Abstract
Background:
Advances in digital technology have led to widespread availability of digital devices and consequent increased usage amongst across the population including practising healthcare professionals. Increased ‘Digital Screen time’ and its effect on physical, psychological health, and sleep patterns has been predominantly evaluated in children, adolescents and adults from various walks of life.
Purpose of the Study:
The purpose of this survey was to evaluate the impact of Digital Screen usage (time and patterns) spent on portable and desktop digital devices amongst physicians, surgeons and radiologists.
Material & Methods:
An online cross-sectional survey of an 11-part questionnaire (multiple choice questions and free text box) was circulated amongst orthopaedic surgeons, radiologists and physicians in India and the UK, to evaluate demographics, speciality and place of practice; Digital platform usage reasons and time; effect on mental health, physical health, sleep time amongst practising healthcare professionals.
Results:
There was an even spread amongst the various age groups. Smartphones were the commonest device utilised for digital screening in 90 (67.7%) doctors with 29 (38.5%) of doctors reporting more than five hours of daily screen time. Sixty-three (47%) of doctors used this for academic purposes, whereas 43 (32%) used it for entertainment more than for academic purposes. Thirty-nine doctors (29%) were unaware of whether screen usage affected mental health. Seventy-two (53%) were of the opinion that screen usage was having a negative effect on their physical health whilst 81 (60%) thought that it was having an adverse effect on their sleeping time respectively.
Conclusion:
A significant proportion of doctors appear to be using digital devices beyond the recommended ‘Digital Screen time’ by various national or international healthcare organisations. There is an emerging need to highlight the deleterious effect of excessive ‘Digital Screen time’ on various health parameters and be part of a global health narrative to mitigate ill-effects and a sustainable lifestyle.
Keywords
Introduction
Revolution in Information and Communication Technology coupled with Digital Innovation has allowed the use of various digital devices (such as smartphones) in every walk of life with enhanced access to the internet and other web applications affecting human interactions.[1] ‘Digital Screen Time’ represents the amount of time spent on devices with ‘screens’ such as smartphones, tablets, laptops or computers, video game consoles.
Digital technologies have had an increased influence on healthcare applications with improved efficiency, ability to access patient data instantly, streamlining diagnoses and treatment plans.[2-4] Mobile health (mHealth) referring to the use of cell phone technology to deliver health care has become ubiquitous due to faster fifth-generation (5G) smartphone technology and high-speed data transfer capabilities.[5]
The use of portable digital devices has transformed the delivery of health care. For example, digital screens replacing clipboards, radiographs may be viewed on tablets and patient information transfer through electronic health or patient records (EHR or EPR), particularly evident during the COVID-19 pandemic in a variety of clinical settings.[6-8] EPR eliminate the risk of lost or misplaced patient charts, ensuring continuity of care. Telemedicine consultations via video chat screens expand access to care, especially for patients in remote areas.
While this digital transformation offers undeniable benefits, it is crucial to acknowledge the potential downsides and ensure doctors maintain a human touch. The deleterious effects of excessive ‘Digital Screen Time’ and usage have been highlighted in the literature, particularly in children and adolescents leading to various health harms including those of obesity, myopia attention disorders, anxiety and depression[9,10] effects
The use of smartphones and medical applications has been evaluated amongst doctors, medical students and junior doctors and other clinical settings; however, literature has not examined patterns of digital usage amongst a spectrum of doctors in different medical subspecialties in two different practising countries with diverse health systems such as the UK and India.[11-13]
The purpose of this survey was to evaluate the impact of Digital Screen usage (time and patterns) spent on portable and tabletop digital devices amongst physicians, surgeons and radiologists. Perceptions of Digital screen time on physical, psychological health, and sleep patterns amongst these healthcare professionals have been explored.
Material and Methods
Study Design
This cross-sectional study (online questionnaire survey) was conducted in March 2024 for a period of four weeks amongst Orthopaedic, Radiology and physicians practising in the United Kingdom and the Indian healthcare system. An online questionnaire was developed, with both multiple choice questions (11) and free text box for comments, using the Google Forms platform to maximise ease of processing, data collection, and facilitate evaluation. Survey questionnaire and options have been highlighted in Supplementary File 1.
The survey was kept open for response submission for four weeks, with a reminder notification sent halfway through, after which submitted responses were collected, scrutinised and summarised accordingly.
Inclusion and Exclusion Criteria
The questionnaire was circulated using social media platforms in orthopaedic, medical and radiology forums. Non-clinicians and those not practising healthcare medicine were excluded from the study.
