Abstract
Introduction:
Burnout is a syndrome occurring from an overwhelming workplace stress. The study was done at a large teaching hospital identified as a COVID-19 treating hospital. During COVID-19 pandemic, the country was in Movement Control Order since 18 March 2020 to contain the spread of the virus, and thus, it has increased the job workload and responsibility. The purpose of this study was to identify the prevalence of burnout among emergency healthcare worker in this hospital and to identify the factors contributed to the burnout.
Methods:
A cross-sectional study was conducted using a questionnaire among emergency healthcare worker from 8 May 2020 to 15 May 2020 during the Conditional Movement Control Order. The questionnaire was adapted from Michelle Post, Public Welfare, Vol. 39, No. 1, 1981, American Public Welfare Association and distributed via Google Forms. It consisted of 28 questions and was rated based on a five-point Likert-type scale. The questions were then summed up to determine the burnout levels.
Results:
There were 216 respondents with 65.7% were nurses, 17.1% were doctors, and the rest were assistant medical officer. 51.3% of the respondents had burnout with 61.2% of nurses, 35.1% of doctors, and 29.6% of assistant medical officer. There was weak correlation (r = 0.148) with the years of experience working in emergency department and the level of burnout (p = 0.03). Among the burnout features were fatigue with 52.2% and frequent physical illness and feel unappreciated with 48.6% and 45.9%, respectively. The job-related issues which predisposed to burnout were demand coping with an angry public with 70.2%, job overload 63.9%, lack clear guideline or rapid program changes 54%, and pay too little 53.1%.
Conclusion:
Emergency healthcare worker has a high rate of burnout especially among the nurses. The factors leading to burnout were frequent exposure to angry public, job overload, lack of clear guidelines, and perception of underpaid.
Introduction
The novel coronavirus (COVID-19) was initially identified in Wuhan city of Hubei, China province in December 2019 and has been continuously spreading and has affected millions of people globally reported by World Health Organization (WHO). WHO has officially declared it a pandemic in March 2020. As of 22 May 2020, Malaysia had a total of 7137 confirmed cases, 115 deaths and the number still in the rising.
The pandemic of COVID-19 has put the healthcare workers (HCWs) across the world to battle against the unseen virus under extreme conditions. These changes would affect the daily life and mental health of these diligent HCWs in order to provide the care for the patients with constrained resources. These would predispose these HCWs to mental health problems and burnout. 1
Burnout is a psychological syndrome resulting from exposure to the overwhelming, chronic stress particularly at work. Burnout was first described by Freudenberger, who explored the phenomenon of burnout. He defined burnout as “to fail, wear out, or become exhausted by making excessive demands, energy, strength or resources.” He also described the physical signs of burnout which were fatigue, frequents headaches, gastrointestinal disturbance, sleeplessness, and shortness of breath. 2
In 2016, Maslach and Leiter further expanded the characteristics of burnout including exhaustion, depersonalization, and inefficacy. The exhaustion was defined as wearing out, loss of energy, depletion, debilitation, and fatigue. The depersonalization was described as inappropriate attitudes toward clients, irritability, and withdrawal. The inefficacy was defined as reduced personal accomplishment, and described as reduce productivity, low morale, and inability to cope. 3
To date, WHO included burnout in the International Statistical Classification of Diseases and Related Health Problems–Eleventh Edition (ICD-11)), but burnout has not been classified as a medical condition. The burnout definition according to ICD-11 is “a syndrome resulting from chronic workplace stress that has not been successfully managed; characterized by feelings of exhaustion, increase mental distance from one’s job or negativism or cynicism and reduce professional efficacy.” 4
Since WHO declared burnout as an occupational phenomenon, the syndrome has become a major health concern worldwide among HCWs. During the COVID-19 pandemic, the burden of HCWs increased and in providing health services they were facing high workloads. Working during the COVID-19 outbreak increases the likelihood of developing burnout. 5
The incidence of burnout has increased among HCWs during this COVID-19 pandemic, but data in Malaysia have been rarely published especially among the emergency HCW. Multiple studies before the pandemic have found high prevalence of burnout in HCWs particularly among the physicians and paramedics. The burnout among HCW is needed to be recognized because of its association with negative consequences on patient care, physician health, and the healthcare system itself. 6
As in Malaysia, sudden surge of patients with limited staff to handle the situation at the initial phase of pandemic has contributed to fatigue. Moreover, there were some person under investigations who have withheld their histories of traveling overseas from the HCWs. Furthermore, daily changes in COVID management guidelines have increased the stress level of the HCW. Uncertainties in the guidelines and fear of nosocomial COVID infection further increased the work-related anxiety.
