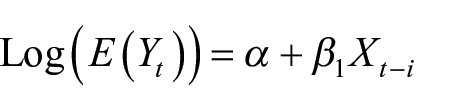Abstract
Background:
Along with the industrialization, the air pollutants have gained more attention and studies especially about respiratory diseases were conducted. Emergency visit reflects acute aggravation of disease rather than chronic exacerbation.
Objectives:
The objective of this study was to evaluate the relationship between the ambient particulate matter and the emergency visits with respiratory disease in South Korea.
Methods:
Patients diagnosed with respiratory disease in the emergency department in 2018 were enrolled. The data of meteorological factors and air pollutants between 4 December 2017 and 31 December 2018 were acquired. Poisson regression was used with daily emergency visits as the response variable and single-day particulate matter concentration as the explanatory variable.
Results:
A total of 4207 patients were enrolled. In Poisson regression analysis of all respiratory diseases, the effects of
Conclusion:
The results can be used to predict the increase of emergency visits and need for medical resources when the ambient particulate matter concentration rises.
Keywords
Introduction
Meteorological changes have had a great impact on human life for a long time and these associations have been revealed by many epidemiological studies.1,2 Known disorders that are largely affected by meteorological factors are neurovascular diseases, 3 cardiovascular diseases,4,5 respiratory diseases, and other diseases under active investigation.6–9
Air pollution contributes substantially to the global burden of disease and mortality, which has increased over the past few years.10,11 Along with industrialization, air pollutants have gained scientific attention and studies especially on respiratory diseases have been conducted. 12 Although both short-term and long-term effects of particulate matter on respiratory disease exist, emergency visits reflect acute disease aggravation rather than chronic exacerbation.13–15 We focused on the relatively short-term effects of airborne particulate matter concentrations on respiratory diseases during emergency room visits.
Previous studies have focused on the lag effect of meteorological factors on emergency respiratory visits in Asian countries, 16 mostly in Hong Kong and China.17–20 Although there are a few studies on the relationship between individual disease (chronic obstructive pulmonary disease (COPD), pneumonia) and particulate matter concentration in South Korea,21,22 a study that includes the entire set of respiratory diseases has not been conducted. So, this study was focused on the effects of particulate matter on the entire set of respiratory diseases in South Korea on behalf of Far East Asia. Additionally, single-day and cumulative effects were analyzed by age and disease subgroups.
Methods
Participant data
This was a retrospective study that included patients who had visited the Emergency Department (ED) of a secondary referral hospital in Gyeonggi-Do (province), South Korea, from 1 January to 31 December in 2018. Patient data were collected from the electronic medical record system and included age, sex, comorbidities, and diagnosis at discharge. Daily emergency room visits by respiratory disease were collected using the International Classification of Disease (ICD) 10th Revision Code, J00-J99. We divided all respiratory diseases into four major groups: upper respiratory tract infection (ICD-10: J00-06, J30-39), lower respiratory infection (ICD-10: J09-18, J20-22), chronic respiratory disease (CRD; ICD-10: J40-47), and other respiratory diseases (ICD-10: J80-86, J90-99, R codes). Patients in bedridden status or from nursing care centers and influenza patients (ICD-10: J09-11) were excluded. The seasons were divided by March to May as spring, June to August as summer, September to November as fall, and December to February as winter. This study was approved by the Institutional Review Board of our hospital and the requirement for informed consent was waived due to its retrospective nature.
Meteorological and air pollutants data
Meteorological and air pollutants data were acquired from the Korea Meteorological Administration. The data were collected from 4 December 2017 to 31 December 2018 based on the hypothesis that weather changes would exert influence over 28 lag days. Meteorological factors were mean temperature, mean relative humidity, mean sea-level pressure, and air pollutants were
Statistical analysis
Poisson regression (a generalized linear model, GLM) was used with daily emergency visits as the response variable and single-day particulate matter concentration as the explanatory variable
E(
To determine the validity of the model setting, goodness-of-fit tests were performed and both the null hypothesis and alternative hypothesis were defined as follows
H0: model setting is invalid versus H1: model setting is valid.
To calculate the test statistics in the Poisson generalized linear model, the dispersion parameter for the Poisson family was taken to be 1. The null deviance was 477.86 with 364 degrees of freedom and the residual deviance was 471.89 with 363 degrees of freedom. The gap between the Null deviance and residual deviance followed the chi-square distribution. So, this was chosen as the test statistic.
