Abstract
Objectives
This study compared outcomes of primary repair and palmaris longus tendon reconstruction in patients with lateral ulnar collateral ligament (LUCL) injuries.
Material and Method
A retrospective comparative cohort study was conducted between 2017 and 2023, including 40 patients who underwent surgery for elbow dislocation or fracture–dislocation with intraoperatively confirmed LUCL injury. Surgical choice was made intraoperatively: repair was performed if the ligament could be reattached without tension, while reconstruction was selected if the tissue was shortened, retracted, or degenerative. Patients were divided into a repair group (n = 17) and a reconstruction group (n = 23). Clinical outcomes included Visual Analog Scale (VAS), Quick Disabilities of the Arm, Shoulder and Hand (QuickDASH), Mayo Elbow Performance Score (MEPS), range of motion (ROM), fracture healing, and complications, with a mean follow-up of 26.4 months.
Results
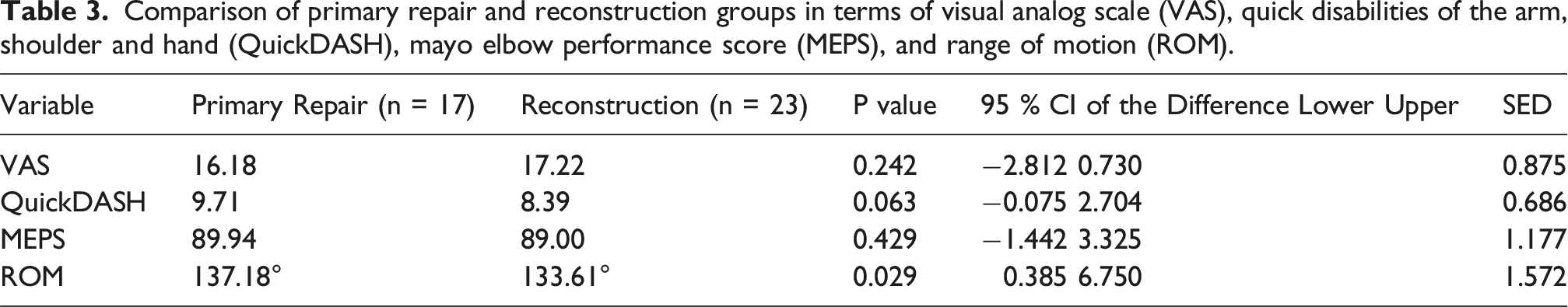
The repair group showed mean VAS 16.2, QuickDASH 9.7, MEPS 89.9, and ROM 137.2°, while the reconstruction group had VAS 17.2, QuickDASH 8.4, MEPS 89.0, and ROM 133.6°. There were no significant differences in VAS, QuickDASH, or MEPS, though the repair group demonstrated superior ROM (p = 0.029). The absolute ROM difference (∼3–4°) was not considered clinically meaningful. In isolated LUCL cases (n = 15), no significant differences were observed between groups. All associated fractures achieved union without non-union or malunion. Complications included heterotopic ossification in seven patients (three repairs, four reconstructions) and two superficial infections, all successfully managed without reoperation. No patient developed recurrent instability, nerve deficits, or clinically significant stiffness.
Conclusion
Both primary repair and palmaris longus tendon reconstruction provided satisfactory outcomes and durable stability. Although the repair group showed slightly greater ROM, this difference was not clinically relevant and disappeared when patients with concomitant fractures were excluded. Injury complexity, rather than surgical technique, appears to be the main determinant of long-term function.
Keywords
Introduction
The elbow is the second most frequently dislocated major joint in adults, and post-traumatic instability is a common sequela.1–3 Stability depends on both static and dynamic structures, among which the lateral ulnar collateral ligament (LUCL) plays a critical role.4–6 Injury to the LUCL is the principal lesion underlying posterolateral rotatory instability (PLRI), which, if left untreated, can lead to chronic pain, recurrent subluxation, and post-traumatic osteoarthritis.7–10
In acute traumatic settings, direct repair of the LUCL can often restore stability when the ligament is avulsed but of sufficient quality to allow reattachment.11–13 In contrast, reconstruction becomes necessary in cases where the tissue is shortened, retracted, or degenerative, rendering repair unreliable.14,15 Although both strategies are widely described, few studies have directly compared outcomes of acute primary repair and tendon reconstruction under similar clinical conditions.16–18
The palmaris longus tendon was selected for reconstruction in this study because of its proximity to the surgical field, appropriate thickness and length for reproducing the LUCL, low donor-site morbidity, and ease of harvest with a short learning curve. 19 These advantages make it a practical and reliable graft option, particularly in the trauma setting.
We hypothesized that, when performed in the acute setting, primary LUCL repair would provide functional outcomes comparable to palmaris tendon reconstruction, with superior range of motion due to preservation of native ligament tissue.