Data Collection
The responses submitted were checked for duplication, pooled, analysed and summarised.
Evaluation Points
The questionnaire focussed on the following views:
Demographics, place and speciality of practice Average digital screen time and purpose of its use: academic or for enterprise Reasons for digital technology usage in clinical practice and academic activities Impact on mental, physical health and sleeping patterns amongst the clinicians
Statistical Methods
Microsoft→ Excel data sheet was used for data collection and descriptive analysis was performed to summarise the data.
No funding was received from any individual or institution for this study. Institutional review board approval was not required for this survey-based study.
Results
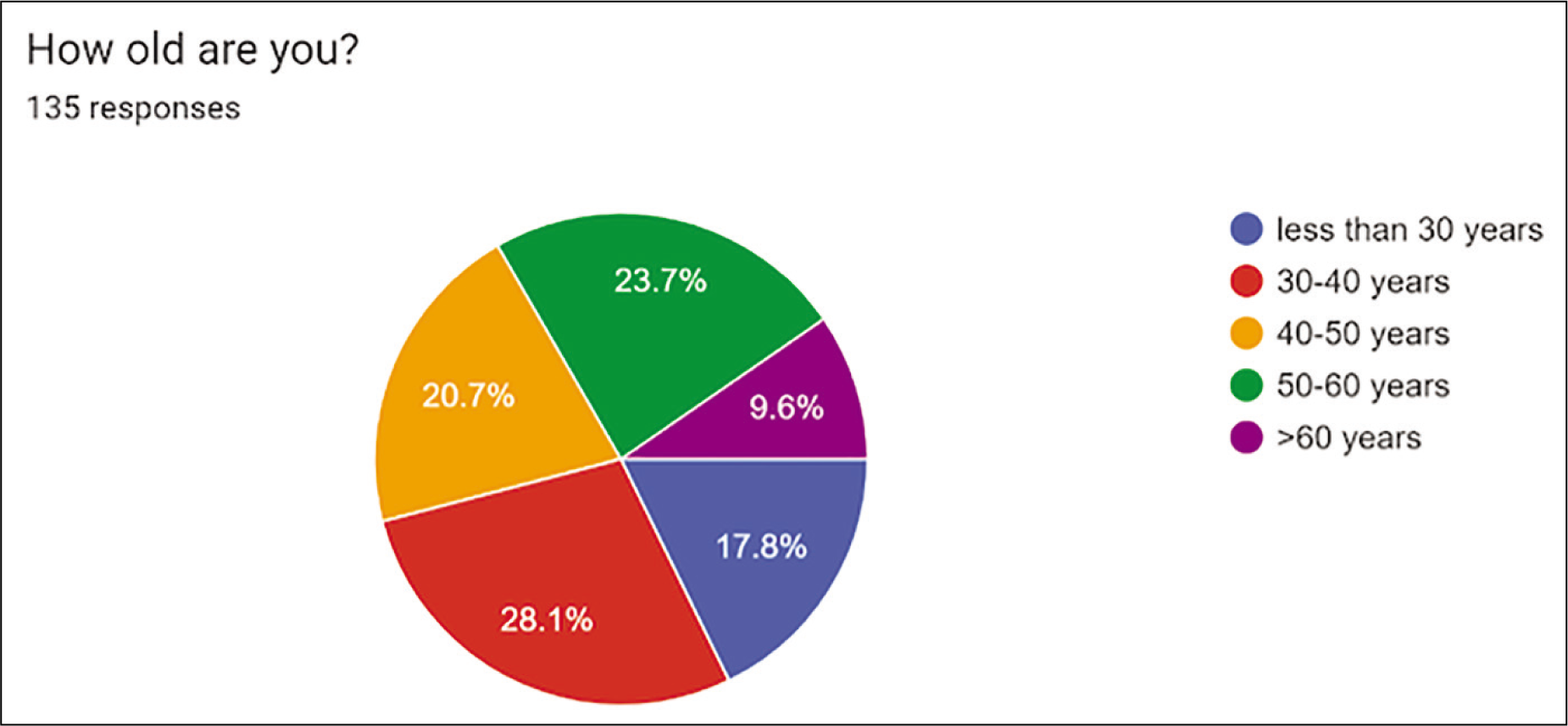
Demographics, place and speciality of practice: A total of 135 replies were received of which 79 (58.5%) are radiologists, 38 (28.1%) are physicians, 18 (13.3%) are surgeons. 28% of doctors participating in survey were aged between 30 and 40 (28.1%), 32 (23%) 50-60 years, 28 (20.7%) 40-50 years, 24 (17.8%) less than 30 years, 13 (9.6%) greater than 60 years [Figure 1]. 36.3% of doctors are working in Tertiary hospitals, 24.4% in each of University Hospitals or Private Hospitals and 20 (14.8%) in a District General Hospital.
