Abstract
Traumatic atlanto-occipital dislocation is associated with significant mortality and morbidity. We present an 18-year-old female who visited the emergency department after a motor vehicle accident. A cervical spine computed tomography scan showed the postero-inferior atlanto-occipital dissociation and several diagnostic methods coincided with the diagnosis of atlanto-occipital dislocation.
An 18-year-old female presented to the emergency department (ED) with comatose mentality after motor vehicle accident. She was on the cardiac arrest state on the scene so she underwent bystander and emergency medical service (EMS) personnel cardiopulmonary resuscitation (CPR) for 10 min. After the CPR, she recovered spontaneous circulation and was brought to the ED. The initial blood pressure was 92/42 mmHg and the pulse rate was 105/min. She was immediately intubated using only succinylcholine. Then whole-body computed tomography (CT) scan was performed (Figure 1).
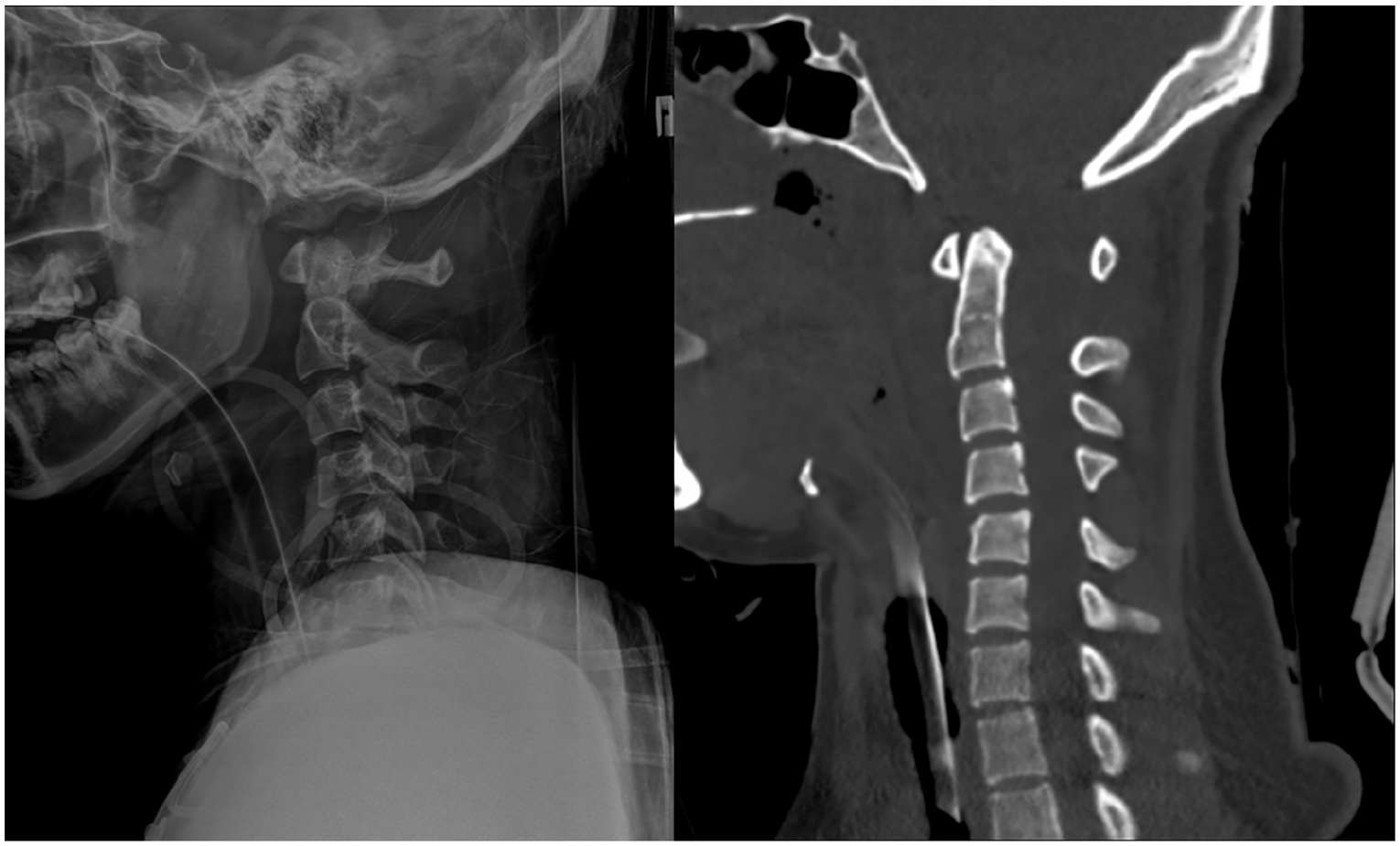
Cervical spine X-ray (left) and CT scan (right).