The degree of freedom for the chi-square distribution was same as the gap between the two deviances (364 − 363 = 1).
If the significance level is chosen as 0.05, the critical region {χ12(0.05)} is 3.84, then the result of test statistic calculation is 477.86 − 471.89 = 5.97. In conclusion, the test statistic (5.97) is larger than the critical region, thus the null hypothesis was rejected. In other words, the model setting was valid.
The Shapiro–Wilk test was used to check data set normality and all p values for the variables were less than 0.05, so the data were not normally distributed. In addition, we used Pearson correlation analysis to evaluate the multicollinearity between independent variables. Analysis of variance (ANOVA) was applied to investigate the seasonal, day-of-week differences between emergency visits. A p-value < 0.05 was defined as statistically significant. We used Microsoft Office Excel version 2010 to record all collected data. The GLM and moving averages were analyzed using basic functions and the “lawstat,” “corrplot,” “rpart,” and “rattle” packages from R version 3.6.1 which was also used for all other statistical analyses.
Results
Participant characteristics
A total of 4207 patients were enrolled. The mean age of enrolled patients was 34.1 (±27.5) and there were 2007 male patients (52.3%). There were 1438 (34.2%) persons aged under 18 years, 2016 (47.9%) were 18–64, and 753 (17.9%) were over 64. The proportion of disease types was 66.89% for acute upper respiratory infection (AURI), 22.04% for acute lower respiratory infection (ALRI), 6.01% for CRD, and 5.06% for other respiratory diseases (ORD). Comorbid conditions included 454 (10.7%) patients with hypertension, 447 (10.6%) with respiratory disease, 252 (5.9%) with diabetes, 205 (4.8%) with cardiovascular disease, 119 (2.8%) with cerebrovascular accident, 83 (1.9%) with dyslipidemia, 70 (1.6%) with chronic kidney disease, and 52 (1.2%) with liver disease. Among the patients, 858 (20.4%) were admitted and 52 (1.2%) patients died after admission (Table 1).
