Abstract
Introduction:
Nurses’ shortage in Western countries has driven reliance on internationally trained Black, Asian, and Minority Ethnic (BAME) nurses, who now play a crucial workforce role. However, they face challenges compared to native nurses, making it essential to understand their experiences for fostering inclusivity. This qualitative evidence synthesis explores the experiences of internationally trained BAME nurses in Western health care settings.
Method:
A comprehensive search of MEDLINE, Embase, CINAHL, Web of Science, and gray literature was carried out. Quality was assessed using the CASP tool, and data were synthesized using Thomas and Harden’s thematic synthesis approach.
Results:
This review of 38 studies identified three themes: Initial Adaptation Hurdles, Professional Adversities, and Coping Strategies. Nurses experienced cultural and communication barriers, unfamiliar policies, and discriminatory interactions, with racism forming part of their professional experiences.
Discussion:
Culturally tailored orientation, mentorship, and equitable opportunities are vital to enhancing integration and satisfaction, strengthening health care safety and performance.
Keywords
Introduction
Global nurse shortages and growing health care demands have resulted in an increased dependence on internationally trained Black, Asian, and Minority Ethnic (BAME) nurses in recent decades (International Council of Nurses, 2020). This trend is reflected in a 60% increase in internationally trained nurses (ITNs) in Western countries since 2010 (Zolot, 2019). Countries like the United Kingdom, Ireland, and Australia have become both the source and host countries for nurse migration (H. Li et al., 2014; Moshiri et al., 2022). This increased migration to Western countries has been driven by aging populations and longer life expectancy, raising the demand for health services (Seol, 2018; Tsujita et al., 2023). Additional factors include a shift from family or home-based care to institutional care, nurse attrition and aging in local workforces, and the growth of medical tourism contribute to the demand for ITNs in developed countries (Tsujita et al., 2023). This demand is further compounded by challenges such as the growing burden of chronic diseases, evolving health care delivery models, nurse–patient ratio guidelines, and workforce shortages due to nurse training rates falling behind the demand (Sasso et al., 2019).
In 2023, approximately one in seven nurses were born or trained in a nation other than where they presently work (World Health Organization, 2025). This suggests that many nurses have migrated or relocated to other countries for better personal and professional opportunities and improved socioeconomic status (Ung et al., 2024). Globalization and supply–demand dynamics have greatly influenced nurses’ international mobility (Sharplin et al., 2025). Ireland, for example, which had previously been a net exporter of nurses, experienced significant nurse shortages in the 1990s and has since begun recruiting ITNs to augment its nursing workforce (Organisation for Economic Co-operation and Development (OECD)/European Commission, 2024). The Nursing and Midwifery Board of Ireland (NMBI), in its State of the Register 2024 report, notes that approximately 39% of the nursing workforce in Ireland is internationally trained, with 31% of these nurses being from BAME backgrounds (NMBI, 2024). Most internationally trained BAME nurses are from India and the Philippines (NMBI, 2024). Although internationally trained BAME nurses have become an integral part of the health care system in Western countries, evidence suggests that the difficulties and challenges they face are far more diverse than those experienced by native nurses (Carter, 2019).
These challenges include loneliness, isolation, communication difficulties, being underestimated by colleagues and patients, as well as racism and prejudice (Iheduru-Anderson et al., 2021). In addition, research indicates that most internationally trained BAME nurses working in Western health care are subject to discrimination (Kline, 2014; Likupe et al., 2014; O’Callaghan et al., 2018; Tuffour, 2022; Walani, 2015), loss of autonomy and independence, poor career growth, poor workplace experiences (Carter, 2019), unequal opportunities, and pervasive double standards (Johnson et al., 2021). A supportive and positive working environment, language and communication skills support, collaborative teamwork climate, managerial support, opportunities for career progression, and positive work–life balance can enhance workplace integration and retention of internationally trained BAME nurses and create a safety culture (Roth et al., 2021). This highlights the need for diversity and inclusivity within the nursing workforce, directly impacting patient care (Williams et al., 2025). However, there is a lack of comprehensive understanding of the experiences of internationally trained BAME nurses. Therefore, this review aimed to synthesize the experiences and perspectives of internationally trained BAME nurses working in Western countries. The following research questions formed the basis for this review:
What does the published literature tell us about the experiences of internationally trained BAME nurses working in Western health care settings?
What knowledge gaps require attention in support of internationally trained BAME nurses in achieving excellence in Western health care settings?
Method
Design
Qualitative evidence synthesis (QES) was selected to systematically identify and synthesize evidence from the published qualitative literature regarding the experiences of internationally trained BAME nurses. A QES is a form of systematic review that systematically collects, appraises, and synthesizes findings from multiple primary qualitative studies. These primary studies typically employ qualitative data collection and analysis methods, producing rich and nuanced insights into participants’ experiences, perspectives, and priorities (Noyes et al., 2019). To enhance transparency, the Enhancing Transparency in Reporting the Synthesis of Qualitative Research (ENTREQ; Supplementary file 1) checklist is completed. This review aimed to gain a comprehensive and in-depth understanding of the experiences of internationally trained BAME nurses working in Western health care settings. The protocol was registered in the International Prospective Register of Systematic Reviews (PROSPERO; CRD42021292136).
Search Strategy
The search terms were based on the SPIDER (Sample, Phenomenon of Interest, Design, Evaluation, Research type) acronym (Cooke et al., 2012) (Table 1) and adapted for the different databases. The search was limited to studies published between January 2000 and March 2025, as this timeframe was to capture contemporary developments in health care systems and migration patterns relevant to the Western health care experiences of internationally trained BAME nurses.
Search Terms.
