Abstract
Aim
To investigate the anti-inflammatory effect of bezafibrate on acute and subacute inflammation in adult male Wistar rats.
Methods
The study was carried out in adult male Wistar rats and they were allocated into three groups, that is, control, aspirin and bezafibrate, after obtaining clearance from Institutional Animal Ethics Committee. Acute inflammation was studied using carrageenan-induced rat paw oedema, and the volume displacement due to paw oedema using the plethysmograph. Subacute inflammation was studied using foreign body induced granuloma models. Analysis was performed using one-way ANOVA followed by post hoc tests of Dunnett’s. The value p < 0.05 was considered statistically significant.
Results
Bezafibrate showed a significant anti-inflammatory effect in acute as well as subacute models of inflammation when compared to control in the present study.
Conclusions
In patients receiving bezafibrate for hyperlipidemia, its anti-inflammatory potential may have an additional benefit in preventing complication of atherosclerosis.
Keywords
Introduction
One of the major causes of death and premature disability in developed societies is atherosclerosis. 1 Dyslipidemia, hypertension and diabetes mellitus are well-established risk factors for atherosclerosis. Proinflammatory and procoagulant states also have a significant role in the progression of atherosclerosis. 2 This overview of atherosclerosis has led to our emphasis on peroxisome proliferators activated receptors (PPARα). PPARα, a nuclear receptor that gets activated by ligands such as fatty acids and fibrates, and regulates the genes involved in fatty acid oxidation, lipid metabolism and glucose homeostasis, which in turn helps to improve markers of atherosclerosis. 3 The activation of PPARα has been shown to improve the overall atherogenic plasma lipid profile, especially levels of triglycerides, and high-density lipoprotein (HDL). In addition to this, PPARα have also been found to modify mechanisms of inflammation in the vasculature along with the acute phase response of the liver.3, 4
Studies have shown that fibrates such as fenofibrate and bezafibrate that activate PPARα may have multiple effects; these effects include improvement in atherogenic plasma lipid profile and reduction of the inflammatory response in the plasma and the vascular wall.4, 5 In a clinical study conducted in patients with hypertriglyceridemia and insulin resistance, bezafibrate, a second-generation fibrate, significantly reduced insulin resistance and triglyceride levels along with a reduction in the production capacity of C reactive proteins (CRP), fibrinogen, interleukin-6 (IL-6), and tumour necrosis factor alpha (TNF-α). 6 Similarly, a few studies suggest that bezafibrate has shown to decrease monocyte release of monocyte chemoattractant protein 1(MCP-1), IL-6, TNF-α and IL-1β in mixed dyslipidemia subjects.6, 7 However, reviewing of the literature reveals a paucity of pre-clinical studies regarding the effects of bezafibrate on inflammation. Hence, in view of the role of inflammation and hyperlipidemia in atherosclerosis, the present study was planned to evaluate the effect of oral bezafibrate on acute and subacute models of inflammation in adult male Wistar rats.
Materials and Methods
The study was conducted after obtaining approval from the Institutional Animal Ethics Committee (IAEC) established according to the rules of the Committee for Control and Supervision of Experiments on Animals (CCSEA), New Delhi. After obtaining adult male Wistar rats weighing 170 ± 25 g from the animal house, they underwent 10 days adaptation period to 12 h of light and 12 h of darkness until the experimentation day. They were given free access to water and fed on pellets of rat food.
Carrageenan-induced Rat Paw Oedema Model
Three groups (control, standard and test groups), each containing six adult male Wistar rats were obtained. They were made to starve overnight with the free supply of water prior to the day of the experiment. The control group was administered 0.5 mL of 1% gum acacia suspension, and the standard group was given aspirin, 200 mg/kg body weight equivalent to 2,222 mg of clinical dose. The test group received bezafibrate, 36 mg/kg body weight equivalent to 400 mg of clinical dose. All the drugs were given orally. For the acute inflammation study, aspirin was administered half an hour before, and bezafibrate was administered 1 h before the induction of rat paw oedema. Using Winter et al. (1962) method, paw oedema was induced by injecting 0.05 mL of 1% carrageenan in 0.9% saline into the sub-plantar area of the left hind paw.
8
The left leg’s malleolus was marked to enable consistent dipping during successive readings. By mercury displacement method using a plethysmograph, paw volume was determined in milliliter (mL) shortly following carrageenan injection (i.e., at 0 h). The same process was carried out again at 0.5, 1, 3, 4 and 5 h. By calculating the difference between 0-h reading and successive readings, the actual paw oedema volume was determined. The given formula was used to estimate the percentage inhibition of rat paw oedema in the aspirin- and bezafibrate-treated groups.
8
Foreign Body-induced Granuloma Model
Three groups of six adult male Wistar rats were created. Under thiopentone anesthesia, after shaving axillae and groin and two sterile cotton pellets of l0 mg each and two sterile grass piths of size 25 × 2 mm were subcutaneously implanted through a tiny incision. After suturing the wounds, the animals were caged individually. On the day of implantation, various treatments were started and were repeated everyday for the next 10 days.
