Abstract
Objective
It aimed to explore the nursing effect of intermittent pneumatic compression pump (IPC) plus enteral nutrition support (ENS) in the prevention of deep venous thrombosis (DVT) in lower limbs of patients after orthopedic surgery (OS).
Methods
235 patients who underwent hip joint surgery between January 2021 and January 2022 were enrolled as regular group (RG, routine care plan), and 268 patients who underwent hip joint surgery between February 2022 and February 2023 were enrolled as joint group (JG, IPC combined with ENS care plan). The RG only received routine nursing, and the JG received IPC plus ENS nursing. The subjects’ coagulation indicators, DVT incidence, postoperative recovery, and other indicators were sorted out.
Results
After IPC plus ENS nursing, hemoglobin (Hb) and platelet (PLT) in the JG were visibly lower as against the RG (p < .05); As against the RG, the diameter of bilateral common femoral vein (CFV) did not decrease, and the maximum blood flow velocity (BFV) and average BFV of bilateral CFV were visibly higher in the JG (p < .05). In the JG, fibrinogen (FIB), prothrombin time (PT), activated partial thromboplastin time (APTT) were visibly increased, while D-dimer (D-D) and thrombin time (TT) were visibly decreased; the incidence of DVT was visibly lower; the immobile time in bed and hospital stay was visibly shortened, and the nursing satisfaction of patients was visibly increased (all p < .05).
Conclusion
IPC plus ENS in the nursing of patients after OS can effectively reduce the incidence of DVT and promote postoperative recovery.
Keywords
Background
Deep venous thrombosis (DVT) is a common complication of patients after orthopedic surgery (OS). This is because the postoperative patients need to stay in bed for a long time after the operation, can’t carry out activities, and reduce the contraction of lower limb muscles, resulting in slow blood flow. It may cause direct or indirect damage to the vessel wall during the operation, which provides the basis for thrombosis. 1 Previous studies have proposed that the coagulation state of patients is closely related to the occurrence of thrombosis after OS. 2 Patients in hypercoagulable state due to inflammatory reaction or other factors after OS will increase the risk of thrombosis. It has high morbidity and potential mortality risk, which seriously affects the rehabilitation and quality of life (QoL) of patients. According to the research, the risk of DVT in patients with trauma related fractures and fractures treated by surgery is visibly increased, of which 40%-60% of DVT events occur during hospitalization or within 3 months after hospitalization, and hospitalization will increase the risk of DVT3,4 Therefore, it is important to take effective preventive measures for patients after OS.
Anesthesia and surgical factors are important reasons for the occurrence of DVT. At present, the nursing methods for orthopedic patients after surgery include limb nursing, such as posture nursing and pressure ulcer nursing, prevention of complications nursing, such as prevention of postoperative pulmonary embolism, bleeding, and psychological nursing. 5 In the prevention of DVT, patients need to actively cooperate, including regular activities, wearing elastic socks, taking anticoagulant drugs. However, patients may not follow medical advice because of pain, inconvenience, or other reasons. During physical prevention, tools such as intermittent pneumatic compression pump (IPC) may reduce the effect due to improper wearing or improper use of equipment. Therefore, the current orthopedic patients’ postoperative care still needs to be continuously improved and adapted to the needs of different groups to overcome the limitations and challenges of existing preventive measures. Studies have shown that IPC can effectively promote blood circulation in the lower limbs, prevent blood stagnation, and then reduce the risk of thrombosis by regularly applying and relieving pressure on the limbs, mimicking the natural contraction of human leg muscles during walking. 6 IPC is simple to use, can reduce the workload of nurses, and is also easy for patients to accept. Studies have used IPC for external assistance in patients with lower limb ischemia, and found that it can increase the capillary flow of toes, prolong the expansion of toe capillaries, and extend the painless walking distance. 7 Enteral nutrition support (ENS) includes oral nutrition supplementation and enteral tube feeding, which maintain the structure of intestinal mucosa and the integrity of its barrier function, 8 and improve the overall nutritional status of patients, which is essential for overall health and recovery. In a study on the perioperative nursing of elderly patients with hip fracture, early enteral nutrition nursing was used, and it was found that the postoperative IL-6 level of patients was visibly reduced, and the wound healing time was visibly shortened. 9 Therefore, this article proposed that IPC and ENS should be able to prevent the formation of DVT in orthopedic patients after surgery and improve the QoL of patients. The two methods complement each other and jointly provide patients with more comprehensive nursing and preventive measures.