The objectives of this study were to determine the prevalence of burnout among emergency medicine department HCWs and to identify and describe the independent factors contributing to burnout among them during this COVID pandemic. It was hoped that further intervention could be constructed to prevent further burnout to occur in future.
Materials and methods
This was a single-center, cross-sectional study of burnout among the HCWs working in the Emergency Medicine Department (ED), during the COVID-19 pandemic outbreak. This study was conducted in a teaching hospital in Malaysia with 1300 bed capacity and 80% of bed occupancy rate. The hospital was one of the designated COVID-19 treating hospitals since March 2020. There were 2421 Patients Under Surveillance (PUS) and 1440 Patient Under Investigation (PUI) for COVID-19 until May 2020. PUS is defined according to the Ministry of Health Malaysia as asymptomatic patient with risk of COVID-19 contact while PUI is symptomatic patient with risk of COVID-19 contact. To date, the hospital has treated 189 COVID-19 positive patients. The study was approved to be conducted by the hospital’s Medical Ethic Committee with ethical approval no. 2020616-8765.
The source of population chosen was HCWs working in Emergency Department at the time of pandemic particularly during the Movement Control Order (MCO) which included the doctors, nurses, and assistant medical officer (AMO). We have excluded the HCWs from the wards who were deployed to ED during this pandemic. A convenience sampling method was used. At the time of study was conducted, there were a total of 279 HCWs working in ED. The participation was purely voluntary and anonymous.
The questionnaire form was adopted from Michelle Post, Public Welfare, Vol. 39, No. 1, 1981, American Public Welfare Association. The questionnaire form was sent to the participants via Google Forms. The Google Forms was opened from 8 May 2020 to 15 May 2020 during Conditional Movement Control Order (CMCO). It consisted of 28 questions on behavior, attitude, and job-related questions and rated based on a five-point Likert-type scale. Then, all points of each question were summed up to determine the levels of burnout as shown in Table 1.
Levels of burnout.

Data were entered and analyzed after data collection was completed. A descriptive statistic was used to summarize the socio-demographic characteristics of the participants. The numerical data were presented as mean values (standard deviation (SD) based on their normality distribution and categorical data were presented as frequency (percentage). The Spearman’s rank-order (rho) was used with the significance value at the 0.05 for the correlation between age, gender, years of working experience, and job position with burnout.
Results
There were 216 staff responded to the questionnaire with overall response rate of 77%. There were more female respondents than male (148 (68.5%) vs 68 (31.5%)) and most of the female were nurses. The mean age of the participants was 30 years old. Majority of the respondents were nurses as shown in Table 2 and about 53% of doctors were non-respondents compared to 10% of nurses and 14% of AMO as shown in Table 3.
Distribution of respondents’ current post in ED.
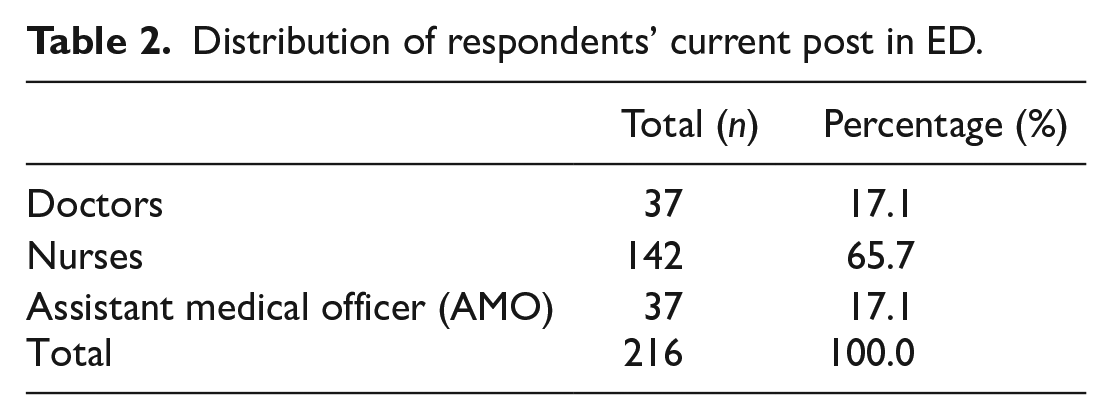
Distribution of respondents and non-respondents in ED.
