Abstract
Background
Bronchial asthma, a hypersensitivity illness, is rising quickly in the modern world, particularly in wealthy nations. However, according to clinical features, bronchial asthma and Ayurvedic Tamaka Shwasa are similar diseases. Asthma is incurable, according to traditional medical knowledge. Both patients and doctors are looking at complementary and alternative systems of medicine as options because current prescriptions do not offer adequate treatment for terminal and long-term cures. Ayurvedic medicine has the potential to be a viable and efficient treatment option for bronchial asthma. Vaman karma is helpful for treatment globally so that people worldwide can keep faith in it based on scientific evidence. The first line of treatment for Tamakshwasa’s Utkleshita vastha is Vamana. To determine Vamana Karma’s involvement in Tamak shwas, a season it connected to Tamak shwasa has been searched for and attempted to be established in this case study.
Purpose
This study aimed to assess the efficacy of Ayurvedic management, including specific Ishwaku vaman karma, in Tamaka Shwasa.
Materials and Methods
A single case study of a 21-year-old man diagnosed with bronchial asthma. He was presented with frequent allergy due to dust, had an onset of sneezing due to cold weather, had a complaint of cold and cough on and off since childhood, and had a history of pneumonia in childhood.
Observation and Outcome
A 9-day symptomatic patient assessment was completed. The patient’s overall quality of life was greatly enhanced, and the outcome was satisfactory. In conclusion, the above-mentioned regimen significantly improved the management of bronchial asthma.
Introduction
The terms “tamaka” and “Shwasa” are combined to form the phrase. Tamaka is the term for sadness. Vachaspatyam claims that the word implies both Roga Bheda and Vayu Vyapara. 1 It represents physiological and pathological respiration and is used to express the word. The disease is called Tamaka as an attack of the disease precipitates during the night, and the state of attack dyspnea becomes so severe that the patient feels like entering into the darkness. 2 The primary contributing factors to Tamaka Shwasa are Dhuma (smoking), Ativyayama (excessive exercise/work), sthananivasa (living in cold climates), (heavy diet), and Sheeta bhojana (cold food that causes vitiation of Vata, which in turn causes vitiation of Kapha, which in turn causes vitiation of Rasa, which inhibits Prana Vata function). 3 Vamana karma is specially indicated in Kaphaja disorders. One such disease involving Kapha is Tamaka Shwasa (bronchial asthma). The act of respiration is the physiological function of Prana Vayu. When Kapha obstructs this Prana Vayu, it gets pratiloma gati. It moves upwards, impairing respiration, resulting in Tamaka Shwasa (bronchial asthma). 4 Minimal is known about the Ayurvedic treatment of Tamaka Shwasa, or bronchial asthma, in the modern world, especially in Vaman. Therefore, an effort was made to determine whether shodhan karma effectively treated patients with Tamaka Shwasa (bronchial asthma).
In India, the prevalence rate of asthma is 2.05% nationwide, affecting 17.23 million people, according to the Indian Study on Epidemiology of Asthma, Respiratory Symptoms, and Chronic Bronchitis in Adults (INSEARCH). The most recent Global Burden of Disease (GBD, 1990–2019) report estimates that 34.3 million Indians suffer from asthma worldwide. Asthma was also linked to 13.2K more fatalities in India. Among Indians, asthma accounted for 27.9% of disability-adjusted life years (DALYs). The overall burden of asthma in India is more than twice as high as the global average in terms of DALYs and mortality. 5
Both adults and toddlers can develop asthma gradually. The inflammation and surrounding muscular contractions cause the tiny airways in the lungs to tighten. This causes the person to have asthma symptoms, such as tightness in the chest, coughing, and wheezing. The worst times of day for these intermittent symptoms are usually after an exercise or at night. The symptoms of asthma may worsen due to other common causes. Everybody has different triggers, including dust, smoke, fumes, colds, grass, pollen from trees, animal fur and feathers, harsh soaps, and smells. 6
Patient Information
It is a single case study having demographic details mentioned in Table 1.
Demographic Details of the Patient.
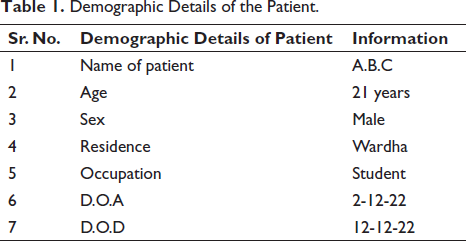
Clinical Presentation of the Patient
The chief and associated complaints of patients are mentioned in Table 2.
Chief Complaints of the Patient.