This article aimed to explore the effect of IPC plus ENS in the prevention of DVT in patients after OS. It provides a scientific basis for the prevention of DVT after OS, and offers effective intervention measures for clinical nursing practice, improving the postoperative outcome of patients.
Materials and methods
Subjects
Clinical data of 235 patients who underwent hip joint surgery from January 2021 to January 2022 were retrospectively collected, and they were set as the RG due to the implementation of routine postoperative nursing measures. Subsequently, clinical data of 268 patients who underwent hip joint surgery at People’s Hospital of Chongqing Liang Jiang New Area from February 2022 to February 2023 were also retrospectively collected, and they were set as the JG due to the implementation of IPC combined with ENS nursing plan postoperatively. Inclusion criteria: Patients with complete clinical data; First OS; Patients had good compliance; The patient’s coagulation function was normal; Patients with hip fracture.
Exclusion criteria: Incomplete clinical data; Patients complicated with diseases affecting coagulation function; Patients with severe ischemic disease of lower extremity vessels; Patients with lower limb deformities.
Nursing methods
Routine nursing measures were adopted in the regular group (RG): only routine anti-inflammatory and thrombosis prevention measures were taken for the participants, and the participants took aspirin orally (specification: 0.3 g, Shandong Weigao Pharmaceutical Co., Ltd., China) according to the instructions; At the 12h before the start of the operation process, the participant was injected with 0.4 mL of low molecular weight heparin (Jiangsu Wanbang Biochemical Pharmaceutical Co., Ltd., China) through the subcutaneous route. After the completion of the operation procedure and the 24-h observation period, when it was confirmed that the wound drainage volume of the participant had visibly decreased, subcutaneous injection would be carried out every 12h, and the amount of each injection remained the same as the initial dose for 10d. When participants with DVT received intravenous thrombolysis with urokinase 500 mL, 500 mL 5% glucose +8000U urokinase was used for 7d. The postoperative daily diet was a routine diet that could be applied.
IPC plus ENS nursing measures were used in the joint group (JG): while participants received standard nursing measures, IPC therapy and ENS strategy were additionally used. Use of IPC: LBTK-M-I 5005 (Dalian Labtek Science & Development Co., Ltd., China) was adopted. The patient was placed supinely on the hospital bed and was sealed with a disposable foot covering. Subsequently, the inflatable pressure device sleeve was connected to its corresponding fitting, and the initial pressure was adjusted according to the circumference of the patient’s lower limb, followed by adjustments based on the patient’s sensations. During the use of IPC, the condition of the device, the position of the tubes, the foot covering, and the pipeline were closely observed to determine whether any alarms occurred. The skin color and temperature of the patient were observed. For ENS: the dietary structure, preferences, and intake of the patient were assessed using a food frequency and a 24-h dietary survey form, and then an oral nutritional supplement plan combined with a personalized diet recipe was adopted for dietary pairing. On the basis of the conventional diet, 125g of whole protein or short peptide nutrition was taken in daily diet, one bag a day, using within 2-3 times, whey protein 10 g/time, twice a day. Participants with insufficient nutritional intake were given ENS by nasal feeding, and 400 mL of nutrient solution (diluted with 600 mL warm water) was infused every day.
Data collection
General information: Participant’s age, sex, type of operation, type of combined disease, etc.
Examination data: Blood routine, hemodynamic monitoring indicators, coagulation indicators, and the degree of lower limb swelling were collected before and after nursing, including hemoglobin (Hb) and platelet (PLT), bilateral common femoral vein (CFV) diameter, maximum blood flow velocity (BFV), and average BFV, the levels of fibrinogen (FIB), D-dimer (D-D), prothrombin time (PT), activated partial thromboplastin time (APTT), and thrombin time (TT).
The postoperative immobile time in bed, postoperative bedridden time, and the incidence of thrombosis were sorted out according to the satisfaction of participants.
The swelling degree of the affected side after nursing was counted (grade I, II, III).
Excel table was adopted to sort out the collected data.
Statistical analysis
Data were processed using the SPSS 27.0 software, with measurement data being expressed as the mean ± sd (
Results
General information
General information of subjects.

