Abstract
Introduction:
Orbital subcutaneous emphysema after trauma has been carefully reported, but its development in the absence of trauma is rare.
Case presentation:
We report on a 70-year-old patient who developed unilateral orbital subcutaneous emphysema, mimicking lacrimal duct occlusion, after this man sneezed, and presented with right crepitant eyelid swelling and progressive ptosis. Orbital subcutaneous emphysema develops when air can get into the periorbital soft tissue, which presents as a result of facial bone trauma, iatrogenic procedures, and gas-forming infectious microorganisms, as seen in many published articles. It is very uncommon to see this kind of case report after sneezing; however, in our case, spontaneous orbital subcutaneous emphysema occurred after sneezing that resolved slowly after a few weeks without surgical intervention. Our patient denied any painful sensation over the right orbital area, including no visual problems with the right eye but right eyeball limited movements. It can be stressful to patients due to its symptoms but is not a true emergency.
Conclusion:
In this article, we should bring awareness to physicians of the possibility of a spontaneously orbital subcutaneous emphysema with complications after sneezing, yielding relevant information for patients to be informed about avoid excessive nose blowing or occluding the nose, creating controlled symptoms.
Introduction
Without any ocular trauma history or previous orbital surgery, orbital emphysema is a rare condition, which may progress and cause serious temporary or permanent visual loss due to orbital compartment syndrome which may cause a compressive or ischemic optic neuropathy. 1 It may cause patient’s anxiety due to these symptoms at emergency department (ER). Orbital emphysema is defined as abnormal presence of air in the orbit that is often caused by traumatic orbital wall fracture, an orbital abscess secondary to gas-forming pathogen organisms, obvious cutaneous or conjunctival lacerations, and rarely a pneumatocele rupture, as seen in several published articles.2–4 Sneezing is an involuntary reflex in daily life that coincides with a sudden, harsh, and boisterous expulsion of air through the nose and mouth. There are rare complications that can be caused by sneezing and nose blowing. On the other hand, retrobulbar hematoma, eyelid swelling, and orbital emphysema with accompanying exophthalmos after nasal or orbital traumatic injury was noted in one article. 5 We present a case of orbital subcutaneous emphysema after sneezing, with the patient complaining of right-sided periorbital painless swelling and right eyelid ptosis, mimicking lacrimal duct obstruction. After supportive treatment, the patient improved the next day. This article creates physician awareness about the possibility of orbital subcutaneous emphysema with related complications after sneezing and informs the patient to avoid excessive nose blowing and to avoid occluding the nose.
Case report
A 70-year-old man with a history of diabetes and hypertension was brought to the ER with complaints of painless right-sided periorbital swelling and right eyelid ptosis that began 2 h earlier after continuous sneezing. Physical examination showed that he was afebrile and his right eyelid had ptosis, with severe swelling over the right periorbital region (Figure 1). His right eyeball movements were extremely restricted on the right side, preserved visual acuity, and no orbital pain. No warmth or erythema over right periorbital and right face regions was noted, but palpable crepitus was seen over the maxillary and temporal region of his face. He denied past history of trauma, upper respiratory tract infection, difficulty with vision, double vision, and recent fever and chills. But he complained of epiphora recently. Our initial impression of this patient was suspected lacrimal duct obstruction; however, due to a progressive swelling and redness over right periorbital and right face regions later, radiographs were arranged for further evaluation. Waters’ view had no obvious signs of orbital bone fracture, except for a radiolucent finding over the upper orbital areas (Figure 2). Since lacrimal duct obstruction of the right orbit was suspected, we consulted with an ophthalmologist. Computed tomography (CT) of the orbits was arranged due to this concern. It revealed emphysematous change over the right orbital cavity, the periorbital cavity, and the infratemporal fossa region (Figure 3). The left orbit and its contents were normal. Closer review of the CT films also revealed a fracture of the right lamina papyracea (Figure 4). After detailed ophthalmologic examinations, there was no sign of intraorbital compression, and the patient was discharged with a prescription for sulfamethoxazole eye drops and was referred to outpatient follow-up suggested by ophthalmologist. Because of the patient’s forceful sneezing, which may have caused right lamina papyracea fracture, we were concerned about orbital subcutaneous emphysema. The symptoms of the patient were improved on next day, and he was educated to avoid excessive nose blowing and to avoid occluding the nose. The emphysema resolved over a few weeks without surgical intervention, as the patient denied painful sensation or any discomfort sensation over the right orbital area at ophthalmological outpatient department.