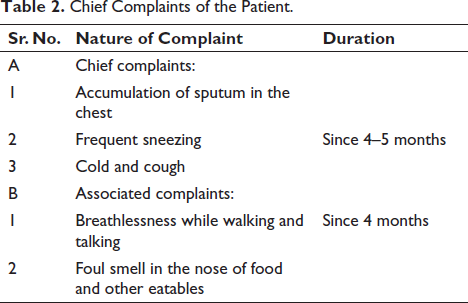
Progression of Disease
A 21-year-old male child, who belongs to a lower-middle-class family, complains of Shwasa kashta (dyspnea) that significantly increases in the evening time and has frequent episodes of allergy due to dust. The patient took homeopathic treatment in 2015–2016 and got relief in allergy only. Then again, due to cold weather in the morning, there was frequent sneezing with shortness of breath and productive cough (sakapha kasa) with breathlessness symptoms, with a history of being diagnosed as child pneumonia in childhood and taken treatment at an allopathic hospital and relieved. Still, after some years, the patient has complaints mentioned in Table 2. Patients took allopathic medicines for 1 month: TAB Azitromycin 500 mg, Cetirizine 5 mg, and cough expectorant. Then, after a few days, the patient suffered from a mild asthmatic attack with severe breathlessness in the morning time. He then took some Ayurvedic medicine from a local Ayurvedic practitioner. After 1 month, he suffered a recurrence of the above symptoms. Therefore, he approached the outpatient department of Panchkarma, Mahatma Gandhi Ayurved College, Hospital & Research Center Salod (H) Wardha, Maharashtra, for further treatment.
History of the Patient
The detailed account of the patient is given as follows:
Family history: No significant family history was found.
History: History of pneumonia 3–4 times in childhood.
Personal history:
Ahar: Vegetarian, daily intake of oily, sweet, and fermented food.
Vihara: Jagrana (night awakening), Atishrama (excessive exertion).
Nidra: Interrupted sleep at night due to aggravation of the symptoms.
Vyasana: Nil.
Vyayam: No.
Clinical Findings
As mentioned in Ashtavidha Pariksha (see Table 3).
Ashtavidh Parikshana.
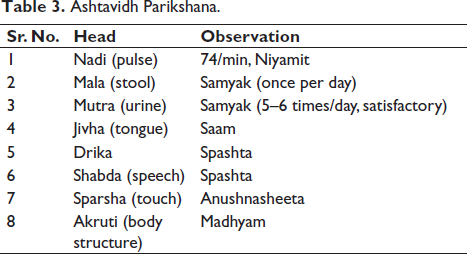
Samprapti Ghataka (Ayurvedic pathophysiology)
Dosha: Vata (prana), kapha (kledaka), pitta (pachaka)
Dushya: Rasadhatu
Strotas: Pranavaha, udakvaha, annavaha
Agni: Jatharagnimandya, Rasaagnimandya
Strotodusti: Sanga in prana vaha due to kapha vimargamana of prana sanga in annavaha due to ama and attipravatti in udakavaha (due to kapha)
Udhbhavastana: Amashaya
Rogamardga: Abhyantara
Vyadhi-svabhava: Chirkari
Sadhya-Asasdhya: Navina-sadhya (ch)
Purana-Yapya (ch)
Examination
The patient had a barrel chest, was nourished, was thin, and did not show signs of icterus, cyanosis, clubbing, lymphadenopathy, or edema. The patient was febrile-oriented with Alae Nasi’s (accessory muscles for respiration). The respiratory system exhibits equal bilateral chest movement and air entry, as well as bilateral wheezing accompanied by retraction and an increase in respiratory rate of 28 breaths per minute. Cardiovascular devices display tachycardia without any additional sounds being heard. The patient was awake, attentive, cooperative, and restless. There was no organomegaly, and the abdomen was soft and untendered. Pulmonary function test (PFT) indicates bronchial asthma.
Investigations: Routine investigations were done with ECG as the protocol of Vaman, which was within the standard limit.
Specific investigations advised PFT Figures 1 and 2 (before and after).
