Abstract
Objectives
Mental health (MH) patients seen in the emergency department (ED) setting are often viewed in isolation, outside of the context of their loved ones, the next of kin (NOK). This is especially problematic when a patient is detained under the mental health act. This project aimed to improve this engagement.
Methods
A sense of urgency was created from a guiding coalition of the local MH and ED executive of a rural hospital. The vision was communicated to the team for action. This was then institutionally incorporated as best practice during a 3 month trial.
Results
NOK were engaged more frequently as a result of this quality improvement strategy, rising to 90.8% (2021) from 63.2% (2020) compared to the previous year χ2 (1, N=166) =18.75, p = .000015. Admissions for all MH patients from the emergency department fell to 28.3% (2021) from 39% (2020) χ2 (1, N=652) =8.32, p = .0039.
Conclusions
Working with NOK is a best practice strategy that was embraced by clinicians when highlighted. This resulted in less restrictive practice and more community treatment. Creating a frame for the patient that is standardised, provides containment and co-designs future health care is beneficial.
In 2021 the health district received feedback from family members. Their relatives had been seen in the emergency department (ED) and the focus was a mental health (MH) problem. Relatives felt excluded from the process of providing care for their loved one who was then discharged from the ED. There was also the suggestion, that critical subsequent events could have been avoided if they had been engaged in care. Patients who are unable, or unwilling, to identify any supports at a critical time are potentially isolated. They may also be regressed in their psychological defences, prompting concern.
In contrast, quality improvement activities had identified that 97.3% of all MH inpatients could identify a next of kin (NOK), when asked, and this person was able to meaningfully contribute to the discharge process. 1
The patient group of most concern in the ED were those detained under the Mental Health Act NSW 2007 (MHA). 2 In a 3 month period in 2020, 34.3% (114 of 332) of MH patients presented under the Mental Health Act Victoria 2014 to an ED in Melbourne. 3 Not all MH patients seen in the ED for assessment are admitted; discharge home is the most common occurrence, followed by admission for MH care and less commonly a medical admission. 3
Relevant provisions of the mental health act NSW 2007 2

The team noted the pressures on the service and the local resources. It takes more time to work with others. Yet also noted were the benefits to patients.
The specific purpose of this project was to work with ED patients who were under the MHA and engage their NOK in the process of discharge planning.
Methods
Between July 2018 and June 2019 there were 11,254 urgent and 15,338 semi-urgent presentations to this rural hospital emergency department. 7
Strategy to engage next of kin

