Abstract
Purpose
This study presents the technique and results of acute correction of distal femoral deformities using retrograde femoral nailing based on preoperative planning without using a fixator.
Methods
Twenty-eight patients (34 limbs: 22 left-sided, 12 right-sided, mean age = 36 years) undergoing distal femoral deformity correction with retrograde femoral nailing between 2013 and 2020 were examined retrospectively. The osteotomy line, block screw location and number were identified by detailed preoperative planning. Osteotomy was performed using the percutaneous multiple drill method, and the retrograde femoral nail was placed.
Results
The average follow-up period was 62.7 months (range: 13–84 months). Postoperatively, the mean mechanical axis deviation was corrected to 6.8 mm (range: 0–8 mm) and the mean mechanical lateral distal femoral angle to 87.42° (range: 84–90°). The Association for the Study an Application of the Method of Ilizarov (ASAMI) score was excellent for all patients. None of the patients had fracture, infection, implant failure, or non-union.
Conclusion
Distal femoral deformities can be corrected acutely, without applying external fixators, with good preoperative planning and using the retrograde femoral nail. This technique is safe and effective, with a low complication rate.
Introduction
Femoral deformities are a common aetiological factor responsible for malalignment of the lower extremities and knee joint incongruencies. These deformities may include axial, coronal, or rotational deformities or limb length discrepancies commonly encountered in clinical practice. 1 The patient usually becomes symptomatic over time, with complaints of abnormal cosmetic appearance, pain sensation, or limited range of motion at the affected knee.
Over the years, extensive research has established that mechanical axis deviation and joint malorientation are known to be important determinants in the treatment of femoral deformities. A deviation of ≥10 mm from the normal mechanical axis may result in >5° joint malorientation in the distal femur and >10° angular deformities in the diaphyseal region necessitating surgical correction. 1 The common correction techniques for distal femoral deformities include open wedge, closed wedge, or dome osteotomy, 2 while external fixators, plates, or intramedullary nails may be used for fixation purposes. 3 However, in many clinics, external fixators are still used as the most common mode of deformity correction. 4 External fixator application is known to have some disadvantages, such as pin-site infection, joint stiffness and contractures, cosmetic problems, and chances of iatrogenic fractures resulting from removal of the fixator. 5 To minimise these disadvantages, fixator-assisted nailing or plating techniques have been developed which allow deformity correction with temporary application of fixator while the as the actual fixation is achieved with nail or plate.6,7
Despite extensive research describing several analysis methodologies, there is no clarity on the exact strategy for an effective treatment plan to ease surgical intervention. In our clinic, a comprehensive approach encompassing preoperative planning, osteotomies, and nail placement techniques for the treatment of distal femoral deformities has been developed. In this paper, we report on the surgical technique and clinical results of this novel methodology used for treating patients with distal femoral deformities.
Materials and methods
This was a retrospective study carried from 2013 to 2020. Approval for this study was obtained from our hospital’s ethical committee. All the surgical operations were performed by two surgeons with advanced deformity surgery experience. A total 34 limbs of 28 patients, who were operated upon for distal femoral deformities with a retrograde intramedullary nail was reviewed.
The indication criteria in this study were femur deformities in the metaphyseal and diaphyseal region. Active infection in the bone to be corrected is contraindicated for the procedure. Previously successfully treated bone infection is not contraindicated but should be considered as a high risk. The patient group with open physis is a relative contraindication. In this group of patients, it is a high risk procedure that requires experience and expertise in order to not damage the physis.
Preoperatively, standard anteroposterior and lateral radiographs, and standing orthoroentgenographic measurements were taken for all patients. The following parameters were measured on the standing orthoroentgenograph – mechanical axis deviation (MAD), limb length discrepancy (LLD), posterior distal femoral angle (PDFA), and mechanical lateral distal femoral angle (mLDFA).
1
Rotational deformity was measured both clinically and using computerized tomography (CT). After the deformity evaluation, preoperative planning was started (Figure 1) so that the osteotomy level, block screw location and number could be determined preoperative. (a) Pre-Op view of patient. (b) Pre-op orthorontgenogram (c). Drawing template and determination of axles (d, e). Determination of osteotomy line and block screw locations (f, g). Post-op orthorontgenogram (h). Post of view of patient.