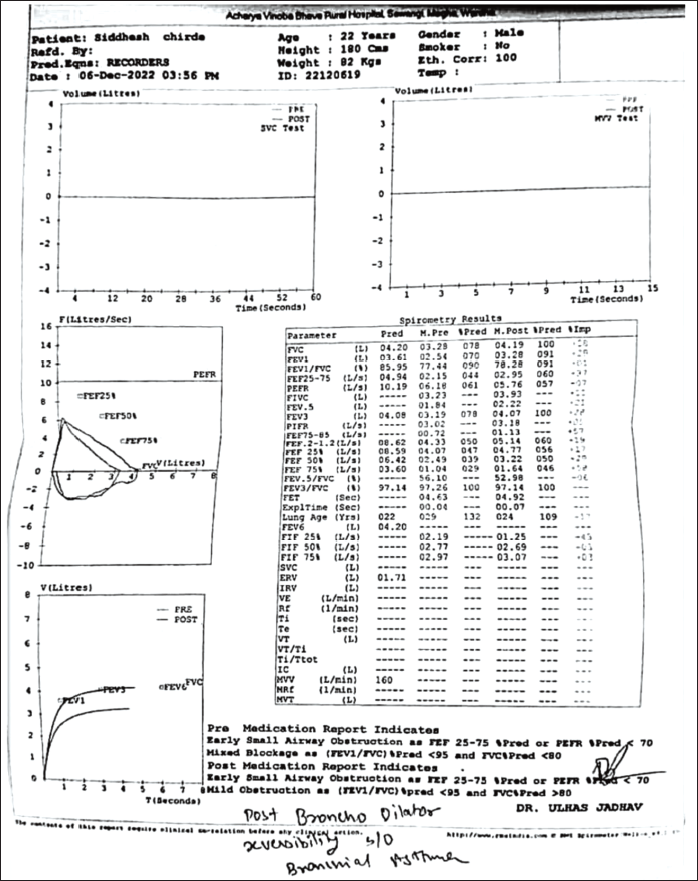
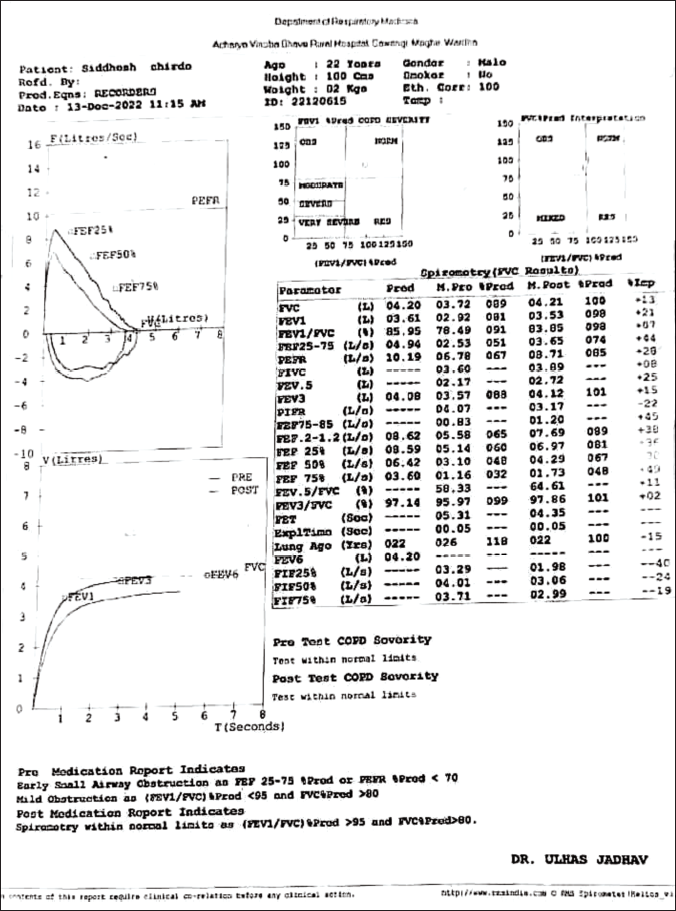
Diagnosis: Tamak Shwas (bronchial asthma).
Therapeutic Interventions
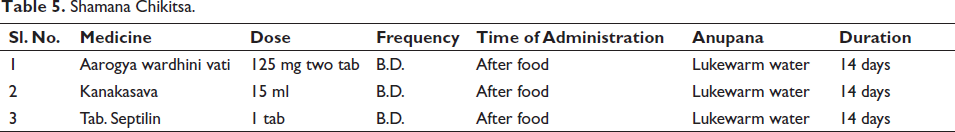
The treatment Panchakarma [Purification and Shamana Chikitsa (Palliative)] is given in Tables 4 and 5, respectively.
Line of Treatment (Panchakarma).
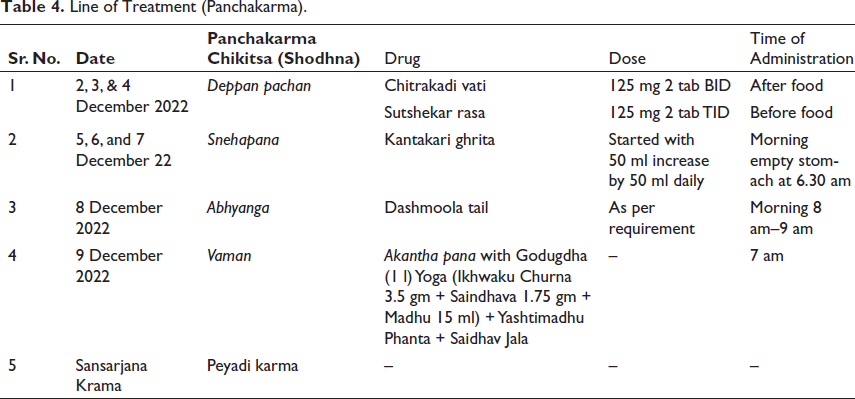
Shamana Chikitsa.
