Abstract
Peripheral nerve plexus blocks have replaced general and neuraxial anaesthesia as the preferred method of anaesthesia for single-limb procedures. The present case report aimed to assess the effectiveness of combined peripheral nerve blocks (PNBs) as the sole anaesthetic option intraoperatively as well as for postoperative pain relief for total hip replacement in elderly patients with comorbidities, as it maintains hemodynamic stability, avoids complications associated with general anaesthesia and neuraxial anaesthesia, improves postoperative analgesia, and reduces the incidence of perioperative MI. This is a case report of a 69-year-old elderly male with hypertension and coronary artery disease who underwent left total hip replacement with continuous combined lumbar and sacral plexus blocks. Thus, to conclude, it was found that combined lumbar and sacral plexus nerve block with sedation provides adequate surgical anaesthesia intraoperatively and postoperative analgesia for unilateral hip surgeries without affecting haemodynamics.
Study Highlights
Following total hip replacement, pain can vary and may become severe.
Regional anaesthesia can enhance functional outcomes and is associated with decreased perioperative mortality and morbidity.
Continuous lumbar and sacral plexus blocks provide effective surgical anaesthesia for total hip replacement.
Continuous sacral and lumbar nerve blocks should be established and maintained using low-concentration local anaesthetic solutions to minimise motor block during the postoperative period.
Introduction
Major surgical procedures with a high risk of perioperative morbidity include primary hip and knee arthroplasty. In order to lower perioperative morbidity, anaesthesia can be very helpful.[1] Preventing myocardial ischaemia and MI is the main objective of the anaesthetic care of a patient with coronary artery disease undergoing non-cardiac surgery. This is achieved by avoiding factors that affect myocardial oxygen supply-demand balance.[2] The risks associated with general anaesthesia primarily involve airway management, respiration (including soft tissue injuries in the mouth and teeth, vocal cord trauma, barotrauma from positive pressure ventilation, aspiration, etc.), and circulation (including negative inotropic and chronotropic cardiac effects from anaesthetics).[3] Changes in cardiovascular physiology in older individuals with cardiac conditions reduce cardiovascular reserve and increase the risk of hemodynamic instability following spinal anaesthesia; as a result, these patients may experience postoperative problems.[4] The use of newer modalities like ultrasound and peripheral nerve stimulators in regional anaesthesia has expanded the scope of anaesthesia from general and neuraxial anaesthesia to peripheral nerve blocks (PNBs) for isolated limb surgeries. Complete lower limb anaesthesia is achieved when a lumbar plexus block and a sacral plexus block are administered together.[5] Reducing stress and unfavourable haemodynamics depends on effective pain management in patients with coronary heart disease.[2] The available data supports PNBs as a means of providing postoperative analgesia, resulting in earlier and better recovery. They also reduce reflex muscle spasms and allow for earlier, more efficient joint mobilisation and physiotherapy. They also prevent the systemic side effects of PCA morphine (sedation, PONV) and continuous epidural analgesia (hypotension, urine retention).[1] Considering the complications associated with general and neuraxial anaesthesia, we decided to proceed with the case with a combined lumbar and sacral plexus block as a sole anaesthetic for a left total hip replacement as it provides complete lower limb surgical anaesthesia, postoperative analgesia, maintains hemodynamic stability and also helps in early mobilisation.
Case Description
A 69-year-old elderly male with a past medical history of hypertension and coronary artery disease presented with complaints of pain in the left hip and was diagnosed with post-traumatic osteoarthritis with a screw intrusion that was fixed four years ago for a left neck femur fracture. Now, he was scheduled for left THR with screw removal. He underwent cryoablation for atrial fibrillation with severe LV dysfunction one year ago and percutaneous transluminal angioplasty to the right coronary artery four years ago for RCA stenosis. The patient was on tablet apixaban 2.5 mg, clopilet 75 mg, spironolactone, and frusemide. His laboratory investigations included a complete blood count with haemoglobin levels of 17 g/mL and a platelet count of 1.79 lacs/mm3. Liver function, kidney function, serum electrolytes, coagulation profile, and blood sugar levels were also normal. An electrocardiogram (ECG) revealed an old inferior wall MI and an echocardiograph demonstrated a regional wall motion abnormality, moderate left ventricular dysfunction, mild aortic regurgitation, mild tricuspid regurgitation, and an ejection fraction of 40% with inferoapical hypokinesia. His chest X-ray revealed increased bronchovascular markings and the venous Doppler of the bilateral lower limb showed no evidence of deep vein thrombosis. On examination, he showed no signs of heart failure, and his vitals were stable. Since it was not an emergency, he was advised to stop tablet apixaban three days before surgery and tablet clopilet 75 mg five days before surgery. Other medications were continued in the perioperative period.
