Abstract
Background
Lateral hinge fracture (LHF) is a known complication of open-wedge high tibial osteotomy (OWHTO), potentially resulting in postoperative instability, displacement, loss of correction, malunion, and non-union. This study tested the hypothesis that patients who develop LHF after OWHTO can achieve clinical outcomes comparable to those without LHF, without requiring additional surgical intervention.
Methods
This retrospective study included 96 patients who underwent OWHTO with a locking plate between 2019 and 2021. Postoperative radiographs and computed tomography (CT) scans identified LHF in 24 patients (25%). Lower limb alignment was assessed using whole-leg standing radiographs at 6 weeks, 3 months, 6 months, and 12 months postoperatively. Clinical outcomes were evaluated using the Hospital for Special Surgery (HSS) score, Knee Society Knee Score (KS), and Function Score (FS).
Results
In patients with LHF, the mechanical axis was 59.0 ± 7.4% at 6 weeks, 57.7 ± 7.8% at 3 months, 55.9 ± 9.5% at 6 months, and 53.9 ± 12.2% at 12 months. In patients without LHF, the corresponding values were 58.5 ± 6.1%, 57.8 ± 6.7%, 56.7 ± 7.0%, and 55.6 ± 7.4%, respectively. Although the mechanical axis decreased by 5.2% in the LHF group and 2.9% in the non-LHF group by 12 months, the difference was not statistically significant (p = .219). Similarly, the longitudinal change in alignment did not differ significantly between groups (p = .743). Postoperative clinical scores improved in all patients, with no significant differences between groups regardless of LHF status.
Conclusion
Patients who experienced LHF following OWHTO demonstrated comparable clinical outcomes and alignment correction to those without LHF, suggesting that LHF does not adversely affect postoperative results.
Introduction
High tibial osteotomy (HTO), including both closed- and open-wedge techniques, is an established treatment for medial compartment osteoarthritis (OA) with varus malalignment, particularly in younger patients.1–4 Among these, open-wedge HTO (OWHTO) has gained increasing popularity in recent years due to advances in locking plate technology and a lower risk of comorbidities typically associated with fibular osteotomies in closed-wedge procedures.5,6
Nevertheless, OWHTO is associated with several complications, including lateral hinge fractures (LHF), increases in posterior tibial slope angle, and elevated patellofemoral joint pressure resulting from changes in patellar height.7,8 Notably, LHF may occur in up to 34% of cases, 4 and has been linked to factors such as osteotomy location, hinge position, and incomplete osteotomy.9,10 However, the association between osteotomy size and LHF occurrence remains controversial.11,12 The presence of LHF can lead to increased micromotion at the osteotomy site due to reduced axial and rotational stiffness, 13 potentially resulting in postoperative instability, displacement, loss of correction, malunion, or non-union.13,14 In such cases, stable fixation—particularly using a locking plate—is essential to facilitate bone healing and preserve alignment. 15 Achieving appropriate lower limb alignment is a key determinant of favorable clinical outcomes. 3
We hypothesized that patients who experience LHF following OWHTO could attain clinical outcomes comparable to those without LHF, even in the absence of additional procedures. This study aimed to evaluate the impact of LHF on postoperative clinical outcomes and alignment changes following OWHTO.
Materials and methods
This retrospective study included 96 patients (mean age, 56.3 ± 4.9 years; range, 35–70 years) who underwent OWHTO using a locking plate between January 2019 and April 2021. Locking plate fixation was performed using either the TomoFix system (Synthes GmbH, Solothurn, Switzerland) in 33 patients or the OhtoFix system (Ohtomedical Co. Ltd, Goyang, Korea) in 63 patients. Patients were categorized into two groups based on the presence or absence of LHF, and subsequent comparisons of radiological and clinical outcomes were performed.
The study protocol was reviewed and approved by the institutional review board (IRB number: 2022-09-041-001).
Surgical technique
Preoperative planning involved full-length anteroposterior weight-bearing radiographs of the lower limbs. The mechanical axis was targeted at a point 62.5% lateral from the medial edge across the maximum mediolateral width of the tibial plateau.
All procedures were performed by a single surgeon. Diagnostic arthroscopy was conducted prior to osteotomy to assess the articular surface and meniscus integrity. When indicated, debridement or meniscectomy was performed. A proximal biplanar osteotomy was executed posterior to the tibial tuberosity following complete dissection of the pes anserinus. The superficial medial collateral ligament was elevated from the periosteum. The posteromedial tibial cortex was then gradually opened, and the osteotomy was stabilized using a locking plate. Allogeneic bone chips mixed with autologous bone marrow aspirated from the ipsilateral anterior superior iliac spine (ASIS) were grafted into the osteotomy site. The superficial medial collateral ligament was subsequently repositioned, and the pes anserinus was reattached to the periosteal membrane.