During surgery, the patients were placed in a supine position on a radiolucent table under general anaesthesia. Before performing the osteotomy, one Schanz screw each for the proximal and distal femur was applied in parallel to correct and control the rotation deformity during surgery. The knee was flexed at about 40°. A guidewire was inserted from the standard entry zone for the retrograde femoral nail, and block screws were applied under the control of the scope. The distal femur was reamed and shaped with rigid reamers. Distal femoral osteotomy was carried out using the multiple drill method with a mini-incision made from the lateral side of the femur. Then, the intramedullary nail was inserted into the femur. Prior to applying the locking screws, rotation control was obtained with the help of Schanz screws, and the amount of correction was controlled by a radiopaque grip placed under the operating table. With the help of a distal locking guide, proximal locking was achieved freehand (Figure 2). All the patients were made to walk on the first postoperative day with partial weight bearing, along with basic active range of motion and quadriceps strengthening exercises. None of the patients received prophylaxis for deep vein thrombosis or vitamin D and calcium supplementation. (a) Schanz screw placement for distal and proximal rotation control. (b) Knee flexion and flexible reaming of the femoral canal. (c) Osteotomy with multiple drill method. (d) İnsertion of a retrograde nail. (e) Locking of distal screws. (f) Final rotation control.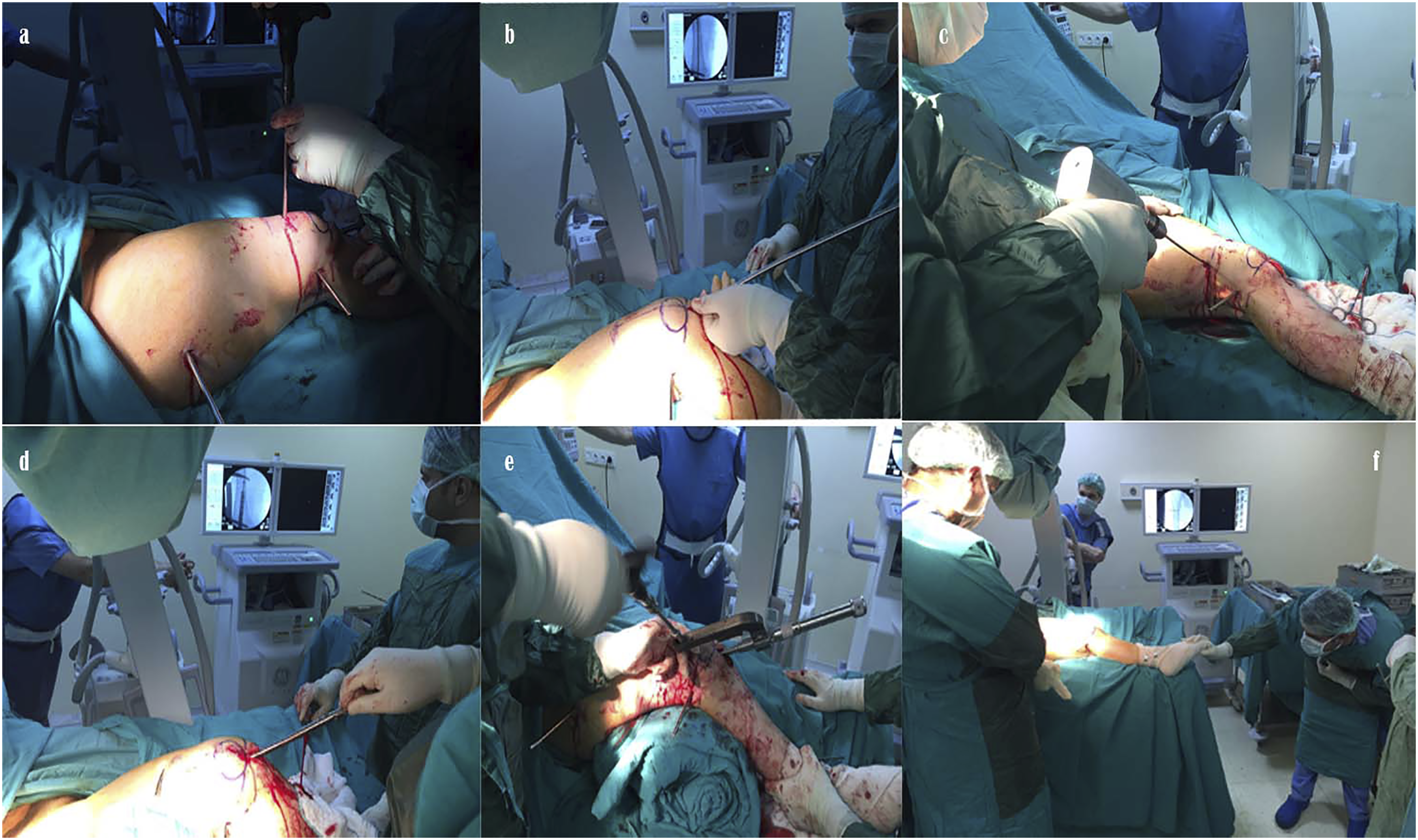
Results
The 34 limbs of 28 patients (15 males and 13 females) included in the study. Mean age: 36 years (range: 15–52 years), 22 were left-sided and 12 were right-sided. 18 had valgus deformities, and 16 had varus deformities. Eleven patients had secondary deformities, 8 patients with rotational deformity and 3 patients with sagittal plan deformity. The different aetiologies for femoral deformities included congenital deformities (n = 11 cases), metabolic bone disease (n = 7), growth arrest (n = 2), malunion (n = 1), complications due to cosmetic lengthening (n = 4), and polyostotic fibrous dysplasia (n = 3). The mean follow-up period for the patients was 62.7 months (range: 13–84 months).