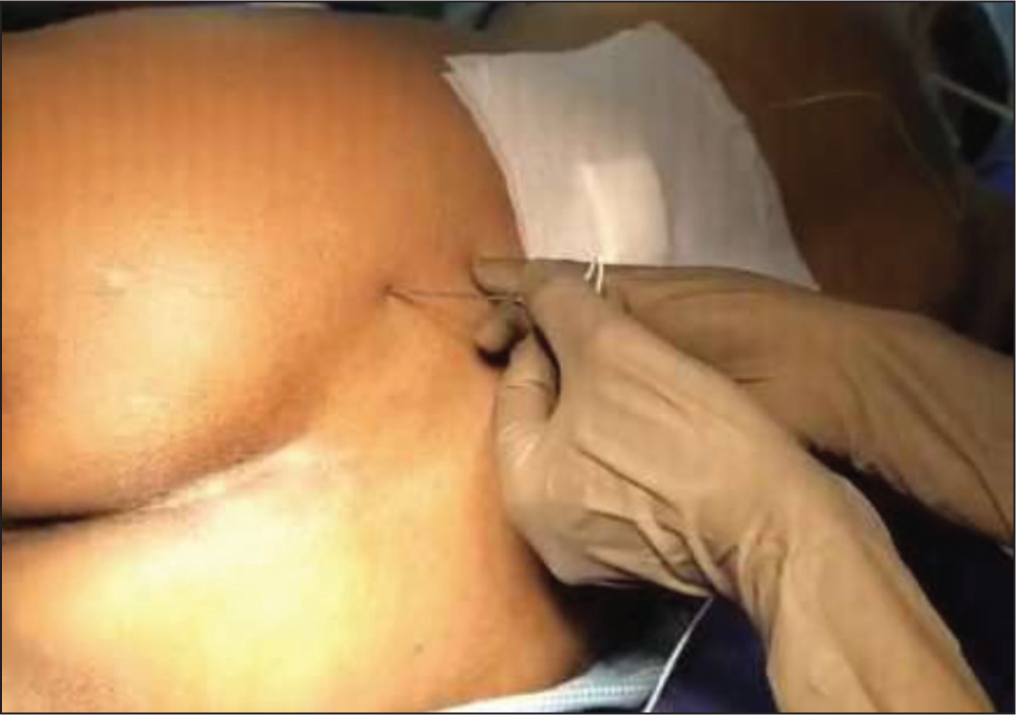
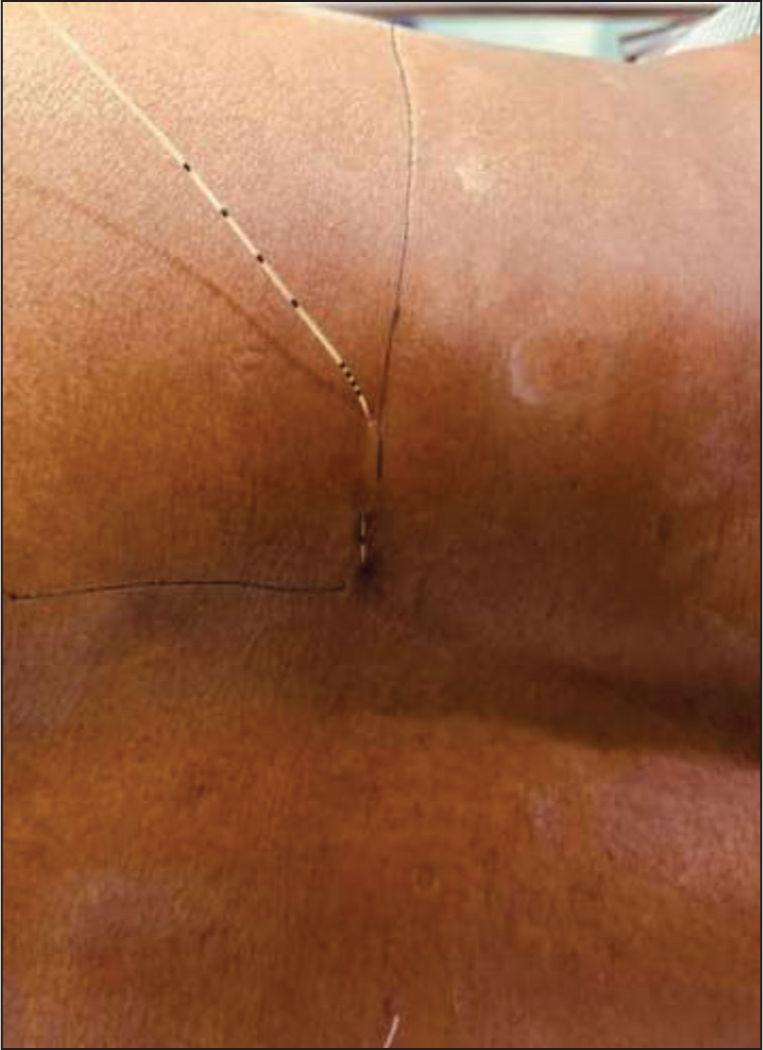
On the day of surgery, in the operating theatre, standard monitors were attached, and pre-operative baseline vitals (HR-85 bpm, BP-140/80 mmHg, and SpO2 -97% on room air) were recorded. An IV line was established, and a plasmalyte solution was started. A small amount of sedation was given with fentanyl (50 mcg) and midazolam (1 mg) intravenously, along with oxygen delivered via facemask at 4-5 LPM, to ensure the patient’s comfort for the block procedure. A solid gel skin electrode was placed at the mid-thigh level. The patient was positioned in the right lateral decubitus position, with the operated side on top, and received a combined lumbar and sacral plexus block with a nerve stimulator [Figure 1]. The needle was inserted perpendicularly at the intersection of two lines: an intercristal line at the level of L4-5 and a line parallel to the spine passing through the posterior superior iliac spine with a slight medial angulation. After infiltration over the entry point with 5 ml of 2% lignocaine, the block was performed using an 18G, 100 mm contiplex needle with the nerve stimulator at a current of 4 mA of 0.1 ms, 2 Hz. The needle could be redirected caudally if the transverse process of L5 was encountered. The endpoint for the lumbar plexus was taken as a quadriceps muscle twitch. The current was lowered until a motor response was visible at 0.4 mA, and contractions obtained at less than 0.3 mA were not accepted to avoid intraneural injection. Once the lumbar plexus was reached, a bolus of 30 ml of 0.25% bupivacaine was given after frequent negative aspiration to avoid intravascular injection, and if resistance was encountered in injecting drugs, the needle position was adjusted. After that, an indwelling nerve block catheter was inserted and fixed [Figure 2].
