Abstract
Objective
To evaluate the use of monochromatic and polychromatic dual-energy spectral computed tomography (CT) imaging for preoperative assessment of gastric vascular anatomy.
Methods
Patients with suspected gastric cancer underwent spectral CT to generate conventional 140 kVp polychromatic and monochromatic images with energy levels ranging from 40 to 140 keV during the late arterial and portal venous phases. Optimal monochromatic images were selected according to the contrast-to-noise ratio (CNR) for the gastric artery. Image quality was subjectively assessed. Display rates of the arteries were recorded.
Results
The study included 64 patients. Monochromatic images at 53 ± 3 keV provided the optimum CNR. At this energy level, subjective image scores were significantly higher for monochromatic images than polychromatic images. There were no significant differences in the display rates of arteries between polychromatic and optimal monochromatic images.
Conclusions
Monochromatic images obtained with spectral CT can improve the visualization of gastric arteries.
Keywords
Introduction
Gastric cancer is one of the most common cancers worldwide. It accounts for approximately 8% of new cancers, with an incidence of 989 600 and mortality rate of 738 000 per year. 1 Careful determination of each patient’s anatomy before gastric cancer surgery is essential due to the complex branching patterns and morphology of gastric blood vessels. 2 Accurate identification of feeding arteries, vascular invasion and artery variation is essential to avoid vascular injury, and minimize bleeding and the duration of surgery. 2
Computed tomography angiography (CTA) is a minimally invasive procedure for observing vascular structures. Multi-detector computed tomography (MDCT) angiography is routinely used for diagnosis and management of patients with abdominal aortic aneurysms3,4 and other vascular pathologies and tumours.5–9 MDCT allows visualization of gastric tumours 10 and assessment of stereoscopic vessel anatomy, 11 exposing the organs involved from any viewpoint. The display rate of larger diameter arteries (e.g. the left gastric artery [LGA] and right gastroepiploic artery [RGEA]) approaches 100%, but those of smaller diameter arteries (e.g. the right gastric artery [RGA], left gastroepiploic artery [LGEA], short gastric artery [SGA] and posterior gastric artery [PGA]) are lower. 12 Spectral CT allows the reconstruction of conventional polychromatic images corresponding to 140 kVp, as well as monochromatic images with energies ranging from 40 to 140 keV. This procedure also reduces beam-hardening artefacts and optimizes contrast via selectable monochromatic energy (keV).13–15
The potential benefits of spectral CT include increased vessel attenuation at lower energies.16,17 The aims of this study, therefore, were to evaluate the use of spectral CT for improving image quality, and to select the optimal single energy level that provides the best contrast-to-noise ratio (CNR) for displaying gastric arteries.
Patients and methods
Study population
The study recruited patients with suspected gastric cancer undergoing CT at the Department of Radiology, First Affiliated Hospital of Zhengzhou University, Zhengzhou, China, between May 2011 and December 2011. Inclusion criteria were: (i) MDCT performed within 14 days before gastrectomy (if required); (ii) no preoperative treatment. Patients with iodine allergy or cardiac, renal or hepatic insufficiency were excluded. Diagnosis was confirmed by biopsy or surgery. The study was conducted in accordance with the Declaration of Helsinki and was approved by the ethics committee of Zhengzhou University, Zhengzhou, China. Written informed consent was obtained from all participants.
Computed tomography
Patients were required to fast for a minimum of 5 h prior to CT examination. At 10 min before CT, patients drank 1 l of water and received 20 mg scopolamine intramuscular injection to minimize peristaltic bowel movement. Patients were then placed in the supine position.
Selecting the optimal contrast-to-noise ratio (CNR) in monochromatic computed tomography angiography of the gastric artery. (A) Axial image showing regions of interest (arrows) at the base of the coeliac trunk and normal gastric wall. (B) GSI Viewer analysis indicating that optimal CNR was achieved at 53 keV.
Dual-phase contrast-enhanced scans were performed using the dual-energy spectral CT mode with a single tube, rapid, dual kVp (80 and 140 kVp) switching technique on a high-definition scanner (Discovery CT 750HD; GE Healthcare, Little Chalfont, UK). The scan encompassed the region from the top of the liver to the lower sides of both kidneys. Imaging parameters were: collimation thickness, 0.625 mm; acquisition slice thickness, 1.25 mm; tube current, 600 mA; rotation speed (gantry rotation time), 0.6 s; and helical pitch, 0.984 : 1. Patients then received 1.5 ml/kg non-ionic contrast medium (Optiray™ 320; Tyco Healthcare, Neuhausen am Rheinfall, Switzerland) intravenous injection at a rate of 3–4 ml/s (total volume 90–120 ml) during the arterial and portal venous phases. The arterial phase imaging delay was determined by the automated image-triggering software (SmartPrep; GE Healthcare), and arterial phase imaging automatically began 12 s after the trigger attenuation threshold (100 HU) reached the level of the supracoeliac abdominal aorta. Portal venous phase imaging began 30 s after the arterial phase imaging.