Postoperative rehabilitation
All patients used a night splint for stabilization and initiated range of motion exercises beginning on postoperative day two. In patients without LHF, partial weight-bearing was allowed at 2 weeks, followed by full weight-bearing with a brace at 4 weeks. In patients with LHF, partial and full weight-bearing with a brace were permitted at four and 8 weeks, respectively.
Evaluation & measurement
Radiologic evaluation was performed using anteroposterior (AP) radiographs of the knee and whole limb for alignment assessment. To assess LHF in all patients, postoperative radiographs were obtained immediately after surgery, followed by computed tomography (CT) examinations conducted 2 days postoperatively. LHF was defined as a complete discontinuity of the lateral cortex observed on either radiographic or CT imaging (Figure 1). The diagnosis of LHF was performed by one orthopedic surgeon. A 60-year-old woman with a type III lateral hinge fracture (arrow) during high tibial osteotomy (HTO) of the right knee. (a) Intraoperative fluoroscopy showing the lateral hinge fracture during HTO. (b) Immediate postoperative anteroposterior (AP) radiograph. (c) Coronal plane computed tomography (CT) image obtained 2 days postoperatively.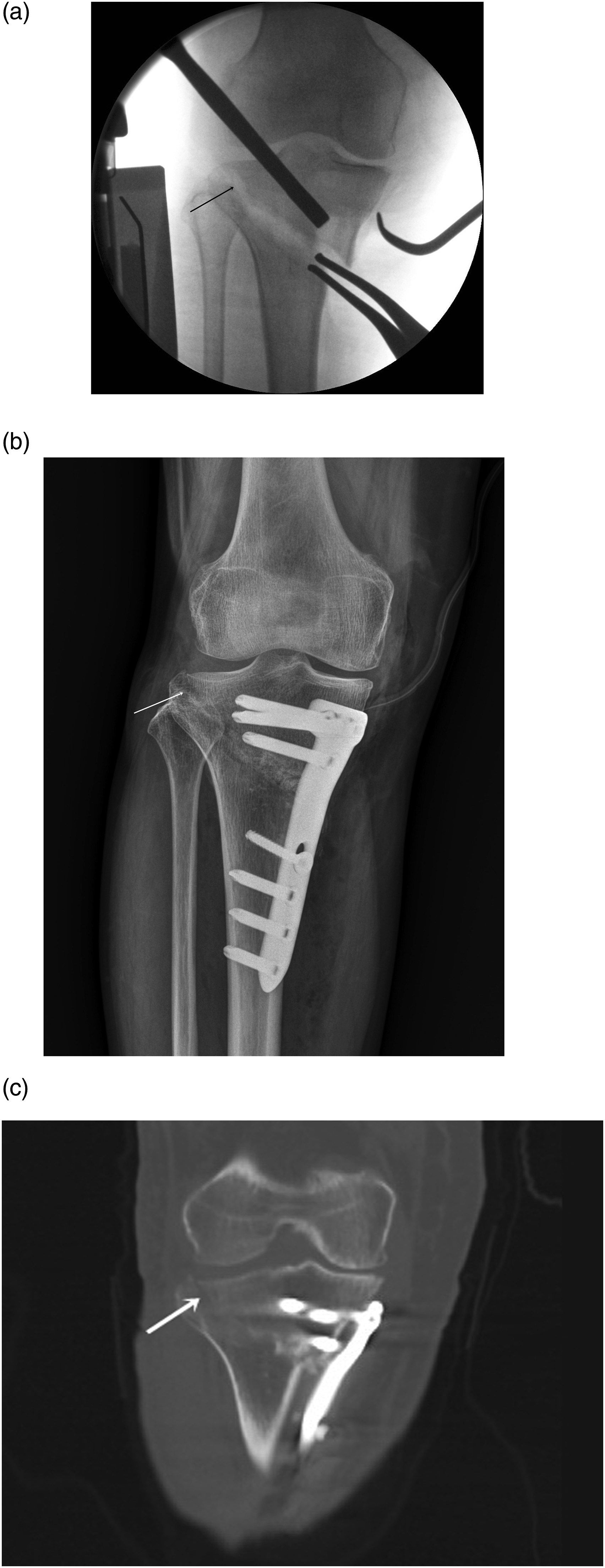
Limb alignment was compared between the two groups at 6 weeks, 3 months, 6 months, and 12 months following surgery in all cases. In patients with LHF after HTO, bone union was assessed using radiographs obtained in anteroposterior, lateral, and oblique views. Fracture union was considered achieved when callus formation was observed in at least three of the four cortices, along with fading of the fracture lines. The medial proximal tibial angle (MPTA) and joint line convergence angle (JLCA) were measured to identify potential causes of postoperative alignment changes due to fixation loss.
Clinical outcomes were assessed using the Hospital for Special Surgery (HSS) score, Knee Society Knee Score (KS), and Function Score (FS), all evaluated at the final follow-up (12 months postoperatively).