The rats were sacrificed on the 11th day with an excess of thiopentone and the grass piths and cotton pellets were removed. Formalin (10%) was used to preserve the grass piths for histopathological studies. The cotton pellets were dissected out from extraneous tissue and were dried overnight at 60°C in an incubator to record their dry weight. By subtracting the initial weight of the cotton pellet (10 mg) from the recorded weight, net granuloma formation was calculated. Mean granuloma dry weight of various groups was calculated and expressed as mg/100 g body weight. The given formula was used to estimate the percentage inhibition of granuloma dry weight in aspirin- and bezafibrate-treated groups.
9
Both the mean volume of displacement for each of the time interval and mean dry granuloma weight were determined, and the standard error of the mean (SEM) for each group was also estimated.
Statistical Analysis
Using Graphpad Prism software, one-way analysis of variance (ANOVA) was used to assess the data, and to compare each group with the control, Dunnet’s test was used. To compare bezafibrate groups to the aspirin group, Bonferroni’s test was used, and p-value < 0.05 was considered significant.
Results
Carrageenan-induced Model for Acute Inflammation
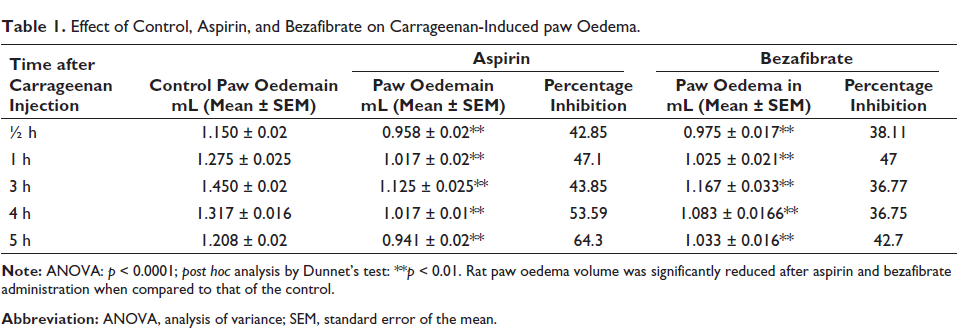
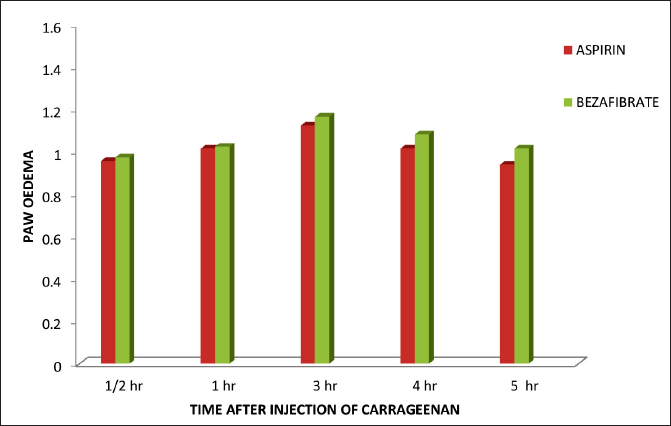
Using plethysmograph, the mean paw oedema volume (in milliliters) was estimated for control, aspirin and bezafibrate groups at 0.5, 1, 3, 4 and 5 h, as depicted in Table 1. From Table 1, it is also clear that groups treated with bezafibrate and aspirin had significant inhibition of paw oedema (p < 0.001). Additionally, as can be seen in Figure 1, bezafibrate’s anti-inflammatory effect was even similar to that of aspirin with a p-value > 0.05.
Effect of Control, Aspirin, and Bezafibrate on Carrageenan-Induced paw Oedema.
Foreign Body-induced Granuloma Model for Subacute Inflammation
The 10-day-old granuloma’s mean dry weight, measured in mg/100 g of body weight, in the aspirin- and the bezafibrate-treated groups were significantly reduced. It was 17.71 ± 0.58 in the control group, but it was significantly reduced (p < 0.01) in the group treated with aspirin with 32% inhibition. Similarly, bezafibrate-treated group (36 mg/kg) demonstrated a significant (p < 0.01) decrease in granuloma weight with a mean value of 14.84 ± 0.595 and a percentage inhibition of 16.15% (Table 2).
Effect of Aspirin and Bezafibrate Treatments on Granuloma Dry Weight.

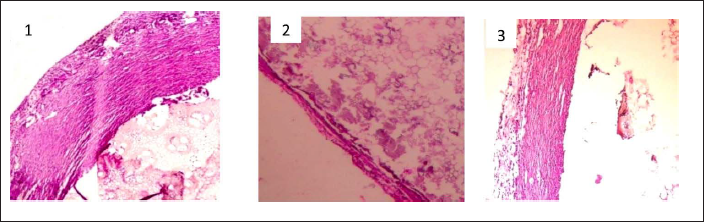
Histopathological studies further confirmed the anti-inflammatory effect of bezafibrate, which was demonstrated in acute and subacute models of inflammation. The sections of the grass pith, which after staining with eosin and hematoxylin, displayed granulation tissue with densely scattered fibroblast, inflammatory cells and collagen in dense sheets in the control group; however, they revealed decreased granulation tissue, reduced number of fibroblasts, collagen content and fibrous tissue in aspirin- and bezafibrate-treated groups (Figure 2).