Contrast of Hb and PLT of subjects
In Figure 1, before nursing, the levels of Hb and PLT of the subjects were equivalent (p > .05). Following nursing, the levels of Hb and PLT of the subjects exhibited a noticeable decrease, with the JG demonstrating a more pronounced reduction in comparison to the RG (p < .05). Hb and PLT were measurement data, and were tested for normality using the Shapiro-Wilk test, which showed that they followed a normal distribution; comparison before and after nursing within the same group was made using the paired samples t-test (two-sided), and comparison after nursing between the two groups was made using the independent samples t-test (two-sided). Contrast of Hb and PLT of subjects. (a): Hb; (b) PLT).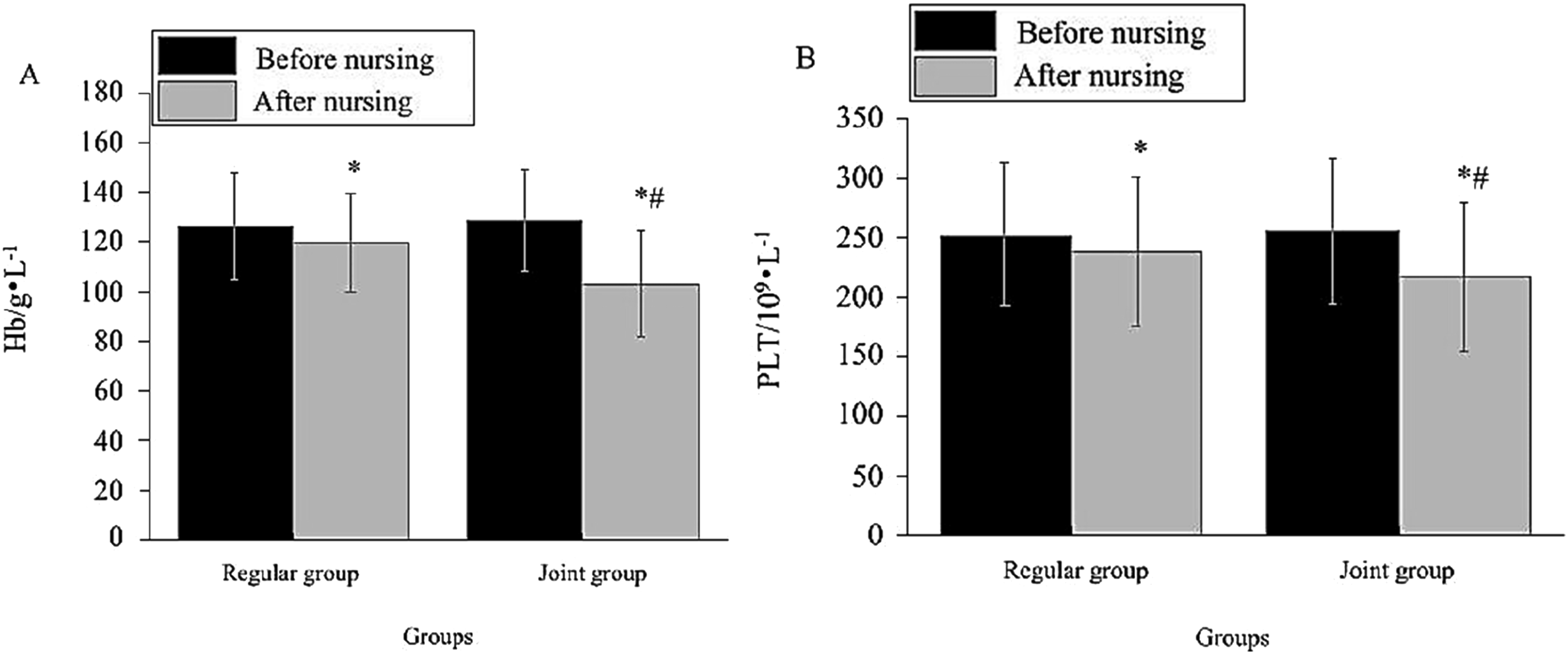
The bar chart in the figure represents the mean values of Hb and PLT, and the error bars represents the standard deviation (sd).