Sacral plexus block-entry point with simulating needle
Indwelling catheter in lumbar plexus
For the sacral plexus block, the anatomical landmark of needle insertion was 6 cm caudad to the line joining the PSIS and the ischial tuberosity. The stimulating needle was inserted perpendicular to the gluteal muscles [Figure 1]. If it hits the sacral plate, the needle tip should not be more than 1.5-2 cm beyond the sacral plate. The evoked muscle responses were either plantar flexion or dorsiflexion of the foot and hamstring muscle contraction at 0.4 mA. 10 ml of 0.09% ropivacaine was administered for the sacral plexus block after frequent negative aspiration and an indwelling nerve block catheter was inserted.
Patient sensory blockade was assessed by loss of pinprick sensation in the operative site and motor blockade was evaluated with bromage scale. Bromage scales 3 and 4 were acceptable for surgery.
Our alternative plan was to convert it into general anaesthesia with an ET tube if the blocks were not satisfactory. After confirmation of satisfactory sensory and motor blockade in the operated limb, the patient was clinically sedated with propofol infusion at a dose of 25 mcg/kg/min to maintain Ramsay’s sedation score of 3–4 to avoid positional discomfort. The patient was then repositioned for surgery. PETCO2 was monitored through the nasopharyngeal airway along with other standard monitors. The incision time for surgery was 30 minutes after block placement.