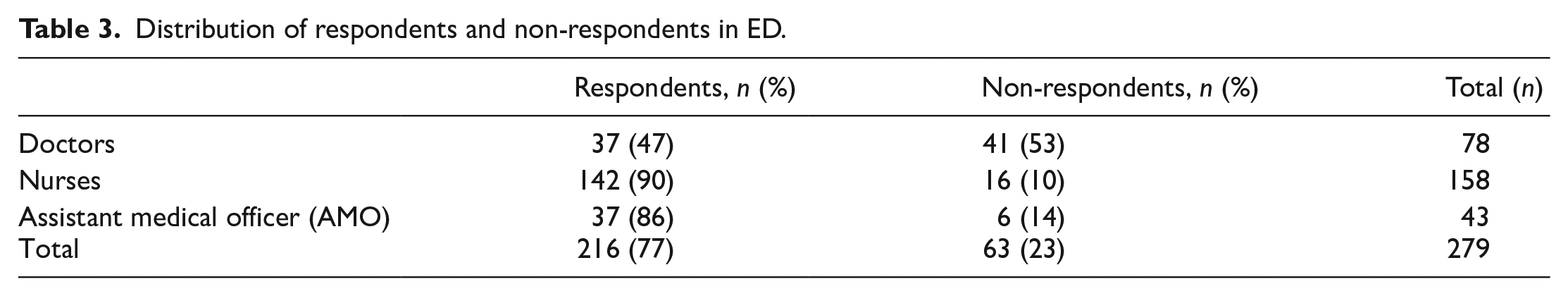
There were a consultant, 4 emergency physicians, 31 trainees in emergency master’s program, and a service medical officer among the doctors who responded to the questionnaire. Majority of them have about 5–10 years of working experience in ED with mean years of working of 6.94 years. The study showed that the burnout rate among the HCWs in ED was 51.3% as shown in Table 4.
Burnout categories.
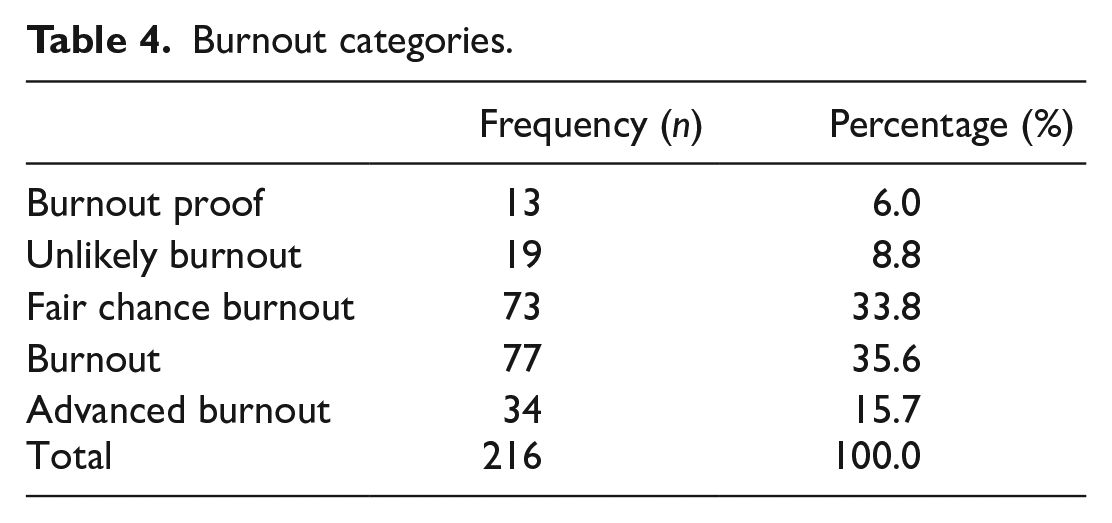
In Figure 1, out of the 51.3% of the HCW in ED had burnout nurses were the highest rate of burnout with 61.2% of them has burnout compared to doctors with only 35.1%.