Materials and methods
Study design and ethical approval
This retrospective comparative cohort study was conducted at a single tertiary referral center between January 2017 and December 2023. Ethical approval was obtained from the institutional review board (Approval No: 504, 19 June 2025), and the study was carried out in accordance with the Declaration of Helsinki.
Patient selection
Patients who underwent surgery for elbow dislocation or fracture-dislocation with confirmed LUCL injury were eligible. Exclusion criteria included age <18 or >65, concomitant medial ulnar collateral ligament injury, follow-up <12 months, systemic infection, or incomplete data.
Diagnosis of LUCL injury
Preoperatively, standard radiographs and CT scans were performed in all patients to evaluate associated osseous injuries. MRI was obtained selectively when soft-tissue injury was suspected but not confirmed radiographically. The definitive diagnosis of LUCL injury was established intraoperatively, defined as avulsion of the ligament from its humeral origin at the lateral epicondyle, with or without associated tissue disruption.
Preoperative management and surgical timing
While awaiting surgery, all patients were managed with a long-arm splint for pain control and to maintain joint stability. No patient received physiotherapy or invasive intervention before definitive surgery. All surgeries were performed within 6 weeks of injury. In general, patients in the repair group underwent earlier intervention (median interval shorter), whereas patients requiring reconstruction had slightly longer delays, often due to concomitant injuries, advanced imaging requirements, or soft-tissue considerations.
Surgical decision-making
After completion of osseous fixation, intraoperative varus stress and pivot-shift testing were performed to evaluate lateral opening and posterolateral rotatory instability. If the ligament could be mobilized and approximated to its anatomic footprint without undue tension,
Surgical techniques
• Primary Repair: The avulsed ligament was mobilized from surrounding soft tissue and reattached to the lateral epicondyle at its anatomic footprint using a 3.0 mm bioabsorbable suture anchor. The repair was reinforced with non-absorbable sutures as necessary. • Palmaris Longus Tendon Reconstruction: Upon confirmation of LUCL injury during surgery and after bone fixation was completed, palmaris longus tendon harvesting was initiated. A 2 cm transverse incision was made at the wrist to access the tendon, and a tendon stripper was used to obtain a graft measuring approximately 16–20 cm. For preparation of the ulnar tunnel, a 3 cm incision was made at the level of the radial neck. The first bone tunnel was drilled using a 2.2 mm drill bit just proximal to the radial crest. A second tunnel was drilled 1.5 cm proximal and slightly posterior to the first preserving a bone bridge between them. Subsequently, the humeral tunnel was prepared. An isometric point on the lateral epicondyle was identified, and a 3.0 mm bioabsorbable knotless anchor (Smith & Nephew) was placed. The palmaris longus tendon, folded in half, was passed through the tunnels and fixed to the lateral condyle using the anchor. Upon completing the reconstruction, the elbow stability of all patients was evaluated intraoperatively using the pivot shift and posterolateral rotatory drawer tests, and the procedure was finalized once no instability was detected (Figure 1).
Schematic illustration demonstrating LUCL reconstruction.
Surgical team
All procedures were performed by two fellowship-trained orthopedic trauma surgeons with comparable experience in elbow ligament reconstruction.
Postoperative rehabilitation
All patients were immobilized in a long-arm splint for 3 weeks, followed by progressive isometric exercises and strengthening as tolerated. Varus stress was avoided for 3 months, after which unrestricted activity was allowed.
Outcome measures
Clinical outcomes included VAS, QuickDASH, MEPS, and range of motion (ROM) at final follow-up. Demographic data (age, sex, injury side) and associated fracture patterns were also recorded.
Statistical analysis
Data were analyzed using SPSS version 30.0 (SPSS Inc., Chicago, USA). Descriptive statistics were expressed as means ± standard deviation. Between-group comparisons were made using independent samples t-test for continuous variables and chi-square test for categorical variables. Adjusted analyses such as multivariable regression or propensity matching were considered; however, these were not feasible due to the limited sample size. A p-value <0.05 was considered statistically significant.
Results
Patient characteristics
Demographic characteristics of the patients.

Associated injuries and fixation methods by treatment group.

Clinical outcomes
Comparison of primary repair and reconstruction groups in terms of visual analog scale (VAS), quick disabilities of the arm, shoulder and hand (QuickDASH), mayo elbow performance score (MEPS), and range of motion (ROM).
Subgroup analysis
Assessment of VAS, QuickDASH, MEPS, and ROM in patients undergoing isolated repair or reconstruction, excluding patients with concomitant fractures.

Fracture outcomes
All associated fractures healed with radiographic union at final follow-up. No cases of non-union or clinically significant malunion were observed.