Image analysis
An abdominal radiologist (Y.W.) used a spectral imaging viewer (GSI Viewer; GE Healthcare) to review polychromatic image sets corresponding to conventional 140 kVp imaging, and monochromatic image sets corresponding to photon energies ranging from 40 to 140 keV. The arterial phase was used for analysis.
The gastric artery CNR was determined using both the polychromatic and monochromatic axial images. To obtain the optimal keV images, circular regions of interest were placed on the base of the coeliac trunk and the gastric wall of the same slice (Figure 1A).
The GSI Viewer automatically calculated and displayed the CNR values for the real-time monochromatic images. The optimal monochromatic level for generating the best CNR between the gastric artery and the gastric wall was selected from the CNR plot. Regions of interest were placed on the base of the coeliac trunk, the gastric wall and the subcutaneous fat tissue in the abdomen of the same slice to measure the CT value in both the optimal monochromatic images and the 140 kVp polychromatic images. The attenuation values were obtained in a manually defined 1–2 cm2 region of interest (ROI). Images were magnified, and care was taken to avoid calcified areas. The ROI was maintained to be as large as possible. CNR was defined as: ROIo − ROId)/SDn, where ROIo is the CT value of the base of the coeliac trunk, ROId is the CT value of the gastric wall of the same slice and SDn is the standard deviation of the subcutaneous fat tissue in the abdomen of the same slice. 18 Final ROI values were the mean of three independent measurements.
Overall subjective image quality was independently assessed by two investigators (J.G. and Y.W.) using volume rendering and thin slice maximum intensity projection. Disagreement was resolved by consensus. The rate of display of the LGA, RGA, LGEA, RGEA, SGA and PGA were recorded. Subjective image quality was evaluated using a five-point scale based on artery visualization and image noise: 5, excellent (arteries were clearly visible and the margins were sharp, no obvious