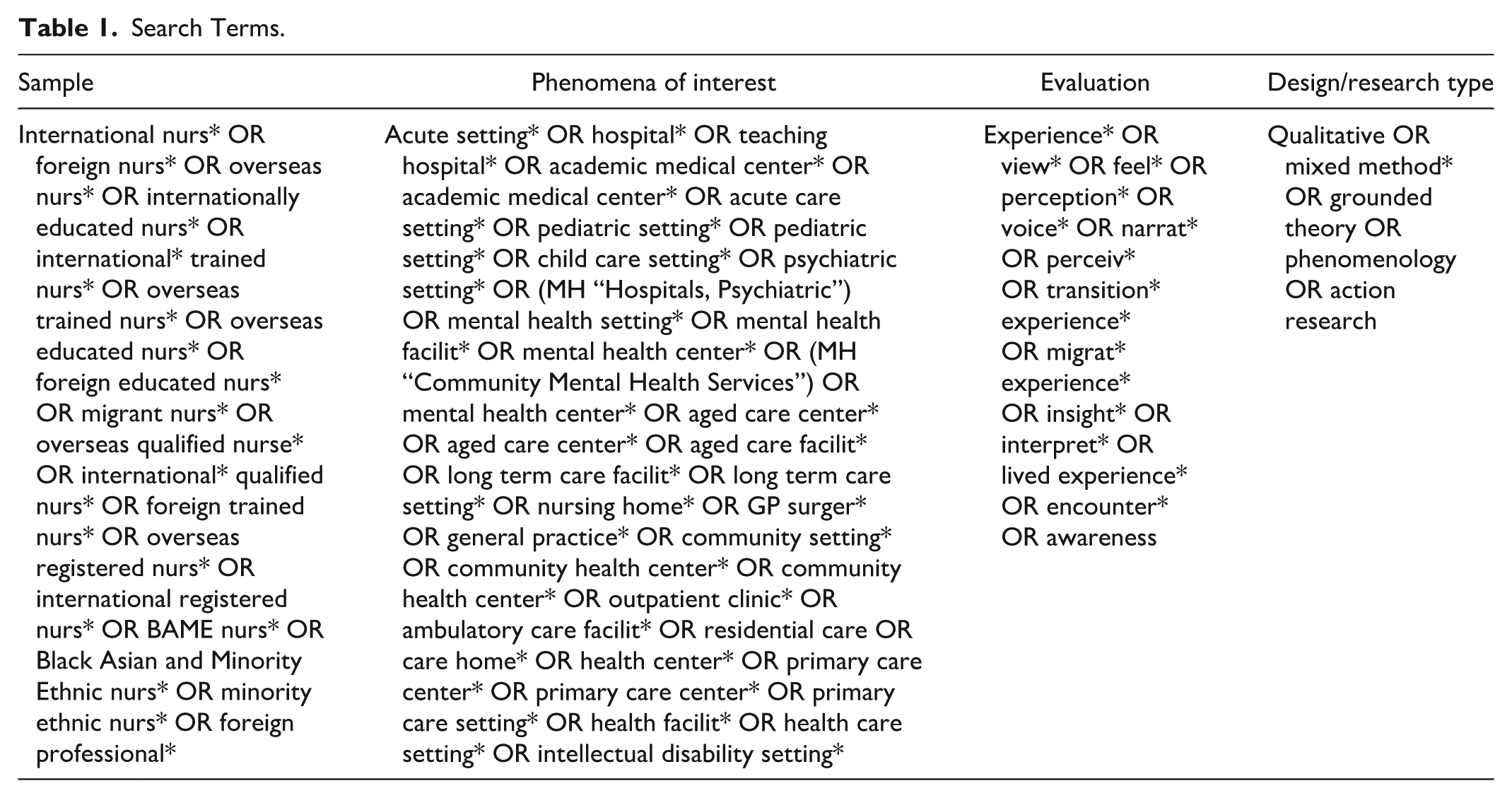
A comprehensive search strategy was conducted, utilizing key search terms and subject headings related to the review’s themes, employing Boolean operators “OR” and “AND” to expand and narrow the search scope. Medical Literature Analysis and Retrieval System Online (MEDLINE), Excerpta Medica Database (Embase), Cumulative Index to Nursing and Allied Health Literature (CINAHL), and Web of Science Core Collection (incorporating the Social Science Citation Index) were systematically searched to identify primary research studies. Language criteria were not applied to search the database to identify potentially eligible non-English publications; however, only English-language studies were included. All database records were downloaded into Zotero, a reference management tool. The relevant studies were uploaded to Covidence (www.covidence.org) for screening, selection, and removal of duplicates.
Inclusion Criteria
The review also used the SPIDER acronym to define the criteria for study inclusion (Cooke et al., 2012). This review included studies focusing on internationally trained BAME nurses working in Western health care contexts, including the United States, the United Kingdom, Canada, Australia, New Zealand, and countries in Western Europe. These nurses often encounter similar challenges related to professional integration, cultural adaptation, and practice within host health care systems. The review aimed to explore the personal and professional experiences of internationally trained BAME nurses, with particular attention to how they navigate their roles in unfamiliar health care environments. Qualitative research designs were considered eligible for inclusion. In addition, qualitative data derived from mixed-methods studies were assessed for relevance and richness. Survey studies containing open-ended responses were also included, where the qualitative data demonstrated sufficient depth to offer meaningful insight into participants’ experiences. Both published and gray literature were included, provided they presented original qualitative data relevant to the phenomenon of interest.
Study Screening and Selection Process
The retrieved papers were uploaded to Covidence, a screening software. Two reviewers (AAJJ and KC) conducted the initial title and abstract screening based on the inclusion and exclusion criteria. The ineligible studies were removed, and the remaining papers were included for full-text review. Two reviewers (AAJJ and KC) were independently involved in the full-text review, and eligible studies were included. Any conflicts were deliberated over and resolved between the two reviewers. The third reviewer (MD) was involved in achieving consensus.
Quality Assessment
The Critical Appraisal Skills Programme (CASP; 2023) qualitative checklist was used to assess the quality and rigor of the included studies. Two reviewers (AAJJ and KC) independently assessed the quality of the studies and then met to discuss the findings. The discrepancies were discussed and agreed upon after the meeting, and a third reviewer (MD) was involved in resolving any conflicts.
Data Extraction
Two reviewers (AAJJ and KC) independently extracted data using a data extraction form that was specifically developed and agreed upon by the review team. The extracted data were then cross-checked to ensure accuracy and consistency. The following information was extracted from the included studies: author, year of publication, country where the study was conducted, funding details (if provided), information about recruitment, sampling, participant profiles, study settings, study duration and timeframe, data collection process, and data analysis. The discrepancies were discussed and subsequently amended.
Data Synthesis
Thomas and Harden’s (2008) thematic synthesis was employed to synthesize the data. The initial coding was conducted using NVivo 12 (Houghton et al., 2017). Two reviewers, AAJJ and KC, conducted the initial coding and subsequently agreed on the initial codes, discussing any disagreements. Then, the codes were listed in an MS Word document, and the interconnection between the codes was visualized. The codes with similar concepts were assimilated together and developed into descriptive themes. Finally, overarching analytical themes were developed from the descriptive themes. The data synthesis process was reflective and iterative, with reviewers meeting at each stage to discuss and agree on outcomes through honest, open, and transparent discussions.
Results
Search Results
Two hundred ninety-four references were identified from the database and were imported into Covidence, a screening software, and nine additional references from other sources were included for review. Covidence automatically eliminated 95 duplicate references, resulting in 208 studies for initial screening. During the initial title and abstract screening, 144 papers were excluded, and 64 papers were selected for full-text review. Three papers could not be retrieved, and the relevant authors were contacted for the full text, but they did not respond. The remaining 61 papers were then reviewed for their full text. Of these, 23 papers were excluded due to: outcomes not relevant (N=18), inadequate data (N=2), wrong study population (N=1), and non-English publication (N=2). Finally, 38 papers were included in the review. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram (Page et al., 2021) provides a comprehensive overview of the screening and selection process (Figure 1).