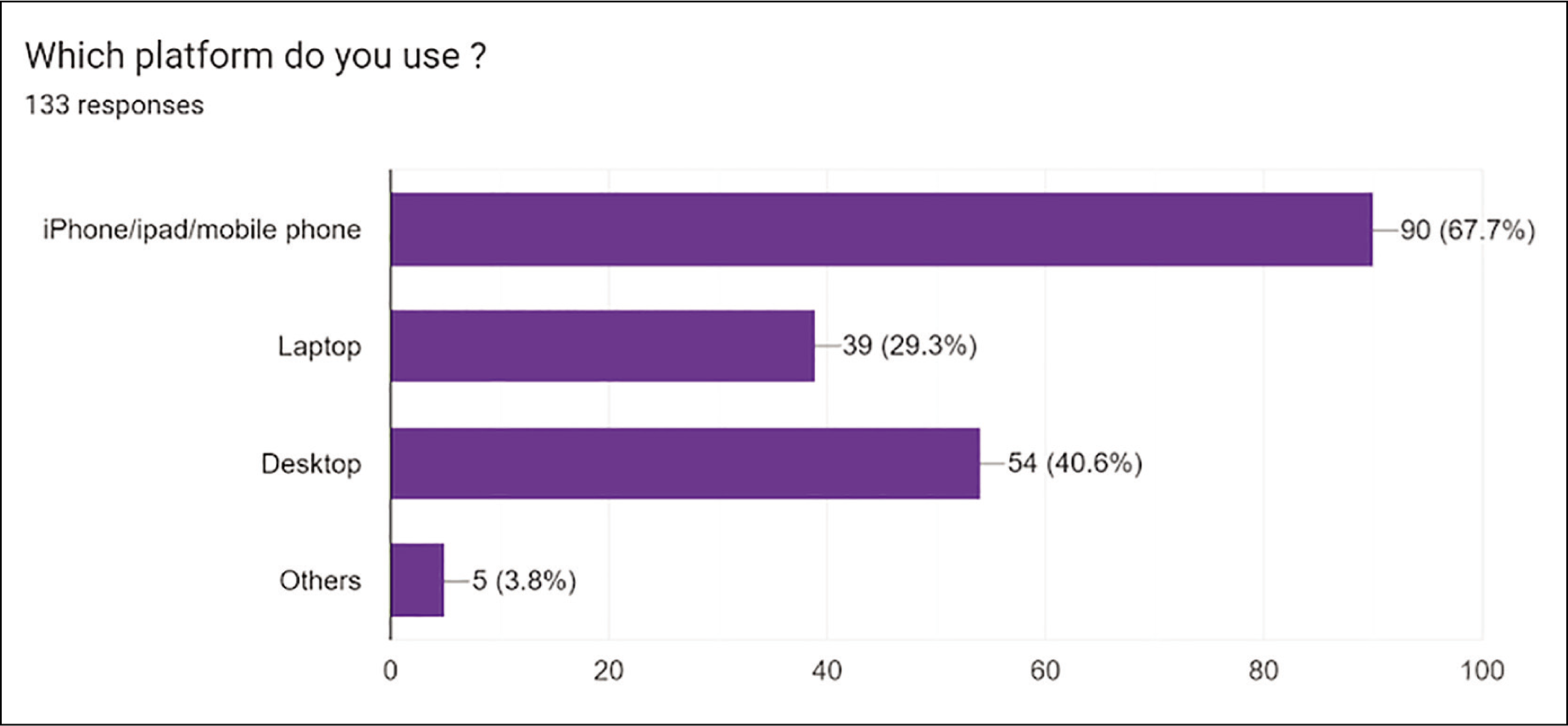
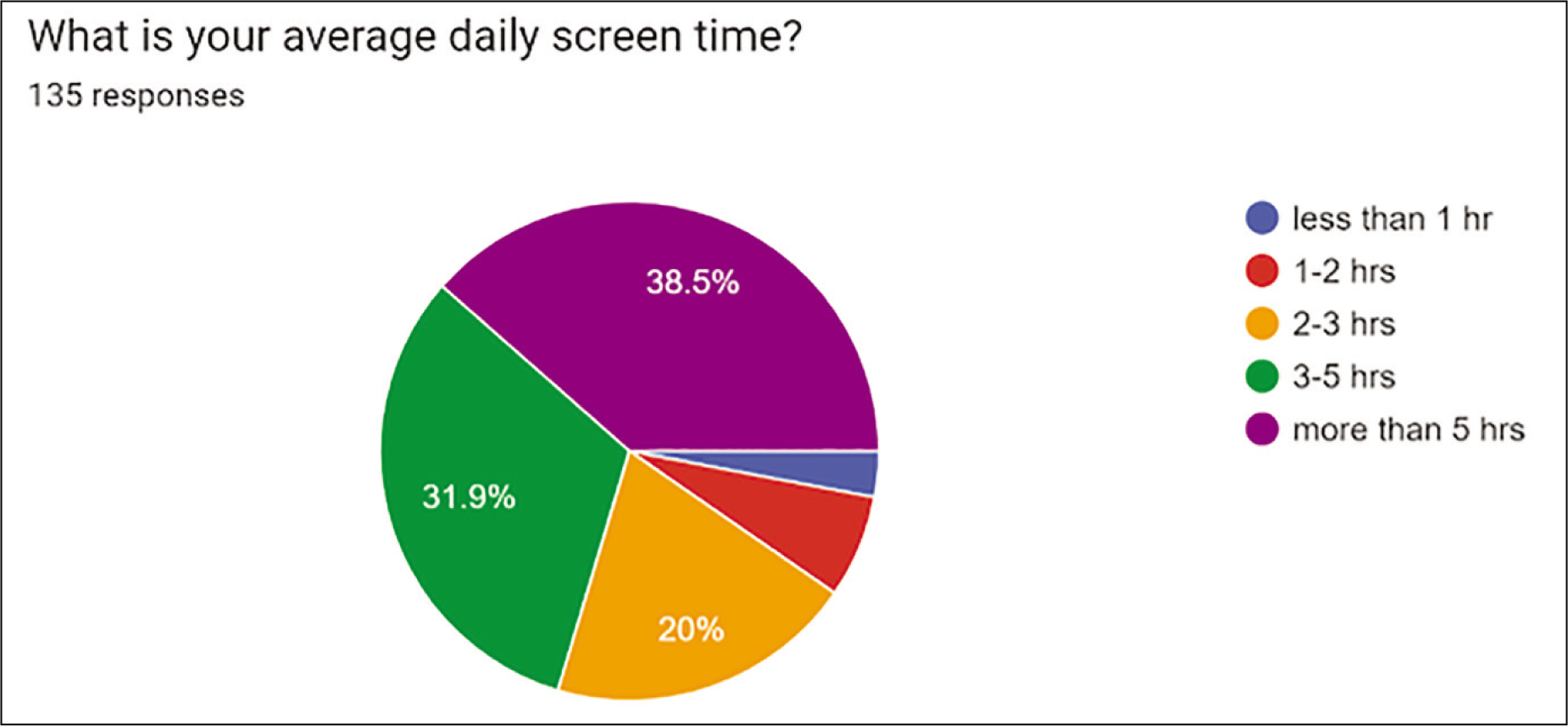
Digital Screen Time: Average daily screen time was less than one hour in 4 (3%), one to two hours in 9 (6.7%), two to three hours in 27 (20%), three to five hours in 43 (32%), more than five hours in 52 (38.5%). 90 (67.7%) of doctors utilised a mobile phone or tablet; 54 (40.6%) used desktop, 39 (29.3%) used laptop and 5 (3.8%) used other types of screen [Figure 2]. The main mode of screen usage was from mobile phone/tablet 90 (67.7%%) with an average daily screen time of more than five hours in 29 doctors (38.5%) [Figure 3].
Reasons for digital technology usage: Out of 135 doctors participated in survey 118 members (87.5%) are using phone and laptop for both academic/entertainment purposes. 63 (47%) of doctors used this for academic purposes more than for academic purposes, whereas 43 (32%) used it for entertainment more than for academic purposes; the remaining 29 (21.5%) used it for both equally.