Demographic data of patients with respiratory disease.
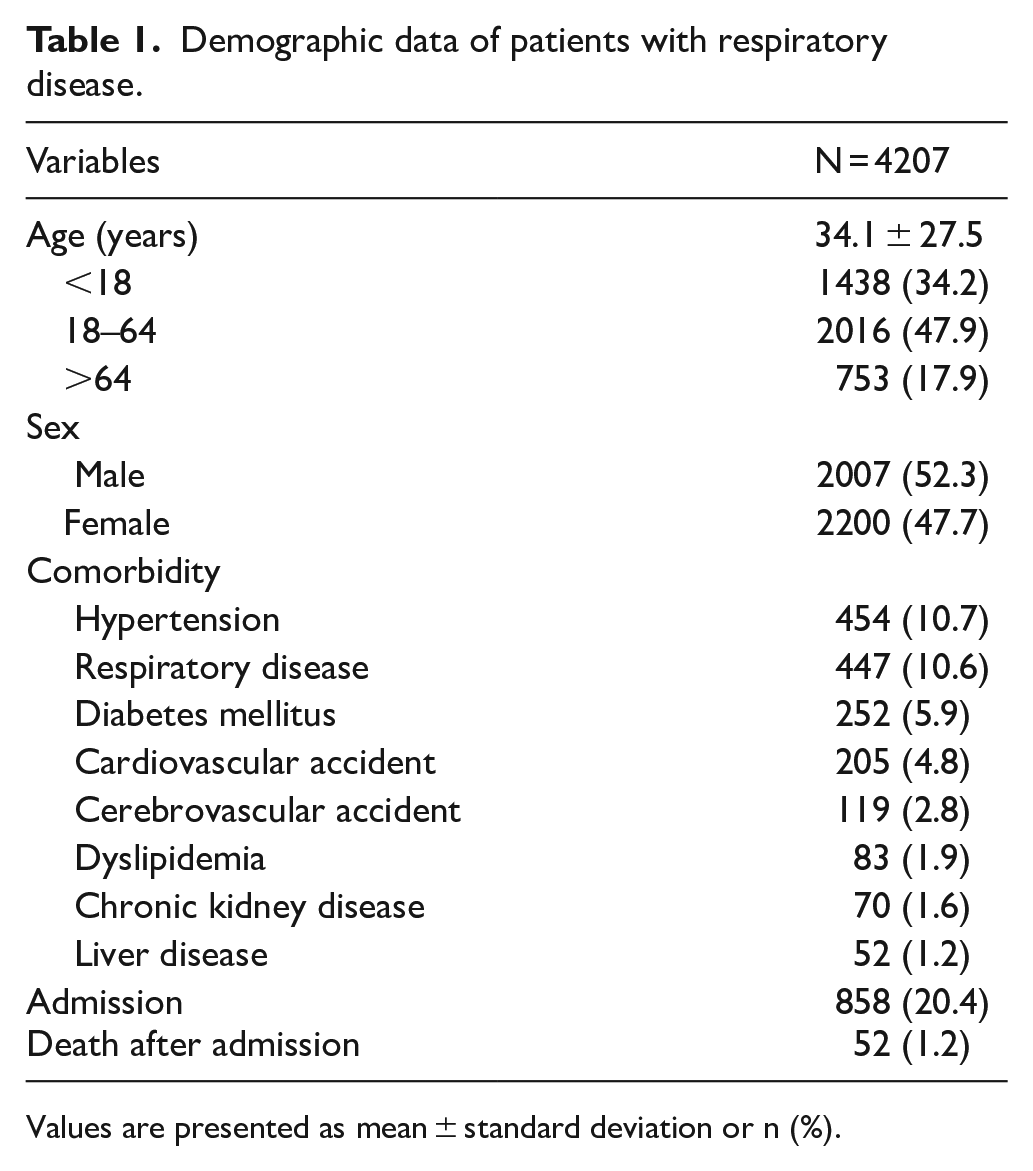
Values are presented as mean ± standard deviation or n (%).
Visit number by month, season, and day of week
Monthly visits were maximum in December with 607 patients and the minimum was in March with 241 patients. Seasonal visits peaked in winter with 1394 (33.1%) patients and were lowest in summer with 882 (20.9%) patients. Day of week visits were greatest on Sunday with 1051 (24.9%) visits and smallest on Thursday with 459 (10.9%) visits (Supplemental Appendix Figure 1).
Relationship between meteorological factors and air pollutants
A total of nine meteorological factors were analyzed. Excluding O3, all air pollutants were positively correlated. Temperature and sea-level pressure were negatively correlated. But the correlation between meteorological factors and air pollutants was not significant (Supplemental Appendix Figure 2).