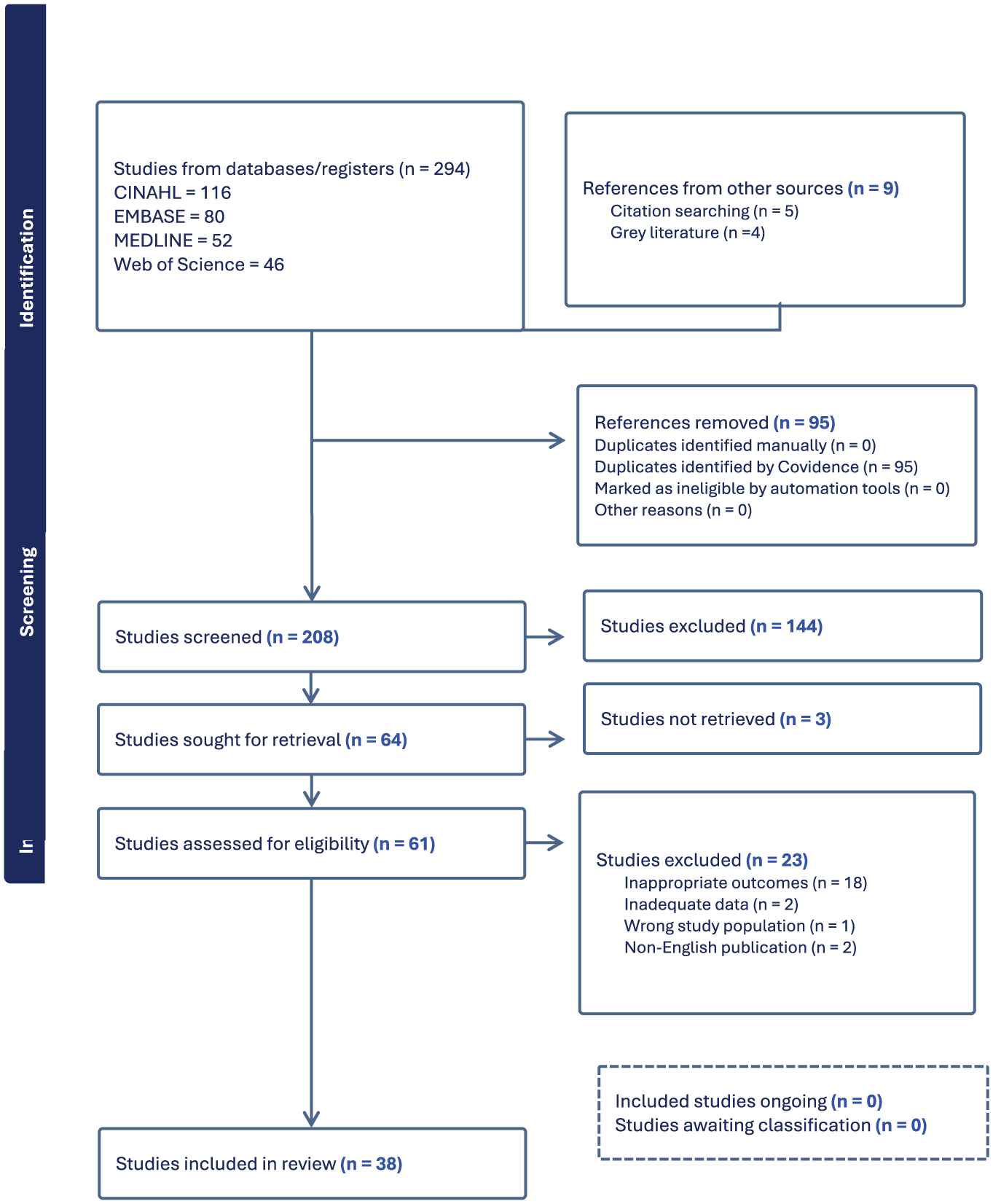
PRISMA Flow Chart of Study Screening and Selection Process.
Quality of the Included Studies
Most of the studies were of good quality and met all the criteria of the CASP checklist (Table 2). In some studies, the relationship between the researcher and participants (reflexivity) was not adequately discussed (Daniel et al., 2001; Deegan & Simkin, 2010; Garside et al., 2023; Ho, 2015; Iheduru-Anderson & Wahi, 2018; Okougha & Tilki, 2010; Philip et al., 2019; C. D. Smith et al., 2011; Wheeler et al., 2014; Withers & Snowball, 2003). Ho (2015) did not describe the research design. However, it appears to be a descriptive design, and Ho (2015) did not elaborate on the ethical process involved in the study for the readers. Regardless of the quality standard, it was decided to include all studies, with the notion that even poor-quality qualitative studies still have the potential to provide essential data that explores relevant phenomena (V. Smith et al., 2022).
Quality of the Included Studies.
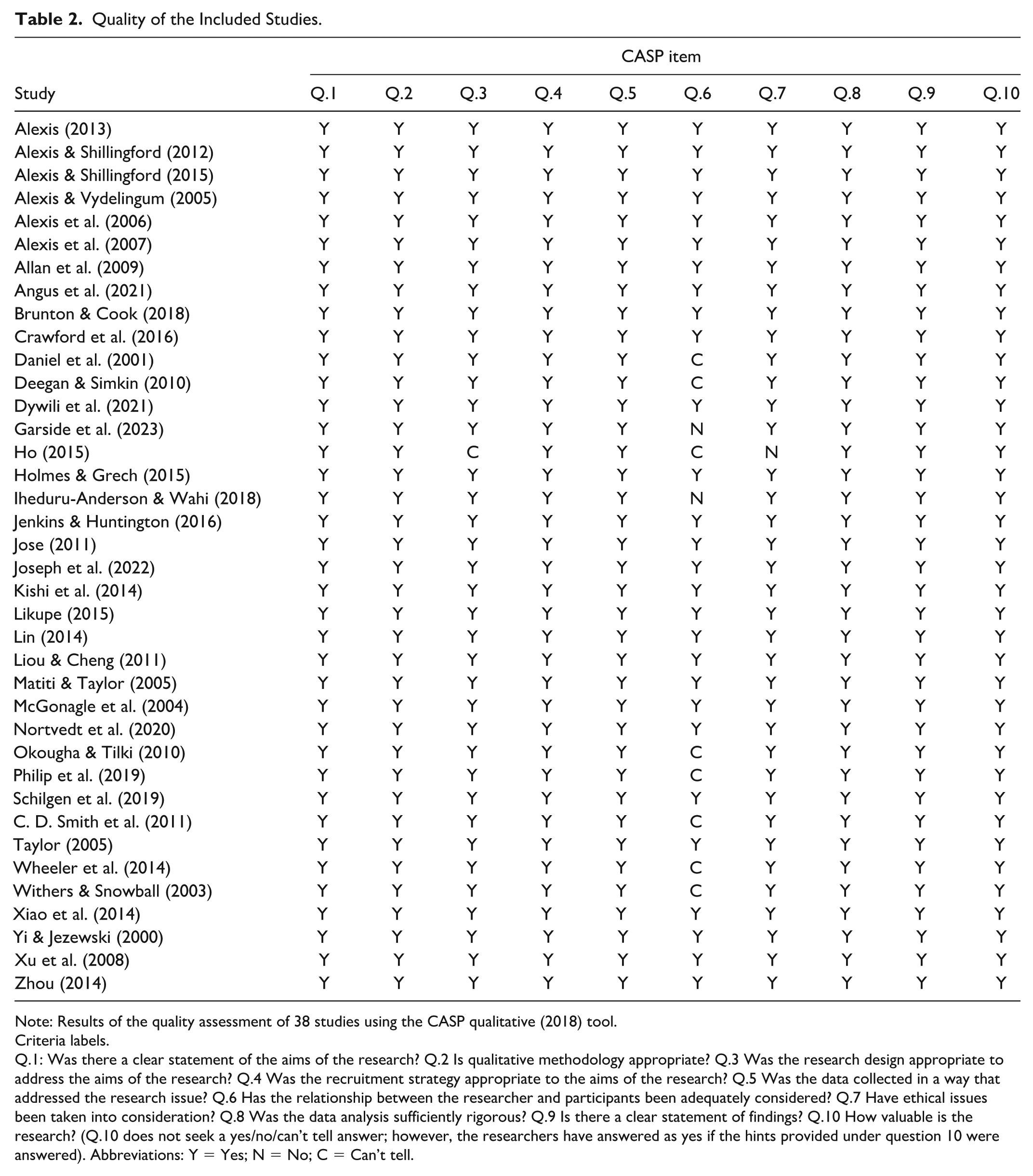
Note: Results of the quality assessment of 38 studies using the CASP qualitative (2018) tool.