Contrast of hemodynamic monitoring indicators of subjects
In Figure 2, there was similar in the diameter of bilateral CFV, maximum BFV, and average BFV in the subjects before nursing (P > .05). Following nursing, the diameter of bilateral CFV in the RG was visibly reduced; the maximum BFV and average BFV of bilateral CFV of the subjects were visibly raised, and the maximum BFV and average BFV of bilateral CFV in the JG were more markedly raised as against the RG (p < .05). The diameter of the bilateral CFV, maximum BFV, and average BFV were all measurement data, which were tested for normality using the Shapiro-Wilk test and were found to follow a normal distribution; comparison before and after nursing within the same group was made using the paired samples t-test (two-sided), and comparison after nursing between the two groups was made using the independent samples t-test (two-sided). Contrast of hemodynamic monitoring indicators of subjects. (a): diameter of bilateral CFV; (b) maximum BFV of bilateral CFV; (c) average BFV of bilateral CFV).
Contrast of coagulation indexes of subjects
Before nursing, the levels of FIB, D-D, PT, APTT, and TT of the subjects were similar (p > .05). Following nursing, FIB, PT, and APTT of the subjects increased markedly, with the JG showing a more pronounced elevation relative to the RG; conversely, D-D and TT in the JG were clearly lower as against the RG (p < .05) (Figure 3). FIB, D-D, PT, APTT, and TT were measurement data, and were tested for normality using the Shapiro-Wilk test, which showed that they followed a normal distribution; comparison before and after nursing within the same group was made using the paired samples t-test (two-sided), and comparison after nursing between the two groups was made using the independent samples t-test (two-sided). Contrast of coagulation indexes of subjects. (a): FIB; (b) D-D; (c) PT, APTT, and TT).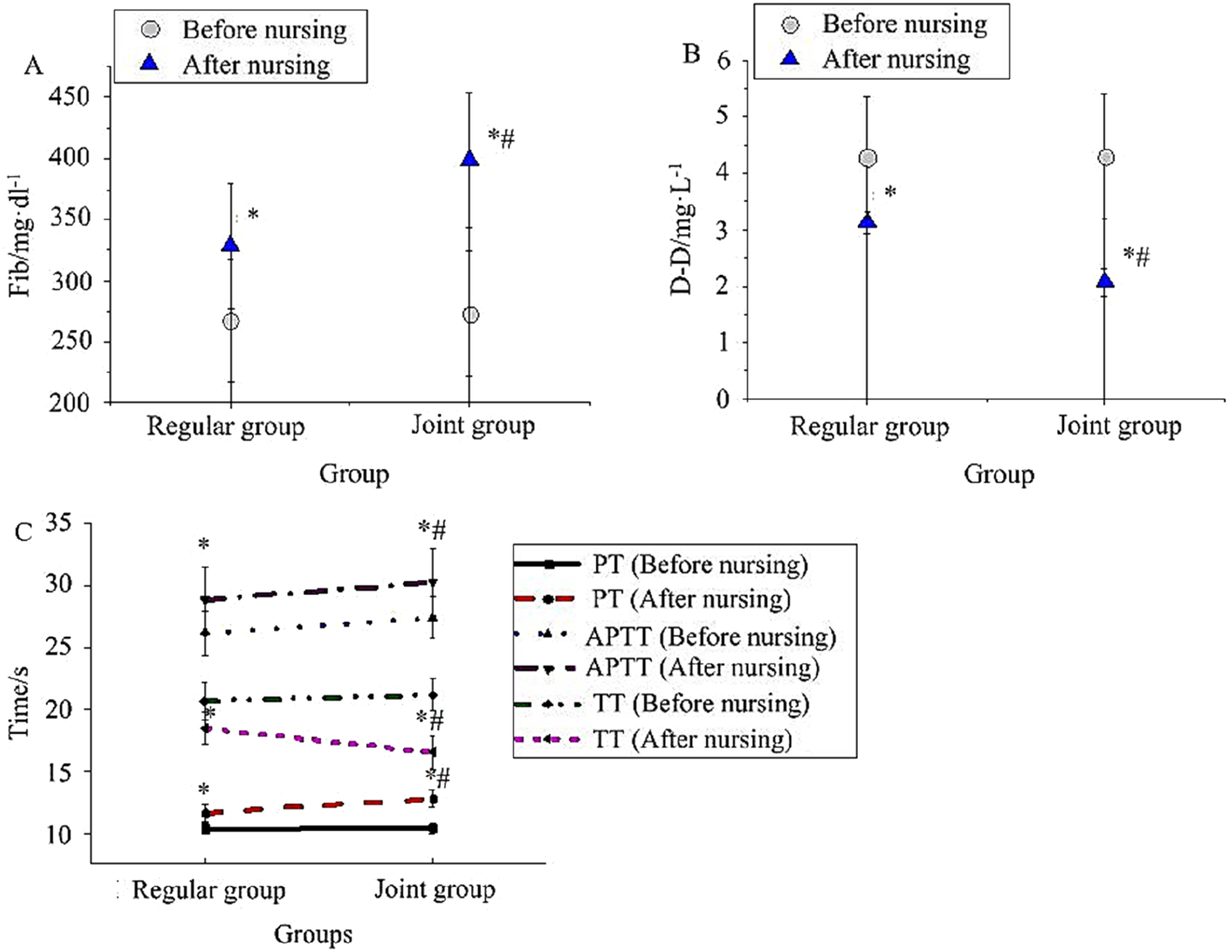
Contrast of swelling degree of lower limbs of subjects