Particulate matter concentration and emergency visits
The Poisson regression on particulate matter and emergency visits and correlation analysis were conducted not only for the entire respiratory disease group but also for the subdivided disease and age groups. The entire group analysis showed the effects of
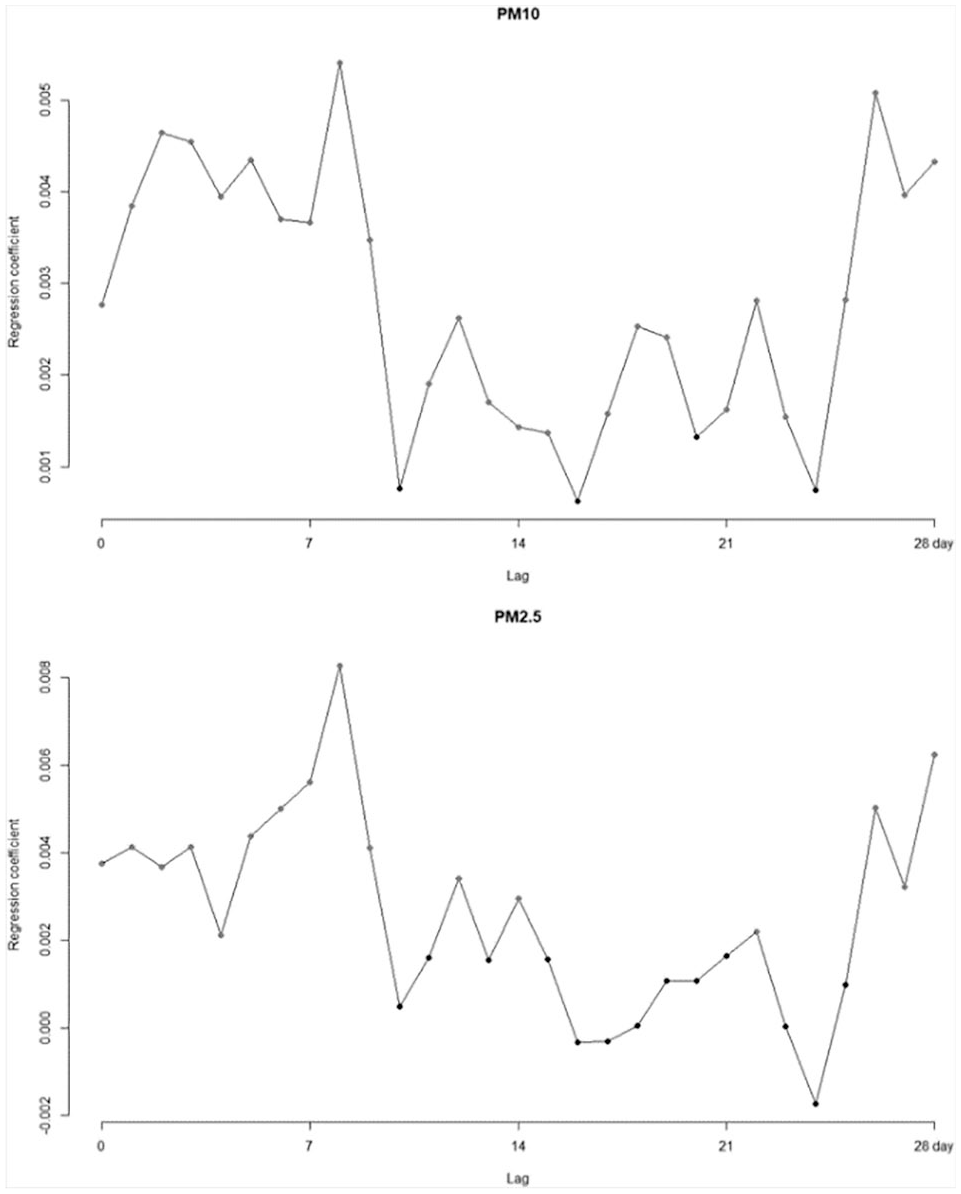
The results of Poisson regression analysis of single-day particulate matter exposure and daily emergency visits by lag days for all respiratory diseases.
The disease group analysis showed the AURI and ALRI groups were similar to the entire group in that lag days 8 and 26 were significantly associated compared to the valley between those days (Supplemental Appendix Figures 3 and 4). The CRD group analysis showed
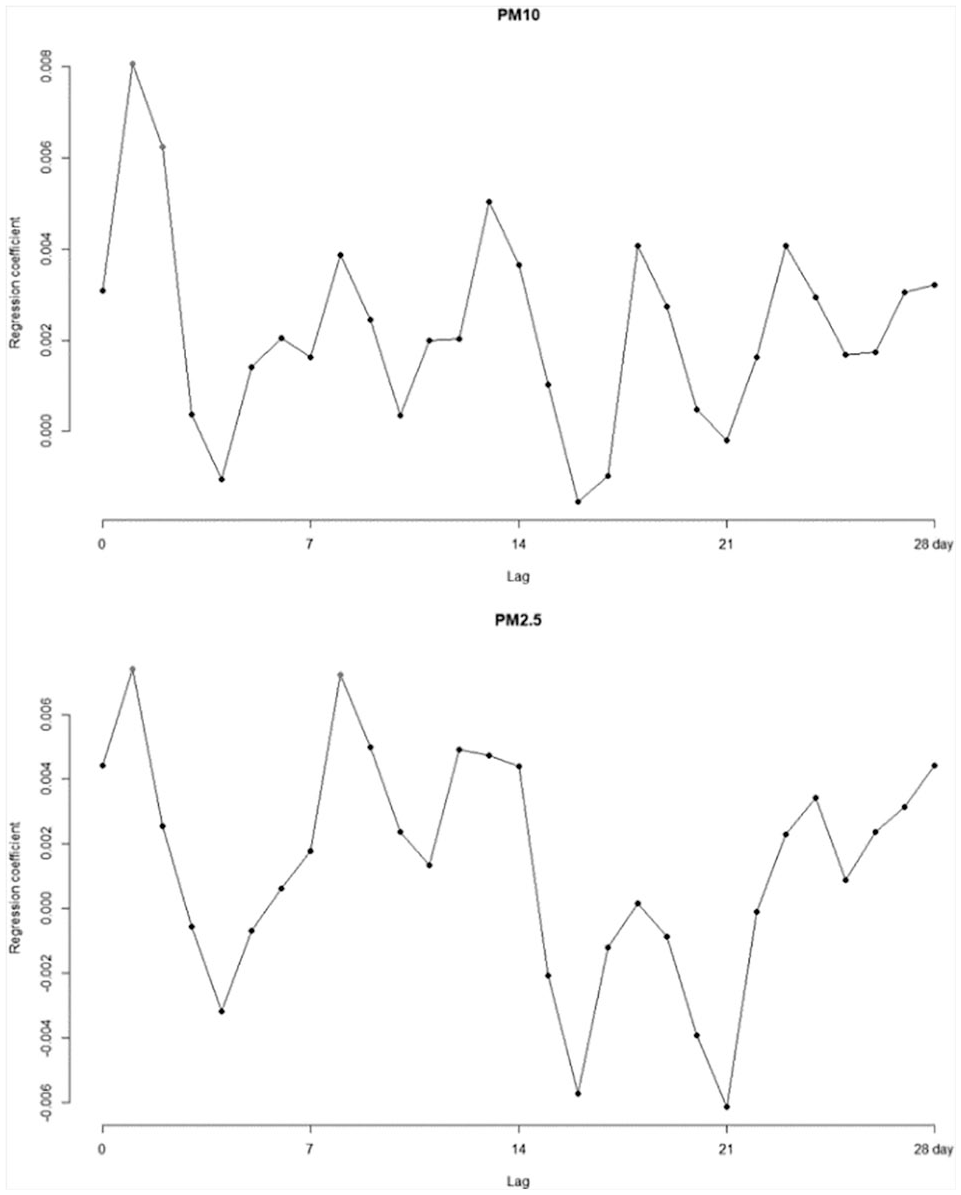
The results of Poisson regression analysis of single-day particulate matter exposure and daily emergency visits by lag days for the chronic respiratory disease group.