Criteria labels.
Q.1: Was there a clear statement of the aims of the research? Q.2 Is qualitative methodology appropriate? Q.3 Was the research design appropriate to address the aims of the research? Q.4 Was the recruitment strategy appropriate to the aims of the research? Q.5 Was the data collected in a way that addressed the research issue? Q.6 Has the relationship between the researcher and participants been adequately considered? Q.7 Have ethical issues been taken into consideration? Q.8 Was the data analysis sufficiently rigorous? Q.9 Is there a clear statement of findings? Q.10 How valuable is the research? (Q.10 does not seek a yes/no/can’t tell answer; however, the researchers have answered as yes if the hints provided under question 10 were answered). Abbreviations: Y = Yes; N = No; C = Can’t tell.
Characteristics of the Included Studies
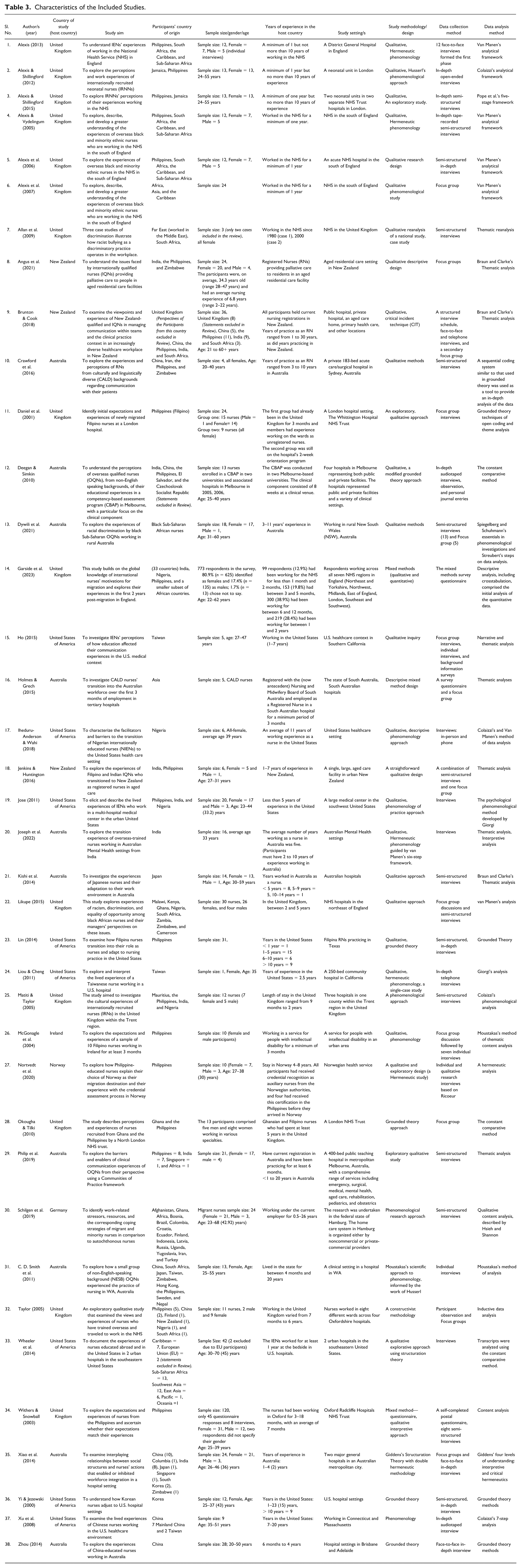
The 38 papers included 1,342 participants, with 773 from a single study (Garside et al., 2023). Participants’ ages ranged from 21 to 70 years, and nursing experience in Western health care settings ranged from 2 weeks (Daniel et al., 2001) to 30 years (Brunton & Cook, 2018). The studies were conducted in the United Kingdom (n = 14), Australia (n = 11), the United States (n = 7), New Zealand (n = 3), Ireland (n = 1), Norway (n = 1), and Germany (n = 1). Settings included acute hospitals (public, national health services, private, urban, and multispecialty), aged residential care, pediatrics, mental health, intellectual disability, community, primary health care, and home care. Most studies used qualitative methodologies, while three employed mixed-methods designs (Garside et al., 2023; Holmes & Grech, 2015; Withers & Snowball, 2003). Study characteristics were provided in Table 3.
Characteristics of the Included Studies.
Themes Identified
In data synthesis, three analytical themes emerged to trace the myriad experiences that internationally trained BAME nurses described: “Initial Adaptation Hurdles,” “Professional Adversities,” and “Strategies for Coping” (Figure 2). The analytical themes describe the experiences of internationally trained BAME nurses during their initial adaptation, including the challenges of adapting to a new culture, communication, and professional relationships, as well as coping strategies in the new environment and aspirations for professional development.
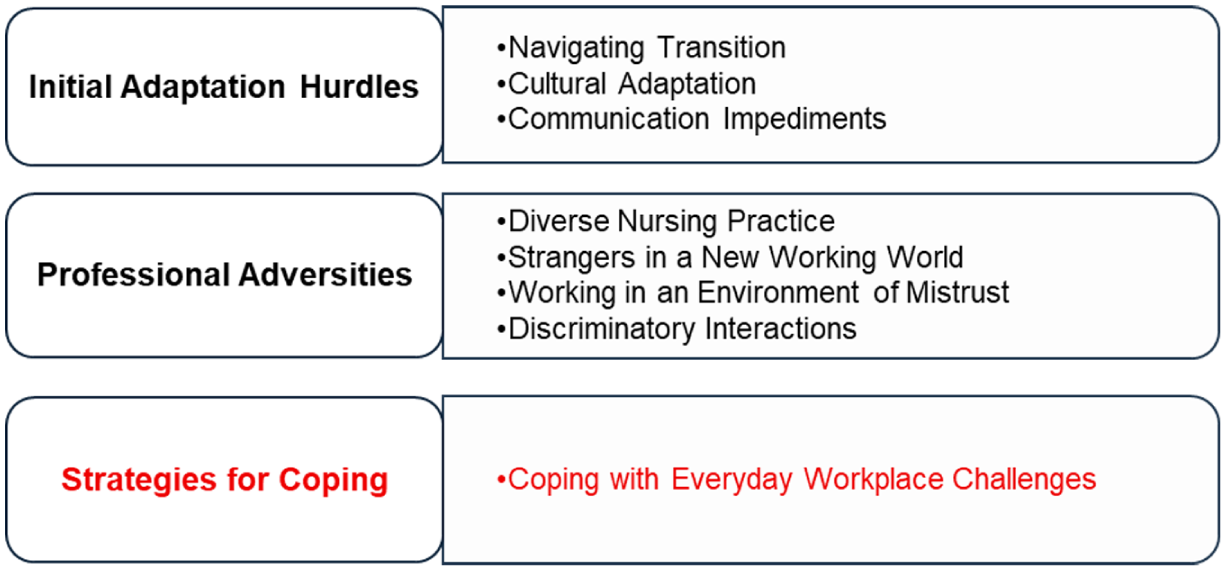
Experiences of Internationally Trained BAME Nurses in Western Health Care Settings.