The degree of lower limb swelling in the two groups of patients after nursing was analyzed. In the RG, 21.70% (51/235) of patients were classified as Grade I, 53.19% (125/235) as Grade II, and 25.11% (59/235) as Grade III. In the JG, 46.90% (123/268) of patients were classified as Grade I, 47.39% (127/268) as Grade II, and 6.34% (17/268) as Grade III. The swelling degree in the JG was found to be significantly more relieved than in the RG (p < .05), and the difference was of significant importance (Figure 4). The degree of lower limb swelling, being count data, was analyzed using χ2 test. Contrast of swelling degree of lower limbs of subjects. Note: *as against the RG, p < .05;The bar chart in the figure represents the number of patients with different degrees of swelling, with no error bars (as the data are count data, showing the distribution of numbers directly).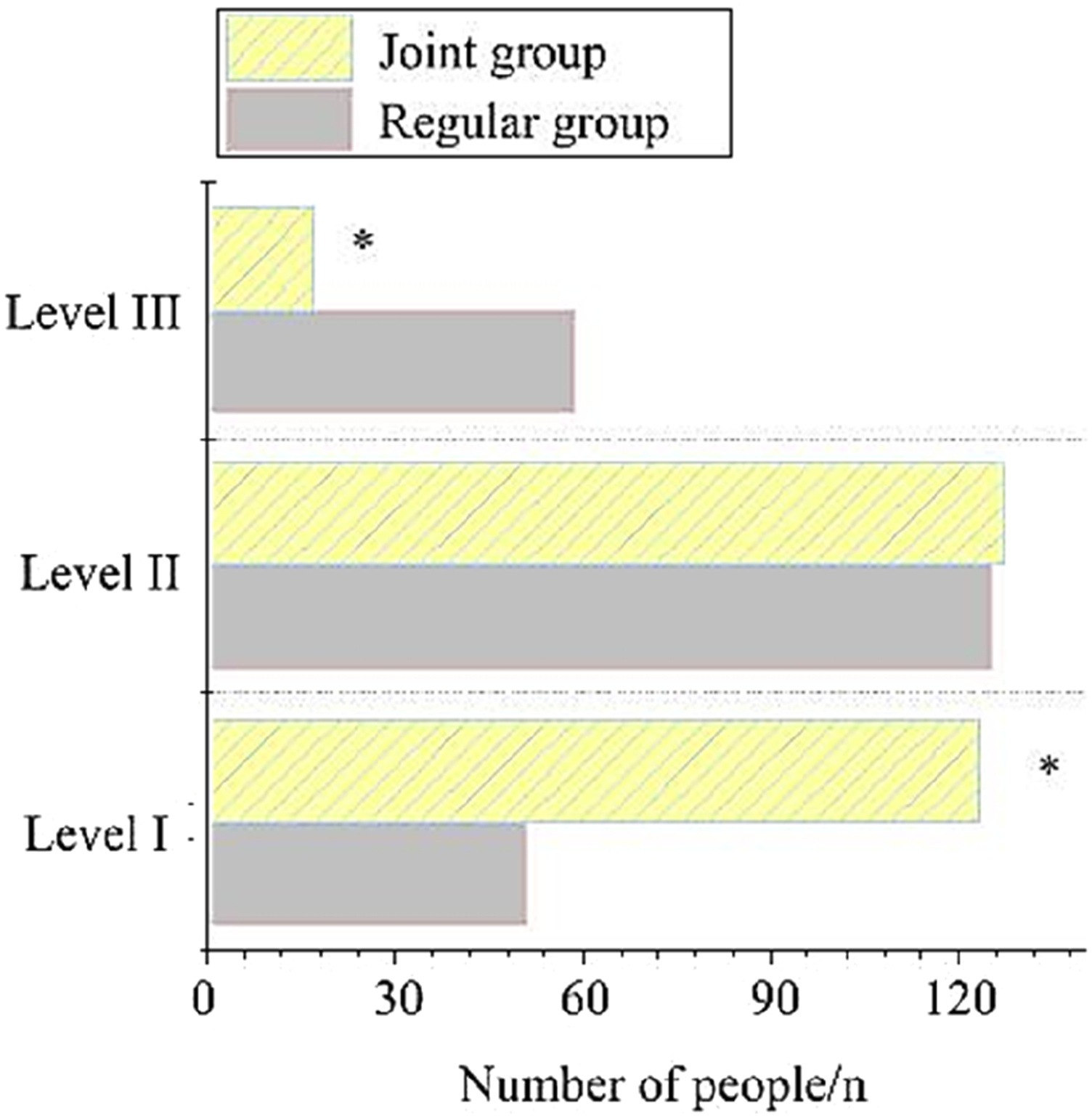
Contrast of clinical symptoms of subjects
The comparison of the immobile time in bed and hospital stay between the two groups of patients was made, with the results presented in Figure 5. The immobile time in bed and hospital stay for the JG were significantly reduced compared to the RG, and the difference was of significant importance (p < .05). The immobile time in bed and hospital stay, being measurement data, were tested for normality using the Shapiro-Wilk test and were found to follow a normal distribution; comparison between the two groups was made using the independent samples t-test (two-sided). Contrast of clinical symptoms of subjects.
Contrast of DVT incidence among subjects
The occurrences of DVT in the two groups of patients were statistically analyzed. In the RG, 8.94% (21/235) of patients were found to have incomplete thrombosis, and 4.26% (10/235) were found to have complete thrombosis. In the JG, 2.99% (8/268) of patients were found to have incomplete thrombosis, and 1.12% (3/268) were found to have complete thrombosis. The incidence of both incomplete and complete thrombosis in the JG after nursing was significantly reduced compared to the RG, and the difference was of significant importance (p < .05) (Figure 6). The incidence of DVT, being count data, was analyzed using χ2 test. Contrast of DVT incidence among subjects.