Statistical analysis
Paired t-tests and chi-square tests were employed to compare preoperative and postoperative parameters. Changes in alignment over time were analyzed using independent t-tests, Bonferroni post hoc tests, and Mauchly’s test of sphericity. A p-value of <.05 was considered statistically significant. All statistical analyses were performed using SPSS Statistics, version 23.0 (IBM Corp., Armonk, NY, USA).
Results
Postoperative radiographs and CT examinations revealed LHF in 24 patients (25%). In nine of these cases, the fracture was detectable only on CT imaging. According to the classification system proposed by Takeuchi et al., 18 patients had type I fractures, one patient had a type II fracture, and five patients exhibited type III fractures. 16
Demographic and preoperative clinical scores by group.

LHF, lateral hinge fracture.
Clinical outcomes before and after HTO in both groups.

LHF, lateral hinge fracture.
Postoperative improvement in clinical outcomes.

LHF, lateral hinge fracture.
In patients with LHF, the mechanical axis was 59.0 ± 7.4% at 6 weeks postoperatively, decreasing to 57.7 ± 7.8% at 3 months, 55.9 ± 9.5% at 6 months, and 53.9 ± 12.2% at 12 months. Among patients without LHF, the mechanical axis was 58.5 ± 6.1% at 6 weeks, 57.8 ± 6.7% at 3 months, 56.7 ± 7.0% at 6 months, and 55.6 ± 7.4% at 12 months postoperatively. Alignment decreased by 5.2% and 2.9% at 12 months in the LHF and non-LHF groups, respectively (p < .001 and p = .008). However, the difference between groups was not statistically significant (p = .219), and no significant group difference was observed in the temporal change in alignment (p = .743; Figure 2). The MPTA remained unchanged from 6 weeks to 12 months postoperatively in both groups (91.6% to 91.6%, p = .951 for LHF; 92.5% to 92.5%, p = .916 for non-LHF). In contrast, the JLCA increased significantly over time in both groups. In patients with LHF, JLCA increased from 2.2° to 2.6° (p = .001), while in those without LHF, it increased from 1.6° to 2.3° (p = .007). Change in mechanical axis after HTO in each group.
Discussion
This study examined the effects of LHF on postoperative clinical outcomes following OWHTO and found no significant differences in loss of correction, improvement in clinical scores, or changes in alignment over time between patients with and without LHF.
LHF after OWHTO has been reported to occur in 0.3% to 34% of cases, 4 and is known to potentially cause postoperative instability, further displacement at the osteotomy site, and subsequent loss of correction and alignment, thereby negatively affecting clinical outcomes.13,14,16 In the present study, 25% of patients developed LHF postoperatively. None of these patients required additional fixation or immobilization; instead, delayed weight bearing alone resulted in bone union within a mean period of 3.6 months. There were no significant differences in clinical outcomes or correction loss between patients with and without LHF. Previous studies have identified several technical factors contributing to LHF, including insufficient posterior osteotomy, anterior placement of fixation, posterior hinge positioning, steeper coronal osteotomy slopes, and larger osteotomy gaps..12,17,18 These findings underscore the importance of meticulous surgical technique, including complete posterior osteotomy prior to gap spreading and careful handling of the lateral cortex.
Although a significant reduction in limb alignment was observed up to 12 months postoperatively in both groups, no intergroup differences were noted. The MPTA remained stable, whereas the JLCA changed in both groups from 6 weeks to 12 months after surgery. These findings suggest that the observed alignment changes likely reflect alterations in joint space or soft tissue balance, rather than fixation failure. Therefore, the preservation of the meniscus or articular cartilage—rather than aggressive meniscectomy—should be prioritized during HTO procedures to maintain soft tissue integrity.
In the current cohort, no patient with LHF received additional fixation such as plating or supplementary screws. Instead, full weight bearing was deferred until 8 weeks postoperatively, which resulted in successful fracture union within a mean duration of 3.6 months. The osteotomy gaps were filled using a mixture of allograft bone chips and autologous bone marrow harvested from the ASIS in all patients. A previous study employing this method reported enhanced early osteotomy gap filling and osteoconductivity, thereby facilitating LHF site healing without the need for additional fixation when paired with delayed weight bearing. 19
This study has several limitations. Its retrospective design, relatively small sample size, and short follow-up period may have limited the generalizability and statistical power of the findings. Furthermore, the relationship between fracture type and clinical outcome could not be thoroughly assessed due to the limited number of LHF cases. Future research should adopt prospective study designs with larger cohorts and extended follow-up durations to validate and expand upon these findings.
Conclusion
In summary, this study demonstrated that the presence of LHF after OWHTO did not adversely affect postoperative clinical outcomes or correction maintenance. Moreover, delayed weight bearing without the need for additional fixation appeared to be a sufficient management strategy for LHF in this context.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Research Foundation (NRF) grant funded by the Korea government (MSIT) (RS-2024-00353326).