Initial Adaptation Hurdles
This analytical theme encompassed participants’ transition into the host health care system and country. It included challenges of transition, cultural disparities, adjusting to a new culture, and communication difficulties during the initial stages.
Navigating Transition
Navigating transition was one of the critical aspects of the migration journey of internationally trained BAME nurses as they adapted and integrated into Western health care settings. Their knowledge and skills were often challenged due to their educational background, which was from low- and middle-income countries. Their native colleagues perceived their experiences as less competent compared to those of other international nurses from developed countries (Alexis & Shillingford, 2012):
They felt that because we came from a Third World country, they felt our experience was not up to par or comparable to persons from the UK or Australia or New Zealand. You were being questioned. (Alexis & Shillingford, 2012, p. 1438)
In addition, their unfamiliarity with the guidelines and routines of the new specialist area significantly impacts their initial adaptation. Many internationally trained BAME nurses were not placed in the same specialty areas they had previously worked in their home country (McGonagle et al., 2004; Xiao et al., 2014). While the majority did not express any concern regarding their placement, they desired at least to be consulted and informed in advance:
I didn’t have experience in ICU [Intensive Care Unit] in my home country. It was very traumatic experiences for me in the beginning. I had only 2 supernumerary shifts in the morning before I started my first shift in the afternoon . . . (Xiao et al., 2014, p. 646).
Additional challenges include a lack of awareness and information about hospital policies and procedures (Ho, 2015; Zhou, 2014), as well as the adoption of advanced technology and the acquisition of new skills in Western health care settings (Garside et al., 2023; Lin, 2014; Matiti & Taylor, 2005). Some participants responded to these challenges by withdrawing from social interaction, using isolation as a strategy to cope with the exclusion and marginalization they encountered (Alexis, 2013). In some cases, this coping mechanism resulted in physical and psychological consequences (Holmes & Grech, 2015):
As much as I live in this country I will always feel like an overseas nurse. They don’t allow you to integrate even if you want to. I tend to keep myself to myself because I know that is best for me. I feel like an outcast at times. (Alexis, 2013, p. 965)
Despite these challenges, successful orientation sessions helped international BAME nurses adjust to their new jobs and environment, while shadowing the preceptor in clinical settings was an effective strategy for learning clinical skills and communication (Ho, 2015; Lin, 2014):
I acquired more communication and nursing skills . . . by shadowing a preceptor than attending the classes. (Ho, 2015, p. 223)
Cultural Adaptation
Although internationally trained BAME nurses experienced culture shock due to the diverse cultures in their new workplaces (Jose, 2011; Schilgen et al., 2019), they believed in treating everyone equally and appreciating their uniqueness. Social and cultural factors affected internationally trained BAME nurses’ performance during orientation and transitioning (Jenkins & Huntington, 2016):
. . . part of our challenges is actually not the skills that we have but the culture shock that we go through—that is actually affecting how we perform as well. (Jenkins & Huntington, 2016, p. 15)
Internationally trained BAME nurses were often admonished by their native colleagues, “remember you are in Australia now” (Holmes & Grech, 2015), which they saw as diminishing their prior education and knowledge (Withers & Snowball, 2003). Working partnerships with nurses from their own culture and peer group discussions helped them through early adaptation programs (Garside et al., 2023; Jenkins & Huntington, 2016). Cultural knowledge in induction and orientation programs and talks on acclimating to the new culture benefited internationally trained BAME nurses in adjusting successfully and efficiently to Western health care settings (Matiti & Taylor, 2005). A few internationally trained BAME nurses exhibited diverse reactions when adapting to the host society’s culture while trying to preserve their own, finding it challenging to balance both as they blended into Western society (Joseph et al., 2022; Zhou, 2014):
My cultural beliefs are strong, and I never changed it . . . to me, it is not accepting . . . it is more of understanding the Australian culture. . . At home, we practice Indian culture . . . But I try to maintain a balance between Australian and Indian culture. (Joseph et al., 2022, p. 44)
Communication Impediments
Internationally trained BAME nurses identified that support from their native colleagues was crucial in overcoming communication challenges (Ho, 2015; Liou & Cheng, 2011). Although they had completed their language exams with good grades, they felt less confident with real-life communication in their new workplaces as the native nurses used colloquial words (Angus et al., 2021; Crawford et al., 2016; Okougha & Tilki, 2010; Withers & Snowball, 2003) and spoke fast (Garside et al., 2023; Matiti & Taylor, 2005), making it hard to understand. Moreover, the language utilized in routine clinical practice diverged significantly from the language used during interviews, and employers overestimated their communication capabilities (Ho, 2015):
Our employers may have overestimated international nurses’ oral communication ability during our job interviews, but the interview language is very different from the language we use in clinics. (Ho, 2015, pp. 221–222)
In addition, they struggled to articulate their ideas, resulting in miscommunications and misunderstandings with their colleagues (Allan et al., 2009; Angus et al., 2021). This led to losing confidence and heightened nervousness (Deegan & Simkin, 2010; Liou & Cheng, 2011). Difficulties in interpersonal communication invariably impacted safety and organizational performance, particularly during the early phases of employment, notably in telephone interactions with physicians (Brunton & Cook, 2018; Ho, 2015; Matiti & Taylor, 2005; Yi & Jezewski, 2000):
I had great fear in communicating by the telephone. I panicked when I talked into the phone. So sometimes I ran to the bathroom when the bell rings. (Yi & Jezewski, 2000, p. 725)
However, they overcame communication difficulties by rising above the challenges with perseverance, a willingness to learn, and developing support networks (Jose, 2011). They worked hard to improve their communication abilities and learn new words and slang by “making a note of words and Googling them” (Brunton & Cook, 2018; Ho, 2015). Some even selected colleagues who comprehensively understood their intercultural communication needs and enabled them to learn and understand the local language and culture (Philip et al., 2019):
My colleagues tried teaching me slangs . . . they used to say, you are an Aussie and you are a Sheila. . . . I used to say, no no I am not Sheila my name is Mary. Later they told me that Sheila in Australia is for woman and bloke is for a man. Yes . . . that is what they did to me but I thought that was very good to get to know the local language and culture. (Philip et al., 2019, p. 92).
Professional Adversities
This analytical theme encompasses four subthemes: “Diverse Nursing Practice,” “Strangers in a New Working World,” “Working in an Environment of Mistrust,” and “Discriminatory Interactions.” Professional adversities referred to the challenges international BAME nurses faced in adapting to unfamiliar clinical practices, negotiating new workplace cultures, and experiencing exclusion and discrimination within professional settings.