image noise or artefacts); 4, superior (the arterial stem was clearly visible but the end was blurred, mild image noise or artefacts); 3, diagnostic (arteries were light, moderate image noise or artefacts, optimal enhancement but insufficient for accurate diagnosis); 2, suboptimal (only the distribution of the arteries was recognised, severe image noise or artefacts, inadequate for diagnosis); and 1, poor (vessels not seen, severe image noise and artefacts, no diagnosis possible) (Figure 2).
Subjective evaluation of computed tomography angiography of a patient with chronic gastritis. (A) Conventional polychromatic imaging, and (B) monochromatic imaging. The left gastroepiploic artery (LGEA) was more clearly visible in (B) than in (A) (subjective image scores 4 and 3, respectively). The subjective scores of the left gastric artery (LGA), right gastric artery (RGA), right gastroepiploic artery (RGEA) and splenic artery (SA) were 5 in the monochromatic image (B) and 4 in the conventional polychromatic image (A).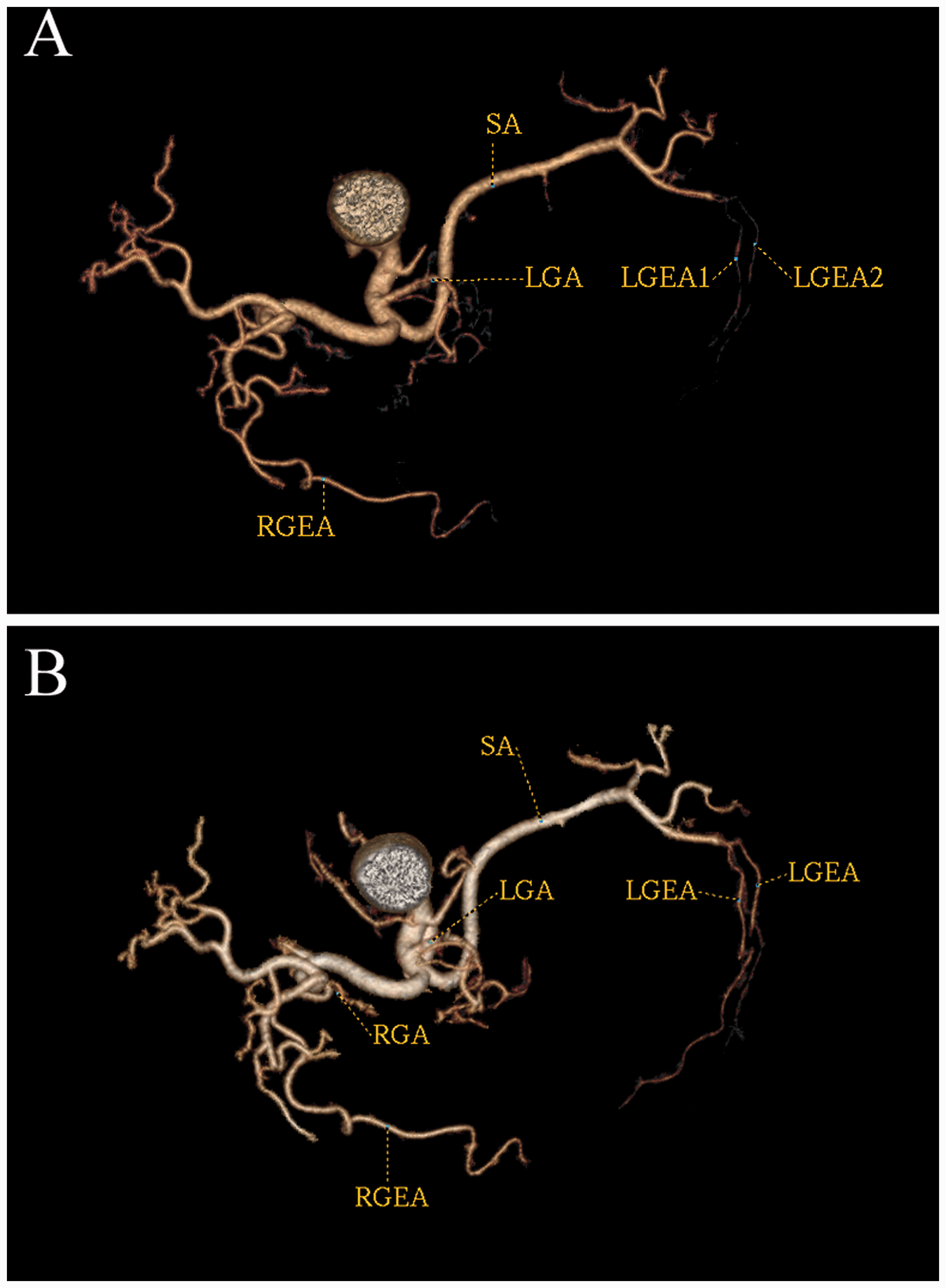
Statistical analyses
Data were presented as mean ± SD or n (%). CT values of the coeliac trunk were compared using paired t-test, and subjective scores were compared using paired t-test. Fisher’s exact probability test was used to compare the rates of display of gastric arteries on volume rendering from the optimal monochromatic and polychromatic images. All statistical calculations were performed using SPSS® version 13.0 (SPSS Inc., Chicago, IL, USA) for Windows®. P-values < 0.05 were considered statistically significant.
Results
The study recruited 64 patients with suspected gastric cancer (46 male/18 female; mean age 61.2 years (range 27 to 79 years). A total of 45 patients had gastric cancer, nine had gastrointestinal stromal tumours, six had gastric lymphoma and four had chronic gastritis.
Subjective image scores of optimal monochromatic (53 keV) gastric arterial computed tomography angiography (CTA) and polychromatic (140 kVp) gastric arterial CTA in patients with suspected gastric cancer (n = 64).