Preoperative characteristics of patients.

Postoperative characteristics of patients.

Discussion
The technique of femoral deformity correction with distal femoral osteotomy and retrograde intramedullary nail administration has multiple advantages, such as acute deformity correction, early mobilization of the patient, and early bone healing. However, to achieve surgical success, this technique requires more skill and rigorous preoperative planning than other techniques. While adjusting the angle of the guidewire with the knee joint depends greatly on the surgeon’s skill, the support point in femoral deformity correction is the position of the block screw. 10 If the block screw is not accurately placed, the angular correction will be either insufficient or more than desired. Furthermore, in the case of the fissure extending to the block screw during osteotomy, it may be imperative to switch to another method to preserve the correction.
Deformities in the knee joint lead to changes in the limb’s mechanical axis, resulting in uneven load distribution and, consequently, the development of early arthrosis in the medial or lateral knee compartment. 11 Distal femoral osteotomies or proximal tibial osteotomies can be performed to reduce the progression of arthrosis by redistributing the load to the anatomical boundaries. 3
Distal femoral osteotomy can be a closed wedge, open wedge, or dome osteotomy. Open wedge osteotomy causes lengthening of the limb, and a graft may be needed to provide union at the osteotomy line; thus, the duration of union is long. On the other hand, closed wedge osteotomy does not require a graft but may cause shortening of the extremity. Similarly, there is no need for a graft in dome osteotomy; a length discrepancy is not seen in the extremity. With the technique which we used in this study, as the correction is provided by bony translation, the contact surface in the osteotomy line increases, which provides a shorter healing time compared to other methods. At our clinic, osteotomy was performed with percutaneous multiple drills and osteotomes, which prevented bone necrosis and delayed union. This technique minimises damage to the periosteum. Additionally, during intramedullary canal reaming, a bone graft was applied to the osteotomy region. 12
When the fixation methods following femoral osteotomy are compared, it has been reported that early rigid internal fixation with plate is more effective; however, internal fixation obscures early initiation of movement and weight-bearing owing to the extensive soft tissue damage during the operation. 3 External fixation, on the other hand, allows the opportunity for gradual correction of postoperative deformity; nevertheless, restriction of early range of motion exercises, pin-site infection, and device-related disturbances are inevitable.3,5 Intramedullary fixation offers a good solution by preventing unnecessary soft tissue damage compared to metal plate fixation as well as allowing early movement and weight-bearing. However, this technique may not be suitable for obtaining rigid fixation in cases of metaphyseal osteotomy. Furthermore, cartilage damage may occur depending on the entry site of the retrograde nail; therefore, care must be taken when determining the site of entry. 13
It is noteworthy that acute deformity correction does not have any negative effects on bone regeneration. 14 None of our patients required grafting to ensure fusion. Although a maximum of 17° of acute deformity correction was done in this study, other studies have reported up to 20° of acute correction.15,16 We also used block screws to provide the alignment and determine the path along which the nail was to be directed. No postoperative loss of alignment was observed in any patient. Although some studies have indicated a relationship between the number of block screws and the protection of optimal alignment, no difference was found in the number of block screws used in our series. 17
Conclusion
We successfully corrected femoral deformities without the application of an external fixator using retrograde intramedullary nailing guided by extensive preoperative planning. The osteotomy level and the number and location of block screws were determined preoperatively to ensure surgical success. However, competent preoperative planning and pattern drawing require experience, which may be a disadvantage of this technique. Nevertheless, there were no instances of fracture, implant failure, or non-union, which emphasise the safety and effectiveness of the procedure in the treatment of femoral deformities.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