Diverse Nursing Practice
Internationally trained BAME nurses expressed that the concept of “caring” was the same across cultures, where the focus of care was always the patient (Brunton & Cook, 2018; Daniel et al., 2001; C. D. Smith et al., 2011). Despite similarities in nursing principles between countries, some encountered differences in practice, such as the concept of 24-hour care, which allows tasks to be passed to the next shift (Daniel et al., 2001). Few felt uncomfortable leaving tasks unfinished, even avoiding breaks, which conflicted with native nurses who accepted task handovers as long as patient care was maintained (Withers & Snowball, 2003):
Another thing that puzzled me is that we shouldn’t worry if we cannot finish some of our responsibilities in our shift because we can just endorse it to the next shift. (Daniel et al., 2001, p. 261)
Nurses were valued for their patient advocacy, patient-oriented attitude, evidence-based practices, and their ability to be listened to by doctors (Withers & Snowball, 2003). These experiences contrasted with their home countries, where doctors made all decisions and were regarded as Akin to Gods (Taylor, 2005; Withers & Snowball, 2003). Thus, independent decision-making was initially scary, making them apprehensive about identifying patients’ problems and determining whom to contact (Jenkins & Huntington, 2016; Zhou, 2014):
Way back in the Philippines. . . maybe you can practice more of your clinical skills, where in here, it’s much of your decision skills that’s being practiced. (Jenkins & Huntington, 2016, p. 16)
In addition, they often found themselves in specialized areas where they lacked expertise upon arrival in Western health care. They could not utilize their nursing skills and felt as though they were losing them (Jenkins & Huntington, 2016). They were stressed by simple hygienic tasks that are usually done by family or nursing assistants in their own countries (Lin, 2014; Withers & Snowball, 2003; Xiao et al., 2014; Xu et al., 2008; Zhou, 2014):
. . . We do not do showering or feeding. Their relatives do or they hire own personal carer to do those for them. Assisting patients’ ADLs [activities of daily living] was a new learning curve for me in the very beginning here. (Xiao et al., 2014, p. 647)
Another challenging area was the practices contradicting their religious beliefs and social customs (Angus et al., 2021). In BAME societies, a patient’s life is prolonged as much as possible, and a dying patient would be cared for at home by family members, as the family would like to spend time with them till their last moment (Angus et al., 2021). For them, withdrawal of active treatment was like abandoning the patients. Another unfamiliar concept for them was the legal consequences of nursing practice in Western health care settings (Lin, 2014). In their home countries, nurses were rarely involved in medical lawsuits. Therefore, they acknowledged that they had to be mindful of the legal aspects of nursing practice, especially nursing documentation, to protect their nursing license in the host country (Lin, 2014):
other than patient safety first, you have to protect your license too because that’s the only thing that holds you here. So, in every step you make, you have to be careful, document everything! (Lin, 2014, p. 685)
Strangers in a New Working World
Internationally trained BAME nurses felt that the nursing system in Western health care settings was much more humane than in their home countries and that the human rights of nurses were respected and safeguarded (Liou & Cheng, 2011). Support for career progression was another positive factor for internationally trained BAME nurses (Garside et al., 2023). Hard work, language skills, and personal capabilities of internationally trained BAME nurses were identified as factors for professional and career development (Alexis & Shillingford, 2015; Zhou, 2014):
The greatest difference in working here is that patients have their human rights, and we nurses have ours. (Liou & Cheng, 2011, p. 107)
Despite the positive experiences in the workplace, they also encountered negative ones. Heavy workloads, staff shortages, and low nurse-to-patient ratios resulted in considerable physical and psychological stress (Alexis, 2013; Alexis & Shillingford, 2012; Schilgen et al., 2019). In addition, a lack of support from senior staff and managers added to the pressures they faced in their new roles, which hindered their ability to provide the best possible care to their patients (Alexis, 2013; Alexis & Shillingford, 2012; Schilgen et al., 2019). Moreover, their colleagues also made them feel inadequate despite their correct actions; these things upset them, but they learned to get used to it (Alexis & Vydelingum, 2005):
I had informed him (doctor) earlier that there were discrepancies in the fluid management of the patient but he did not bother to check, only to realise that the patient was acutely ill. . . . Although I had already drawn this to the doctor’s attention, and he refused to see the patient, this senior nurse did not want to know. She made me feel so inadequate. I am very upset now thinking about it but you just tend to get used to it. (Alexis & Vydelingum, 2005, p. 466)
Nevertheless, beyond these professional pressures, some internationally trained BAME nurses reported feeling unwelcome and unaccepted by certain colleagues, as they were perceived as not knowledgeable enough to be part of the team (Philip et al., 2019). Sometimes, they felt like aliens and were not adequately informed of what to expect in the new working environment (Alexis & Shillingford, 2012; Daniel et al., 2001), creating a hostile work environment, experienced bullying (Iheduru-Anderson & Wahi, 2018), and felt intimidated and excluded (Lin, 2014). This hostile environment led them to seek new workplaces where they could feel accepted and form friendships (Alexis, 2013; Angus et al., 2021), and they attributed this treatment to their ethnicity (Iheduru-Anderson & Wahi, 2018):
The nurses I worked with there were horrible. They were insensitive, they acted like they did not want me there. . . . They gang up on me and they were always reporting me to the manager for no apparent reason. . . . Overall, it was a hostile environment. (Iheduru-Anderson & Wahi, 2018, p. 606)
In contrast to these negative experiences, many BAME nurses also recounted moments of genuine support and acceptance. In general, they felt welcomed and accepted by their native colleagues in their new work environment (Alexis & Vydelingum, 2005), which increased their confidence (Alexis & Shillingford, 2012; Daniel et al., 2001; Kishi et al., 2014; Taylor, 2005). In addition, collaborating with knowledgeable and experienced preceptors who provided support and explanations of the work routines, nursing skills, and medical equipment was identified as crucial to acquiring knowledge specific to their new work environment (Ho, 2015):
Observing the preceptor and being supported by an experienced nurse has helped me a lot. It made me feel secure when I was a novice in a completely strange work environment. (Ho, 2015, p. 224)
Working in an Environment of Mistrust
Internationally trained BAME nurses faced a lack of trust from native and senior colleagues, often feeling watched without being provided with guidance or support (Alexis & Shillingford, 2012; Holmes & Grech, 2015), and some even stated they felt like a “specimen under observation” (Daniel et al., 2001; Holmes & Grech, 2015). They felt targeted by native colleagues despite their best efforts (Allan et al., 2009; Dywili et al., 2021; Likupe, 2015). Since they were constantly monitored, they experienced declining confidence, felt powerless, and could not meet workplace standards (Alexis et al., 2007). They also expected a shift in attitude from being fault-finding and labeled incompetent to receiving constructive and supportive feedback when mistakes occurred (Jose, 2011). This led to a sense of defeat, with some contemplating returning to their home country (Alexis et al., 2007; Allan et al., 2009):
I said I don’t know why you always pick on me because I am only human! I tried my best and I know I am capable of doing what I am supposed to do. I then received a letter saying I had to go. (Allan et al., 2009, p. 903)
In addition, they reported being deliberately undermined, with some colleagues fabricating lies about their actions to create grounds for complaints against them (Allan et al., 2009). During their job transition, many felt treated like students rather than qualified nurses (Alexis & Shillingford, 2012; Taylor, 2005). They felt like they were “going back to square one” without autonomy or the chance to practice the skills they had mastered in their home countries (Alexis & Shillingford, 2012):
It was a bit frustrating to start with. There was even a point that we really wanted to quit. You can’t really suggest because they will tell you forget about your past experience, this is a different place, this is UK. I mean it was quite frustrating because they don’t give you the independence that you are used to. You don’t have the liberty to do most of the stuff that you were doing back home, but to be treated like students. (Alexis & Shillingford, 2012, pp. 1438–1439)
As a result, internationally trained BAME nurses had to work hard to prove themselves to gain recognition in their workplace (Alexis & Shillingford, 2012; Alexis & Vydelingum, 2005; Brunton & Cook, 2018; Taylor, 2005; Xu et al., 2008). Furthermore, to establish their competence as nurses in the eyes of their patients and other multidisciplinary team members, they were required to put in additional effort (Alexis, 2013; Jose, 2011; Wheeler et al., 2014), thus proving that they had come to assist and work alongside their native counterparts and that they could compete to do so (Jenkins & Huntington, 2016):