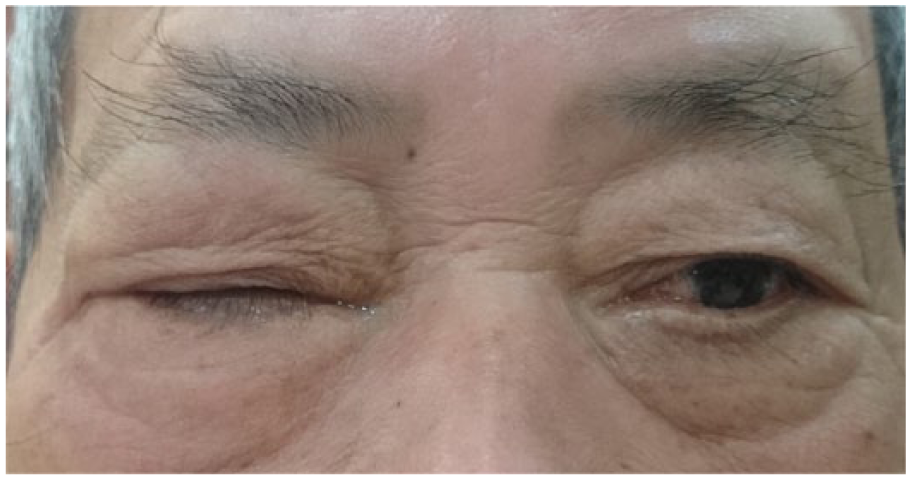
On physical examination, the patient was afebrile and his right eyelid showed ptosis, with severe swelling over the right periorbital region.
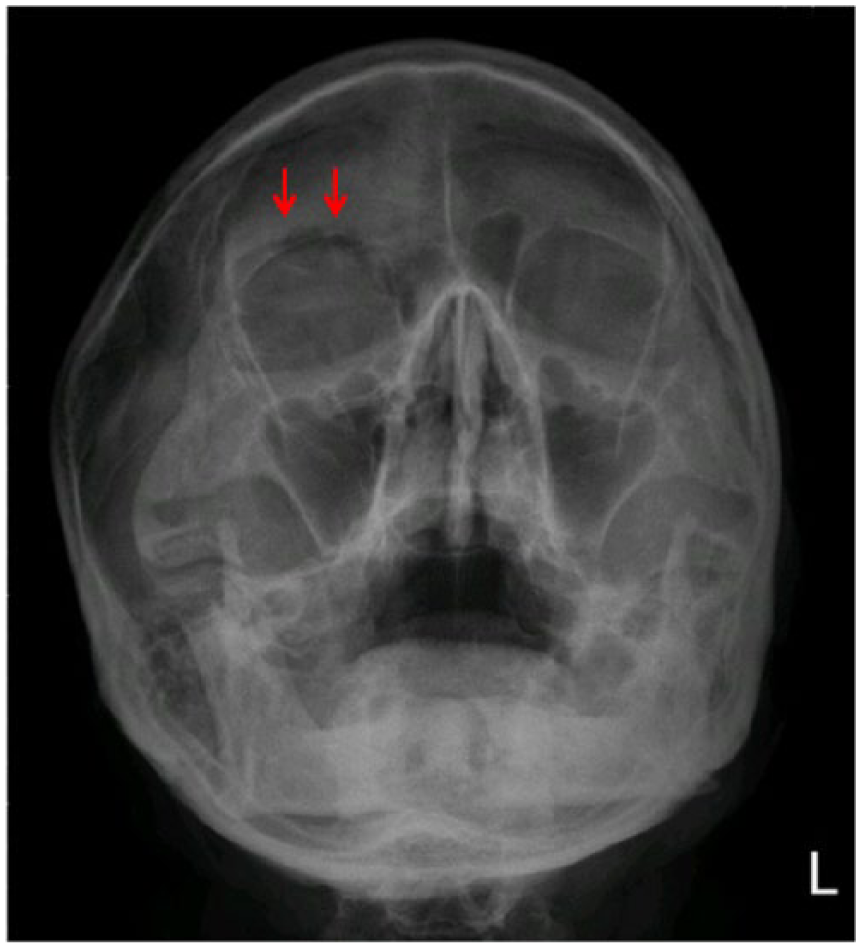
Waters’ view had no obvious orbital bone fracture, except for a radiolucent finding over the upper orbital areas (red arrows).