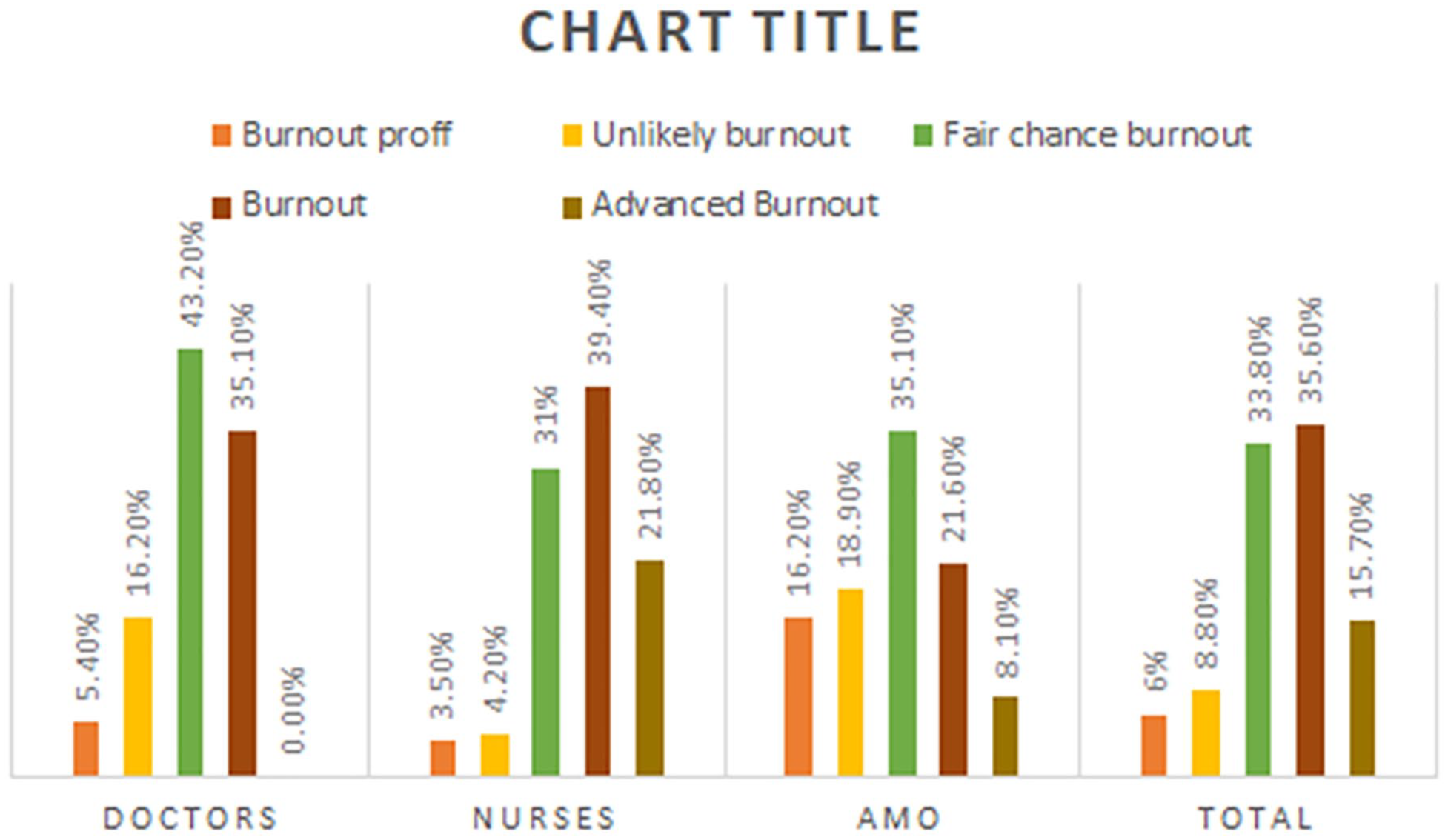
Distribution of burnout categories among HCWs in ED.