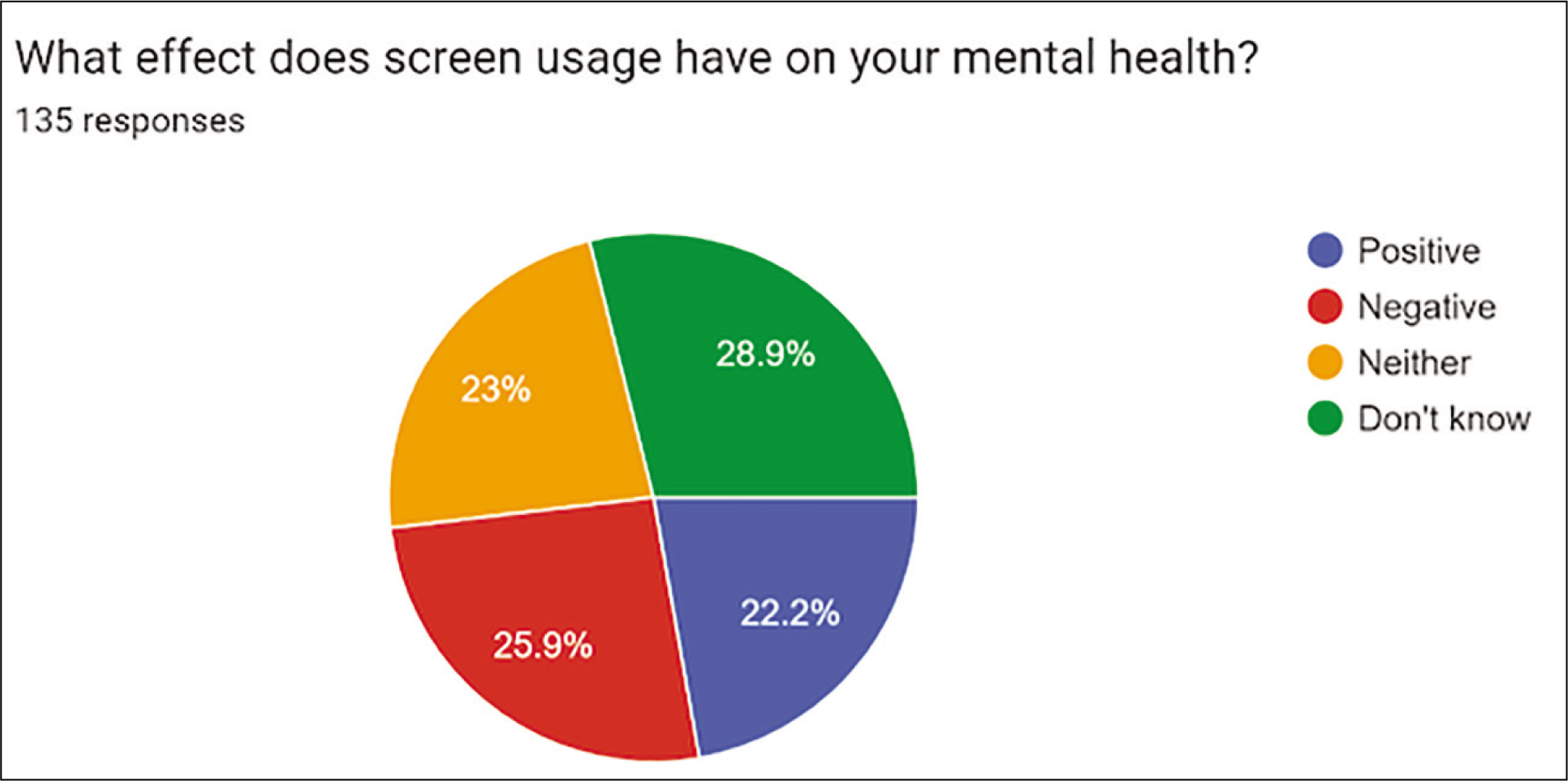
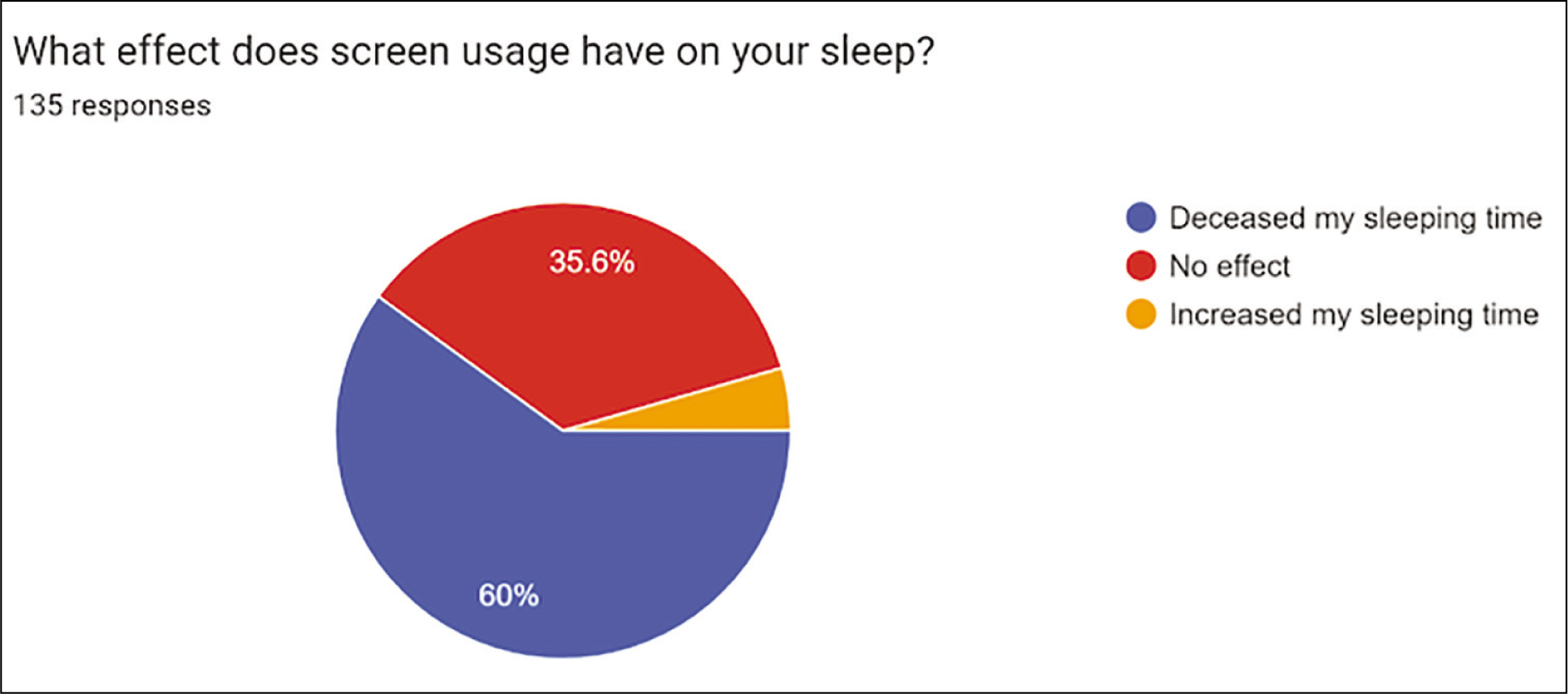
Impact on mental, physical health and sleeping patterns amongst the clinicians: 39 (29%) participants stated they are unaware of whether screen usage affects mental health. 30 (22.2%) said it had a positive impact, 35 (26%) said it had a negative impact and 31 (23%) said they were indifferent [Figure 4]. The majority of doctors, 71 (53%), stated screen usage had a negative impact on their physical health. 33 (25%) stated they did not know what effect it had, 23 (17.2%) were indifferent to the effects on health and 7 (5.2%) stated it had a positive impact on physical health [Figure 5] 81(60%) stated that they had a negative effect on sleeping time; 48 (35.6%) had a positive effect and 6 (4.4%) had an increased sleeping time [Figure 6].