We also conducted moving average analysis with Z-values to evaluate the cumulative effect of particulate exposure. The Z-value increased until it peaked at cumulative lag day 14, but in calculations that included longer days, this showed a declining trend (Figure 3). The two age subgroups for persons younger than 18 and 18–64 had trends similar to the entire age group (Supplemental Appendix Figures 7 and 8), whereas those aged older than 64 were affected by particulate matter mostly at lag days 2, 8, and 11 for both particulate sizes (Figure 4). Emergency hospital admission increased for
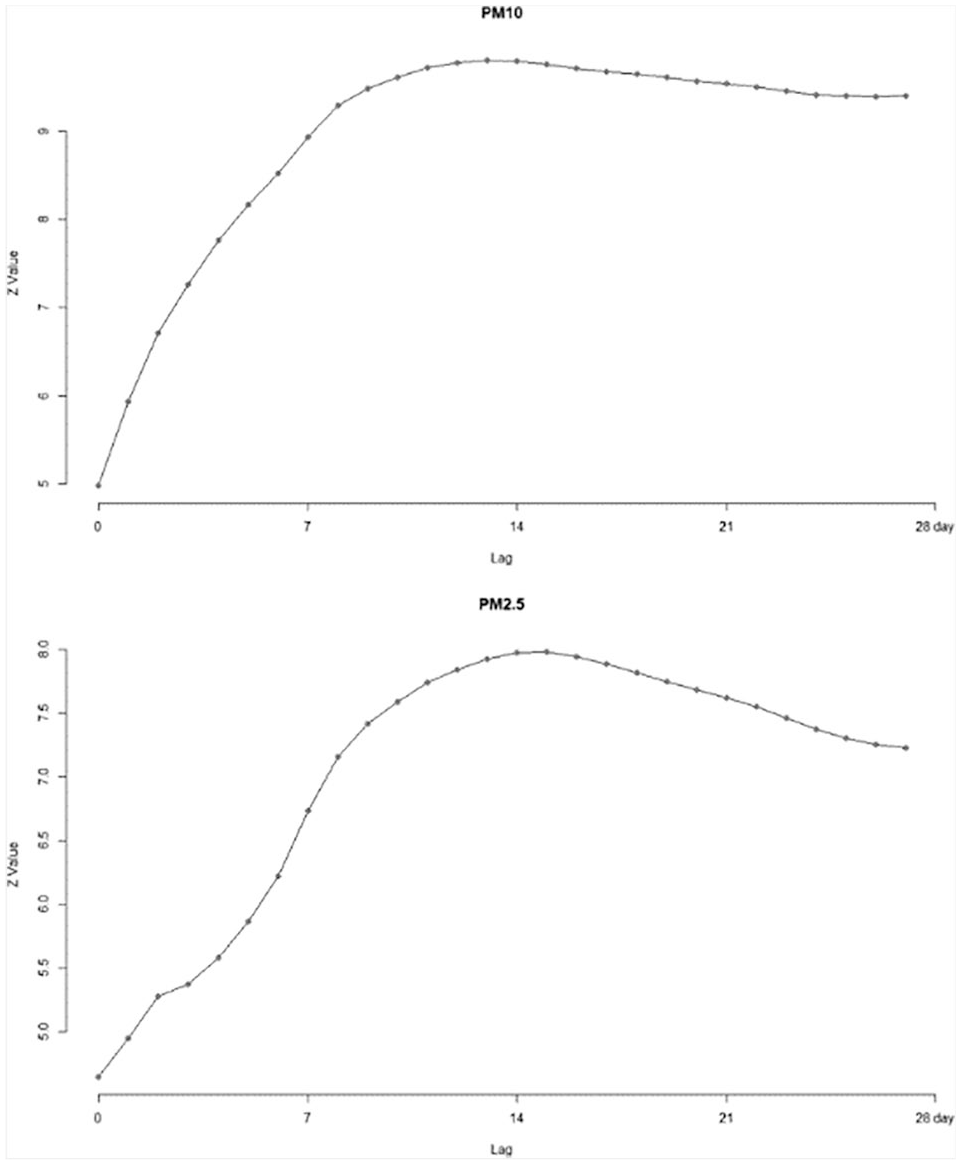
Z-score of Poisson regression analysis of moving average over 0–28 cumulative lag days. Horizontal axis represents the total period of inclusion.
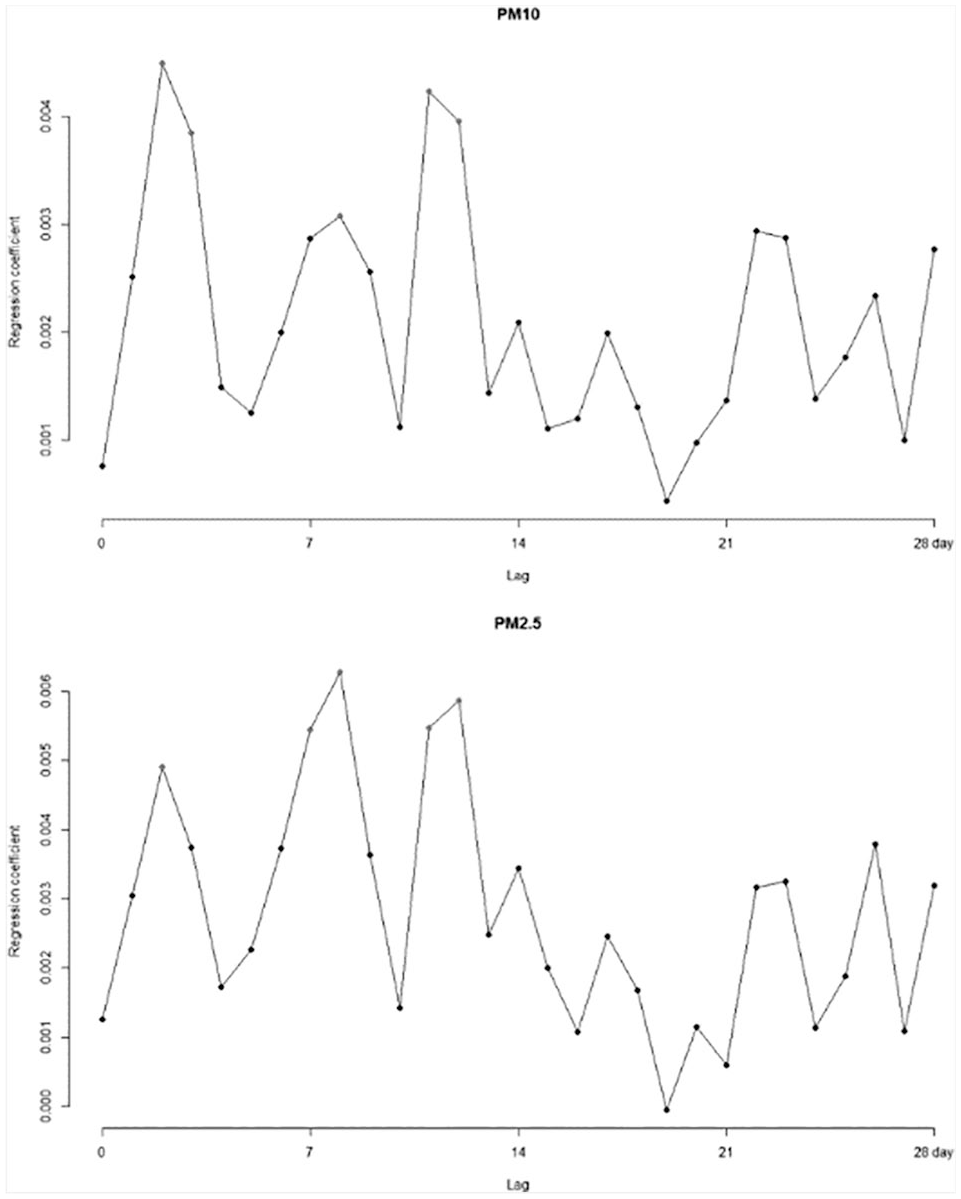
The results of Poisson regression analysis of single-day particulate matter exposure and daily emergency visits by lag days in the group aged >65.