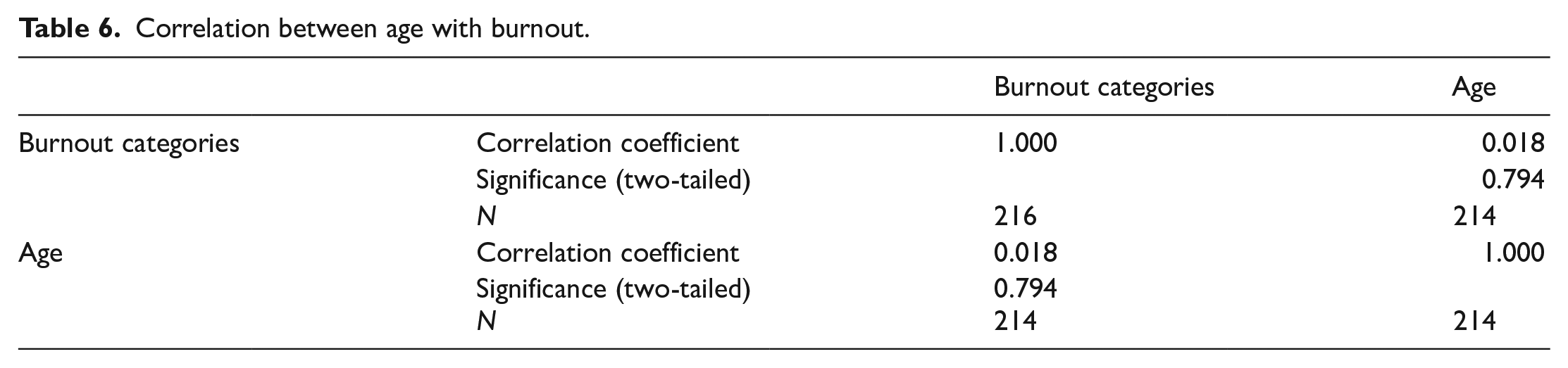
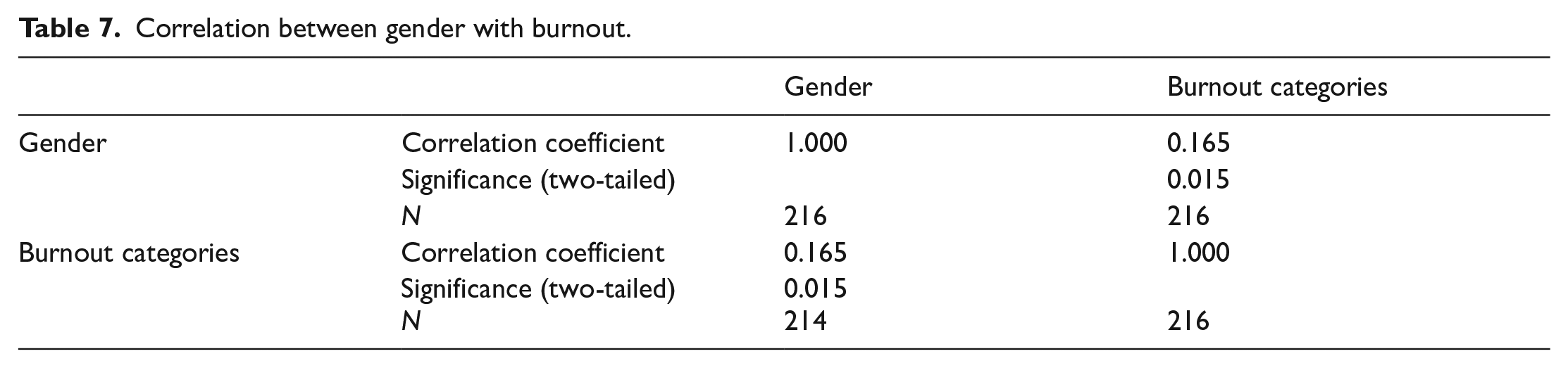
In our study, as shown in burnout as shown in Tables 5–7, we also evaluated the factors that correlate with burnout. We found out that there was significant correlation between years of working in ED with burnout as the p-value = 0.03. However, there was no significant correlation between burnout with age and gender as the p-values were 0.794 and 0.015, respectively.