This brings down my confidence. . . when co-workers question our capabilities for the reason that we are foreign nurses. (Brunton & Cook, 2018, p. 22)
Internationally trained BAME nurses attempted to “find their own identity in professional practice” and cope with their new work environment (Deegan & Simkin, 2010). They preferred to better themselves clinically and engage in conversations with their managers to ensure they were not making any mistakes. Even if they did, they sought to avoid these in the future (Schilgen et al., 2019). In addition to supporting their families financially and exploring the host country, one reason for migrating to Western health care settings was the opportunity to advance personally and professionally by expanding their roles as specialist nurses (Alexis & Shillingford, 2015; Iheduru-Anderson & Wahi, 2018):
I like the specialties here because, you specialise in one thing, this is your area and you know it well. That’s better than being everywhere. I prefer the specialties. (Iheduru-Anderson & Wahi, 2018, p. 607)
Discriminatory Interactions
Internationally trained BAME nurses faced unequal opportunities and a lack of support for career progression and further education, as they were frequently denied advancement despite having the necessary experience and expertise (Alexis et al., 2006; Alexis et al., 2007; Dywili et al., 2021; Likupe, 2015). Instead, these opportunities were often granted to native junior nurses, a practice attributed to ethnicity and skin color (Alexis et al., 2006; Iheduru-Anderson & Wahi, 2018; Likupe, 2015; Wheeler et al., 2014; Zhou, 2014). Although equal opportunity policies existed, they were poorly implemented, and many managers showed reluctance to promote or trust internationally trained BAME nurses in leadership roles (Allan et al., 2009; Dywili et al., 2021). Preferential access to professional courses for native nurses further deepened these disparities (Alexis & Vydelingum, 2005). Regardless of doing the same job as their white colleagues, they were treated as second-class citizens (Alexis et al., 2006; Dywili et al., 2021), and their native counterparts progressed to higher grades faster than them (Alexis et al., 2006, 2007; Philip et al., 2019):
This particular hospital will give you a lot of reasons why they are not going to promote you and I think this is unfair. Other staff will be recruited from outside and they will be promoted very quickly. (Alexis et al., 2007, p. 2225)
Discrimination also extended to daily work practices, including biased patient assignments and unjust criticism when patient outcomes deteriorated (Alexis & Shillingford, 2012; Wheeler et al., 2014). Many internationally trained BAME nurses felt disrespected, silenced, and hesitant to challenge discriminatory behaviors (Brunton & Cook, 2018; Philip et al., 2019), though some reported such incidents to higher authorities (Joseph et al., 2022; Wheeler et al., 2014). They also experienced prejudice from patients and families, who questioned their competence, qualifications, and language abilities based on skin color and accent (Dywili et al., 2021; Wheeler et al., 2014). Some families even rejected their care or bypassed them to interact with native staff (Dywili et al., 2021; Schilgen et al., 2019; Wheeler et al., 2014):
I think the most challenging. . . part is dealing with the family. Yeah, because it’s not just the patient that you’re looking after, but it’s the family as well. . . I think some of them find it hard that their relatives are going into aged care, and sometimes they can’t cope. So sometimes it’s quite hard to deal with them. With the residents—it’s fine. . . (Jenkins & Huntington, 2016, p. 16)
Despite these challenges, many nurses maintained professionalism, sought direct patient dialogue, or focused on personal migration goals (Philip et al., 2019; Schilgen et al., 2019). Notably, some patients expressed deep appreciation (Philip et al., 2019; Schilgen et al., 2019; Wheeler et al., 2014), acknowledging that these nurses played a vital role in sustaining the health care system (Alexis, 2013):
I was so happy that this patient appreciated all the help I gave. She also said that if it was not for people like me, the NHS would not be able to function. ..... To be honest I do not need my manager to give me credit because I know it would not come but at least my patients are appreciative. (Alexis, 2013, p. 965)
Strategies for Coping
While experiences of racial prejudice and discrimination were common, participants also described how they navigated and responded to these challenges. However, most of them developed strategies to deal with these challenges in their new work environment. Some chose to be resilient through positive coping mechanisms and focusing on personal and professional development (Angus et al., 2021; Joseph et al., 2022):
I had to cope with racism many times from patients but at least they are unwell . . . but I had a particular staff challenging me negatively on many occasions . . . I am a resilient person. I intervened. (Joseph et al., 2022, p. 45)
They also learned to adjust to the situations and kept a low profile when they felt their colleagues had unjustly scrutinized them (Holmes & Grech, 2015). Some empowered themselves by learning the system despite their odds through hard work and determination, thus enabling them to support the new nurses who come to work in Western health care settings (Iheduru-Anderson & Wahi, 2018):
I will tell other Nigerian nurses the same thing, you will get used to it, just don’t let it bother you, don’t let them break you. It is just a phase, we all go through. (Iheduru-Anderson & Wahi, 2018, p. 607)
Internationally trained BAME nurses employed various strategies to adapt to the new work environment, including recognizing their self-worth (Lin, 2014), contributing and adapting to the new working environment, resorting to spirituality, seeking support from other minority or ethnic colleagues, and utilizing available resources to overcome their everyday stressors (Alexis, 2013; Lin, 2014; Wheeler et al., 2014). Moreover, despite the challenges, some internationally trained BAME nurses maintained a strong sense of identity and recognized the value of their culture, skills, education, and experience, as well as what they could contribute to their host country (Philip et al., 2019). At the same time, they also held clear expectations of the opportunities the host country could offer them (Philip et al., 2019). Some embraced these differences in nursing practices by being open-minded, which increased their ability to adapt to new work settings (Lin, 2014; Philip et al., 2019):
Just like everything else, you master. It’s not something that I needed to be recognised [for]. I need to recognise myself that I can do the job. (Lin, 2014, p. 686)
Instead of succumbing to self-pity, several nurses were open-minded and vocal about their challenges, which helped them resolve workplace issues (Dywili et al., 2021). They demonstrated their strengths and ability to perform tasks, adopting new cultural and communication patterns, using local colloquialisms in their talks, and learning the language and regional accents (Nortvedt et al., 2020; Philip et al., 2019). Some used positive entertainment as a means to cope with their problems (Alexis & Shillingford, 2012):
I try to overcome the difficulties by being open-minded, at the same time being vocal, telling them what you feel, so they know, so they could do something about it. (Alexis & Shillingford, 2012, p. 1439)
In addition to the self-coping mechanisms, internationally trained BAME nurses sought help and support from their family, friends, and other BAME colleagues (Alexis & Shillingford, 2012). Some individuals discussed work-related problems with their families before addressing them with their managers (Schilgen et al., 2019). Collaborating with and supporting other minority and ethnic colleagues who began working with them in Western health care settings helped them to cope with their challenges (Alexis, 2013). Some felt comfortable and supported by non-BAME ITNs who shared many commonalities (Schilgen et al., 2019):
I was not alone and we stuck together. I think that was what made the difference. If I had come alone and just in this environment, I don’t think I would have stayed. (Alexis & Shillingford, 2012, p. 1439)
Discussion
This review identified that better working conditions in Western health care settings are a primary motivation factor for migration (Roth et al., 2021). During and after the transition, many of these nurses experienced challenges due to differences in the nursing practices of their host countries (Rajpoot et al., 2024). Therefore, it is imperative that experienced nurses provide clinical orientation and mentoring to facilitate the development of competence and the familiarization with the new working environment (Goh & Lopez, 2016; Kamau et al., 2023). Many internationally trained BAME nurses felt that coming from low- and middle-income countries undermined their training, experience, and skills, compelling them to prove themselves (Kamau et al., 2023). Moreover, recognizing their competencies and assigning roles aligned with their expertise could help mitigate feelings of deskilling and enhance their sense of value (Kamau et al., 2023; Pressley et al., 2022). While extended orientation has recognized benefits, its impact is maximized when embedded within comprehensive transition-to-practice models (Bell et al., 2025; Ernawaty et al., 2024; Kamau et al., 2022). These models typically integrate structured onboarding with incremental skill development, formalized mentorship or preceptorship supported by mentor training, and targeted linguistic and cultural interventions (Gularte-Rinaldo et al., 2023; Lambert et al., 2024).