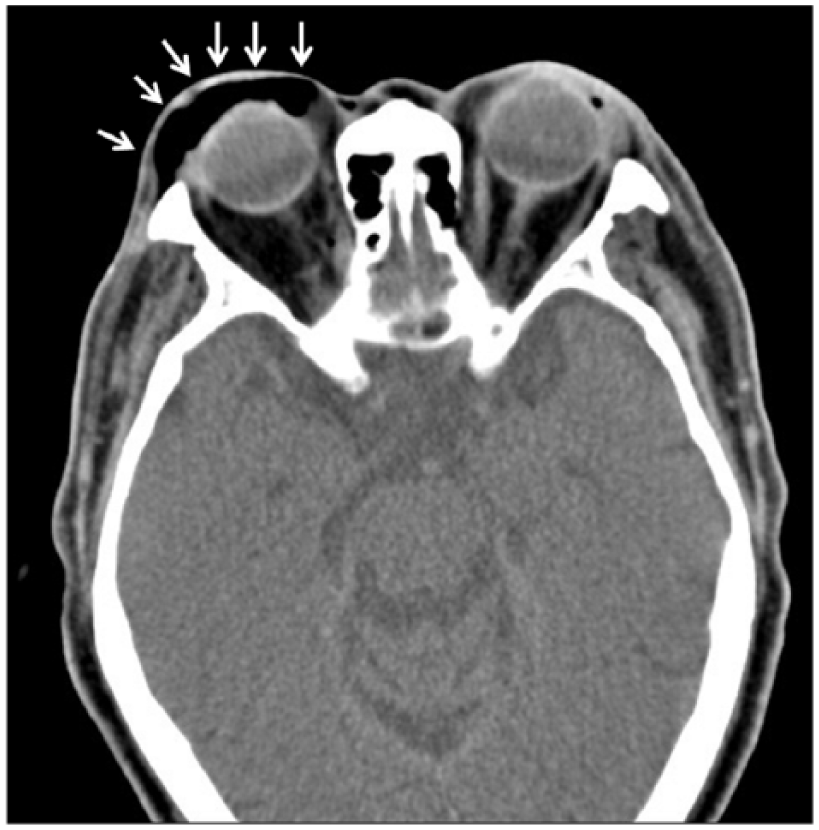
Follow-up CT of the orbits revealed emphysematous change over the right orbital cavity, periorbital cavity, and the infratemporal fossa region (white arrows).
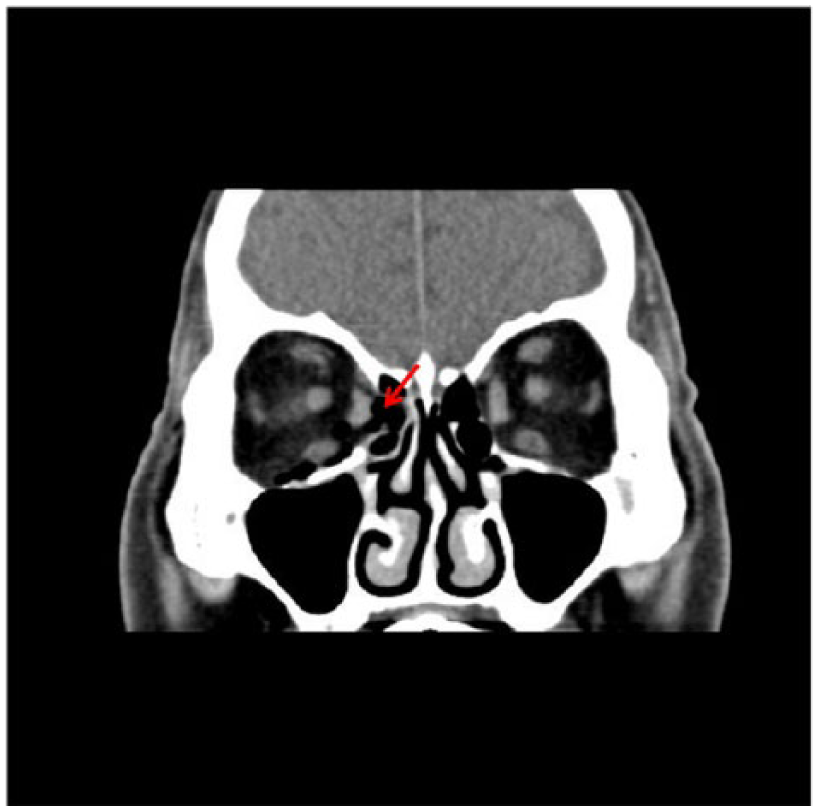
CT showed a fracture of the right lamina papyracea (red arrow).