Questions
Answers
Cervical spine X-ray and CT showed disarticulation of the atlas from the skull base and the posterior dislocation of the cervical spine from the occipital condyles (Figure 1). These are suggestive findings for the diagnosis of atlanto-occipital dislocation (AOD).
Several methods are proposed for the diagnosis of AOD (Figures 2 and 3):
Power’s ratio: the ratio of the basion–posterior atlas arch to the opisthion–anterior atlas arch as measured on a true sagittal cervical spine CT, which is abnormal if greater than one;
Basion–dens interval: considered abnormal in the presence of a displacement > 10 mm;
Harris method: considered abnormal if there is anterior displacement > 12 mm between the basion and the posterior C2 line.
AOD is not common and most patients die immediately after the injury. However, because of the improvements in prehospital and hospital care, there are an increasing number of patients surviving in the ED. Because AOD can be difficult to diagnose and may be easily overlooked on routine cervical spine radiographs, emergency physicians should have a high index of suspicion for early diagnosis and avoiding neurological deterioration due to delay in care.
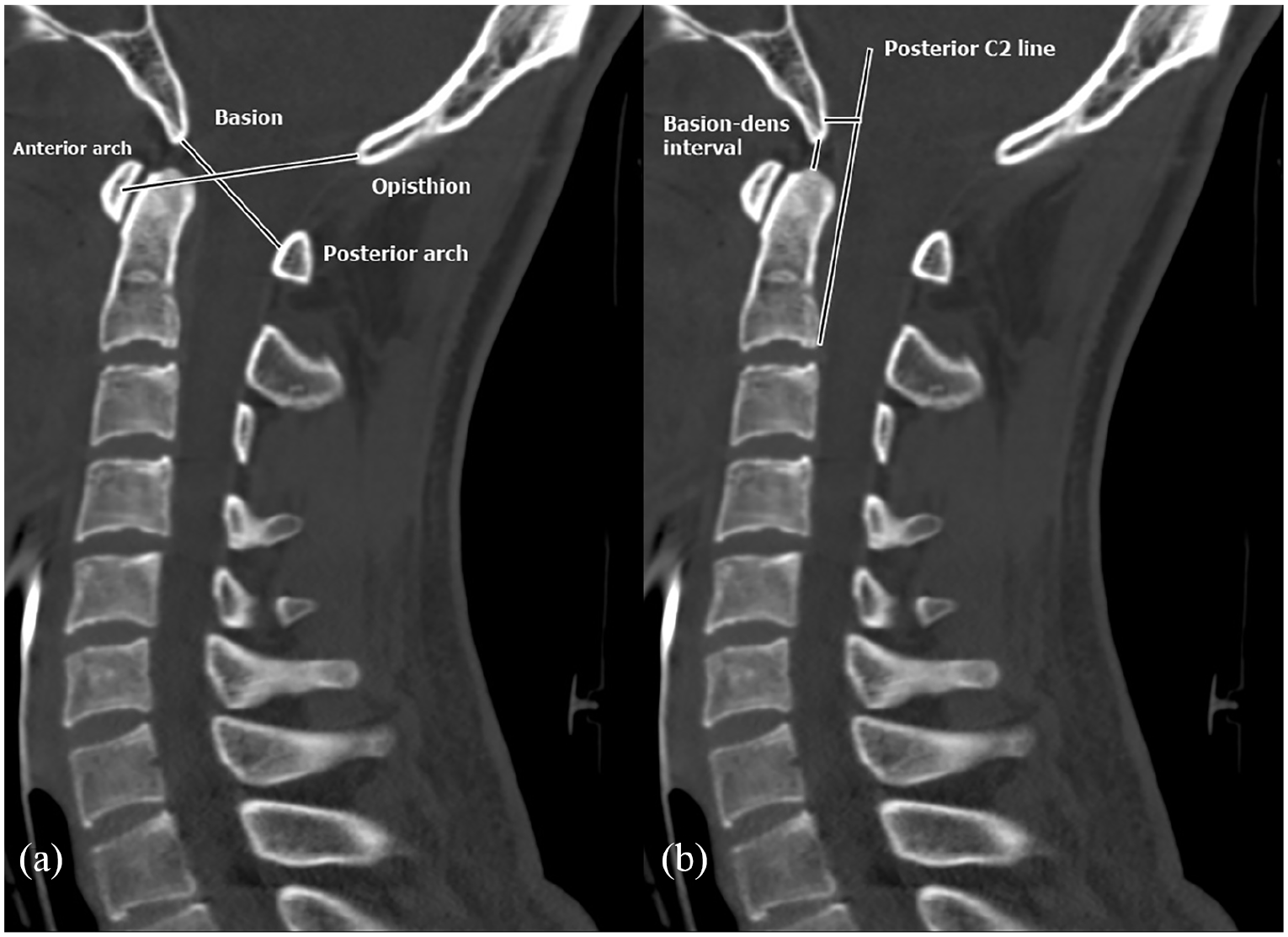
Cervical spine CT scan with normal findings: (a) Power’s ratio and (b) Basion–dens interval and Harris method.