Real-life communication is identified as a challenge despite all the English language tests they undergo (Bayuo et al., 2023). Besides, language-related challenges can lead to misinterpretations and misunderstandings at work and affect employees’ performances (Fiset et al., 2024), impacting patient and organizational safety. Employers in Western health care settings must make accommodations to facilitate and improve orientation experiences by incorporating standard abbreviations used in practice, implementing assertiveness training, and transcribing orders and medications to create a culture of patient safety (Moyce et al., 2016).
A deeper understanding of internationally trained BAME nurses’ cultural values, beliefs, and practices is needed to promote cultural pluralism in a diverse health care setting (Balante et al., 2021). When they migrate to a foreign country, they lose their familiar social environment and enter a new culture where many familial cues are removed (Pressley et al., 2022; Skaria et al., 2019), leading to transition shock and causing psychological discomfort. Internationally trained BAME nurses learn to balance the two cultures by embracing the new cultural and nursing practices and reflecting on and preserving their heritage and nursing identities (Al-Hamdan et al., 2015), especially around death and dying, Western family functioning, and the family’s role in caring for their loved ones. Therefore, cultivating cultural competency in a culturally diverse workplace (Alostaz & Chen, 2024; Ong-Flaherty, 2015) and providing culturally sensitive training (Rajpoot et al., 2024) and culturally sensitive clinical mentorship support (Goh & Lopez, 2016) is essential to successfully integrating these nurses into the new environment (Al-Btoush & El-Bcheraoui, 2024; Ramji et al., 2019).
Improving interpersonal interactions in clinical environments is the most important factor in creating a sense of belongingness (Fattahi-Bafghi & Barkhordari-Sharifabad, 2022). Buddying with other internationally trained BAME nurses of the same cultural background, especially during early transition, helps promote a sense of belongingness (Villamin et al., 2025), which in turn enables them to overcome challenges such as isolation and interpersonal conflicts (Dahl et al., 2022; Safari et al., 2022). Racial discrimination and prejudices from work colleagues, family members, and patients have emerged as a significant challenge experienced by internationally trained BAME nurses (Kmietowicz, 2024). The experience of open racial discrimination and preferential treatment in the workplace undermines self-confidence and professional efficacy and affects their physical, psychological, and professional well-being (Abrahim et al., 2025; Iheduru-Anderson, 2020a; Iheduru-Anderson et al., 2021; J. Li et al., 2021).
The equitable treatment of internationally trained BAME nurses and support for career progression and professional development are vital for job satisfaction and retention within the nursing workforce and are essential for the overall performance and quality of patient care in an organization (Humphries et al., 2015; Roth et al., 2021; Sasso et al., 2019; Walani, 2015). Hence, health care organizations’ commitment to Equality, Diversity, and Inclusion (EDI) (Al-Btoush & El-Bcheraoui, 2024) and adherence to equal opportunities policy and guidelines, providing fair opportunities for internationally trained BAME nurses alongside native nurses, enhances staff engagement and morale (Iheduru-Anderson, 2020b).
Resilience enables them to adapt to adversity, maintain emotional stability, engage in self-care, have better job performance, and enhance personal growth and well-being (Dahl et al., 2022; Kim & Chang, 2022; Ungar, 2014). Health care organizations, managers, and native nurses should be cognizant of the factors that foster and impede the resilience of these nurses so that they can provide supportive coping strategies, and a supportive work environment is crucial for internationally trained BAME nurses to develop resilience (Dahl et al., 2022). In addition, cultural networks, family and community support, and a supportive working environment are almost as important as individual coping strategies to overcome challenges in the new work environment and successful retention of these nurses (Dahl et al., 2022; Skaria et al., 2019).
Implications for Research
The findings from this review may help health care providers develop appropriate support systems to facilitate internationally trained BAME nurses’ successful transition and progression by addressing their diverse needs. Most studies in this review have focused on the initial transition and integration experiences of internationally trained BAME nurses, highlighting the need for further research beyond this early period. It would be valuable to investigate whether the experience of racism and discrimination stems from their minority status in the Western workforce or is directly associated with their ethnic backgrounds.
Strengths and Limitations
A key strength of this review is that it synthesizes findings from 38 qualitative studies on the experiences of internationally trained BAME nurses working in various Western health care settings, enhancing the validity of the findings and highlighting this issue as a global phenomenon. In addition, by not restricting the search by publication date, the review captures a comprehensive range of insights, reflecting both historical and recent perspectives on the experiences of these nurses. However, the included studies employed various qualitative research methodologies and theoretical approaches, which influenced the interpretation and comparison of the findings. Moreover, the review focused solely on the qualitative studies and the qualitative data from the mixed-methods studies on the experiences of internationally trained BAME nurses, potentially overlooking data from quantitative studies. While a few studies focused on specific ethnic groups, most included mixed cohorts representing a broad range of BAME backgrounds. This approach can limit understanding of the unique experiences of individual ethnic groups, reducing the ability to infer findings for any one group. Each ethnic group may face distinct experiences due to variations in cultural norms and nursing practices.
Conclusion
The review highlights that internationally trained BAME nurses who are employed in Western health care settings face a wider array of challenges than their native counterparts. Western health care settings must acknowledge the issues and challenges being faced by internationally trained BAME nurses while assimilating and working in Western nursing environments, and implement strategies to cultivate resilience in these nurses. Establishing an inclusive workplace environment and encouraging interpersonal relationships helps develop a sense of belongingness. Health care organizations and management commitment to maintain ongoing vigilance on workplace racial discrimination, compliance with equal opportunities policy and guidelines, equality of career and professional development opportunities for internationally trained BAME nurses would lead to favorable workplace experiences as well as quality patient care provision, positive staff morale, staff retention, and increased patient safety outcomes and organizational productivity.
Supplemental Material
sj-docx-1-tcn-10.1177_10436596251398994 – Supplemental material for Experiences of Internationally Trained Black, Asian, and Minority Ethnic Nurses Working in Western Health Care Settings: A Qualitative Evidence Synthesis
Supplemental material, sj-docx-1-tcn-10.1177_10436596251398994 for Experiences of Internationally Trained Black, Asian, and Minority Ethnic Nurses Working in Western Health Care Settings: A Qualitative Evidence Synthesis by Anto Ajithpaul Joseph Jayasundar, Mel Duffy and Kumaresan Cithambaram in Journal of Transcultural Nursing
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article:
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