Contrast of nursing satisfaction of subjects
The satisfaction of the two groups of patients after nursing was statistically analyzed (Figure 7). In the JG, there were 187 cases extremely satisfied, 55 cases satisfied, and 26 cases dissatisfied; in the RG, there were 103 cases extremely satisfied, 81 cases satisfied, and 51 cases dissatisfied. The satisfaction with nursing in JG (90.30%) was significantly higher than in RG (78.30%), and the difference was of significant importance. The nursing satisfaction, being count data, was analyzed using χ2 test. Contrast of nursing satisfaction of subjects.
Discussion
IPC and ENS are two common methods to prevent DVT following OS. IPC can reduce the risk of thrombosis by periodically applying pressure on the lower limbs, simulating the role of muscle pump, promoting blood reflux, reducing the retention time of blood in the vein. 10 IPC can increase BFV, improve blood stasis, and activate fibrinolytic system through pressure induction to improve hypercoagulability. ENS refers to the provision of essential nutrients through the gastrointestinal tract to maintain or restore the nutritional status of patients. 11 Following OS, patients often suffer from decreased appetite and impaired digestion and absorption due to pain, anesthesia, or surgical trauma. At this time, ENS is particularly important.12,13 Enteral nutrition can not only provide energy and protein, promote wound healing and body recovery, but also improve the immune function of patients and reduce the occurrence of complications such as infection. 14 The combination of IPC and ENS has a synergistic effect in the prevention of DVT following OS. IPC contributes to the absorption and utilization of nutrients in the intestine by improving blood circulation and providing a more adequate blood supply to the intestine. The good nutritional status of patients can enhance the physical fitness of patients, improve the tolerance and recovery ability of surgical trauma, and indirectly reduce the risk of DVT. IPC plus ENS plays a major role in the prevention of DVT following OS.