Demographics: Pie chart showing age of participants
Bar chart demonstrating digital platform usage by type amongst the clinicians
Pie chart demonstrating digital screen usage time in hours amongst the clinicians
Pie chart demonstrating the perceived effect of screen usage on mental health
Pie chart demonstrating the effect of screen usage on physical health
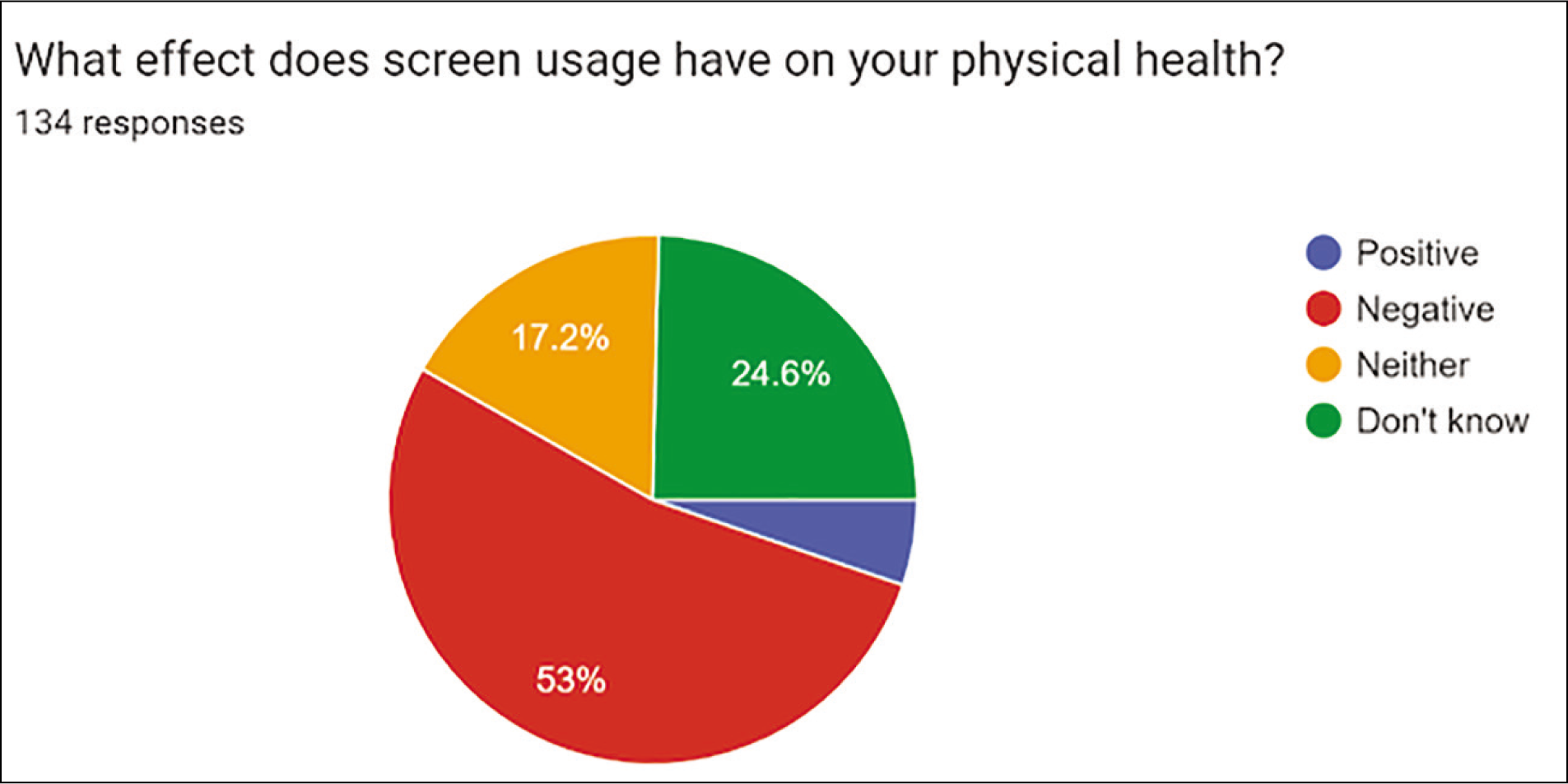
Pie chart demonstrating the effect of screen usage on physical health
Discussion
The rising utility of computer-based systems within modern healthcare systems has led to significant changes in digital screen time amongst healthcare professionals. This stems from a general drive for information technology (IT) based healthcare systems, evident in the National Health Care (NHS) within the United Kingdom, which outlines its commitment to digital care records and referral systems to better streamline patient care.[14] This is compounded by rising personal screen time usage from social media, digital utility products, entertainment and research activities which healthcare workers often engage in.[15] As a result, a healthcare professional is likely to have significant and increasing screen time usage; 38% of patients in our study reported an average screen time of more than five hours per day and only 3% reported a screen time of less than 1 hour. Further factors such as the department or specialty may also be contributory factors; typically, a radiologist would be expected to spend a larger proportion of their day interpreting images whilst sitting at a desk, compared to a surgeon who standing during theatre lists.[16]
Although technology has led to significant increases in efficiency, accessibility and delivery of services in healthcare, high digital screen usage can also have negative effects on an individual. These include sleep disturbance (reduction or disruption), mental health issues (anxiety and depression) and physical health issues (obesity, back pain and visual disturbance).[17,18]
In our cohort, 26% of doctors stated that their current screen time usage had a negative effect on their mental health. Several studies have investigated this correlation. One factor that may contribute to this is information overload. Individuals are exposed to vast amounts of electronic information, compared to the equivalent in a physical format which would traditionally take longer to filter through, and this requires a more rapid processing of information within a shorter space of time. Another factor is the accessibility of work-related data remotely; the recent COVID-19 pandemic which has been a catalyst in digital infrastructure to enable this.[19] This may blur the boundaries between professional and personal life, leading to a poorer work-life balance and subsequent increased stress and anxiety levels.[20] However, the flexibility offered by home-working does carry many benefits, especially with childcare, commuting and economically, as evidenced by 26% of our cohort who reported a positive impact on their mental health.[21] Furthermore, the post-pandemic rise in medical teleconsultations has resulted in a reduction of direct patient interaction which could contribute to poorer mental health through a sense of detachment or poor job satisfaction.