The decision tree analysis showed split points for both particulate matter and lag day for predicting emergency visits. A total of 100 different seeds (models) were simulated and the main split point (stump) was constant in every analysis. For
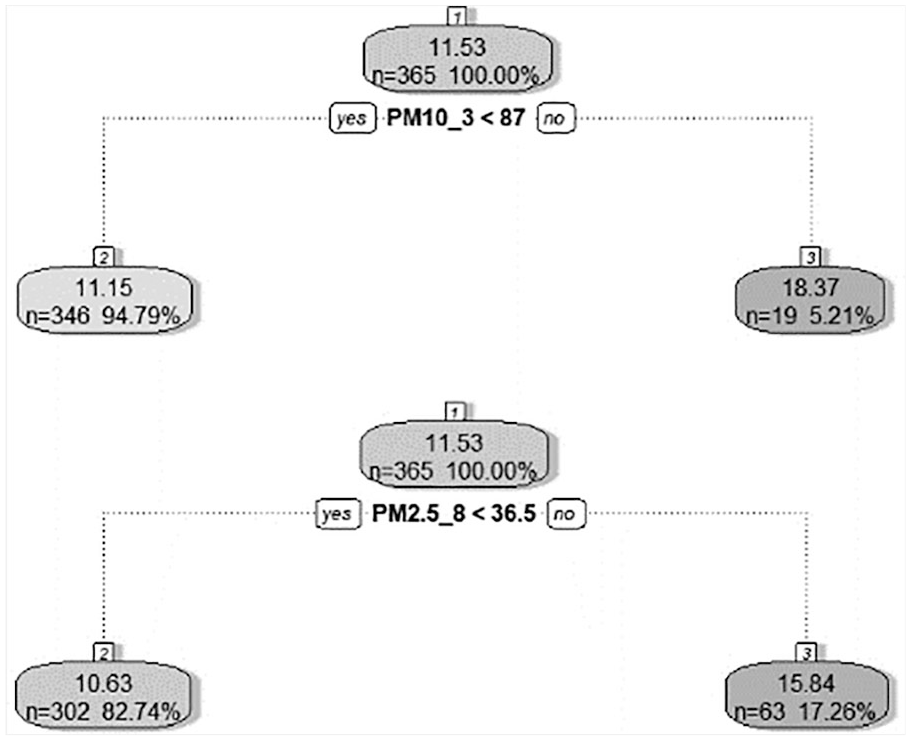
Decision tree to identify the split value for particulate matter concentration and lag days. The number at the top of the square is the average predictive number for emergency visits for all respiratory diseases and the number at the bottom of the square is the number and proportions for the entire group. At the middle of the graph, the split point for lag day (former) and concentration (latter) of particulate matter exposure is shown.
Discussion
Climate change has become a global issue. Meteorological factors and airborne particulate matter affect human respiratory diseases, which is one of the most common disease types managed by emergency physicians. Due to the nature of emergency care, visiting patients do not present with any specific respiratory disease. This study was conducted to prepare and redistribute the resources for acute respiratory aggravation after particulate matter concentration increases. To the best of our knowledge, this study is one of the few that investigates the single-day and cumulative effects of airborne particulate exposure on the entire set of respiratory diseases seen in South Korean patients.