Discussion
This present study demonstrates that bezafibrate has a significant anti-inflammatory effect in animal models of acute and subacute inflammation when compared to the control group, and the anti-inflammatory effect of bezafibrate was even comparable to aspirin.
PPARα is a ligand-activated transcription factor that is strongly implicated in lipid metabolism, beta oxidation of fatty acid as well as inflammation. PPARα modulates the density and size of low-density lipoprotein (LDL) particles and limits LDL oxidation; in addition to this, it also inhibits the formation of foam cells by increasing reverse cholesterol transport. Inhibition of macrophage foam cells thus inhibits the production of various inflammatory cytokines. 3 PPAR activators were shown to inhibit the activation of inflammatory response genes (such as TNF-α, IL-2, IL-6, IL-8 and metalloproteases) by negatively interfering with the nuclear factor-kappa B (NF-kB), signal transducer, activator of transcription (STAT) and activator protein-1 (AP-1) signalling pathways. 10
Fibrates by virtue of their hypolipidemic effect have been shown to delay the formation of atherosclerotic disease and reduce cardiovascular disease. 10 It is well accepted that inflammation is an important contributor to the evolution of atherosclerosis and its complications, such as plaque rupture, inflammatory infiltrate and thrombosis, in addition to dyslipidemia.2, 11 In dyslipidemics, there is increased LDL oxidation that enhances the formation of foam cells. This oxidised LDL is highly cytotoxic to various cells, including endothelial cells and acts as a chemoattractant for other monocytes. This additionally promotes the gene expression of MCP and macrophage colony-stimulating factors derived from endothelial cells. These cells, in turn, will further amplify the inflammatory cascade.12, 13 On the other hand, inflammatory mediators such as TNF-α, macrophage colony-stimulating factor and IL-1 enhance LDL binding to smooth muscle and endothelium and its oxidation, which promotes LDL-receptor gene transcription.14–16 As a result, an endless loop of lipoproteins oxidation and inflammation is developed in the arteries.2, 13 Therefore, drugs that have a dual anti-inflammatory effect and hypolipidemic effect will have added advantages in the treatment of atherosclerosis by breaking this vicious circle.
Patients with dyslipidemia normally receive one of the hypolipidemic drugs. This is by virtue of their hypolipidemic effects; however, the anti-inflammatory potential of drugs like bezafibrate has not received as much heed. The findings of this study are in agreement with earlier reports, where patients with isolated hypertriglyceridemia who received bezafibrate for 12 weeks showed a reduction in lymphocyte release of IL-2, IFN-γ and TNF-α, which was accompanied by a reduction in plasma highly sensitive CRP levels. 7 The use of bezafibrate was also found to decrease monocyte release of MCP-1, IL-6, TNF-α and IL-1β in mixed dyslipidemia subjects.6, 7 It is evident that bezafibrate exerts its anti-inflammatory action by negatively interfering with NF-kB through PPARα. 10 As was previously mentioned, dyslipidemia by itself can cause inflammation. Thus, the anti-inflammatory effect may be partly explained by its hypolipidemic actions as well. 16
The present study reinforces the previous study results that bezafibrate may have anti-inflammatory potential. This anti-inflammatory and hypolipidemic effect of bezafibrate will have an added advantage in the management of atherosclerosis and its complications. Further, the role of bezafibrate in other inflammatory diseases, in patients with dyslipidemia, and insulin resistance has to be evaluated.
Conclusion
In animal models of both acute and subacute inflammation, bezafibrate has shown significant anti-inflammatory effect that was almost equivalent to the anti-inflammatory effect of aspirin. The use of bezafibrate in treating dyslipidemia can reduce the atherosclerotic complications on account of their anti-inflammatory and hypolipidemic properties. Moreover, fibrates like bezafibrate might open up novel opportunities for treating various inflammatory diseases.
Footnotes
Acknowledgements
Authors would like to thank the technical staff and the Central animal house of KLE University’s J N Medical college Belagavi for their support during the study.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The study was conducted after obtaining approval from the Institutional Animal Ethics Committee (IAEC) - MDC/AH/3(2).
Funding
The author received no financial support for the research, authorship and/or publication of this article.
Abbreviations
PPARα - peroxisome proliferators activated receptors alpha
HDL- high-density lipoprotein
CRP- C reactive proteins
IL - interleukin
TNF-α - tumour necrosis factor alpha
MCP 1 - monocyte chemoattractant protein 1
IAEC - Institutional Animal Ethics Committee
CPCSEA - Committee for the Purpose of Control and Supervision of Experiments on Animals
LDL - low-density lipoprotein
NF-kB - nuclear factor-kappa B
STAT - signal transducer, activator of
transcription
AP-1 - activator protein-1
ANOVA - analysis of variance
SEM - standard error of the mean.