The vision was to increase the NOK participation rate for MHA patients who subsequently left the ED in the 3 months from July 2021. The patients presenting voluntarily were not a target group. However, clinicians were encouraged to use their discretion to engage next of kin in this group too.
A retrospective audit was undertaken to clarify if the 2021 intervention had been successful. All people seen under the MHA between the 3-month periods of July to September 2020 and July to September 2021 were compared. Chi-square (χ2) analysis was used to evaluate the change across the two periods. Admission rates of MH patients to Dubbo hospital for these periods were also evaluated to determine the potential impact of NOK engagement (as the impact of the WANTED project may generalise to all patients) with Chi-square (χ2) analysis. Qualitative rounding was undertaken with 12 key clinicians (across disciplines and departments). This focussed on identifying what had been successful in the project and what could be improved. Questions were also asked about the need for any additional resources.
Results
Next of kin (NOK) Consulted for patients in the Emergency Department (ED) who presented under the mental health act (MHA)
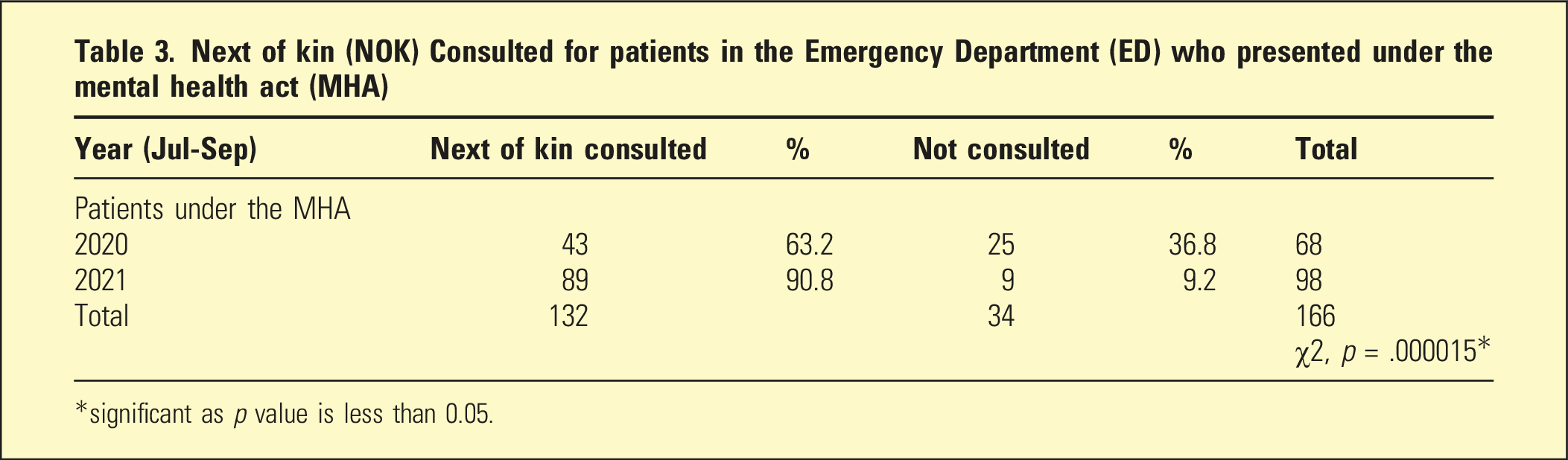
*significant as p value is less than 0.05.
Total mental health patients admitted to Dubbo Hospital from the emergency department (ED)
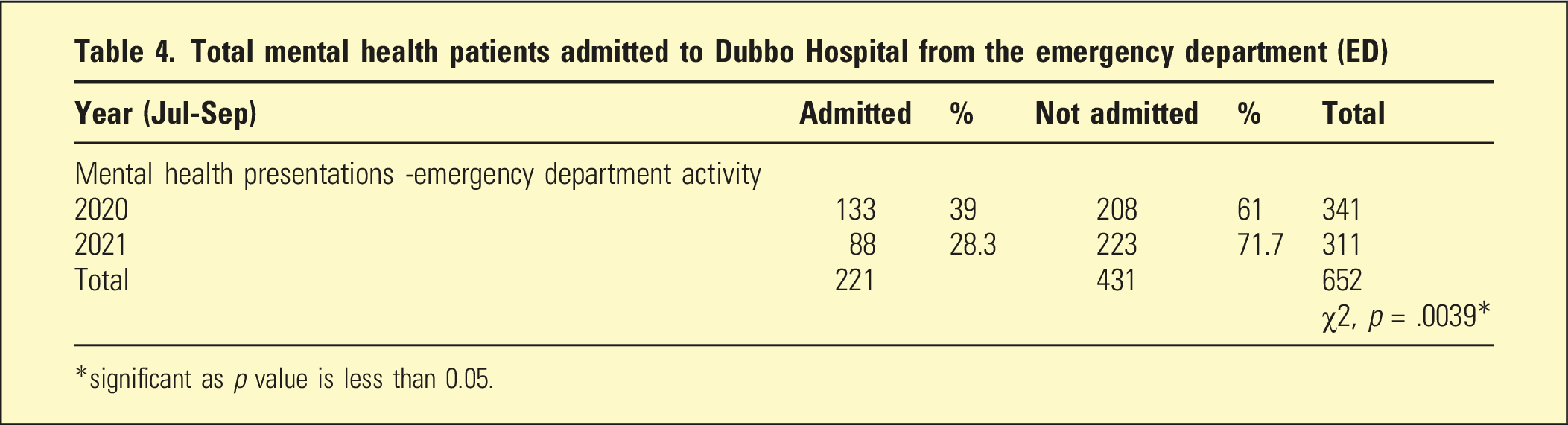
*significant as p value is less than 0.05.
Four key qualitative themes were noted on rounding with the clinicians engaged in this project in the ED. Engaging NOK should generally be attempted for all MH patients in the ED, not just patients under the MHA. Secondly, this was a clear gap that had been addressed by a framework via this project. The third key response was that there had been a change in culture, that this was the new norm. Finally that NOK were seen as allies. Importantly, there was no negative feedback.
Discussion
Transformation efforts may fail because there is not a sense of urgency, a guiding coalition (the local MH and ED executive) and a vision that is then communicated with others (the clinicians), who can then act on that vision to institutionally incorporate. 8 This was the goal and frame of this quality improvement activity.
A case for consideration

Beliefs that it may be more effort to engage NOK were addressed amid the clinician group. Dissatisfaction of both patients and their NOK cluster around the main theme of interpersonal dissatisfaction, rather than disappointment in the competency of clinicians. 9 This may be due to limited opportunities for meaningful engagement or poorly framed expectations. In contrast, working with patients, as well as their loved ones, is now considered an integral part of both high quality care and improved patient safety across the spectrum of medical care. 10 Patient engagement is known to enhance care, service delivery and governance. 11 The project results are consistent with an emerging literature of inclusion of patients, their families and a co-design approach in health care.
Most importantly, in this project the co-design of present and future care plans with the patient themselves was key. Of doing with and not doing to, or for. 12 Clinicians communicated with the patient that a safe plan for discharge, into the care of someone they identified, who potentially loved them, was expected as best practice health care.
Limitations
Feedback was not collated from the patient and next of kin group and this is a limitation, but also a future opportunity. The authors also noted the lower number of MH presentations under the MHA in 2020 versus 2021 and hypothesised major social and behavioural changes including lockdowns and outbreaks, amid SARS-CoV-2. 13
Conclusion
The concept of always attempting to include the NOK became normative and institutionalised amid the cohort of MH patients under the MHA in the ED, with the consent of the person and communicated as a best practice value of the organisation. Clinicians reported that this practice also generalised to other MH patients seen within the ED. The hospital admission rate was lowered and the community treatment rate was increased within the context of this new milieu.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