Correlation between years of working in ED with burnout.
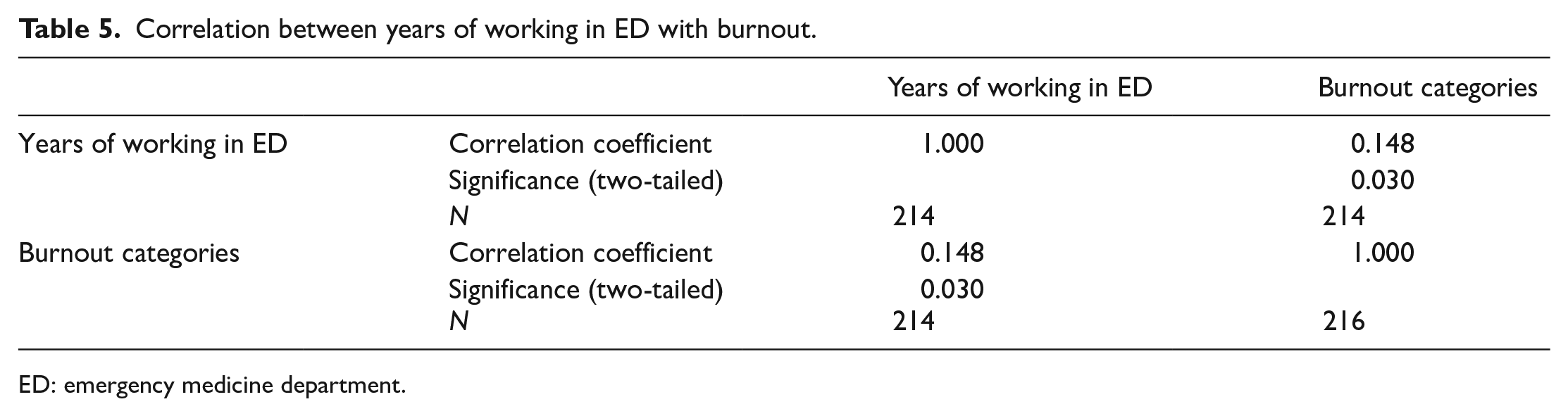
ED: emergency medicine department.
Correlation between age with burnout.
Correlation between gender with burnout.
Based on the questionnaire on behavior, attitude, and job-related questions, we evaluate the factors that contributed to the burnout. Most of the respondents felt tired, fatigued rather than energetic even when getting enough sleep (52.2%), suffered from physical complaints or frequent illness (48.2%), and felt unappreciated or at used on the job (45.9%). Few of them rigidly following orders without providing creative opinions (31.5%). When working in ED, the job position demand coping with an angry public (70.2%). Most of the respondents felt that his or her job overload themselves with work demand, long shifts and frequent overtime or deny vacation, sick leaves, or time-outs (63.9%). With current situation of pandemic outbreak, most of them felt that lack of clear guidelines or required them to deal with rapid program changes (54%). They also felt that current job position paid too little (53.1%).
Discussion
Most of the respondents were female which majority of them were nurses. The mean years of working in ED were 6.94 years which also reported by de Paiva et al. 7 who conducted a research in Brazil found that most of the HCWs in Brazil had been working for 5–10 years. Our study revealed that 35.6% of the emergency HCW had burnout which was consistent with the finding reported by Moukarzel et al., 8 2019 which was about 34.6%.
Nurses had the highest rate of burnout at 39.4% when compared to the doctors were about 35.1%. This might due to the stress induced by patients’ families and dealing with violence as evaluated by Abdo et al. 9 Furthermore, nurses were exposed to the pressure from patients and relative. 10 Lack of support of the hospital management also contributes to the burnout among nurses as reported by Basis, 10 2017.
