfaction, and poorer health outcomes compared with their cisgender peers. This study underscores the urgent need to investigate TGD nurses’ experiences using inclusive data collection methods and to explore the underlying causes of these outcomes. Nursing as a profession, along with health care organizations, should continue fostering open dialogue about TGD health in the context of current federal-level hostility toward TGD health, rights, and research.
Supplemental Material
sj-docx-1-tcn-10.1177_10436596261426096 – Supplemental material for Job and Health Outcomes Among Transgender and Gender-Diverse Nurses
Supplemental material, sj-docx-1-tcn-10.1177_10436596261426096 for Job and Health Outcomes Among Transgender and Gender-Diverse Nurses by Hyunmin Yu, Daniela Golinelli, José A. Bauermeister, Karen B. Lasater and Matthew D. McHugh in Journal of Transcultural Nursing
Footnotes
Author Contributions
All authors made contributions to the conception and design of this article. All authors contributed to the acquisition, analysis and interpretation of data. HY drafted the manuscript. DG, JAB, KBL, and MDM revised the manuscript. All authors approved the final manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The primary author (HY) received postdoctoral fellowship funding from the Eidos LGBTQ+ Health Initiative at the University of Pennsylvania School of Nursing.
Ethical Approval and Informed Consent Statements
All study procedures received approval from the University of Pennsylvania Institutional Review Board (IRB protocol number: #834307). Prior to participation, nurses were provided with information describing the purpose of the study, the voluntary nature of participation, and assurances of confidentiality and anonymity. Informed consent was implied through completion of the survey.
Data Availability Statement
The data sets used and/or analyzed during the current study are not available.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