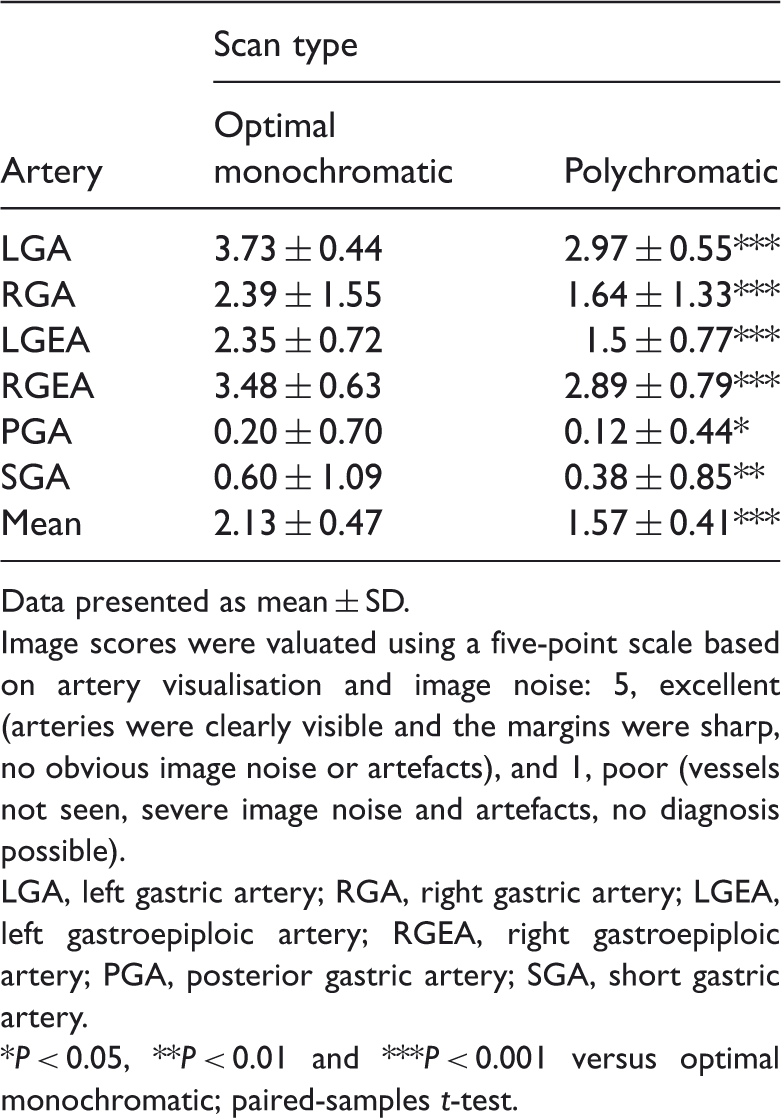
Data presented as mean ± SD.
Image scores were valuated using a five-point scale based on artery visualisation and image noise: 5, excellent (arteries were clearly visible and the margins were sharp, no obvious image noise or artefacts), and 1, poor (vessels not seen, severe image noise and artefacts, no diagnosis possible).
LGA, left gastric artery; RGA, right gastric artery; LGEA, left gastroepiploic artery; RGEA, right gastroepiploic artery; PGA, posterior gastric artery; SGA, short gastric artery.
P < 0.05, **P < 0.01 and ***P < 0.001 versus optimal monochromatic; paired-samples t-test.
Table 2 shows data regarding mean CT values, CNRs and image noise of the coeliac trunk. All parameters were significantly higher in optimal monochromatic imaging than polychromatic imaging (P < 0.001 for each comparison; Table 2). Optimal monochromatic imaging allowed the visualization of smaller vessels than was possible with polychromatic imaging (Figure 3).
Computed tomography angiography of a 73-year-old man with gastric carcinoma. Optimal monochromatic imaging at 53 keV (B) allowed the visualization of smaller vessels than was possible with polychromatic imaging (A). LGA, left gastric artery; RHA, right hepatic artery; SMA, superior mesenteric artery. Computed tomography parameters in optimal monochromatic (53 keV) gastric arterial computed tomography angiography (CTA) and polychromatic (140 kVp) gastric arterial CTA in patients with suspected gastric cancer (n = 64). Data presented as mean ± SD. CNR, contrast-to-noise ratio. P < 0.001 versus optimal monochromatic; paired-samples t-test.
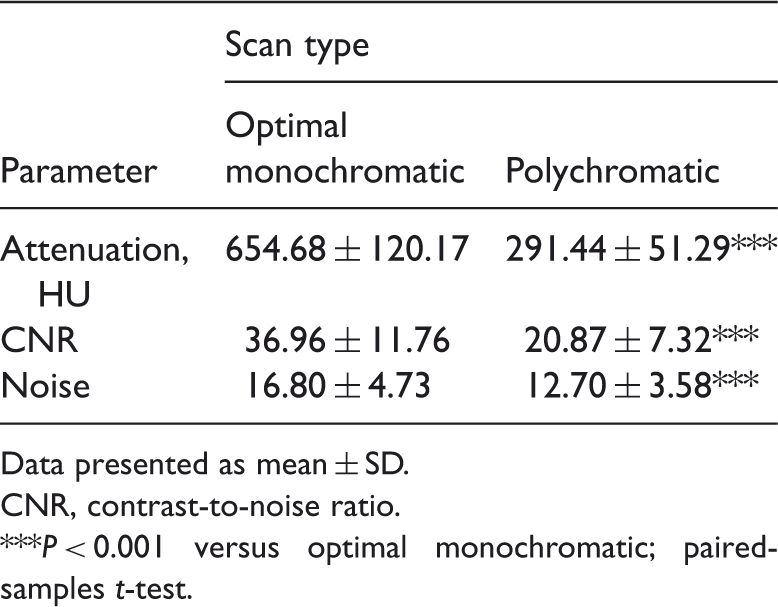
There were no significant differences in the display rates of any artery on volume rendering (VR) images generated using optimal monochromatic or polychromatic modes (Table 3 and Figure 4).