From the total burnout and advance burnout, our study noted that nurses still at the highest rate of burnout which was 78.4%. This finding almost corresponded to the study by Hooper et al., 11 2010 which reported that 82% of emergency nurses had moderate to high levels of burnout. These might be due to their work conditions and responsibilities with more prolonged contact with person under investigations or COVID-19 patients. Also, they concern of exposing the family members with virus increase the anxiety. Hence, they have higher stress level as reported by Spoorthy et al. 12
In this study, burnout correlated with increasing years of working in ED (p-value = 0.03) which also evaluated in the study by Popa et al. 13 Popa et al., 13 2015 reported that staff working more than 5 years in the department had higher burnout when compared with those working less than 5 years. The longer HCW working in the ED, they are more likely to develop burnout. The longer the HCW works, the more experienced and more responsibilities they would have, thus high likely to develop burnout.
Our study did not find correlation between gender and age with burnout.13,14 Popa et al., 13 2015 also found no correlation between burnout with age. Huda and Hajar, 2018 also found there were no correlation between burnout with age and gender as the p-values were 0.315 and 0.339, respectively. 14 As in our country, female and male equally working to support the family after graduation from university. This correlate with the age of 20 years old to 60 years old when pension.
Most of the respondents (52.2%) reported the symptoms consistent with burnout such as that they felt tired, fatigue rather than energetic when getting enough sleep. This was similar with a study in Croatia. 15 This might be due to increase job workloads and increase number of shifts worked per month. 16 We also found that 63.9% of the respondents felt that job overloads and were paid with low wages (53.1%). Other factor that contributing to burnout was nurses reported that the job demand coping with an angry public (70.2%). With prolonged waiting time, public may get angrier and can predisposed to verbal violence at workplace. 17
Limitation of the study
The result sample was in ED only and this might not be generalized to other department. Other limitation is that we do not know that the non-responder might suffer from burnout, thus refusing to participate.
Conclusion
Emergency HCW has a high rate of burnout especially among the nurses and senior staffs in comparison to the juniors. They commonly exhibited fatigue, feeling tired, and suffered from frequent illness as part of their burnout symptoms. The factors leading to burnout in our institution during this pandemic were frequent exposure to angry public, job overload, lack of clear guideline, and perception of underpaid. Thus, further study suggested for intervention to improve the burnout among emergency HCWs before burnout affected the mental health of the HCW, patients’ care, and institution.
Supplemental Material
sj-pdf-1-hkj-10.1177_1024907921989499 – Supplemental material for Assessment of burnout among emergency medicine healthcare workers in a teaching hospital in Malaysia during COVID-19 pandemic
Supplemental material, sj-pdf-1-hkj-10.1177_1024907921989499 for Assessment of burnout among emergency medicine healthcare workers in a teaching hospital in Malaysia during COVID-19 pandemic by Mohd Idzwan Zakaria, Ruzaina Remeli, Mohd Fitri Ahmad Shahamir, Mohd Hafyzuddin Md Yusuf, Mohammad Aizuddin Azizah Ariffin and Abdul Muhaimin Noor Azhar in Hong Kong Journal of Emergency Medicine
Footnotes
Acknowledgements
This study was approved by the Medical Research Ethics Committee, University Malaya Medical Centre. The authors thank the hospital director and all the emergency staff for their cooperation during data collection.
Author contributions
M.I.Z. designed the protocol on methodology, sample collection, ethical approval, and writing, reviewing and editing the manuscript. M.I.Z. also supervised in completing the manuscript. R.R. was involved in research literature, gaining ethical approval, and writing and editing the manuscript. A.M.N.A. was involved in development and participant recruitment together with M.F.A.S. A.M.N.A. also involved in gaining the ethical approval. M.H.M.Y. and M.A.A.A. involved in data analysis and wrote the first draft of manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was self-funding.
Availability of data
The data sets generated and analyzed during this study are available from Ruzaina Remeli (corresponding author).
Informed consent
Informed consent was obtained via Google Forms from the participants before answering the questionnaire.
Ethical approval
Ethical approval for this study was obtained from the Medical Research Ethics Committee (2020616-8765). The study protocol conforms the ethical guideline of the 1975 Declaration of Helsinki.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