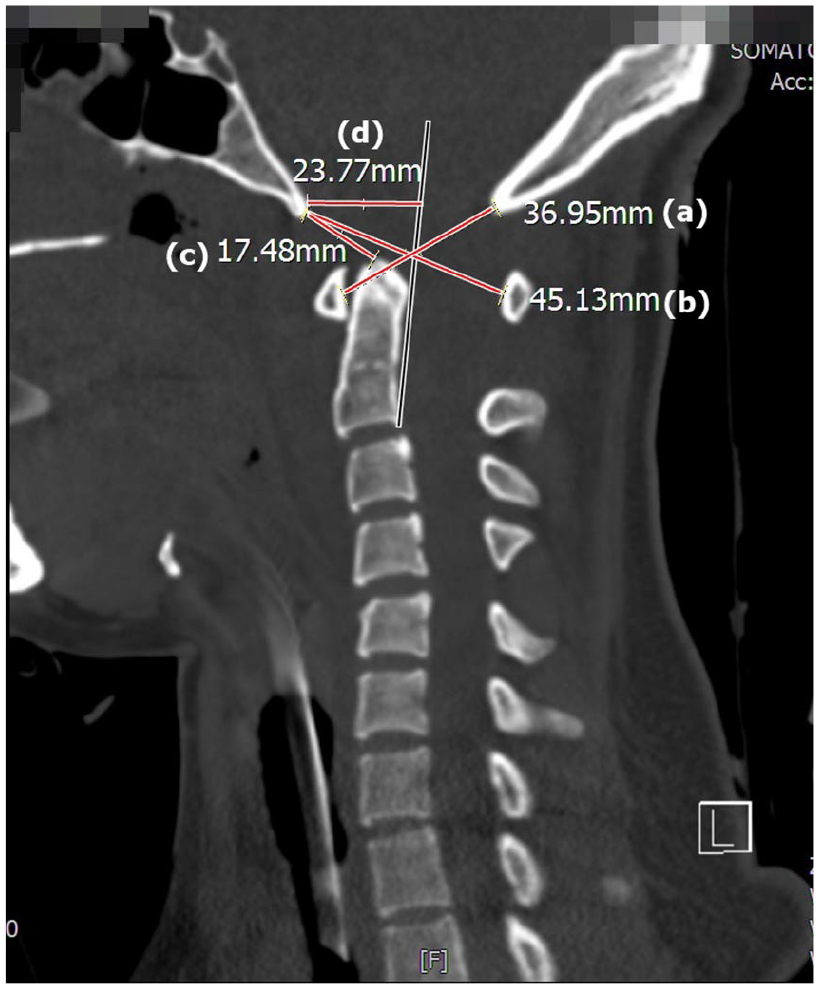
Assessment of this case: Power’s ratio (i.e. (b)/(a)) is greater than 1, Basion–dens interval (c) is greater than 10 mm, and Harris method (d) is greater than 12 mm.
Discussion
AOD is a highly unstable craniocervical injury, resulting from damage to ligaments with or without bony structures connecting the skull to the cervical spine. 1 Traumatic AOD is associated with a high mortality rate and devastating neurologic morbidity, so it was once thought to be uniformly fatal. 2 However, recent studies and case reports have demonstrated increased numbers of survivors with improved neurologic outcomes, which is attributed to advancements in prehospital care, field resuscitation, cervical immobilization, and rapid transport to a trauma center. 3 Missed or delayed diagnosis of traumatic AOD is relatively common and is associated with worsening neurologic function and outcome. 4 Emergency physicians should have a high suspicion of the diagnosis of AOD in patients presenting with shock, mental change, and motor weakness after a blunt, high-energy injury. In such cases, cervical immobilization and cervical CT scan should be considered for early diagnosis.
Footnotes
Author contributions
Y.P. and B.Y. had full access to all the data and drafted the manuscript. G.L. and J.L. participated in the study design.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
Data and materials can be made available to the public through direct requests to the corresponding author.
Ethical approval
The study procedures were in accordance with ethical standards.
Human rights
The study protocol conforms to the ethical guidelines of the 1975 Declaration of Helsinki.
Informed consent
Written informed consent was obtained from each patient included in the study.