Thirty-five percent of patients reported a change to their sleep pattern or time, and this finding has been echoed in multiple studies.[22] This is primarily thought to be due to the impact of the blue light emitted by digital screens. Blue light may suppress the production of melatonin which is an essential regulatory hormone for the circadian rhythm. This results in a delay in the onset of sleep or a reduction in the quality of sleep. The type of content engagement will also contribute towards this; checking stressful work emails is expected to have a relatively negative impact when compared to playing a game, although both emit blue light. Newer smartphones have a ‘night mode’ functionality which transforms much of the ‘blue light’ to a ‘warm light’ to mitigate this. Other studies in healthcare professionals, for example during the COVID-19 pandemic, have also found a correlation between digital screen time and disruption of sleep.[23]
The majority of the patients (56%) in this study reported a negative effect on physical health which may occur in several forms; digital eye strain, neck and back pain, weight gain and strain injuries (e.g., carpel tunnel syndrome). Digital eye strain is an entity characterised by visual and ocular symptoms such as dry eyes, blurred vision and headaches.[24,25] It has previously been demonstrated that higher screen times are associated with myopia (near-sightedness) and certain authors have suggested it may contribute to retinal damage.[26] Extended periods of sitting and poor posture, typically occurring with prolonged time at a desktop screen, may cause or aggravate lower back pain. A flexed lumbar posture results in a decreased variation in muscle activity which results in a difficulty to deactivate lumbar muscles during periods of rest. This contributes to increased muscular fatigability, altered biomechanics and back pain.[27,28] Although varying between disciplines, healthcare professionals can do a large proportion of sedentary job-related duties with relatively low levels of activity.[29] Ryan et al. reported employees with a desk job spent 66% of their time seated.[30] Reduced energy expenditure can result in healthcare workers gaining weight and developing metabolic syndromes; Sari et al. reported 51.9% and 14.8% of physicians were overweight or obese, respectively, in their study. The effects of desk screen use on back health and calorie balance can be addressed through the introduction of standing desks and breaks with exercise.[27] For example, Josaphat et al. found that food consumption and satiety were not affected despite the use of standing desks, suggesting this may produce a calorie deficit.[31] It is important for healthcare professionals, and the departments that they work in, to have an awareness of the impact of a sedentary job routine on their physical health so that they may put measures in place to prevent this.
Conclusion
Technological developments of recent decades have transformed healthcare systems to be more digitalised in their approach to patient care and pathways. As a result, healthcare workers, in particular doctors, have significant screen time usage due to their work, which is compounded by personal or research activities. Although usage of screen-based devices may have certain positive impacts on an individual’s lifestyle, it is vital that healthcare workers are aware of the potential negative effects on sleep quality, mental wellbeing and physical health which may follow prolonged screen time.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Institutional ethical committee approval number
No patients were involved in the study. Institutional review board approval was not required for this survey-based study.
Credit author statement
Conception and design, or acquisition of data, or analysis and interpretation of data: Chapala S, Botchu R
Design, or acquisition of data, or analysis and interpretation of data: Chapala S, Botchu R
Drafting the article or revising it critically for important intellectual content: Chapala S, Hussein M, Shirodkar K, Iyengar KP, Vaishya R, Botchu R
Final approval of the version to be published: Chapala S, Hussein M, Shirodkar K, Iyengar KP, Vaishya R, Botchu R
Patient consent
Consent was not applicable, as this is a review article compiled from various research articles and guidelines and not from patients directly.
Data availability
Data is available to share on request.
Use of artificial intelligence
No form of AI was used in the preparation of this work.