Therapeutic Outcome
Observations
Noted improvement in symptoms is shown in Table 6. The successful intervention of the treatment complete remission from all signs of bronchial asthma, including the accumulation of sputum in the chest and frequent sneezing after the entire Vaman procedure. Criteria for assessment for subjective parameters—MRC dyspnea scale was used. 7
Therapeutic Outcome.
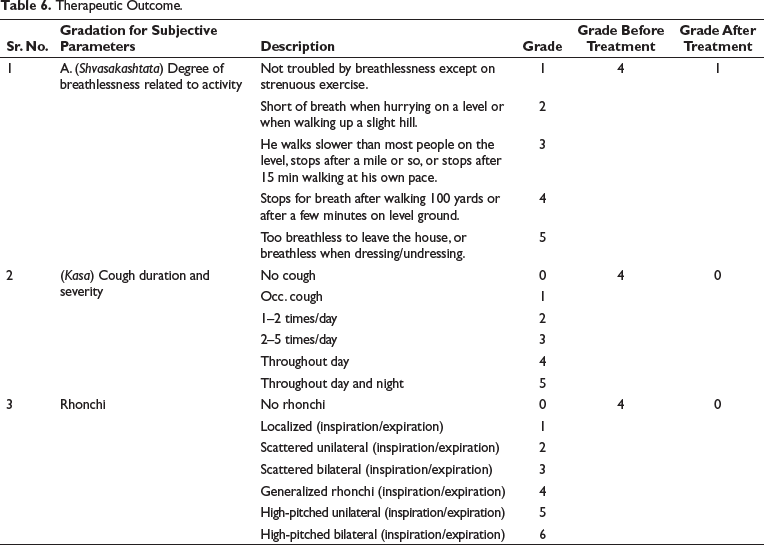
Discussion
Tamaka shwas and bronchial asthma are associated in current times. The subject in this case study had a condition related to severe asthma. Vamana, because of its Veerya (potency), Dravyas circulate fast in both the body’s large and small capillaries, giving them the qualities of Vyavayi and Vikasi. It permeates every part of the body. Due to Ushna Guna, Doshas began to melt in the body, seen in the patient’s sweat on their forehead or occasionally their entire body. Several classical literary works recount Vamana Karma’s roles in Tamaka. The preferred method of treatment or process in Vegakalinavastha is Vamana Karma or Sadyo Vamana. Vegagavastha doshas are at an aroused stage, which is a prepared state to be removed from the body or eliminated. Therefore, Abhyanga and Swedana, followed by Vamana Karma, clearing the Sanga (airway barrier), will be beneficial for the Vilayana of this Grathitha Kapha. The Kapha is ejected from the airways, then it returns to Amashaya where Vamana expels it. 8
Ikshwaku is tikta, katu rasatmakdravya, and have sheetaveerya. It has laghu (light), Ruksha, and teekshna properties and has pittaghna and kaphaghna prabhava. 9
Samshodhana (radical treatment), Bhedaka (penetration), and Kaphanissaraka qualities of vitiated and sluggish Ikshvaku may cause Kapha to be evacuated from the system, clearing the pathways of circulation and allowing Vayu to travel freely. Still, after one years cough expectorant is removed. After the vitiated Kapha is removed, the sufferer ultimately finds relief. Therefore, the Ikshvaku lady appears more advantageous than Tamaka Shwasa. 10
Tab Chitrakadi Vati: The main ingredients of Chitrakadi vati are Chitrak, Yavakshar, and Lavan, and the remaining drugs have deepan pachaniya properties, so they are used before vaman as deepana pachan. 11
Tab Sutshekar Rasa—impaired digestion, 12 so used for deepana pachan.
The management of acute and recurring upper respiratory tract infections is said to benefit from the anti-bacterial and anti-inflammatory characteristics of Tab. Septiline. 13 It has reportedly been shown to reduce gram-negative and gram-positive bacterial growth and aid in the mucosa’s development of tolerance to certain situations. 14
Tab Arogyavardhini is used as Sarvaroga prashamani (it can alleviate all types of disorders from the body). 15
Syp. Kanakasava acts as a bronchodilator and an immune regulator. 16
Conclusion
Based on the fundamentals of Ayurveda, this case study demonstrated that Tamaka shwas could be successfully handled with Shodhana and Shamana Chikitsa. No, this treatment plan is what caused the unintended adverse effect. Future clinical trials should be planned in a broad population using the same protocol.
Footnotes
Acknowledgments
The authors are very grateful to the Dean and all research cell teams of the University and Mahatma Gandhi Ayurveda College Hospital and Research Center, Salod (H), Wardha.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