We collected data for meteorological factors and particulate matter concentration until 28 days before emergency visits because, in previous studies on pneumonia and COPD, no lag effect longer than 28 days was found to be significant.21,22 Patients in the bedridden status and from nursing care centers were excluded because they are less likely to have been exposed to the outside atmosphere. Also, influenza patients were excluded because pneumonia has been a confounding variable in previous studies. 17
This study focused on airborne particulate matter more than other meteorological factors. The possibility that other meteorological factors act as confounding variables cannot be excluded completely, but the results can have sufficient validity because the correlations between the air pollutants and meteorological factors were relatively weak.
Airborne particulate matter has been shown to injure the lung’s normal protective mechanisms and induce inflammatory reactions. Smaller particle sizes are more easily absorbed into the lower respiratory tract which makes it harder for such particles to be excreted.23,24 Many studies have investigated the short-term and long-term effects of particulate matter exposure on morbidity and mortality.25–27 In previous studies on patients with pneumonia and COPD, the effect of airborne particulates was greater at lag days longer than 14.21,22 In this study, the effects of airborne particulate matter peaked at lag days shorter than 8, and longer than 26 for the entire respiratory disease group. This may be due to subject differences.
The reason for dividing the entire group into subgroups is that AURI and ALRI account for the majority of emergency visits, and thus the entire group’s characteristics could be influenced by the majority of patients. As a result, the AURI and ALRI groups showed similar trends to the entire group, whereas the CRD group was affected at lag day 1 for
The age over 64 group demonstrated significant lag days of 2, 8, and 11 which is shorter than the age under 64 groups with significant lag days of 3–8. Of the CRD patients, 69.8% were aged over 65 and this large majority of elderly persons is responsible for the faster lag effect seen in the CRD group compared to the other groups.
Disease severity represented by both emergency hospital admissions and length of hospital stay were also correlated with airborne particulate matter concentration. This result applies to ED preparedness because the same number of visits with greater illness severity is accompanied by use of many medical resources as well as social costs.
In addition to the effect of daily exposure, long-term cumulative exposure was shown to be related to morbidity and mortality by Brunekreef and Holgate. 13 The moving average analysis with Z-score in this study showed that gross emergency visits were proportional to the cumulative days of exposure. But up to 14 days, cumulative days were significantly correlated with emergency visits while cumulative days longer than 14 days were weakly correlated with emergency visits. Therefore, when predicting emergency visits with cumulative days of exposure, inclusion of the most recent 14 days should be more predictive than longer periods.
The air pollutants that the Korea Meteorological Administration measure include
Several study limitations should be noted. First, the small sample size due to the short-term single center study limits our statistical power. Nonetheless, our study included all patients who visited the ED and reported respiratory disease for 1 year and thus it has sufficient statistical power. A long-term multicenter study might be needed to make a generalizable predictive model because the sources of particulate matter and population lifestyle vary with the geographical location of this study. Second, most clinical diagnoses that are made in the ED have the possibility of being different than the final diagnosis and often infectious disease pathogens which need further evaluation to detect are not identifiable. Third, we could not identify whether patients with respiratory morbidities were more affected by particulate concentration or not. Unlike the other studies that targeted specific respiratory diseases, we included the entire set of respiratory diseases, and therefore, it was difficult to analyze various respiratory morbidities separately.
Conclusion
In conclusion, the lag effect of single-day and cumulative airborne particulate exposure increased the number of emergency visits by respiratory disease patients. Both CRD and old age were related to the earlier effect. These findings suggest the possibility of establishing a predictive model for respiratory diseases by age and disease entity. More accurate and practical models can be obtained with the supplementation of this study’s limitations.
Supplemental Material
Supplementary_material – Supplemental material for Single-day and cumulative effects of ambient particulate matter exposure on emergency department visits for respiratory disease in South Korea
Supplemental material, Supplementary_material for Single-day and cumulative effects of ambient particulate matter exposure on emergency department visits for respiratory disease in South Korea by Hakjung Kim and Woosung Yu in Hong Kong Journal of Emergency Medicine
Footnotes
Author contributions
H.K. contributed to this study as the first author and W.Y. contributed as a corresponding author. H.K. and W.Y. conceived the study, designed the analysis, and drafted the manuscript. All authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
The materials described in the manuscript will be freely available to any scientist wishing to use them for non-commercial purposes, without breaching participant confidentiality.
Ethical approval
This study was approved by the local ethics committee. To maintain patient confidentiality, the forms did not include any data that would have enabled identification of any patients.
Informed consent
Since the study was a retrospective design, informed consent was not obtained.
Human rights
This study was conducted according to the World Medical Association Declaration of Helsinki.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.