Volume rendering computed tomography angiography of a 62-year-old male patient with gastric carcinoma indicating similar artery visualization in both (A) polychromatic image and (B) optimal monochromatic image at 53 keV. CHA, common hepatic artery; GDA, gastroduodenal artery; LGA, left gastric artery; LGEA, left gastroepiploic artery; PHA, proper hepatic artery; RGA, right gastric artery; RGEA, right gastroepiploic artery; SA, splenic artery. Rate of display of gastric arteries in optimal monochromatic (53 keV) gastric arterial computed tomography angiography (CTA) and polychromatic (140 kVp) gastric arterial CTA in patients with suspected gastric cancer (n = 64). Data presented as n (%). LGA, left gastric artery; RGA, right gastric artery; LGEA, left gastroepiploic artery; RGEA, right gastroepiploic artery; PGA, posterior gastric artery; SGA, short gastric artery. No statistically significant differences (P ≥ 0.05; Fisher’s exact probability test).

Discussion
Dual-energy CT (DECT) and spectral CT extend the capabilities of conventional CT and provide additional tools for vascular analysis.19–21 The single tube, rapid dual-tube voltage switching technique of CT spectral imaging provides monochromatic images that depict how an imaged object would appear if the X-ray source produced single energy X-ray photons, resulting in high contrast resolution. 14 DECT imaging at 70 keV has been shown to yield lower noise and higher image quality than conventional CT. 19 In addition, image quality and CNR of intra- and extrahepatic portal veins were improved with spectral CT imaging at 51 keV. 13
The optimal energy for gastric artery CNR was approximately 53 keV in the present study. Optimal monochromatic scanning resulted in significantly better vascular opacification than that seen with polychromatic imaging, as determined by subjective image analysis. The utility of CTA is largely determined by CNR. Although image noise was significantly higher in optimal monochromatic scanning than polychromatic mode in the current study, the monochromatic images had significantly higher subjective scores. This may be due to higher intravascular attenuation, and introduces the possibility of performing vascular studies using DECT with lower contrast medium and iodine dose. The current observations were similar to those of others. 22
The rates of display of LGEA, RGA and SGA were slightly higher in optimal monochromatic images than polychromatic images in the present study, but these differences were not statistically significant. The present study found that DECT allowed radiologists to select an optimal imaging plane to accurately evaluate the gastric arteries. In addition, the use of a monochromatic X-ray beam reduces beam-hardening artefacts and attenuation effects commonly seen in conventional CT scans with polychromatic X-ray beams. 23 Studies have indicated an optimal monochromatic energy of 72 ± 5 keV for gastric cancers. 24 Thus, a combination of images at approximately 50 and 70 keV could fulfil the dual objectives of higher contrast for vascular imaging and lower noise for evaluating gastric lesions. The use of different energies of spectral CT may contribute to more accurate evaluation, particularly when contrast enhancement is poor. 17 DECT may provide new opportunities for detailed preoperative evaluation of gastric morphology and the vascularity of primary lesions. This finding may lead to opportunities for reducing radiation dose in the future.
This study had several notable limitations. First, this investigation was a preliminary study with a relatively small number of patients, and further prospective clinical trials are required to validate our results. Secondly, one region of interest was placed on the base of the coeliac trunk instead of the gastric artery. This had no effect on the results, however, since the attenuation of the arteries was >150 HU and there is little distinction between the coeliac trunk and gastric artery at >150 HU. Finally, this study did not investigate gastric veins, but further studies are currently underway.
In conclusion, monochromatic images obtained with spectral CT can enhance the attenuation of iodine contrast media at certain energy levels. These monochromatic images can improve the visualization of gastric arteries.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflict of interests.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