Discussion
Sneezing is a common involuntary reflex in daily life, which is accelerated with boisterous expulsion of air through the respiratory tract. Rapidly increased intranasal pressure while sneezing may produce complications like epistaxis, headache, cerebrovascular accident, transient hemiparesis, myocardial infarction, rupture of existing aortic aneurysm, and pneumomediastinum. A rare ophthalmic complication is acute angle closure glaucoma and pneumatocele of the lacrimal sac, as reported. 5 Orbital subcutaneous emphysema can also occur and usually presents as a benign disease, which can resolve without any medication, unless complicated with severe visual loss, positive afferent pupillary defect, corneal edema, a pale optic nerve head, or secondary to rapidly increased intraocular pressure.6,7 Orbital subcutaneous emphysema is usually seen in association with medial orbital wall fractures after blunt trauma. Less commonly, it can occur spontaneously after violent sneezing, coughing, or nose blowing;6,8,9 secondary to compressed air injuries; it may also be associated with bacterial infections of the orbit. 10 Diagnosis can be made based on the history and physical examination, with further orbital CT to confirm intraorbital air with defects in the orbital bone. Management of orbital emphysema associated with fractures or trauma includes prophylactic oral antibiotics with nasal decongestants, as well as to avoid further nose blowing, a protocol for the management of orbital emphysema was suggested by Hunts et al. 11 in 1994. Regular follow-up without medication and a recommendation to avoid nose blowing may be useful for mild symptoms. On the other hand, surgical intervention for direct decompression and air drainage via a needle can be done in the ER if necessary. 3 In some cases, observation and regular follow-up are required. If the orbital air is absorbed, surgical intervention may be unnecessary (unless the patient has significant progressive discomfort, in which case orbital needle decompression with a syringe may be necessary). If vision loss occurs, performing emergency orbital CT to identify localization of the air mass is critical. Needle decompression with a syringe can be done immediately, which has also been described by Linberg 12 as a procedure for orbital emphysema with potential complications such as scleral perforation, retrobulbar hemorrhage, and optic nerve damage. If ischemic damage to the optic nerve occurs, it can be prevented by intravenous steroid administration. If vision loss is severe (absence of light perception), surgical decompression is suggested. 11 This patient had epiphora and palpable crepitus over the maxillary and temporal region of the face, when lacrimal duct obstruction should be considered. However, this patient presented progressive swelling and redness over right face later. Orbital CT was an imaging modality of choice in the evaluation of orbital subcutaneous emphysema. Slavsky et al. 13 presented orbital emphysema secondary to ethmoidal fracture, which is often seen after trauma with orbital cellulitis in children; it resolves after 4 days of outpatient treatment without surgical intervention. Rapid orbital subcutaneous emphysema is caused by forceful sneezing, due to increased intranasal pressure, which can lead to dehiscence of the lamina papyracea. 7 It sometimes causes bacterial infections in the orbit and severe ophthalmic complications, requiring further surgical intervention. 11 In rare cases, patients have been reported to develop retinal artery compression or compressive optic neuropathy through orbital emphysema. 13 In conclusion, sneezing may cause orbital subcutaneous emphysema due to dehiscence of the lamina papyracea, which is important to quickly recognize and treat in order to avoid permanent visual loss. Regular follow-up with or without medication is considered in cases with mild symptoms. Early needle decompression may be required for progressive symptoms with severe visual loss, although surgical intervention or antibiotics may also be considered, given the severity of the disease. In our case, spontaneous orbital subcutaneous emphysema mimicking lacrimal duct obstruction occurred after sneezing that slowly resolved over several weeks without surgical intervention. Our patient denied painful sensation over the right orbital area or any visual issues with the right eye. This can still be stressful to patients, given their symptoms; however, as stated earlier, it is not a true emergency.
Footnotes
Acknowledgements
The authors would like to thank our department colleagues and the devotion of this patient. H-Y.C. and H.P.C. made a substantial contribution to the concept or design of the work; C-F.L., C-C.Y, N-J.P. made a substantial contribution to acquisition, analysis, or interpretation of data. H-Y.C. and H.P.C. drafted the article or revised it critically for important intellectual content. H-Y.C. and H.P.C. approved the version to be published. Each author should have participated sufficiently in the work to take public responsibility for appropriate portions of the content: Yes.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
All data and materials can be found at clinical imaging system of our hospital and comply with corresponding regulations.
Ethical approval
This case report complies with hospital and journal regulations for publication.
Human rights
Anonymized patient information to be published in this article and we also carefully read the regulations of human right on submission guideline of Hong Kong Journal of Emergency Medicine.
Informed consent
Written informed consent was obtained from a legally authorized representative(s) for anonymized patient information to be published in this article. Patient gave written informed consent for publication and agreed the photography from his face.