Complications
No patient developed recurrent instability, clinically significant stiffness, or postoperative nerve deficits. Superficial skin infections occurred in two patients (5%), which resolved with oral antibiotic therapy. Heterotopic ossification (HO) was observed in 3 patients in the primary repair group and 4 patients in the reconstruction group. All cases were managed with standard prophylaxis and treatment protocols, including non-steroidal anti-inflammatory drugs and supervised physiotherapy. Importantly, HO did not result in clinically relevant pain or limitation of range of motion during follow-up. No patient required reoperation for complications.
Discussion
The present study compared the outcomes of primary LUCL repair and palmaris longus tendon reconstruction in patients with traumatic elbow instability. In the overall cohort, primary repair was associated with a statistically greater range of motion at follow-up, although no significant differences were observed in pain (VAS), function (QuickDASH), or elbow performance (MEPS) scores. Importantly, subgroup analysis restricted to patients with isolated LUCL injuries demonstrated no differences between repair and reconstruction, indicating that the presence of concomitant fractures and the complexity of the injury likely play a greater role in determining postoperative motion than the surgical method itself.
These findings are consistent with previous reports that emphasize the feasibility of primary repair in acute injuries, particularly when the ligament is avulsed and tissue quality permits reattachment.12,18,20 Early repair offers the theoretical advantage of preserving native ligament tissue, minimizing surgical morbidity, and facilitating rehabilitation.14,21 However, other studies have shown that once associated fractures or chronic degenerative changes are present, reconstruction becomes necessary to restore stability.7,22,23 Our results reinforce this concept: outcomes between repair and reconstruction were broadly equivalent when comparing similar injury profiles, whereas differences emerged in the context of more complex fracture–dislocations.
The use of the palmaris longus tendon as a graft in this study also warrants emphasis. It remains one of the most frequently employed autografts for LUCL reconstruction due to its proximity to the surgical field, adequate length and diameter, ease of harvest, and minimal donor-site morbidity.7,19,24,25 These advantages make it particularly suitable in the trauma setting, where surgical time and reliability are important considerations. Our findings support its continued use as a practical and effective option for ligament reconstruction.
The clinical significance of the ROM difference observed in the overall cohort must be interpreted with caution. Although statistically significant, the magnitude of improvement (≈3–4°) is unlikely to represent a meaningful functional advantage for patients in daily activities. This aligns with other series in which differences in ROM outcomes often failed to translate into measurable improvements in function or patient-reported disability.18,26 The consistency of pain and function scores between groups in our study further supports the interpretation that both approaches yield satisfactory results in appropriately selected patients.
Complication rates were low in both groups. No patient developed recurrent instability, nerve deficits, or clinically relevant stiffness. Heterotopic ossification occurred in three patients in the repair group and four in the reconstruction group, a finding consistent with previous reports that describe HO as a frequent but often clinically silent event after elbow trauma.27–29 All cases were successfully managed with NSAID therapy and supervised physiotherapy, and none resulted in symptomatic restriction or required reoperation.
Limitations
This study has several important limitations. First, its retrospective design introduces inherent risks of selection bias and confounding by indication, since the decision to repair or reconstruct was made intraoperatively. Second, the patient population was heterogeneous, with many cases involving fracture–dislocations requiring additional fixation, which may have influenced outcomes. Although we attempted to mitigate this by performing a subgroup analysis, the number of isolated LUCL cases was small, limiting statistical power. Third, preoperative baseline functional scores were unavailable, preventing precise measurement of postoperative change. Fourth, adjusted analyses such as multivariable modeling or propensity score matching could not be performed due to limited sample size. These factors constrain the generalizability of our findings.
Conclusion
In summary, both primary repair and palmaris longus tendon reconstruction yielded satisfactory outcomes for LUCL injuries associated with elbow trauma. Although the repair group demonstrated a statistically superior ROM in the overall cohort, this difference was small, of uncertain clinical relevance, and not present when patients with associated fractures were excluded. Consequently, our findings do not support the superiority of one method over the other but rather emphasize that injury complexity is a key determinant of functional outcome. Larger prospective studies with homogeneous populations and adjusted analyses are needed to clarify the optimal treatment strategy for LUCL injuries.
Footnotes
Ethical considerations
The research was conducted in accordance with the guidelines outlined in the Declaration of Helsinki and was approved by the Local Ethics Committee. This is a Local Ethics Committee-approved retrospective study; patient data will not be shared with third parties (The study was approved by the Scientific Ethics Committee of Ankara Training and Research Hospital on 19 June 2025 with the approval number 504).
Author contributions
All authors declare that they have participated in the design, execution, and analysis of the paper, and that they have approved the final version.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that underlie the conclusions of this research are accessible from the corresponding author upon a reasonable request.