The occurrence of DVT is closely related to blood stasis, vessel wall injury, and hypercoagulability. In related fracture surgery, elderly patients often have the characteristics of cardiopulmonary dysfunction, which will lead to local swelling, venous reflux disorder, and other events following surgery. In addition, some patients will have enhanced coagulation with vessel wall injury during surgery, which will lead to blood stasis. Hb and PLT in blood routine are important indicators reflecting the coagulation function and blood status of the body. 15 The results of this article showed that the subjects’ Hb and PLT were markedly reduced following nursing, especially in the JG. This indicates that the joint care program may have a positive effect on improving the blood flow of patients and reducing the risk of thrombosis. 16 applied IPC to the population of chronic wounds of the lower extremity, and the results suggested that it had obvious effect in the treatment of venous stasis ulcer of the lower extremity. In a review on the addition of antiplatelet drugs to the treatment of DVT, 1,625 patients were included. The results suggested that in the case of chronic DVT, the use of antiplatelet drugs (such as aspirin) following standard initial anticoagulant treatment can reduce the formation of DVT or the recurrence of pulmonary embolism. 17 Hemodynamic indexes, CFV diameter, and BFV were observed to directly reflect the blood flow status of lower limb veins. Following nursing, the diameter of the CFV in the RG decreased, while there was no obvious change in the JG, indicating that the combined nursing scheme may be more effective in maintaining the patency of the vein. The BFV of the subjects was markedly increased, especially in the JG, further confirming the synergistic effect of IPC and ENS in promoting blood flow. In some studies, IPC was used to control the swelling caused by lymphedema. In the study, the lymphatic vessels on the tail of rats were used to simulate the spatiotemporal oscillation pressure wave generated in the process of IPC. The results suggested that IPC could help regulate the lymphatic contractility. 18 This is similar to the results of this article. FIB, D-D, PT, APTT, and TT are key indicators to evaluate the risk of thrombosis. Following nursing, the increase of FIB, PT, and APTT and the decrease of D-D and TT in the JG were more obvious, indicating that the combined nursing scheme has more obvious advantages in regulating coagulation function and reducing the risk of thrombosis. In a review on the impact of nutritional supplements on the clinical outcomes of hip fracture surgery patients, it was found that the use of oral nutritional supplements was not associated with shorter hospital stay, but was associated with the improvement of sarcopenia markers and functional status. 19 This is similar to the results of this article. The swelling degree of the JG following nursing was markedly lighter than that of the RG, indicating that the combined nursing program has an obvious outcome in reducing postoperative swelling and improving patient comfort. 20 found that in the acute stage of DVT, pressurization can markedly reduce pain and swelling (91.7%) and prevent PTS (66.2%) according to a 626 investigation reports. This is consistent with the results of this article. 3751 patients were also included in the study, and pressure therapy was used for prevention. The results suggested that adding pressure therapy on the basis of drug treatment could relieve pain and reduce the degree of swelling faster, and it was proposed that the incidence and severity of post thrombotic syndrome in patients using medical pressure socks decreased by 16%-27%. 21 The immobile time in bed and hospital stay in the JG was markedly reduced. The reduction of immobile time was helpful to prevent the complications that may be caused by long-term bed rest. It was found that the incidence of incomplete and complete embolism in the JG after nursing was significantly reduced compared to the RG (p < .05), and the difference was statistically significant. The study of 22 has confirmed that IPC can prevent the formation of DVT. In a meta-study involving 8796 patients, it was found that adjuvant IPC was associated with a reduced risk of VTE and DVT, indicating that IPC can improve the prevention of DVT in drug-treated thrombotic diseases. 23 IPC can reduce the risk of thrombosis by promoting blood circulation, while ENS can promote the recovery of patients and enhance physical resistance by providing necessary nutrition. The combined use of the two can not only improve the prevention effect of DVT, but also improve the overall postoperative recovery of patients.
Conclusion
In summary, IPC plus ENS has shown obvious outcome in the nursing of lower extremity DVT prevention following OS. The nursing program can reduce the level of coagulation factors, reduce the incidence of DVT, shorten the immobile time in bed and hospital stay, improve nursing satisfaction, and is of great significance to promote the rapid recovery of patients and improve the QoL. In the future clinical practice, this nursing scheme should be further promoted and optimized to achieve a more comprehensive postoperative nursing effect.
Footnotes
Ethics approval
This study has been approved by the People’s Hospital of Chongqing Liang Jiang New Area. All the experiments of this study were conducted in accordance to the relevant guidelines and regulations or in accordance to the Declaration of Helsinki.
Informed consent
Written informed consent was obtained from all participants.
Authors’ contributions
YN, YW and QQ designed the study and wrote the manuscript, data and helped to draft the manuscript. All authors have read and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
All data generated or analyzed during this study are included in this published article.