Vitals remained stable throughout the surgery. The drug concentrations used for the combined lumbar and sacral plexus block were sufficient for intraoperative sensory and motor blockade. The procedure duration was two hours.
Postoperatively, a nerve block infusion of 0.18% ropivacaine was initiated at a rate of 10 ml per hour for the lumbar plexus and 0.09% ropivacaine at a rate of 2 ml per hour for the sacral plexus. The patient also received intravenous paracetamol 1g every 12 hours.
Foley catheterisation postoperatively was avoided due to the use of a low concentration of ropivacaine for nerve blocks, which does not induce motor blockade. Postoperative pain was assessed by VAS score. His VAS score never exceeded two at various time intervals until the nerve block catheters were removed, so he did not need any other rescue analgesics. He was allowed to mobilise after four hours following surgery, and no complications related to the block were observed.
Injection of unfractionated heparin 5000U OD was administered for three days. On the first postoperative day (POD), clopidogrel was resumed. Nerve block catheters were removed on the second postoperative day, and the patient was discharged. The cardiologist recommended starting apixaban.
Discussion
When it comes to the perioperative management of elderly patients, hemodynamic instability is a major issue due to long-term drug intake and comorbidities induced by chronic underlying conditions like hypertension, diabetes mellitus, and cardiovascular diseases.[6] The principle for anaesthesia selection is to reduce or avoid the effect of anaesthesia on systemic and vital organ functions as much as possible.[7] A combined PNB for THA may have the following benefits: fewer opioid requirements, shorter PACU discharge times, less discomfort during early ambulation and participation in physical therapy programmes, avoidance of stressful intubation, elimination of multiple attempted lumbar punctures, improved hemodynamic stability, and overall higher patient satisfaction.[8] While the sacral plexus block blocks the sciatic nerve, posterior cutaneous nerve of the thigh, superior and inferior gluteal nerves, pudendal nerve, pelvic splanchnic nerve, inferior hypogastric plexus, and the terminal portion of the sympathetic trunk, the lumbar plexus block blocks the femoral nerve, lateral femoral cutaneous nerve, and the obturator nerve.[5] So perhaps a better option would be peripheral nerve blockade with combined lumbar and sacral plexus block, which acts on a single leg only and produces a smaller physiological disturbance with a similar anaesthetic effect.[9]
Similar to our case, Shah et al.’s study[5] found that combined lumbar and sacral plexus blocks maintain hemodynamic stability. To prevent complications related to nerve blocks, we performed frequent aspiration before injecting the drug, avoided injecting drugs against high resistance, and ensured that the twitch response was <0.3 mA. Amiri et al.[6] also referenced similar precautions in their research.
Similar to the work done by S et al.,[9] in our case, combined lumbar and sacral plexus block provided excellent perioperative and postoperative analgesia without any problems related to nerve injury, hypotension, or contralateral leg blockade.
With all the advantages of PNBs compared to general anaesthesia and neuraxial blockade, combined lumbar and sacral plexus blocks were chosen as the preferred anaesthetic method for our patient.
Conclusion
In hip replacement surgery, continuous lumbar and sacral plexus block can be used as an alternative sole anaesthetic option, particularly for elderly patients with coronary artery disease. This method maintains hemodynamic stability better than neuraxial blockade and general anaesthesia. It provides good muscle relaxation and intraoperative analgesia. Additionally, it offers effective postoperative analgesia through continuous infusion, facilitating early mobilisation and discharge.
Footnotes
Acknowledgements
To the Research Department Apollo Hospitals, Chennai.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Ethical Approval
Institutional ethical committee approval has been obtained.
Patient consent
Verbal informed consent was obtained from the patient.
Credit author statement
Conceptualization and design of the study report: Vinitha and Senthil Meena.
Data collection and analysis: All authors.
Writing manuscript: Vinitha.
Referencing Vinitha.
Multiple draft versions including rewriting the revised submission: Vinitha, Senthil Meena.
Administrative support: Vasantha Roopan.
Concept and identification of unmet need in available literature: All authors.
All the authors have reviewed and approved the manuscript.
Data availability
Yes.
Use of artificial intelligence
Nil.
